Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
South African Journal of Occupational Therapy
versão On-line ISSN 2310-3833
versão impressa ISSN 0038-2337
S. Afr. j. occup. ther. vol.44 no.1 Pretoria Jan. 2014
SECTION 1
Anxiety and the perceived adequacy of information received by family members during the in-patient rehabilitation of patients with brain injury
Deborah BarrieI; Denise FranzsenII; Katherine GradidigeIII
IB.OT (Stellenbosch University); M.Sc OT (Wits); Postgraduate Student Department of Occupational Therapy, School of Therapeutic Sciences, University of Witwatersrand Occupational Therapist: Summit Rehabilitation, Auckland Park
IIBSc OT (Wits), MSc OT (Wits); Senior Lecturer, Department of Occupational Therapy, School of Therapeutic Sciences, University of the Witwatersrand
IIIBSc OT (Wits), MSc OT (Wits); Part-time Postgraduate Lecturer, Department of Occupational Therapy, School of Therapeutic Sciences, University of the Witwatersrand
ABSTRACT
Whilst patients with brain injury are undergoing rehabilitation, their families are expected to understand and remember complex information provided by the healthcare team. Previous studies have shown that high levels of anxiety impair a person's information recall and their ability to interpret complex information.
This study aimed to describe the level of anxiety of family members of patients with brain injury admitted to a six-week rehabilitation programme. The relationship between the family members' level of anxiety and their perception of the adequacy of the information provided by the rehabilitation team, as well as the length of time since the patients' injury and their Functional Independence Measurement (FIM) score was established. Family members completed the anxiety subscale (HADS-A) of the Hospital Anxiety and Depression Scale and an Information Checklist on three separate occasions during the patients' admission.
Results indicate that family members were anxious throughout the duration of the patient's rehabilitation with a decrease in average anxiety scores and a corresponding increase in the satisfaction with the information offered over this time. No significant correlation was found between the family members' anxiety and other variables, indicating that factors influencing family members' anxiety were not related to the length of time since injury and the severity of the patient's motor and cognitive outcomes.
Key words: Anxiety, Perception of adequacy of information received, Family members', Patients with brain injury
INTRODUCTION
When an individual suffers a life threatening incident like a traumatic brain injury (TBI) and stroke, relatives or family members' first experience of shock and stressors include a sense of uncertainty and fear of losing the patient1. These stressors change when the patient survives and is admitted to rehabilitation2. The emotional and behavioural responses then include anxiety that the families experience related to a lack of understanding about the implications of the patient's condition as well as how they will care for the patient at home2. Planning for the patient's future as well as possible financial problems and changes in the responsibilities and roles within the family have all been cited as anxiety provoking3.
To assist the families of patients with brain injury with these is-sues4, comprehensive family and caregiver education programmes have become critical in providing families with the opportunity to obtain the necessary knowledge and understanding of the patient's condition5. In the private health care context in South Africa, family members and the identified primary caregiver of the patients with brain injury are provided with education and training by the multi-disciplinary team treating the patient during inpatient rehabilitation. Occupational therapists are involved in family meetings and individual consultation. They offer verbal and written information to those who will assist in self-care tasks and other activities once the patients are discharged. The goal of this is to equip family members' to assist the patients at home, post discharge, as they still often require care due to their residual deficits, be they physical, cognitive or both6.
The effectiveness of these education programmes can also be impacted on by the length of inpatient rehabilitation which can be relatively short, usually a period of six to nine weeks for private health care in South Africa, as determined by the availability of funds from private medical insurance.
Research shows that various other factors including the family's emotional response as well as the timing, amount and relevance of the information provided, result in the family members often reporting that they did not receive the relevant information or did not remember the information they were given6. Thus the education of the family members' needs to be intensive if all the information they require is to be imparted in the time available4. It is therefore important for the rehabilitation team to take responsibility for both the content and the educational process when imparting this knowledge7.
LITERATURE REVIEW
Patients with brain injury and their family members' are reported to experience a "rollercoaster of emotions" 8:19 throughout the period of their recovery, rehabilitation and discharge preparation. Research on these emotions, usually measured using self-report scales, include reports of depression, psychosocial dysfunction, emotional and psychological distress and burden of care8.
A study by Paterson et al9 indicated that family members' of patients with TBI and stroke appear to experience severe anxiety in the period of in-patient rehabilitation leading up to the discharge of patients with brain injury. It has been found that the impact of these emotions affected the family members' ability to absorb information as they were not able to give their full attention to learning and processing the information provided10.
A study by Morris11 confirmed this when caregivers of patients with TBI reported that anxiety restricted their ability to absorb the information, affecting their perception and experience of the education programme offered, even when it was presented in a written format . Ley12 had also previously demonstrated a relationship between anxiety and the ability to process information accurately in family members' with high levels of anxiety in his study.
The inability to understand the complexity of the brain injury or the healthcare system and medical jargon were reasons family members' gave for not being able to understand and pay attention to the information they were given. The family members' and caregivers reported that the healthcare and rehabilitation settings were foreign to them and they were not clear about the roles of the different healthcare professionals, so they were not sure whom to ask about the various aspects of care. They also found family meetings intimidating and rushed9. Not being able to concentrate and process and recall complex information could possibly also lead to a further increase in anxiety.
A later study in 2006 by Lefebvre and Levert13 on the perceptions of family members' of the education and information they received while patients received rehabilitation, indicated that they felt that they did not receive sufficient information and that the information that they did receive was often irrelevant and imprecise. Even after the patient with brain injury was discharged from in-patient rehabilitation, family members' were confused about the prognosis of the condition, services and equipment available and what to expect in terms of the patients' abilities and behaviour. These concerns occurred even though rehabilitation professionals had a well-documented family education programme and reported that family members' were supplied with extensive verbal information and written material, as well as individual consultations and multidisciplinary discharge planning meetings during the patients' in-patient rehabilitation period9.
It is thus the responsibility of the rehabilitation team not only to provide relevant, clear and adequate information to the families, but to evaluate and be aware of the family members' ability to understand and absorb the information. Murray et al14 indicated that providing honest information about the patient's status and prognosis, community resources, financial support, resources for emotional support and practical advice was ranked highly in meeting the needs of families of patients with brain injury. Other studies have concluded that information must be complemented with hands on training to decrease caregiver burden and to improve learning15,16. A study by Smith and Testani-Dufour16 reported that the family members' literacy levels as well as their learning readiness should be assessed prior to an education programme being started. Motivation and ability to learn at a particular time was considered in the learning readiness and it was suggested that factors such as level of anxiety should be examined when determining the readiness to learn16,17.
Timing is therefore important when providing information and it was found that some family members' wanted information immediately to help them cope with the situation whereas others were only ready to start with the education programme in the second week of rehabilitation. However the length of the in-patient treatment may be dictated by external factors like medical insurance availability, so that waiting for the time when the family member is ready to receive the information or providing the necessary repetition is not always possible9.
The amount of information family members' received also overwhelmed them and while rehabilitation professionals believed that written information could overcome these problems, family members' reported either not remembering getting the written information or not reading it as there was too much. Relevance of information was also a concern in individual consultations and multidisciplinary discharge planning meetings, which family members' felt did not focus on the family's concerns but rather priorities set by the rehabilitation professions for the patient with brain injury9.
Aim of the study
The aim of this study was to describe the relationship between the anxiety levels of family members or caregivers of patients with brain injury, and their perceptions of the adequacy of the information they received as well as their ability to understand and use the information, in two private health care in-patient rehabilitation facilities in South Africa. The effect of the timing of the information delivery, the functional level of independence of the patients with brain injury as well as the length of stay at a rehabilitation facility on the family members' and caregivers' perception of the adequacy of the information was also investigated.
METHODOLOGY
A quantitative, prospective, longitudinal, analytic survey study design was used with family members' who were to be the primary caregivers of patients with moderate to severe brain injury. These family members were recruited when the patients were admitted for rehabilitation in two private health care facilities. They were included if they were over 18 years of age; able to complete the self-report questionnaires and were willing to be available for at least six weeks, to complete the follow-up questionnaires. No exclusion criteria for pre-existing anxiety disorders were applied. Once ethical clearance to complete the study and written permission were obtained, each member of the family selected, provided signed informed consent to participate in the study.
Data were collected from the family members on three separate occasions using a demographic information sheet and the Anxiety Scale of the Hospital Anxiety and Depression Scale (HADS), a 14-item self-reporting assessment of anxiety and depression18. Only the HADS-Anxiety (HADS-A) subscale was used as only anxiety was assessed. An optimal balance between sensitivity and specificity has been achieved in most studies with a score of 8 or above on the HADS-A indicating a problem. Convergent correlations between the HADS-A and other anxiety scales were in the range 0.49 to 0.83 indicating the HADS-A performs well in assessing the symptom severity and the presence of anxiety disorder in the general population, patients and caregivers. Internal consistency for the. HADS-A measured using Cronbach's alpha varies from 0.68 to 0.9319.
An Information Checklist developed by the researcher used a Likert scale with a score of 5 points for "Received Sufficient Information"; a score of 3 points for "Received information, but not sufficient"; and a score of 1 point for "Did not receive sufficient information". This questionnaire was used to determine the family members' perception of the understanding and adequacy of the information they received. In the final data collection period they were also asked to complete a questionnaire about any medication they were taking for control of anxiety.
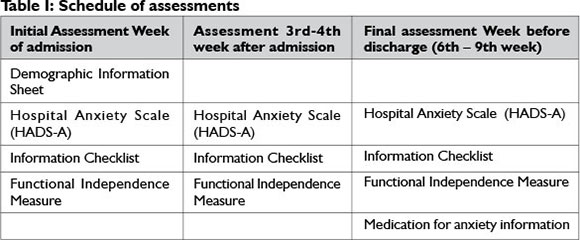
The researcher recruited the participants and provided them with the abovementioned questionnaires, which were handed out and completed within the first week of the patient's admission, during the 3rd - 4th week after admission, and within the last week before discharge. Throughout the patients' stay at the rehabilitation facility, the scores from the Functional Independence Measure (FIM)19, which were routinely recorded during this period by the team to assess the patients' level of independence on a weekly basis, were also collected for the study (see Table I).
The mean age of the members of the families participating was 46.85 years with the oldest respondent being 77 years old and the youngest 22 years of age. Sixty one point seven percent (61.7%) of the participants were female. The largest group of participants (44%) were the spouses of the patients, while parents or siblings made up 17.6% of the sample. The rest of the participants were either the patients' children or some other relation.
Forty seven percent (47%) of the participants had a Grade 12 as their highest level of education and 41.2% had post school qualifications with 2.9% having completed post-graduate studies. Only 8.8% had a level of education at Grade 10 or less.
The patients with brain injuries were transferred to the rehabilitation facility from the acute facility with a mean of 33 days after the onset of the illness or injury.
Anxiety and information outcomes
There was a decrease in the mean anxiety scores of the HADS-A assessment over the weeks of the patients' stay in the rehabilitation units (Table 2). A statistically significant difference was demonstrated between the initial and 3rd-4th week assessment on the HADS-A scale (p=0.01), and between the initial and final assessment on the HADS-A scale (p=0.02).
Family members' completed the questionnaires independently and returned them to the researcher in a sealed envelope. Since the researcher was an active member of the therapy team, to ensure that she did not influence the amount and type of information given to the family members', she was blinded to the data until after the final data collection period. All data remained in the sealed envelopes until the patient was discharged.
Data were analysed through the Epilnfo statistical package20 by means of a non-parametric Chi-Squared test due to the small sample size. The difference between the Anxiety Scale of the HADS over the three different occasions was established. Spearman rank correlation coefficients were used to determine the relationship between the time since injury, the change in anxiety scores, the change in perceived information adequacy and the change FIM scores.
RESULTS
Demographics
Although a total population sampling was used and 34 members of the family of the patients with brain injury were recruited over a six week period, not all the assessments were completed by all the participants, with only 17 participants completing the questionnaires in the final assessment. This loss to follow up was as a result of the medical condition of some patients deteriorating which resulted in a transfer to another hospital. Three patients passed away during the study and others were discharged from rehabilitation for various reasons before the 6th week.
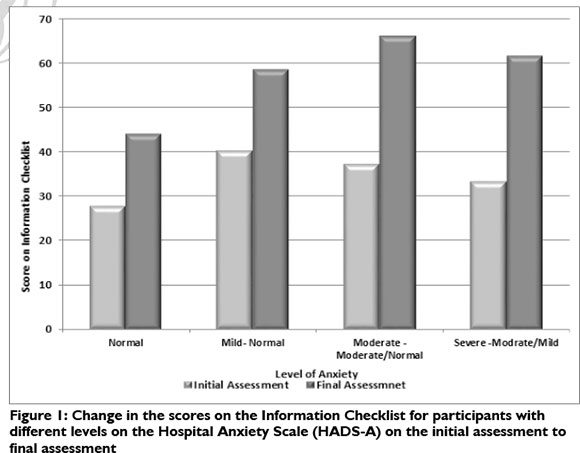
The mean anxiety level however remained above the cut-off of seven on the scale, which indicates a normal range for anxiety. All family members' anxiety moved down one level on average except for those with moderate anxiety, where the level still varied between moderate and normal anxiety (Figure 1 on page 34).
Out of a possible score of 70 on the Information Checklist the mean scores for the perceived adequacy of information over the three assessment periods can be seen in Table 2. Family members reported an increase in the adequacy of the information given to them over time although a statistically significant difference was only demonstrated between the initial and final assessment (p=0.01) with a score of 60 out of 70 being achieved in the final assessment.
Family members' also commented on what expectations they had in relation to what information they required when they indicated that insufficient information was provided. This included:
- "Daily updates on improvement and what I can expect; Weekly updates from the doctor "
- "To know if he will be the same person he was before all this happened, or will he regain his memory and function just like a normal person."
- "Recovery process - what to look for, how long, what to expect. Activities that can be undertaken"
There was also an increase in the mean score of the total FIM score across the data collection period out of a possible 210 points (Table 2). A statistically significant difference was demonstrated between the initial and 3rd- 4th week assessment (p=0.00) as well as initial and final assessments (p<0.00).
A non-significant moderate correlation was noted in the change in the HADS-A Scale scores between initial and final assessments and change in Information Checklist Scores between initial and final assessments. When this change was correlated a negative association (r = - 0.54) between these two variables was found. This indicated that as the participants' anxiety decreased, the scores for perceived adequacy of information improved.
When the change between the initial and final scores on the Information Checklist which were significantly different were further analysed it was clear that the participants with severe initial levels of anxiety had a lower score for the perceived adequacy of the information received when compared to those with initial moderate to mild anxiety levels (see Figure 1). The participants with initial moderate to severe anxiety levels were also found to have the greatest increase in their perception of the adequacy of the information received in relation to decreased anxiety levels. Unexpectedly those who reported normal anxiety levels reported the lowest scores on the Information Checklist for both the initial and final assessments.
No association was found between the length of time since injury with only a low correlation between the change in the patients' functional independence (FIM score) and the change in the anxiety scores of the participants (r = 0.25). Four participants were taking prescribed medication from a medical doctor and one was taking herbal medication in addition to the prescribed medication. There was a correlation between those taking prescribed medication and their anxiety scores.
DISCUSSION
The initial mean assessment score on the HADS-A found that family members' of the patients with brain injuries, presented with 'moderate' levels of anxiety in the first week of the patients' admission for inpatient rehabilitation. Follow up assessments in the 3rd - 4th week and in the discharge week found that the mean anxiety score had decreased significantly to a 'mild' level, particularly in the pre-discharge week.
This significant decrease seen in the mean level of anxiety of family members' over the period of the study according to the literature could be attributed to a number of factors, including gaining insight into the client's condition, improvements noted in the client and coping mechanisms of the family members'15,21-23.
The main of objective of this study was to establish the relationship between the family members' anxiety levels and their perception of the adequacy of the information they received from the rehabilitation team. Results indicate that a moderate relationship does exist as there is a decrease in anxiety measured on the HADS-A and an increase in the processing of information by family member participants. These findings support the research which found that the level of anxiety experienced by family members' affects their ability to process and recognise the adequacy of the information provided to them about goals9, plans and care of patients with brain injury during rehabilitation. In this study the statistically significant decrease in the participants' anxiety occurred first during the second assessment with the significant increase in the Information Checklist scores indicating a better understanding of the information given occurring later in the third assessment.
The lack of significance of the association between the changes in the two variables may have been affected by the small sample size. The high scores on the Information Checklist that some participants had on first assessment could not be greatly improved resulting in a ceiling effect in the Information Checklist. The literature indicates however that people show poor memory recall and information processing during periods when they are experiencing anxiety24 which may affect their perception of the information received at a later date even if they were satisfied initially11. The information score of only one participant decreased over the assessment period however, so this does not really seem to have been true for this study. The fact that simple written information was provided to compliment the verbal information provided may have compensated for any memory problems. Timing of the provision of information however must be considered and for those with moderate to severe anxiety intensive information and goal setting should occur within the first weeks after the patient is admitted to rehabilitation.
Of concern are the low scores of those participants who reported normal anxiety levels. This aspect needs further investigation as these family members' may still be in denial or depressed which affects their ability to recognise the need for and to process information that they will need to care for the patient with brain injury. Their lack of anxiety may be related to the lack of insight about the seriousness of the patients' circumstances. This was not related in any way to the length of time since the patients' injury or severity of the brain injury as reflected in the FIM scores or patients' level of function as there was only a low correlation between these factors the level of the participants anxiety.
Based on these results, it is recommended that the rehabilitation team recognise this association and adjust their presentation of information to family members' of clients with brain injury in inpatient rehabilitation facilities, accordingly.
RECOMMENDATIONS
- Information about the clients' care and discharge planning should be provided early in the rehabilitation period but should be reaffirmed and discussed with the family towards the middle and the end of the clients' period of rehabilitation once the initial levels of anxiety have decreased.
- A written action plan should be given to families during any interaction in a simple format. This will assist in reminding the various parties about the information discussed and what plans were drawn up.
- Coping and anxiety reduction measures should also be considered as part of the programme offered to family members in the rehabilitation facility. This can be done in conjunction with the counsellors or social workers who are employed at the rehabilitation facility. If this is not possible, then the team should strongly recommend that the family source support on their own.
- Family members' who have a normal level of anxiety initially should be monitored to determine their insight and other emotional problems. Their ability to understand the relevance of the information discussed with them should be evaluated and other intervention provided if necessary.
Unfortunately, the small sample size with a large drop-out rate of 40% from the 36 participants recruited initially, means these results may have resulted in a type II error and they cannot be generalised to other situations.
An important theme of this study is the need for the rehabilitation team treating the patient with brain injury, to remember that the family members need as much special care during this difficult time as the patient.
REFERENCES
1. Engström A, Söderberg S. The experiences of partners of critically ill persons in an intensive care unit. Intensive and Critical Care Nursing, 2004; 20(5): 299-308. [ Links ]
2. Verhaeghe S, Defloor T, Grypdonck M. Stress and coping among families of patients with traumatic brain injury: a review of the literature. Journal of Clinical Nursing, 2005; 14(9): 1004-12. [ Links ]
3. Van Horn E, Tesh A. The effect of critical care hospitalization on family members: stress and responses. Dimensions of Critical Care Nursing, 2000; 19(4): 40-9. [ Links ]
4. Russell M, Krouse S, Lane A, Leger D, Robson C. Intervention for motor disorders. Traumatic brain injury rehabilitation: Children and adolescents. Boston: Butterworth-Heinemann; 1998. p. 61-84. [ Links ]
5. Dell Orto A, Power P Brain injury and the family: A life and living perspective. New York: CRC Press, 2000. [ Links ]
6. Ryan M. The teachable moment: The Washington Center Internship Program. In: P H, Wutzdirff A, editors. Knowing and doing: Learning through experience. San Francisco: Jossey Bass; 1988. p. 39--47. [ Links ]
7. Hansen M, Fisher J. Patient-centered teaching from theory to practice. American Journal of Nursing, 1998; 98(1): 56-60. [ Links ]
8. Turner B, Fleming J, Ownsworth D, Cornwell P. Perceptions of recovery during the early transition phase from hospital to home following acquired brain injury: A journey of discovery. Neuropsychological Rehabilitation, 2011; 21(1): 64-91. [ Links ]
9. Paterson B, Kieloch B, Gmiterek J. They Never Told Us Anything':Postdischarge Instruction for Families of Persons with Brain Injuries. Rehabilitation Nursing, 2001; 26(2): 48-53. [ Links ]
10. Blinder D, Rotenberg L, Peleg M, Taicher S. Patient compliance to instructions after oral surgery procedures. International Journal of Oral Maxillofacial Surgery, 2001; 30(2): 216-9. [ Links ]
11. Morris K. Psychological distress in carers of head injured individuals: the provision of written information. Brain Injury Journal, 2001; 15(3): 239-54. [ Links ]
12. Ley P Communicating with patients: Improving communication, satisfaction and compliance. New York Croom Helm, 1988. [ Links ]
13. Lefebvre H, Levert M. Breaking the news of a traumatic brain injury and incapacities. Brain Injury Journal, 2006; 20(7): 711-8. [ Links ]
14. Murray G, Butcher I, McHugh G, Lu J, Mushkudiani N, Maas A, et al. Multivariable prognostic analysis in traumatic brain injury: results from the IMPACT study. Journal of Neurotrauma, 2007; 27(2): 329-37. [ Links ]
15. Kalra L, Evans A, Perez I, Melbourn A, Patel A, Knapp M, et al. Training carers of stroke patients: randomised controlled trial. British Medical Journal, 2004; 328(1): 1-5. [ Links ]
16. Smith M, Testani-Dufour L. Who's Teaching Whom? A Study of Family Education in Brain Injury. Rehabilitation Nursing, 2002; 27(6): 209-14. [ Links ]
17. Vanetzian E. Learning readiness for patient teaching in stroke rehabilitation. Journal of Advanced Nursing, 1997; 26(5): 589-94. [ Links ]
18. Zigmond A, Snaith R. The hospital anxiety and depression scale. Acta Psychiatrica Scandinavica, 1983; 67(6): 361-70. [ Links ]
19. Bjelland I DA, Haug TT, Neckelmann D. The validity of the Hospital Anxiety and Depression Scale. An updated literature review. Journal of Psychosomatic Research, 2002; 52(2): 69-77. [ Links ]
20. Epi-Info Software. 2012. [accessed 21 March 2011] http://wwwn.cdc.gov/epiinfo/html/ [ Links ]
21. Degeneffe C. Family caregiving and traumatic brain injury. Health and Social Work, 2001; 26(4): 257 - 68. [ Links ]
22. Bekker K. Family needs following traumatic brain injury. Unpublished Master's thesis. Port Elizabeth: University of Port Elizabeth, 2000. [ Links ]
23. Blake H. Caregiver Stress in traumatic brain injury. International Journal of Therapy and Rehabilitation, 2008; 15(6): 263-71. [ Links ]
24. Thomson A, Cunningham S, Hunt N. A comparison of information retention at an initial orthodontic consultation. European Journal of Orthodontics, 2001; 23(2): 169-78. [ Links ]
 Correspondence:
Correspondence:
Deborah Barrie
debarrie@gmail.com














