Servicios Personalizados
Articulo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en Google
Similares en Google
Compartir
South African Journal of Psychiatry
versión On-line ISSN 2078-6786
versión impresa ISSN 1608-9685
S. Afr. j. psyc. vol.21 no.1 Pretoria feb. 2015
http://dx.doi.org/10.7196/sajp.576
ARTICLE
Depressive symptoms in community-dwelling persons aged >60 years in Inanda, Ntuzuma and KwaMashu in eThekwini, KwaZulu-Natal
J NarainsamyI; J ChippsII; B CassimIII
IMB ChB, FCP (SA); Department of Geriatrics, Nelson R Mandela School of Medicine, University of KwaZulu-Natal, Durban, South Africa
IIBSc, MPH, PhD; School of Nursing and Public Health, University of KwaZulu-Natal, Durban, South Africa
IIIMB ChB, FCP (SA), MD, FRCP (UK); Department of Geriatrics, Nelson R Mandela School of Medicine, University of KwaZulu-Natal, Durban, South Africa
ABSTRACT
BACKGROUND: Physical and psychological ailments increase with age; while the physical ailments are well documented, mental health issues have received less attention.
OBJECTIVE: To determine the prevalence of depressive symptoms and associated risk factors in individuals aged >60 years living in a low-resource peri-urban area in South Africa.
METHODS: Secondary analysis was performed on data obtained from a primary study conducted to determine the influence of socioeconomic and environmental factors on the health status and quality of life in older persons living in the Inanda, Ntuzuma and KwaMashu (INK) area. The Center for Epidemiologic Studies Short Depression Scale (CES-D 10) was used to screen for depressive symptoms in the week preceding the interview, and respondents were categorised as having no (score <10), mild (10 - 14), or severe (>14) depressive symptoms. Risk factor associations were tested using Pearson's χ2 tests and logistic regression.
RESULTS: There were 1 008 respondents (mean (standard deviation) age 68.9 (7.4) years), of whom 503 (49.1%) did not meet criteria for depressive symptoms. Of the 505 (50.1%) respondents who met the CES-D 10 criteria for depressive symptoms, 422 (41.9%) had mild and 83 (8.2%) had severe depressive symptoms. In the univariate analysis, significant associations were found with age (p=0.011), household size (p=0.007), income (p=0.033), disability (p=0.001), nutritional status (p<0.001), the inability to count on family (p=0.008) and lack of mastery (p<0.001). In direct binary logistic regression, there were significant associations with lack of mastery (p<0.001), inability to count on family (p=0.027), malnutrition (p<0.001) and household size (p=0.024).
CONCLUSION: This study highlights the high prevalence of depressive symptoms in the elderly in the INK area, and the need to promote successful ageing of the elderly population in this area.
The number of people over 60 years old is expected to double by 2025 worldwide, and to reach 2 billion by 2050.[1] The elderly population faces unique stressors that contribute to an increase in disease, affecting their biopsychosocial wellbeing. The South African (SA) older population is faced with inherent stressors that increase their predisposition to depression and other health issues.[2] The HIV/ AIDS pandemic and other communicable diseases, especially tuberculosis, have placed an enormous financial and emotional burden on the elderly population, who may be either infected or affected. Older people often support entire households and take over the rearing of orphaned children.[3] Furthermore, the monthly pension received is not a substantial amount in view of inflation costs, and many older-person-headed households are living below the poverty line.
Psychological distress and specifically depression may prevent successful ageing. The available data on depression in SA reflect a varied prevalence among the different ethnic groups, age categories and areas in which the studies were conducted. Using the present state exam, which is a screening tool assessing an individual's mental state at the time of the interview, the prevalence of depression in a population of mixed ethnicity >65 years old living in Cape Town in 1987 was 13%.[4] In 2008, 3 840 South Africans aged >50 years participated in the Study of Global Ageing and Adult Health, with 4% reporting depressive symptoms in the preceding 12 months.[2]
The population in the Inanda, Ntuzuma and KwaMashu (INK) area is estimated to be 510 000, with 6% of the population aged >60 years. This is a densely populated peri-urban area with poor infrastructure and unemployment. There is a paucity of data available on depression in the SA older population in general and even less on peri-urban populations such as those in the INK area. The objectives of this study were to determine if depression or depressive symptoms were significant problems in this population and to identify possible risk factors.
Method
This study was a secondary quantitative data analysis study of data collected in a primary cross-sectional study. The primary study was undertaken to assess the influence of socioeconomic and environmental factors on the health status and quality of life in older persons in the INK area. A total of 1 010 respondents was randomly selected (using cluster sampling and a Kish grid) from the 18 812 older persons living in the INK area. Ethical approval was granted for the original study and for this study by the Biomedical Research Ethics Committee of the University of KwaZulu-Natal and the Department of Health. Sample size in the original study was calculated based on a conservative percentage of 50%, as the prevalence was not known for all the conditions being investigated, and a precision of 3% to give smaller confidence intervals. Questionnaires were available in the local indigenous language, isiZulu, or English. The data were collected from face-to-face interviews after obtaining informed consent by trained field interviewers. The questionnaire included a number of well-validated instruments relevant to older persons' health (Table 1). Depressive symptoms were captured using the Center for Epidemiologic Studies Short Depression Scale (CES-D 10). The CES-D scale and the Beck Depression Inventory (BDI) are the two most-used screening tests for depressive symptom; however, they measure different aspects of the construct for depressive symptoms. Reports have shown that the BDI has higher specificity and the CES-D has higher sensitivity.[5] The CES-D 10 comprises 10 questions with negative responses graded as follows: rarely or none of the time = 0; some of the time = 1; occasionally = 2 or all of the time = 3, with a total score of 30. Two items (numbers 5 and 8) require positive responses and were reverse-scored. A CES-D 10 score of <10 indicates no depressive symptoms, 10 - 14 mild depressive symptoms and >14 severe depressive symptoms.
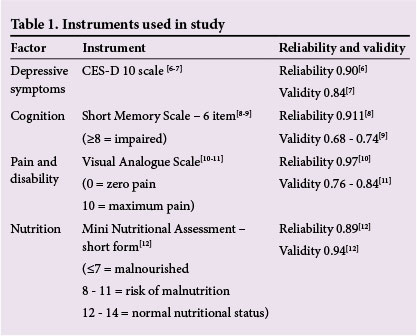
Risk factor information was captured using validated instruments for cognition, pain and disability, and nutrition (Table 1). In addition, respondents were asked to grade their general health status as very good, good, average or poor, and medical history was obtained for self-reported presence of common diagnosed medical disorders such as diabetes mellitus, hypertension and arthritis. A direct review of medication was undertaken and stratified into <2 and >3 drugs. Mobility was categorised as being able to mobilise with or without assistance, and the ability to complete light household tasks and work in the garden. Pain and disability were categorised as none, mild, moderate or severe based on pain rating. Mastery was assessed using questions from the original Perlin Mastery Scale,[13] namely: did the respondents believe they had control of their future; could they do everything; and were they in control of things that happen to them? Social integration was assessed using the respondents' ability to count on friends and family, and whether or not they belonged to a social organisation.
Statistical analysis
The data were analysed using the IBM (USA) SPSS Stats version 21 program. The response rate and sample description were analysed using descriptive statistics including frequency, mean and standard deviation (SD) for age, gender, date of birth, marital status, household size and literacy. Data were cleaned and in cases with missing data (items not answered) for the specific scales, the sums were computed after imputation of the missing values. To test the association between depressive symptoms and risk factors, following a review of the literature, the following risk factors were identified as independent variables: health status, medical history, medication history, cognition, pain, disability, nutrition, functional assessment, physical activity, mastery and social integration. Pearson's χ2 test was used to test for associations between the degree of depressive symptoms and the risk factors; the confidence level was set at 95% (p<0.05). Direct binary logistic regression containing all seven independent variables (age group, household size, income, nutrition, disability, ability to count on family, and ability to control things happening to the respondent) was used to determine the effect of these on the likelihood that respondents would report that they had a problem with depressive symptoms.
Results
Of the 1 010 respondents interviewed, two were excluded as they did not meet the selection criteria, therefore 1 008 respondents who completed the CES-D 10 questionnaire were selected for the study. The average age of the respondents was 68.9 (SD 7.4) years (range 60 -103). The female-to-male ratio was 3.4:1, and 43% of the respondents were widowed. Most households were multigenerational and included grandchildren (73%), while 10% of the respondents lived alone. Of the respondents, nearly three-quarters (73.9%) were literate (Table 2).
The CES-D 10 had moderate reliability, with a Chronbach's α of 0.687. Of the 1 008 respondents, 505 (50.1%) met the CES-D 10 criteria for reporting depressive symptoms. Of these, 422 (41.9%) reported mild depressive symptoms and 83 (8.2%) severe depressive symptoms. The relationship between depressive symptoms and sociodemographic factors is shown in Table 2. The presence of depressive symptoms increased with age (χ2=11.1, p=0.011). Gender, marital status and literacy showed no significant differences between the categories. There was a significant association between household size and presence of depressive symptoms (χ2=9.9, p=0.007) with 45.4% of respondents who were living alone reporting depressive symptoms compared with 75% of respondents living in larger households with >11 dwellers, though most of these were mild depressive symptoms (55.6%). There was a significant association between low income (<ZAR1 600) and overall depressive symptoms, with 52.3% reporting depressive symptoms (χ2=5.5, p=0.033).
Health-related and social risk factors for depressive symptoms
Health and social risk factors for depressive symptoms are shown in Table 3. Depressive symptoms were strongly associated with poor nutrition (χ2=63.3, p<0.001) and disability (χ2=17.5, p=0.001). Respondents who were either malnourished or at risk for malnutrition reported the highest frequency of depressive symptoms (74.2% and 60.2%, respectively) compared with those with a normal nutritional status (37.5%). Depressive symptoms were also significantly associated with increasing self-reported disability status, and increased from 45.7% in respondents with no disability to 64.0% in those with severe disability (χ2=17.7, p=0.001). There was no significant relationship between degree of pain or functional ability and depressive symptoms.
Though the presence of depressive symptoms was not significantly associated with general health status (χ2=3.7, p=0.289), severe depressive symptoms were strongly associated with a decrease in health status, with depressive symptoms being present in 4% of respondents reporting very good health, 4.5% reporting good health, 8.7% reporting average health and 17.1% reporting poor health (χ2=31.9, p<0.001). Although the presence of depressive symptoms was higher in those who mobilised without assistance, this did not reach statistical significance (χ2=2.7, p=0.258). However, respondents requiring assistance in mobilising were significantly more likely to have mild depressive symptoms than those who did not (47.0% v. 41.7%; χ2=10.9, p=0.017). While there was no significant association between depressive symptoms and impaired cognition (χ2=0.01, p=0.834), respondents with impaired cognition reflected a higher percentage of severe depressive symptoms compared with those with normal cognition (11.3% v. 4.3%; χ2=17.9, p<0.001).
There was a significant association between depressive symptoms and lack of mastery and social support; depressive symptoms were reported by 56.3% of the respondents who reported an inability to control things happening to them (χ2=17.9, p<0.001) and 51.9% of respondents who did not have a family member to rely on (χ2=17.6, p=0.006). The ability to rely on friends was not related to depressive symptoms.
The direct binary logistic regression model was statistically significant (n=986, χ2=23.2, p=0.003), indicating that the model was able to distinguish between respondents who reported and did not report depressive symptoms. The model as a whole explained between 10.6% (Cox and Snell R2) and 14.1% (Nagelkerke R2) of the variance in depressive symptoms, and correctly classified 62.1% of cases. Four of the seven independent variables made a unique statistically significant contribution to the model, namely little control or mastery (p<0.001), inability to count on family (p=0.027), malnutrition (p<0.001) and household size (p=0.024).
Discussion
The study found that over half of the respondents reported the presence of depressive symptoms. This finding was consistent for all the individual 10 items in the CES-D 10. This is an unusually high prevalence, and should be considered in terms of the findings from other countries, using similar instruments. A Spanish study found a high depression prevalence of 34.5% among 85-year-old community-dwellers using the Geriatric Depression Scale (GDS). In Norway, participants in the 86 - 90-year age group reported a prevalence of 9.6% using the Hospital Anxiety and Depression Scale (HADS-D).[14] A report from India looking at depression in villages in participants aged >60 years found a similar prevalence of 47%. The prevalence was highest among those aged >80 years, and was associated with poor socioeconomic status, female gender, illiteracy and complete dependence.[15]
In SA studies, different prevalences have been reported. Peltzer,[2] reported a 4% prevalence of depression in persons aged >50 years using self-reported depressive symptoms in the preceding 12 months, and Tomlinson et al.,[16] using the World Health Organization Composite International Diagnostic Interview version 3.0 (CIDI 3.0) reported a lifetime prevalence of 9.7% in the overall population and 19.4% in the population >50 years old, with the highest frequency of depression in the black population (75.4%). The lack of consistent instruments makes comparisons between groups difficult; however, the markedly higher frequency of depressive symptoms in the INK area may be explained by the unique stressors that the elderly in this area face, such as poverty, crime and the HIV and TB pandemic. [17] Recent crime statistics released by the SA Police Services for 2012/2013 revealed that KwaMashu section E had one of the highest murder rates in the country, with 120 murders recorded for this time period.
The four factors that significantly contributed to the reports of depressive symptoms were malnutrition (p<0.001), household size (p=0.024), little control or mastery (p<0.001) and an inability to count on family (p=0.027). Poor nutrition has been identified as a risk factor for depression in studies from both developing and developed countries. A study of institutionalised British elderly, using the Mini-Nutritional Assessment and the Geriatric Depression Scale,[18] found a significant association between malnutrition and depression, as did a Brazilian study.[19] The findings in the INK population are consistent with these studies. The burden of poor nutrition may be linked to the dire financial situations in which these individuals find themselves, as the majority of our respondents live below the poverty line, with a household income of <ZAR1 600 per month. Females may be marginalised, with lack of financial independence and in some cases be victims of abuse, which may contribute to the higher prevalence of depressive symptoms. Those individuals in larger households with grandchildren are likely to encounter an increase in financial demands to sustain the household, which may explain our findings.
Social integration and social support have to be addressed in this community, as these will enhance the sense of belonging and will positively affect depressive symptoms, as discussed by Tuesca-Molina et al.[20]The ability to rely on family members for support is proven to be important to the elderly population in the current study, as with other populations.[21] However, the breakdown of the nuclear family unit is a problem that may be difficult to remedy, as factors such as employment opportunities influence this phenomenon.
Study limitations
In this study, the CES-D 10 scale was used to assess the presence of depressive symptoms. Although the CES-D has not been designed for the clinical diagnosis of depressive disorder, but rather looks at depressive symptoms in the week preceding the interview, reported predictive validity is high, with sensitivities ranging between 97 and 100%, specificities between 84 and 93% and positive predictive values between 38 and 85%.[22] The CES-D scale was assessed in a black SA student population in 1991, and results were comparable with those in previous reports, with similar reliability and validity scores.[23] Similar scales, the Kessler Psychological Distress 10-item scale (K10) and the abbreviated 6-item scale (K6), were reported on in a 2011 SA study.[24]These scales share similarities with the CES-D 10 scale. The study divided the population by ethnicity into a group comprising black individuals and another group with minorities (Indian, white and mixed ethnicity). It was reported that these scales had a lower ability to differentiate between depression and anxiety disorders in the black group, who were more likely to answer affirmatively to the questions 'How often do you feel that everything is an effort?' and 'How often do you feel worthless?'[25] It remains to be determined if the CES-D scale has a similar limitation in the SA black population.
Conclusion
This study has shown that despite possible limitations of the instrument used, older people in the INK area reported high rates of depressive symptoms, which are comparatively greater than other prevalence data available to date. Although they share similar risk associations and demographic profile with other populations studied in the past, in this population the additional risk factors associated with depressive symptoms may be influencing the prevalence of these symptoms. International reports have shown that depression is associated with increased overall mortality in the elderly.[26] The INK population may therefore be at significant risk for both suicide and increased mortality in view of the high frequency of depressive symptoms shown in this study. This information should be used to screen for depressive symptoms and risk factors routinely, and the relevant bodies including healthcare practitioners, community leaders, community elders, social workers, and organisations involved with the elderly should be encouraged to become involved in promoting successful ageing.
Acknowledgements. This study was funded by the SA Netherlands Research Programme on Alternatives in Development (SANPAD).
References
1. World Health Organization launches new initiative to address the health needs of a rapidly ageing population. Cent Eur J Public Health 2004;12(4):210,216. [ Links ]
2. Peltzer K, Phaswana-Mafuya N. Depression and associated factors in older adults in South Africa. Glob Health Action 2013;6:1-9. [http://dx.doi.org/10.3402/gha.v6i0.18871] [ Links ]
3. Kimuna SR, Makiwane M. Older people as resources in South Africa: Mpumalanga households. J Aging Soc Policy 2007;19(1):97-114. [http://dx.doi.org/10.1300/J031v19n01_06] [ Links ]
4. Ben-Arie O, Swartz L, Dickman BJ. Depression in the elderly living in the community: Its presentation and features. B J Psychiatry 1987;150:169-174. [ Links ]
5. Skorikov VB, van der Voort DJ. Relationships between the underlying constructs of the Beck Depression Inventory and the Center for Epidemiological Studies Depression Scale. Educ Psychol Meas 2003;63(2):319. [http://dx.doi.org/10.1177/0013164402251035] [ Links ]
6. Radloff LS. The CES-D Scale: A self-report depression scale for research in the general population. Appl Psych Meas 1977;1(3):385-401. [http://dx.doi.org/10.1177/014662167700100306] [ Links ]
7. Yesavage JA, Sheikh JI. Geriatric Depression Scale (GDS). Recent evidence and development of a shorter version. Clin Gerontol 1986;5(1-2):165-173. [http://dx.doi.org/10.1300/J018v05n01_09] [ Links ]
8. Brooke P, Bullock R. Validation of a 6 item cognitive impairment test with a view to primary care usage. Int J Geriatr Psychiatry 1999;14(11):936-940. [ Links ]
9. Katzman R, Brown T, Fuld P, Peck A, Schechter R, Schimmel H. Validation of a short Orientation-Memory-Concentration Test of cognitive impairment. Am J Psychiatry 1983;140(6):734-739. [ Links ]
10. Bijur PE, Silver W, Gallagher EJ. Reliability of the visual analog scale for measurement of acute pain. Acad Emerg Med 2001;8(12):1153-1157. [ Links ]
11. Boonstra AM, Schiphorst Preuper HR, Reneman MF, Posthumus JB, Stewart RE. Reliability and validity of the visual analogue scale for disability in patients with chronic musculoskeletal pain. Int J Rehabil Res 2008;31(2):165-169. [http://dx.doi.org/10.1097/MRR.0b013e3282fc0f93] [ Links ]
12. Rubenstein LZ, Harker JO, Salva A, Guigoz Y, Vellas B. Screening for undernutrition in geriatric practice: Developing the short-form mini-nutritional assessment (MNA-SF). J Gerontol A Biol Sci Med Sci 2001;56(6):M366-M372. [ Links ]
13. Eklund M, Erlandsson LK, Hagell P. Psychometric properties of a Swedish version of the Pearlin Mastery Scale in people with mental illness and healthy people. Nord J Psychiatry 2012;66(6):380-388. [http://dx.doi.org/10.3109/08039488.2012.656701] [ Links ]
14. Solhaug HI, Romuld EB, Romild U, Stordal E. Increased prevalence of depression in cohorts of the elderly: An 11-year follow-up in the general population - the HUNT study. Intm Psychogeriatr 2012;24(1):151-158. [http://dx.doi.org/10.1017/S1041610211001141] [ Links ]
15. Swarnalatha N. The prevalence of depression among the rural elderly in Chittoor District, Andhra Pradesh. J Clin Diagn Res 2013;7(7):1356-1360. [http://dx.doi.org/10.7860/JCDR/2013/5956.3141] [ Links ]
16. Tomlinson M, Grimsrud AT, Stein DJ, Williams DR, Myer L. The epidemiology of major depression in South Africa: Results from the South African Stress and Health study. S Afr Med J 2009;99(5 Pt 2):367-373. [ Links ]
17. Kuo C, Operario D, Cluver L. Depression among carers of AIDS-orphaned and other- orphaned children in Umlazi Township, South Africa. Glob Public Health 2012;7(3):253-269. [http://dx.doi.org/10.1080/17441692.2011.626436] [ Links ]
18. Smoliner C, Norman K, Wagner KH, Hartig W, Lochs H, Pirlich M. Malnutrition and depression in the institutionalised elderly. Br J Nutr 2009;102(11):1663-1667. [http://dx.doi.org/10.1017/S0007114509990900] [ Links ]
19. Cabrera MA, Mesas AE, Garcia AR, de Andrade SM. Malnutrition and depression among community-dwelling elderly people. J Am Med Dir Assoc 2007;8(9):582-584. [http://dx.doi.org/10.1016/j.jamda.2007.07.008] [ Links ]
20. Tuesca-Molina R, Fierro Herrera N, Molinares Sosa A, et al. [Socializing groups as protective factor against depression in elderly people. Barranquilla, Colombia.] Rev Esp Salud Publica 2003;77(5):595-604. [ Links ]
21. Chi I, Chou KL. Social support and depression among elderly Chinese people in Hong Kong. Int J Aging Hum Dev 2001;52(3):231-252. [ Links ]
22. Irwin M, Artin KH, Oxman MN. Screening for depression in the older adult: Criterion validity of the 10-item Center for Epidemiological Studies Depression Scale (CES-D). Arch Intern Med 1999;159(15):1701-1704. [ Links ]
23. Pretorius TB. Cross-cultural application of the Center for Epidemiological Studies Depression Scale: A study of black South African students. Psychol Rep 1991;69(3 Pt 2):1179-1185. [ Links ]
24. Peltzer K, Pengpid S, Skaal L. Prevalence of psychological distress and associated factors in urban hospital outpatients in South Africa. S Afr J Psychiatr 2012;18(1):12-15. [ Links ]
25. Andersen LS, Grimsrud A, Myer L, Williams DR, Stein DJ, Seedat S. The psychometric properties of the K10 and K6 scales in screening for mood and anxiety disorders in the South African Stress and Health study. Int J Methods Psychiatr Res 2011;20(4):215-223. [http://dx.doi.org/10.1002/mpr.351] [ Links ]
26. Pulska T, Pahkala K, Laippalla P, Kivelá SL. Major depression as a predictor of premature deaths in elderly people in Finland: A community study. Acta Psychiatr Scand 1998;97(6):408-411. [ Links ]
 Correspondence:
Correspondence:
J Narainsamy (narainsamyjay21@yahoo.com)














