Servicios Personalizados
Articulo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en Google
Similares en Google
Compartir
South African Journal of Occupational Therapy
versión On-line ISSN 2310-3833
versión impresa ISSN 0038-2337
S. Afr. j. occup. ther. vol.44 no.1 Pretoria ene. 2014
SECTION 1
Job satisfaction of nursing auxiliaries pre and post training, in a longterm mental health institution for patients with profound intellectual and multiple disabilities
Janine van der Linde
BOT (UFS), MSc OT (Wits); Position: Lecturer E-Learning/Occupational Therapy, School of Therapeutic Sciences, University of the Witwatersrand. Chief Occupational therapist at Witrand Hospital during project
ABSTRACT
Staff working with patients with profound intellectual and multiple disabilities (PIMD) typically experience increased burnout and poor job satisfaction. Occupational therapists became concerned about the morale and work performance of Nursing Auxiliary Stimulation Staff (NASS) who are involved in the execution of the occupational therapy programme, at an institution providing residential care to 650 persons with PIMD in the North West province of South Africa. The aim of the study was to determine the impact of a staff development programme to increase knowledge, skills and attitudes to work with PIMD on their perceived job satisfaction over time. The objectives of the study were firstly to develop an in-service training programme and secondly to describe the pre-and post-intervention (educational input).
METHODOLOGY: A quantitative descriptive design was used to determine job satisfaction through a questionnaire pre and post intervention. The study sample involved all 12 female NASS working at the institution.
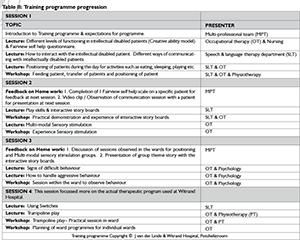
RESULTS: The results indicated a job satisfaction of 56% prior to the training programme, which increased to 78% directly after the training and 90% two months post the training.
CONCLUSION: The outcome of this study indicates that the implementation of a training programme for NASS resulted in improved and sustained job satisfaction.
Keywords: Burnout, Stress, Profound intellectual and multiple disabilities (PIMD), Training programme
INTRODUCTION
Nakken and Vlaskamp1 describe a patient with profound intellectual and multiple disabilities (PIMD) as having a combination of cognitive impairment and neuro-motor dysfunction. The intellectual disability is so severe that it cannot be measured by standardised cognitive tests such as the Wechsler Adult Intelligence Scale (WAIS) and Stanford-Binet2. The severity of the cognitive and physical disability is compounded by the fact that these patients are also more susceptible to medical conditions such as sensory impairments, epilepsy, gastric reflux, chronic respiratory disorders and behavioural difficulties1,3.
Looking after the needs of patients with PIMDS requires the input of a multi-professional team for care as determined by the Mental Healthcare Act 17 of 20024. They are dependent on nursing staff within institutions to address their daily needs, and on therapeutic professionals e.g. Occupational therapists (OT) to provide habilitation programmes. As the burden of care is extremely high it is frequently found that staff working with this population suffer from stress, burnout and low staff/job satisfaction which may influence the quality of care that is provided to these patients56. This was experienced at the study site, a government institution providing residential care to 650 patients with PIMD in the Dr. Kenneth Kaunda region of the North West Province in South Africa. The state funded institution employs a multi-professional team consisting of medical officers, nursing staff, allied healthcare staff such as OTs, Physiotherapists and Speech and language therapists to meet patient needs.
Due to high patient case loads and staff shortages in the OT department nursing auxiliary staff were drafted to assist with the execution of the activity based therapeutic input in the wards (known as stimulation programs) designed by the OT department7.
They work under the supervision of a trained psychiatric nurse and an OT and are known within the hospital as nursing auxiliary stimulation staff.
Service delivery is focussed on the provision of high levels of care with regular staff input; however a decline was noticed over time in the effectiveness of the therapeutic programmes. In the investigation to determine the ineffectiveness of the programme it was found that job satisfaction played a role in the execution of the programme. The low job satisfaction of nursing auxiliary stimulation staff was suspected to be due to high levels of stress and burnout.
Reportedly the level of functioning of the patients played a role in the increased levels of stress experienced by the NASS. They indicated that it was too hard to engage in activities with PIMD as they needed intensive input and did not react as fast or in the same way as less disabled and higher functioning patients.
This article describes the results of an intervention study that investigated changes in staff job satisfaction following participation in a training programme aimed at increasing their knowledge and skills base for working with PIMD. The study formed part of a larger project that looked at the implementation of an occupational therapy programme that is more appropriate to the decreased level of functioning of the patients. The objectives of study were to develop a training programme to increase the knowledge and skills of the NASS and to determine how this intervention programme would influence their job satisfaction.
LITERATURE REVIEW
Burnout and stress
The Oxford Concise Medical Dictionary8:6:30 defines stress as "any factor that threatens the health of the body or has an adverse effect on its functioning". Sources of stress are factors such as feeling out of control, overwhelmed by the high work load, inadequate rewards, unreasonable expectations, conflicting viewpoints and job security9. Bigby10 and Mills11 further identified organisational aspects such as poor staff to patient ratio as well as personal factors such as the age, qualification level of staff, years of experience working with this population, skill utilisation and even factors such as challenging behaviours of patients. Chung12 added other factors such as lack of adequate training and supervision, mismatch of skills and knowledge, and lack of support at work from co-workers and management.
Looking closer at personal characteristics and attitudes it was found that attributes such as age, gender, staff qualification and educational level played a role alongside organisational factors. A study by Kozak et al6 found that female staff have a higher level of stress, but there is no consensus about this and a study by Kowalski et al13 found that males are four times more likely to experience emotional exhaustion than females11,13.
Maslach and Goldberg14:64 define burnout as: "a type of prolonged response to chronic emotional and interpersonal stressors on the job. It is an individual stress experience embedded in a context of complex social relationships, and it involves the person's conception of both self and others." Emotional exhaustion results in feelings of being emotionally overextended and lack of energy to interact with other people, whereas Depersonalisation results in a detachment from other people and can lead to callous behaviour14. Experiencing reduced accomplishments result in feelings of poor achievement, poor job productivity and impression of not coping with job demands. Staff experiencing burnout is found to be less productive, which in turn will influence the nursing quality of care, and will result in less interaction with patients. It can further cause physical illness that result in frequent absenteeism. These behaviours can then result in an increased workload for other staff6,11.
Burnout and stress are prevalent in staff caring for patients with intellectual disabilities, although stress is commonly found in all jobs, it is suspected to be higher in jobs that require more emotional input, such as in caring for clients with intellectual disabilities6,9,11,13,15.
It is understandable for staff to experience burnout and stress as patients with PIMD are dependent on nursing staff for their everyday needs and care. The burden of care placed on nurses is intensified by the health needs of these patients who frequently suffer from epilepsy, constipation, contractures of limbs that require specific lifting and positioning, chronic respiratory disorders with resultant pneumonia, and difficulty with feeding requiring the use of feeding tubes16. Nakken et.al.1 and Zijlstra et.al.3 discussed the role of the PIMD's medical condition in their participation in the activities and their consequent level of functioning1,3. They state that care staff felt insecure regarding the execution of tasks when the patient becomes physically ill, and that this results in inactivity and consequently poor levels of adaptive response and levels of alertness.
The level of functioning of a patient also plays a role in causing stress and burnout. Bigby et al10 found that, although staff members had a positive attitude toward low functioning patients, they did not find it possible to include them in activities. Vlaskamp et al 17 did a study to determine whether staff members know what the clients' abilities are and how staff apply their knowledge in choosing the correct activities. The results indicated that they did not have adequate knowledge regarding appropriate activities, and that their vocational training was not directed to this type of knowledge.
Lambrechts et al18 and Zijlmans et al19 indicated that staff reacted emotionally to challenging behaviour of patients. Unpredictability of behaviour was found to be especially stressful. Mills and Rose11 found that this became wearisome for staff, resulting in staff feeling inadequate to manage the behaviour.
Burnout in staff working with patients with PIMD comes at a high cost, not only to the institution, but also to the individuals. Studies conducted by Lin et al15 Kowalski et al13, Mills and Rose11 and Kozak et al6 confirmed this and found that burnout resulted in high absenteeism, poor job satisfaction, reduced commitment from staff, and loss through resignation. This in turn resulted in a high turnover of staff, and/or staff shortages, as well as a high economic cost because of the continuing instruction of new staff.
Training
Addressing burnout and the resultant low job satisfaction in staff working with patients with PIMD is important to ensure that they receive a high quality of care and interaction. When burnout is experienced work has no meaning and could cause negativity. This has an influence on relationships with co-workers and patients (reduced interactions) and results in poor job satisfaction, which in turn has an influence on the quality of care provided to patients20.
Recommendations to address these issues indicate that intervention should include balancing the demands of the job with skills and ability, increasing workers resources such as more equipment and improving staff coping skills6. Increasing staff ratios to assist with the demands of the job would usually be the first option to improve this situation, but Felce et al21 proposed that increases in staff is not as effective as would be expected. Bigby et al10 confirmed this and also found that improving the ratio of staff to patients did not have much of a positive effect and sometimes even resulted in less staff interaction with patients.
Innstrand et al20 suggested that in order to address job related stress, the area of greatest concern in causing this stress should be addressed first. However this is different from other studies which found that training of staff in the handling of clients with intellectual disability and the execution of programmes played a significant role in the improvement of quality of life in these patients, and also in the quality of life and job satisfaction of the caregivers9-11,15.
Investigations have found that certain types of training are more effective than others22,23. The literature describes a combination of on the job and theoretical training to be the most effective method of instruction. Different educational techniques e.g. providing literature, role playing, video demonstration, prompting and verbal feedback were found to assist in the teaching of staff22, with verbal feedback the most effective in the training programme. Cooper and Browder24 described the use of a multi-component staff training programme that included these components.
A review by Van Oorsouw et al22 indicated that it is important to identify the goal for staff training, the format of the training programme and the techniques that are used to give the information to staff members. They also suggested that the goal of the training program needed to specify if the focus of the training would be on changing the skills of staff, behaviours of the clients, or on providing practical skills on the implementation of a care plan. In addition they recommended that the following factors be taken into account when a programme is developed:
- The level of functioning of patients
- The issues that influence staff motivation and the provision of quality care for patients.
- The overall goal of the treatment programme, which ideally should also address the nursing staff's knowledge and skills in order to improve their job satisfaction.
- The format and teaching techniques that were going to be used as the literature indicates that a multi-component training programme works best22.
METHODOLOGY
Study design
A quantitative descriptive design was used to determine the job satisfaction of staff prior to the training programme, again a month later and then taking an annual average over two years. The job satisfaction questionnaire consisted of the in house job satisfaction tool used by the hospital management for quality control purposes. It used a 3 point Likert scale that asked the staff to rate their satisfaction with their job as 1 - poor, 2 - fair, and 3 - good. The limitation of the tool is that it is not a standardised assessment with proven validity and reliability and may result in some bias. All information was then included in the design and implementation of the training programme.
A semi-structured questionnaire was used prior to the start of the training programme to determine how staff experience their job by asking them to answer the following questions in writing:
1. What do they dislike in their work?
2. What would they like to change in their work?
3. Any other issues that have an impact on their work?
4. What do they enjoy about their work?
The results of this questionnaire were analysed by determining common factors and then determining the percentage off staff experiencing the same difficulties.
The outcome of the training programme was measured in terms of improvement of the job satisfaction of the nursing auxiliary stimulation staff.
Population and Sample
The NASS population consisted of a group of 12 female NASS who were not only involved in the care of the patients in the ward, but who were also involved in executing the occupational therapy programme that was run in each ward. Due to the small sample size these participants were not randomly selected but the whole group was included in the study.
Ethics
The training programme within the hospital was approved by the Hospital and Nursing management and participants received a certificate on completion of the programme.
Written approval was given for the study by the Hospital Ethical and Patient Safety Group and the North West Department of Health. Ethical clearance was also received from the Human Research Ethics Committee from the University of the Witwatersrand.
Research procedure
In March 2011 NASS members were asked to complete a job satisfaction questionnaire and semi structured questionnaire, prior to the development of the training programme.
The development of the nursing auxiliary training program
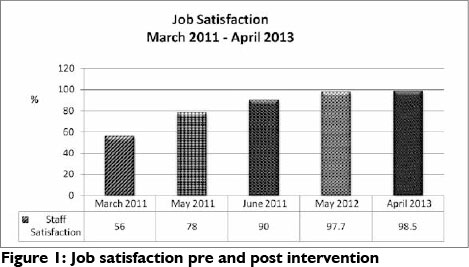
The training programme focussed on providing skills and knowledge regarding the execution of the therapeutic programme that the NASS were involved in. The programme was developed with input from an occupational therapist, speech and language therapist, physiotherapist and psychologist. Incorporating the critical components of each profession ensured a holistic design approach.
In order to determine the topics for training, the level of functioning of the patients was taken into account. A range of educational methods were used including videos, practical workshops, role play, providing a manual and practice evaluation exercises.
The following were included in the design and execution of the programme:
1. A manual was developed to provide reading material and information to be used to refresh memory regarding training.
The content was in simple language with diagrams, pictures and exercises to make it accessible to all staff irrespective of education. Within the manual the goal of the training was made very clear i.e. to improve the nursing auxiliaries' skills and NOT the patients' skills.
2. Learning objectives clarify what level of knowledge was expected.
3. Practical sessions included making their own micro switch toy (the micro switch is connected to a toy and with a minimum of movement results in the toy making a noise or lighting up), presenting an interactive story board story and how to communicate with patients and how to provide choices to them.
4. Learner assessments were included in the training to ensure that skills were transferable to the actual work environment. Each topic required an activity to be done within the class situation, as well as an activity to practise during the week and then to give feedback following week during class. This assisted the therapists in correcting any incorrect behaviour.
5. Practical homework was given as part of the intervention and evaluation processes. Feedback of the home work was provided at the next session to ensure carryover and reinforcement of information.
Execution of training programme
The training programme began at the beginning of April 2011 and ran until May 2011. The programme was first implemented with the 12 nursing auxiliary stimulation staff involved in the care and therapeutic programmes. On completion of the training of the NASS, the same programme was repeated with the Nursing unit managers to ensure that they were aware of the expectations for the nursing auxiliaries. Training was done once a week on Thursday from 8:00 to 16:00 for 4 weeks.
Analysis of results
Descriptive statistics e.g. means, modes, and percentages were used to look at the demographic information of the NASS, the difficulties they experienced and job satisfaction.
RESULTS
Nursing auxiliary demographic information
Table III shows the background information for the NASS that participated in the study. All were females and their ages ranged from 35 - 46 years. They had been working in the hospital for an average of 18 years and 6 months.
Job satisfaction
The NASS were asked to complete a job satisfaction questionnaire as well as a questionnaire that delved into more detail around the things they disliked or would like to change in their work, as well as the aspects of their work that they enjoyed most (see Table IV).
Table IV indicates that 40% of the NASS disliked doing tasks other than those allocated to them, and 40% felt that they did not have support from their managers. More than half of the group (56%) indicated that they would appreciate better team work. Feeling depressed or experiencing burnout was reported by 44% of the group as a factor impacting on their work and 67% of the group felt that the shortage of staff influenced their work. The low functioning of patients (20%), not enough space for activities (33%) and the need for more finances/equipment (78%) also played a role in job dissatisfaction. Only 56 % of the NASS were satisfied with their job and the tasks that they did. This increased dramatically at the end of May and June 2011 (78% and 90% respectively) following the training course.
The outcome of the training programme was positive as reported in the job satisfaction questionnaire as well as in verbal communication with the staff members. Figure I demonstrates a satisfactory improvement in the number of participants being satisfied with their job from March 2011 until June 2011 and that there was no regression from that time until April 2013. Thus showing the apparent success of the training programme.
DISCUSSION
Demographic variables such as age and length of service are described in the literature as playing a role in burnout6,25.
Younger staff members were found to be more susceptible to burnout whereas the older nursing staff experienced less burnout and low job satisfaction6,26-28. Ahola et al29 further explained that increased levels of burnout are found in younger employees involved in caring jobs, but that this is different in the general working environment in which older people experience higher levels of burnout. Kozak et al6 however found that burnout is seen in older employees ranging from 30 to 39 years. The present study found an age range from 36 - 46 years with all participants being female.
Humpel and Caputi30 further linked age to levels of work experience and indicated that having less experience is linked with a greater risk of experiencing psychological distress with resultant burnout. In contrast to the literature that indicated that burnout is more prevalent in staff being employed for shorter periods and with less experience6,30, it was found that the study population who had, on average been employed for 18 years, still experienced low levels of job satisfaction.
Innstrandet al20 proposed a positive approach for addressing stress by looking at the greatest areas of concern first. The training programme, therefore, focussed on addressing the issues as commented on by the NASS.
Issues such as poor role clarification, performing other jobs, staff shortages and the levels of functioning of patients, were identified by this population and were very much in line with factors indicated in the literature6,9,13. Lin et al15 also described similar indicators that have an influence on job satisfaction such as poor role definition, conflict between co-workers and poor support.
In the feedback from the NASS population they indicated that they disliked having to do other tasks allocated to them that they would appreciate better team work and that staff shortages played a role in their job satisfaction. The NASS group is required to execute the therapy programme in the wards, but is frequently asked to assist with other tasks in the wards due to the staff shortage within the institution. This caused frequent difficulties with role clarification and a feeling of poor support from the Nursing unit managers.
The training programme focussed mainly on skills development, mastery of skills and work design, but indirectly it addressed the other issues such as clarifying the role of the NASS and working with difficult low functioning patients. By including the Nursing unit managers in the same training an effort was made to clarify the role of the NASS within the institution and to encourage team work.
Working with low functioning patients, and patients with challenging behaviours and the need for more equipment and finances were also identified within the literature to play a role in job satisfaction and was addressed in the training programme11,31.
By using a multi-component training programme as suggested by Cooper and Browder24, Van Oorsouw et al22 and van Vonderen et al23 specific issues such as "Different levels of functioning in intellectual disabled patients (Creative ability model)" and "How to handle aggressive behaviour" were addressed. The NASS was given the opportunity to improve their competence and handling skills through practice and feedback from their peers and presenters.
Finally a set therapeutic programme was implemented within the wards to suit the developmental needs of all PIMDs within the institution. Education on the execution of this programme was included during the training programme to provide staff with the necessary skills to feel competent in their work, which will increase job satisfaction.
Limitations: The sample population of nursing auxiliaries was too small and there was no control group to use for comparison of results. The effect of the training programme on the patient population was not measured and there are no data to show that it improved the quality of care. However observations during the course of training and the feedback provided by all participants showed that this initiative was successful.
CONCLUSION
The outcome of this study indicated that the implementation of a training programme for nursing auxiliaries caring for patients with PIMD resulted in improved and sustained job satisfaction. This study should be repeated on a larger population to determine if the findings are valid for a larger sample.
REFERENCES
1. Nakken H, Vlaskamp C. A Need for a Taxonomy for Profound Intellectual and Multiple Disabilities. Journal of Policy and Practice in Intellectual Disabilities, 2007; 4(2): 83-7. [ Links ]
2. Silverman W, Miezejeski C, Ryan R Zigman W, Krinsky-McHale S, Urv T. Stanford-Binet and WAIS IQ differences and their implications for adults with intellectual disability (aka mental retardation). Intelligence, 2010; 38(2): 242-8. [ Links ]
3. Zijlstra HP, Vlaskamp C. The Impact of Medical Conditions on the Support of Children with Profound Intellectual and Multiple Disabilities. Journal of Applied Research in Intellectual Disabilities, 2005; 18(2): 151-61. [ Links ]
4. Mental Healthcare Act 17 of 2002, Government of South Africa (2002). [ Links ]
5. Devereux J, Hastings R Noone S. Staff Stress and Burnout in Intellectual Disability Services: Work Stress Theory and its Application. Journal of Applied Research in Intellectual Disabilities, 2009; 22(6): 561-73. [ Links ]
6. Kozak A, Kersten M, Schillmöller Z, Nienhaus A. Psychosocial work-related predictors and consequences of personal burnout among staff working with people with intellectual disabilities. Research in Developmental Disabilities, 2013; 34(1): 102-15. [ Links ]
7. Nursing Act No. 33 of 2005, Nursing Council of South Africa.(2005). [ Links ]
8. Oxford Concise Medical Dictionary. Fifth ed. Oxford: Oxford University Press; 1998. [ Links ]
9. Innstrand ST, Espnes GA, Mykletun R. Burnout among people working with intellectually disabled persons: a theory update and an example. Scandinavian Journal of Caring Sciences, 2002; 16(3): 272-9. [ Links ]
10. Bigby C, Clement T, Mansell J, Beadle-Brown J. 'It's pretty hard with our ones, they can't talk, the more able bodied can participate': staff attitudes about the applicability of disability policies to people with severe and profound intellectual disabilities. Journal of Intellectual Disability Research, 2009; 53(4): 363-76. [ Links ]
11. Mills S, Rose J. The relationship between challenging behaviour, burnout and cognitive variables in staff working with people who have intellectual disabilities. Journal of Intellectual Disability Research, 2011; 55(9): 844-57. [ Links ]
12. Chung MC, Corbett J. The burnout of nursing staff working with challenging behaviour clients in hospital-based bungalows and a community unit. International Journal of Nursing Studies, 1998; 35(1-2): 56-64. [ Links ]
13. Kowalski C, Driller E, Ernstmann N, Alich S, Karbach U, Ommen O, et al. Associations between emotional exhaustion, social capital, workload, and latitude in decision-making among professionals working with people with disabilities. Res Dev Disabil, 2010; 31(2): 470-9. Epub 2009/12/17. [ Links ]
14. Maslach C, Goldberg J. Prevention of burnout: New perspectives. Applied and Preventive Psychology, 1998; 7(1): 63-74. [ Links ]
15. Lin J-D, Lee T-N, Yen C-F Loh C-H, Hsu S-W, Wu J-L, et al. Job strain and determinants in staff working in institutions for people with intellectual disabilities in Taiwan: A test of the Job Demand-Control-Support model. Research in Developmental Disabilities, 2009; 30(l): 146-57. [ Links ]
16. Tadema AC, Vlaskamp C. The time and effort in taking care for children with profound intellectual and multiple disabilities: a study on care load and support. British Journal of Learning Disabilities, 2010; 38(1): 41-8. [ Links ]
17. Vlaskamp C, Hiemstra SJ, Wiersma LA. Becoming Aware of What You Know or Need to Know: Gathering Client and Context Characteristics in Day Services for Persons With Profound Intellectual and Multiple Disabilities. Journal of Policy and Practice in Intellectual Disabilities, 2007; 4(2): 97-103. [ Links ]
18. Lambrechts G, Kuppens S, Maes B. Staff variables associated with the challenging behaviour of clients with severe or profound intellectual disabilities. Journal of Intellectual Disability Research, 2009; 53(7): 620-32. [ Links ]
19. Zijlmans LJM, Embregts PJCM, Bosman AMT, Willems APAM. The relationship among attributions, emotions, and interpersonal styles of staff working with clients with intellectual disabilities and challenging behavior. Research in Developmental Disabilities, 2012; 33(5): 1484-94. [ Links ]
20. Innstrand ST, Espnes GA, Mykletun R. Job Stress, Burnout and Job Satisfaction: An Intervention Study for Staff Working with People with Intellectual Disabilities. Journal of Applied Research in Intellectual Disabilities, 2004; 17(2): 119-26. [ Links ]
21. Felce D, Repp AC, Thomas M, Ager A, Blunden R. The relationship of staff: Client ratios, interactions, and residential placement. Research in Developmental Disabilities, 1991; 12(3): 315-31. [ Links ]
22. van Oorsouw WMWJ, Embregts PJCM, Bosman AMT, Jahoda A. Training staff serving clients with intellectual disabilities: A meta-analysis of aspects determining effectiveness. Research in Developmental Disabilities, 2009; 30(3): 503-11. [ Links ]
23. van Vonderen A, Duker P Didden R. Instruction and video feedback to improve staff's trainer behaviour and response prompting during one-to-one training with young children with severe intellectual disability. Research in Developmental Disabilities, 2010; 31(6): 1481-90. [ Links ]
24. Cooper KJ, Browder DM. Preparing staff to enhance active participation of adults with severe disabilities by offering choice and prompting performance during a community purchasing activity. Research in Developmental Disabilities, 2001; 22(1): 1-20. [ Links ]
25. Maslach C, Schaufeli WB, Leiter MP Job burnout. Annu Rev Psychol, 2001; 52: 397-422. Epub 2001/01/10. [ Links ]
26. Soares JJF Grossi G, Sundin Ö. Burnout among women: associations with demographic/socio-economic, work, life-style and health factors. Archives of Women's Mental Health, 2007; 10(2): 61-71. [ Links ]
27. Hayes LJ, O'Brien-Pallas L, Duffield C, Shamian J, Buchan J, Hughes F et al. Nurse turnover: A literature review. International Journal of Nursing Studies, 2006; 43(2): 237-63. [ Links ]
28. Maslach C, Leiter MP Burnout. In: Editor-in-Chief: George FinkAs-sociate Editors:Bruce M, Kloet ERd, Robert R, George C, Andrew S, Noel R, et al., editors. Encyclopedia of Stress (Second Edition). New York: Academic Press; 2007. p. 368-71. [ Links ]
29. Ahola K, Honkonen T, Virtanen M, Aromaa A, Lonnqvist J. Burnout in relation to age in the adult working population. J Occup Health, 2008; 50(4): 362-5. Epub 2008/06/10. [ Links ]
30. Humpel N, Caputi P Exploring the relationship between work stress, years of experience and emotional competency using a sample of Australian mental health nurses. Journal of Psychiatric & Mental Health Nursing, 2001; 8(5): 399-403. [ Links ]
31. Collins K, Jones ML, McDonnell A, Read S, Jones R, Cameron A. Do new roles contribute to job satisfaction and retention of staff in nursing and professions allied to medicine? Journal of Nursing Management, 2000; 8(1): 3-12. [ Links ]
 Correspondence:
Correspondence:
Janine van der Linde
Janine.vanderlinde@wits.ac.za