Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
South African Journal of Occupational Therapy
versão On-line ISSN 2310-3833
versão impressa ISSN 0038-2337
S. Afr. j. occup. ther. vol.43 no.3 Pretoria Mar. 2013
ARTICLES
Quality management in occupational therapy
Helen RobinsonI; Prof Annali BothaII
IDipl OT (London), MPH (UniSA/UKZN). Occupational Therapist, Mahikeng, North West Province
IIB Our (Pret), M Our (Pret), d Our (Pret). Associate Professor - Community Health, Department of Health Studies, University of South Africa
ABSTRACT
Although quality management is used in occupational therapy in South Africa, no comprehensive description or standardisation of it exists and literature in the context of this topic is scarce. As a consequence of this, the purpose of this study was to describe the extent of occupational therapists' involvement in quality management.
A quantitative study in the form of a survey was carried out. A convenience sample of 80 occupational therapists was surveyed, using a structured questionnaire. Results of the study indicated that most occupational therapists have some knowledge of quality frameworks. Standardisation of documentation and its auditing appear to be one of a number of problems. Another challenge is that occupational therapists may work in relative professional isolation making it problematic to implement quality management.
Recommendations were made for occupational therapy practice and further research, as well as a proposed quality management framework for occupational therapy in South Africa.
Key words: Quality management, occupational therapy, audit, minimum standards, professional development.
INTRODUCTION
Historically, quality in healthcare has been of concern for almost as long as humans have been promoting health and healing the sick.
Increasing litigation, an emphasis on the consumer in healthcare and the need for fiscal restraint makes quality management an essential component of practice for healthcare professionals1. Spiralling healthcare costs globally and locally have highlighted the need to manage the inefficiencies in health services that drain resources. Costly and inefficient health services mean that fewer individuals are able to benefit from them2. Assessing the quality of care has become progressively more important to providers, regulators and purchasers of care, with a greater focus on evidence-based medicine and cost-effectiveness3.
Allied health professionals, including occupational therapists (OTs) are becoming more exposed to the necessity of explaining and demonstrating the value they bring as experts and professionals. This means that the interventions that therapy professionals provide must have a strong base of evidence of their effectiveness, and outcomes should be measurable4. In South Africa the re-structuring of the entire health system is impending in the form of a National Health Insurance scheme, priority aims of which include access to quality healthcare and the minimising of financial risk5. In such a climate it is more important than ever before that therapy and rehabilitation services are of a suitably high quality, are cost-effective and provide discernible positive outcomes for those receiving them. Quality activity will continue to grow, not only being profession-specific with the focus on clinical care, but also as a management concept in healthcare, critical to evaluating and maintaining efficacy and efficiency6,7.
There is a general lack of research evidence as to which frameworks and quality methods are most effective8,9. Additionally there is a paucity of valid and reliable measurement techniques, a lack of definition of key indicators for quality in occupational therapy (OT) both locally and internationally and very few guidelines on the methods used for quality management.
Measuring the outcome of treatment and health services is challenging. In occupational therapy, quality of life through improved function and adaptive responses is a key aim of treatment. However, it is not always straightforward to achieve consensus as to what the desired outcomes are and there are often difficulties with confounding influences - factors outside of treatment which might influence the patients' progress1. This means that structure- and process-orientated aspects of service delivery, such as treatment planning and assessment, environment/equipment, timeframes, patient satisfaction and throughput of patient numbers, risk being prioritised over the actual outcome of treatment. Conversely, in some circumstances a high standard for such processes is actually associated with a better outcome for the patient10, meaning that if service delivery processes are being carried out well, it is more likely that the patient is gaining from their actual treatment, even if it is difficult to measure the outcome directly. One example of a locally developed quality initiative that looks at structure (such as treatment environment and facilities), process (such as assessment, treatment planning and implementation) and outcome is Beukes' work, which provides research-based consensus for developing and measuring standards for vocational assessment11.
This structure-process-outcome framework for quality in healthcare, originally developed by Donabedian, is largely interpreted as an inspection-based or standards-based approach to quality evaluation12, other examples in South Africa are that of the Council for the Accreditation of Health Services in South Africa (COHSASA) and the National Department of Health's National Core Standards initiative. However, other frameworks for quality management exist and include industry-derived models, such as total quality management and its health-orientated derivative– continuous quality management. These have been largely devised in the United States, and place the focus of a service on the customer (or patient, when applied to healthcare), with the use of quality circles an important tool13. Another framework is that of clinical governance which uses a number of ‘key pillars’ for quality14. Netcare private health group uses a clinical governance model15. In South Africa, the National government’s ‘Batho Pele’ approach provides a legislative and policy framework for quality service delivery in the public sector which extends to healthcare through the Patients’ Charter16.
Almost all quality frameworks make use of a cyclic approach ('quality cycle'), albeit in different forms. But in general, problems are analysed or standards set. Following measurement and intervention there is a return to the original issues to reflect on progress, set new goals and begin the cycle again.
There are many quality methods or tools that can be used to measure, monitor and improve quality, either within the structure of a framework or independently. For the purpose of this study, defining methodology by that related to audit/criteria-setting, that related to professional and clinical development, and that directly evolving from the key quality models/frameworks provides a useful way of identifying, with greater clarity, the types of quality activities that OTs are involved in. Identifying the core values of a health service and setting minimum standards may have little meaning in practice if such standards are not measured by some form of auditing, examples being clinical audit, where treatment is examined against established clinical guidelines, processes or protocols, audit of documentation and peer reviews. Stemming more directly from some of the existing quality frameworks are quality methods such as monitoring of adverse clinical, financial or health and safety events, reviewing the performance of staff and eliciting the views of service users to guide quality. Methodology relating to professional and clinical development may include continuing education, use of evidence-based practice (EBP), special interest groups and practitioner specialisation in a clinical field. Professional interest organisations such as the Occupational Therapy Association of South Africa (OTASA) generally play a prominent role in such activities.
OTs are being encouraged to take ownership of many aspects of quality management in the profession, in a dynamic healthcare system, whether this is under the umbrella of accreditation procedures, within other frameworks, or independently. From this it can be deduced that quality- management frameworks are being used, as well as methods for measuring and improving quality in OT. The problem is, however, that there is no comprehensive description of them and no standardisation of their use.
The purpose of this study was to describe the extent of occupational therapists' involvement in quality management.
The objectives of the study were to:
♣ Describe the extent to which OTs are involved in quality management activities
♣ Describe the methods that OTs are using when improving quality
♣ Make recommendations for the implementation of quality-management programmes for use in the profession.
LITERATURE REVIEW
The last two decades have seen the rise and fall of a number of concepts, ideas and methods in healthcare quality improvement17 The content of most quality-management methodologies is broadly similar, despite changing and often confusing terminology - there is considerable inconsistency in the literature in the way common terms are used in quality management12,18. This emphasised a need for careful conceptual and operational definitions when undertaking the study.
Quality
It was not necessary to define quality in operational terms, as the study did not seek to measure quality itself. However, to provide context, it is worth noting that Donabedian observed that "quality of care is a remarkably difficult notion to define"19:692. Donabedian clarifies further by describing quality as "a reflection of the values and goals current in the medical care system and in the larger society of which it is part"19:692. Possibly more relevant in healthcare today, Ovretveit states that quality is "fully meeting the needs of those who need the service most, at the lowest cost to the organisation, within the limits and directives set by higher authorities and pur-chasers"20:2. More recently, attempts to define quality emphasise aspects such as patient safety, effectiveness of treatment, efficiency and the need to be patient-centred21.
Quality management
The terms 'quality', 'quality improvement', 'quality assurance' and 'quality management' are frequently confused or used interchangeably. For the purpose of this research 'quality' is an attribute of health services or healthcare. 'Quality management', 'quality assurance' or 'quality improvement' refer to a process of achieving quality. They have slightly different meanings in relation to the stage of the healthcare process that quality intervention occurs13. However, the terms are so frequently used interchangeably for the purpose of this study, the term 'quality management' was used and refers to any process that OTs utilise that has been initiated with the explicit purpose of managing or improving quality of care or service provision.
Use of quality management
Donabedian asserted that a practitioner has a legitimate responsibility to apply knowledge in the management of a 'dysfunctional' state22. This comprises of identifying the dysfunction or diagnosis, making a decision on intervening, choosing objectives or aims of treatment, determining how to achieve those objectives and skilfully executing techniques to achieve the objectives. To ensure quality in this patient care process, a quality framework with effective quality tools and measurement techniques is required.
There is evidence that OTs are involved in quality-management methods. For example, the Gauteng Provincial Health service developed its own standards and audit tools used throughout hospital OT services and other therapy services in Gauteng23,24. These minimum standards and audit tools were developed from within the services and were not tested for validity or reliability. In the Western Cape, a study of OTs in leadership roles revealed that 95.8% of respondents were involved in quality assurance as a leadership function, such as involvement in quality control, documentation control and benchmarking25. In the private sector, therapists at Lifehealthcare use outcome measures and the International Organisation for Standardisation (ISO) quality accreditation in their rehabilitation units as part of quality management26. The board for occupational therapy of the Health Professions Council of South Africa (HPCSA) publishes minimum standards for care27. OTASA provides private practitioners with minimum standards of practice for various aspects of practice28. Despite these initiatives, guidance on how practitioners should implement and monitor standards of practice, measure outcomes, or implement other quality initiatives is scarce, and it is difficult to find comprehensive information on what is being used, where and how.
Ovretveit and Gustafson emphasised the need to evaluate the quality of quality-management programmes29. By describing what is happening, others can understand what is being done and replicate interventions that are working. Within the therapy professions, Kober explored the methodology used for clinical audit in the therapy professions (OT, physiotherapy, clinical psychology and speech therapy) in the United Kingdom (UK)30. This involved examining how topics are selected and described the method being used to evaluate quality, such as case presentations, peer review, adverse/sentinels events, criteria-based audit and patient surveys. However, Kober's research did not cover in detail how therapists analyse information or utilise it to improve practice. Hebert, Thibeault et al31, cite a study carried out in community OT services in Canada looking at quality-evaluation methods used. It was found that performance evaluation, peer evaluation and file inspection were commonly used and that client service evaluation was the least-used method31. Haglund, Hallberg and Pettersson32, carried out a literature review of involvement in quality assurance by OTs. They also sent out a postal questionnaire to all OTs in Sweden working in the field of psychiatric care, this questionnaire covered the aims and goals of OT services, frequency of monitoring and the different methods used. The most common methods of measuring quality were patient interviews and questionnaires. Gnanalingham33 examined how well the audit cycle was being completed in health services in the UK and this included clinical support services (physiotherapy, OT, dietetics).
It was evident from the literature review that previous research on quality management within the profession was limited, even more so in the local context. A description of the current situation in SA would yield further information that could provide direction and inform policy.
METHOD
A quantitative descriptive design was used to investigate the quality-improvement methodology that OTs working in the healthcare field use and were familiar with. The study population was composed of OTs in South Africa working predominantly in a healthcare-related environment, and a convenience sample of all OTs on the OTASA database was used, as well as OTs listed on a public sector mailing list, totaling 1571 OTs. A questionnaire was emailed or posted to the participants. The design of the questionnaire can be seen in Table 1. The questions covered the following information regarding the profession and quality management: which OTs are involved (i.e. characteristics); what knowledge OTs have about the subject; what OTs are doing in relation to the subject (i.e. behaviours), and finally they ask about outcomes. These factors were integrated, in the question layout, with themes drawn from the literature search.
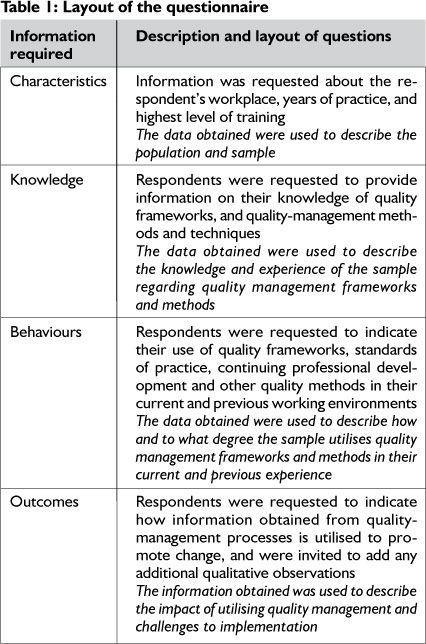
Section 1 consisted of an overview of terms relating to quality management. It was decided to avoid explicit and comprehensive definitions, as one of the aims of the research was to discover the level of knowledge about quality-management concepts.
Sections 2, 3 and 4 reflected the requirements, and therefore, the objectives of the research and are detailed in Table I which describes how the questions were formulated, the layout of the questionnaire and how the responses (data) were used.
Validity
The questionnaire was piloted on 2 OTs with experience in quality management, and feedback was solicited regarding the content. The inputs of the study supervisor and that of an expert in the field of quality management were also used regarding the content. The questionnaire was pre-tested on a convenience sample of 10 OTs requesting their feedback on how well they understood the questionnaire and it's ease of use. Email was considered likely to produce a higher response rate than a postal survey, therefore improving the external validity and generalis-ability of results.
Limitations
For the actual survey, two samples of OTs were used, firstly the questionnaire was circulated to all OTs who are members of OTASA; secondly the questionnaire was circulated to a group of OTs who are known to work in government health services. Using the HPSCA database would have provided the entire study population of practising OTs and therefore been more representative; however it does not contain email addresses and therefore risked a poorer response rate. It should be remembered that any convenience sample, such as the one used, may differ in demographics such as experience or location and not be truly representative of the entire study population.
There was a risk that OTs unfamiliar with or less knowledgeable about quality improvement were less likely to participate, which would have provided a biased result of the extent of participation in quality improvement.
The questionnaire was not standardised and despite piloting, this would have been less reliable than a standardised measurement tool.
Ethical clearance was obtained from the University of South Africa research ethics committee.
RESULTS AND DISCUSSION
The survey questionnaire was sent out to a total of 1571 OTs, of whom 1546 were contacted by email and 25 by post. A reminder was sent 6 weeks after the initial mailing of the survey questionnaire. In total, 80 responses were received, giving a low response rate of just over 5%.
The data elicited from the survey was entered into the EPI Info™ statistical programme. This was used to produce frequency distributions for the responses and make observed/expected comparisons in order to determine associations between some of the variables where this was relevant to the research questions. Although a p-value of <0.05 was taken as significant, conclusive interpretation is cautious for some relationships owing to the small sample size, with 'expected' table values < 5 in some instances.
Respondents' demographic information
The largest group was comprised of OTs in individual private practice (30%; n=24). The largest group of government employees who responded were those working in specialist/academic hospitals (13.8%; n=11). 5% (n=4) worked in Primary Health Care settings and 8.7% (n=7) in district or regional government hospitals. Just over half of the sample had 15 years experience or less (53.9%) and the majority of respondents (57.7%) are basic degree qualified, with the remaining 43.3% having some post-graduate or specialised training.
Quality frameworks, concepts and models
Table II summarises the section of the questionnaire which asked about respondents' knowledge, familiarity with and experience of quality frameworks, concepts and models.
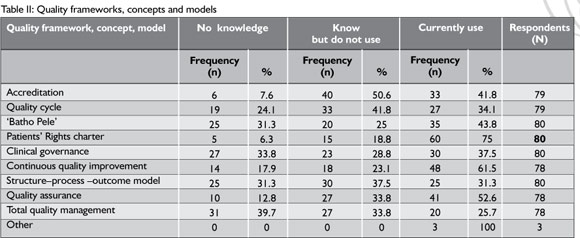
The results showed that almost all OTs make use of, or know about at least one relevant quality concept. The Patients' Rights Charter was broadly familiar and used by most respondents (75%), followed by Continuous Quality Improvement (61.5%), and Quality Assurance (52.6%). Total Quality Management was unfamiliar (39.7% with no knowledge) and least used (25.7%). Almost a third of respondents (31.3%) had no knowledge of the 'Batho Pele' approach to public service delivery. Although only 6.3% of respondents claimed no knowledge of the Patients' Charter, less familiarity with the government-led 'Batho Pele' approach to service quality was possibly due to a considerable proportion of the sample working in the private sector.Table III summarises the results from the section of the questionnaire that asked about other aspects of practice that frame quality, including the use of minimum standards and value statements. Table IV demonstrates more specifically where practitioners source standards for practice.
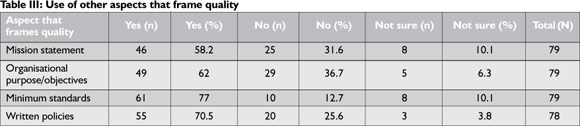
Most practitioners make use of some form of minimum standards (77%), with 70.5% using written policies/procedures to guide services. Although mission statements (58.2%) and the use of objectives or statements of purpose (62%) are less widely used, being mostly confined to OTs working in larger organisations/departments, the use of any of these aspects was associated with using the other aspects, e.g. those using standards of practice were more likely to make use of a mission statement or written policies.
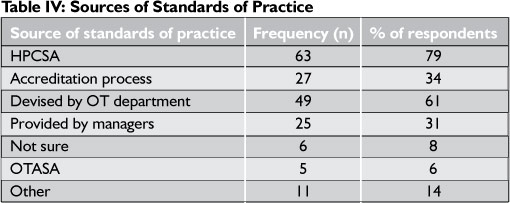
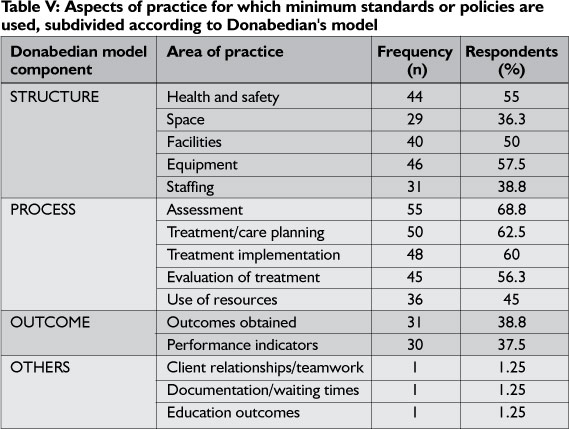
Table IV and Table V reflect the section of the questionnaire that asks where respondents obtained standards to guide their work and for which aspects of service standards are used.
The results show that OTs using standards of practice source them predominantly from within the OT profession, mostly by devising them in their own work place (61 %), or obtaining them from the HPCSA (79%). This is encouraging, as the literature suggests that setting standards from within the profession is fundamentally positive, as standards will be relevant, achievable, and realistic if set by those who understand the challenges and emphasis of the profession. Standards obtained from outside the profession, mainly from accreditation processes, were a source cited by 27%; and respondents cited COHSASA and the National Core Standards. A few respondents (6%) cited OTASA as a source.
Other sources not detailed in Table IV were: other OTs' standards, continuous professional development (CPD) activities, international sources, the policies of their own organisation, and the National Occupational Therapy Forum.
In the structure subsection, the majority of OTs used minimum standards or written policies for equipment (57.5%) followed by health and safety regulations (55%) and financial management structures (53.8%). For process, respondents most commonly used standards for assessment (68.8%), followed by treatment planning (60%) and treatment evaluation (56.3%). The information in Table V suggests that respondents used standards of practice for process aspects of their work more than they do for structure or outcome aspects.
Also evident in the results were associations seen throughout the three components of structure, process and outcome, both within each component and between components. An example of within component was having standards for process aspects of practice being significantly associated with having standards for other aspects of process (e.g. assessment/treatment planning: p<0.0001). An example of between components was an association between outcome and structure (outcomes obtained/facilities: p=0.00l). These results suggest that the three aspects are being used simultaneously to some degree but that standards to guide how, when and where outcomes are measured is an essential area for further investigation.
Quality management activities and methods
Table VI shows respondents' involvement in various quality activities and methods.
Involvement in audit/criteria-based activities
Results as reflected in Table VI suggested that direct observation of another therapists' treatment was frequently used although there is suspicion of misinterpretation by some respondents of the nature of this activity because it was not highly rated during piloting. Consequently, this result was treated with caution. Placing observation of treatment aside, documentation audit was the most utilised audit technique, with 63.9% of respondents reporting that they used it at some time (daily, weekly, monthly or at varying intervals). Accreditation was used at some time by just under half (48%) of the sample.
A relationship was observed between documentation audit and some quality models and frameworks, namely the quality cycle (p<0.0001), Batho Pele approach (p=0.012), continuous quality improvement (p=0.004) and quality assurance (p=0.013). This suggested that use of documentation auditing is associated with knowledge of quality models. Documentation audits are a useful starting point for quality activities, and the quality of documentation is considered to correlate with the overall quality of care34. It would be judicious to support and encourage this quality activity, although at present no standardised documentation-auditing tools exist for OT.
Involvement in professional/clinical development activities
Of quality-management methods related to professional development, CPD was highly prominent. From Table VI, it can be seen that all respondents had knowledge of CPD or participated in it at some time.This is unsurprising given that participation in CPD is a compulsory requirement for continued registration in South Africa. Just under half of OTs made use of clinical guidelines/protocols on a daily basis (46.8%) and there was no relationship between use of this method and any particular quality models and standards of practice. This suggests that for the use and awareness of clinical guidelines there exists a universality that is not related to knowledge of specific areas of quality management.
Many respondents were aware of EBP but were not putting it to use (34.3%), with only 30% reporting practice based on evidence on a daily basis. The results also indicated that courses/workshops were the most used source of clinical guidelines and/or treatment protocols. In reality it can be challenging to implement EBP effectively35 and these results combined with an increasing emphasis on EBP in healthcare suggests that this will benefit from continued and increasing attention from within the profession locally.
Involvement in quality methods related to quality models and frameworks
For quality methods that are directly associated with quality frameworks and models, quality meetings stand out as the most utilised (65%). An association was seen between using quality meetings and the use of standards. There also existed a high level of awareness of patient satisfaction surveys and individual performance management. There was also high awareness, if less use, of other methods such as benchmarking, patient-satisfaction surveys and adverse event monitoring. These latter methods, unsurprisingly, were not so well utilised by individual private practitioners and this highlights some of the difficulties that practitioners working alone face when implementing quality activities. OTs often work in relative professional isolation, both in government and in private practice, and these practitioners may find it more difficult to implement quality-improvement measures or quality-management techniques.
From the results, a number of recommendations was made and conclusions drawn.
RECOMMENDATIONS
Recommendations for occupational therapy practice
♣ Increased standardisation for documentation, and its auditing, should be promoted and advocated.
♣ The HPSCA professional board already sets broad minimum standards and should remain the guiding mechanism for standards. OTs should be encouraged to work within the profession for guiding standards, principles and procedures, particularly with regards to profession-specific processes such as treatment and care planning.
♣ Quality meetings, for those in a position to meet, are a potentially useful starting point for quality activities and should be encouraged.
♣ Quality management to be included in or emphasised in OT curricula. This should be incorporated into their clinical field-work practicals.
♣ Participation in quality management to be incorporated into job descriptions and linked with performance-related benefits where this is not yet done.
♣ Specific support and information to be available for OTs who work in relative professional isolation to enable them to participate more widely in quality management. For example OTs in private practice could be encouraged to form partnerships or small group forums for quality activities.
Recommendations for further research
♣ An investigation could be done to research the gap between the perception of knowledge of EBP and its implementation in practice.
♣ Forms of adverse-events monitoring, such as health and safety monitoring, need to be explored for relevance and further encouraged and developed, particularly in a climate of increasing litigation for both clinical and non-clinical events.
♣ Research related to the development of OT-specific standardised auditing tools could be done. This could include minimum standards for documentation.
♣ Barriers to implementing quality management need to be explored further to ensure that quality frameworks and methods used are effective in promoting genuine and tangible change for the better.
♣ A quality framework for occupational therapy could be developed.
CONCLUSION
This research revealed that occupational therapists have awareness of quality management methodologies, in particular the use of minimum standards, accreditation, auditing and continuing professional development, yet there appear to be challenges to putting knowledge of quality management into practice effectively. In order to keep pace with changes to healthcare policy, priorities and health systems, quality management must be a dynamic process. This research has provided some insights into the current situation in South Africa, but it is also recommended that monitoring of how quality management is carried out within the profession is continued. This should be done alongside continued efforts to promote and maintain quality through the application of quality management principles, and development and application of quality management techniques in occupational therapy practice.
REFERENCES
1. McColl, M & Quinn, B. A quality assurance method for community occupational therapy. Canadian Journal of Occupational Therapy, 1985; 39(9):570-577. [ Links ]
2. Koning, H, Verver, J, van den Heuvel, J, Bisgaard, S, Does, R. Lean Six Sigma in Healthcare. Journal for Healthcare Quality, 2006; 22(8):4-11. [ Links ]
3. Mainz, J. Defining and classifying clinical indicators for quality improvement. International Journal for Quality in Health Care, 2003; 15(6): 523-530. [ Links ]
4. Malby, B (Ed.) Clinical audit for nurses and therapists. London: Scutari Press, 1995. [ Links ]
5. Berger, J, Hassim, A, Heywood, H, Honermann, B, Krynauw, M, Rugege, U. A guide to the National Health Act. 2013. Cape Town: Siber. [ Links ]
6. Graham, N. Quality in healthcare. Gaithersburg: Aspen, 1995. [ Links ]
7. Muller, L & Flisher, A. Standards for the mental health care of people with severe psychiatric disorders in South Africa: Part l. Conceptual issues. South African Psychiatric Review, 2005; 8:140-145. [ Links ]
8. Ovretveit, J. "What are the advantages and limitations of different quality and safety tools for health care?" Copenhagen: WHO Regional Office for Europe (Health Evidence Network report). 2005. <http://www.euro.who.int/document/e87577.pdf> (15 Feb 2009) [ Links ]
9. Grol, R, Berwick, D, Wensing, M. On the trail of quality and safety in healthcare. British Medical Journal, 2008; 336:74-76. [ Links ]
10. Mant, J. Process versus outcome indicators in the assessment of quality in health care. International Journal for Quality in Health Care, 2001; 13(6): 475-480. [ Links ]
11. Beukes, S. The accreditation of vocational assessment areas: Proposed standard statement and measurement criteria. South African Journal of Occupational Therapy, 2011; 41(3): 42-49. [ Links ]
12. Norman, I & Redfern, S. What is audit? In: Kogan M, Redfern S. Buckingham. Making use of clinical audit - A guide to practice in the health professions. Open University Press, 1995: 1-20. [ Links ]
13. Moullin, M. Delivering excellence in health and social care. Buckingham: Open University Press, 2002. [ Links ]
14. Sale, D. 2005. Understanding clinical governance and quality assurance: Making it happen. London: Macmillan Press. [ Links ]
15. Clinical Governance. [s.a]. Netcare. From: http://www.netcare.co.za/2391/clinical-governance (accessed 3rd September 2010). [ Links ]
16. Batho Pele - Principles. [s.a.]. National Department of Public Service and Administration. From: http://www.dpsa.gov.za/batho-pele/Principles.asp (accessed 8th September 2010). [ Links ]
17. Walshe, K. Pseudoinnovation: the development and spread of healthcare quality improvement methodologies. International Journal for Quality in Healthcare, 2009; 21(3):153-159 [ Links ]
18. Arah, O, Westert, G, Hurst, J, Klazinga, N. A conceptual quality framework for the OECD Health Care Quality Indicators Project. International Journal for Quality in Health Care, 2006; 18 (Suppl. 1):5-13. [ Links ]
19. Donabedian, A. Evaluating the quality of medical care. Milbank Quarterly, 2005, 83(4): 691 -729, reprinted from Milbank Memorial Fund Quarterly, 1966; 44(3): 166-203. [ Links ]
20. Ovretveit, J. Health service quality - an introduction to quality methods for health services. Oxford: Blackwell, 1992. [ Links ]
21. Minkman, M, Ahaus, K, Huijsman, R. Performance improvement based on integrated quality management models: what evidence do we have? - A systematic literature review. International Journal for Quality in Health Care, 2007; 19(2):90-104. [ Links ]
22. Burns, N & Grove, S. The practice of nursing research: conduct, critique and utilization. St. Louis: Elsevier, 2005. [ Links ]
23. Foote, H, Lamont, S, Burger, E & Leishman, A. Introduction of a quality assurance programme in Gauteng health hospital occupational therapy services. South African Journal of Occupational Therapy, 2006; 36(1): 6-10. [ Links ]
24. Gauteng Department of Health. Revised standards and audit tools for health professionals. Gauteng: Department of Health, 2007. [ Links ]
25. Mostafa, M. Perspectives on occupational therapy leadership functions in clinical practice. MOT Dissertation, University of Stellenbosch, 2007. [ Links ]
26. "Life Healthcare: Funders - enhancing the care continuum. Life Rehabilitation. 2013. <http://www.lifehealthcare.co.za/hospitals/Rehabilitation/Life_Rehabilitation_ Funders.htm> (3 Mar 2013) [ Links ]
27. Health Professions Council of South Africa. Standards of Practice for Occupational Therapists. Form 265. Pretoria: HPCSA, 2006. [ Links ]
28. "Special interest groups - the private practice sector."OTASA. 2012. <http://www.otasa.org.za//members-only/interest_groups/instopp.html> (8 Jun 2012) [ Links ]
29. Ovretveit, J & Gustafson, D. Evaluation of quality improvement programs. Quality and Safety in Healthcare, 2010; 1:270-275. [ Links ]
30. Kober, A. The nature of clinical audit and progress made. In: Kogan M, Redfern, S. Making use of clinical audit - A guide to practice in the health professions. Buckingham: Open University Press, 1995: 55-80. [ Links ]
31. Hebert, M, Thibeault, R, Landry, A, Boisvenu, M & Laporte, D. Introducing an evaluation of community-based occupational therapy services: A client-centred practice. Canadian Journal of Occupational Therapy, 2000; 67(3):146-154. [ Links ]
32. Haglund, L, Hallberg, I, Pettersson, M. Psychiatric occupational therapy service - quality assurance. Nordic Journal of Psychiatry, 2004; 58:403-407. [ Links ]
33. Gnanalingham, J, Gnanalingham, M & Gnanalingham, K. 2001. An audit of audits - are we completing the cycle? Journal of the Royal Society of Medicine, 2001; 94:288-289. [ Links ]
34. Corben, V The Buckingham nursing record audit tool: a unique approach to documentation. Journal of Nursing Management, 1997; 5:289-293. [ Links ]
35. Buchanan, H, Jelsma, J, Siegfried, N. 2009. Implementing evidence-based practice in the Western Cape. Conference presentation. Occupational Therapy Association of South Africa Congress/2009. [ Links ]
 Correspondence:
Correspondence:
Helen Robinson
msinsi@mweb.co.za
APPENDIX
Survey on quality management in occupational therapy in health services
The survey is divided into 4 short sections. Some of the concepts used in this study that you might be familiar with under a different name will be explained first. After each question there are a number of answers to choose from. Please indicate your answer by typing or writing an ‘x’ in the relevant space. Where indicated in the question you may choose more than one answer if it is applicable to you.


















