Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
South African Journal of Occupational Therapy
On-line version ISSN 2310-3833
Print version ISSN 0038-2337
S. Afr. j. occup. ther. vol.44 n.1 Pretoria Jan. 2014
SECTION 1
Factors that influence choice of placement for community service among occupational therapists in South Africa
Lebogang Johanna MasekoI; Angeleen ErasmusII; Tania Di RagoII; Jade HooperII; Jo O'ReillyII
IBSc OT (Wits), MPH Wits (Health Systems and Policy); Lecturer, Department of Occupational Therapy, Faculty of Health Sciences, University of the Witwatersrand
IIFinal Year Occupational Therapy students at the time the study was undertaken (2012)
ABSTRACT
BACKGROUND: Provision of health care to all in South Africa is a major challenge as a result of historical inequalities and a mal-distribution of health professionals and services. The disparity in the availability of these services is particularly apparent between rural and urban areas, with relatively few health professionals practicing in rural South Africa. Community service was thus introduced by the Minister of Health in 2003 for all graduates in the medical and allied fields as a means to retain human resources in the public sector and address the inequality of service delivery.
AIM: The purpose of this study was to determine the factors that influence choice of placement for community service amongst occupational therapists in South Africa.
METHODS: Occupational therapists completing their community service year in 2012 participated in this study. Electronic surveys were formulated to explore the factors influencing choice of placement for community service. The surveys were used to determine the relationship between graduates' attitudes and experiences when selecting a placement.
RESULTS: The results indicated that the majority of the participants agreed with the statements that family contact, proximity to home and exposure/experience gained during undergraduate studies were influential in the choice of placements for community service. Urban placements were favoured over rural placements. Financial incentives were found to have minimal influence on the selection of rural placements. Experiences during undergraduate studies, including the perceptions and opinions of students towards their university supervisors, and even more so their clinical supervisors, were found to have a significant influence on choice of placement. The National Department of Health could potentially use this information to review the level of success gained in achieving the initial goals of community service.
Key words: Community service, occupational therapists, community service placement, financial incentives, rural, urban
INTRODUCTION
South Africa has been faced with difficulties in employing and maintaining the number of health professionals at rural hospitals, clinics and health centres in the public sector, thus resulting in a poor health professional-to-patient ratio in rural vs. urban areas. The disparity in the availability of healthcare services and professionals is particularly apparent between the private and public sectors, the provinces, as well as the rural and urban areas, with relatively few health professionals practicing in the rural parts of South Africa1-3. For example, in the under-developed provinces such as the Eastern Cape and the Northern Cape there is a total of 192 and 88 occupational therapists respectively, as compared to the more developed provinces of Gauteng and the Western Cape which have 1500 and 1109 occupational therapists respectively4.
Human resource development and management are among the more difficult challenges in low and middle income countries such as South Africa as the pool of health workers has been depleted and could be getting worse5. This is due to a number of factors such as the low rate of production of health workers, deaths, attrition and emigration. Migration to greener pastures, where almost a third to a half of South Africa's medical graduates emigrate to work abroad in countries like America and the UK continues to be a problem for the South African health system5.
The process of planning improvements in human resources for health is guided by the National Department of Health's Ten Point Plan, which incorporates human resources planning, development and management as one of the priorities6. The human resource and health priorities are located within the policy initiative launched by the Minister of Health in August 2011 to develop a National Health Insurance as the primary financing mechanism for the health system, and thereby provide more equitable access to healthcare7.
A number of initiatives have been implemented to remediate and overcome the adverse effects of limited healthcare services in an effort to increase the number of health care workers in the public health service. These include the emphasis on scarce skills and the implementation of rural allowances, which came into effect on 1 July 20033,8, and more importantly the extension of compulsory community service (CS) to include all newly graduated health professionals including occupational therapists. The aim of this was to structure the placement of these health professionals within the public service as well as to retain the workforce in the country1,3,9,10.
Various factors can lead to a therapist's choice of a particular placement for the year of CS. These factors can range from experiences during undergraduate training, environmental / physical factors, individual personality traits as well as exposure to various fieldwork settings and fields of practice.
This paper aims to explore the factors that influence choice of placement for community service occupational therapists.
LITERATURE REVIEW
Compulsory CS in South Africa was implemented by the Minister of Health in 2003 for all graduates in the medical and allied health fields as a means to retain human resources as well as overcome the mal-distribution of personnel between the private and public sector, urban and rural areas as well as between the provincesI,3,5,8.. This compulsory requirement entails one year of practice in the public sector for all health professionals following their graduation. If the health professionals do not complete CS they cannot be registered by the Health Professional Council of South Africa (HPCSA) to practise in South AfricaI,3. The CS programme includes a process in which five pre-determined placements are selected by the students in their final year of study3. As stipulated by the South African Qualifications Authority (SAQA) the occupational therapist will be registered in the Public Service: Community Service Category for the duration of that year3.
The responsibility for the final placement of CS health professionals in public service posts in the provinces lies with the National Department of Health. The process of placement is usually finalised by September of each year to ensure that graduates have certainty about where they will take up posts from January of the following year3. According to the National Department of Health the main objective of community service is to ensure improved provision of health services to all the citizens of our country. This also provides young professionals with an opportunity to develop skills, acquire knowledge, behaviour patterns and critical thinking that will help them in their professional development3,11.
Not only does community service allow for the provision of occupational therapy services in under-developed rural areas, it also provides opportunities for the newly qualified occupational therapist to prepare, apply and reflect on the academic and practical coursework completed during the four years of study. Furthermore, it allows the therapist to refine and develop skills as members of the multi-disciplinary team, while contributing towards the delivery of more equitable health services11,12 .
Success or failure of these programmes largely depends on the degree of support given in the broader health system13. Governments must clearly state what they expect from compulsory service personnel. In South Africa for example, vague guidelines for community service doctors resulted initially in uneven utilisation by clinics and hospitals14. Several authors advised that compulsory service should be supplemented by a support system and incentives2,15 to maximise the service, however this may be more costly than compulsory service without incentives. For instance, in Zambia, before its incentive-based health workforce retention scheme was implemented, many doctors assigned to rural areas resigned from government service to avoid serving in rural posts15. In South Africa, better staffing levels in rural hospitals, shorter patient wait times and more frequent visits to outlying clinics by health workers have since been reported13 as a result of the programme.
The retention of health professionals in the rural areas after their community service has been completed remains unclear for most countries, including South Africa15.
Factors influencing choice of placement
Many factors have been shown to influence the choice of placement among individual community service therapists. These are broadly classified into four categories, each with various components related to the category. These are the physical environment (preference of working in a rural and urban area, resources and environment), human environment (managerial structures and human relations), incentives (financial and non-financial) and individual factors (attitudes, personality, values and undergraduate experience)8,10.
Similarly, the Public Service Co-ordinating Bargaining Council (PSCBC) identified the following factors as being influential in the choice of placement: funds, financial incentives (for rural environments), job satisfaction, career opportunities, security, family, work relationships, and workload1.
Physical Environment
The physical environment is an influential factor in community service placement choice and incorporates aspects such as preference for working in a rural or urban area, available resources and the work environment6,10,16. In South Africa, private hospitals and urban-based public health facilities are generally more resourced than rural-based public health facilities7,10,13. Negative influential factors regarding work in rural environments include the desire to work as a 'specialist', personal, social and professional factors such as a lack of professional development opportunities in a rural setting, lack of support, professional and social isolation as well as workload11. Positive influential factors include the tranquility of rural environments and feelings of safety as compared to urban settings11 .
Human Environment
The human environment refers to managerial structures and human relations such as adequate supervision and support. Staff shortages and losses in the public health sector due to immigration, as well as migration to the private sector, exacerbate retention problems because they result in increased workloads that contribute to the demanding nature of the health workplace10. They erode supervision, mentorship and support for the newly qualified community service therapists10. At the same time, population health needs are growing and changing in South Africa, in ways that add to these demands.
Incentives
The World Health Organization (WHO) defines incentives as "all rewards and punishments that providers face as a consequence of the organisations in which they work, the institution under which they operate and the specific interventions they provide"17:61. Incentives for health workers are broadly seen as either financial or non-financial:
Financial incentives may be direct or indirect. Direct financial incentives include salary, pension and allowances for accommodation, travel, childcare, clothing and medical needs. Indirect financial benefits include subsidised meals, clothing, transport, childcare facilities and support for further studies8,13.
Non-financial incentives include holidays, flexible working hours, access to training opportunities, sabbatical/study leave, planned career breaks, occupational health counseling and recreational facilities18. Non-financial incentives create a stabilising influence, after the more rapid effects of financial incentives, by sustaining health worker commitment and sending a message that health workers are supported. Although non-financial incentives are ultimately financial because they cost money to provide, they cater to longer-term career, welfare and systems benefits that may provide greater stability13.
Individual factors - attitudes, personality, values and undergraduate experience
Undergraduate rural programmes have been shown to promote students' positive perceptions of rural and remote practice through exposure to a rural location, and factors such as rural fieldwork experience and fieldwork supervisors are likely to be influential11. Occupational therapy students, in comparison to other allied health students, consistently ranked at or near the top, measures of awareness of community needs, perceptions that specific actions can relieve community need, perceptions that they possess skills to effectively serve the community, sense of responsibility to serve the community, sense of moral obligation based on personal norms, and ability to empathise with those in need11. Literature also shows that students that are originally from rural backgrounds are more likely to seek employment placement in those areas. A curriculum that includes rural fieldwork reinforces their intentions to practise in those areas. The likelihood of students with a rural upbringing seeking rural employment was found to be higher than their urban counterparts11.
Most of the research carried out so far looks specifically at factors influencing choice of rural placement for community service.
METHODS
Aim
The purpose of this study was to determine the factors that influence choice of placement for community service amongst occupational therapists in South Africa.
Study design
A cross-sectional, descriptive, quantitative study was conducted.
Study population and sampling
The 2011 final year occupational therapy students of the University of the Witwatersrand, University of Pretoria, and University of Limpopo were approached to participate in the study while they were completing their community service in the year 2012. The participants were contacted telephonically at the various hospitals at which they were working. Their e-mail addresses were obtained and information sheets were sent to these participants' electronic mail addresses. Convenience sampling was used as the researchers not only contacted the specified universities, but also approached the community service therapists at various occupational therapy events such as workshops and courses as well as while on clinical fieldwork at hospitals in Gauteng. Thereafter, 'snow-ball sampling' was used to recruit more participants who were asked to pass on the researchers' contact details to other community service therapists who might not be known to the researchers. These potential participants were asked to contact the researchers if they were interested in being part of the study. Participants were included if they were completing their community service year in 2012, had internet access and had returned completed questionnaires, and excluded if they had completed their CS before 2012, refused to participate and/or returned incomplete questionnaires.
Instrumentation
A self-administered electronic survey in the form of a questionnaire consisting of closed-ended questions was used. A 5-point rating/ likert scale was used in which numbers were assigned to answers to determine the degree of intensity of the influential factors affecting the individuals' choice of placement for CS. The answers were quantified via an ordinal technique ranging from 1- strongly disagree to 5-strongly agree, thus formatted to provide a numerical representation of each participant's answers. The survey questions were based on literature investigating factors that influence occupational therapists' perceptions of rural and remote practice. The most frequently identified factors, from the literature, as influencing choice of placement were selected to form the basis of the questions I9.
Response bias was dealt with in two ways:
- Wave analysis - submissions were monitored weekly to determine the average response rate and changes in these responses.
- Generic reminder electronic mails - a reminder was sent to all participants, informing them of the final date for submission.
Data analysis
Descriptive analysis was carried out and results represented in the form of graphs and tables.
RESULTS
Out of a total of seventy potential participants who were sent the electronic information sheet with the link to the questionnaire, thirty two questionnaires were completed, however not all thirty two participants completed all the sections of the questionnaire. This meant that only thirty questionnaires had completed data and were eligible for analysis. The demographics of the participants are represented in Table 1.
The majority of the participants (93.3%) were within the age group 20-25 and were single. Sixty percent were graduates of the University of the Witwatersrand (Wits) and the majority were working in urban settings (76.7%).
The questionnaire was drawn up by the researchers and piloted for content validity and clarity with a random selection of 10 community service occupational therapists who completed their community service year at the end of 20II. These individuals came from five hospitals in the Johannesburg area. Feedback on the questionnaire received from the pilot study was used to address inconsistencies, irrelevant information that needed to be removed as well as any relevant, additional information that needed to be included. The questionnaire consisted of two sections- the first section required participants to complete their demographic information and the second section consisted of likert scale questions, making up a total of 2I questions, not grouped into any particular categories.
Research procedure
After ethical clearance was granted by the University of the Witwa-tersrand Committee for Research on Human Subjects, participants were approached. The study was explained to them and consent was obtained. The participants were informed that any exchanged information would only be accessed by the researchers, thereby respecting confidentiality.
Accessing the web link which re-directed participants to the electronic survey was regarded as implied consent and was communicated to potential participants on the information sheet. Data collection took place from January until end of July 2012. By setting a time limit the number of participants and non-participants were identified, allowing for a response/non-response analysis. Once completed, the surveys were returned to the researchers electronically for further analysis.
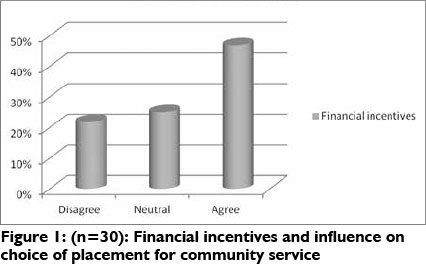
Financial incentives
Almost half of the participants (46.8%) agreed with the statement that financial incentives such as rural and scarce skills allowances influence choice of placement for community service in rural areas.
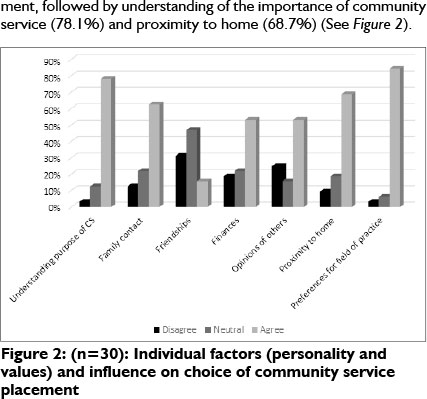
Individual Factors
Individual preference for field of practice was found to be the most likely individual factor influencing choice of community service placement, with 84.3% of the participants agreeing with this statement, followed by understanding of the importance of community service (78.1%) and proximity to home (68.7%) (See Figure 2).
Opportunity for personal growth and dependants
Seventy five percent of the participants reported that they considered opportunities for personal growth in their choice of community service placement, while 53% considered their dependants as having an influence (See Figures 3 and 4).
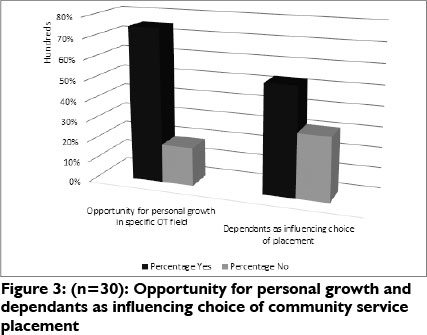
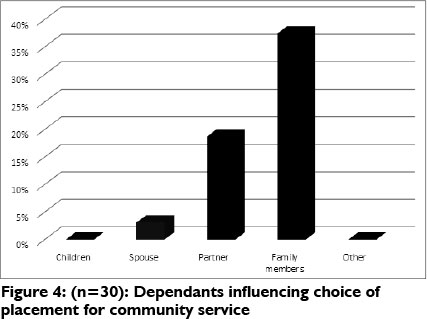
Family members were found to be the most influential dependants in the choice of placement (37.5%), followed by the partner (18.7%).
Human Environment
Experience gained during years of study was the most influential for 81.2% in their choice of community service placement, as well as exposure to rural and urban placements (71.8% and 68.7% respectively). The majority of the participants (65.6%) agreed with the statement that urban placements are generally favoured over rural placements as community service placement choices. It was agreed that clinical supervisors had more of an influence on choice of CS (56.6%) than did the University supervisors (40.6%) although they did play a role (see Figure 5).
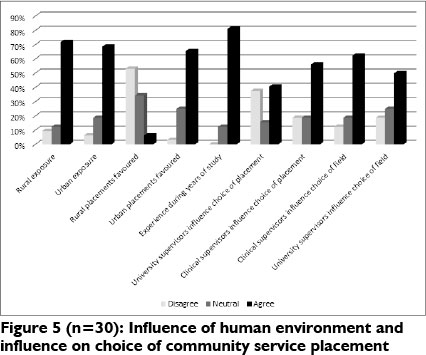
Physical Environment
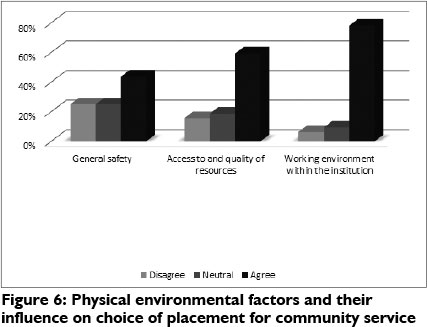
The physical environmental factors that were of importance to the participants were the working environment within the institution (78.1%), access to and quality of resources (59.3%) and general safety and access to medical resources (43.7%) (see Figure 6).
DISCUSSION
Occupational therapists completing their community service year in 2012 completed electronic surveys that were formulated to explore factors that influenced their choice of placement for community service. Participants reported that they selected placements for community service based on opportunity for personal growth and professional development. This may account for the low percentage selecting rural placements as it is felt that there is less mentorship, supervision and assistance provided in those settings, thus demanding more initiative and responsibility on the part of the newly qualified therapists11. In urban placements, where OT departments tend to be larger, there are opportunities for CS therapists to be placed in a specific field of practice, or rotated between specific fields of practice during the CS year. In rural OT departments, CS therapists are more likely to obtain 'generalist' experience, as well as management and service development experience.
On the other hand, some CS therapists may see this demand for more initiative and responsibility as a positive factor i.e. they do not continue to be 'spoon-fed' and constantly watched during CS, which enables them to gain independence.
Proximity to home, family contact, relationships and dependents were factors that significantly influenced their choice of placement, while the influence of friendships was found to be of neutral value on choice of placement. These factors may negatively impact on the choice of rural placements as these often require relocation. Given that the majority of the participants were within the age group 2025 it is unsurprising that they would prefer placements that were in close proximity to home and family members20 as some might still need the support of their families, especially in their first year of work, which can be a daunting experience. On the other hand, it would not have been uncommon to assume that young professionals in this age group might rather welcome some adventure or opportunity to spread their wings.
Exposure to rural and urban settings throughout the course of tertiary studies was identified as an important factor, thus emphasising the need for opportunities to practise in both settings during the years of undergraduate studies. Without prior rural exposure graduates would be less likely to select a rural placement due to lack of awareness of what to expect and how occupational therapy is applied in a rural setting16, and concerns about being under-prepared and unskilled for rural practice11. Financial incentives were found to motivate choice of placement in rural settings, although only 46.8% agreed with the statement, proving to be less significant than in previous research. This factor, could have been influenced by the inherent bias in the sample, in that most participants had chosen or were working in more urban placements. On the other hand this also raised questions regarding the effectiveness of incentives in attracting health professionals to work in rural settings13.
Learning and growth is facilitated by the resources available in the working environment11,16,19,20,21,22, which makes it unsurprising that the availability of resources, opportunities for learning, career development and growth as well as the working environment within various placements, proved to be a factor that the majority of the participants agreed with.
Preference for a particular field of practice when choosing a CS placement was agreed with by most participants, and placements that offered physical occupational therapy services appear to be favoured above paediatrics, public health and psychiatric placements. The reasons for this may not necessarily be based on preference alone, but also on the number of posts available within each field of practice23.
Experiences during undergraduate studies were highly regarded as an influencing factor as 86.7% agreed with this statement. This is because fieldwork experiences have a high influence on the students' future employment intentionll. Similarly, perceptions of graduates towards university supervisors as role models did not prove to be a significant influencing factor on choice of placement, whereas perceptions towards clinical supervisors were. Graduates spend more one-on-one time with clinical supervisors on fieldwork as compared to university supervisors, which may account for this finding. Positive experiences with clinical supervisors may enhance the preference for a particular placement and clinical field, while negative experiences may have the opposite effect thus placing emphasis on the importance of role-modelling within the clinical settings. Additionally, the same clinical supervisors may ultimately end up being their colleagues and / or supervisors during their CS year, so it is not surprising that this factor has an influence on choice of placement.
Limitations to the study
Due to the nature of the survey being in electronic format, this excluded people who have little or no internet access. The sampling of CS therapists only in one province- Gauteng- may have had a negative influence on the results, and thus limited the interpretation of the results. Sampling therapist in a (relatively) well-resourced province, introduced bias into the data as the therapists who do their CS in Gauteng - in urban areas - could be more likely to prioritise those factors, than say a sample of CS therapists that selected outlying provinces and rural areas. In addition, sampling therapists already doing their CS year, as opposed to students who are in the process of making their CS selections, might also have produced different results.
CONCLUSION
There are varying human environmental, physical environmental and individual factors that influence choice of placement for community service among occupational therapists in South Africa, and certain factors were found to have more influence than others. Individual preference in terms of the different fields of practice (physical, psychiatry, paediatric and public health) was selected as the most significant influencing factor when selecting placement for community service and highlights the importance of exposure to the various fields of practice during undergraduate studies so as to establish a preference. In the same light, perceptions and opinions of graduates regarding their university supervisors, and even more so, their clinical supervisors were found to influence choice and attitudes towards the different fields of practice, emphasising the importance for university supervisors as well as clinical supervisors to provide good role modelling within the clinical setting.
The proximity of the community service placement to the home and factors such as family contact, relationships and dependants are highly regarded, and could have been influenced by the fact that the majority of the participants were within the 20-25 age group and might not necessarily want to be away from their families, especially in their first year of working. Opportunity for personal growth and professional development were regarded as significant influencing factors, indicating that CS occupational therapists prefer placements where they are able to learn and gain experience in order to further improve their clinical skills.
Rural and urban fieldwork exposure and experiences throughout the duration of undergraduate studies have proven to have impact on graduates' opinions and preferences in terms of selecting community service placements in those areas. Without these experiences, graduates would be less likely to select certain placements, thus reinforcing the value of rural and urban fieldwork exposure in undergraduate studies and the importance of the inclusion of both types in university curricula.
RECOMMENDATIONS
On a broader policy scale, the NDoH would benefit from paying attention to the factors found to be most influential in CS placement selections, in an effort to evaluate the extent to which the original objectives of CS are being achieved. For example, the majority of participants agreed with the statement that financial incentives such as rural and scarce skills allowances influence choice of placement for community service towards rural areas, however they also felt that urban placements are generally favoured over rural placements. This not only contradicts the view that financial incentives such as the rural allowance play an important role in attracting graduates to rural environments, but also raises the question that perhaps further exploration into the effectiveness of financial incentives in attracting graduates to rural placements is required. Focussing on factors that are identified as most influential could assist in not only placing suitable graduates in specific placements, but possibly improve the retention of these graduates in those posts in the public service as well.
REFERENCES
1. Health Do. Department of health allied health professions community service: 2007 letter. 2007. [ Links ]
2. Organization WH. World Health Organization Global Policy recommendations on access to health in remote and rural areas, through improved recruitment and retention: The South African Context. Equinet and RHAP 2011. [ Links ]
3. Health NDo. National Department of Health Annual Report 2003/2004. Pretoria: National Department of Health, 2004. [ Links ]
4. Daffue Y. Regional breakdown of occupational therapists per province based on postal address. In: Maseko L, editor. Health Frofessions Council of South Africa IT Department- Statistics and data analysis 2014. [ Links ]
5. McPake CHaB. How to bridge the gap in human resources for health. The Lancet, 2004; 364(9443): 1451-6. [ Links ]
6. Health NDo. NDOH Human Resources for Health. In: Health Do, editor. Pretoria, 2013. [ Links ]
7. Health Mo. National Health Insurance. Policy Paper. Government Notice 657. Pretoria2011. [ Links ]
8. Ditlopo P Blaauw D, Bidwell P Thomas S. Analyzing the implementation of the rural allowance in hospitals in North West Province, South Africa. Journal of Public Health Policy, 2011; 32: S80-93. [ Links ]
9. Health Ndo. Human Resources for health South Africa. HRH strategy for the health sector:2012/13-2016/17. In: health Ndo, editor. Pretoria2012. [ Links ]
10. Gilson L EE. Supporting the retention of health resources for health: SADC policy context. In: (HST) RNfEiHiSAEaHST, editor: Centre for Health Policy, School of Public Health University of Witwatersrand; 2005. [ Links ]
11. McAuliffe T, Barnett F. Perceptions towards rural and remote practice: A study of final year occupational therapy students studying in a regional university in Australia. Australian Occupational Therapy Journal, 2010; 57(5): 293-300. [ Links ]
12. Hoppes S, Hellman CM. Understanding occupational therapy students' attitudes, intentions, and behaviors regarding community service. American Journal of Occupational Therapy, 2007; 61(5): 527-34. [ Links ]
13. S R. Monitoring the effect of the new rural allowance for health professionals. Health Systems Trust, 2004. [ Links ]
14. SJ R. Compulsory community service for doctors in South Africa- an evaluation of the firt year. South African Medical Journal, 2001; 91: 329-36. [ Links ]
15. WHO. compulsory service programmes for recruiting health workers in remote and rural areas: do they work? Bulletin of the WHO, 2010; 88(5). [ Links ]
16. Brockwell D, Wielandt T, Clark M. Four years after graduation: occupational therapists' work destinations and perceptions of preparedness for practice. Australian Journal of Rural Health, 2009; 17(2): 71-6. [ Links ]
17. Organization WH. World Health Report 2000: Health Systems: Improving Performance. Geneva: WHO, 2000. [ Links ]
18. Zurn P Dal Poz MR, Stilwell B, Adams O. Imbalance in the health workforce. Human Resources for Health, 2004; 2(1): 13. [ Links ]
19. Polatajko H, Quintyn M. Factors affecting occupational therapy job site selection in underserviced areas. Canadian Journal of Occupational Therapy, 1986; 53(3): 151-8. [ Links ]
20. S R. Junior occupational therapists' continuity of employment: What influences success? Occupational Therapy International Journal, 2006; 6(4): 277-97. [ Links ]
21. Mills A, Millsteed J. Retention: an unresolved workforce issue affecting rural occupational therapy services. Australian Occupational Therapy Journal, 2002; 49(4): 170-81. [ Links ]
22. Ho C-C. A study of the relationships between work values, job involvement and organisational commitment among Taiwanese Nurses [professional doctorate]. Queensland: Queensland University of Technology; 2006. [ Links ]
23. Lehmann U, Dieleman M, Martineau T. Staffing remote rural areas in middle-and low-income countries: a literature review of attraction and retention. BMC health services research, 2008; 8(1): 19. [ Links ]
 Correspondence:
Correspondence:
Lebogang Johanna Maseko
Lebogang.Maseko@wits.ac.za














