Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
South African Journal of Occupational Therapy
On-line version ISSN 2310-3833
Print version ISSN 0038-2337
S. Afr. j. occup. ther. vol.52 n.1 Pretoria Apr. 2022
http://dx.doi.org/10.17159/2310-3833/2022/vol52n1a4
RESEARCH ARTICLE
Health seeking pathways for stroke survivors in a rural setting: Optimising early intervention for stroke rehabilitation in occupational therapy
Phakeme Z. MkhizeI, *; Stanford M. PhehlukwayoII; December M. MpanzaIII
IB.Occ Ther (UKZN), M.Occ Ther (UKZN), PhD Candidate (UKZN). https://orcid.org/0000-0002-8763-9135; Lecturer, Discipline of Occupational Therapy, School of Health Sciences, College of Health Sciences, University of KwaZulu-Natal, Durban, South Africa
IIB Occ Ther (Hons) (MEDUNSA), Dip Occ Ther (MEDUNSA), LLM (Public Health) (UKZN). http://orcid.org/0000-0001-6769-3030; Retired, South Africa
IIIB. Occ Ther (UKZN), M. Occ Ther (UKZN), PhD candidate (UKZN). http://orcid.org/0000-0003-2777-9256; Lecturer, Discipline of Occupational Therapy, School of Health Sciences, College of Health Sciences, University of KwaZulu-Natal, Durban, South Africa
ABSTRACT
BACKGROUND: Health seeking behaviour and health seeking pathways are interdependent concepts underpinning access to healthcare. Understanding these concepts is critical for appropriate and time-dependant stroke interventions
METHOD: An explorative qualitative study design using one-on-one semi-structured interviews were conducted with 16 participants who were either stroke survivors or caregivers of stroke survivors. The Socio-Ecological Model (SEM) was used to guide data collection and the discussion of the findings in line with the objectives of this study
FINDINGS: The traditional health practitioners (n=11) were the most preferred first encounter followed by public hospital (n = 2) and private hospital (n=1) while others (n=2) self-medicated. On average, it took 30 days for stroke survivors to navigate the health system. The two themes emerging from this study, were 'health seeking delays', and 'the health seeking behaviour factor'
CONCLUSIONS: A combination of factors influenced the health seeking delays at the levels of the SEM. The participants' health seeking behaviours were influenced by their knowledge, attitude, and beliefs at individual and interpersonal levels as well as dissatisfaction with health services at organizational and public policy levels of the SEM. In the South African rural settings, stroke survivors seek medical help from multiple service providers prior to consulting the public healthcare system due to diverse factors that affect them at interpersonal organizational, community and policy levels
Keywords: health seeking behaviour, traditional health practitioners, public healthcare, private healthcare, access to healthcare, socio-ecological model, occupational therapy stroke intervention.
INTRODUCTION
Strokes contribute to mortality and morbidity globally where temporal or permanent disabilities are caused1,2. Strokes are one of the leading causes of death contributing to the burden of diseases and economic burdens in South Africa (SA)3. Occupational therapy is one of the key role players in the rehabilitation of stroke survivors and the main role is achieving independence in activities of daily living (ADLs)3.
However, a few clients and families delay in seeking consultation and care4. Some clients manage to arrive in time within the health system but go through the system without the occupational therapy intervention5. Furthermore, a stroke is a time-dependent condition which can become complicated if not treated immediately. Studies have shown that specialist care as soon as one suffers from a stroke saves lives and reduces disability6,7. Access to specialist care is often delayed and, in some instances, does not happen at all68.
Delays in early interventions at any stage of the care pathway can result in preventable complications and increased burden of disease or death. Amongst the size and type of the stroke suffered, disability amongst stroke survivors is due to delays in treatment, which causes more complications that could have been prevented9,10,11. However, accessing health care upon a stroke onset and consulting relevant health practitioners such as occupational therapists within a hospital depends on a number of factors such as pre-hospital factors and hospitalisation factors. In a rural setting, pre-hospital factors may include difficult terrains, long distances to healthcare facilities, poor transportation and communications, and cultural beliefs on disease and disability causation, which influence the health seeking behaviours12.
At a hospital level, factors such as poor referral systems result in failure or delayed access to rehabilitation services like occupational therapy5,6. It is necessary for occupational therapists to broaden their understanding of factors influencing the health seeking pathway of stroke survivors in a rural setting to contribute to optimising early occupational therapy intervention. Thus, this study sought to explore the factors influencing health seeking pathways of stroke survivors in a rural setting within the KwaZulu-Natal (KZN) Province, South Africa. The objectives of the study included, firstly, to describe health seeking pathways of stroke survivors in a rural setting. Secondly, to identify factors that influenced delays in seeking timely interventions after the onset of stroke. Thirdly, to investigate factors that influenced the health seeking behaviour of stroke survivors.
LITERATURE REVIEW
Stroke can be identified as a burden of disease, as stroke survivors experience residual impairments that can negatively impact on their occupations1,2. The time from the stroke onset to hospital presentation is a critical factor in considering eligibility for thrombolytic therapy1,3. However, access to specialist care is often delayed and, in some instances, may not happen at all4,5,6. There are various factors associated with delays to seeking health care such as the lack of knowledge, economic status, rural health and cultural beliefs7. Health seeking pathways refer to a sequence of consultation at specific health service contact points from when the problem is recognised to when an individual receives help8. In SA, factors influencing a delay in consultation after a stroke onset have not been well documented.
Rehabilitation, ideally provided by a multidisciplinary team, plays an essential role in minimising the impact of impairments on the occupations of persons with disabilities9. Physiotherapists (PT) and occupational therapists are mostly the rehabilitation workers servicing rural areas in South Africa9,10. Occupational therapy enables stroke survivors to relearn everyday activities in order to lead a full and independent life. Occupational therapists assess difficulties of a stroke survivor, adapts activities (personal care, social or leisure) and help the stroke survivor to practice them to improve their abilities. The occupational therapist further teaches strategies and techniques to overcome difficulties, provide psychosocial support, provide assistive devices, equipment and visit survivors' homes to advise on any useful changes for the stroke survivor to reengage in life with the possibility of returning to work11,12. Although the benefits and critical role of rehabilitation of stroke survivors have been noted, stroke survivors do not always arrive at rehabilitation centres in time and some do not attend rehabilitation at all4,5,6.
Limited understanding of health seeking behaviour and health-seeking pathways for stroke survivors continues to contribute to delays in early interventions, which results in unnecessary complications, and increase the burden of disease and of care for stroke survivors.
Theoretical framework
The Socio-ecological model (SEM), shown in Figure 1 (below) guided the planning and interpretation during the different phases of this study. It is a theory-based framework that aids in understanding multiple levels of a social system and the interactions between four levels/bands of influence which represent the interpersonal, organizational, community and policy levels13,14. It also seeks to unravel how the individual's personal and environmental factors determine their behaviours.
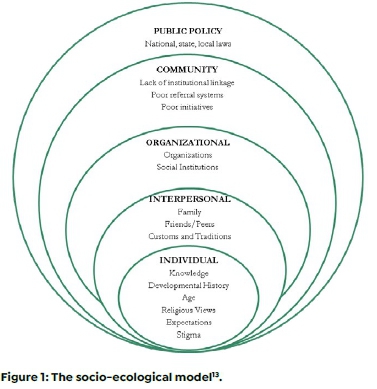
Bronfenbrenner14 identified five hierarchical levels that affect behaviour, namely:
• Individual: Characteristics such as knowledge, attitude, behaviour, developmental history, and stigma.
• Interpersonal: Informal and formal social networks and social support systems such as family, friends/peers, co-workers, religious networks, customs, and traditions.
• Community: The relationships between the organisations, institutions, and informal networks within defined boundaries. These include village associations, community leaders, businesses, and transportation.
• Organizational: The organisations or institutions, through their rules and regulations, will ensure that operations are conducted, and the quality of these operations are kept to standard.
• Policy/Enabling Environment: The local, state, national and global laws and policies regarding the allocations of resources and access to healthcare services, restrictive policies or the lack of policies.
In this study, the SEM was used to understand how the stroke survivors' knowledge, attitude and beliefs influenced their health seeking behaviour at an individual level. The interpersonal level was used to guide the description of socio-cultural influence on a stroke survivor's health seeking patterns. Furthermore, the appropriate health facility stroke treatment protocols and related procedures were reviewed to understand how these facilitated appropriate access to stroke rehabilitation by stroke survivors. The community level was utilised to explore available community infrastructure, referral systems and health programmes which facilitated effective stroke rehabilitation within the study site to reveal which health seeking pathways were utilized by stroke survivors within this rural setting. Lastly, the relevant health legislative frameworks were reviewed to establish if they supported appropriate resource allocation and access to stroke health services.
The model illustrated that there is indeed a link between these five levels and that there is influence from one level to another given the person's physical, social and political environments are essential in distinguishing the person's behaviour. In this study, it was vital to understand the key factors that contribute to a stroke survivors' activity level and health seeking patterns1 .
METHOD
Aim
The study aimed to explore the factors influencing health seeking pathways of stroke survivors in a rural setting within the KwaZulu-Natal (KZN) Province, South Africa.
Study setting
This study was conducted in Ceza, a rural district, which falls under Ward Four of the Zululand Municipality in the KZN Province of SA. It is a rural area remotely located from most basic utilities with poor infrastructure. High unemployment rates in the area render the largest section of its population to be living in poverty.
Study method
An explorative, qualitative study design was utilised to fulfil the aims of this study. The explorative design is suitable for studies where there is limited knowledge about the area being investigated16. This method allowed the researchers to gain more detailed and rich data in the form of comprehensive written descriptions or visual evidence. In addition, the method allowed deeper exploration of the context and social meaning and how it impacts on individuals16.
Population and sampling procedure
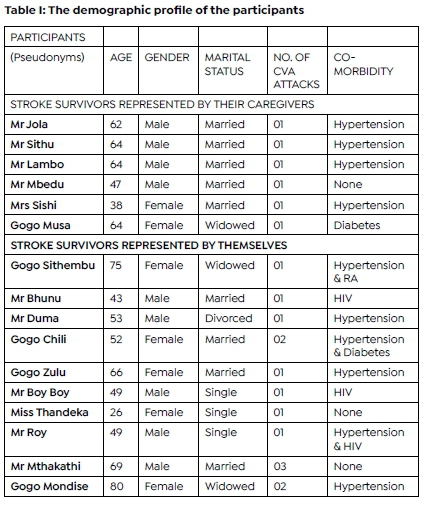
The target population comprised stroke survivors (participants) between 18 and 80 years of age, of any gender and race, (and) from acute to chronic stages of recovery and diagnosed with Transient Ischemic Attack, Ischemic or Haem-orrhagic stroke. A total of 16 participants were selected for the study using purposive sampling procedure. Among the 16 participants, six could not express themselves verbally due to speech impairments as a result of stroke complications. Their caregivers, who were present from the time of the initial stroke attack and during the health seeking pathway phase, spoke on their behalf whilst they (participants) affirmed the information shared using non-verbal communication such as nodding. This allowed for the inclusion of stroke survivors within the whole spectrum of phases and types of strokes including those with a speech impairment. Table I (page 27) presents a summary of the demographic profile of the stroke survivors and classify those who were represented by their caregivers.
Purposive sampling involves the selection of key variables which are likely to have an impact on participants' views17. The sample size for this study was guided by saturation guidelines as applied in qualitative research. In qualitative research, the point of saturation refers to the interview stage where researchers are not receiving any new information from the participants. A practical estimated sample size for a point of saturation is 15 participants18. In this study, a sample size of 16 participants was selected to make up for any possible attrition during the study.
Data collection procedure
Upon the receipt of Gatekeeper permission, prospective participants were invited to participate in this study through the local Community Health Workers (CHWs) using the Information document compiled by the authors. The local CHWs were known in the community by the Tribal Authority Leadership and the two local councillors who granted gatekeeper permission for the study. This provided a link and facilitated the community entry protocol for the Ceza community. The CWH link was suitable because they possessed profiles of specific households where stroke survivors resided, and they were allocated to oversee their health and basic needs.
An interview schedule comprised of questions that were divided into two categories: initial questions and follow-up questions. These were in relation to health seeking patterns followed by stroke survivors, the duration of time taken by stroke survivors between the onset of stroke and the encounter with the health system and the factors which influenced their health seeking behaviour. An IsiZulu translated demographic questionnaire, translated by the principal author and cross-checked by the co-authors, was used to collect the stroke survivors' background information namely age, gender, marital status, number of stroke attacks and comorbid conditions. Similarly, 16 one-on-one semi-structured interviews were conducted with each participant within their homes for a duration of 45 minutes. All interviews were recorded.
Data analysis
All audio recordings were transcribed independently by the principal author to ensure confidentiality. The principal author then directly translated the transcripts which were also cross-checked by the co-authors, from IsiZulu into English. A total of 16 transcripts were available for analysis. First, data were transcribed using verbatim quotes to demonstrate the findings19,20. Data were then analysed using thematic analysis21. The authors read and re-read the data to identify the first level of coding. The codes were then reduced into categories and notes were written regarding themes and subthemes.
Trustworthiness
In this study, the data were examined to ensure that the research findings are robust, rich, comprehensive, and well-developed. All data were further analysed by the authors to determine and improve the trustworthiness of the findings. Credibility was ensured through sharing data and interpretations with the participants to clarify what their intensions were and to correct any errors. Researcher reflexivity throughout the study was used to ensure dependability. Transferability was achieved through the authors' documentation and justification of the methodological approach, and the critical processes and procedures that helped to construct and create meaning associated with the study. Bracketing and triangulation was used to reduce bias and ensure conformability22.
Ethical clearance and considerations
Ethical approval was obtained from an accredited Research Ethic Committee, the Humanities and Social Sciences Research Ethics Committee of the University of KwaZulu-Natal (HSS/0690/018M). A consent letter in the participants' preferred language, informing them about and their rights in the study was signed by the participants, confirming their willingness to participate in the study. The principal author conducting the interviews ensured that no emotional and/ or social harm to the participants occurred through cultural sensitivity and the respect of participants opinions. Open and honest communication with the participants was always ensured to maintain transparency. The participants were allocated pseudonyms to ensure anonymity.
FINDINGS
This study involved 16 participants whose age ranged from 18 to 80 years. Participants were made up of 10 stroke survivors that were able to conduct the interview independently, as well as stroke survivors who were represented by their caregivers as they could not communicate independently. Both males and females were included in the study with the male: female ratio of 9:7. The most common comorbidity was hypertension and a few participants reported Diabetes mellitus, Rheumatoid Arthritis (RA) and Human Immune-deficiency Virus (HIV). Table I (above) presents a summary of the demographic profile of the stroke survivors.
The findings are presented in line with the objectives of the study. The first part describes the findings on the health seeking pathways of the participants to address the first objective. The second part presents the duration and related health seeking delay factors, between the onset of stroke and encounter with the system of care for the participants, which is in line with the second objective. The final part presents factors, which influenced the participants' choice of health service providers, which address the third objective of the study.
Health seeking pathways for stroke survivors
Most participants (11 out of 16) preferred the traditional health practitioners (THP) as their first port of call with the health system after a stroke onset. The second most preferred first encounter was the public hospital (2 participants). The least preferred first encounter with the health system was the general practitioner(GP) (1 participant), the clinic (1 participant) and a private hospital (1 participant). Twelve participants were admitted into a public hospital and 1 participant was admitted into a private hospital. Out of the 12 participants admitted at a public hospital, 11 were referred to a physiotherapist and 1 to a speech-language therapist (SLT). Furthermore, 5 of these participants were referred to tertiary hospitals for further management due to the lack of appropriate services and resources at their base hospitals. The one participant who was admitted into a private hospital was further referred to a private physiotherapist. It was the same participant who self-referred to a private occupational therapist after hearing about occupational therapy services. Although there were occupational therapy services available within the public hospital, none of the admitted participants were referred to the public hospital occupational therapist. See Figure 2 (page 28)
Theme 1: Health seeking delays for stroke survivors
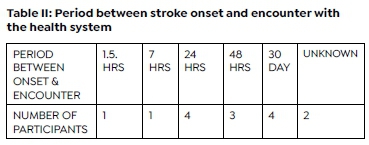
Overall, the time taken by the participants to seek help between the onset of a stroke and their first encounter with the health system ranged from one and a half hour to one month. One participant did not seek medical assistance from any healthcare practitioner but self-medicated using traditional methods. See Table II (above).
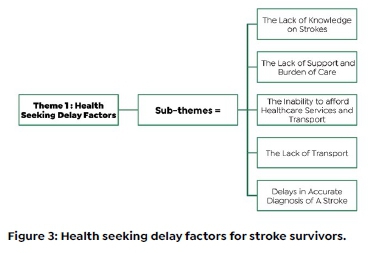
Five sub-themes emerged from the health seeking delays theme namely: The lack of knowledge of strokes, Inability to afford health services and transport, The lack of support and burden of care, The lack of transport and a Delay in the accurate diagnosis of stroke. See Figure 3 (below).
Sub-theme 1: The lack of knowledge of strokes
Certain participants and caregivers of participants lacked westernised knowledge of the symptoms and causes of a stroke as well as the phases that a stroke can be divided into. Due to the lack of this knowledge, certain caregivers did not know what to make of the stroke presentations and follow-up actions they should take when seeking care for the stroke survivors. Furthermore, certain participants and caregivers of the participants reported to believe that stroke was a result of witchcraft and other individuals' doings to impose harm, death and disability onto another.
"Mhlampe akusheshanga ukuthi thina asibanga nalo ulwazi lokuthi ngoba eshawe i-stroke, kufuneka simphuthumise ka dokotela" (Maybe we were not quick enough to realise that he had a stroke and therefore, we needed to take him to see the doctor) (Mr Mbedu's caregiver, Interviewee 9)
"I don't know [what causes a stroke or the phases of stroke]" (Mr Duma, Interview 5; Mr Mbedu, Interview 9) "Mina angazi sidalwa yinL.bathi usuke ucabanga uma besho, angazi ke ukuthi usuke ucabangani ke" (I don't know what causes a stroke.... they say it's because of thinking too much and I'm not sure what those thoughts may be in relation to) (Gogo Zulu, Interviewee 11)
"Istroke senzeka mhlazane eshawa inyoni egeza phandle" (The stroke occurred as a result of a bird that strike him as he was bathing outside) (Mr Jola's caregiver, Interview 1) "senziwa imisebenzi yabantu...ngacushwa befuna ukuqedha ngami" (It resulted from peoples' doing; a method of witchcraft imparted onto me so I could die) (Mr Mthakathi, Interviewee 16)
Sub-theme 2: The inability to afford healthcare services and transport
Participants stated that certain healthcare nodes such as the clinic and physiotherapy appointments were terminated due to increased costs in travel and the payments required for the health care service.
Participants also expressed their lack of patience with commencing treatment and therefore opted to terminate continued care as they failed to see improvements in their condition.
"We went to a physiotherapist and we paid. That's where they stretched him. We eventually stopped because we had to pay for the car to take him there." (Mr Lambo's caregiver, Interviewee 3).
"Yes, I think I took him for three months and I gave up because I was not seeing any differences and I thought I was wasting bus fare money" (Mr Jola's caregiver, Interviewee 1)
Sub-theme 3: The lack of support and burden of care
Caregivers of stroke survivors indicated that delays in seeking healthcare stemmed from having multiple responsibilities to take care of prior to attending to the stroke survivor.
"I could not take him to the hospitaL.That's because I was also taking care of my husband." (Gogo Musa's caregiver, Interviewee7)
"Actually, I was delayed because I was not there, I had other responsibilities within the house that needed my attention. The child took him" (Mr Jola's caregiver Interviewee 1)
Sub-theme 4: The lack of transport
Caregivers stated that they had to wait overnight for transport to seek healthcare due to the unavailability of transport within their residing area. Observations by the researcher also indicated that some areas were isolated and inaccessible due to their geographical location and the topography of the Ceza rural settlement. The caregivers further indicated that they faced difficulties when an ambulance had been requested, as it was usually unavailable and therefore took a long time to arrive.
"He was taken to the hospital in the morning because my husband could not get transport at night... Due to the lack of transport, we were delayed." (Mrs Sishi's caregiver, IInterviewee 6)
"An ambulance comes after a delay though. Whether it's from Ceza or Enkonjeni it's the same: sometimes you get lucky when you call and it's in the area." (Mr Sithu's caregiver, Interviewee 2).
Sub-theme 5: Delays in accurate diagnosis of a stroke
One participant shared that her delays in seeking health care occurred as a result of the hospital failing to diagnose her with a stroke, irrespective of arriving timely upon her stroke onset. The participant had to stay overnight at the Tertiary hospital as she battled to get transport to take her back to her base hospital.
"Kwa delay e.......hospital bethi ababoni ukuthi ngiphethwe yini, ngaleso sikhathi leso yayopha ingozi leyo..." (There was a delay at the hospital whereby they could not diagnose me of a stroke. At that time, I had further bleeding in the brain) (Miss Thandeka, Interviewee 13)
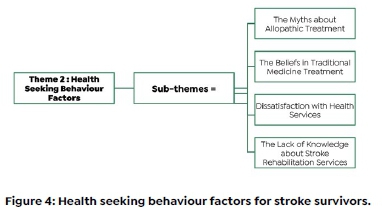
Theme 2: Health seeking behaviour for stroke survivors
Four sub-themes emerged from the health seeking behaviour theme namely, the myths about allopathic treatment for stroke, the beliefs in traditional medicine treatment, dissatisfaction with health services and the lack of knowledge about stroke rehabilitation services (see Figure 4 below).
Sub-theme 1: The myths about allopathic treatment for stroke
Certain participants had the belief that if one started at the public hospital for stroke treatment, the stroke would never be reversed. This contributed to the delays in seeking and accessing primary public healthcare. Findings further indicated that the decision for caregivers to seek healthcare for the stroke survivor from a particular healthcare node was influenced by the stroke survivors' culture and beliefs. As a result of these cultural beliefs, the majority of participant's first pathway to seeking health care was at the THPs.
"They say if you go to the hospital first and they give you an injection, you won't be cured for ever... You do not heal at all. You must see a traditional health practitioner first. And then go to the hospital... I would be bed-ridden. So whatever muthi [traditional medicine] was given to me, I used it. I can't even tell you which one helped" (Mr Sithu, Interviewee 2)
"I had a belief that when you had a stroke, you use Zulu medicine first" (Mr Lambo's caregiver, Interview 3) "Traditional Healers can (cure a stroke) and you have to start there first otherwise your stroke cannot be reversed" (Mr Duma, Interviewee 5)
Participations reported to have feared possible adverse outcomes if they sought healthcare at a public healthcare facility immediately upon a stroke onset and not at the THPs.
"Because I heard that you can't be cured once you get an injection." (Mr Bhunu, Interviewee 8)
"Kwathiwa ke angeke ngisakwazi ukukhuluma sidalwa. uma ngiqala esibhedlela, futhi ngeke ngisheshe ngilapheke" (They said I'll be unable to talk if I begin at the hospital. They further said I will not be able to get immediate treatment) (Gogo Chili, Interviewee 10)
Sub-theme 2: Belief in traditional medicine treatment
Participants expressed a strong belief in consulting a THP. Participants who were either unconscious or could not remember the events after the stroke onset indicated that they would have taken the same health seeking pathway decision to consult at a THP first as their families had chosen for them.
"I would have started with Traditional medicine, then would have gone to the hospital." (Mr Bhunu, Interview 8)
"Yes, that's what I would have done [started at the traditional health practitioner] myself" (Mr Duma, Interviewee 5)
Sub-theme 3: Dissatisfaction with health services
While some participants decided to choose the THP as their first encounter in the health care system, there was some dissatisfaction about the service received from these practitioners.
"They (THP) failed... Eish, these people do not know anything." (Mr Jola's caregiver, Interviewee 1) "anginelisekanga ngoba angikaze ngisizakale, ukube ngasizakala ngabe ngikhuluma ngichamsele nje" (I was not satisfied with the service I received as I did not feel better after consulting with the THP. If I did, my speech would have improved) (Gogo Chili, Interviewee 10)
Similarly, participants who chose the hospital were also not satisfied with the services received. They observed no change after receiving care and the hospital staff asked the participants to carry out some stroke interventions on their own.
"At the hospital, nothing was getting better since he did not even have a wheelchair. I even got help from another client to carry him" (Mr Sithu's caregiver, Interviewee 2)
"No, whenever I went, they would tell me when to come back. The last time I went, they did not say though ... I did not get any pills from the hospital" (Mr Bhunu, Interviewee 8)
"Indlela angiphendula ngayo.wangicasula impela ethi angihambe ngiyothoba." (The way that she answered me was very rude. She instructed me to place a heat pack only) (Mr Roy, Interviewee 14)
Sub-theme 4: Lack of knowledge about stroke rehabilitation services
Participants were not aware of what occupational therapy is and what services are offered within this profession. When asked about the difference between an occupational therapist and a physiotherapist, participants were unable to differentiate as they could not report what the other profession's speciality was. They further insisted on not coming across an occupational therapist when the researcher had described the difference in their roles.
"No... we have never heard of that [occupational therapist] ...No... we just saw one type of physiotherapist" (Mrs Sishi's caregiver, Interviewee 6)
"I don't even know what that [occupational therapist] is.... We went to a physiotherapist and we paid. That's where they stretched him" (Mr Lambo's caregiver, Interviewee 3)
DISCUSSION
The aim of this study was to investigate the health-seeking pathways of stroke survivors in a rural setting. The themes that emerged from the findings are discussed in relation to the current literature, theoretical framework, and objectives of this study.
As highlighted in the introduction, health-seeking pathways provide information on the sequence of consultations by health service users at specific health system contact points from recognition of the need to get help to the point when the individual receives help15. The SEM community layer focuses on the relationships between the organisations, institutions, and informal networks within defined boundaries. In this study, the findings indicated that the most preferred first encounter within the health system was the THP. The health seeking patterns which emerged from this study reflected that limited referrals were made to the rehabilitation practitioners like the occupational therapist. Although some were referred to physiotherapist, no referrals were made internally within the multi-disciplinary team from the physiotherapist to the occupational therapist as illustrated in Figure 2 (page 28).
Health seeking delay factors for stroke survivors
The lack of transport and unaffordable travel expenses were identified as contributors to pre-hospital delays in accessing healthcare and continuity of care. The lack of transport and travelling expenses were also exacerbated by the geographical location of some households and the topography of the Ceza area. This is supported by a study by Mandelzweig et al.23 which identified the demographic and clinical variables such as hospital and clinical accessibility as some of the risks for delay in seeking help. A study by Mshana et al.24 showed that the cost of services, knowledge limitations on illness and wellbeing and cultural prescriptions affected the health seeking practices of communities in Tanzania's health system. This study further indicated that stroke survivors delayed up to one month before seeking health care in a health care system.
Several studies have identified gaps in stroke knowledge about risk factors, severe warning signs and known responses to signs4,5,25. It was evident in this study that the lack of knowledge regarding stroke and the healthcare system negatively influenced the health seeking behaviour for the participants as they had limited knowledge of stroke in relation to prevention, symptoms and care from the allopathic medicine perspective, which has thus led to conforming in myths. Furthermore, the burden of care overload, which emanated from the multiple responsibilities of carers and failure in the early diagnosis of stroke due to inaccurate diagnoses, emerged as one of the critical drivers of health seeking delays for stroke interventions. According to the SEM13, the individual's knowledge and attitude represented the innermost characteristics of the Individual Level which influenced the participants' underlying cause for delay in seeking help. On the other hand, being unable to afford services that would aid in timeous medical assistance and the late diagnosis of a stroke, constituted by health system shortcomings, contributed to delays in seeking help at the Organizational Level of the Model.
Stroke survivors' health seeking behaviour factors
Conceptually, help-seeking behaviour refers to the process of actively seeking help from others to get help on health problems experienced. Health seeking behaviour is determined by various physical, socio-economic, cultural, and political contexts26. The findings in this study showed that cultural practices and beliefs influenced the health seeking pathways navigated by the participants. Some participants held a false belief that allopathic interventions resulted in irreversible symptoms of a stroke. The majority of participants believed that stroke was a result of witchcraft and thus the underlying reason for seeking help from a THP first was to remove the spell cast on them before seeking any other help. This perception corresponds to the findings from Legg and Penn27 which showed that stroke survivors believed that stroke was a result of spiritual causes and misfortune, which caused them to acquire aphasia. Similarly, a Tanzanian study by Mshana et al.24 revealed stroke survivors preferred to consult THPs as they believed that strokes mandated from supernatural causes like demons and witchcraft. Furthermore, studies revealed that the quality of rehabilitation provided by therapists was compromised by the omission of certain services because they were against their cultural beliefs27,28,29.
As illustrated by the SEM, the individual level represents the stroke survivor. The SEM13 further indicated that stroke survivors' cultural beliefs influenced their health seeking pathways and thus led them to the use of THPs first. The caregivers of the stroke survivors as well as Community Healthcare Workers (CHW) refer to the SEM's interpersonal level whereby deciding for the stroke survivor was dependent on the families' own cultural beliefs as well as the CHWs clinical beliefs regarding a stroke. This, therefore, led to influenced health seeking behaviour of the stroke client.
It has been well documented that dissatisfaction with the quality of care received in hospitals and in public health care services has led to discontinued care25,30. In this study, the participants, amongst other mentioned reasons, avoided going to public hospital partly due to the negative attitude of the staff, lack of support and compassion from the hospital staff.
Lastly, it was found that participants confused the role of an occupational therapist by frequently referring to an occupational therapist as a physiotherapist. Booth and Hewison31 indicated that the role-overlap between occupational therapists and physiotherapists has been a subject of debate for at least three decades. This overlap continues to disadvantage stroke survivors in accessing appropriate services, which result in delayed interventions and unnecessary complications.
The Community Level of the SEM, which focuses on the relationships between the organisations, institutions, and informal networks, can be used within defined boundaries. It was further evident that there is a gap in the policies at the policy level that ensure appropriate and efficient referral systems occur within the healthcare system. The South African Stroke Society provides a guideline for a functional stroke unit that states that a stroke unit compromises of specialised staff, within core discipline[s]: medical, nursing, physiotherapy, occupational therapy, speech and language therapy and social work that is coordinated to treatment and care9. However, despite the comprehensive and advanced rehabilitation policies and legislation, there is still a lack of services and implementation of these policies, particularly in ensuring early occupational therapy rehabilitation for stroke clients.
The findings in this study revealed that there were no appropriate communications and referral systems between the multi-disciplinary team. Furthermore, there is a poor referral and communication system between the community THPs and CHWs, and between THPs and the public healthcare system as stroke survivors continue to arrive with complications to the public hospitals. Yet strategies to bridge this gap to ensure THPs refer to the CHWs, Clinics, GPs and the public hospital within the advised time frame remains unaccomplished.
Implications and limitations of the study
This study was conducted in a rural setting and findings cannot be transferred into semi-rural, informal settlements, semi-urban or urban settings; but the issues explored within the context of this study provided deeper insights into the situation. A study on more diverse above-mentioned settings would provide a broader picture on issues which influenced health seeking pathways and behaviour for stroke survivors. Furthermore, findings indicated that some participants were confused between occupational therapy and physiotherapy, which implies that some participants might have been referred to an occupational therapist but noted it as a physiotherapist. Studies are necessary to explore the stroke client's awareness of the occupational therapy role in comparison to the physiotherapy role.
CONCLUSIONS AND RECOMMENDATIONS
The health seeking pathways for stroke survivors showed that the THP was the preferred first encounter. This, however, contributed significantly to delays in seeking public health care in a health system. Clinically, this has implications for the development of well-coordinated referral systems that would link the THP, public health system, the GP and relevant rehabilitation practitioners that would include an occupational therapist, physiotherapist and the speech and language therapist to enhance the early identification and interventions for stroke survivors. It is recommended that occupational therapists working at a community level strengthen partnerships with any health providers within the health seeking pathway of stroke survivors so referrals can be executed timeously, thus optimising early occupational therapy intervention. In addition, at a hospital level, occupational therapists should strengthen the partnership and referral procedure with physiotherapists, speech and language therapists and outpatient department health practitioners for early optimisation of occupational therapy stroke intervention.
The participants' health seeking delays were influenced by a combination of factors at individual, interpersonal, community and organizational levels of the SEM. These included lack of knowledge and financial constraints at an individual level; lack of support and burden of care overload at an interpersonal level; lack of transport at community level and delays in accurate diagnosis as well as appropriate healthcare practitioner referrals of a stroke at organizational level. The participants' health seeking behaviour was equally influenced at various levels of the SEM and included knowledge, attitude and beliefs at individual and interpersonal levels and unsatisfactory health services at organizational and public policy levels. Both the participants' health seeking delays and health seeking behaviour equally reflected major health system shortcomings, which could be addressed at a policy level. Furthermore, it is recommended that health promotion and prevention programmes be considered to address the factors influencing health seeking behaviour, such as the beliefs surrounding a stroke, when educating communities or individuals about strokes.
ACKNOWLEDGEMENTS
Funding received from the UKZN College of Health Sciences.
DATA AVAILABILITY STATEMENT
Upon reasonable request, the data is available from the corresponding author: Phakeme Z Mkhize mkhizep@ukzn.ac.za
DECLARATION OF CONFLICTING INTERESTS
The authors declare that they have no conflicts of interest to disclose.
AUTHOR CONTRIBUTIONS
P.Z. Mkhize was the primary researcher responsible for the project design, data collection and analysis. S.M. Phehluk-wayo and D.M. Mpanza were supervisors on the project, contributed to the writing of the paper, and analysed data in the project.
REFERENCES
1. Lloyd-Jones D, Adams RJ, Brown TM, Carnethon M, Dai S, et al. Executive Summary: Heart Disease and Stroke Statistics-2010 Update. Circulation [Internet]. Ovid Technologies (Wolters Kluwer Health). 2010 Feb 23; 121(7):948-54. Available from: http://dx.doi.org/10.1161/circulationaha.109.192666 [ Links ]
2. Heart Disease and Stroke Statistics-2017 Update: A Report from the American Heart Association. Circulation [Internet]. Ovid Technologies (Wolters Kluwer Health); 2017 Mar 7;135(10). Available from: http://dx.doi.org/10.1161/cir.0000000000000491 [ Links ]
3. Cawood J, Visagie S. Environmental factors influencing participation of stroke survivors in a Western Cape setting. African Journal of Disability [Internet]. AOSIS; 2015 Oct 30;4(1). Available from: http://dx.doi.org/10.4102/ajod.v4i1.198 [ Links ]
4. Bonita R, Broad Jb, Anderson Ne, Beaglehole R. Approaches to the Problems of Measuring the Incidence of Stroke: The Auckland Stroke Study, 1991-1992. International Journal of Epidemiology [Internet]. Oxford University Press (OUP); 1995;24(3):535-42. Available from: http://dx.doi.org/10.1093/ije/24.3.535 [ Links ]
5. Evenson KR, Rosamond WD, Morris DL. Prehospital and In-Hospital Delays in Acute Stroke Care. Neuroepidemiology [Internet]. S. Karger AG; 2001;20(2):65-76. Available from: http://dx.doi.org/10.1159/000054763 [ Links ]
6. Lacy CR, Bueno M, Kostis JB. Stroke time registry for outcomes knowledge and epidemiology S.T.R.O.K.E. Journal of Stroke and Cerebrovascular Diseases [Internet]. Elsevier BV; 1997 Oct;6(6):470. Available from: http://dx.doi.org/10.1016/s1052-3057(97)80182-6 [ Links ]
7. Silvestrelli G, Parnetti L, Paciaroni M, Caso V, Corea F, Vitali R, et al. Early admission to stroke unit influences clinical outcome. European Journal of Neurology [Internet]. Wiley; 2006 Mar;13(3):250-5. Available from: http://dx.doi.org/10.1111/j.1468-1331.2006.01187.x [ Links ]
8. Yanagida T, Fujimoto S, Inoue T, Suzuki S. Causes of prehospital delay in stroke patients in an urban aging society. Journal of Clinical Gerontology and Geriatrics [Internet]. Elsevier BV; 2014 Sep;5(3):77-81. Available from: https://www.sciencedirect.com/science/article/pii/S2210833514000069?via%3Dihub [ Links ]
9. Mellor RM, Bailey S, Sheppard J, Carr P, Quinn T, Boyal A, et al. Decisions and Delays Within Stroke Patients' Route to the Hospital: A Qualitative Study. Annals of Emergency Medicine [Internet]. Elsevier BV; 2015 Mar;65(3):279-287. e3. Available from: http://dx.doi.org/10.1016/j.annemergmed.2014.10.018 [ Links ]
10. Barber PA, Zhang J, Demchuk AM, Hill MD, Buchan AM. Why are stroke patients excluded from TPA therapy? An analysis of patient eligibility. Neurology [Internet]. Ovid Technologies (Wolters Kluwer Health); 2001 Apr 24;56(8):1015-20. Available from: https://n.neurology.org/content/56/8/1015 [ Links ]
11. Cawood J, Visagie S. Stroke management and functional outcomes of stroke survivors in an urban Western Cape Province setting. South African Journal of Occupational Therapy [Internet]. Academy of Science of South Africa; 2016;46(3). Available from: http://dx.doi.org/10.17159/2310-3833/2016/v46n3a5 [ Links ]
12. Rhoda A, Mpofu R, De Weerdt W. Activity limitations of patients with stroke attending out-patient facilities in the Western Cape, South Africa. South African Journal of Physiotherapy [Internet]. AOSIS; 2011 Feb 19;67(2). Available from: http://dx.doi.org/10.4102/sajp.v67i2.41 [ Links ]
13. Kilanowski JF. Breadth of the socio-ecological model. Journal of Agromedicine [Internet]. Informa UK Limited; 2017 Jul 25; Available from: http://dx.doi.org/10.1080/1059924x.2017.1358971 [ Links ]
14. Bronfenbrenner U. Toward an experimental ecology of human development. American Psychologist [Internet]. American Psychological Association (APA); 1977;32(7):513-31. Available from: https://content.apa.org/record/1978-06857-001 [ Links ]
15. Shin C-N, An K, Sim J. Facilitators of and barriers to emergency medical service use by acute ischemic stroke patients: A retrospective survey. International Journal of Nursing Sciences [Internet]. Elsevier BV; 2017 Jan;4(1):52-7. Available from: http://dx.doi.org/10.1016/j.ijnss.2016.12.008 [ Links ]
16. Rahman MS. The Advantages and Disadvantages of Using Qualitative and Quantitative Approaches and Methods in Language "Testing and Assessment" Research: A Literature Review. Journal of Education and Learning [Internet]. Canadian Centre of Science and Education; 2016 Nov 10;6(1):102. Available from: https://www.ccsenet.org/journal/index.php/jel/article/view/64330 [ Links ]
17. Baldwin SA. Organizing your ideas and creating a thesis. Writing your psychology research paper [Internet]. American Psychological Association; 2018;39-56. Available from: https://content.apa.org/record/2017-32524-003 [ Links ]
18. Mills J, Birks M. Introducing Qualitative Research. Qualitative Methodology: A Practical Guide [Internet]. SAGE Publications, Inc.; 2-16. Available from: http://dx.doi.org/10.4135/9781473920163.n1 [ Links ]
19. Burnard P, Gill P, Stewart K, Treasure E, Chadwick B. Analysing and presenting qualitative data. British Dental Journal [Internet]. Springer Science and Business Media LLC; 2008 Apr;204(8):429-32. Available from: http://dx.doi.org/10.1038/sj.bdj.2008.292 [ Links ]
20. Creswell JW, Miller DL. Determining Validity in Qualitative Inquiry. Theory Into Practice [Internet]. Informa UK Limited; 2000 Aug;39(3):124-30. Available from: https://www.tandfonline.com/doi/abs/10.1207/s15430421tip3903_2 [ Links ]
21. Braun V, Clarke V, Hayfield N, Terry G. Thematic Analysis. Handbook of Research Methods in Health Social Sciences [Internet]. Springer Singapore; 2018;1-18. Available from: https://link.springer.com/referenceworkentry/10.1007/978-981-10-2779-6_103-1 [ Links ]
22. Shenton AK. Strategies for ensuring trustworthiness in qualitative research projects. Education for Information [Internet]. IOS Press; 2004 Jul 19;22(2):63-75. Available from: https://content.iospress.com/articles/education-for-information/efi00778 [ Links ]
23. Mandelzweig L, Goldbourt U, Boyko V, Tanne D. Perceptual, Social, and Behavioral Factors Associated With Delays in Seeking Medical Care in Patients With Symptoms of Acute Stroke. Stroke [Internet]. Ovid Technologies (Wolters Kluwer Health); 2006 May;37(5):1248-53. Available from: http://dx.doi.org/10.1161/01.str.0000217200.61167.39 [ Links ]
24. Mshana G, Hampshire K, Panter-Brick C, Walker R. Urban-Rural Contrasts In Explanatory Models And Treatment-Seeking Behaviours For Stroke In Tanzania. Journal of Biosocial Science [Internet]. Cambridge University Press (CUP); 2008 Jan;40(1):35-52. Available from: http://dx.doi.org/10.1017/s0021932007002295 [ Links ]
25. Li Z, Jongbloed L, Dean E. Stroke-Related Knowledge, Beliefs, and Behaviours of Chinese and European Canadians: Implications for Physical Therapists. Physiotherapy Canada [Internet]. University of Toronto Press Inc. (utpress); 2014 Apr;66(2):187-96. Available from: http://dx.doi.org/10.3138/ptc.2012-69bc [ Links ]
26. Tseng W-S. Cultural Psychiatry Training. Handbook of Cultural Psychiatry [Internet]. Elsevier; 2001;795-808. Available from: http://dx.doi.org/10.1016/b978-012701632-0/50128-5 [ Links ]
27. Legg C, Penn C. A stroke of misfortune: Cultural interpretations of aphasia in South Africa. Aphasiology [Internet]. Informa UK Limited; 2013 Feb;27(2):126-44. Available from: http://dx.doi.org/10.1080/02687038.2012.684338 [ Links ]
28. Wegner L, Rhoda A. The influence of cultural beliefs on the utilisation of rehabilitation services in a rural South African context: Therapists' perspective. African Journal of Disability [Internet]. AOSIS; 2015 Mar 26;4(1). Available from: http://dx.doi.org/10.4102/ajod.v4i1.128 [ Links ]
29. Cammarata M, Mueller AS, Harris J, Vrkljan B. The Role of the Occupational Therapist in Driver Rehabilitation after Stroke. Physical & Occupational Therapy In Geriatrics [Internet]. Informa UK Limited; 2017 Jan 2;35(1):20-33. Available from: https://www.tandfonline.com/doi/full/10.1080/02703181.2016.1277443 [ Links ]
30. Haldar S, Mishra SR, Pollack AH, Pratt W. Informatics opportunities to involve patients in hospital safety: a conceptual model. Journal of the American Medical Informatics Association [Internet]. Oxford University Press (OUP); 2019 Oct 3;27(2):202-11. Available from: https://academic.oup.com/jamia/article/27/2/202/5580382 [ Links ]
31. Booth J, Hewison A. Role overlap between occupational therapy and physiotherapy during in-patient stroke rehabilitation: an exploratory study. Journal of Interprofessional Care [Internet]. Informa UK Limited; 2002 Jan;16(1):31-40. Available from: http://dx.doi.org/10.1080/13561820220104140 [ Links ]
* Corresponding Author: Phakeme Z. Mkhize. Email:mkhizep@ukzn.ac.za














