Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
Clean Air Journal
On-line version ISSN 2410-972X
Print version ISSN 1017-1703
Clean Air J. vol.28 n.2 Pretoria 2018
http://dx.doi.org/10.17159/2410-972x/2018/v28n2a19
RESEARCH ARTICLE
A critical review of health risk assessments of exposure to emissions from coal-fired power stations in South Africa
Kristy E. LangermanI,* ; Christiaan J. PauwII
IDepartment of Geography, Environmental Management and Energy Studies, University of Johannesburg, PO Box 524, Auckland Park, 2006, South Africa, klangerman@uj.ac.za
IIThe Nova institute, 13 Beuke Place, The Willows Ext 14, Pretoria, South Africa, christiaan.pauw@nova.org.za
ABSTRACT
Emissions from coal-fired power stations increase the incidence of respiratory, cardiovascular and cardiopulmonary diseases and contribute to premature deaths. Wildly varying estimates of the magnitude of these health impacts have been published, however. This paper investigates the reasons for the large discrepancies calculated in five comprehensive health risk assessments of South African coal-fired power station emissions. We review the approaches and input data used by the studies. We also evaluate the exposure-response functions (which relate the pollution concentration to which the population is exposed, to the increase in health risk) used by each study and pay specific attention to whether the exposure-response functions are relevant to the South African context. Health risks are under-estimated in studies that only consider impacts in industrialised areas, or assume high counterfactual concentrations. Health risks are probably over-estimated, however, in other studies which use linear or exponential exposure-response functions that are not applicable in areas where exposure levels are much higher (such as solid fuel-using communities). A more accurate estimate of health effects would be obtained by applying integrated exposure-response functions to quantify health risks at actual exposure levels, and then apportioning the health effects relative to the contribution made by each source to total exposure levels. A fair assessment of the health risk of South Africa's older coal-fired power stations should also weigh the health costs of the emissions against the health benefits of electricity use in lower income households.
Keywords: health impact, coal-fired power stations, exposure-response function, electrification.
Introduction
The World Health Organisation (WHO 2016) estimates that there were 3 million premature deaths worldwide in 2012 due to ambient particulate matter pollution. A premature death is a death that occurs before the average age of death in a certain population (National Cancer Institute 2015). The health risk is spread disproportionately across the globe, with highest risks in low- and middle-income countries in the Western Pacific (where there were on average 65 age-standardised deaths per 100 000 capita attributable to ambient air pollution in 2012). There is a much lower risk due to ambient air pollution exposure in North and South America (only 7 age-standardised premature deaths per 100 000 capita in high-income countries, and 18 age-standardised premature deaths per 100 000 capita in low- and middle-income countries in 2012; WHO 2016). In South Africa, 14 356 premature deaths were estimated to have occurred in 2012 due to acute lower respiratory illness (ALRI), chronic obstructive pulmonary disease (COPD), lung cancer, ischemic heart disease (IHD) and strokes. These account for 3.0% of the 480 476 deaths that occurred in South Africa in 2012 (StatsSA 2014).
The South African Comparative Risk Assessment (Norman et al. 2007) estimated premature mortality from urban air pollution to be 4 637 (0.9% of all deaths) in 2000. These figures were calculated considering monitored particulate matter with aerodynamic diameter of less than or equal to 2.5 micrometres (PM2.5) and particulate matter with aerodynamic diameter of less than or equal to 10 micrometres ((PM10) concentrations, in the large metropolitan areas of Cape Town, eThekwini, Johannesburg and surrounds, Ekurhuleni, the Vaal Triangle and Nelson Mandela Metro, and so largely exclude the impact of power station emissions and other industrial activities on the Mpumalanga Highveld.
Fine particulate matter is derived from a large number of combustion sources, including power stations, industries, mines, vehicles, vegetation fires and domestic burning. There have been many attempts to apportion particulate matter to the sources from which it is derived, based on chemical signatures of particulate samples (for example, Annegarn et al. 1999) and chemical transport or dispersion modelling (for example, the Highveld and Vaal Triangle Priority Area Baseline Assessments). Apportionment of the particulate matter is no easy task because the bulk of fine particulate matter is formed in the atmosphere (Maenhaut et al. 1996; Piketh et al. 1999). A source apportionment is, however, necessary in order to apportion the harmful health effects of particulate pollution.
The health impacts of emissions from power stations have received particular attention, with Myllyvirta (2014) and Holland (2017) calculating that around 2 239 deaths per year in South Africa are due to particulates from coal-fired power stations. These figures are much higher than those previously calculated by van Horen (1996) - 174 premature deaths per year; Scorgie et al. (2004; henceforth called the FRIDGE (Fund for Research into Industrial Development Growth and Equity) study) - 10 deaths per year; Scorgie and Thomas (2006; henceforth called the Airshed and Infotox study) - 17 deaths per year; and Grobler (2016) - 57 deaths per year. The reasons for the disparities in the estimates of the health effects of South Africa's coal-fired power station emissions are explored in this paper. Coal-fired power generation is but one source of many that contribute to ambient particulate matter levels in South Africa. Nevertheless, emissions from coal-fired power stations are the sole focus of this paper because of the magnitude of the emissions, their extensive area of impact, and the large investments required for emission reduction that are the subject of much debate in South Africa at the moment.
Health effects of coal-fired power station emissions
Impurities in coal are released during combustion in the boiler of a coal-fired power station. More than 99% of ash is removed by fabric filter plants or electrostatic precipitators in South African power stations, but most of the other pollutants, like sulphur dioxide (SO2), oxides of nitrogen (NOx) and trace substances like mercury are released, unabated, to the atmosphere (Pretorius et al. 2015). These pollutants are released through tall stacks (ranging between 152 m and 300 m for Eskom's power stations), are diluted and undergo chemical transformations, and finally come to the surface where they may be inhaled or affect the physical environment. As the plume ages, most of the SO2 and NOx is converted to secondary fine particulate matter in the atmosphere. Highest ground-level concentrations of SO2 and NOx typically occur during the day when turbulent eddies bring less diluted plumes to the ground, but plumes may also be advected for long distances (many tens of kilometres) before they are brought to the ground.
When pollutants from coal combustion (and other types of combustion) are inhaled, they may have a range of harmful effects on health during the entire human lifespan. This review only considers health risk assessments that focus on exposure to ambient particulate matter, SO2, NO2 and ozone (O3) (where included in the studies), but a more thorough review of the effects of power station emissions on health is given here to provide a comprehensive picture.
Exposure to air pollution affects early childhood development. Heavy metal and ultrafine particulates are able to cross the placental barrier and have the potential to harm the foetus and its developing organs (Wick et al. 2010). There is strong evidence that ozone and SO2 are associated with premature birth, with weaker evidence for particulates (Ha et al. 2014). Exposure to particulates, and perhaps also to ozone, NO2 and carbon monoxide (CO) during pregnancy may affect foetal growth and increases the risk of low birth-weight (Glinianaia et al. 2004; WHO 2013). The concern with premature birth and low birth-weight is that they have an impact on the developing organs.
Heavy metals, like lead and mercury, have been associated with neurodevelopmental harm, leading to reduced cognitive function, lower intelligence quotient (IQ), attention deficit hyperactivity disorder and possibly autism spectrum disorder during childhood (Canfield et al. 2003; Liu and Lewis 2014.
Young children are particularly vulnerable to the effects of air pollution. After birth, the organs are still maturing and infants have a relatively high metabolic rate so they breathe a greater volume of air than adults, relative to their size (RCP 2016). Early-life exposure to air pollution is also thought to cause epigenetic modification through changes in DNA methylation (Janssen et al. 2013; Jiang et al. 2014).
Long-term exposure to air pollution (particularly particulates, black carbon and NO2) suppresses the development of lung function (Chen et al. 2015; Hwang et al. 2015; Kulkarni et al. 2006), and may speed up the decline of lung function into older age (Rice et al. 2015; Adam et al. 2015). Even relatively small disturbances in the normal development or functioning of organs can significantly change the number of individuals in a population who develop diseases as a consequence. For example, a small change in lung function can shift the normal distribution of lung function in a population downwards, increasing the number of people in the lower tail who have low enough lung function to cause disease (RCP 2016). Acute exposure to high levels of air pollution results in an increased incidence of respiratory symptoms in children.
Outdoor air pollution causes instances of lung cancer (IARC 2013; Raaschou-Nielsen 2013). Long-term exposure to air pollution (NO2 and particulates) has been linked to the development of asthma (McConnell et al. 2010; Gasana et al. 2012; Anderson et al. 2013; Chen et al. 2015), and there is evidence that air pollution can make asthma worse in people who already have it. There is a strong link between air pollution and cardiovascular disease (myocardial infarction, heart disease and stroke) (Brook et al. 2010; WHO 2013; Newby et al. 2015).
Calculating health effects of air pollution
Ostro's (1994) impact pathway approach to calculate the health impact of outdoor particulate air pollution has been adopted by the majority of health risk assessments conducted to date. The method for calculating the health impact of elevated particulate matter concentrations is as follows, and is similar to the methods used for SO2, NO2 and O3:
i) Assess ambient exposure of the population to particulate matter based either on fixed-site measurements from ambient air quality monitoring stations or on model-based estimates.
ii) Identify a counterfactual exposure (also called a 'target' or 'background' PM concentration), below which it is assumed there is no harmful health effect. This level is used for comparison, to determine the potential benefit (in terms of disease reduction) of reducing the risk factor.
iii) Determine the size of the population group exposed to particulate matter.
iv) Determine the incidence of the health effect being estimated, e.g. the underlying mortality rate of the population, in deaths per hundred thousand.
v) Use exposure-response functions (also called dose-response functions or concentration-response functions) that relate the concentrations of PM2.5 or PM10 to selected health effects
vi) Calculate the attributable fraction for each health outcome based on the relative risk of the exposed population
vii) Calculate the attributable health burden by multiplying the population-attributable fraction by the health outcome.
Health outcomes
A rather bewildering array of health effects are reported by different studies. Premature mortality and morbidity (such as number of hospital admissions or incidences of an illness) outcomes are often calculated. Disability-adjusted life years (DALYs) are a measure of the total health impact (quality of life and longevity) and are calculated by adding the years of life lived with disability and the years of life lost. The effects of pollution on the development of foetuses and young children are usually not directly accounted for.
Health effects are typically divided into categories, based on the length of exposure (short-term or long-term), the type of health effect and the age of the population:
i) all-cause mortality, due to short-term exposure to PM10. This is not used in DALY calculations and should not be added to any other health estimate;
ii) respiratory mortality, due to short-term exposure to PM10 for children <5 years;
iii) cardiopulmonary mortality due to long-term exposure to PM2.5 for adults >25 years; and
iv) lung cancer mortality, due to long-term exposure to PM2.5 for adults >25 years (Ostro 2004; WHO 2016).
Exposure-response relationship
The relationship between exposure to a particular concentration of pollutants and the health effect is expressed either as an exposure-response function, or as a relative risk. The relative risk of exposure is determined by two main methods. In the first method, the relationship between short-term exposure (one- or two-day averages) and daily health impact (e.g. daily mortality) is determined through time series studies where the associations between changes in health outcomes and changes in exposure indicators are evaluated. The outcome is a count (i.e. the Poisson distribution) and the model form is usually log-linear. The Harvard Six Cities time-series analysis is an example of such a study. In the second method, the health effects of chronic, long-term exposure to (annual average) ambient concentrations are determined by cross-sectional 'ecologic' studies which compare exposure and responses at the community level and, more usefully, by prospective cohort studies which use data from a sample of individuals observed over time (for example the Harvard Six Cities study (Dockery et al. 1993) and the American Cancer Society (ACS) study (Pope et al. 1995)). The outcome of these studies is continuous (person-time per exposure) and the relationship is (somewhat) linear (USEPA 2004). The types of exposure-response functions used in the five studies reviewed in this paper are listed in Table 2.
Künzli et al. (2001) (and the USEPA (2004)) conclude that "time-series analyses underestimate causes of death attributable to air pollution and that assessment of the impact of air pollution on mortality should be based on cohort studies." Time series approaches only capture the deaths of already frail persons, induced by exposure to air pollution shortly before death. Cohort studies capture all cases of deaths related to pollution exposure, including the risk of underlying diseases leading to frailty.
Considering the example of PM10 concentrations, an exposure-response relationship is multiplied by the increase in PM10 concentrations and the number of exposed people to calculate the health impact I:
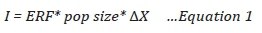
where
ERF is the exposure-response function;
pop is the size of the exposed population; and
ΔX is the change in PM10 concentration (mg/m3) due to the source of concern
As an illustration, considering the central estimate for PM10 mortality for people <65 years old of 0.23*10-8 in the van Horen (1996) study (Table 2), one person in 0.23*108 (23 million) will die for each 1 mg/m3 increase in PM10 concentration.
Health impact I, expressed as the number of cases that can be attributed to the exposure, can also be calculated from the relative risk as:
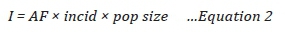
where
AF is the attributable fraction of deaths due to exposure to PM10; and
incid is the incidence of death in the population (non-accidental mortality).
The attributable fraction AF is given by:

where RR is the relative risk of death due to exposure to PM10 and is given by:

where
β is the fractional increase in mortality/morbidity incidence per 1 mg/m3 increase in pollution concentration;
X is the current annual mean concentration of the pollutant of concern; and
XO is the threshold/baseline concentration of the pollutant.
(X-X0 corresponds to ΔX in equation 1.)
For example, if there is an increase of 0.8% in the mortality rate due to a 10 mg/m3 increase in PM10 concentration, the value of βX would be 0.0008.
The exposure-response function and the relative risk function calculated for an incremental increase in pollution of X-X_0 are related as follows:
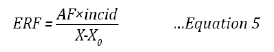
In many studies, a linear relationship is assumed between amount of pollution inhaled and severity of the health response (e.g. van Horen 1996). However, the development of integrated exposure-response functions which combine exposure-health relationships for ambient air pollution, household air pollution, second-hand tobacco smoke and active smoking has shown that there is a levelling-off of the health impact at higher exposure levels (Pope et al. 2009; Pope et al. 2011; Smith et al. 2014; Burnett et al. 2016).
Counterfactual exposure
The counterfactual exposure, also called the background or threshold concentration, is the baseline concentration for comparison of the health risks. The World Health Organisation (2013) argues that there is no safe level of exposure to particulate matter below which there are no negative health effects. Several studies select zero µg/m3 as the counterfactual concentration (for example, van Horen (1996) and in all likelihood, Myllyvirta (2014)). However, others argue that zero exposure is not a practical counterfactual level because this is impossible to achieve, even in pristine environments (Brauer et al. 2012). Lim et al. (2012) define the theoretical-minimum-risk exposure distribution based on the minimum concentration in the studies used to estimate risk (below which there is clearly no evidence of an association between exposure and health).
Studies on health impacts of South African coal-fired power stations
To date, five comprehensive assessments have been performed on the impact of South African coal-fired power station emissions on human health. Van Horen's (1996) PhD thesis is a comprehensive assessment of the environmental externalities in South Africa's energy sector. He considers the health effects of particulate matter and ozone that form as a result of power station emissions. The FRIDGE study by Scorgie et al. (2004) was sponsored by the National Economic, Development and Labour Council (NEDLAC), and considers the health costs of air pollution from a comprehensive range of sources. It also considers the cost-benefit ratio of interventions to improve air quality. The Airshed and Infotox study (Scorgie and Thomas 2006) was commissioned by Eskom and also considers most major sources of air pollution. The Myllyvirta (2014) study was commissioned by Greenpeace, and is the basis for the Holland (2017) study. It considers emissions in excess of the 2020 limits for new plants in the Listed Activities and Associated Minimum Emission Standards published in terms of Section 21 of the National Environmental Management: Air Quality Act (Act No 39 of 2004). Steyn and Kornelius (2018) calculate the health benefits (expressed in monetary terms) of reducing SO2 emissions from power stations, from current levels to compliance with the new plant SO2 emission standard of 500 mg/Nm3. A comparison between the inputs used for these five studies is given in Table 1.
All studies use dispersion or chemical transport models that calculate the secondary formation of particulates from SO2 and NOx emissions. The van Horen (1996) and Myllyvirta (2014) studies use models that are not customised to the South African environment. Steyn and Kornelius (2018) only consider ambient SO2 and secondary particulate (sulphate) levels for SO2 emissions in excess of 500 mg/Nm3.
The FRIDGE (2004) study assumes daily counterfactual concentrations of 25 µg/m3 for PM10 and 15 µg/m3 for PM2.5, based on the recommendations of the CEPA/FPAC Working Group (1998). The Airshed and Infotox (2006) study uses annual counterfactual concentrations of 15 µg/m3 for PM10 (as per Cohen et al. 2004), 25 µg/m3 for SO2 and 20 µg/m3 for NO2 (these levels are 50% of the annual average air quality limits recommended by the WHO (2000)). Van Horen (1996) and Steyn and Kornelius (2018) use a counterfactual exposure of zero. The counterfactual concentration used by Myllyvirta (2014) is not clear. The Krewski et al. (2009) study, from which Myllyvirta's relative risk factors are drawn, uses a counterfactual concentration with uniform distribution between 5.8 and 8.8 µg/m3, but Myllyvirta (2014) applies the relative risk factors to exposure concentrations of less than 3.4 µg/m3, so it is assumed that a counterfactual concentration of zero was in fact used.
The scope of the studies also differs. Van Horen (1996) and Myllyvirta (2014) consider the impact over the whole of South Africa, while the FRIDGE (2004) and Airshed and Infotox (2006) studies only consider the industrialised Highveld. Steyn and Kornelius (2018) consider the Highveld Priority Area (the industrialised Mpumalanga Highveld and eastern Gauteng), and include emissions from the Sasol Synfuels Steam Stations. Myllyvirta (2014) also considers the three return-to-service power stations (Camden, Grootvlei and Komati) and is the only study to consider Medupi Power Station.
The exposure-response functions used to relate exposure to the pollutant and health outcome are given in Table 2. The van Horen (1996) and FRIDGE (2004) studies use functions for acute (daily) exposures derived from time series studies for mortality estimates, while the Airshed and Infotox (2006), Myllyvirta (2014), and Steyn and Kornelius (2018) studies use functions for chronic (annual average) exposure derived from cohort studies for the mortality estimates. The van Horen (1996) and FRIDGE (2004) calculations of premature mortality are probably an underestimate of the actual impact (Künzli et al. 2001; USEPA 2004). All hospital admissions are calculated from acute (daily) exposure functions. Myllyvirta's (2014) relative risk functions are sourced from the American Cancer Society study, with the reference given as Krewski et al. (2009). However, the relative risks appear rather to come from an original analysis of the American Cancer Society Study by Burnett et al. (2012 - supplemental material).
It is difficult to compare the dose-response functions with the relative risk functions as they are presented in Table 2, so a few of the relative risk functions used by Myllyvirta (2014), Airshed and Infotox (2006) and Steyn and Kornelius (2018) have been converted to dose-response functions using Equation 5 (Table 3). The PM10 daily mortality exposure-response functions used by van Horen (1996) and FRIDGE (2004) differ by an order of magnitude, which is surprising since they are both apparently the factor used in the EXMOD model used by van Horen (1996). There may be an error in van Horen's table. The dose-response function used by Steyn and Kornelius (2018) for mortality due to chronic exposure to sulphates is slightly lower than the function used by Myllyvirta (2014) for mortality due to chronic exposure to PM2.5, which is consistent since sulphates are just one of many components of PM2.5. The exposure-response factor used by van Horen (1996) for PM10 respiratory hospital admissions is three orders of magnitude lower than that used by FRIDGE (2004) and Airshed/Infotox (2006), while the factor used by Steyn and Kornelius (2018) is one order of magnitude lower.
There are also significant differences in the incidence of death or disease in the general population, as used in the health risk studies (Table 4). The rates of respiratory hospital admissions used in FRIDGE (2004) and by Steyn and Kornelius (2018) are much higher than those used in Airshed and Infotox (2006). The total mortality rates used in FRIDGE (2004), Airshed and Infotox (2006) and Steyn and Kornelius (2018) are similar, while the cardiovascular mortality rate used in Airshed and Infotox (2006) is higher than that used in the FRIDGE (2004) and Myllyvirta (2014) studies.
The FRIDGE study predicts by far the highest number of hospital admissions due to exposure to air pollution - 5 456 per year. Steyn and Kornelius (2018) calculate the lowest number of hospital admissions (98 in total), since they are only considering the impact of SO2 emissions in excess of the Minimum Emission Standards in the Highveld Priority Area.
Table 5 is not an exhaustive list of the health impacts considered in the health risk assessments. Rather, a number of health outcomes covered by most studies have been selected for comparison. Other types of health outcomes considered include chronic bronchitis, restricted activity days (van Horen 1996 and FRIDGE 2004) and asthma attacks (van Horen 1996 and Steyn and Kornelius 2018).
Relevance of exposure-response functions
It is worth reflecting on the shape of the exposure-response functions used in the different studies, and the exposure levels over which they are applied. The exposure-response functions by van Horen (1996) and FRIDGE (2004) are linear, while those used by Airshed and Infotox (2006), Myllyvirta (2014) and Steyn and Kornelius (2018) are exponential (as per Ostro 2004). The exposure-response relationships given by these two types of functions are similar at low concentrations, but differ significantly at higher concentrations.
Several recent studies have developed integrated exposure-response (IER) functions that model disease risks across three orders of magnitude in the range of PM2.5 exposure associated with three main sources of combustion pollution: ambient air pollution, second-hand tobacco smoke and active tobacco smoking (Pope et al. 2009; Pope et al. 2011; Smith et al. 2014). Burnett et al. (2016) also included household air pollution due to domestic solid fuel burning. The WHO's Ambient air pollution: Global assessment of exposure and burden of disease (2016) uses IER functions developed by Burnett et al. (2016) for the Global Burden of Disease (GBD) 2010 study, and updated by the GBD 2013 study. The IER functions show a greater increase in relative risk of mortality for an incremental increase in PM2.5 concentration at lower concentrations, but a much smaller increase in relative risk at higher concentrations. It is preferable to use the IER functions when exposure levels of the population in question exceed the ambient concentrations in the North American or European studies from which the exposure-response functions used in the health risk assessments reviewed here were derived.
The relative risk factors derived from the American Cancer Society study used by Myllyvirta (2014) were derived at an annual average PM2.5 concentration of 14.2 µg/m3, with PM2.5 concentrations ranging between 5.8 and 22.2 µg/m3. Measured annual average PM10 concentrations in South Africa ranged between 10 µg/m3 in Brackenham, Umhlathuze and 98 µg/m3 in Sharpville, Gauteng, in 2016. PM2.5 concentrations are not measured as widely, but in the Highveld Priority Area the annual average PM2.5 concentrations ranged between 11 µg/m3 in Middelburg and 43 µg/m3 in Secunda in 2016. In the Vaal Triangle Priority Area, annual average PM2.5 concentrations in 2016 ranged between 24 µg/m3 in Diepkloof and 42 µg/m3 in Kliprivier (Khumalo, 2017).
In more remote areas, the exposure-response function used in the Myllyvirta (2014) study is certainly applicable, but in the industrialised areas it may well not be. Two out of the five monitoring stations in the Highveld Priority Area, and all six monitoring stations in the Vaal Triangle Airshed Priority Area, have annual average concentrations which exceed the upper level of concentrations measured in the American Cancer Society study from which the relative risk functions were derived.
In each of the health risk assessments, the predicted ambient air pollutant concentration was taken to be the exposure; i.e. it was assumed that the pollutant concentrations predicted for a certain location were inhaled by the people living in that location. This is not the case in areas where people burn solid and liquid fuels in their homes for cooking or space heating, as shown by measurements collected by Wernecke (2018) in the low-income areas of Kwadela and KwaZamokuhle on the Mpumalanga Highveld (Table 6). Coal is burnt for heating in around 70% of households in Kwadela, and 60% of households in KwaZamokuhle. Personal exposure to PM4 ranges between an average of 38 µg/m3 in summer and 161 µg/m3 in winter. A rough calculation, assuming that summer conditions prevail for nine months of the year and winter conditions for three months, suggests that annual average personal exposure to PM4 in communities where domestic burning is prevalent ranges between 46 µg/m3 and 80 µg/m3. (While the proportion of PM4 which is PM2.5 is not known, measurements by Nimra et al. (2015) show that the PM2.5:PM4 ratio is at least 0.95).
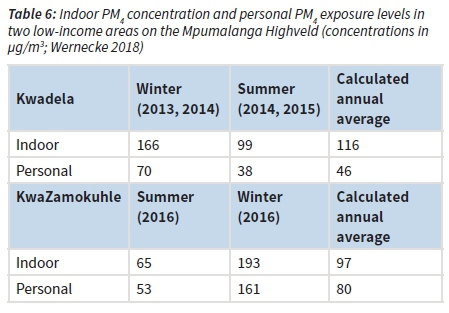
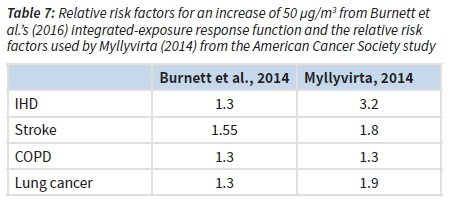
The Myllyvirta relative risk factor for IHD of 1.26 for an increase of 10 mg/m3 in annual average PM2.5 concentrations is similar to the IER function at lower concentrations, but they diverge sharply for a PM2.5 concentration increment of 25 mg/m3 or more. As shown in Table 7, if the Myllyvirta relative risk factors were to be used to account for the health impacts of all sources contributing to PM2.5 exposure levels, the health risks would be significantly over-estimated. A much more accurate estimate of health effects would be obtained by applying an IER function to quantify health risks at actual exposure levels, and then apportioning the health effects relative to the contribution that each source makes to total exposure levels.
Health benefits of coal-fired power stations: electrification
A discussion of the negative health effects of coal-fired power stations is not complete without a consideration of the health benefits brought about by electrification, mainly through decreasing the inhalation of smoke from indoor fires. Spalding-Fecher and Matibe (2003) compare the costs of the impact of air pollution on health with the health costs avoided through electrification, based on van Horen's (1996) analysis. They consider total avoided health costs for low income households electrified by 1999 (relative to power stations operating in 1999), based on reduced mortality and morbidity from air pollution from indoor coal and wood fires; reduced mortality and morbidity from accidental paraffin poisoning; reduced mortality and morbidity from fires and burns caused by paraffin and candles; and the reduced social costs of fuel wood scarcity. They calculate that the health costs avoided by electrification were R958 million in 1999 (range: R173 million - R2 324 million), while the health costs arising from air pollution from power stations was only slightly higher at R1 177 million (range: R852 million - R1 450 million).
The FRIDGE (2004) study estimates that electrification would reduce annual respiratory hospital admissions (due to exposure to PM10, SO2 and NO2 exposure) by 7 946, and reduce mortality by 22. These benefits outweigh the health costs of coal-fired power stations calculated by this study (5 439 respiratory hospital admissions and 10 deaths a year). While the costs and health impact figures calculated in these studies are highly uncertain and likely to be underestimated, the comparison in each study is valuable because similar assumptions were used to calculate the impact of both electrification and exposure to coal-fired power station emissions.
Conclusions
A careful analysis of the assumptions and inputs used in the four health risk assessments of emissions from South African coal-fired power stations conducted to date has shown reasons for the disparities in the calculated health effects. The health impacts calculated by the FRIDGE (2004) and Airshed and Infotox (2006) health risk assessments are in all likelihood too low because of the high counterfactual concentrations used (daily PM10 concentration of 25 µg/m3 and daily PM2.5 concentration of 15 µg/m3 in the FRIDGE (2004) study, and annual PM10 concentration of 15 µg/m3 in the Airshed and Infotox (2006) study). Health risks at lower PM concentrations are not accounted for. In the Airshed and Infotox (2006) study, modelled PM10 annual average concentrations are below the counterfactual concentrations everywhere in the modelling domain, so no health effects from PM exposures are considered at all. Steyn and Kornelius (2018) restrict themselves to an assessment of SO2 emissions and impacts in the Highveld Priority Area. The FRIDGE (2004) and Airshed and Infotox (2006) studies also only cover a limited geographical area, while the van Horen (1996) and Myllyvirta (2014) studies consider exposure throughout South Africa.
It is difficult to comment on the van Horen (1996) results, because it seems that there was an error in the transcription of the exposure-response functions.
The Myllyvitra (2014) health risk assessment of exposure to power station emissions appears to be a reasonable quantification of the health risk in remote areas, but is probably a large over-estimation of the health risk in more polluted areas, and especially in communities where personal exposure is elevated due to people inhaling smoke from domestic burning.
A fair health risk assessment of coal-fired power station emissions should offset the health costs of emissions from power stations with the health benefits from converting low-income households from solid/liquid fuels to electricity. This requires a quantification of the relationship between the electricity price and the rate of domestic solid/liquid fuel use. At a minimum, the increase in domestic electricity use, relative to domestic fuel use, achieved by keeping the electricity price low by continuing to use old coal-fired power stations (rather than replacing them with cleaner generation options) should be weighed against the health costs of coal-fired power stations.
References
Adam M., Schikowski T., Carsin A.E. et al., 2015, 'Adult lung function and long-term air pollution exposure. ESCAPE: a multicentre cohort study and meta-analysis', Eur Respir J 45:38-50. [ Links ]
Anderson H.R., Favarato G., Atkinson R.W., 2013, 'Long-term exposure to air pollution and the incidence of asthma: metaanalysis of cohort studies', Air Qual Atmos Health 6:47-56. [ Links ]
Annegarn H.J., Grant M.R., Kneen M.A. and Scorgie Y., 1999, Direct Source Apportionment of Particulate Pollution within a Township, Report for the Department of Minerals and Energy, Low Smoke Coal Programme, Report No. DME/2/DME-99, University of Witwatersrand, Johannesburg. [ Links ]
Atkinson R.W., Mills I.C., Walton H.A. and Anderson H.R., 2014, 'Fine particle components and health - a systematic review and meta analysis of epidemiological time series studies of daily mortality and hospital admissions', Journal of Exposure Science and Environmental Epidemiology 25 (2): 208-214. [ Links ]
Bradshaw et al., 2003, Initial Estimates from the South African National Burden of Disease Study, 2000, MRC Policy Brief No. 1. [ Links ]
Brauer M., Amann M., Burnett R.T., Cohen A., Denterner F., Ezzati M., et al., 2012, 'Exposure assessment for estimation of the global burden of disease attributable to outdoor air pollution,' Environ Sci Technol 46:652-660. [ Links ]
Brook R.D., Rajagopalan S., Pope C.A. 3rd et al., 2010, 'Particulate matter air pollution and cardiovascular disease: an update to the scientific statement from the American Heart Association', Circulation 121:2331-78. [ Links ]
Burnett R.T., Pope C.A. III, Ezzati M., Olives C., Lim S.S., Mehta S., Shin H.H., Singh G., Hubbell B., Brauer M., Anderson H.R., Smith K.R., Balmes J.R., Bruce N.G., Kan H., Laden F., Prüss-Ustün A., Turner M.C., Gapstur S.M., Diver W.R., Cohen A., 2014, 'An integrated risk function for estimating the global burden of disease attributable to ambient fine particulate matter exposure', Environ Health Perspect 122:397-403. [ Links ]
Canfield R.L., Henderson C.R. Jr, Cory-Slechta D.A. et al., 2003, 'Intellectual impairment in children with blood lead concentrations below 10 microg per decilitre, New England Journal of Medicine, 348:1517-1526. [ Links ]
Chen Z., Salam M.T., Eckel S.P., Breton C.V., Gilliland F.D., 2015, 'Chronic effects of air pollution on respiratory health in Southern California children: findings from the Southern California Children's Health Study', J Thorac Dis 7:46-58. [ Links ]
City of Johannesburg (Joburg), 2000, Johannesburg State of Environment Report, 2000. [ Links ]
Cohen A. et al. 2004, 'Mortality Impacts of Urban Air Pollution', in: Comparative quantification of health risks: global and regional burden of disease attributable to selected major risk factors, M. Ezzati et al., eds. Geneva: World Health Organization, pp. 1353-1434. [ Links ]
Da Costa M., 2009, Private Hospital Review 2009, Hospital Association of South Africa. [ Links ]
Dockery D.W.C.A., Pope X., Xiping J., Spengler J., Ware M.F., Ferris B. and Speizer F., 1993, An Association between Air Pollution and Mortality in Six US Cities., New England Journal of Medicine 329 (24):1753-59. [ Links ]
Gasana J., Dillikar D., Mendy A. et al., 2012, 'Motor vehicle air pollution and asthma in children: a meta-analysis', Environ Res 117:36-45. [ Links ]
Glinianaia S.V., Rankin J., Bell R. et al., 2004, 'Particulate air pollution and fetal health: a systematic review of the epidemiological evidence', Epidemiology 15:36-45. [ Links ]
Grobler M., 2016, Evaluating the costs and benefits associated with the reduction in SO2 emissions from industrial activities on the Highveld of South Africa, MEng dissertation, University of Pretoria. [ Links ]
Ha S., Hu H., Roussos-Ross D. et al., 2014, 'The effects of air pollution on adverse birth outcomes', Environmental Research 134:198-204. [ Links ]
Holland M., 2017, Health impacts of coal fired power plants in South Africa, report for Groundwork (South Africa) and Health Care Without Harm. [ Links ]
Hwang B.F., Chen Y.H., Lin Y.T., Wu X.T., Leo Lee Y., 2015, 'Relationship between exposure to fine particulates and ozone and reduced lung function in children', Environ Res 137:382-90. [ Links ]
IARC (International Agency for Research on Cancer), 2013, Outdoor air pollution a leading environmental cause of cancer deaths, Press release no 221, Lyon. www.iarc.fr/en/media-centre/iarcnews/pdf/pr221_E.pdf [ Links ]
Janssen B.G., Godderis, L., Pieters, N. et al., 2013, 'Placental DNA hypomethylation in association with particulate air pollution in early life', Part Fibre Toxicol 10:22. [ Links ]
Jiang R., Jones M.J., Sava F., Kobor M.S., Carlsten C., 2014, 'Short-term diesel exhaust inhalation in a controlled human crossover study is associated with changes in DNA methylation of circulating mononuclear cells in asthmatics', Part Fibre Toxicol 11:71. [ Links ]
Khumalo T., 2017, 2017 State of Air Report and National Air Quality Indicator, presentation given at the 12th Air Quality Governance Lekgotla, 2-3 October 2017, Sandton. [ Links ]
Krewski D., Jerrett M., Burnett R.T., Ma R., Hughes E., Shi Y., Turner M.C., Pope C.A. III, Thurston G., Calle E.E., Thun M.J., 2009, Extended Follow-Up and Spatial Analysis of the American Cancer Society Study Linking Particulate Air Pollution and Mortality, HEI Research Report 140, Health Effects Institute, Boston, MA. [ Links ]
Kulkarni N., Pierse N., Rushton L., Grigg J., 'Carbon in airway macrophages and lung function in children', N Engl J Med 355:21-30. [ Links ]
Künzli N., Medina S., Kaiser R., Quénel P., Horak Jr. F., Studnicka M., 'Assessments of deaths attributable to air pollution: should we use risk estimates based on time series or on cohort studies?', American Journal of Epidemiology, 153(11):1050-1055. [ Links ]
Lim S.S., Vos T., Flaxman A.D., Danaei G., Shibaya K., Adair-Rahani H., et al., 2012, 'A comparative risk assessment of burden of disease and injury attributable to 67 risk factors and risk factor clusters in 21 regions, 1990-2010: a systematic analysis for the Global Burden of Disease Study 2010', Lancet 380:2224-2260. [ Links ]
Lin C.A., Pereira L.A.A., Nishioka D.C., Concecao G.M.S., Braga A.L.F. and Saldiva P.H.N., 2004, 'Air pollution and neonatal deaths in Sao Paulo, Brazil', Brazillian Journal of Medical and Biological Research 37: 765-770. [ Links ]
Liu J. and Lewis G., 2014, 'Environmental toxicity and poor cognitive outcomes in children and adults', Journal of Environmental Health 76:130-138. [ Links ]
Maddison D., 1997, A Meta-analysis of Air Pollution Epidemiological Studies, Centre for Social and Economic Research on the Global Environment, London, University College London and University of East Anglia. [ Links ]
Maenhaut W., Salma I., Cafmeyer J., Annegarn H. J., and Andreae M. O., 1996, 'Regional atmospheric aerosol composition and sources in the eastern Transvaal, South Africa, and impact of biomass burning', J. Geophys. Res.-Atmos. 101: 23631-23650. [ Links ]
McConnell R., Islam T., Shankardass K. et al., 2010, 'Childhood incident asthma and traffic-related air pollution at home and school', Environ Health Perspect 118:1021-6. [ Links ]
Myllyvirta L., 2014, Health impacts and social costs of Eskom's proposed non-compliance with South Africa's air emission standards, Greenpeace International. [ Links ]
National Cancer Institute, 'Definition of premature death - NCI Dictionary of Cancer Terms', https://www.cancer.gov/publications/dictionaries/cancer-terms/def/premature-death, accessed on 2018-07-06 15:38:38 [ Links ]
Newby D.E., Mannucci P.M., Tell G.S. et al., 2015, 'Expert position paper on air pollution and cardiovascular disease', Eur Heart J 36:83-93b. [ Links ]
Nimra A., Ali Z., Kahn M.N., Gulshan T., Sidra S., Gardezi J.R., Tarar M.R., Saleem M., Nasir Z.A. and Colbeck, I., 2015, 'Comparative ambient and indoor particulate matter analysis of operation theatres of government and private (trust) hospitals of Lahore, Pakistan', Proceedings of The National Conference and Training Workshop "Wildlife and Aerobiology" held on February 6-7, 2015, Lahore, Pakistan. [ Links ]
Norman R., Cairncross E., Witi J., Bradshaw D. et al., 2007, 'Estimating the burden of disease attributable to urban outdoor air pollution in South Africa in 2000', South African Medical Journal 97(7):782-790. [ Links ]
Ostro B., 1994, Estimating the Health Effects of Air Pollution: A Method with an Application to Jakarta, Policy Research Working Paper 1301, World Bank Policy Research Department, Washington DC. [ Links ]
Ostro B., 2004, Outdoor air pollution: Assessing the environmental burden of disease at national and local levels, WHO Environmental Burden of Disease Series, No. 5, World Health Organisation, Geneva. [ Links ]
Piketh S., Annegarn H. and Tyson P., 1999, 'Lower tropospheric aerosol loadings over South Africa: The relative contribution of aeolian dust, industrial emissions, and biomass burning', J. Geophys. Res.-Atmos. 104: 1597-1607. [ Links ]
Pope C. A. III, Thun M. J., Namboodiri M. M., Dockery D. W., Evans J. S., Speizer F. E., Heath C. W., Jr., 1995, 'Particulate air pollution as a predictor of mortality in a prospective study of U.S. adults,' Am. J. Respir. Crit. Care Med. 151:669-674. [ Links ]
Pope C.A. III, Burnett R.T., Krewski D., Jerrett M., Shi Y., et al. 2009, 'Cardiovascular mortality and exposure to airborne fine particulate matter and cigarette smoke', Circulation 120:941-48. [ Links ]
Pope C.A. III, Burnett R.T., Turner M.C., Cohen A., Krewski D., et al. 2011, 'Lung cancer and cardiovascular disease mortality associated with ambient air pollution and cigarette smoke: shape of the exposure response relationships, Environ. Health Perspect. 119:1616-21. [ Links ]
Pretorius I., Piketh S., Burger R. and Neomagus H., 2015, 'A perspective on South African coal fired power station emissions', Journal of Energy in Southern Africa 26 (3): 27-40. [ Links ]
Raaschou-Nielsen O., Andersen Z.J., Beelen R et al., 2013, 'Air pollution and lung cancer incidence in 17 European cohorts: prospective analyses from the European Study of Cohorts for Air Pollution Effects (ESCAPE)', Lancet Oncol 14:813-22. [ Links ]
Rice M.B., Ljungman P.L., Wilker E.H. et al., 2015, 'Long-term exposure to traffic emissions and fine particulate matter and lung function decline in the Framingham heart study', Am J Respir Crit Care Med, 191:656-64. [ Links ]
Rowe R.D., Bernow S.S., Bird L.A., Callaway J.M., Chestnut L.G., Eldridge M.M., Lang C.M., Latimer D.A., Murdoch J.C., Ostro B.D., Patterson A.K., Rae D.A., White D.E., 1994, New York state environmental externalities cost study, report 2: methodology, RCG/Hagler, Bailly, Inc., Empire State Electric Energy Research Corporations, Albany. [ Links ]
Royal College of Physicians (RCP), 2016, Every breath we take: The lifelong impact of air pollution, Report of a working party, London. [ Links ]
Scorgie Y., Burger L., Annegarn H., Kneen M., 2004, Study to Examine the Potential Socio-Economic Impact of Measures to Reduce Air Pollution from Combustion. Part 3 Report: Quantification of Environmental Benefits Associated with Fuel Use Interventions, Fund for Research into Industrial Development Growth and Equity (FRIDGE). [ Links ]
Scorgie Y. and Thomas R., 2006, Eskom Mpumalanga Highveld Cumulative Planning Study: Air Pollution Compliance Assessment and Health Risk Analysis of Cumulative Operations of Current, RTS and Proposed Eskom Power Station Located within the Mpumalanga and Gauteng Provinces, Report No. APP/06/ESKOM-05 Rev 1.0, project done on behalf of Eskom Holdings Limited. [ Links ]
Smith K.R., Bruce, N. et al., 2014, 'Millions dead: How do we know and what does it mean? Methods used in the comparative risk assessment of household air pollution', Annual Review of Public Health 35:185-206. [ Links ]
Smith K.R., McCracken J.P., Weber M.W., Hubbard A., Jenny A. et al., 2011, 'Effect of reduction in household air pollution on childhood pneumonia in Guatemala (RESPIRE): a randomised controlled trial', Lancet 378:1717-1726. [ Links ]
Steyn M. and Kornelius G., 2018, 'An economic assessment of SO2 reduction from industrial sources on the highveld of South Africa', Clean Air Journal 28 (1): 23-33. [ Links ]
StatsSA (Statistics South Africa), 2002, Causes of Death in South Africa 1997-2001, Advanced Release of Recorded Causes of Death, StatsSA. [ Links ]
StatsSA (Statistics South Africa), 2014, Mortality and causes of death in South Africa: Findings from death notification, Statistical release P0309.3, Statistics South Africa, Pretoria. [ Links ]
Stedman J.R., Linehan E. and King K., 1999, Quantification of the health effects of air pollution in the UK for the review of the national air quality strategy, A report produced for the Department of the Environment, Transport and the Regions. [ Links ]
USEPA, 2004, Epidemiology of human health effects associated with ambient particulate matter, in Air Quality Criteria for Particulate Matter, Vol. II of II, Document no EPA/600/P-99/002bF, Research Triangle Park, NC. [ Links ]
Van Horen C.R., 1996, The cost of power: Externalities in South Africa's energy sector, PhD thesis, UCT. [ Links ]
Wernecke B., 2018, Ambient and indoor particulate matter concentrations on the Mpumalanga Highveld, MSc dissertation, North-West University. [ Links ]
Wick P., Malek A., Manser P et al., 2010, 'Barrier capacity of human placenta for nanosized materials', Environmental Health Perspectives 118:432-436. [ Links ]
WHO, 2000, Guidelines for air quality, World Health Organisation, Geneva. [ Links ]
World Health Organisation, 2013, Review of Evidence on Health Aspects of Air Pollution - REVIHAAP Project, World Health Organisation, Bonn, www.euro.eho.int/_data/assets/pdf_file/0004/193108/REVIHAAP-Final-technical-report-final-version.pdf/. [ Links ]
World Health Organisation (WHO), 2016, Ambient air pollution: a global assessment of exposure and burden of disease, World Health Organisation, Geneva. [ Links ]














