Servicios Personalizados
Articulo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en Google
Similares en Google
Compartir
Health SA Gesondheid (Online)
versión On-line ISSN 2071-9736
versión impresa ISSN 1025-9848
Health SA Gesondheid (Online) vol.19 no.1 Cape Town ene. 2014
ORIGINAL RESEARCH
The GAMMA® nursing measure: Its development and testing for nursing utility
Hendrik J. LoubserI; Judith C. BruceII; Daleen CasteleijnIII
ISouth African Database for Functional Medicine, South Africa
IISchool of Therapeutic Sciences, University of the Witwatersrand, South Africa
IIIDepartment of Occupational Therapy, University of the Witwatersrand, South Africa
ABSTRACT
BACKGROUND: In the specialised nursing fields of gerontology, oncology, rehabilitation and home-based care where people live with permanent or temporary disabilities, nurses are I unable to perform routine and empirical scoring of their patients' abilities to live independently, because of the lack of valid nursing measures indicating patients' frailty or vulnerability. These independent living abilities are also referred to as the instrumental activities of daily I living (IADLs).
OBJECTIVES: To provide nurses with a nursing scale, named the GAMMA, which enables nurses I to routinely observe, score and record their patients' IADLs and to test its nursing utility.
METHOD: A study with two sequential phases was done. Firstly, descriptive data were collected I from key informants, namely a registered social worker and two registered nurses, skilled in caring for disabled persons living in long-term care facilities. The data were analysed using inductive content analysis techniques in order to design and construct the GAMMA nursing scale. In the second study, the utility of the GAMMA was studied by training and testing the application of the GAMMA within a group of registered nurses (n = 5) working in three I retirement villages. After four months, focus group interviews were conducted with the registered nurses in order to explore the GAMMA's nursing utility. Descriptive data were analysed using deductive content analysis techniques.
RESULTS: The outcome of the study provided good results. High levels of agreement between I participants confirm the GAMMA's acceptance, usefulness and confidence as a nursing scale to empirically establish the transition of nursing care between independent living and assisted living.
CONCLUSION: The GAMMA has the characteristics which allow it to be used routinely as a nursing scale in gerontology, oncology, rehabilitation and home-based care nursing processes.
OPSOMMING
AGTERGROND: In die gespesialiseerde verpleegareas van gerontologie, onkologie, rehabilitasie en tuisversorging waar pasiënte leef met permanente of tydelike gestremdhede, is verpleegkundiges nie in staat om gereeld en empiries te bepaal wat hul pasiënte se vermoëns is om onafhanklik te lewe, as 'n aanduiding van hul verswaktheid of broosheid nie. Die vermoëns om onafhanklik te lewe word ook na verwys na as die instrumentele aktiwiteite van daaglikse lewe (IADLs).
DOELWITTE: Om die verplegingswetenskappe te voorsien van 'n skaal, genoemd die GAMMA, wat die verpleegkundige in staat kan stel om as roetine prosedure pasiënte se IADLs waar te neem, te meet en te noteer, en om die nuttigheid van hierdie skaal vir verpleging te bepaal.
METODE: 'n Studie met twee opeenvolgende fases was gedoen. Eerstens was 'n ondersoek geloods om beskrywende data te versamel van 'n geregistreerde maatskaplike werker en twee geregisteerde verpreegkundiges wat ervare is in die versorging van gestremde mense wat in lang termyn fasiliteite woon. Die data was geanaliseer met induktiewe inhoudstegnieke om die konstruksie van die GAMMA te ontwikkel. In die tweede studie was die GAMMA se bruikbaarheid vir verpleegkundiges bestudeer deur eers opleiding en toetsing aan geregistreede verpleegkundiges (n = 5) te bied in drie aftree oorde. Vier maande na implementasie het 'n fokus groep met die geregistreede verpleegkundiges vergader om die die GAMMA se nuttigheid vir verpleegkundiges te evalueer. Beskrywende data was geanaliseer met behulp van deduktiewe inhouds analiese tegnieke.
RESULTATE: Die uitkoms van die GAMMA het goeie resultate opgelewer. Daar was hoë vlakke van aanvaarding, betroubaarheid en vertroue in die GAMMA as 'n empiriese verplegingsskaal om die oorgang tussen onafhanklike en ondersteunende lewenstyl te bepaal.
GEVOLGTREKKING: Die GAMMA het die eienskappe om as roetine prosedure gebruik te word as 'n verplegingsskaal in die gerontologie, onkologie, rehabilitasie en tuisversorging verplegingsprosesse.
Introduction
Background
All longitudinal studies exploring a person's degree of frailty or vulnerability should include the patient's ability to live independently in their chosen environment, usually their own home. The independent living abilities are also referred to as the instrumental activities of daily living (IADLs). Although most research in the area of IADLs continues to be in the science of gerontology, insights into IADLs are also valuable in the rehabilitation sciences, convalescent care and for people living with physical, mental or intellectual disabilities.
The first IADL scoring framework was published in 1969 by Lawton and Brody in their classic article, Assessment of older people: self-maintaining and instrumental activities of daily living, using the phrase 'instrumental activities of daily living'. IADLs are human functions that underpin and sustain more nuanced and complex social activities than the well-known activities of daily living (ADLs). The original Lawton and Brody IADL items include the abilities to use a phone, do shopping, prepare food, do housekeeping, do laundry and to manage one's own transportation, medication and finances. These IADLs are considered to be the minimal daily functions a person must be capable of in order to live independently. Losing one or more of these activities increases the risks with regard to living independently. This correlation between IADL measures and the ability to live independently unlocks the possibility for the nurse practitioner to both measure and quantify the nebulous concept of frailty and vulnerability from its onset and through its progression. Although the terms frailty and vulnerability are mostly associated with the end stages of the ageing process, they also refer to disabled and vulnerable people who are not necessarily old.
According to Pel-Littel et al. (2009), nearly all studies in clinical frailty report deterioration in the person's IADLs. The most common characteristic associated with the elderly person's frailty is an unstable physical and mental condition and diminished physical reserves. When these reserves are exhausted, the decline in daily functioning manifests itself. Markle-Reid and Browne (2003) refer to this critical point where the balance is disturbed as being the indicator that the frailty threshold has been exceeded. Thus, the extent to which deterioration of IADLs is detected becomes a determinant of the onset of frailty in elderly or disabled persons.
According to Lynch (2004), physical ageing is associated with a progressive loss of muscle anabolic hormones and growth factors, leading to loss of muscle mass (sarcopenia), a slowing of movement and a decline in strength. These factors increase the risk of injury from sudden falls in the frail elderly and leads to growing dependence on others to accomplish even the most basic tasks required for independent living. There is a debate as to whether these intrinsic changes are immutable or reversible. However, there is a definite need for restorative nursing strategies that can slow the effects of ageing on muscle function and restore muscle size and strength in the frail elderly in order to maintain or even improve their quality of life.
The consequences of frailty are usually measured in terms of mortality, morbidity and institutionalisation. The frail population, as a result of either the ageing process or disability, are vulnerable to increasing dependence and are at a higher risk of being institutionalised (Bandeen-Roche et al. 2006). They therefore risk a lower quality of life than their non-frail peers (Strawbridge et al. 1998). Their unstable physical and mental condition and diminished physical reserves also leave the frail elderly vulnerable to illnesses and at risk of injuries requiring admission to acute nursing care settings (Van Helden et al. 2008). Pel-Littel et al. (2009) report an absence of a gold standard to measure frailty, meaning that it is not yet possible to comment on the validity and reliability of the diagnosis of frailty. Although a limited number of total frailty tests have been developed, little is known about their validity.
Problem statement
The consequences to the nursing profession of not being able to measure physical frailty and vulnerability mostly relate to the planning and management of nursing services to these populations. In South Africa, the gerontological nursing services have a structured approach in supporting the independent living needs of elderly persons. This usually starts with periodic home visits to older persons living independently in order to assess their needs for supportive services. These nurses are known as 'cottage nurses' in the retirement village industry. If nursing support is required and rendered, allowing the older person to continue to live independently, the person is considered to be receiving 'assisted living nursing services'. When the burden of rendering assisted living services reaches a distinctive peak, the older person is triaged, depending on the need, to either frail- or Alzheimer-institutionalised living nursing services. Finally, the end-of-life care needs are taken care of, with an emphasis on dignity preservation. These levels of care, settings and services are all managed by the nursing profession and are based on rendering functional support to the elderly person. However, without an empirically-sound measurement of elderly persons' functional abilities to live independently, the triaging of an elderly person between these interfaces remains subjective and often becomes a matter for debate between the elderly, their families, the nurse and the management team of the retirement village. This is even more so when the high costs of rendering assisted living and frail care are taken into consideration.
Purpose and objectives
The purpose of this study was to avail nurses with an objective and useful nursing scale that can be used routinely to score their patients' IADLs. To achieve this, two objectives were identified, each to be achieved in sequential phases:
• Firstly, to design and develop the GAMMA as a nursing scale that will allow the nurses to observe, score and record their patients' IADLs routinely. • Secondly, to test whether the GAMMA has nursing utility, that is, whether the GAMMA is acceptable enough to the nurses, to the extent that they would embrace it as a useful nursing scale to be used routinely.
Significance
Restorative nursing activities include the observation of frail and vulnerable persons performing their daily IADLs, whilst scoring and recording their performance of these activities. Nursing auxiliaries (NAs) and caregivers (CGs) provide 90% of the care at this patient-nurse interface (Resnick 2004), but they are currently unable to provide a scoring for the daily IADLs as no such nursing scale exists. This leaves the nurses without any empirical data regarding patient frailty and vulnerability on which to base their restorative nursing assessments and care plans. Furthermore, there are no routine longitudinal datasets on patients' restorative outcomes. This study will contribute to such data and resolve this paucity.
Definition of key concepts
GAMMA
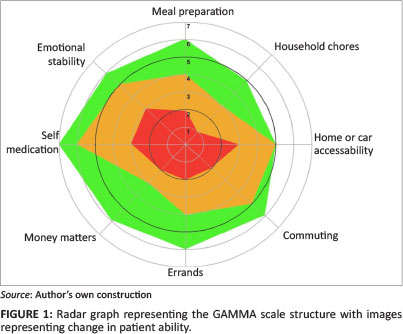
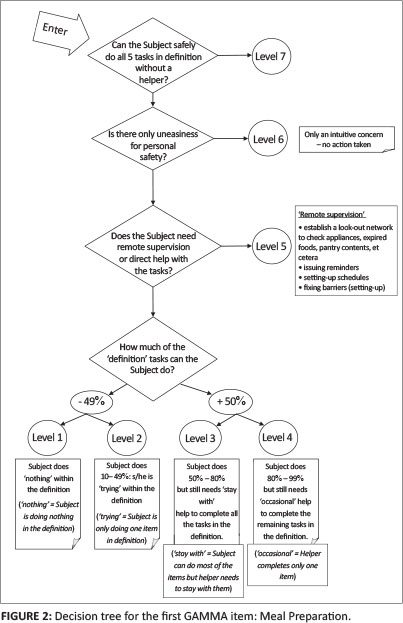
The name GAMMA refers to the third letter in the Greek alphabet and is the third in a suite of routine nursing measures being developed by the researchers. In Figure 1, a graphic impression of the items measured in the GAMMA is presented and in Figure 2, a decision tree is presented in order to illustrate how nurses arrive at these categories.
Restorative nursing
Sister Verah McIver, in 1967, created an ability-enhancing nursing model through training programmes for NAs and management and supervision programmes for registered nurses in charge of units. She called it the Restorative Nursing Care Model. Contemporary definitions refer to it as an enabling nursing process aimed at promoting physical and personal independence in order to restore the dignity and wholeness of the patient or disabled person (Mantle & Funke-Furber 2003).
Nursing utility
The utility of an instrument is the degree of conviction the users have regarding its usefulness in their professional practice (Toomey, Nicholson & Carswell 1995), taking into consideration application practicalities such as relevance, suitability, feasibility, accuracy, comprehensiveness, credibility, flexibility, value and adaptability (Barbara & Whiteford 2005). As the GAMMA is intended to serve the nursing profession, this article would refer to its nursing utility.
Scale versus measure
In general, the terms 'scale', 'instrument', 'test', 'tool' and 'questionnaire' may all refer to the concept of producing numerical scores in order to explain a phenomenon at an ordinal level (Bond & Fox 2007). However, none of these terms refers to a 'measure', which identifies a higher level of measurement qualities, namely linear interval characteristics
(Stevens 1946). During its development, the GAMMA is ordinal in nature and should be referred to as a 'scale'. Only when the GAMMA's construct validation with Rasch analyses has been proven successful, may it be referred to as a 'measure' (Loubser 2012).
Patients
For the sake of uniformity, 'patients' include all clients, residents, persons, elderly persons and people living with intellectual, physical and/or mental disabilities receiving any extent of nursing care.
Independent living
Independent living refers to patients who have the ability, self-reliance and self-confidence to continue living in their own home without supervision or support.
Assisted living
Assisted living refers to patients living with frailty, disability or an impairment that requires on-going supervision and support in order to continue living in their own home.
Registered nurse
A registered nurse (RN) is a person who has completed a four-year academic programme in nursing or a two-year bridging programme at an accredited Nursing Education Institution (NEI) and who is registered with the South African Nursing Council.
Nursing auxiliary
A nursing auxiliary is a person who has completed a one-year academic programme at an approved nursing school and who is enrolled with the South African Nursing Council as a nursing auxiliary.
Research method and design
A study with two sequential phases, as described below, was executed sequentially in order to satisfy the two objectives mentioned previously.
First phase: Development of the GAMMA
Research design
A qualitative, exploratory and contextual research design was followed in the development of the GAMMA. Qualitative research seeks to understand the actions and processes within the specific context of restorative nursing for persons requiring assistance with regard to living independently. Explorative research actively examines this interface as the specific phenomenon of interest rather than merely observing and reporting (Lobelo 2004:20). A panel of experts in assisted living were selected purposively to be involved in the review of existing instruments and their revision and development so as to comply with nursing utility specifications. The participation of experts, according to Foxcroft et al. (2004), contributes significantly to the content validity of the expected scale.
Sampling
At the onset of the study, three key informants were selected based on their expertise in restorative care. They were a social worker with extensive practical experience in designing restorative methods for people with intellectual disabilities to live independently and two RNs. The first RN had 17 years' experience working as a 'cottage nurse' in a large retirement village; and the second RN had 11 years' experience working in the community rendering home-based care to patients requiring convalescent care after discharge from acute or subacute facilities. These three participants were selected purposively for their expert intuitive knowledge gained from their extensive experience in the restorative care of three diverse groups of patients, all at risk of frailty and vulnerability and thus requiring similar considerations.
Data collection
Unstructured individual interviews were held with each of the key informants so as to explore and understand what their daily tasks entailed, why they were doing what they were doing, what they hoped to achieved and, finally, how they knew they were successful in what they were doing. The discussions were open but at the same time focused on probing their perceptions of what is considered to be improvement or decline and how they could recognise a change in the patient's ability to live independently. These interviews were recorded and transcribed and field notes were taken.
Following key informant interviews and the documentation of the data, the Lawton Scale (Lawton & Brody 1969) was introduced to each informant individually in order to verify its usefulness in their work environment. Their individual responses were documented carefully in field notes.
Data analysis
When data saturation had been achieved, the interviews were stopped and data analysis commenced. An inductive content analysis technique was used as no previous studies were found to have dealt with this particular phenomenon. Firstly, using the Lawton Scale as the departure point, consensus was achieved on the core items that infer to the wider concept of independent living. Consensus was achieved on eight items, which then served as the coded descriptive dataset for content analysis. This was followed by an analysis of each item in order to establish a framework of categories representing seven sequential steps of ability from 'not able at all' (score 1) to 'fully able' (score 7). The informants participated not only in the design and development process, but also in the reviews, editing and final approvals. When completed, the GAMMA manual for training, testing and credentialing of prospective users was concluded.
Results
The informants' collective concern was that the Lawton Scale was not an observational scale but a questionnaire that would introduce bias from discerning patients dreading change. However, they were satisfied that the structure of the Lawton scale could be converted into a routine nursing scale. With the Lawton Scale's potential to be developed into an ordinal nursing scale, the participants proceeded with the reconstruction of the Lawton Scale in order to perform an empirical assessment of their patients' independent living abilities. This reconfiguration of the Lawton scale was facilitated by means of probing questions. The advantages of the unstructured interviews were that participants' non- verbal behaviour and mannerisms could also be observed and answers could be clarified if misunderstood.
From the onset, there was consensus that the GAMMA must satisfy the following four objectives:
• The GAMMA must be useful at the nurse-patient interface when independent living abilities are a concern. The GAMMA scores must facilitate a uniform language in IADL restorative nursing.
• The GAMMA instrument must improve the quality of IADL restorative nursing services.
• The GAMMA must fit into the nursing process and care plans for persons living independently.
Finally, the first study resulted in a GAMMA scale consisting of eight items as illustrated in Figure 1 and an organised structure of the categories of the item 'Eating' as illustrated in Figure 2. Because of space constraints, the remaining items cannot be published.
Meal preparation
The definition of meal preparation is the ability on the part of the subject to prepare a nutritious meal. This includes: (1) planning (setting up a nutritional menu and shopping list); (2) setting up (e.g. using microwave/kettle, etc.); (3) preparing (e.g. peeling vegetables, making a sandwich, etc.); (4) cooking (e.g. boiling, frying, grilling, baking); and (5) dishing up (e.g. laying out eating utensils, dishing food onto plates or into storage containers, etc.).
Second phase: Establishing nursing utility
Research design
To establish the GAMMA's nursing utility, a qualitative exploratory descriptive design was followed. Focus group interviews were used to collect narrative data as nurses described their experience of implementing the GAMMA over a period of five months.
Population and sampling
To prevent bias when testing nursing utility, a new nursing population, unfamiliar with the GAMMA, was required to provide the information to analyse its nursing utility. Five registered nurses working in three retirement villages for a minimum period of three years were selected purposively because of their skill and good intuitive understanding of their client's ability to live an independent life. During the course of their work, they have observed their patients performing their daily IADLS without applying a scale or any other type of nursing measure. None of these nurses were involved or had any previous knowledge of the GAMMA or its development. Once their voluntary participation was confirmed, they were issued with the GAMMA manual, then trained and tested until they were proficient in the application of the GAMMA. No further exclusion criteria were applied.
Data collection
The RNs were originally asked to do a cross-sectional score of all the residents in their retirement village as additional information during their nursing assessment. However, once they experienced their ability to place an empirical value on a previously nebulous quality they collected scores longitudinally on their more vulnerable patients in assisted living units. The patients were observed according to the training manual and the nurses arrived at a specific score. The scores were recorded empirically in hard copy in the nursing records. The nurses could also plot the scores on the radar graph (Figure 1) in order to view the patient's ability graphically. A software database was provided for use in the importing of the GAMMA scores and to generate radar graphs of patient abilities, which could be printed as hard copies.
A focus group session was held with five nursing participants to explore the usefulness of the GAMMA in the nursing care plan of retirement villages. The participants were given the opportunity to express themselves in as much detail as possible. The exploratory nature of the research helped the researcher to gain a deeper understanding if, how and where the GAMMA changed their work experience. The discussion followed a semi-structured approach, whereby the four objectives for the development of the GAMMA (detailed under 'Data collection') were used to verify and simultaneously collect the richness of the descriptive information. Mannerisms and non-verbal behaviours were observed and recorded and statements or comments could be clarified if misunderstood. The interview was recorded and transcribed.
Data analysis
In the first phase, the GAMMA was developed with informants experienced in the observation of patients with impaired IADLs. As a result, the GAMMA can be assumed to have a high degree of nursing utility (Hsieh & Shannon 2005). Therefore, a deductive approach to content analysis was followed by creating a coded framework for analysis using the same four broad objectives used in the development, namely:
• Determine usefulness at the nurse or patient interface (code A).
• Facilitate a uniform language (code B).
• Improve the quality of nursing services (code C).
• Fit the nursing process and care plans (code D).
As a result, the four objectives were posed as four broad questions to the participants in order to retest the assumption that the GAMMA does indeed have good nursing utility. These four questions were thus anchored as the four categories for deductive content analysis (Hsieh & Shannon 2005).
Ethical considerations
This study was approved by the Human Research Ethics Committee (Medical) of the University of the Witwatersrand and an ethical clearance certificate (M 10524) was obtained in May 2010. Written approval from managers of the clinical facilities was also obtained. The purpose of the study was explained to the participants before data were collected. The participants gave written informed consent to be involved in this study on a voluntary basis. Participants could exercise their right to withdraw from the study at any time without penalty or prejudice. The researcher also ensured anonymity and privacy and the protection of participants against discomfort or harm, be it physical, emotional, spiritual, economic, social or legal.
Trustworthiness
The four criteria of trustworthiness, namely credibility, dependability, confirmability and transferability, were adhered to. Credibility was achieved by prolonged engagement with the participating nurses, allowing enough time during the interview to verbalise their perceptions regarding the development and utility values of the GAMMA. Sections of this study were also examined by internal and external examiners as part of a PhD thesis awarded by the University of Witwatersrand.
Dependability was achieved by means of a detailed description of research methodology, peer review and triangulation of sources, namely empirical data and literature control, as well as through the use of a coding process during data analysis.
Confirmability was achieved through the use of a detailed description of the research process, as well as during data collection through unstructured individual interviews where audio recordings were used and detailed field notes taken.
Transferability was achieved through the purposeful selection of the sample, as well as a dense description of the research methodology and results of the study, so that researchers who are interested in conducting similar research could be thoroughly informed.
Results
In an attempt to convey the richness of the data as expressed in the language used by the participants in the focus group, any direct quotations used must be interpreted as coming from a spokesperson in the group when expressing an experience or opinion. Some responses are paraphrased, rather than providing direct quotes. The codes (A1, B2, etc.) were used to classify the relevant response under the coded framework when doing the data analyses.
The nurses agreed that the GAMMA empirical scores and radar graphs of patient functioning 'really give you a picture of the residents' ability' (A1) to continue living independently. Importantly, the GAMMA 'helps to evaluate the person with a holistic approach as it shows how the person functions as a whole being' (B1). As a result, it also gives the nurses a new and 'more comprehensive awareness of the needs of the residents' (A2, B2, C1, D1) which would enable them to continue living independently. The ability to record this status empirically and to monitor functional ability empirically over time in a resident facility is of particular significance.
With the GAMMA scores now available and illustrative of what the patients are capable of and what they are not, the nurses have become aware of their own shortcomings in rendering appropriate supportive services in order to address patient needs. Nurses now realise they need to 'totally move away from the old way of nursing and caring' (A3, C2) by first evaluating the patient's capabilities and then find new techniques and care plans with regard to 'trying to help the person to continue in a process of being able to help himself for as long as possible' (A4, C3). Nurses have also discovered that by continuing with the traditional methods of nursing care, they were 'giving help without specifically doing something to slow the process of decline' (A5, C4). It has become clear that they should move away from the ever-increasing nursing support to rather focus on early intervention with restorative methods and techniques in order to 'keep them [the patients] independent for as long as possible' (A6, C5, D2). Evidently, nurses in geriatric nursing have become aware that their main focus can no longer only be 'structured around the medical side, maintaining hygiene and manage medication' (A7, B3, C6, D3). This will have to include techniques 'to secure independent living for as long as possible' (A7, B3, C6, D3).
The GAMMA seems to be particularly useful in its ability for the early identification of preventative problem areas that can be resolved with pro-active restorative nursing, allowing residents to maintain their independence longer. For this reason it is a valuable tool for the cottage nurse as it 'makes her look at [be aware of] the various segments of what is going on in the independent and assisted living scenarios' (A8, D4). Previously, the 'items addressed by the GAMMA were overlooked, taken for granted, or nurses were not even aware of its importance to promote independent living' (A9, B4, C7). Following on this evidence, the participants concurred that the GAMMA nursing scale is useful and contributes significantly to the nursing care plan and process.
The caring professional nurse's motto is 'I want to help you', but then they wrongly identify nursing tasks to make the person dependent on the nurse. The 'GAMMA has changed this mind-set' (A10, C8, D5). With the comprehensive view rendered by the GAMMA, the nurse is now compelled to make a paradigm shift when considering what nursing techniques the patient requires in order to maintain their independence. For this reason, 'the GAMMA should form an integral part of the nursing process' (D6).
The participants, however, warned that by nature nurses are very task oriented and the difficulty is going to be to turn the staff away from this, toward a restorative approach in maintaining the patient's independence. However, with proper training, support and supervision, nurses envisage that the implementation of the GAMMA will benefit everyone. Currently, every nursing day is inundated with nursing tasks and, as the residents become older and frailer, these tasks increase. The value of the GAMMA nursing scale lies in its ability to diagnose the primary causes of oncoming frailty much earlier and to point out the area where early restorative support is needed in order to maintain independence for as long as possible (A11, C9, D7). Training of nursing auxiliaries should be focused not only on how to use the scale but, more importantly, on 'looking at what the scale is pointing out to you and trying to better that [weaknesses] rather than listing it as a new nursing task' (A12, C10, D8). To entrench this 'new way of thinking' might be a challenge, but if successful, it would reduce the nursing burden of perpetual task rendering (A13, C11, D9). The consensus was that the GAMMA will facilitate this process and 'at the end, it is going to be easier on all the staff from not being task orientated [sic]' (A14, B5, C12, D10).
The participants were determined that, if implemented correctly, the GAMMA will facilitate major improvements in the quality of nursing of older persons (C13). If nurses merely observe and record the GAMMA indicators and do not act upon them appropriately, the quality of nursing care will not be enhanced (C14). Implementing the GAMMA requires a comprehensive care team which includes the non-nursing staff members such as the observant caregiver, gardener, cleaner, reception staff, administration person and, most importantly, the manager. The care team also has to include the patient and/or resident and their family members. 'The simplicity of the GAMMA includes everyone' (B6). Everyone must be aware, observant and report to the nurses when they observe any changes in patients (B7). However, it is the nurses' responsibility to score, record and respond both appropriately and timeously.
Interesting and unforeseen evidence was provided on the improvement of communication and relationships between the nursing professionals and the village managers and trustees. Nurses have found the GAMMA scores and radar graphs to be a useful tool and language in communicating meaningfully with the managers and village trustees about the aging residents' abilities and needs (B8). The nurses reported a sudden clarity and interest shown by the managers and trustees (B9). This new simplistic intelligibility has motivated 'managers [to] request that all new prospective residents are screened using the GAMMA nursing scale and radar profile to establish (and communicate) the level of care to be provided' (B10). The nurses also reported significant buy-in amongst 'managers [with regard to] use [of] the GAMMA as the point of departure at meetings with the nursing staff' (B10). Furthermore, the managers also 'request the GAMMA scores and radar graphs as an information briefing before entering into family meetings on resident issues' (B11). The GAMMA scores also seem to help the 'manager to have a better understanding of the nursing complexities' (B12), thereby initiating a more reassuring relationship when nurses have to implement new and creative restorative techniques in order to facilitate independence.
In some retirement villages, the auxiliary nurses had already been given an informal GAMMA introduction. 'High levels of acceptance and job satisfaction amongst the auxiliary nurses' were reported (A15, B13, D11). With their new intelligence, the auxiliary nurses communicate continuously and test their scores with the other nursing staff, report when they observed increased scores as a method of seeking acknowledgement and seemed eager and ready to implement the GAMMA officially. 'They are like a sponge ready to draw up the knowledge' (A16, B14, C15, D12).
In the last question for suggestions on improving the GAMMA, a concern was raised that the GAMMA item that scores self-medication creates a problem. As the Medicines and Related Substances Control Act 101 (South Africa 1965) on medication stands now, the GAMMA score 4 on self-medication cannot be utilised as Medicines and Related Substances Control Act 101 forces nurses to fill the daily boxes, thus arriving at a score of 3. This irregularity in nursing logic might impact on the validity of the GAMMA. In the final analysis, a suggestion was put forward to consider collapsing the two items pertaining to transport, for example, home-care accessibility and commuting, into a single item. The nurses also remarked that the emotional stability item is not an easy item to observe and might require further work.
In concluding the interview, a nursing professional in the position of retirement village manager provided the following conclusion:
'[it seems that the GAMMA] brings the quality [of nursing] care to its rightful position. Quality care can now be processed, managed and maintained in a very scientific way. It is important as it forms an integral part of the nursing process. You got quality care that you can measure and that is very important. The results you get with the GAMMA scores allow you to maintain and enhance quality care ... and you can calculate it [provide empirical proof].' (A17, B15, C16, D13)
Discussion
Prior to the GAMMA nursing scale, nurses working with elderly, frail and disabled persons were not able to establish empirically whether their patients benefited from the care they receive. This also puts nurses at a further disadvantage as they cannot manage the nursing process without measurements. Without a measure to provide empirical evidence of a patient's functional gains, the emerging science of restorative nursing (Resnick 2004) may lack scientific merit. These studies are the first of, hopefully, many research papers that will pre-empt the development of a new branch of nursing science: restorative nursing science in South Africa.
Without any training in restorative nursing techniques, nurses working with frail and disabled patients have discovered by themselves when implementing the GAMMA that it is not their primary task to do everything for the patient, but to score and assess the patients' functional ability and to find ways and means to improve the previous score. This was explained by a respondent in the second study that nurses became aware that 'looking at what the scale is pointing out to you and trying to better that [weakness] rather than listing it as a new nursing task' (C1). This finding indicates that the GAMMA has the potential to transform nursing from an input-driven science to a patient outcomes-driven science. To achieve this, nurses have recognised that they must adopt the basic principles of restorative nursing (Resnick et al. 2009). In practice, this new awareness has many beneficial implications for the nurses. It has challenged nurses to substitute their monotonous and laborious task-directed input approach with personal challenges and achievements that are evident in their patient outcomes. The results further indicated that the ultimate beneficiaries are the patients who regain their independence. This has improved the quality of the nursing process significantly.
More interesting was the observation that the GAMMA facilitated a new universal language at all possible levels: (1) the retirement facility management requires GAMMA scores on patients at their meetings, (2) the auxiliary nurses find it useful to apply in their daily interactions and (3) the gardeners, drivers, cleaners and administration staff all become aware of the person's functional status and report back to the nursing staff if they observe a change. The GAMMA created a standardised format for a comprehensive care team to work together, focusing on the same goal, namely, improving patient functionality. This is a patient evidence-based outcomes approach.
Limitations of the study
Had time and cost not been constraints in this study, the sample should also have included other case-mixes such as persons living with intellectual disabilities, congenital disabilities, post-trauma disabilities or chronic or terminal disease that render them progressively disabled.
The RNs reported that high levels of acceptance were found amongst the auxiliary nurses in the use of the GAMMA. In retrospect, it is a key limitation of this study that auxiliary nurses were not included in the second phase of this study.
Recommendations
Future education and training programmes that prepare practitioners for care of the aged and for persons living with physical and intellectual disability should include training in the application of the GAMMA nursing scale. It should also include restorative care-plan methods and techniques to help patients advance on their GAMMA scores. Furthermore, professional nurses must implement the restorative care mindset into the nursing process and discover ways to manage it effectively.
The change from traditional curative practice to restorative practice is a necessary mindshift that many nurses may find difficult. Changing the nursing focus from implementing nursing tasks to actively improving patient independence will require on-going motivation and reassurance of RNs and other categories of caregivers. This study showed that the GAMMA could an important facilitator for the process.
A recommendation for further research is to follow up this study with an investigation to establish whether the GAMMA scale can also function as an interval measure, meaning that its construct validity must be subjected to Rasch analyses. However, the follow-up Rasch analysis can only be completed when enough GAMMA scores have been collected. The Rasch results will guide the researcher with regard to verifying the potential structural weaknesses in the scale that must be rectified before it satisfies to the characteristics of an interval measure.
Finally, the recommendations from the participants on improvements of the GAMMA must be addressed.
Conclusion
Strong implicit and explicit evidence supported the GAMMA's nursing utility with regard to facilitation of a restorative nursing process. It has made the nurses aware of the value of having the IADLs embedded into the restorative nursing process. This was manifested in the ease with which the extended care team are able to recognise, observe and express the GAMMA scores in their daily routine and, implicitly, with the apparent new awareness that improvement in GAMMA scores has a direct correlation with improvement in the patient's independence and resultant wellbeing.
The GAMMA was developed by South African nurses for South African nurses in order to render better restorative nursing care for patients requiring IADL functional gain. The nursing participants in this study were very receptive with regard to developing and applying the GAMMA. The nurses reported the GAMMA to be a useful nursing measure that would improve the quality and effectiveness of nursing care for patients with restricted independent living abilities.
Acknowledgements
The authors would like to acknowledge the nurses that participated voluntarily in the study and also their colleagues from the School of Therapeutic Sciences at the University of Witwatersrand for their support as peer reviewers in the study, specifically Dr Marietha Nel for her scientific and language editing.
Competing interests
The South African Database for Functional Measures (Pty) Ltd provided financial support for this study. Although the SADFM gave written permission to publish this article and although the copyright of this article vests with the publishers, the patent rights of the GAMMA vest with the SADFM (RSA patent registration number 2008/09086).
Authors' contributions
This article was based on the primary research done by H.J.L. (South African Database for Functional Medicine) under the supervision of J.C.B. (University of the Witwatersrand) and
D.C. (University of the Witwatersrand) for the PhD thesis titled 'The validation of nursing measures for patients with unpredictable outcomes'. The draft was formulated by H.J.L. and J.C.B., with D.C. contributing to the finalisation of the article.
References
Barbara, A. & Whiteford, G., 2005, 'Clinical utility of the Handicap Assessment and Resource Tool: An investigation of its use with the aged people in hospital', Australian Occupational Therapy Journal 52(1), 17-25. http://dx.doi.org/10.1111/j.1440-1630.2005.00476.x [ Links ]
Bandeen-Roche, K., Xue, Q.L., Ferrucci, L., Walston, J., Guralnik, J.M., Chaves, P. et al., 2006, 'Phenotype of frailty: characterization in the women's health and aging studies', Journal of Gerontology: Series A, Biological Sciences and Medical Sciences 61(3), 262-266. http://dx.doi.org/10.1093/gerona/6L3.262 [ Links ]
Bond, T.G. & Fox, C.M., 2007, Applying the Rasch Model: fundamental measures in the human sciences, 2nd edn., Lawrence Erlbaum Associates, Mahwah, NJ. [ Links ]
Foxcroft, C., Patterson, H., Le Roux, N. & Herbst, D., 2004, Psychological assessment in South Africa: a needs analysis: the test use patterns and needs of psychological assessment practitioners: final report. July, Human Sciences Research Council, viewed 28 January 2014, from http://www.hsrc.ac.za/en/research-outputs/view/1642 [ Links ]
Hsieh, H.F. & Shannon, S.E., 2005, 'Three approaches to qualitative content analysis', Qualitative Health Research 15(9), 1277-1288. http://dx.doi.org/10.1177/1049732305276687 [ Links ]
Lawton, M.P. & Brody, E.M., 1969, 'Assessment of older people: self-maintaining and instrumental activities of daily living', Gerontologist 9(3 Part 1), 179-186. http://dx.doi.org/10.1093/geront/9.3_Part_1.179 [ Links ]
Lobelo, M.I., 2004, 'Experiences of relapsed psychiatric patients in Mafikeng in the North-West Province', MCur Thesis, Dept. of Nursing Sciences, Rand Afrikaans University. [ Links ]
Loubser, HJ., 2012, 'The validation of nursing measures for patients with unpredictable outcomes', Doctoral Thesis, Dept. of Nursing Sciences, Witwatersrand University. [ Links ]
Lynch, G.S., 2004, 'Tackling Australia's future health problems:Developing strategies to combat sarcopenia - age-related muscle wasting and weakness', Internal Medicine Journal 34(5), 294-296. http://dx.doi.org/10.1111/j.1444-0903.2004.00568.x [ Links ]
Mantle, J. & Funke-Furber, J., 2003, In dialogue with Verah Mclver - The forgotten revolution: the Priority Method: A restorative care model for older persons, Trafford, Victoria. [ Links ]
Markle-Reid, M. & Browne, G., 2003, 'Conceptualizations of frailty in relation to older adults', Journal of Advanced Nursing 44(1), 58-68. http://dx.doi.org/10.1046/j.13652648.2003.02767.x [ Links ]
Pel-Littel R.E., Schuurmans, M.J., Emmelot-Vonk, M.H. & Verhaar, H.J., 2009, 'Frailty: defining and measuring of a concept', The Journal of Nutrition, Health & Aging 13(4), 390-394. http://dx.doi.org/10.1007/s12603-009-0051-8 [ Links ]
Resnick, B., 2004, Restorative care nursing for older adults: A guide for all care settings, Springer Publishing Company, New York. [ Links ]
Resnick, B., Cayo, J., Galik, E. & Pretzer-Aboff, I., 2009, 'Implementation of the 6-week educational component in the Res-Care intervention: Process and outcomes', Journal of Continuous Education in Nursing 40(8), 353-350. http://dx.doi.org/10.3928/00220124-20090723-04 [ Links ]
South Africa, 1965, Medicines and Related Substances Control Act, 101 of 1965, Government Printers, Pretoria. [ Links ]
Strawbridge, W.J., Shema, S.J., Balfour, J.L., Higby, H.R. & Kaplan, G.A., 1998,
'Antecedents of frailty over three decades in an older cohort', Journal of Gerontology. Series B, Psychological Sciences and Social Sciences 53(1), S9-S16. http://dx.doi.org/10.1093/geronb/53B.LS9
Stevens, S.S., 1946, 'On the theory of scales and measurements', Science 103(2684), 677-680. http://dx.doi.org/10.1126/science.103.2684.677 [ Links ]
Toomey, M., Nicholson, D. & Carswell, A., 1995, 'The clinical utility of the Canadian Occupational Performance Measure', Canadian Journal of Occupational Therapy 62(5), 242-249. http://dx.doi.org/10.1177/000841749506200503 [ Links ]
Van Helden, S., Van Geel, A.C., Geusens, P.P., Kessels, A., Niewenhuijzen-Kruseman, A.C. & Brink, P.R., 2008, 'Bone and fall-related fracture risks in woman and men with a recent clinical fracture', Journal of Bone and Joint Surgery. American Volume 90(2), 241-248. http://dx.doi.org/10.2106/JBJS.G.00150 [ Links ]
 Correspondence:
Correspondence:
Hendrik Loubser
PO Box 2356
Houghton 2041, South Africa
Email: hennie@sadfm.co.za
Received: 26 Apr. 2013
Accepted: 28 Oct. 2013
Published: 03 Mar. 2014














