Servicios Personalizados
Articulo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en Google
Similares en Google
Compartir
South African Journal of Occupational Therapy
versión On-line ISSN 2310-3833
versión impresa ISSN 0038-2337
S. Afr. j. occup. ther. vol.47 no.2 Pretoria ago. 2017
http://dx.doi.org/10.17159/231-3833/1017/v47n2a7
SCIENTIFIC ARTICLES
Professionalism - A case for medical education to honour the societal contract
Nico NortjéI; Jocelene De JonghII
IMA (Psychology), M.Phil. (Ethics), PhD (US)- Section of Integrated Ethics in Cancer Care, The University of Texas MD Anderson Cancer Center, Houston, United States of America & Department of Psychology, University of the Free State, South Africa
IIPhD (UWC)- Department of Occupational Therapy, University of the Western Cape, South Africa
ABSTRACT
BACKGROUND: This study explores the concept ofprofessionalism from the vantage point of a cohort of students as well as professionally qualified and practising occupational therapists. With the changes health care delivery is experiencing nationally as well as internationally, there is an urgent need to identify students and qualified professionals' expectations of what influences the development thereof, as well as elicit perceptions of attributes which contribute to professionalism.
METHODS: The study is primarily a descriptive study with a specific focus on a mixed method of quantitative and qualitative research designs, using interpretative phenomenological analysis methodology. Data were gathered from 56 final-year and 55 professionally registered occupational therapists, who participated in a pen-and-paper questionnaire consisting of three sections.
RESULTS: The results of this study indicated a clear differentiation between the influence of both the formal and hidden curricula and that clinical competence, client-centred practice and professional standards contributed mostly to professional behaviour.
CONCLUSION: This study brings to light the experiences of students and professional practitioners to what they expect would influence the professional conduct. The findings are open to theoretical generalizability and raise issues that may be used by academic staff in the preparation of students to become more professional, as well of future Continuous Professional Development training.
Key Words: Professionalism; Clinical competence; Client-Centred practice; Professional standards
INTRODUCTION
Professionalism extends beyond ethics which is concerned with the choices between what is right and wrong in certain clinical settings. Medical professionalism is said to be the keystone of the social contract between medicine and society at large1and the features of professionalism most identified in the literature highlight integrity, respect, competence, honesty, trustworthiness and accountability as pillars of the keystone. Society's belief in healthcare professionalism means that society trusts healthcare professionals to establish and enforce standards for ethics and competence. However, at present, the healthcare profession is confronted by an explosion of technological advances, constraints to health care delivery, changing market forces, bioterrorism, and globalisation, which means that practitioners are faced with an increasing challenge to their definition of professionalism2. Together with the aforementioned is the fact that there is a revolution in transparency in healthcare services which constitutes an unprecedented amount of information (reliable and unreliable) being made available to the public which could potentially undermine confidence in the profession3. Since trust in the provision of a professional service is fundamental to the social contract between the medical profession and individual patients, society, and the publics, failure to ensure trustworthiness may cause the public to no longer believe in professionalism, and alternative forces (i.e. consumerism; political agendas) and belief systems may fill the void4.
Taking cognisance of the aforementioned, there is a great need in training of healthcare students in written and unwritten expectations entailing moral commitments, fundamental to both the societal contract and the details of professionalism5. Professionalism, therefore, must be planned, taught, learned and assessed explicitly6,7. Al-Eraky8 argues that two schools of thought guide the teaching and learning of professionalism, by either outlining a list of values and desirable professional behaviours or as a normative belief method of how one's internal moral conviction should guide one's professional conduct. Rather than seeing the two as opposing methodologies in how to teach professionalism they should be seen as complimentary as one that addresses a cognitive function and the other a more moral dimension.
The objectives of this study are the following:
To examine the understanding of both professionally registered occupational therapists as well as student occupational therapists as to the concept of professionalism;
To examine what could contribute to the development of professionalism amongst the aforementioned two groups; and
To elicit perceptions of attributes which contribute to professionalism, as described by the two groups.
METHODOLOGY
Research Design
The study is primarily a descriptive study with a specific focus on a mixed method of quantitative and qualitative research designs.
Data Gathering Process
The data were collected by virtue of a pen-and-paper questionnaire given to the participants, where they had to elaborate on their understanding of professionalism (open ended qualitative question); rank 12 attributes most cited by literature; and indicate which sphere of interaction influences professionalism the most.
A nonprobability sampling technique was employed as the focus of the research is exploratory to gain more knowledge on occupational therapy students' and professionals' views of professionalism as well as the contributors and attributes which develop professionalism. The two cohorts included were final-year undergraduate occupational therapy students as well as professionals who attended a continuous professional development (CPD) workshop. The inclusion criteria for the students were that they needed to have had a clear understanding of English, have had three or more practical fieldwork experiences with direct patient contact and be in their final year of undergraduate study. The inclusion criteria of the professionals were that they had to be registered with the Health Professions Council (HPCSA) in the category of Occupational Therapy as well as have a clear understanding of English.
A total of 56 final-year students from the University of the Western Cape (South Africa) and 55 professionally registered occupational therapists participated voluntarily in this study (n=111). A control group was not included as the aim of this study was not to address any threats to the validity of the data, but rather to elaborate the richness of the group studied and to identify commonalities and differences within the group.
The three tables below indicate a frequency distribution of the age and gender of the participants in each of the two groups group.
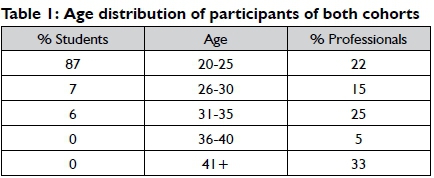
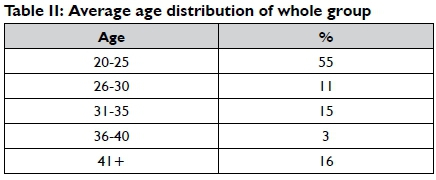
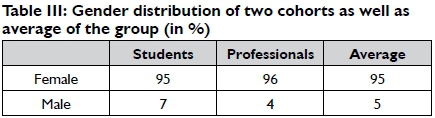
The majority of the participants were female (95%), while males comprised only 5% of the sample. In line with this, Harvison9 indicates a general tendency in the USA for more females than males to work in the field of occupational therapy.
Data Analysis
For the qualitative phase of this study, Interpretative Phenomeno-logical Analysis was used in order to identify pertinent themes. For the quantitative phase of this study, frequency tables were compiled for both cohorts for the following variable combinations: 1) Interventions which contribute to professionalism; and 2) attributes associated with professionalism. Averages were then calculated to identify the most important aspects.
Ethical Approval
This study was submitted and received ethical clearance (REC/2015/05/006) from a registered research ethics committee. Participants were not obliged to complete the questionnaire and anyone could have left the study at any time without experiencing any adverse effects.
RESULTS
This section is divided into two phases.
Phase 1
Phase 1 reports on the most significant themes related to the meaning of the concept 'professionalism' as identified by each cohort.
Clinical Competence (training)
Many participants refer to the theme as having the necessary training and exposure to deliver a service which is within the scope of the qualification; evidence based; and what society expects of a suitably qualified person. Effectiveness and positive results are seen as positive outcomes of clinical competence. Being clinically competent also means to many that one has the ability to discern what therapeutic interventions work and what interventions will not contribute positively to a client, hence taking calculated risks. As one participant noted:
"Providing the most updated treatment and always ensuring your client understands the treatment you will be providing, both the positive and negative effects".
Client-centred Practice
Respecting clients for opposing views and not to be judgmental is seen as an important client-centred ability. Many responses allude to the fact that one needs to be transparent in your decisions and ask the client to participate in the treatment. As one participant noted:
"Considering your client's cultural and religious background when planning treatment by building good interpersonal relationships. Always considering your client's context as it can have an effect on the outcome of the treatment".
Professional Standards
Making a factual diagnosis in line with the professional standards of care accepted by the body of members. Furthermore, professional standards are also seen as respecting the four main tenets of Georgetownian ethics (beneficence; non-maleficence; justice; and autonomy). Some participants also considered the importance of professional boundaries.
Phase 2
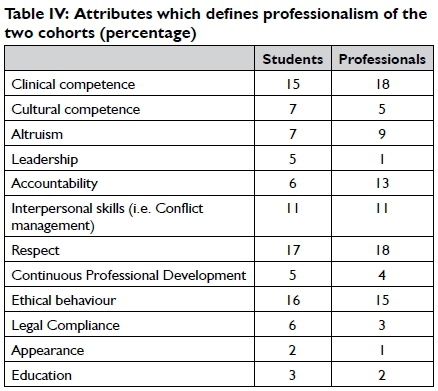
The second phase reports on the ranking by participants of the most important attributes students and professionals perceive as contributing to the development of professionalism. These attributes were chosen from various attributes as reported in literature10,11,12,13.
From the aforementioned the six most influential attributes defining professionalism according to the students are (in descending order) Respect (17%); Ethical behaviour (16%); Clinical Competence (15%); Interpersonal Skills (i.e. conflict management) (11%); Cultural Competence (7%); and Altruism (7%). For the cohort of professionals who have been working in the field as professionals the results varied somewhat where (in a descending order) they were: Clinical Competence (18%); Respect (18%); Ethical behaviour (16%); Accountability (13%); Interpersonal Skills (11%); and Altruism (9%).
Figure 1 indicates that the six attributes defined by the group as a whole mirror that of the professional group.
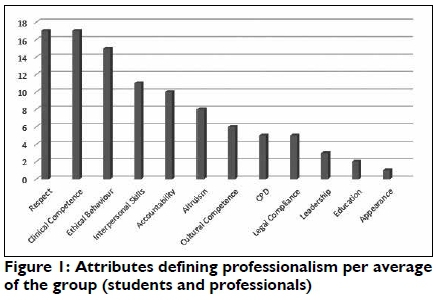
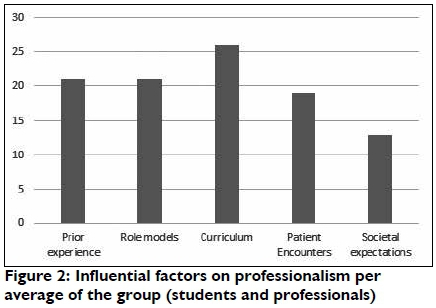
The results, as presented below, also indicate which factors are the most influential in promoting professionalism in the field of occupational therapy.
As can be seen from the Table V, the curriculum, (not inclusive of the hidden curriculum) is seen as the most influential factor for both groups. 'Patient encounters' is seen by the student cohort as equally important as 'prior experience', where 'patient encounters' is not seen as influential to the same extent by the professional group.
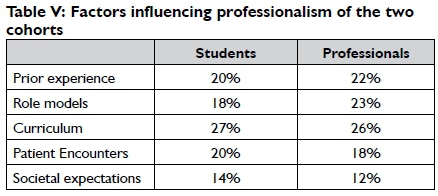
According to the professional group, 'role models' (the hidden curriculum) and 'prior experience' (dealing with colleagues) is more influential. For both groups, 'societal expectations', also referring to the social contract1 is seen as the least important.
DISCUSSION
It is evident from the findings of this study, pertaining to a definition of what constitutes professionalism, are in line with the findings of a recent study14 where professionalism did not equate to social standing, wealth production, physique, or appearance, but rather to good behaviour, high values, and positive attitudes; viewing the profession as a vocation or calling dedicated to caring for and protecting clients.
A joint project by the American Board of Internal Medicine Foundation, the American College of Physicians Foundation, and the European Federation of Internal Medicine (The Medical Professionalism Project) argued that professionalism focusses on attributes such as altruism, trust, honesty, patient empowerment, and commitment to social justice as well as scientific and clinical competence; while emphasising the promotion of patients' best interests and honouring the exercise of the public trust14. These attributes are in line with those highlighted by the results found in this study. Both cohorts identified respect as the most important attribute as this is all-encompassing of both external (clients and colleagues) as well as internal (own moral values). In discussions with the students, they were of the opinion that to them the idea of respecting people from a varied background is becoming essential as society's norms are also changing and many communities are becoming more integrated.
CONCLUSION AND RECOMMENDATIONS
The word 'profession' derives from the Latin profession meaning public declaration. Therefore, as a normative belief system, medical professionalism's main aim is to profess on how best to organise and deliver health care, and to jointly declare (by virtue of professional bodies and codes) what the public and individual patients can expect regarding common competency standards and ethical values. In so doing, to implement honourable means to guarantee that all professionals live up to these undertakings15. Furthermore, this study concurs with other authors5 who argue that professionalism is essentially beyond ethics, values and beliefs and includes behaviours and attributes which need the mastering of a complex body of information and skills, caring of others, guarantee of competency, truthfulness, unselfishness and the promotion of public good, autonomy, self-regulation and accountability to society. As can be seen by the various aspects of trying to define professionalism, it is not a static concept but a dynamic, continuous and ever-changing concept, just as the unwritten expectations of professionals held by society are constantly evolving, and being redefined16.
Traditionally, professional values and behaviours were not necessarily taught but rather mirrored ("caught") from role models17. The presence of good role models is still important in promoting professionalism, however, literature argues that this informal process is no longer considered sufficient with the current heterogeneity of students, therefore professionalism must explicitly be taught in the formal curriculum6,13. The results from this study indicate the same trend that both cohorts as well as the entire group felt that professionalism should be taught at tertiary level. The results do however indicate the importance of good role models. These role models are seen as people with similar experiences and who have managed to get through them positively. The influence of role models was repeatedly mentioned in both groups. Observing the professionals' behaviour in certain moral positions, contributes to the participants' understanding of various dimensions of their future professional lives. Given the fact that the influence of role models is ongoing (within the field of education and professional practice) the scope and content of its effect cannot be fully controlled. Although this may be seen as a weakness, the benefit (which is overriding) is that often there is inconsistency between the education and the real life situation. Therefore, seeing how others deal with or manage a specific situation could be greatly beneficial. The same holds true for observing how not to deal with a specific situation.
Professionalism resulting in quality patient care is the main focus of healthcare at large. Although this endeavour should remain central to healthcare delivery, the fast pace of advancement in the field is creating a concern that healthcare providers cannot keep abreast with the changes. As medicine and society evolve, the details of our societal contract have been rewritten and the nature of being a good healthcare provider is continuously renegotiated5. In order to address this new challenge faced by students and professionals alike, self-reflection and reflection among peers is fundamental to the understanding and development of professionalism18, rather than only addressing it in educational settings at tertiary level.
REFERENCES
1. Spiwak, R., Mullins, M., Isaak, C. Barakat, S, Chateau, D. & Sareen, J. Medical Students' and Postgraduate Residents' Observations of Professionalism. Education for Health. 2014; 27(2): 193-199. [ Links ]
2. ABIM Foundation, ACP-ASIM Foundation, and European Federation of Internal Medicine. Medical Professionalism in the New Millennium: A Physician Charter. Annals of Internal Medicine. 2002; 136 (3): 243-246. [ Links ]
3. Levey, N.N. Medical Professionalism and the Future of Public Trust in Physicians. JAMA. 2015; 313 (18): 1827-1828. [ Links ]
4. Becker, GJ. Understanding and Applying the Principles of Contemporary Medical Professionalism: Illustration of a Suggested Approach, Part 2. Journal of the American College of Radiology. 2015; 12 (1), 12-14. [ Links ]
5. Hillis, DJ & Grigg, MJ. Professionalism and the role of medical colleges. The Surgeon. 2015; 13:292-299. [ Links ]
6. Cruess S, Cruess R. Professionalism must be taught. BMJ. 1997; 315: 1674-1677. [ Links ]
7. Sivalingam N, Mal M. Teaching and learning of professionalism in medical schools. Ann Acad Med. Singapore; 2004; 33(6): 706-710. [ Links ]
8. Al-Eraky, MM. Twelve Tips for teaching medical professionalism at all levels of medical education, Medical Teacher. 2015; 37 (11): 1018-1025. [ Links ]
9. Harvison , N. Academic Programs Annual Data Report Academic Year 2011-2012. American Occupational Therapy Association. 2012; Bethesda. Available: https://www.aota.org/-/media/Corpo-rate/Files/EducationCareers/Accredit/47682/20ll-2012-Annual-Data-Report.ashx (Accessed 5 October 2016). [ Links ]
10. Brody, H. & Doukas, D. Professionalism: a framework to guide medical education. Medical Education. 2014; 48: 980-987. [ Links ]
11. Mueller,PS Teaching and Assessing Professionalism in Medical Learners and Practicing Physicians. Rambam Maimonides Medical Journal. 2015; 6(2): 1-13. [ Links ]
12. Chandratilake, M, McAleer, S & Gibson, J. Cultural similarities and differences in medical professionalism: a multi-region study. Medical Educator. 2012; 46: 257-266. [ Links ]
13. Al-Eraky, MM, Donkers, J, Wajid, G & Van Merrienboer, JJG. Faculty development for learning and teaching of medical professionalism, Medical Teacher. 2015; 37 (supl): S40-S46. [ Links ]
14. Shapiro, J., Nixon, LL., Wear, SE. & Doukas, DJ. Medical professionalism: what the study of literature can contribute to the conversation. Philosophy, Ethics, and Humanities in Medicine. 2015; 10(10): 1-8. [ Links ]
15. Mueller,PS. Teaching and Assessing Professionalism in Medical Learners and Practicing Physicians. Rambam Maimonides Medical Journal. 2015; 6(2): 1-13. [ Links ]
16. Hordichuk, CJ, Robinson, AJ & Sullivan, TM. Conceptualising professionalism in occupational therapy through a Western lens. Australian Occupational Therapy Journal. 2015; 62: 150-159. [ Links ]
17. Nortjé, N. Attributes contributing to the development of professionalism as described by dietetic students. SA Journal of Clinical Nutrition. 2016; 1(1): 1-3. [ Links ]
18. Cruess RL, Cruess SR. Professionalism is a generic term: Practicing what we preach. Med Teach. 2010; 32(9): 713-714. [ Links ]
19. Horlick M, Masterton D, Kalet A. Learning skills of professionalism: A student-led professionalism curriculum. Med Educ. 2006; 11: 1-8. [ Links ]
 Correspondence:
Correspondence:
Nico Nortje
nortjenico@gmail.com














