Servicios Personalizados
Articulo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en Google
Similares en Google
Compartir
South African Journal of Occupational Therapy
versión On-line ISSN 2310-3833
versión impresa ISSN 0038-2337
S. Afr. j. occup. ther. vol.43 no.3 Pretoria mar. 2013
SCIENTIFIC ARTICLES
Towards evidenced-based practice - A systematic review of methods and tests used in the clinical assessment of hypotonia
Pragashnie Naidoo
B.OccTh (UDW), M.OccTh (UKZN), CAMAG (ABIME). Lecturer, Discipline of Occupational Therapy, School of Health Sciences, University of Kwa-Zulu Natal
ABSTRACT
BACKGROUND: There is much contention about the measures used for the assessment of hypotonia in children and in order to determine what is available within the scientific literature, a systematic review to provide a critical appraisal of the studies describing the methods and tests used in the clinical assessment of hypotonia in children was undertaken.
METHODS: A systematic process in searching and identifying relevant literature was followed. An analysis and synthesis of the literature was undertaken by two reviewers, with a specific review question, search strategy and inclusion criteria.
RESULTS: A hierarchy of the levels of evidence is reported in this paper Twelve studies met the inclusion criteria, and were evaluated according to the critical review form for quantitative studies developed at McMaster University Occupational Therapy Evidence-Based Practice Research Group. A quality score was also provided in addition to the important characteristics of the included studies.
CONCLUSIONS AND IMPLICATIONS OF KEY FINDINGS: There appeared to be a paucity of scientific literature that documented the objective assessment of hypotonia in children. This review has thus identified the need for more studies with greater methodological rigour in order to determine best practice with respect to the methods used in the assessment of low muscle tone in the paediatric population.
Key words: clinical assessment; hypotonia, low muscle tone, systematic review.
BACKGROUND
A key competency in providing health care in any setting is the appraisal of relevant research and the application of evidence into practice. Evidence based practice (EBP) has gained momentum over the last decade. Prior to its introduction, clinicians tended to base their decisions on professional expertise and client information with little attention being given to what the literature, specifically the research literature, reported1 thus seems imperative that the evidence from the literature be located, appraised and interpreted in order to assist the clinician to apply the evidence to practice. Additionally, clinicians are challenged to apply evidence from the scientific literature to help them determine, not only the appropriateness of selected methods and choices in client assessment, but also appropriate methods of for the management of the client. Drawing on research as a component of decision making, reduces bias and empowers both the clinician and client in making informed decisions based on strong evidence thereby ensuring good practice2.
The assessment of hypotonia has been a contentious issue over the last few decades. Anecdotal evidence suggests that children have been "labeled" with the diagnosis of hypotonia, without there being objective evidence to support the findings. The author has experienced this in clinical practice. A search of the scientific literature reflected a paucity of research to guide the assessment of hypotonia in children. A systematic review thus seemed a logical step not only to locate all relevant literature to guide practice in this area, but also to identify possible gaps to inform future research.
OBJECTIVES
The objective of this study was to identify and appraise existing assessments reported in the literature that could be used by clinicians (occupational therapists, physiotherapists and paediatricians) to detect hypotonicity in children and to the identify any gaps that would inform future research into the assessment of hypotonia in children.
METHODS
Design: This study followed the design of a systematic review, without meta-analysis. The author developed a systematic review protocol which was peer-reviewed by a colleague trained in systematic reviews, prior to the data collection phase.
Instruments/Tools used in this Systematic Review
1. The Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) Statement3 was used to help the author to ensure transparent and complete reporting of the findings of the systematic review. The PRISMA Statement is an evidenced-based minimum set of items for reporting systematic reviews. It consists of a 27-item checklist and a four-phase flow diagram, illustrating the flow of information through the different phases of a systematic review. The checklist and flow diagram were both used in reporting the findings in this review.
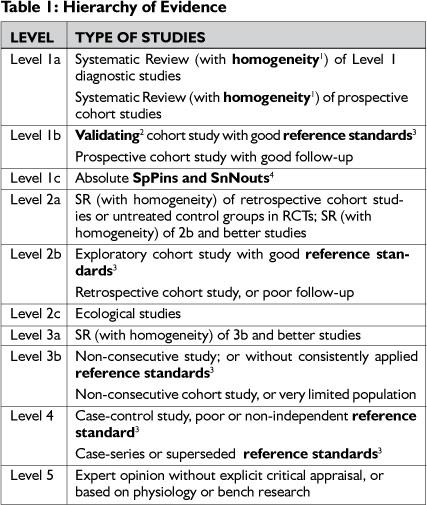
2. The Oxford Centre for Evidence-based Medicine (OCEBM) levels of Evidence4 (2009 version): This hierarchy was used as a first step to classify the research articles into categories based on the strength of the design for answering the review question (refer to Table 1).The 2009 version of the tool4 was utilised over the 2011 version5 due to its more descriptive presentation (i.e. a total of 5 sub-categories, within the description of the 5 levels). Whilst the levels of evidence approach to evaluation is attractive in part because of its apparent simplicity, more careful reading around levels of evidence shows that determining the appropriate level of evidence represented by a given research study requires both an assessment of the quality of the work as well as the research design6,7,8. Hence a critical appraisal tool was also utilized.
3. The Critical Review Form for Quantitative Studies developed by the McMaster University Occupational Therapy Evidence-Based Practice Research Group9 was used to assess the methodological quality of each of the studies. It comprises ten questions related to the methodological quality of each study, related to the following components, viz. study purpose, literature and justification, design, sampling, outcomes, intervention, results, conclusions and implications. The reviewer commits to a yes/no response for each of the questions related to these components.
4. Assessment of Multiple Systematic Reviews (AMSTAR)10 Tool: This tool was developed to assess the methodological quality of a systematic review. It consists of 11 items and has good face and content validity for measuring the methodological quality of systematic reviews10. The author uses this tool at the end of this paper in an attempt to describe the strengths and limitations of this review.
Criteria for considering studies for this review
Types of studies: All studies that described the process, methods, and tests/assessments used to detect/diagnose low muscle tone (hypotonia) were included as the clinical assessment of low muscle tone is not diagnosis- dependent. All studies that were classified between levels 1-4 on the OCEBM Levels of evidence4 will be considered for the critical appraisal. Level 5 was excluded as these included studies that were expert opinion and not based on empirical research. Studies describing or determining the effectiveness of therapy or intervention strategies for treating hypotonia were excluded.
Types of participants: Studies that included children (0-12 years) who presented with low muscle tone were included, irrespective of the underlying diagnosis. Studies had to include clinicians within the disciplines of occupational therapy, physiotherapy (physical therapy) and paediatrics (paediatricians and paediatric neurologists).
Types of intervention: Studies in which methods and/or tests were used in the assessment and diagnosis of low muscle tone in the paediatric population by clinicians as well as the most valid clinical criteria or characteristics that were used in the diagnosis of low muscle tone in the paediatric population were included.
Search methods for identifying studies: The following electronic databases were searched from their inception until January 2013: MEDLINE, CINAHL, ERIC, ScienceDirect, Google Scholar, Physiotherapy Evidence Database (PEDro), Health Source: Nursing and Academic Edition and Academic Search Complete (EBSCo). The following limits were set: articles had to be full text and in English. The following search strings were utilised: (defin* OR assess* OR test OR evaluat*) and (hypotonia OR low muscle tone)and (children).
Data collection process: Each study was assessed and rated independently by two reviewers, one of which was the author (primary reviewer), and a secondary reviewer, for their quality and suitability. Titles and abstracts were screened independently by each reviewer and those that were not relevant were removed. The full text of the remaining articles, were then examined and the inclusion criteria used to identify relevant articles.
Synthesis of results: Studies were individually rated by each reviewer, with the following process:
1) Classifying the strength of the study designs: Studies were categorised based on the strength of the design according to the OCEBM levels of evidence4 (refer to Table 1).
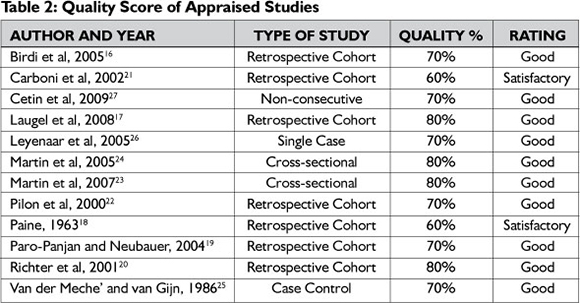
2) Determining the quality of the individual studies6: Each reviewer then reviewed the ten criteria outlined in the Critical Review Form for Quantitative Studies9 for assessing the methodological quality of the studies, with yes/no responses. For every yes response a score of one was allocated and a percentage calculated at the end of scoring. This is in keeping with other studies that used appraisal tools to determine a quality score11. The grading of the quality assessment checklist score is described as follows; 0-40% (poor); 40%-70% (satisfactory) and 70-100% (good) (refer to Table 2).
3) Identification of important characteristics of individual studies6: Each reviewer extracted characteristics of the included articles, which outlined the year of the study, study design, participants/ subjects, intervention and outcomes of the studies. These are described in Table 3 on pages 4 and 5.
The reviewers then collated their findings. Disagreements were discussed until consensus was reached.
RESULTS
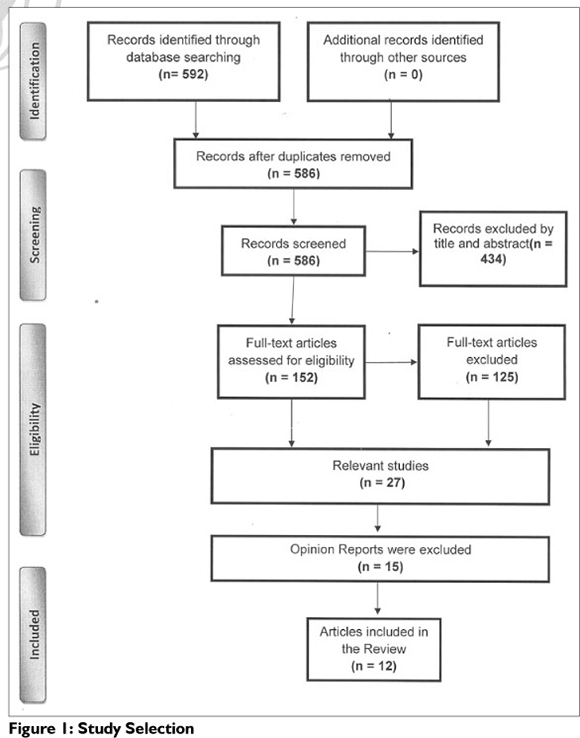
A total of 592 citations were initially identified (Figure 1 on page 6). After removing duplicates, there were 586 potentially relevant articles. An additional 125 articles were excluded from the title and abstract due to the fact that these studies focussed on intervention for children with hypotonia12,13, developmental outcomes for infants with hypotonia14 and assessment of the spectrum of muscle tone.15 Of the remaining 461 articles only 27 articles fulfilled the inclusion criteria, as outlined above. Of these 27 articles, 15 were classified as Level 5 on the OCEBM levels of evidence, based on reading of the full text article, and were excluded from the critical appraisal process, as these articles were based on expert opinion. The remaining 12 articles were exposed to the critical appraisal process. Full texts of these articles 16-27 were re-read by the reviewers, to determine once more if the studies met the inclusion criteria. Discrepancies were discussed until consensus was reached.
Quality score and important characteristics of included studies: Following extraction, each included article was appraised and a quality score calculated. These quality scores based on the critical review form for quantitative studies9 is described in Table 2.Ten out of the 12 included studies achieved a good rating. Additionally, the important characteristics of the included studies as suggested by Domholdt6, were extracted (refer to Table 3). No systematic reviews were identified. Five retrospective cohort studies14-18, two longitudinal studies19,20, two exploratory studies21,22, one case control study23, one case study24 and one non-consecutive cohort study25 were accessed.
DISCUSSION
With respect to the clinical examination and tests and methods used in the assessment of low muscle tone, in four of the retrospective studies16,17,19,20, authors aimed at assessing the reliability of the first physical examination and the contribution of different procedures in the assessment process used to diagnose hypotonia. Findings indicated that a good medical history and proper clinical observation including, a neurologic examination, enabled health practitioners to detect hypotonicity in the majority of children. Clinical observation was found to be critical to the accurate evaluation of these children. They further added that the selective use of specific molecular and genetic tests that is based on the initial clinical evaluation, is likely to be more time and cost effective. With respect to clinical characteristics, Carboni et al21, identified a positive correlation between hypotonia and joint laxity, whilst Martin et al23,24, gained consensus amongst paediatric therapists on the clinical characteristics such as decreased strength, decreased activity tolerance, delayed motor skills development, rounded shoulder posture, leaning onto supports, hypermobile joints, increased flexibility and poor attention and motivation which contributed towards a diagnosis of hypotonia. No statistically significant or clinically meaningful relationships between hypotonia and motor development were found in the study by Pilon et al22. Leyenaar et al26, used a case study of a 5-month old child to describe an approach to diagnosis of hypotonia in infancy. Authors of a paper on hypotonia and reflexes25, based their judgements on a case control study in which they determined that that long-latency stretch reflexes play no role in the clinical assessment of "normal tone" and that passive movements during the clinical examination are of great value, but only to detect spasticity or rigidity. Whilst a number of opinion papers have highlighted the importance of the physical or clinical examination in the evaluation of hypotonia32,40-42,only a few research studies, most of which were retrospective, were found to provide scientific evidence that supported this16,17,19,20.
In summary, the following were highlighted from this review as being useful in the assessment of hypotonia in children; a good medical history and proper initial clinical observation, a neurologic examination, decreased strength, decreased activity tolerance, delayed motor skills development, rounded shoulder posture, leaning onto supports, hypermobile joints, increased flexibility and poor attention and motivation. Albeit limited, these indicators have contributed to describing the value of clinical assessment in the diagnosis of hypotonia as well as related characteristics.
STRENGTHS AND LIMITATIONS OF THE REVIEW
The author used the AMSTAR tool10 in an attempt to critically appraise and identify the strengths and limitations of this systematic review.
The strengths of this review can be summarized as follows:
♣ An a priori design was developed and peer reviewed prior to the initiation of the study
♣ The author followed a clearly defined process for searching and identification of relevant articles
♣ There were duplicate study selection and data extraction. Two independent reviewers were involved in the rating of the studies
♣ A consensus procedure for disagreements was in plac
♣ The types of participants and interventions were clearly defined
♣ The data collection process and methods had been systematically indicated
♣ The studies were critically appraised with a quality score being allocated
♣ Pertinent information was extracted and tabulated (characteristics of included studies) in an attempt to further describe the appraised studies
A limitation within this review was that the review question was specifically targeted at assessment methods, tests and clinical characteristics that are used to detect hypotonia. However, given that the words "methods" and "tests" were used without clarity on this being clinical "tests" and "methods", the search revealed studies that utilised neuro-imaging, genetics, metabolic screening tests etc. This may also be an indication of the paucity of literature and lack of scientific evidence on assessments with high sensitivity and specificity, or limitations in the search strategy. Notwithstanding this, these tests and methods should have perhaps been included as part of the exclusion criteria for this review. Given that there were no RCT's available, a meta-analysis was not conducted, but the identified studies were still exposed to a critical appraisal as described in this review.
AUTHOR'S CONCLUSIONS
This systematic review aimed to determine the methods, tests and clinical criteria that are used in the assessment and diagnosis of hypotonia in the paediatric population by occupational therapists, physiotherapists, paediatricians and paediatric neurologists. The major conclusion from this systematic review is that there is limited scientific evidence to indicate the most valid and reliable methods and tests that assist in the clinical evaluation of hypotonia in the paediatric population. Only two studies investigated characteristics or criteria that may be used in drawing conclusions about a child's hypotonic status, one of which was a follow-up study of the original one that attempted to highlight characteristics associated with low muscle tone. These results may be clinically important when looking at cost and the associated risk of invasive and unnecessary testing with diagnostic tools20,26,34 as indicated in the literature. Whilst the review does indicate the gains made in the last decade, especially with regard to the retrospective studies mentioned here, there remains insufficient scientific evidence, in the form of systematic reviews and randomised control trials in answering the clinical question adequately.
Implications for Practice and Research
This review highlights the gaps in the literature related to the evidence for assessment of hypotonia in the paediatric population. Objective assessment instruments that are both sensitive and specific in detecting hypotonicity in children are needed. This review may assist a multi-disciplinary team by providing information on the available evidence in assessing hypotonia in children. This review provides initial data and evidence on the gaps so that the scientific community may move towards conducting studies with greater methodological rigor in order to determine best practice with respect to assessment methods and in identifying criteria in the assessment of low muscle tone in the paediatric population.
ACKNOWLEDGMENTS
The author would like to acknowledge Mrs d Mahlangu for her assistance in the review process, Prof P Brysiewicz, University of KwaZulu-Natal for peer review of the proposal, Ms S Titus, University of Western Cape, Dr H buchanan, University of Cape Town and Dr T Kredo, South African Cochrane Centre for their inputs on systematic reviews and Prof RWE Joubert for her supervision of the study.
CONFLICT OF INTEREST
The PhD from which this paper has emanated is funded by the Medical Research Council of South Africa in terms of the National Health Scholars Programme from funds provided for this purpose by the National Department of Health.
REFERENCES
1. Hoffman T, Bennett S & Del Mar C. 2010. Introduction To Evidence-Based Practice. In: Hoffman T, Bennett S & Del Mar C, editors. Evidence-Based Practice Across The Health Professions. Sydney: Elsevie20r, 2010. [ Links ]
2. Graham ID, Logan J, Harrison MB, Straus SE, Tetroe J, Caswell W & Robinson N. Lost In Knowledge Translation: Time For A Map? Journal Of Continuing Education In The Health Professions, 2006; 26:13-24. [ Links ]
3. The PRISMA Statement. <http://www.prisma-statement.org> (23 June 2013). [ Links ]
4. The Oxford Centre For Evidence-Based Medicine Levels Of Evidence, March 2009. <http://www.cebm.net> (30 September 2011). [ Links ]
5. The Oxford 2011 Levels Of Evidence. 2011. <http://www.cebm.net> (30 September 2011). [ Links ]
6. Domholdt E. Rehabilitation Research: Principles And Applications Missouri, Elsevier Saunders,2005. [ Links ]
7. Sharma S. Levels Of Evidence. Evidence-Based Ophthalmology, 2011;12:9-10. [ Links ]
8. Wright KB. Researching Internet-Based Populations:Advantages And Disadvantages Of Online Survey Research, Online Questionnaire Authoring Software Packages, And Web Survey Services. Journal Of Computer-Mediated Communication, 2005;10. [ Links ]
9. Roman NV & Frantz JM. The prevalence of intimate partner violence in the family: a systematic review of the implications for adolescents in Africa. Family Practice. Advance access published 30 January 2013. [ Links ]
10. Shea BJ, Grimshaw JM, Wells GA, Boers M, Andersson N. et al. Development of AMSTAR: a measurement tool to assess the methodological quality of systematic reviews. BMC Medical Research Methodology, 2007;7:1-7. [ Links ]
11. Law M, Stewart D, Pollock N, Letts L, Bosch J & Westmorland M. Quantitative Review Form Guidelines, 1998. <http://wwwfhs. mcmaster.ca> (06 August 2013) [ Links ]
12. Mintz-Itkin R, Lerman-Sagie T, Zuk L, Itkin-Webman T & Davidovitch M. Does Physical Therapy Improve Outcome In Infants With Joint Hypermobility And Benign Hypotonia. Journal Of Child Neurology, 2009; 24:714-719. [ Links ]
13. Vaivre-Douret L, Ennouri K, Jrad I, Garrec C & Papiernik E. Effect Of Positioning On The Incidence Of Abnormalities Of Muscle Tone In Low-Risk, Preterm Infants. European Journal Of Paediatric Neurology, 2004:21-24. [ Links ]
14. Strubhar AJ, Meranda K & Morgan A. Outcomes Of Infants With Idiopathic Hypotonia. Pediatric Physical Therapy, 2007; 19:227-235. [ Links ]
15. Kathrein JE. Interrater Reliability In The Assessment Of Muscle Tone Of Infants And Children. Physical And Occupational Therapy In Pediatrics, 1990;10:27-41. [ Links ]
16. Birdi K, Prasad AN & Prasad C. The Floppy Infant: Retrospective Analysis Of Clinical Experience (1990-2000) In A Tertiary Care Facility. Journal Of Child Neurology, 2005;20:803-808. [ Links ]
17. Laugel V Cosse'e M, Matis J, De Saint-Martin A, Echaniz-Laguna A, Mandel J, Astruc D, Fischbach M & Messer J. Diagnostic Approach To Neonatal Hypotonia: Retrospective Study On 144 Neonates. European Journal Of Pediatrics, 2008;I67: 517-523. [ Links ]
18. Paine RS. The Future Of The Floppy Infant: A Follow-Up Study Of 133 Patients. Developmental Medicine And Child Neurology, 1963;5:115-124. [ Links ]
19. Paro-Panjan D & Neubauer D. Congenital Hypotonia: Is There An Algorithm? Journal Of Child Neurology, 2004;19:439-442. [ Links ]
20. Richter LP Shevell MI & Miller SP Diagnostic Profile Of Neonatal Hypotonia: An 11 -Year Study. Pediatric Neurology, 2001 ;25:35 -37. [ Links ]
21. Carboni P Pisani F Crescenzi A. & Villani C. Congenital Hypotonia With Favourable Outcome. Pediatric Neurology, 2002;26:383-386. [ Links ]
22. Pilon JM, Sadler GT & Bartlet DJ. Relationship Of Hypotonia And Joint Laxity To Motor Development During Infancy. Pediatric Physical Therapy, 2000:10-15. [ Links ]
23. Martin K, Kaltenmark T, Lewallen A, Smith C & Yoshida A. Clinical Characteristics Of Hypotonia: A Survey Of Pediatric Physical And Occupational Therapists. Pediatric Physical Therapy, 2007;19:217-226. [ Links ]
24. Martin K, Kirschner A, Deming K, Gumbel R & Voelker L. Characteristics Of Hypotonia In Children: A Consensus Opinion Of Pediatric Occupational And Physical Therapists. Pediatric Physical Therapy, 2005;17:275-282. [ Links ]
25. Van Der Meche' FGA & Van Gijn J. Hypotonia: An Erroneous Clinical Concept. Brain, 1986;109:1169-1178. [ Links ]
26. Leyenaar J, Camfield P & Camfield C. A Schematic Approach To Hypotonia In Infancy. Paediatric Child Health, 2005;10:397-400. [ Links ]
27. Cetin E, Cuisset JM, Tiffreau V Valle' L, Hurtevent JF & Thevenon A. The Value Of Elecromyography In The Aetiological Diagnosis Of Hypotonia In Infants And Toddlers. Annals Of Physical And Rehabilitation Medicine, 2009;52:546-555. [ Links ]
28. Gowda V, Parr J & Jayawant S. Evaluation Of The Floppy Infant. Paediatrics And Child Health, 2007;18. [ Links ]
29. Peredo DE & Hannibal MC. The Floppy Infant: Evaluation Of Hypotonia. Pediatics In Review, 2009;30. <http://pedsinreview.aappublications.org> (02 August 2011). [ Links ]
30. Prasad AN & Prasad C. Genetic Evaluation Of The Floppy Infant. Seminars In Fetal & Neonatal Medicine, 2011;16:99-108. [ Links ]
31. Van Toorn R. Clinical Approach To The Floppy Child. CME, 2004;22:449-455. [ Links ]
32. Johnston HM. Editorial: The Floppy Weak Infant Revisited. Brain And Development, 2003;25:155-158. [ Links ]
33. Harris SR. Congenital Hypotonia: Clinical And Developmental Assessment. Developmental Medicine And Child Neurology, 2008;50:889-892. [ Links ]
34. Jan MS. The Hypotonic Infant: Clinical Approach. Journal Of Pediatric Neurology, 2007;5:181-187. [ Links ]
35. Bodensteiner JB. The Evaluation Of The Hypotonic Infant. Seminars In Paediatric Neurology, 2008; 15:10-20. [ Links ]
36. Curran A & Jardine P The Floppy Infant. Current Paediatrics, 1998;8:37-42. [ Links ]
37. Walton JN. The Floppy Infant. Cerebral Palsy Bulletin, 1960;2:10-18. [ Links ]
38. Lisi EC & Cohn RD. Genetic Evaluation Of The Pediatric Patient With Hypotonia: Perspective From A Hypotonia Specialty Clinic And Review Of The Literature. Developmental Medicine And Child Neurology, 2011;53:586-599. [ Links ]
39. Igarashi M. Floppy Infant Syndrome. Journal Of Clinical Neuromuscular Disease, 2004;6. [ Links ]
40. Miller VS, Degado M & lannaccone ST. Neonatal Hypotonia. Seminars In Neurology, 1993;13:73-83. [ Links ]
41. Crawford TO. Clinical Evaluation Of The Floppy Infant. Pediatric Annals, I992;2I: 348-354. [ Links ]
42. Zellweger H.The Floppy Infant: A Practical Approach. Helv Paediatr Acta, 1983;38:301-306. [ Links ]
 Correspondence:
Correspondence:
Pragashnie Naidoo
naidoopg@ukzn.ac














