Servicios Personalizados
Articulo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en Google
Similares en Google
Compartir
South African Journal of Occupational Therapy
versión On-line ISSN 2310-3833
versión impresa ISSN 0038-2337
S. Afr. j. occup. ther. vol.44 no.1 Pretoria ene. 2014
SECTION 1
Occupational therapy manager's role in and perceptions of clinical education
Patricia De WittI; Alan RothbergII; Judith BruceIII
IDip OT (Pret), MSC OT (Wits); Adjunct Professor and Head, Department of Occupational Therapy, School of Therapeutic Sciences, University of the Witwatersrand
IIMBBCh (Wits), FC Paed (Wits), PhD (Wits); School of Therapeutic Sciences, Faculty of Health Sciences, University of the Witwatersrand
IIIB Cur (UWC), MSc Nursing (Wits), PhD (Wits); School of Therapeutic Sciences, Faculty of Health Science, University of the Witwatersrand
ABSTRACT
This study explored the role and perceptions of clinical education by the occupational therapy (OT) managers of clinical training sites.
A descriptive, quantitative survey design was used and a self-administered questionnaire was developed. The questionnaire was developed from the literature and comprised of four sections: nature of the site; clinical training at that site; management of clinical education and perceptions of benefits and challenges. The content validity of the questionnaire was established.
The questionnaires were sent to the heads of OT departments (n=22) that are utilised for the clinical education of occupational therapy students. Fourteen questionnaires were returned (73.7%).
Only 45.5% (n=39) of the occupational therapists employed in these sites were involved in clinical education. The most common criteria for being involved were clinical experience and where OTs qualified. Most OT managers played a supportive (36%) or logistical role (43%) in clinical education; 22% were actively involved while 28% had no involvement. The two most frequent benefits of providing clinical education were perceived to be assistance in managing the clinical load and keeping up to date, while time and staff issues were perceived to be the challenges.
The importance of involvement of all tiers of management in clinical education is not widely appreciated.
Key words: Occupational therapy students, Clinical education, Occupational therapy manager
INTRODUCTION
All occupational therapy (OT) students are required to complete a minimum of 1000 hours of clinical practice in clinical settings, transitioning their classroom education into clinical competencies by participating actively in the OT process of clients with diverse occupational dysfunctions1,2.
In the BSc OT degree offered by the University of the Witwatersrand (Wits) these 1000 hours are distributed throughout the four years of study. Blocks of clinical education are linked to clinical education outcomes associated with specific problems through a hybrid Problem Based Learning (PBL) curriculum, with most clinical hours being completed in the final year; each final year student completes seven clinical education blocks that vary in duration and represent the major fields of practice and levels of health care. The blocks collectively contribute to the development of the clinical competencies described in the exit level outcomes of the undergraduate degree3.
In the final year of study most of the clinical education is the responsibility of the occupational therapists who are employed at the 22 clinical education sites on the academic department's clinical training platform. In addition to managing their clinical work load these occupational therapists are responsible for providing students with teaching and learning activities appropriate to the clinical outcomes that are prescribed for each block. There is no formal training for clinical occupational therapists who undertake the clinical education of OT students. The academic department has a programme of activities to assist these clinical educators with this task, but this programme has tended to be more procedural (what objectives need to be met in the block) rather than equipping clinical educators with teaching and evaluation skills. There are no financial rewards for clinical staff who become clinical educators; however continuing education units (CEUs) are awarded according to the Regulations of the Health Professions Council of South Africa (HPCSA)4.
As in many other parts of the world, availability of appropriate clinical education sites with sufficient clinical staff willing to become clinical educators has become a critical problem5-8. This problem has been exacerbated by the University's pressure to increase student numbers, and the clinical sites' reported work-related pressures that are linked to inadequate staffing, high staff turnover, inadequate resources and high clinical workloads.
A key role player in this scenario is the OT clinical manager who is responsible for the annual decision of the clinical department to become a new or repeat clinical education site each year. These managers are also responsible to the clinical site's top management for any impact clinical education of students may have on overall service delivery9.
The purpose of this study was to explore the role and perceptions of OT managers at the various clinical education sites on the Wits clinical teaching platform, as well as their level of involvement with the clinical education process, in order to answer the research question: What do clinical managers think about and contribute to clinical education at the training sites of the Wits OT teaching platform?. This study is a component of a wider study into "Supervision of the clinical work of BSc OT students by clinical occupational therapists" which examined the perception of all role players in the clinical education process. This article only reports on the perspective of the OT manager.
The objectives of the study component reported here were to:
- Explore the involvement of OT managers in the clinical education process,
- Examine how clinical education is managed at the different sites,
- Explore the OT managers' perceptions of the benefits and challenges of clinical education.
LITERATURE REVIEW
There are many layers of management, both within and outside a clinical education site that influence the success of OT clinical education at that site. Occupational therapy clinical department heads are considered to be middle managers, answerable to the organisation's senior management and also to staff within the OT team. The OT managers are responsible for service delivery as well as staff development, which includes developing a culture of education to enable both the continuing professional education (CPD) of staff as well as clinical education of students10.- Support from the facility management enables the OT managers to access and develop the four core constituents essential for a clinical education site that have been described by Alsop and Ryan11. These include:
- access to learning opportunities;
- human resources (such as a clinical educator, access to members of the multidisciplinary team);
- non-human resources (such as work space, information technology (IT) and academic resources) and
- the organisation of the placement (including organisational structures, service and educational philosophy, defined standards of service and quality assurance measures, and collaborative relationships with the academic staff to facilitate a positive student-friendly clinical education experience)11.
Clinical education sites have a variety of structures (subject to their staff complement), with clinical education management roles and functions being either delegated to a single therapist or devolved to other staff that may or may not have a senior position and relevant experience. The key management tasks associated with being a clinical education manager are: deciding on the model of clinical education to be used, developing a positive learning environment; preparing occupational therapy staff for their involvement in clinical education, and defining their responsibilities as well as educational outcomes for the students, as set out by the academic department, that need to be facilitated and met; ensuring there are sufficient resources to support the educational process; orientating students to the placement, the placement policies and service outcomes; overseeing students' performance, monitoring progress and dealing with critical incidents; and reflecting on and reviewing the success of the placement for clinical education12,13.
In the past decade a number of different models of clinical education have been described to manage the increasing number of students14. The apprentice model is the most common and is the model in which one student is assigned to a single occupational therapist6. The collaborative model is where a single clinician is responsible for the clinical education of a number of students15,16. Then there are the single student multiple clinical educator model and multiple student multiple clinical educator models17,18.
Irrespective of the model of clinical education used, the day-today clinical education processes are usually assigned to the clinical occupational therapists who deliver OT services13. Thus a clinical educator is the qualified occupational therapist tasked with providing the daily clinical education opportunities, teaching, guiding and evaluating the clinical learning of an OT student in a client care context. This role is critical for a student to enable them to transition their theoretical knowledge into practice19, and the quality of this clinical learning experience has important implications for the future of the profession20,21. The role of the clinical educator has changed over time as clinical education has transformed from learning from the 'expert', as in the apprenticeship model of learning19, to experiential hands-on learning as an extension of academic activities including reflection, critical thinking and conceptual learning in the context of practice22.
The American Occupational Therapy Association (AOTA) has defined competencies for clinical educators in five standards for continued professional competence: knowledge, clinical reasoning, interpersonal skills, performance skills and ethical reasoning, all of which cover professional practice, education, supervision and administrative competencies23.
In South Africa there is no statutory requirement other than the six months of clinical experience recommended by the HPCSA2. This is less than the one year recommended by the World Federation of Occupational Therapy1. The belief that qualified occupational therapists are automatically able to be successful clinical educators has its roots in both the Hippocratic Oath and the apprenticeship model19. This model proposes that more senior members of the profession should "watch over and guide" students and act as "gate keepers" of the profession19. This belief is now being challenged as it is increasingly recognised that the set of competencies and teaching strategies needed to be a clinical educator are different from those needed to be a competent therapist24.
The AOTA has recognised that one of the key characteristics of successful OT clinical educators is for them to value education highly and for lifelong learning to be a professional goal23. This characteristic is reported to be essential for the provision of learning opportunities for students in order to transition from the classroom to a practice that is in keeping with current theory and evidence23.
RESEARCH METHOD
A self-administered survey design was used to describe how OT managers perceive the clinical education that occurs in their departments. All OT clinical managers were asked to respond in their own time to the same structured questions. The advantages of using a self-administered survey was that respondents could complete the survey in their own time, respondents' anonymity could be preserved, and researcher bias was eliminated25.
The survey was specifically designed for this research with questions that were based on the literature, ensuring that each variable was clearly defined26. The survey comprised four sections with a combination of closed- and open-ended questions: Section 1 asked questions about the nature of the clinical education site; Section 2 included questions about the clinical training of students within the site; Section 3 asked questions about the management of clinical education within the site; and Section 4 included open questions to examine the OT manager's perception of the challenges and benefits of the clinical sites' involvement in clinical education.
The first draft of the survey was sent to an external clinical education expert and l2 academic staff for critique and feedback to establish the face and content validity25. Their comments were noted. Corrections were made as suggested and the second draft was then piloted.
Two OT managers on the OT clinical education platform of another university were asked to complete the survey and give feedback on: the time the survey took to complete; the relevance of the questions considering the purpose of the survey; the ease of answering; and any ambiguous or unclear questions26,27. Their comments and corrections were incorporated into the final survey.
A letter of invitation, an information sheet (including an informed consent form) and a copy of the finalised survey (both as a hard copy and an electronic copy on a compact disc), were mailed or hand-delivered to the departmental heads of all clinical training sites. The completed questionnaires were returned to the departmental secretary so that there was no contact between the researcher and the participants, and anonymity was thus maintained26. It was anticipated that since this was a specifically targeted survey a return rate of 75% would be acceptable25.
The participant responses in tick boxes were transferred onto an EXCEL R spread sheet and were analysed using descriptive statistics including means, medians, ranges and frequency. The responses to the open-ended questions were recorded in tables, one for each open-ended question and the contents analysed. Similar responses were grouped together and the frequencies recorded.
RESULTS
The survey was circulated to the 22 clinical education sites on the Wits clinical education platform. Fourteen surveys were returned. One response was returned for three urban public health sites as they all fall under the same department head/manager. Thus the return rate was effectively l4 of 20 (73.7%) which is just below the return rate that was targeted.
Nature of clinical education sites
Each student has 8 clinical blocks in the final year that cover the main fields of practice which is consistent with training a generalist clinician: 2 blocks in the physical field; 2 in mental health facilities (one acute and the other chronic); 2 paediatric blocks (one block focussed on children with cerebral palsy in a Learners With Special Needs (LSEN) School and the other on children with learning disabilities in the departmental clinic) and 2 blocks in Public health (one in an urban and the other in a rural site). Clinical education takes place mostly in OT departments which deliver services within the hospital or to community structures from the hospital base. Other clinical education sites (4.9%) included LSEN schools, private practices, a non-profit organisation (NPO) and primary care clinics. Of the responding sites nine belong to provincial departments of health while the others were private or an NPO. Figure 1 reflects the nature of the services at the different sites. There were no surveys returned from the LSEN schools.
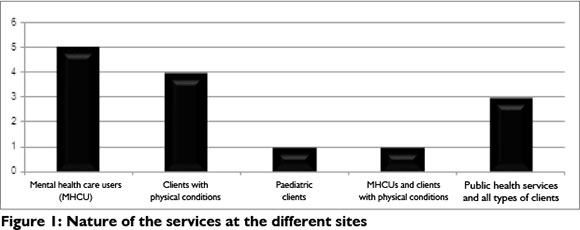
Clinical education of students within each site
Occupational therapy managers were asked to report the number of students that had completed clinical blocks in the previous year.
Three OT managers failed to complete this section of the survey but the remaining 11 sites reported that 118 students had completed clinical blocks in their sites with the total number of students varying from two to 35, with a median of 32 and a mean of 10.7 students per site per year.
Twelve sites reported a long association with the Wits academic department while two reported being involved in clinical education for less than two years.
Management of clinical training within the site
Eleven OT managers (78.6%) reported that the clinical education of OT students was the responsibility of the OT department alone, with only 3 sites reporting that the site senior management (management structures above the OT service manager) was involved.
Only one site had a formal education policy pertaining to the clinical education of OT students.
There were 86 OTs employed in the 14 sites at the time of the study. The number of staff numbers varied from 1 to 21 OTs, and the median being 3. Only 39 of the 86 OTs were clinical educators, in addition to their assigned clinical responsibilities, which represents 45.3% of the OT staff working in these sites. Four sites reported that all their OTs were involved in the clinical education of the OT students, while in other sites the number varied from 1 to 15.
Occupational therapy managers reported that they used several criteria to assign the staff the clinical educator role. Competence, and where staff trained were the most frequently criteria used. This question was included to confirm a finding from an earlier phase of the study that only some staff were required to be clinical educators in spite of reports from the Deputy Director Professional Services: Allied Health within Gauteng Health that clinical education was included in the job description of all OTs in the service. Figure 2 shows the frequency of criteria used.
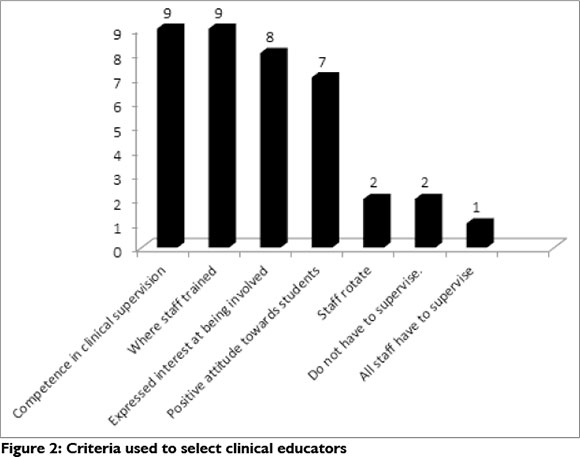
As hospitals tend to limit the number of students that they will accommodate per block, managers were asked to list the factors that they considered when making this decision. The most frequently reported factor in determining the number of students a specific site could accommodate in a particular block was the reluctance of clinical educators to supervise more than one or two students. Other factors mentioned were the numbers requested and negotiated with the university, bed occupancy, availability of appropriate clients and accommodation for students.
The analysis of the open-ended question around the management of clinical education within each site revealed a dependence on departmental circumstances, but no common trends could be identified.
Figure 3 illustrates the role that OT managers perceive they play within the clinical education process, with the logistical role being the most common (43%). This included activities such as organising accommodation, transport, home and work visits, defining policies and procedures for students, ensuring students have the resources for their clinical work to meet their educational objectives, liaising with the university staff and attending university meetings.
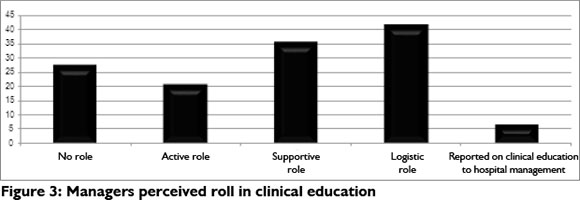
OT managers' perceptions of benefits and challenges of clinical education
Occupational therapy managers were asked to list what they considered to be the five most important benefits to their department of being involved with clinical education of OT students. Not all OT managers listed 5 benefits and the median was 1. The responses were grouped into 2 categories: what the clinical department has to gain and what the students have to gain. These are listed in Table I. The most frequent benefits in these categories were: assistance with client care (14) and input into the development of the student and profession respectively (11).
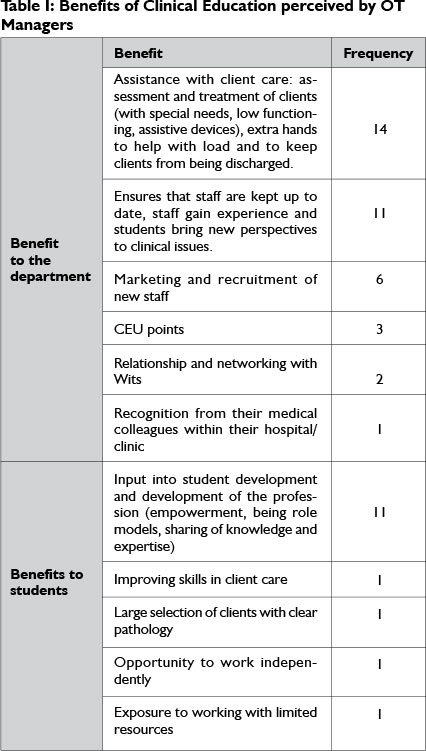
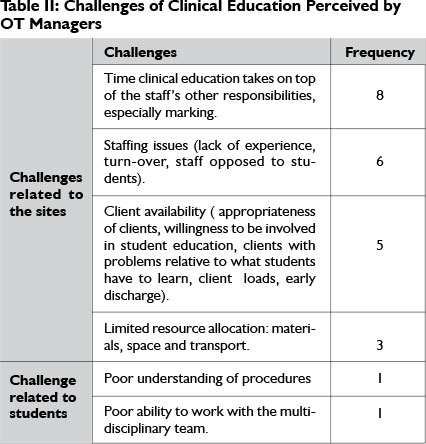
One OT manager reported that there were no challenges, while all the others listed fewer than 5 challenges (median=1). The challenges listed were again grouped into 2 categories on the basis of the comments: challenges related to the site and those related to the students (see Table II). The most frequently reported challenge was the time clinical education takes in addition to clinical responsibilities. The next was staffing, which included lack of experienced staff; staff turnover and staff opposed to clinical education. Other challenges listed were client availability and lack of departmental resources (materials, space and transport). There were only 2 challenges relating to students and they were each listed once: students' inability to work within the multi-disciplinary team and their poor understanding of departmental processes.
DISCUSSION
Although the return rate of questionnaires was slightly lower than was anticipated, the responses were likely representative of most health delivery sites in which the students undertake their clinical education. The fact that no sites belonging to the Gauteng department of education responded was a limitation to the study and may have influenced the results as these sites tend to have very stable and experienced staff. The most probable explanation for their not returning the surveys was that the due date was during the school holidays. These results also cannot be generalised to the whole country as only a small number of clinical educators on the Wits clinical education platform was sampled.
In 2010 there were 39 students in the final year class and of the 8 clinical blocks completed, only one block is in a university based site. Thus the academic department would have had to negotiate a total of 273 clinical education block placements for this final year class. With this in mind the fact that the number of students placed varied from two to 35 in a single site over the year with a median of 12, supports the finding that some clinical education sites limit the student numbers to two and sometimes three per block. The clinical education sites that accommodated the 35 students are typically the academic hospitals with multiple departments, but usually no more than two students were accommodated even in these departments. Numbers are limited as clinical managers seem to favour the apprenticeship model of clinical education in which only one student is allocated to each clinical educator, which has not been found to be superior to other models of clinical education such as the collaborative models16,28,29. Numbers are also limited because only 45.3% of staff are involved in clinical education, with the commonest criteria for allocating clinical educators being competence in clinical education and where the staff member had trained. While experience may be a criterion for selecting staff to be clinical educators, there are sites, (particularly those at the primary care level) where there are only community service occupational therapists who are clinical educators. The academic department has only one criterion to guide who is appropriate to be a clinical educator of the student and that is they must have a current HPCSA registration. Thus the idea that staff trained at Wits should be the clinical educators of the Wits students is complex. While it speaks to differences in programme structure and teaching and learning strategies and approaches, all South African graduates and community service OTs should have mastered the clinical competencies prescribed in the HPCSA minimum standards to graduate and thus register2.
The majority of these findings are consistent with the literature from other countries5,30-32. However, there are implications for students as sites are selected based on availability and logistics rather than the quality of the leaning experience the student might have. In addition, students are usually at a different clinical education site every block which occurs about every 5 weeks, this demands continuous adaptation to new staff and a new context without much settling-in time33. Since only one site falls within a five kilometre radius from the campus, and some sites as far as 350 kilometres away, travelling time, transport costs and in some cases accommodation costs must also be factored in.
In most clinical placement sites senior management appears to have little awareness of the clinical education that is taking place within the OT departments, with only three department heads reporting on clinical education activities to their senior managers. While this may be historical because most clinical sites have a long association with Wits, this may influence the capacity of the OT department to successfully provide clinical education. The literature suggests that clinical education is most successful in clinical sites where there is an ethos of learning that is embodied within the strategic values and objectives of the organisation, and is supported practically by resource availability for education purposes and releasing of staff for clinical education training and updates9. This is difficult in many departments where the stated focus is on service delivery, and the fact that only one department has a teaching and learning policy that pertains to students may be symptomatic of this.
Occupational therapy managers view the most important benefit of being involved in clinical education as the provision of assistance with managing the clinical load. The idea that students contribute to a clinical department's management of the clinical load is well-described in the literature28,34-36. Paradoxically, while students help to manage the clinical load, their clinical education requirements also create work, which presents departments with great challenges such as the time the clinical education takes8. These two conflicting issues suggest that clinical departments and the Wits academic department have a different view of the goals of clinical education in the overall education process which includes: service delivery to develop clinical competency, and development of clinical competencies through a structured education programme of learning. The latter includes the time-consuming educational activities of student observation, feedback and evaluation37. A further implication of this is the academic department's experience that clinical sites are reluctant to take on the clinical education of the more junior students in the first to third year of study because they need too much input and cannot contribute to service delivery.
The challenge of keeping up to date is also well described in the literature. However clinical education enables staff members to collect CEU points which are essential for maintaining clinical competence and registration by the HPCSA. In addition, it enables staff to keep up to date with new developments within the profession as reflected in the changing educational content taught to students. While on one hand this is a positive benefit, it also becomes a challenge as clinical educators seldom incorporate these new developments into their practice. This often creates a source of conflict between what is taught and what is practised. Students are negatively influenced by this and it is often also a source of conflict between the academic staff and the clinical educators. This represents the 'knowledge gap' that exists between academics and clinical OTs.
CONCLUSION
Occupational therapy site managers, together with their facility senior managers, have an important role to play in the success of a facility as a clinical education site. They are required to provide an environment with a culture of learning, resources for teaching and learning and regular review of the success of such activities. On the Wits clinical education platform most facility senior managers appear to be relatively unaware of the clinical education of occupational therapy students in their departments. In some departments the OT manager has no role in the clinical training programme, in others the role is logistical or supportive and only in a few do the OT managers have an active role. The OT managers perceive the main benefits of clinical education to be assistance in managing the clinical load and an opportunity for staff to keep up to date. Time demands and staff issues are the greatest challenges.
REFERENCES
1. Hocking C, and Ness NE. Revised Minimum Standards for the Education of Occupational Therapists002: World Federation of Occuaptional Therapists. [ Links ]
2. HPCSA, Professional Board for Occupational Therapy, Medical Orthotists and Prosthotists and Art Therapy, Minimum Standards of Training for Occupational Therapists, 2010. [ Links ]
3. Boyt Schell B, Gillen G, Schaffa M, Cohn M. Professional Reasoning in Practice, in Willard and Spackman's Occupational Therapy, Boyt Schell B, et al., Editors. 2013, Wolters Kluwer Lippincott Williams and Wilkins: Philidelphia: 384-394. [ Links ]
4. Health Professions Council of South Africa, Continued Professional Development: Guidelines for health Professionals, 2009: Pretoria. [ Links ]
5. Baldry Currens J and Bithell P The 2:1 Clinical Placement Model: Perceptions of clinical educators and students. Physiotherapy, 2003. 89(4): 204-218. [ Links ]
6. Huddleston R. Clinical Placements for the Professions Allied to Medicine, Part 1: A Summary. British Journal of Occupational Therapy,1999. 62 (5): p. 213-219. [ Links ]
7. Bonello M. Fieldwork within the context of Higher Education: a Literature review. British Journal of Occupational Therapy, 2001. 64(2): 93-99. [ Links ]
8. Steele-Smith S. and Armstrong M. "I would take more students": Student Supervision strategies. British Journal of Occupational Therapy, 2001. 64(11): 549-551. [ Links ]
9. Brown L, and Kennedy-Jones M. Part 2 The Manager Role, in Transforming Practice Through Clinical Education, Professional Supervision and Mentoring, M. Rose and D. Best, Editors. 2005, Churchill Livingstone Elsvier: Edinburg. 1-369. [ Links ]
10. Goa K and Calderon A. Roles, Skills and Competencies of Middle Managers in Occupational Therapy. The Health Care Manager, 2007; 26(1): 74-83. [ Links ]
11. Aulsop A. and Ryan S. Making the most of Fieldwork Education : A Practical Approach. 2nd edl999, London Chapman and Hall, 243. [ Links ]
12. BestD. Exploring the Role of the Clinical Educator, in Clinical Education, Professional Supervision and Mentoring, M. Rose and D. Best, Editors. 2005, Elsvier Churchill Livingstone: Edinburgh: 45-48. [ Links ]
13. Bester J and Beukes S. Assuring Quality in Clinical Education. South African Journal of Occupational Therapy, 2011, 41(3): 30-34. [ Links ]
14. Sweeney G, Webley P and Treacher A. Supervision in Occupational Therapy, Part 3:Accomodating the Supervisor and Supervisee. British Journal of Occupational Therapy, 2001c. 64(9): 426-431. [ Links ]
15. Ladyshewsky R. Enhancing Service Productivity in Acute Care In Patient Settings Using a Collaborative Clinical Education Model. Physical Therapy, 1995. 75(6): p. 503-510. [ Links ]
16. Jung B, Sainsbury S, Grium R, Wilkins R, Tryssenaar J. Collaborative fieldwork education with student occupational therapists and occupational therapist assistants. Canadian Journal Of Occupational Tharapy, 2002. 69(2): p. 95-103. [ Links ]
17. Hallin K, Kiessling A, Waldner A, Hendriksson P. Active interprofessional education in a patient based setting incrreases perceived collaboration and interprofessional competence. Medical Teacher, 2009. 31: p. 151-157. [ Links ]
18. Ponzer S, Hylin U, Kusoffsky A, Lauffs M, Lonka K, Malliasson A. Interprofessional training in the context of clinical practice: goals and students' perceptions on clinical education wards. Medical Education, 2004. 38(7): 727-736. [ Links ]
19. Costa D.M. Clinical Supervision in Occupational Therapy: A Guide for Fieldwork and Practice. 1 ed2007, Bethesda: American Occupational TherapyAssociation, Inc. 277. [ Links ]
20. Higgs J. Foreword, in Transforming Practice through Clinical Eduaction, Professional Supervision and mentoring, M. Rose and D. Best, Editors. 2005, Elsevier Churchill Livingstone: Edinburgh: ix-x. [ Links ]
21. Crowe MJ and Mackenzie L. The influence of fieldwork on the preferred future practice areas of final year occupational therapy students. Australian Occupational Therapy Journal, 2002, 49(1): 25-36. [ Links ]
22. Weddel K. Competency Based Education and Content Standards. 2006 [cited 2012 26.11.2012]; Available from: http://www.cde.state.co.us/cdeadult/download/pdf/competencyBasedEducation.pdf. [ Links ]
23. Costa D. Fieldwork Issues: Fieldwork Educator Readiness, 2007, American Occupational Therapy Association: Bethesad: 1-3. [ Links ]
24. Campbell J. Essentials of Clinical supervision, 2006, Hoboken: Wiley. [ Links ]
25. Forsyth K. and Kviz F. Survey Research Design, in Research in Occupational Therapy: Methods of Inquiry for Enhancing Practice, G. Kielhofner, Editor 2006, F.A. Davis Company: Philadelphia:91-109. [ Links ]
26. Kielhofner G. Developing and Evaluating Quantitative Data Collection Instruments, in Research in Occupational Therapy: Methods of Inquiry for Enhancing Practice, G. Kielhofner, Editor 2006, F A Davis Company: Philadelphia: 155-176. [ Links ]
27. Creswell J. Quantitative Methods, in Research Design: Qualitative, Quantitative and Mixed Methods Approaches. 2009, Sage: Los Angeles: 145-171. [ Links ]
28. Barthomai S. and Fitzgerald C. The Collaborative Model of Field-work Education: Implemention of the model in a regional hospital rehabilitation setting. Australian Journal of Occupational Therapy. 2007, 54: S23-S30. [ Links ]
29. Lekkas P, Larsen J, Kumar S, Grimmer K, Nyland L, Chipchase L, Buttrumo O. Carr L, Finch J. No model of clinical education for physiotherapy students is superior to another : a systematic review. Australian Journal of Physiotherapy, 2007. 53: 19-28. [ Links ]
30. Rodger S, Webb G, Devitt L, Wrightson P McMeeken L. Clinical Education and Practice Placements in the Allied Health Professions: An Internnational Perspective. Journal of Allied Health, 2008. Spring 37(1). [ Links ]
31. Sweeney G, Webley P Treacher A. Supervision in Occupational Therapy, Part 1:The supervisors anxieties. British Journal of Occupational Therapy, 2001a. 64(7): 337-345. [ Links ]
32. Sweeney G, Webley P, Treacher A. Supervision in Occupational Therapy, Part 2: The Supervisee's Dilemma. British Journal of Occupational Therapy, 2001b. 64(8): 380-431. [ Links ]
33. Garret S, Schkade J. Occupational Adaption Model of Professional Development as Applied to Level II Fieldwork. American Journal of Occupational Therapy, 1995. 49(1): 119-126. [ Links ]
34. Thomas Y, Lickson D, Broadbridge J, Hooper L, Hawkins R, Mc-Bryde K. Benefits and challenges of supervising occupational therapy fieldwork students: Supervisors' perspective. Australian Journal of Occupational Therapy, 2007. 54: p. S2-SI2. [ Links ]
35. Fisher, A. and Savin-Baden M. Modernising Fieldwork,Part I: Realising the Potential. British Journal of Occupational Therapy, 2002. 65(5): 229-236. [ Links ]
36. Fisher A, Savin-Baden M. Modernising Fieldwork, Part 2: Realising the New Agenda. British Journal of Occupational Therapy, 2002. 65(6). [ Links ]
37. Marriott J, Galbraith K. Part 3 Instructor, Observer and Provider of Feedback, in Transfroming Practice through Clinical Education, Professional Supervision and Mentoring, M. Rose and D. Best, Editors. 2005, Churchill Livingstone Elsivier: Edinburg. p. I-369. [ Links ]
 Correspondence:
Correspondence:
Patricia De Witt
Patricia.DeWit@wits.ac.za














