Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
SA Journal of Radiology
versão On-line ISSN 2078-6778
versão impressa ISSN 1027-202X
S. Afr. J. radiol. (Online) vol.19 no.1 Johannesburg 2015
http://dx.doi.org/10.4102/SAJR.v19i1.747
ORIGINAL RESEARCH
Ultrasound diagnosis of ulnar nerve entrapment by confirming baseline cross-sectional area measurement for normal and abnormal nerves
Tania Roodt; Barbara van Dyk; Sylvia Jacobs
Department of Radiography, University of Johannesburg, South Africa
ABSTRACT
BACKGROUND: Magnetic resonance imaging is most commonly employed, alongside electro-diagnostic studies, in the diagnosis of ulnar nerve entrapment. It is expensive, time consuming, not readily available to the general public, and limits imaging to a segment of the nerve at any given time. In contrast, high-frequency ultrasound is an inexpensive imaging modality with a flexible field of view through which the nerve can be traced. An ultrasound cross-sectional area (CSA) >0.075 cm2 has previously been suggested as indicative of nerve entrapment.
OBJECTIVES: To confirm the suggested CSA measurement of 0.075 cm2 and discuss the difference in CSA measurement between abnormal nerves, nerves in the contra-lateral elbow of the same participant, and those of asymptomatic participants
METHODS: Ultrasonography was performed on both elbows of 25 patients with confirmed unilateral ulnar nerve entrapment and on 25 healthy controls for comparison. Three CSA measurements were taken of the ulnar nerve along its course, and the mean measurement was recorded
RESULTS: CSA measurements were significantly different between patients with ulnar nerve entrapment and healthy controls (p < 0.05). In our study, a CSA >0.070 cm2 defined ulnar nerve entrapment at the elbow.
CONCLUSION: Ultrasound CSA measurement of the ulnar nerve is accurate in the diagnosis of ulnar nerve entrapment. The range of values and varied criteria previously reported call for standardisation of the procedure and CSA measurement. We suggest that a measurement of 0.070 cm2 be considered as a new baseline for the optimal diagnosis of ulnar nerve entrapment.
Introduction and background
High-frequency ultrasound is an inexpensive and non-invasive imaging modality that has become an appealing adjunct to electro-diagnostic studies in the evaluation of entrapment neuropathies.1,2 Currently, magnetic resonance imaging (MRI) is the most commonly employed imaging tool in the diagnosis of ulnar nerve entrapment; however, it is expensive, time consuming, not readily available to the general public and allows only a segment of the nerve to be imaged at any given time.3,4,5 In contrast, ultrasound provides a flexible field of view through which the nerve can be traced, and is able to clearly differentiate the nerve from the surrounding anatomical structures.1
Ulnar nerve entrapment may result in painful tingling or debilitating weakness of the hands or upper extremities.6 Peripheral nerves are vulnerable to compression at sites of fibrous and fibro-osseous tunnels. The most common site for ulnar nerve entrapment is consequently where the nerve passes through the cubital tunnel owing to pathological narrowing of the tunnel.7
Recent technological advances in ultrasound have enabled investigation of the condition with high-resolution ultrasound along the path of the nerve with relative ease.1,3,8,9 Chiou et al. suggested that an ulnar nerve cross-sectional area (CSA) measurement >0.075 cm2 was indicative of nerve entrapment.2 This measurement was derived from a small sample of 24 patients of whom 14 were symptomatic and 10 asymptomatic, making the reliability of the suggested measurement of 0.075 cm2 questionable.2 Further research, on a larger sample, was thus indicated to test the reliability of the suggested CSA measurement.
Objectives
Our aims were to: (1) compare the previously suggested baseline CSA measurement of 0.075 cm2, for ulnar nerve entrapment, with findings from the present study to improve future diagnosis of the condition; (2) elaborate on the difference between normal and abnormal nerves by comparing the CSA measurement of abnormal ulnar nerves with the nerve in the contra-lateral elbow in the same participant and to that of asymptomatic participants; and (3) to report the effect of confounding factors on the size of the ulnar nerve.
Method
A prospective quantitative comparative research approach allowed statistical comparison of results in order to meet the objectives.
Research population and sampling
A quota non-probability sampling method was employed by recruiting patients with ulnar nerve entrapment, as confirmed by electro-diagnostic studies and referred for ultrasound examination of the elbow. Patients with a predisposition for ulnar nerve entrapment owing to a previous fracture, arthritis, elbow pain or surgery which complicates interpretation of the ultrasound image, were excluded from the study.
Asymptomatic participants who acted as controls were recruited from the general public.
Research procedure
Ultrasound scans were performed on a Toshiba Xario ultrasound unit (Model SSA-660A), using a 12 mHz linear transducer with a small footprint. The ulnar nerve was examined both during flexion and extension of the elbow. During the acquisition of flexion views, the patient was seated next to the examination couch with the palm in contact with the examination table and the elbow rotated postero-laterally so that the humerus was at right angles to the trunk (Figures 1-2). This position accentuated the anatomical landmarks.
For extension views, the patient was positioned with the shoulder and elbow in extension. The dorsal aspect of the hand was in contact with the examination table and the palm inverted (Figure 3).
The examination commenced with a longitudinal survey of the ulnar nerve to search for oedematous thickening of the nerve or loss of normal ultrasound characteristics. Figure 4 demonstrates a normal ulnar nerve, at the level of the cubital tunnel, in a longitudinal plane with the elbow in flexion.
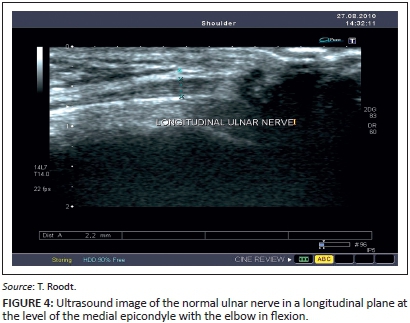
The probe was then rotated through 90° into the transverse plane until the nerve appeared as an oval or round structure (Figure 5). To obtain this image, the medial aspect of the transducer (side of the marker on the transducer) was placed at the medial epicondyle and the lateral aspect of the transducer on the olecranon process (Figure 6).
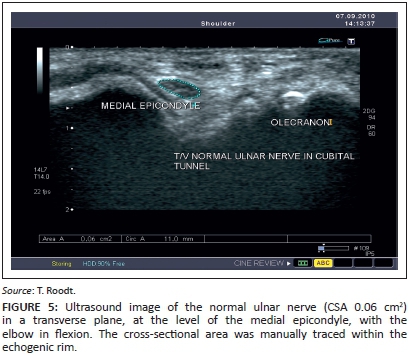
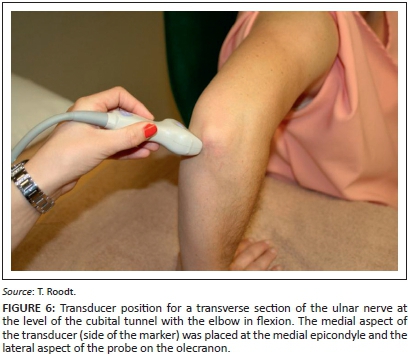
Area measurements were performed on a transverse section of the nerve during flexion, by using the manual free-hand tracing method. Three successive CSA measurements were obtained within the echogenic rim of the ulnar nerve (Figure 5) at:
1. the level of the medial epicondyle of the elbow
2. 50 mm proximal to the level of the medial epicondyle
3. 50 mm distal to the level of the medial epicondyle.
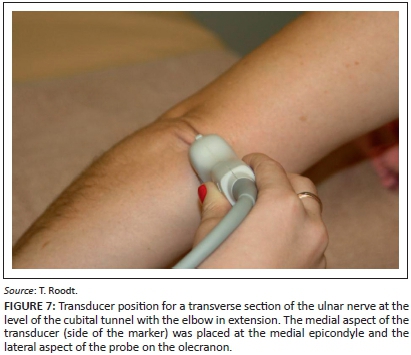
The same measurements were repeated with the elbow in extension, with the medial aspect of the transducer (side of the marker) placed at the medial epicondyle and the lateral aspect of the probe on the olecranon (Figure 7). This procedure was followed by three successive measurements of the contra-lateral arm in the same patient and compared with similar area measurements performed on control asymptomatic participants. Measurements were recorded on CD and the mean measurement was used for data analysis.
Data collection and statistical analysis
Twenty-five patients with unilateral ulnar nerve entrapment, confirmed by electro-diagnostic studies, were studied. Data were collected from the pathological nerve, contra-lateral arm of the same patient, and also from the dominant arm in 25 asymptomatic healthy participants for comparison.
Descriptive statistical analysis was performed with SPSS version 18.0, with ranges presented in graphical form. The Shapiro-Wilk test was used to examine the normality of data distribution in the small sample and to test the null hypothesis. Skewness of data necessitated the use of non-parametric tests to establish statistical significance. A p-value < 0.05 was considered as statistically significant.
Ethical considerations
The study was approved by the Higher Degrees and Ethics Committees, Faculty of Health Sciences, University of Johannesburg. Participants were briefed on the purpose of the research and the procedure for data collection. Agreement to participate was indicated by signing informed consent while anonymity was ensured by using a research number.
Validity and reliability
All ultrasound scans were performed by the researcher, and measurements were confirmed by a radiologist to minimise data collector bias. Standardisation was ensured by the use of the same ultrasound unit with an automatic calibration function, a 12 mHz linear transducer with a small footprint (PLT-1204AT), and a mechanical index of0.6 accurate to 0.1 mm.
Results
The ulnar nerve CSA measurement was significantly greater in symptomatic patients than in the asymptomatic control group (p< 0.05) at all three measured levels. The bottom of the range in patients with confirmed ulnar nerve entrapment, with the elbow in flexion, was recorded as 0.07 cm2 (range 0.07 cm2-0.25 cm2; median 0.10 cm2, mean 0.116 cm2) whilst the same measurement represented the maximum measurement for asymptomatic nerves in control participants (range 0.04 cm2-0.07 cm2; median 0.051 cm2, mean 0.052 cm2). Measurements of the contra-lateral elbow overlapped between the measurements of the symptomatic and asymptomatic participants (range 0.05 cm2-0.17 cm2; median 0.08 cm2, mean 0.09 cm2) (Figures 8-9; Tables 1-3).
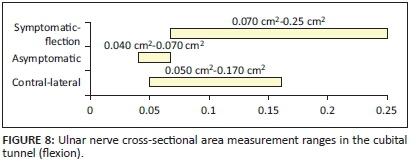
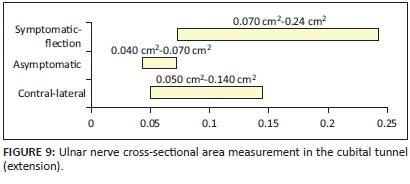
CSA measurements in symptomatic and asymptomatic participants were significantly different (p = 0.001) at the level of the cubital tunnel. Measurements of the contra-lateral elbow overlapped between that of symptomatic and asymptomatic participants ( p = 0.000).
A significant difference in CSA measurements (p= 0.000) was recorded between symptomatic and asymptomatic participants, 50 mm distal to the level of the cubital tunnel.
The study likewise revealed a significant difference, although smaller, between CSA measurements 50 mm proximal to the level of the cubital tunnel with the arm in flexion (p = 0.003).
Confounding factors explored in the study included gender, race, height, age, weight, BMI, handedness, occupation and participation in sport. Owing to the small sample size, correlation coefficients, lying between -1 and +1, were employed to determine the correlation between measurements and confounding factors. With a correlation coefficient ≥0.6 indicating a strong correlation, a positive correlation was found between the CSA of the ulnar nerve and age (0.6), occupation (0.6) and weight/BMI (0.4) in both flexion and extension.
The unpaired f-test showed statistical significance (p= 0.004) between CSA measurements taken in flexion and extension in asymptomatic participants.
Discussion
Results of the present study concurred that the CSA of the ulnar nerve at all three levels was significantly increased in patients with confirmed ulnar nerve entrapment in comparison with asymptomatic participants.1,10 Although the majority of cubital tunnel CSA measurements in symptomatic patients were greater than the previously suggested 0.075 cm2, a measurement of 0.070 cm2 was recorded in two patients with confirmed ulnar nerve entrapment.
In keeping with results from previous studies,8,11,12 the CSA measurement of the contra-lateral elbow overlapped between the measurements recorded in symptomatic and asymptomatic participants for both flexion and extension of the elbow. This finding confirms the suspicion that ulnar nerve entrapment at the elbow occurs bilaterally in the majority of cases, although only one arm may present with symptoms of the condition.7,11,12 Populations at risk of flexion-induced ulnar neuropathy include office workers who habitually lean their flexed elbows against a desk or table.13
Moreover, in agreement with Thoirs,10 the CSA measurement of the ulnar nerve was greater when made with the elbow in extension than in flexion in the asymptomatic group (Table 4). This difference may be explained by the alteration in the length of the path of the nerve that occurs with elbow flexion, leading to changes in the shape and thickness of the nerve.
The results of our study concur with previous findings by showing that the ultrasound measurement of the ulnar nerve is susceptible to confounding factors arising from physical characteristics of the individual.2,9,10 However, owing to the small sample size, further investigation is needed to validate the magnitude of confounding factors on the ulnar nerve size.
Limitations of the study
Although the study population was more than double that of the previous study, 25 participants per group is still considered a small sample for meaningful statistical analysis, and thus remains a limiting factor in the present study. Furthermore, it was difficult to match the two groups, which led to participants in the symptomatic group being significantly older than the asymptomatic healthy group. Previous studies have suggested that ulnar nerve entrapment is a condition of middle age.10,14 The average age for the symptomatic group was 46 years (range 23-72) compared to an average of 36 years for the asymptomatic group (range 23-56).
Conclusion and recommendations
Whilst an electro-diagnostic study provides detailed physiological information, ultrasound provides detailed anatomical information of nerves. High-frequency ultrasound examination of the elbow is useful to detect soft tissue and bony abnormalities whilst providing information on adjacent anatomical structures.3
Ultrasonography is faster and less expensive than a comparable MRI test, is not associated with exposure to ionising radiation, and has no known adverse biological effects.3 Despite an increasing number of published articles, many practitioners still remain unaware of the effectiveness of high-resolution ultrasound for assessing peripheral nerves.
Although the numbers in our sample are too small to prove statistical significance, the results of the study suggest that a CSA measurement of 0.070 cm2 should be considered as a new baseline to differentiate between normal nerves and nerves affected by entrapment pathology, for the optimal diagnosis of ulnar nerve entrapment. With a new cut-off value of 0.070 cm2, it can be argued that patients with ulnar nerve entrapment might have been compromised if the previously suggested value of 0.075 cm2 had been adhered to.1 Further research on a bigger study population may be indicated to confirm our findings.
Furthermore, the enlargement of the asymptomatic contra-lateral nerve may indicate an underlying pathological condition or an habitual action, such as leaning on the elbow, that makes the nerve more vulnerable to injury.
The broad range of normative values reported in the literature15 and varied criteria used in the diagnosis of ulnar nerve entrapment, call for standardisation of the ultrasound procedure and CSA measurement. The results of the present study demonstrate that the ulnar nerve can be reliably measured in cross-section when a closely controlled positioning and measurement protocol is followed.
In conclusion: the ultrasound CSA measurement of the ulnar nerve, made at the level of the medial epicondyle, is found to be a robust discriminator of ulnar nerve entrapment, making it a useful diagnostic test for the evaluation and diagnosis of ulnar nerve entrapment.
Competing interests
The authors declare that they have no financial or personal relationships which may have inappropriately influenced them in writing this article.
Authors' contributions
As the primary researcher of the Master's project from which the present article emanated, T.R. (University of Johannesburg) wrote the present article with thorough concern for the design, interpretation of data, and critical revision of the intellectual content to take public responsibility for it. She approves it for publication.
As supervisor of the research project, B.v.D. (University of Johannesburg) participated sufficiently in the conception and design of the present work, the data analysis (where applicable), critical review of the intellectual content and the writing of the article to take public responsibility for it. She reviewed the final version of the article and approves it for publication.
As co-supervisor of the Master's project, S.J. (University of Johannesburg) participated sufficiently in the conception, design, interpretation of data, critical revision of the intellectual content and the writing of the article to take public responsibility for it. She approves it for publication.
References
1. Ginn SD, Cartwright MS, Chloros GD, et al. Ultrasound in the diagnosis of a median neuropathy in the forearm: Case report. J Brachial Plex Peripher Nerve Inj. 2007;2:23. [ Links ]
2. Chiou H, Chou Y, Cheng S, et al. Cubital tunnel syndrome: Diagnosis by high-resolution ultrasonography. J Ultrasound Med. 1998;17:643-648. [ Links ]
3. Introcasco JH, van Holsbeeck MT. Sonography of the elbow, wrist and hand. 2nd ed. Mosby, Maryland Heights: 2001; pp. 539-540, 528-529. [ Links ]
4. Maravilla KR, Bowen BC. Imaging of the peripheral nervous system: Evaluation of peripheral neuropathy and plexopathy. Am J Neuroradiol. 1998;19:1011-1023. [ Links ]
5. Steinback LS, Chung CB. MRI of the upper extremity. Philadelphia: Lippincott, Williams & Wilkins; 2010; p. 192. [ Links ]
6. Bayramoglu M. Entrapment neuropathies of the upper extremity. J Neuroanatomy. 2004;3:18-24. [ Links ]
7. Hochman M, Zilberfarb JL. Nerves in a pinch: Imaging of nerve compression syndromes. Radiol Clin North Am. 2004;42:221-245. http://dx.doi.org/10.1016/S0033-8389(03)00162-3 [ Links ]
8. Beekman R, Schoemaker MC, van der Plas JPL, et al. Diagnostic value of high-resolution sonography in ulnar nerve neuropathy at the elbow. Neurology. 2004;62:767-773. http://dx.doi.org/10.1212/01.WNL.0000113733.62689.0D [ Links ]
9. Martinoli C, Bianchi S, Gandolfo N, Valle M, Simonetti S, Derchi LE. US of nerve entrapment in osteofibrous tunnels of the upper and lower limbs. Radiographics. 2000;20:S199-S217. http://dx.doi.org/10.1148/radiographics.20.suppl_1.g00oc08s199 [ Links ]
10. Thoirs K, Williams MA, Phillips M. Systemic review of sonographic measurements of the ulnar nerve at the elbow. J Diagn Med Sonogr. 2007;23:255-262. http://dx.doi.org/10.1177/8756479307306110 [ Links ]
11. Pais P, Fodor D, Fisher T. Bilateral cubital tunnel syndrome: Case report with review of the literature. Med Ultrasonogr. 2009;11:31-36. [ Links ]
12. Dellon AL, Hament W, Gittelshon A. Non-operative management of cubital tunnel syndrome: An 8-year prospective study. Neurology. 1993;43:1673-1677. http://dx.doi.org/10.1212/WNL.43.9.1673 [ Links ]
13. Miller TT, Reinus WR. Nerve entrapment syndromes of the elbow, forearm, and wrist. Am J Roentgenol. 2010;195:585-594. http://dx.doi.org/10.2214/AJR.10.4817 [ Links ]
14. Yoon JS, Hong S, Kim B, et al. Ulnar nerve and cubital tunnel ultrasound in ulnar neuropathy at the elbow. Arch Phys Med Rehabil. 2008;89:887-889. http://dx.doi.org/10.1016/j.apmr.2007.10.024 [ Links ]
15. Koenig RW, Pedro MT, Heinen CPG, et al. High-resolution ultrasonography in evaluating peripheral nerve entrapment and trauma. Neurosurg Focus. 2009;26:1-6. http://dx.doi.org/10.3171/FOC.2009.26.2.E13 [ Links ]
 Correspondence:
Correspondence:
Barbara van Dyk
PO Box 772, Roodepoort 1725
South Africa
Email: bvandyk@uj.ac.za
Received: 30 Oct. 2014
Accepted: 15 May 2015
Published: 05 Aug. 2015














