Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
South African Journal of Occupational Therapy
On-line version ISSN 2310-3833
Print version ISSN 0038-2337
S. Afr. j. occup. ther. vol.43 n.3 Pretoria Mar. 2013
ARTICLES
A Clinical Skills Unit: Addressing the need for Continued Professional Development (CPD) in Allied Health Professions
Santie van VuurenI; Mariette NelII
IM occupational Therapy, PhD (Health Professions Education). Head: School for Allied Health Professions, and Senior Lecturer: Department of Occupational Therapy, Faculty of Health Sciences, University of the Free State, Bloemfontein, South Africa
IIMMedSc. Lecturer, Department of Biostatistics, Faculty of Health Sciences, University of the Free State, Bloemfontein, South Africa
ABSTRACT
INTRODUCTION: The Health Professions Council of South Africa (HPCSA) monitors compulsory continuing professional development (CPD) to ensure that healthcare professionals update their knowledge and skills to the benefit of their clients. One of the objectives of the Clinical Skills Unit (CSU) in the School for Allied Health Professions at the University of the Free State (UFS) was to use it for CPD as part of a responsibility towards alumni. This study investigated the needs of qualified dieticians (DT), occupational therapists (OT) and physiotherapists (PT) to assist in the provision of relevant CPD activities at the Unit.
METHODS: A descriptive, comparative study was conducted. Two hundred and fifty-eight questionnaires were distributed in the Free State and Northern Cape provinces, to members of the professional groups mentioned above. To ensure reliability, 10% of the sample was re-tested after one month.
RESULTS: One hundred and twenty-seven professionals responded to the questionnaire, with 55.6% being from the Free State. CPD activities were attended in Bloemfontein by 65.9%. Most of the CPD activities (70.6%) attended prior to the study were theoretical in nature and 85% of respondents would have prefered to observe experts and learn by doing. Differences between the groups were significant for some of the questions, for example, dieticians preferred a large group didactic approach while the other professional groups prefered to observe experts and be involved in the learning process. All the professionals prefered CPD activities to be presented by an expert in their specific field of practise.
CONCLUSIONS: Taking into consideration the views of professionals and the results of international studies, the CSU at the UFS will be able to address the CPD needs of allied health professionals in the Free State and Northern Cape.
Keywords: clinical skills unit; continued professional development; allied health professions.
INTRODUCTION
The importance of educating health professionals to keep up with the communities' changing needs was advocated nearly a century ago by Abraham Flexner1. The Alma Ata Declaration of 1978, the World Health Organisation (WHO)2 also put forward the view that health services should be more equitable and appropriate to the needs of the people. This view was confirmed, for South African healthcare workers, in the Cape Town Declaration of 19953.
One of the factors that affect the health services of a country is the human resources that are available to render these services. In a press release entitled World Health Report4,the WHO noted that health care workers, who lack the necessary training and knowledge, may be a major obstacle for health systems in the world. With the new health dispensation in South Africa, namely the imminent rollout of the National Health Service, not only will it be important to maintain skills, but also to learn new and innovative ways of delivering quality services, with a greater focus on preventative and promotive healthcare and orientated to the needs of the community.
Continuing Professional Development (CPD) comprises postgraduate clinical education aimed at engaging the practitioner in a lifelong process of learning5. The goal of CPD as described by Amerih6 supports the view of the WHO4, in that it continuously improves the quality of healthcare practice, providing opportunities for professional growth and maintaining up-to-date knowledge and skills. A statement on CPD for health and social practitioners in the United Kingdom7, clearly states that the purpose of CPD is to enhance the quality of care that patients and clients receive from their healthcare providers.
Woollard8 and Philips9 assert that it is the responsibility of higher education institutions (HEI's) not only to ensure that undergraduate students attain the minimum standard of education, but also, that alumni maintain the required minimum standards. In some countries, CPD is managed by a separate entity, for example, the Beeches Management Centre7 in the United Kingdom and the Mayo Clinic10 in the United States of America. According to Castleman,11the coordination and management of CPD activities by higher education institutions (HEIs) in South Africa vary considerably, with many institutions failing to acknowledge CPD as an integral part of their responsibility. The current scenario is that in most HEIs, CPD is decentralised to various professional groupings.
The monitoring of CPD is the responsibility of the Health Professions Council of South Africa (HPCSA)12 and its constituent Professional Boards. In 2005, the HPCSA established an overarching CPD committee consisting of representation from all twelve Professional Boards. As a first step, the Health Professions Amendment Bill of 200613, Section 26, stated that the Council could make rules in terms of registration, the conditions related to registration and retaining registration, the nature and providers of CPD activities. After extensive research and consultation, the CPD framework was officially implemented in January 200712. It is mandatory for all practising health professionals, (including dieticians, physiotherapists and occupational therapists) to be registered with the HPCSA. It is the view of the Council that CPD plays a vital role in helping healthcare professionals acquire new and updated levels of knowledge, skills and ethical values. This view is shared by the Canadian Association of Occupational Therapy14 which recognises that access to and acquisition of current relevant and evidence-based knowledge, skills and behaviours are the key to the development and use of best practices in occupational therapy.
South African health professionals are, by law compelled to accumulate 60 Continuing Education Units (CEUs) in any given two-year period. Therefore, random audits are done to establish the compliance of registered members. Non compliance can lead to suspension of registration with the Council13.
Three of the programmes, namely dietetics and nutrition, occupational therapy and physiotherapy in the School for Allied Health Professions (SAHP), located in the University of the Free State (UFS) in Bloemfontein, South Africa, at the time of the study have to adhere to these regulations.
The results of an international study by Amerih6 reported that only 25% of occupational therapy (OT) respondents indicated that CDP activities were readily available, and that therapists in developed countries were more likely to participate in CPD activities than those in developing countries. CPD is also mandatory for physiotherapists in many countries and a range of formal and informal activities exist15. A study by Gunn16 supports evidence that CPD has an effect on the clinical practises of physiotherapists based in community primary care, and that undertaking CPD improves confidence as well as competence. A study by Martin et al.17 concluded that CPD existed to ensure that scientific information was accessible to all dieticians in South Africa and that this could only happen if a system existed that was supportive of learning opportunities. The HPCSA is, however, concerned about the percentage of non-compliance among health workers registered by the various Professional Boards. For example, according to the HPCSA only 32% of Dieticians18 and 29% of Occupational Therapists19 were CPD-compliant over the last few years.
Research by Van Vuuren and Nel20 on the value of a Clinical Skills Unit (CSU) led to the planning, construction and establishment of a CSU for the School for Allied Health Professions at the University of the Free State. The CSU is viewed as a facility in which students, physicians, nurses and other health professionals can learn clinical and communication skills, to a specific level of competence, prior to, and in coordination with patient contact21. The perceived vision and functions22 of the CSU at the School for Allied Health Professions were undergraduate clinical skills training, postgraduate clinical skills training (including CPD activities), community service, and student and staff wellness. After commissioning of the facility in 2011, strategies had to be developed to ensure that these functions were established. Dent23:406 asserted that "Clinical Skills Centres (CSC) must develop continuously if they are to respond to the current demands and future challenges" and continues his argument that if CSC's wanted to expand their activities, including the offering of CPD, they should:
(i) Be recognised as an independent entity;
(ii) engage an efficient management structure;
(iii) secure a substantial and reliable budget;
(iv) co-operate with academic standards committees (in this case the HPCSA and the South African Qualifications Authority [SAQA]);
(v) maintain good relations with other key stakeholders within the Faculty;
(vi) develop a recognised career structure that attracts and supports its teaching staff;
(vii) value the human resources at the centre and
(viii) remain approachable to everyone.
However, in order to utilise the full potential of a Clinical Skills Unit for CPD activities, Eraut24 noted that sufficient attention was rarely given to the identification of learning needs, the prioritisation of these needs and matching the needs to learning opportunities and activities in delivering CPD activities/programme. Grant25 argued that learning is more likely to lead to change when a needs assessment has been conducted and the education is linked to practice. Literature therefore supports the argument that establishing the learning needs and priorities of professionals is important before CPD is planned and offered. The investigation can be viewed as a necessary step to fully utilise the Clinical Skills Unit for CPD of allied health professionals.
PROBLEM STATEMENT
Allied health professionals in central South Africa, especially the Free State and Northern Cape provinces, do not always, for a variety of reasons, have access to a range of CPD activities. In addition, at times they are required to attend such activities, sometimes at great cost, outside the provinces, to adhere to the expectations of the HPCSA. In the opinion of the first author who has been involved in the training of allied health professions in the Free State for more than thirty years, a high percentage of CPD activities focus on knowledge provision, usually in big groups rather than skills acquisition as well as limited provision for individual activities or the development of specific needs. In addition, very little research or exploration has been undertaken to ascertain what CPD activities allied health practitioners might like to have access to. As the University of the Free State and the CSU at the School for Allied Health Professions is currently the only Institution of Higher Education in both these vast rural provinces, it is crucial that the Institution and its entities should play a role in the provision of CPD.
STUDY METHODS
Aim of the study
The aim of the study was to investigate the CPD needs of the identified allied health professionals (occupational therapists, physiotherapists and dieticians,) in the Free State and Northern Cape provinces of South Africa. The data could then be used to develop a proposal for the offering of CPD activities within the CSU, at the School for Allied Health Professions.
Methods
The research design was of a descriptive nature26. A survey was undertaken by means of a self-administered questionnaire that collected information on the views of the identified allied health professionals. Approval to conduct the study was granted by the Ethics Committee of the Faculty of Health Sciences, University of the Free State.
Study population and sampling
The HPCSA registers indicated that at the time of investigation, there were 138 occupational therapists, 169 working physiotherapists and 141 dieticians in the Free State and Northern Cape (448 in total.) All 448 of these professionals were contacted to participate in the study but only 258 practitioners could be tracked down according to the contact details on the lists. The administrative officer at the CSU continued to communicate with these practitioners to explain the purpose of the study, verify their details, their preferred manner of receiving communication and to enquire if they would also be willing to participate in a reliability test one month after all the questionnaires were returned.
Data Collection
The above mentioned questionnaire was developed from the lit-erature10-21,23 and the personal experience of the first author. This structured questionnaire included questions on: the background information of participants; the frequency of attending CPD activities; the places where they most frequently accessed CPD activities; topics that they wished to be covered to enable service delivery and when it was preferable for these to be scheduled. Before the questionnaires were sent out, a pilot study was conducted to ensure that the questions were unbiased and clear. The Heads of the Departments of Occupational Therapy, Physiotherapy and Nutrition and Dietetics, at the UFS were used to pilot test the questionnaire, to clarify questions and make suggestions on additional questions. The time needed to complete the questionnaire was also established. Changes made to the questionnaire included adding to some of the questions "any other comments" as well as clarifying a few of the questions.
Due to the vast geographical area of the Free State and Northern Cape provinces, a postal survey supplemented at times by, electronic mail and fax was conducted. Questionnaires sent by post included a franked envelope. The majority of participants preferred email as the means of communication. A telephone call to remind participants of outstanding questionnaires was made by the administrative officer two weeks after distribution of the questionnaire. All the participants who did not return their questionnaires were contacted again after one month.
Reliability was provided by re-testing 10% of the sample. The reliability questionnaires were sent to 13 professionals representing the three groups, one month after all the questionnaires were returned (n=127). They were selected to represent the groups proportionally.
The validity of this study is supported by the fact that CPD activities are currently compulsory for all the participants, and they should have had some previous experience of CPD activities.
Data analysis
The analysis of the data was done by the Department of Biostatis-tics, Faculty of Health Sciences, UFS. Descriptive statistics, namely frequencies and percentages for categorical data and medians and percentiles for continuous data, were calculated. Further statistical analysis was done by comparing the responses of the three different groups as well as the differences in the needs of the different age groups by means of 95% confidence intervals (CI) for the percentage difference.
The reliability questionnaires were compared with the questionnaires received earlier. When 20% or more of participants gave a different answer to a question it was deemed unreliable. Nine opinions to four questions were thus deemed unreliable and excluded from the analysis.
RESULTS
One hundred and twenty-seven questionnaires of a total of 258 questionnaires were received back, giving a response rate of 49% considered by the researchers as in keeping with a typical rate for mailed questionnaires27. Forty four percent (44.1 %) of respondents were occupational therapists (OT), 24.4% were dieticians (DT), and 31.5% physiotherapists (PT). Sixty-eight per cent (68.5%) of the participants had worked for a period of less than 10 years. The median period of working was five years, ranging from less than a year to a maximum of 44 years. The majority (71.7%) were working in the public sector. Their place of work was mainly situated in the larger urban areas of the Free State (55.6%) and Northern Cape (44.4%).
Approximately two thirds of the participants (65.9%) had attended CPD activities in Bloemfontein (the capital city in the Free State Province) in the past. Other places where activities were attended included Kimberley (18.3% of participants) and Johannesburg, Pretoria, and Cape Town (15.9% participants. Of these activities, 70.6% were mainly theoretical sessions. Almost all (97.6%) of the participants indicated they would prefer to attend skills sessions, rather than pure theory sessions. A 95% confidence interval (95% CI) to indicate differences between the professional groups was used to analyse the differences in response of the three professional groups.
Table 1 shows the participants' view with regard to preferred learning opportunities during CPD. The results depicted in the table 1 were fairly similar for all three professional groups, and the view was expressed that the activities should cater for both experienced and newly qualified professionals.
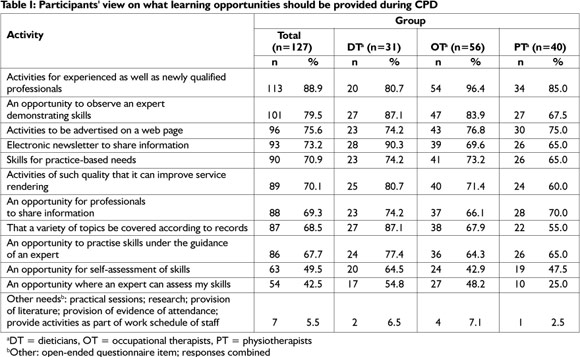
All the groups were positive about web-based activities 76.8% of occupational therapists indicated a need for a web page, compared to 74.2% of dieticians and 75% of physiotherapist's. A statistically significant difference was found on the following questions:
Organise an opportunity in which an expert assesses an individuals' skill on request. Differences were found between DT and PT [7.0%; 49.1%] as well as OT and PT [3.5%; 40.0%]; Record of CPD activities should be kept to ensure that a variety of topics are covered. The results showed the same tendency between OT and DT [-49.1% ; -10.7%] and Introduce an electronic newsletter to share information.A significant difference was found between OT and DT [-35.1% ; -2.2%] and DT and PT [5.4% ; 42.1%].
The results regarding specific skills that should be part of CPD activities as indicated by the participants are listed in Table 2 on page 44.
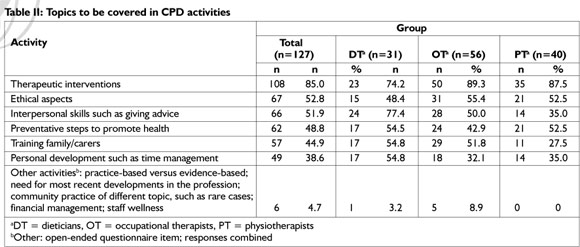
The results in Table 2 reflect the generic topics that allied health professionals want to be addressed during CPD. All the groups placed the highest priority (89.3% of OT; 74.2% of DT and 87.5% of PT) on the addressing of therapeutic intervention skills. A statistically significant difference was found between the different professions on the following questions: Interpersonal skills such as consultation:between DT and PT [6.0% ; 44.3%]), and OT and DT [-59.5% ; -19.2%]; and to educate family and care givers:the differences were between OT and DT [-47.0% ; -4.4%] and PT and OT [4.3%; 41.2%].
The majority of participants (85%) indicated that they would like to learn by doing and would prefer small workshops (89.8%) to learn their skills (see Table III).In the event of the seminar format being used, the theory should be presented by an expert on the topic. Participants working more than 10 years indicated a preference for individual learning activities (65%), compared to professionals working less than 10 years (34.48%.)
A statistically significant difference was found between the DT and PT with regard to observing experts applying procedures on standardised patients [-50.3%;-10.5%]). Observing the demonstration of professional skills by experts; for example, administration of standardised assessment skills:There were no statistical significant difference found between OT and DT [-8.6% ; 23.1%]; and DT and PT [-41.3%; -1.6%].
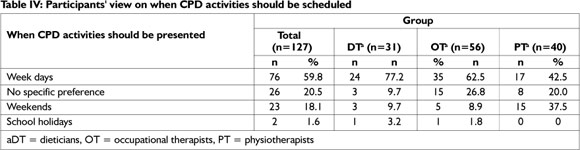
As shown in Table IV on page 44, a slight majority (59.8%) of respondents preferred to attend CPD activities on week days, while 18.1% preferred weekends. With regard to the three different groups, 42.5% of physiotherapists indicated a preference for activities on week days compared to 62.5% of occupational therapists and 77.4% of dieticians.
DISCUSSION
Apart from the main purpose of the CSU to train undergraduate students' skills, one of the other envisaged functions was also to provide for Continued Professional Development.
Non-compliance to CPD activities by dieticians, occupational therapists and physiotherapists has been noted as a concern, and will impact on the offering of quality healthcare in South African. Literature reports that non-compliance is higher among occupational therapists in developing countries6, like South Africa. However, limited information is available on the reasons for the non-compliance. Some of the reasons25 may be that limited attention is given to identifying practitioners learning needs, and prioritising and matching these in delivering CPD. In vast provinces such as the Free State and Northern Cape insufficient communication of CPD activities and updating their contacting details with the HPCSA may also play a role.
The results indicate that the participants have a specific view of CPD activities and suggested that specific topics for example, therapeutic interventions, are covered. In a study involving nurses and allied health professionals in the UK, participants placed emphasis on the importance of applying learning to practice. They were also of the opinion that this may be intuitive without formal measurement or documentation27. It underlines the importance of the results of this study where a formal opportunity was created to establish the focus of CPD from this group.
These results underpin the importance of covering a variety of topics relevant to the service needs during CPD. With the exception of the dieticians, participants preferred the format of the learning experience to be presented in small groups, rather than large formal lectures. According to the 2008-2009 annual report of the Health Professions Council (HPC) of the United Kingdom28, many professionals in the UK emphasised that formal didactic learning was not the only means to keep up-to-date. In terms of the way in which activities are presented, the results of this study correspond with the view of the NHS29 that the focus should be on practical experience, and skills units that simulate learning through practise are becoming more commonplace and should be encouraged.
Participants with more than ten years of experience indicated a need for individually structured activities to develop or recap their skills. Literature supports an emerging difference in CPD needs and provision among specialist (ex. more experienced) and more junior staff30.
All the participants were of the opinion that they wanted experts in their field of practice to present CPD activities. They would welcome the development of electronic media to communicate CPD activities, make online requests for activities and register for these activities. Also to enable the sharing of opinions and asking for advice and guidance. This concurs with the view of Dent 23 that a CSC should be approachable to those in need of additional help. The results showed that practitioners would prefer a different approach to the majority of current activities by using more practical learning that focuses on skills. These results are similar to the view of Austin31 on CPD.
Most of the participants indicated that they have come to Bloemfontein for CPD in the past, so the CSU is well situated at the University of the Free State. The CSU was planned for the use of all the allied health professionals in the School of Allied Health Professions at the UFS. The unit is staffed with a manager, administrative assistants, technical assistants for set-ups, has state of the art equipment, information technology facilities, and an outdoor area where training of specific outdoor skills can take place.
In keeping with Dent's23 view on what a CSU should offer, the CSU at the School for Allied Health Professions is well placed to address the CPD needs as expressed by the participants of this study. Dent23 recommended that a CSU should be a separate entity. The CSU at the UFS is a separate entity and serves all the programmes within the School. Further, the unit is managed by its own complement of staff under the leadership of the Head of the School. Another recommendation24 is that it should maintain good relations with other key sections within the Faculty. The Faculty of Health Sciences has formed an interest group within the faculty with representation from the skills/simulation unit of the SAHP Schools of Medicine and Nursing to enable collaboration and sharing between the Schools.
With reference to the results reported here, the unit has the facilities and resources to (i) address the needs of "learning while practising"; staff are employed to do practical set-ups according to the presenters needs; (ii) host small workshops/seminars; the floor space of the unit has been designed to easily be altered or changed according to specific needs; (iii) allow for the opportunity to observe or learn from experts; (iv) make use of multimedia; the unit, for example, has its own computer laboratory and audiovisual equipment; and (vi) perform activities in small groups or on an individual basis.
The results of this study will not only give direction to the various professional groups responsible for CPD, but ensure that the CSU becomes a place that draws professionals to activities of quality, in order to comply with CPD. In addition, this will hopefully see a move away from pure gathering of the required CPUs points, but rather afford practitioners the time and space to learn and master new skills and knowledge.
Quality assurance measures are also compulsory for all departments and unit at the UFS and regularly monitored. The Liaison group of the Health Professions Council UK28 recognised that the quality of CPD activities was in many instances more important to maintain high standards in practice, than the quantity of CPD undertaken. It is recommended that peer evaluation of the activities and the organisation, administration and management of the activities is implemented to adhere to quality assurance measures at the CSU. Furthermore, the CSU can implement and ensure quality assurance for example peer and expert evaluation of all activities, which is a priority.
Implications for practice
The CSU should consider developing a web-based environment to offer information of CPD activities, other practice-related enquiries and offer activities applicable according to indicated needs of the different professional groups. Expert presenters should be invited to present CPD activities and these presentations and demonstrations should focus on skills and these could be streamed live to give access to health professionals. CPD activities should be hosted in small workshops, seminars or discussion groups. A well equipped unit such as the CSU can bring about the opportunity for evidence based professional- and educational research, as well as inter professional research.
CONCLUSION
While there is evidence of non-compliance to CDP by allied health professionals in South Africa, the reasons are currently unknown especially for the practitioners in the Free State and Northern Cape provinces. The building of the CSU at the SAHP also envisioned the provision of CPD activities, but the view of practitioners was needed to ensure that their needs were met. Results of the study showed that the CSU at the UFS has the potential to address the CPD needs of allied health professionals in the Free State and Northern Cape.
ACKNOWLEDGEMENTS
Dr. Daleen Struwig, medical writer, Faculty of Health Sciences, UFS, for assistance with technical and editorial preparation of the manuscript.
REFERENCES
1. Flexner A. Medical education in the United States and Canada. A report to the Carnegie Foundation for the advancement of teaching. Boston: D B Updike, The Merry mount Press, 1910. http://www.carnegiefoundation.org/sites/default/files/elibrary/Carnegie-Flexner_Report.pdf. (28 June 2010). [ Links ]
2. Wilm S. The context of the 1988 Edinburgh Declaration of the WFME in Health Policy - Health for all by the year 2000. Frankfurt: Institute for General Practise and Family Medicine. [ Links ]
3. World Federation for Medical Education (WFME). African Regional Conference on Medical Education: Cape Town Declaration. Cape Town: World Federation for Medical Education, 1995. [ Links ]
4. WHO (World Health organisation). World Health Report outlines need for more investment in health workforce to improve working conditions, revitalize training institutions and anticipate future challenges. Geneva: World Health Organisation, 2006a. [ Links ]
5. HPCSA (Health Professions Council of South Africa). Global challenges in continuing professional development. South Africa: HPCSA CPD Committee, 2010. [ Links ]
6. Amerih H. International occupational therapists' continuing education needs and opportunities: a survey. Open Journal of Occupational Therapy, 2013; 1,2: 1-3. [ Links ]
7. Beeches Management Centre. Allied Health Professions. Centre for Professional Development - Newsletter. First edition. 2003. http://www.dhsspsni/ahp_cpd_newsletter.pdf (7 May 2012). [ Links ]
8. Woollard RF. Caring for a common future: medical schools' social accountability. Medical Education, 2006; 40: 301-313. [ Links ]
9. Phillips A. Allied Health Professions: Centre for Professional Development. Newsletter. 2003. www.fhodkinson@beeches.bmc.n-nhs.uk (10 Dec 2010). [ Links ]
10. Mayo School of Continuous Professional Development (MSCPD). http:www.mayo.edu/cme/ (7 May 2012). [ Links ]
11. Castleman EM. A model to manage continuous professional development for the alumni of a private higher education institution. Thesis: PhD in Health Sciences Education. Bloemfontein: University of the Free State, 2007. [ Links ]
12. Health Professions Council of South Africa (HPCSA). Continued Professional Development. http://www.hpcsa.co.za/cpd-overview.php (28 June 2010). [ Links ]
13. Republic of South Africa. Health Professions Amended Bill. Government Gazette No. 28754 of 28 April 2006. Pretoria, 2006 [ Links ]
14. Canadian Association of Occupational Therapy (CAOT). CAOT Position statement on continuing professional development. 2006. www.caot.ca/default.asp?pageID=153 (26 March 2010). [ Links ]
15. French HP Dowds J. An overview of continuing professional development in physiotherapy. Physiotherapy, 2008; 94: 190-197. [ Links ]
16. Gunn H. 2009. Continuing professional development of physiotherapists based in community primary care trusts: a qualitative study investigating perceptions, experiences and outcomes. Physiotherapy, 2009; 95: 209-214. [ Links ]
17. Martin C, Labadarios D, Marais D, Wentzel-Viljoen E. Dietician's perceptions of the continuing professional development system in South Africa. South African Journal of Clinical Nutrition, 2008; 21: 27-33. [ Links ]
18. HPCSA (Health Professions Council of South Africa) 2011. Dietetics and Nutrition Newsletter. www.hpcsa.co.za/downloads/news/dietetics/newsletter_20ll.pdf. (24/04/2013) [ Links ]
19. Health Professions Council of South Africa (HPCSA). OCP News, August 2012. [ Links ]
20. Van Vuuren S, Nel M. Clinical skills centre: possibilities for the training of South African occupational therapists. South African journal of Occupational Therapy, 2010; 40: 3. [ Links ]
21. Sebiany AM. New trends in medical education. The clinical skills laboratories. Saudi Medical Journal, 2003; 24:1043-1047. [ Links ]
22. Van Vuuren S, Moja LVM, Viljoen M. School for Allied Health Professions: Clinical Training Grant (Higher Education Institution). Proposal for funding. Bloemfontein: University of the Free State, 2011. [unpublished] [ Links ]
23. Dent JA. Adding more to the pie: the expanding activities of a clinical skills centre. Journal of Royal Society of Medicine, 2002; 95: 406-410. [ Links ]
24. Eraut M. Do continuing professional development models promote one-dimensional learning? Medical Education, 2001; 35: 8-11. [ Links ]
25. Grant J. Learning needs assessment: assessing the needs. British Journal of Medicine, 2002; 324: 156-159. [ Links ]
26. Maree K. First Steps in Research. Pretoria: Van Schaik, 2008. [ Links ]
27. Leedy PH, Omrod JE. Practical Research: Planning and Design. Ohio: Merrill Prentice Hall, 2001. [ Links ]
28. Health Professions Council, UK. Continuing Professional Development Annual Report 2008-2009. http://www.hpc_uk.org/assets/documents/10002019 (3 May 2013). [ Links ]
29. Department of Health, United Kingdom, NHS. Meeting the Challenge: A Strategy for the Allied Health Professional Development for Health and Social Practitioners. 2007. http://l78.239.l6l.l48/resources/20.pdf (7 May 20l2). [ Links ]
30. Haywood H, Pain H, Ryan S, Adams J. Continued Professional Development: Issues Raised by Nurses and Allied Health Professionals Working in Musculoskeletal Settings. Wiley Online Library, 2012. www.wileyonlinelibrary.com. (l May 2013. [ Links ])
31. Austin A, Glover MacLeod N, Croteau D. Continuous professional development: a qualitative study of pharmacists' attitudes, behaviours and preferences in Ontario, Canada. American Journal of Pharmaceutical Education, 2005; 69: 25-33. [ Links ]
32. Friedman A, Phillips M. Leaping the CPD hurdle: a study of the barriers and drivers to participation in continuing professional development. Paper presented at the British Educational Research Association Annual Conference, l3-l5 September 200l, University of Leeds. http://www.leeds.ac.uk/educol/documents/00001892.htm (3 May 2013). [ Links ]
 Correspondence:
Correspondence:
Santie van Vuuren
gnatsvv@ufs.ac.za














