Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
SA Journal of Radiology
versão On-line ISSN 2078-6778
versão impressa ISSN 1027-202X
S. Afr. J. radiol. (Online) vol.18 no.2 Johannesburg 2014
http://dx.doi.org/10.4102/sajr.v18i2.670
PICTORIAL REVIEWS
Sports hernia: A pictorial review
Peter Mercouris
Lake, Smit and Partners, Durban, South Africa
ABSTRACT
Sports hernia represents a complex clinical and imaging entity. The purpose of the review is to provide a practical imaging approach to this condition. The review includes an overview of the anatomy and biomechanics of sports hernia by means of colour illustrations. The role of imaging, and particularly magnetic resonance imaging, is highlighted.
Introduction
Athletic pubalgia is a general term to describe exertional pubic or groin pain.1 Groin pain in elite athletes is common and accounts for approximately 5% - 18% of all athletic injuries and is especially prevalent in kicking sports.2 The differential diagnosis is broad but the most common causes are considered to be adductor longus injury, common adductor-rectus abdominis dysfunction, osteitis pubis and sports hernia.1 This review is of the imaging of sports hernia.
Definition
Sports hernia represents an acquired deficiency of the inguinal wall and has been described by a myriad of names, such as Gilmore's groin, groin disruption, pubalgia, sportsman's hernia, prehernia complex, incipient hernia, symphysis syndrome and inguinal canal disruption.2 Practically, it is best appreciated as a deficiency that involves the anterior inguinal wall (external oblique muscle and aponeurosis), the posterior inguinal wall (transversus abdominis and internal oblique muscles), or both. Anterior inguinal wall deficiency represents an injury of the external oblique muscle aponeurosis, whereas posterior inguinal wall deficiency represents an injury at the level of the transversus abdominis and internal oblique muscles and aponeuroses.2
Clinical presentation
Athletes give a history of an insidious onset of groin pain that is initially experienced at the end of a game, progressing to pain during play and eventually pain at rest. Some may also experience pain at night.3 On physical examination, point tenderness may be elicited at or near the pubic symphysis, and there may be resistance or pain on ipsilateral hip adduction. Classically, there is no palpable hernia on physical examination.4
Anatomy
Anatomically, the anterior aspect of the pubis acts as a common origin for important musculotendinous, aponeurotic and ligamentous structures around the symphysis pubis (Figure 1). This prepubic soft-tissue complex is known as the prepubic aponeurotic complex (P-PAC) (Figure 2) and includes interconnections between the adductor tendons, rectus abdominis, inguinal musculoaponeurotic structures, articular disc and pubic ligaments of the symphysis pubis.1 Laterally, the caudal rectus abdominis lies just posteromedial to the superficial inguinal ring, and probably plays a role in reinforcing the wall of the posteromedial superficial inguinal canal.5

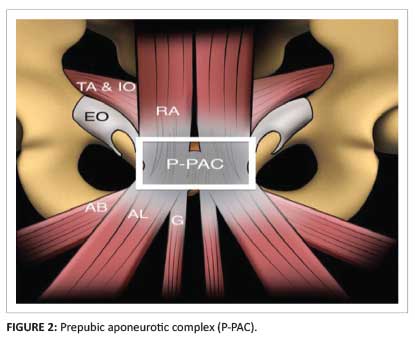
Biomechanics
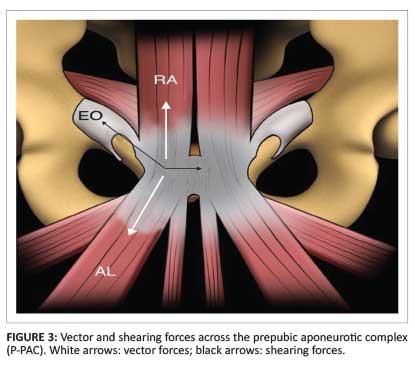
The rectus abdominis and adductor longus are relative antagonists during core rotation and extension, with the result that the former elevates the anterior pelvis and the latter depresses it (Figure 3).3 There is therefore a dynamic imbalance between the strong adductors and weak abdominal musculature, resulting in shearing forces across the inguinal wall musculoaponeurotic and symphyseal structures (Figure 3).
Imaging
The fascial structures of the inguinal canal are not reliably imaged and sports hernia is therefore a clinical diagnosis and a radiological diagnosis of exclusion.2 Imaging in affected athletes is usually normal but occasionally injury to the inguinal aponeurotic structures can be identified. Imaging is, however, still important to exclude injury to the other musculoaponuerotic structures that constitute the prepubic aponeurotic complex.
The imaging approach of athletic pubalgia and sports hernia includes primarily the use of radiography, ultrasound and magnetic resonance imaging (MRI), with computed tomography (CT) and nuclear medicine imaging playing ancillary roles.
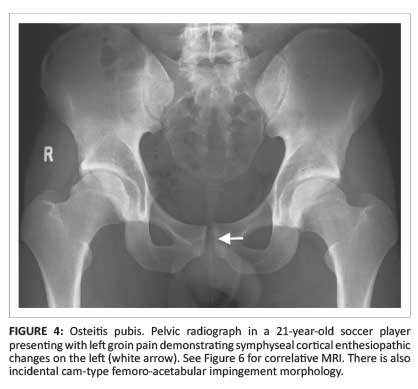
Obtaining a pelvic radiograph is still a good imaging principle to follow, although this is usually normal. A pelvic radiograph is useful in demonstrating symphyseal alignment and may indicate a potential osseous cause for the groin pain including hip, sacro-iliac, lower lumbar spine, and symphyseal (Figure 4) and apophyseal pathology.
Ultrasound, as with radiography, is also usually normal. Ultrasound is accurate in evaluating true inguinal and femoral hernias but these are rare in athletes.3 There is perhaps a role for dynamic ultrasound in evaluating potential posterior inguinal wall deficiency. This application arose from a study amongst Australian footballers in the late 1990s that documented the presence of abnormal ballooning of the posterior wall during straining. This sign was considered to be more specific if bilateral and in older athletes.6 Current consensus appears to indicate that this sign is too nonspecific and nonsensitive for widespread practical use.3
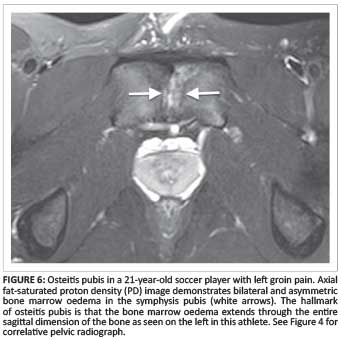
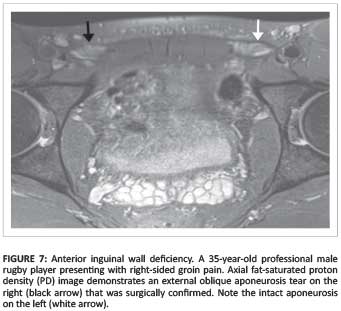
The goal of imaging is to accurately evaluate the musculoaponeurotic structures of the groin and is best achieved by MRI. MRI is both sensitive (98%) and specific (89% - 100%) in patients with athletic pubalgia for injuries involving the rectus abdominis (Figure 5d), the adductor tendon origin (Figure 5), and the symphysis (Figure 6) itself.7 MRI is usually normal in sports hernia but an injury to the anterior (Figure 7 and Figure 8) or posterior wall (Figure 9) can sometimes be identified (Table 1). MRI is also useful in evaluating the regional osseous structures, as stress fractures (Figure 10) are common causes of groin pain beyond the inguinal and P-PAC regions (Table 1).




Conclusion
Sports hernia represents an acquired deficiency of the inguinal wall. Imaging is usually normal in affected athletes, and the entity remains a clinical diagnosis.
Acknowledgements
I thank Neil Northey for the medical illustrations.
Competing interests
The author declares that he has no financial or personal relationship(s) that may have inappropriately influenced him in writing this article.
References
1. MacMahon PJ, Hogan BA, Shelley MJ, Eustace SJ, Kavanagh EC. Imaging of groin pain. Magn Reson Imaging Clin N Am. 2009;17(4):655-666. http://dx.doi.org/10.1016/j.mric.2009.06.013 [ Links ]
2. Koulouris G. Imaging review of groin pain in elite athletes: An anatomic approach to imaging findings. Am J Roentgenol. 2008;191(4):962-972. http://dx.doi.org/10.2214/AJR.07.3410 [ Links ]
3. Robinson P, Bhat V, English B. Imaging in the assessment and management of athletic pubalgia. Semin Musculoskelet Radiol. 2001;15(1):14-26. http://dx.doi.org/10.1055/s-0031-1271956 [ Links ]
4. Zajick DC, Zoga AC, Omar IM, Meyers WC. Spectrum of MRI findings in clinical athletic pubalgia. Semin Musculoskelet Radiol. 2008;12(1):3-12. http://dx.doi.org/10.1055/s-2008-1067933 [ Links ]
5. Khan W, Zoga AC, Meyers WC. Magnetic resonance imaging of athletic pubalgia and sports hernia. Current understanding and practice. Magn Reson Imaging Clin N Am. 2013;21(1):97-110. http://dx.doi.org/10.1016/j.mric.2012.09.008 [ Links ]
6. Orchard JW, Read JW, Neophyton J, Garlick D. Groin pain associated with ultrasound finding of inguinal canal posterior wall deficiency in Australian Rules footballers. Br J Sports Med. 1998;32(2):134-139. [ Links ]
7. Zoga AC, Kavanagh EC, Omar IM, et al. Athletic pubalgia and the 'sports hernia': MR imaging findings. Radiology. 2008;247(3):797-807. http://dx.doi.org/10.1148/radiol.2473070049 [ Links ]
 Correspondence:
Correspondence:
Peter Mercouris
580 Currie Road, Durban
4001, South Africa
Email:pmercouris@iafrica.com
Received: 11 Jun. 2014
Accepted: 22 Sep. 2014
Published: 11 Dec. 2014














