Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SA Journal of Radiology
On-line version ISSN 2078-6778
Print version ISSN 1027-202X
S. Afr. J. radiol. (Online) vol.18 n.1 Johannesburg Oct. 2014
http://dx.doi.org/10.4102/sajr.v18i1.695
REVIEW ARTICLES
Current radiological strategies for the assessment of right lower quadrant abdominal pain
Pumersha NaidooI; Bhugwan SinghII
IDepartment of Radiology, Nelson R. Mandela School of Medicine, University of KwaZulu-Natal, South Africa
IIDepartment of Surgery, Nelson R. Mandela School of Medicine, University of KwaZulu-Natal, South Africa
ABSTRACT
Right lower quadrant abdominal pain is a common clinical entity. Imaging and the radiologist play an integral role in achieving a diagnosis, so guiding prompt management of patients. This review discusses the spectrum of pathology and imaging findings, and highlights and contrasts the preferred imaging modalities in different subsets of patients.
Introduction
Right lower quadrant abdominal pain is a common clinical occurrence, with a wide spectrum of aetiologies that can present a diagnostic challenge for clinicians. Appendicitis is invariably the first differential diagnosis and most common cause of right lower quadrant pain. However, other considerations include infective, inflammatory and malignant conditions involving the ileo-caecal region, right colon, mesentery and surrounding anatomical structures.1HIV has affected the spectrum of pathology afflicting the right lower quadrant and altered the traditional diagnostic challenges presented by this anatomical region. The attendant clinician must be alert to this influence.
Imaging is currently at the forefront in assessing and diagnosing patients with right lower quadrant pain, thus guiding appropriate clinical management. Ultrasound (US) is the preferred imaging modality in children, pregnant women, and generally young patients, owing to the absence of ionising radiation. Advances in computed tomography (CT) with multiplanar reformations and 3D reconstruction have led to some clinicians considering multi-detector CT (MDCT) as the modality of choice when evaluating patients with right lower quadrant pain. CT is considered to be the first line imaging investigation for diffuse or peritonitic clinical pictures, and in elderly patients.1, 2
Magnetic resonance imaging (MRI) has an emerging imaging role in female patients being assessed for gynaecological diseases - during pregnancy for non-obstetric conditions - and in patients where iodinated contrast is contraindicated, as well as for the evaluation of Crohn's disease.1, 3, 4MRI offers short imaging protocols of approximately 10 minutes, and high contrast resolution, without the use of intravenous contrast or radiation burden. MRI and CT yield high sensitivities and specificities, without being user dependent.5
In this review, we consider the spectrum and typical imaging findings of common pathologies affecting the right lower quadrant. We highlight the preferred imaging modalities in accordance with the ALARA (as low as reasonably achievable) principle and diagnostic yield.1
Inflammatory and infective conditions
Acute appendicitis
Acute appendicitis is the most common non-traumatic abdominal emergency. However, only one-half of patients have a classical presentation (leucocytosis, fever and right lower quadrant pain), and the exact cause may be multifactorial. Currently, plain film radiography has a limited role, and has been superseded by US and CT.4MRI is beneficial in those patients for whom a CT scan is not warranted and for whom ultrasound is inconclusive.5Using high-frequency US with mild compression, an inflamed appendix is typically dilated - more than 6 mm in diameter. An appendicular wall thickness of more than 3 mm may be present with peri-appendicular or pericaecal hyperechogenicity - in keeping with fat infiltration from the inflammatory process (Figure 1).2
Typical CT features of an inflamed appendix, using multi-planar reconstruction (MPR), manifest as enlargement of the appendix (diameter > 7 mm), mural thickening and enhancement, and peri-appendiceal fat stranding (Figure 2).
Secondary signs include the presence of an appendicolith, focal wall thickening of the terminal ileum or caecum, and lack of gas and oral contrast within the appendix. Focal caecal wall thickening results in funnelling of oral contrast, termed the arrowhead sign. The complications associated with acute appendicitis include perforation, a peri-appendiceal abscess, pericaecal phlegmon, an extraluminal appendicolith, and small bowel obstruction (Figure 3).6, 7, 8
Distal appendicitis is diagnosed when a normal proximal appendix is visualised with an inflamed distal portion. A transition point is visualised with distal luminal narrowing and wall thickening or enlargement. Surrounding inflammatory changes are usually present; however, there is no caecal apical thickening or the arrowhead sign, as these are contiguous inflammatory changes. The normal appearance of the proximal appendix can lead to a missed diagnosis of distal appendicitis; therefore it is important to trace the appendix in its entirety.5, 9
Stump appendicitis is a rare complication of appendicectomy that can occur from 2 months to 50 years post-surgery. It occurs when the appendiceal remnant becomes inflamed. The imaging features are similar to acute appendicitis. The increased incidence of stump appendicitis is thought to be directly related to the length of the stump (longer stumps are more prone to infection) and the growing number of laparoscopic appendicectomies. It is important to remember that a past history of appendicectomy does not exclude appendicitis.10, 11
An appendicular mass or lump may be individualised; there can be adhesion of adjacent viscera (ileum, bladder, greater omentum) to the infectious location (Figure 4).2
Factors that complicate the diagnosis of appendicitis when using CT include lack of intra-abdominal fat or an unusual location of the caecum or appendix. Intra-abdominal fat acts as a natural contrast agent, allowing easy visualisation of an inflamed appendix. Therefore, in thin patients, the appendix may be difficult to visualise, leading to a false negative diagnosis of appendicitis. Since the caecum is a highly mobile structure and variable in position, locating the ileocaecal valve and accordingly then the appendix, may be beneficial. Multiplanar reconstruction (MPR) images are useful in visualising a retrocaecal, pelvic or transmesocolic appendix.6Two recent studies assessed the value of a non-visualised appendix in patients with clinically suspected appendicitis. They reported that the absence of a visualised appendix on CT almost excludes acute appendicitis (negative predictive value 98%).12, 13
Acute appendicitis is the most common gastrointestinal emergency requiring surgery in pregnant patients. The clinical manifestations in pregnancy are nonspecific and the caecum is displaced anteriorly and out of the pelvis, which makes visualisation of the appendix difficult. There is superior migration and rotation of the appendix as the pregnancy progresses, with the appendix frequently being found in the right upper quadrant.
There is a longstanding dilemma when considering the use of diagnostic imaging for evaluating pregnant patients with non-obstetric conditions such as acute appendicitis. Imaging modalities that do not make use of ionising radiation (such as US and MRI) are preferred as first options. If ionising radiation is to be used, a low radiation dose CT scan must be performed.3The American College of Radiology (ACR) criteria for evaluating pregnant patients for this clinical challenge include the use of targeted right lower quadrant US with graded compression as the first-line imaging modality, with MRI as second option, and followed by abdominal CT scan.3, 14
With targeted compression US, the appendix is better visualised in the first two trimesters. In the third trimester, detection can be improved by placing the patient in the left lateral decubitus position; however, this reduces sensitivity. The sonographic features are similar to a non-gravid patient.
If US evaluation is indeterminate and further imaging is clinically indicated, MRI may be undertaken.3MRI allows cross-sectional imaging with identification of appendicitis, and with no exposure to ionising radiation. With excellent soft-tissue contrast resolution, additional structures may be viewed, thereby excluding other sources of abdominal pain. On MRI, the imaging features of appendicitis include an appendiceal diameter > 7 mm, wall thickness > 2 mm, T2 high signal intensity in the wall and T2 hyperintensity in the peri-appendiceal fat stranding and surrounding fluid.4In the non-pregnant patient, contrast-enhanced and diffusion-weighted imaging may be of value - especially in patients who have equivocal wall thickness and no peri-appendiceal fat stranding. Strong contrast enhancement or restricted diffusion is indicative of appendicitis. In general, the major drawbacks of MRI are high cost, long imaging times and limited availability.5, 15
Appendicitis in pregnant patients is associated with premature labour, foetal mortality and a higher rate of perforation than in the general population. There should be no delay in the diagnosis. If MRI cannot be performed, CT of the abdomen and pelvis should be used as a second-line imaging modality. However, clinicians and radiologists must be aware of the theoretical risk of radiation-induced childhood cancer (approximately one cancer per 500 foetuses exposed to 30 mGy). Intravenous and oral contrast agents are preferred in some centres to improve visualisation of the appendix in pregnant patients.3, 15
Crohn's disease
Crohn's disease is a chronic relapsing auto-immune disorder. Whilst predominantly affecting young patients (between 15 and 30 years), it may occur in older patients up to 65 years of age. The disorder can manifest anywhere in the gastrointestinal tract. The ileocaecal region is the most affected and often mimics acute appendicitis. A CT scan excellently depicts the extent and severity of Crohn's disease. Typical CT scan findings include bowel wall thickening (generally > 1 cm), mucosal hyperenhancement, pericolonic fat stranding, and mural stratification owing to intramural oedema. Segmental involvement of the bowel with skipped normal areas are helpful in distinguishing Crohn's disease from ulcerative colitis. Further findings, such as engorgement of the vasa recta that penetrate the bowel wall (the comb sign), are an important feature of active disease (Figure 5).
Sclerolipomatous or fibrofatty proliferation along the mesenteric border of the affected bowel (the creeping fat sign) may be visualised. Mesenteric lymph nodes may also be present. Associated complications include fistulae, abscesses and small bowel strictures. With the aid of CT MPR, these complications are easily characterised (Figure 6).
Positive oral contrast agents may allow better depiction of fistulous tracts; however, this may obscure bowel wall hyperenhancement. MRI and MR enterography demonstrate similar bowel-related imaging findings noted on CT scan.
Owing to the young patient population affected by Crohn's disease and its chronicity, MRI is considered as the first-line imaging option in some centres, to reduce the radiation burden.1, 2, 16CT enterography and small bowel follow-through studies also have high appropriateness ratings in the diagnosis and monitoring of Crohn's disease.17MRI short tau inversion recovery (STIR) and T2-weighted sequences allow correct localisation of the inflammatory process and the extent of disease. Contrast-enhanced sequences can estimate the severity of the episode and also depict complications such as perforation and abscesses (Figure 7).
The use of diffusion-weighted imaging (DWI) appears to be promising, with restricted diffusion believed to be strongly correlated with severity and complications.5A recent study assessed the capability of MRI to quantitatively assess the response to therapy in Crohn's disease.18The results clearly showed the distinction between normal and pathological bowel wall, and depicted significant variation in bowel wall thickness and enhancement, so reflecting any favourable response to treatment.
Diverticulitis
Diverticulitis is a common cause of abdominal pain. When encountered in the right lower quadrant, it may be caused by diverticulitis in a loop of the sigmoid colon located in the right iliac fossa or, less commonly, the caecum or ascending colon. Typical features on CT include extensive pericolonic fat stranding (maximal at the site of the diverticulae), mesenteric fluid and bowel wall thickening with enhancement. It is important to differentiate diverticulitis from acute appendicitis; the key finding is visualisation of a normal appendix. Right-sided diverticulae are less common and frequently associated with a stercolith. Furthermore, ileal diverticulae are less frequent than colonic diverticulae; ileal diverticulae are located on the mesenteric border and are usually asymptomatic. When ileal diverticulae are inflamed, these must also be distinguished from appendicitis.
Complications of diverticulitis include fistulae, abscesses, free perforation and bowel obstruction (Figure 8).1, 2, 16
CT is an effective imaging modality that enables prompt diagnosis. Using coronal STIR MRI sequences, the area of inflammation can also be readily identified. Guided by this, bowel wall thickening, diverticulae and a narrowed lumen can be visualised. The inflamed areas will enhance on the post-contrast images and complications can be readily detected.5
Tuberculous enterocolitis
Tuberculosis (TB) is endemic in the South African population, with a marked increase resulting from the AIDS epidemic. TB involvement of the gastrointestinal tract is well recognised, with the ileocaecal region most commonly affected (Figure 9).
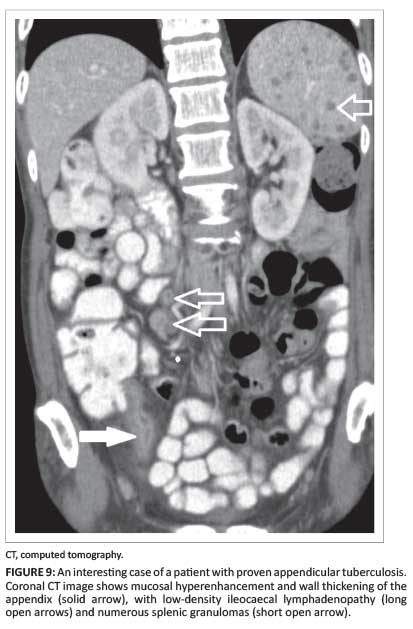
With barium studies, an early manifestation is spasm and hypermobility, with oedema of the ileocaecal valve leading to its incompetence (Figure 10).

The caecum and terminal ileum are usually both affected; the CT features are concentric mural thickening and enhancement, which may cause luminal narrowing leading to proximal bowel dilatation and obstruction (Figure 11).
Advanced gastrointestinal TB characteristically appears as napkin ring stenosis, with a conically shaped, shrunken caecum retracted out of the right iliac fossa.19
It can be a radiological and clinical challenge to differentiate TB from Crohn's disease, considering the overlap in clinical presentation and imaging features (Table 1). This is important as it has significant therapeutic implications.20
Epiploic appendagitis
First described by Lynn et al. in the mid-1950s, epiploic appendagitis is a well-recognised cause of pain in the right lower quadrant.2, 21It is thought to be caused by inflammatory and ischaemic changes secondary to torsion or venous thrombosis of the epiploic appendages. The diagnosis is usually established with CT, allowing early recognition and conservative management. The CT appearance is that of an oval lesion of fat density with a hyperattenuating rim. Pericolonic fat attenuation and wall thickening of the adjacent colon may also be present (Figure 12).1, 17, 21
Right lower quadrant pain associated with immunosuppression
Neutropaenic colitis (typhilitis)
Neutropaenic colitis usually occurs in patients receiving chemotherapy for malignancies such as leukaemia, and for other immunosuppressive states. Clinically, it manifests with right lower quadrant pain, fever, diarrhoea and sometimes peritonitis. CT is considered the study of choice, and the features include caecal dilatation, circumferential wall thickening, intramural air and pericaecal fat stranding and fluid (Figure 13).
The presence of pneumoperitoneum, pneumatosis, gastrointestinal bleeding and fluid collections may require urgent surgical care. In an immunocompromised patient with symmetrical and circumferential caecal wall thickening, neutropaenic colitis should be suggested first.1, 2, 16
Right lower quadrant pain associated with neoplastic conditions
Lymphoma
Ileocaecal lymphoma is not uncommon. The four forms of ileocaecal lymphoma are the circumferential, polypoid, ulcerative and aneurysmal varieties. Ileocaecal lymphoma usually manifests as areas of bowel wall thickening with uniform attenuation and poor enhancement. Long segments of bowel involvement may be demonstrated. Signs of bowel obstruction are uncommon. The polypoidal variety can act as lead point for intussusception. The ulcerative form can develop fistulous tracts with adjacent structures. The aneurysmal form may demonstrate dilatation of the lumen of the bowel or cavity of the lymphoid mass. Enlarged mesenteric and retroperitoneal lymph nodes are common (Figure 14).1
Colonic carcinoma
Most colorectal carcinomas are adenocarcinomas. In comparison with the left colon, and owing to the larger calibre of the right colon, tumours in the latter location can grow to a large size without causing bowel obstruction (Figure 15).
Patients may present with rectal bleeding, anaemia or a palpable mass.1, 16CT scanning (MDCT and CT colonography) can be used for screening of colon carcinoma for the staging of the disease, for assessing and staging of recurrent disease, and also for detection of distant metastases.22Carcinomas may demonstrate variable appearances, and perforation can occur, leading to peritonitis or intraperitoneal abscess formation (Figure 16).
Abscess formation and peritonitis may simulate an inflammatory process rather than a malignancy (Figure 17).1
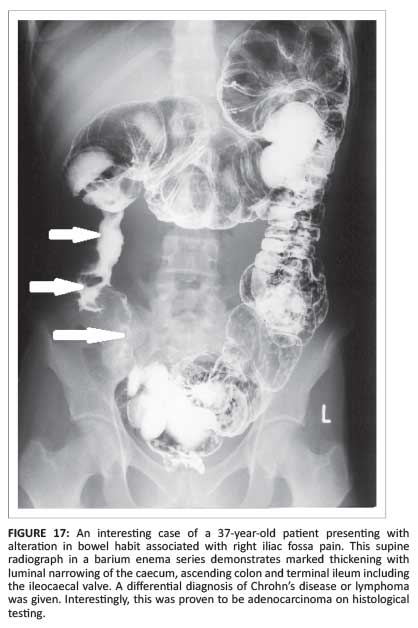
Right lower quadrant pain associated with gynaecological diseases
Pelvic inflammatory disease
Pelvic inflammatory disease (PID) is seen in sexually active female patients and manifests as lower abdominal pain. The source of infection is usually an ascending lower genital tract infection. PID encompasses endometritis, salpingitis and tubo-ovarian abscesses. Neisseria gonorrhoea and Chlamydia trachomatis are the most common pathogens.23
US may demonstrate loss of normal tissue planes and an ill-defined uterus. Thickening of the endometrium may be present, but is nonspecific. Fluid may also be seen in the endometrial cavity. Salpingitis may progress to hydro- or pyosalphinx, and is usually visualised as complex fluid with echogenic debris distending the fallopian tubes. At a later stage, a tubo-ovarian abscess may form.23
On CT, a complex hypodense fluid collection with thickened and irregular walls of a tubo-ovarian complex, is seen within the pelvis (Figure 18).23
MRI STIR and T2-weighted images may demonstrate a cystic enlarged ovary. On T2-weighted images, signal hyperintensity can be localised within the parametrial tissues. A tubo-ovarian abscess appears with mild T1 hyperintensity and high signal intensity on T2-weighted images. Post-contrast MR images demonstrate a thick, enhancing wall of the abscess - with or without an adjacent hydrosalpinx.5, 17
Endometriosis
Endometriosis is a chronic gynaecological disorder characterised by growth of endometrial tissue outside the endometrial cavity - primarily in the pelvis, peritoneum and ovaries.24This ectopic mucosa undergoes cyclical hormonal changes and also bleeds, forming haemorrhagic cysts (Figure 19).

Although US can visualise these lesions, CT and MRI are better for evaluating and characterising them. MRI has a greater sensitivity owing to the detection of blood and blood products. These appear as T1 hyperintensities, also known as the light bulb appearance on fat suppression sequence, which results from the intracellular methaemoglobin.
On T2-weighted images, endometriomas appear hypointense. This hypointense signal can also be described as shading that completely occupies the cyst or is seen as a dependent layer. It is thought to be the result of high concentrations of protein and iron from recurrent haemorrhages.17Minimal enhancement is demonstrated on post-contrast scans (Figure 20).24
Endometriomas are demonstrated on non-contrast CT scan as areas of hyperattenuation with solid and cystic heterogenous adnexal masses and fluid-fluid levels within the cysts. Cysts often rupture, leading to haemoperitoneum. The sonographic appearance of endometrioma demonstrates a uniform, low-level echogenicity or a ground glass appearance. The rupture of endometriomas may simulate complex masses, which can make diagnosis challenging.17, 23
Ectopic pregnancy
When patients present with features suggestive of an ectopic pregnancy, hormonal (β-hCG) levels and pelvic US should be performed. Transvaginal US is the preferred method of evaluation, although abdominal US can demonstrate ectopic pregnancies when β-hCG levels exceed 6 500 mIU/ml.25Tubal pregnancies are the most common ectopic location. On MRI, a tubal pregnancy is described as a sac-like, cystic tubal structure with a T2 hyperintense thick wall. The cystic sac may demonstrate T1 hyperintense to intermediate signal intensity, depending on the haemorrhagic component. It is thought that intravenous contrast may help to confidently diagnose an ectopic pregnancy, but contrast is rarely administered in pregnant patients. T2 hyperintensity or T1 hyperintensity may represent free fluid or haemoperitoneum within the abdomen.26Approximately 35% of ectopic pregnancies may not demonstrate any adnexal abnormalities (Figure 21).25
It is crucial to differentiate normal pregnancy from ectopic pregnancies with the use of US (Table 2).
Right lower quadrant pain associated with miscellaneous causes
Intussusception
Intussusception is not common in adults; it presents as vague abdominal pain, and occurs when a proximal segment of bowel (intussusceptum) telescopes into an adjacent distal segment (intussuscipiens) (Figure 22).
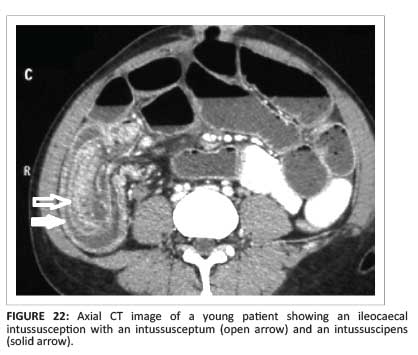
In adults, there is often an underlying lead point such as benign or malignant neoplasms (e.g. lipoma, polyps, lymphoma, carcinoma, metastases and leiomyomas). In contrast with children, operative treatment is usually necessary in adults.1, 16, 27Gayer et al. report an increased incidence of intussusception in patients with AIDS; compare the association of AIDS with numerous infectious and neoplastic conditions (infectious enteritis, Kaposi's sarcoma, non-Hodgkin's lymphoma). Intussusception should be considered in AIDS patients with prolonged abdominal pain.27Although diagnosis can be made using other imaging modalities (including barium enema, US and gastrointestinal series), CT is considered the modality of choice. Not only can the diagnosis be made accurately, but the cause and complications - such as bowel obstruction - can be assessed (Figure 23). The three typical characteristics are the reniform appearance, sausage appearance and target-shaped bowel-within-bowel appearance.1, 16, 27
Caecal volvulus
Caecal volvulus is seen in patients with an abnormally mobile caecum; this allows twisting along the long axis, leading to bowel obstruction. Three types of caecal volvulus have been described:
- type 1: the caecum twists in the axial plane, rotating along its long axis
- type 2: the distended caecum twists and inverts
- type 3: caecal bascule - the distended caecum folds anteriorly, without torsion.
The diagnosis of caecal volvulus and its complications (ischaemia and obstruction) can be readily made using MDCT. A distended caecum and swirl of mesenteric vessels is demonstrated in types 1 and 2 caecal volvulus. Concentric wall thickening, mesenteric fat stranding, and pneumatosis intestinalis are all signs related to complications.1
In addition to the causes of right lower quadrant pain enumerated and discussed above, six other causes are listed, together with their respective imaging findings, in Table 3.
Diagnostic algorithm
There is a wide spectrum of conditions affecting the right lower quadrant, some with disease-specific investigations and imaging modalities. Therefore it is vital that a structured guideline be used. The Department of Health in Western Australia has devised several diagnostic imaging pathways as a guide for their practitioners. These pathways are reviewed and updated periodically. The imaging pathway for right iliac fossa pain is particularly pertinent for use in the South African medical setting as it is practical and takes into consideration local availability and imaging constraints (Figure 24).
Conclusion
Right lower quadrant pain is a common clinical situation. When considering imaging, age and sex of the patient are essential factors, as the differential diagnoses may differ.2ACR criteria still rate US and CT as the primary imaging modalities for evaluating acute abdominal and pelvic conditions such as appendicitis, diverticulitis, PID and ectopic pregnancy.5US is clearly preferred in young and pregnant patients, whilst CT is considered first-line imaging for the elderly and those with peritonism.2MRI is not the modality of choice in all patients, but is a method with high accuracy and may be beneficial in a subset of patients for whom CT is not warranted.5All these imaging modalities are of value under certain circumstances, and must not oppose each other but rather have complementary functions, which will allow precise diagnosis and prompt management of patients presenting with right lower quadrant pain.1, 2
Acknowledgements
We thank Dr J. Maharajh and Dr A. Mitha for their help in compiling the images.
Competing interests
The authors declare that they have no financial or personal relationship(s) that may have inappropriately influenced them in writing this article.
Authors' contributions
Both authors have contributed in various degrees to the article produced. P.N. (University of KwaZulu-Natal) was responsible for the study conception and design, acquisition and analysis of data and drafting of manuscript. B.S. (University of KwaZulu-Natal) was responsible for the analysis and interpretation of data and the critical revision of manuscript.
References
1. Purysko AS, Remer EM, Leão Filho HM, Bittencourt LK, Lima RV, Racy DJ. Beyond appendicitis: Common and uncommon gastrointestinal causes of right lower quadrant abdominal pain at multidetector CT. Radiographics. 2011;31(4):927-947. http://dx.doi.org/10.1148/rg.314105065 [ Links ]
2. Millet I, Alili C, Pages E, et al. Infection of the right iliac fossa. Diagn Interv Imaging. 2012;93:441-452. http://dx.doi.org/10.1016/j.diii.2012.04.026 [ Links ]
3. Patel SF, Reede DL, Katz DS, et al. Imaging the pregnant patient for non-obstetric conditions: Algorithms and radiation dose considerations. Radiographics. 2007;27:1705-1722. http://dx.doi.org/10.1148/rg.276075002 [ Links ]
4. Spalluto LB, Woodfield CA, DeBenedectis CM, et al. MR imaging evaluation of abdominal pain during pregnancy: Appendicitis and other nonobstetric causes. Radiographics. 2012;32:317-334. http://dx.doi.org/10.1148/rg.322115057 [ Links ]
5. Heverhagen JT, Klose KJ. MR imaging for acute lower abdominal and pelvic pain. Radiographics. 2009;29:1782-1796. http://dx.doi.org/10.1148/rg.296095518 [ Links ]
6. Kin HC, Yang DM, Fin W, et al. Added diagnostic value of multiplanar reformation of multidetector CT data in patients with suspected appendicitis. Radiographics. 2008;28:393-406. [ Links ]
7. Simpson J, Scholefield JH. Acute appendicitis. Surgery. 2008;26(3):108-112. http://dx.doi.org/10.1016/j.mpsur.2008.01.003 [ Links ]
8. Rao PM, Wittenberg J, McDowell RK, et al. Appendicitis: Use of the arrowhead sign for diagnosis at CT. Radiology. 1997;202:363-366. http://dx.doi.org/10.1148/radiology.202.2.9015058 [ Links ]
9. Rao PM, Rhea JT, Novelline RA. Distal appendicitis: CT appearance and diagnosis. Radiology. 1997;204:709-712. http://dx.doi.org/10.1148/radiology.204.3.9280247 [ Links ]
10. Shin LK, Halpern D, Weston SR, et al. Prospective CT diagnosis of stump appendicitis. AJR. 2005;184:S62-S64. http://dx.doi.org/10.2214/ajr.184.3_supplement.01840s62 [ Links ]
11. Sharma M, Agrawal A. Pictorial essay: CT scan of appendicitis and its mimics causing right lower quadrant pain. Indian J Radiol Imaging. 2008;18:80-89. http://dx.doi.org/10.4103/0971-3026.37051 [ Links ]
12. Ganguli S, Raptopoulos V, Komlos F, et al. Right lower quadrant pain: Value of the nonvisualised appendix in patients at multidetector CT. Radiology. 2006;241:175-180. http://dx.doi.org/10.1148/radiol.2411050191 [ Links ]
13. Nikolaidis P, Hwang CM, Miller FH, et al. The nonvisualised appendix: incidence of acute appendicitis when secondary inflammatory changes are absent. AJR. 2004;183:889-892. [ Links ]
14. Tkacz FN, Anderson SA, Soto F. MR imaging in gastrointestinal emergencies. Radiographics. 2009;29:1767-1780. http://dx.doi.org/10.1148/rg.296095509 [ Links ]
15. Pedrosa I, Levine D, Eyvazzadeh AD, et al. MR imaging evaluation of acute appendicitis in pregnancy. Radiology. 2006;238:891-899. http://dx.doi.org/10.1148/radiol.2383050146 [ Links ]
16. Silva A, Beaty SD, Hara AK, et al. Spectrum of normal and abnormal CT appearances of the ileocecal valve and cecum with surgical correlation. Radiographics. 2007;27:1039-1054. http://dx.doi.org/10.1148/rg.274065164 [ Links ]
17. Singh A, Danrad R, Hahn PF, et al. MR imaging of the acute abdomen and pelvis: Acute appendicitis and beyond. Radiographics. 2007;27:1419-1431. http://dx.doi.org/10.1148/rg.275065021 [ Links ]
18. Sempere GA, Sanjuan VM, Chulia EM, et al. MR evaluation of inflammatory activity in Crohn's disease. AJR. 2005;184(6):1829-1835. http://dx.doi.org/10.2214/ajr.184.6.01841829 [ Links ]
19. Burrill J, Williams CF, Bain G. Tuberculosis: A radiologic review. Radiographics. 2007;27:1255-1273. http://dx.doi.org/10.1148/rg.275065176 [ Links ]
20. Pulimood AB, Amarpurkar DN, Ghoshal U, et al. Differentiation of Crohn's disease from intestinal tuberculosis in India in 2010. World J Gastroenterol. 2011;17(4):433-443. http://dx.doi.org/10.3748/wjg.v17.i4.433 [ Links ]
21. Bunni J, Corrigan A, Jacob K, et al. Epiploic appendagitis: A case report highlighting correlation between clinical features, computed tomography images and laparoscopic findings. Int J Surg. 2010;8:401-403. http://dx.doi.org/10.1016/j.ijsu.2010.04.010 [ Links ]
22. Taylor CR, Pfeifer KE, Wang SY. Imaging in adenocarcinoma of the colon [homepage on the Internet]. [ Links ] No date [cited 2013 Aug. 7]. Available from http://emedicine.medscape.com/article/367061-overview
23. Potter AW, Chandrasekhar CA. Ultrasound and CT evaluation of acute pelvic pain of gynaecological origin in nonpregnant premenopausal patients. Radiographics. 2008;28:1645-1659. http://dx.doi.org/10.1148/rg.286085504 [ Links ]
24. Chamie LP, Blasbalg R, Pereira RMA, et al. Findings of pelvic endometriosis at transvaginal US, MR imaging and laparoscopy. Radiographics. 2011;31:77-100. http://dx.doi.org/10.1148/rg.314105193 [ Links ]
25. Lin PE, Bhatt S, Dogra VS. Diagnostic clues to ectopic pregnancy. Radiographics. 2008;28:1661-1671. http://dx.doi.org/10.1148/rg.286085506 [ Links ]
26. Parker III RA, Yano M, Tai AW, et al. MR imaging findings of ectopic pregnancy: A pictorial review. Radiographics. 2012;32:1445-1460. http://dx.doi.org/10.1148/rg.325115153 [ Links ]
27. Gayer G, Zissin R, Apter S, et al. Adult intussusception - a CT diagnosis. Br J Radiol. 2002;75(890):185-190. http://dx.doi.org/10.1259/bjr.75.890.750185 [ Links ]
28. Angelelli G, Scardapane A, Memeo M, et al. Acute bowel ischemia: CT findings. Eur J Radiol. 2004;50(1):37-47. http://dx.doi.org/10.1016/j.ejrad.2003.11.013 [ Links ]
29. Brandt LJ, Feuerstadt P, Blaszka MC. Anatomic patterns, patient characteristics, and clinical outcomes in ischemic colitis: A study of 313 cases supported by histology. Am J Gastroenterol. 2010;105(10):2245-2252. http://dx.doi.org/10.1038/ajg.2010.217 [ Links ]
30. Romano S, Romano L, Grassi R. Mulidetector row computed tomography findings from ischemia to infarction of the large bowel. Eur J Radiol. 2007;61(3):433-441. http://dx.doi.org/10.1016/j.ejrad.2006.11.002 [ Links ]
31. Stark JE, Siegel MJ. Ovarian torsion in prepubertal and pubertal girls: Sonographic findings. AJR. 1994;63:1479-1482. http://dx.doi.org/10.2214/ajr.163.6.7992751 [ Links ]
32. Vijayaraghavan SB. Sonographic whirlpool sign in ovarian torsion. J Ultrasound Med. 2004;23:1643-1649. [ Links ]
33. O'Conner OJ, Maher MM. Imaging of cholecystitis. AJR. 2011;196(4):W367-W374. http://dx.doi.org/10.2214/ajr.10.4340 [ Links ]
34. Kambadakone AR, Eisner BH, Catalano A, et al. New and evolving concepts in the imaging and management of urolithiasis: Urologists' perspective. Radiographics. 2010;30:603-623. http://dx.doi.org/10.1148/rg.303095146 [ Links ]
35. Takahashi N, Vrtiska TJ, Kawashima A, et al. Detectability of urinary stones on virtual non-enhanced images generated at pyelographic-phase dual-energy CT. Radiology. 2010;256(1):184-190. http://dx.doi.org/10.1148/radiol.10091411 [ Links ]
36. Macari M, Hines J, Balthazar E, et al. Mesenteric adenitis: CT diagnosis of primary versus secondary causes, incidence, and clinical significance in pediatric and adult patients. AJR. 2002;178:853-858. http://dx.doi.org/10.2214/ajr.178.4.1780853 [ Links ]
37. Lucey BC, Stuhlfaut JW, Soto FA. Mesenteric lymph nodes seen at imaging: Causes and significance. Radiographics. 2005;25:351-365. http://dx.doi.org/10.1148/rg.252045108 [ Links ]
38. Puylaert JBCM. Right-sided segmental infarction of the omentum: Clinical, US, and CT findings. Radiology. 1992;185:169-172. [ Links ]
39. Pereira JM, Sirlin CB, Pinto PS, et al. Disproportionate fat stranding: A helpful CT sign in patients with acute abdominal pain. Radiographics. 2004;24:703-715. http://dx.doi.org/10.1148/rg.243035084 [ Links ]
40. Department of Health Western Australia. Diagnostic Imaging Pathways [homepage on the Internet]. Available from http://imagingpathways.health.wa.gov.au [ Links ]
 Correspondence:
Correspondence:
Pumersha Naidoo
25 The Curl, Sunningdale
Durban 4051, South Africa
Email: pumershanaidoo@gmail.com
Received: 18 July 2014
Accepted: 14 Sept. 2014
Published: 05 Dec. 2014














