Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
South African Journal of Child Health
On-line version ISSN 1999-7671
Print version ISSN 1994-3032
S. Afr. j. child health vol.14 n.1 Pretoria Apr. 2020
http://dx.doi.org/10.7196.SAJCH.v14.i1.1650
RESEARCH
Patterns of healthcare utilisation and barriers affecting access to child healthcare services in low-income urban South African settings
S A AdediniI, IV; M SelloII, III; D ThaeleI, III; S A MadhiI
IPhD; Medical Research Council: Respiratory and Meningeal Pathogens Research Unit, University of the Witwatersrand, Johannesburg, South Africa
IIMA; Medical Research Council: Respiratory and Meningeal Pathogens Research Unit, University of the Witwatersrand, Johannesburg, South Africa
IIIMA; School of Clinical Medicine, University of the Witwatersrand, Johannesburg, South Africa
IVPhD; Programme in Demography and Population Studies, Schools of Public Health and Social Sciences, University of the Witwatersrand, Johannesburg, South Africa
ABSTRACT
BACKGROUND. Improving access to quality healthcare can contribute to reducing childhood mortality. Therefore, understanding the patterns of healthcare utilisation for common childhood conditions as well as barriers to healthcare use is important in planning appropriate public health programmes and interventions.
OBJECTIVE. The objective of the present study was to examine patterns of child healthcare uptake and barriers that affect access to healthcare in two South African (SA) low-income urban settings.
METHODS. A healthcare utilisation survey was conducted between April and September 2015, using a cross-sectional study design. Data were analysed using descriptive and inferential statistics. Information was collected on 531 children and their caregivers from 503 randomly selected households.
RESULTS. Our findings revealed that 81.9% of respondents preferred clinics as their first choice, and 84.2% preferred hospitals as their second point of call. About 5% of caregivers preferred faith-based/traditional healers as their second point of call. Barriers to accessing healthcare were reported for more than half of the sampled children (52.0%), such as long queues at the health facility (HF), poor attitudes of healthcare workers, lack of medicine and the distance to the HF, which constitute major barriers. These findings were echoed in multivariable analysis. For instance, distance to the HF (odds ratio (OR) 2.01; confidence interval (CI) 1.04 - 3.89, p<0.05) was a strong predictor for barriers to accessing child healthcare services.
CONCLUSION. Considering the benefits of unrestricted access to quality care for positive child health outcomes, the present study underscores the need for improved access to adequate healthcare in the selected locations in SA.
Access to quality healthcare holds great potential for the survival of under-5 children and their mothers;[1-4] nevertheless, healthcare access remains limited in sub-Saharan Africa (SSA),[5,6] thus contributing more than half of the global figure of 5.9 million deaths of under-5 children.[7] Two-thirds of these deaths could be prevented by adequate access to proven healthcare interventions.[8]
Although the South African (SA) under-5 mortality rate (42 per 1 000 live births) is much lower than SSA's average (78 per 1 000 live births),[9,10] the national estimate possibly masks sub-national variations. Provincial estimates indicate variations in under-5 mortality rates (per 1 000 live births) from 43 in Gauteng to 78 in Eastern Cape provinces,[11] which could be due to variable access to healthcare. Eighty percent of SA's population depends on the public health sector, and only 16% have private medical insurance,[12] which places huge strain on public health facilities; the number of patients per clinic is currently estimated at 13 718, which exceeds the World Health Organization (WHO)'s recommendation of 10 000 per clinic.[12 Moreover, there is a shortage of medical doctors, with the ratio of physicians per 1 000 population unchanged between 2004 (0.77) and 2011 (0.76).[13]
One of the targets of the Sustainable Development Goals (SDGs) is to provide affordable and quality universal healthcare coverage.[14] Although SA's national health policy aligns with the SDG targets and emphasises provision of healthcare for all, wide sub-national
variations exist. Ninety-six percent of live births in the 5 years preceding the 2016 South Africa Demographic and Health Survey (2016 SADHS) were assisted by a skilled provider; nevertheless, ~40% of under-5 mortality in SA still occurs during the first month of life,[9] which suggests possible systemic barriers to adequate uptake of healthcare services during the antenatal, delivery and postnatal periods. While evidence on healthcare use is available at national and provincial levels through routine specialised surveys such as the General Household Surveys (GHS) and Demographic and Health Surveys (DHS), there is a paucity of data on patterns of healthcare utilisation (HCU) at district or sub-district levels, including in low-income urban settings such as Soweto and Orange Farm (townships in south-west Johannesburg). The present study examined patterns of child healthcare uptake and barriers affecting access to healthcare utilisation in 2 SA low-income urban settings.
Public healthcare in Soweto and Orange Farm
Soweto has a substantial number of healthcare facilities at the primary and secondary/tertiary levels. These include 23 primary healthcare (PHC) clinics and 2 public hospitals - Chris Hani Baragwanath Academic Hospital (CHBAH) and Jabulani Hospital. While PHCs offer services during the day only, the 2 hospitals offer 24-hour services. The PHCs are well sited across Soweto to ensure reasonable proximity of 2 km or less to most households within the community. CHBAH is a 2 850-bed hospital, and is the third-largest in the world.[15] It includes 250 general paediatric beds and 200 neonatal beds. Jabulani Hospital was opened in June 2014 and has 60 paediatric beds. Although Orange Farm has more than 10 PHCs, CHBAH remains an important source of care and referral for most residents in this community. Private healthcare is generally expensive in SA, and less than 10% of Soweto and Orange Farm residents have private medical insurance.[12] It is estimated that more than 90% of all hospitalisations of residents of these communities take place at CHBAH. All healthcare for pregnant women and children <6 years old, including diagnostic tests and treatments at the hospital and PHCs, are free. Although there is a wide network of private general practitioners (GPs) and traditional healers in Soweto and Orange Farm, CHBAH remains the primary source of care as well as referral for serious illnesses from these GPs.
Study design and participants
The present paper used data collected for a larger study on HCU among under-5 children in Soweto and Orange Farm. The study undertook a community-based cross-sectional survey with the aim of assessing patterns of healthcare-seeking behaviour among primary caregivers of under-5 children, including the level of hospitalisation among the children. The HCU survey assessed the factors influencing non-utilisation ofhealthcare facilities for children in the study settings. A cross-sectional survey was conducted among a representative sample of 503 randomly selected households in Soweto and Orange Farm. Soweto is a low-income, urban black community of about 1.3 m people, including 125 000 children under 5 years old. Orange Farm township was established in 1988 to accommodate the ever-increasing population of the Johannesburg Metropolis. Orange Farm has a total of 8 sub-places and a population of 76 767.[12]
Potential participants were selected through a two-stage sampling selection process. In the first stage, selected communities were stratified according to neighbourhoods with homogenous dwelling units (DUs). Each neighbourhood was further sub-divided into clusters, and clusters were randomly selected in the sampled neighbourhoods, with the number of selected clusters proportional to the size of each neighbourhood. In the second stage, the boundaries of each residential neighbourhood were delineated on aerial maps available from Google Earth. Geographic co-ordinates were randomly selected within each neighbourhood, where the number of co-ordinates selected was proportional to the population size of that neighbourhood. The DUs closest to the randomly selected geographic co-ordinates were selected. Thereafter, a representative sample of 503 households was chosen from the selected DUs. Eligible respondents, i.e. mothers or primary caregivers (who gave consent to participate in the survey) with at least 1 child aged 0 - 59 months in the sampled households, were interviewed, using a semi-structured questionnaire preloaded into digital devices using open data kits (ODKs). The questionnaires were designed to collect information on household demographic and socioeconomic characteristics and child healthcare utilisation over the previous 12 months. Most of the questions were close-ended with pre-coded responses from which study participants could choose and, in most cases, there was the option of 'Other, specify', if the respondent's answer was different from all the pre-coded answers provided in the questionnaire. Further, questions that required numerical responses were structured in the questionnaire in a way that allowed respondents to freely provide numerical answers. For instance, respondents were allowed to freely report the estimated distance to the nearest health facility in kms.
Variables measurement
The outcome variable analysed in this study is 'barriers to healthcare use', defined as having any form of barrier affecting access to utilisation of modern medical services for children aged 0 - 59 months; and coded as '1' if any barrier was reported, or '0' if no barrier was reported.
The selected explanatory variables for the study included the demographic and socio-economic variables. The operational definitions for these selected characteristics are presented in Table 1.

Statistical analysis
Analysis included descriptive and inferential statistics, using univariate, bivariate and multivariable analytical approaches. The univariate analysis was conducted to describe the data with the use of frequencies and percentages. Bivariate analysis was done to explore statistically significant relationship between the outcome variable and each of the explanatory variables, using the Pearson χ2test. The multivariable analysis simultaneously examined the relationship between the outcome variable and all the explanatory variables. We employed binary logistic regression in the multivariable analysis, given the dichotomous nature of the outcome measure. We fitted two models to identify the predictors of child healthcare utilisation in the study locations. Model 1 presents findings from statistical analysis which examined the relationship between HCU and each of the selected explanatory variables. Model 2 is the full model which simultaneously examined association between HCU and all the selected explanatory variables. The unit of analysis was children <5 years old. We present results in the form of odds ratios (ORs) and 95% confidence intervals (CIs). All analysis was done using STATA (StataCorp., USA) version 13.0.
Ethical consideration
The study was approved by the Health Research Ethics Committee of the University of the Witwatersrand, Johannesburg, SA (ref. no. 170216).
Results
Descriptive statistics
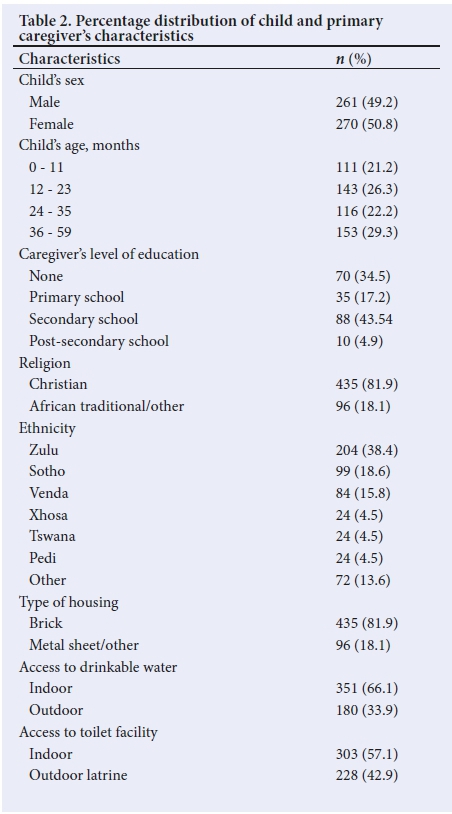
Household demographic information is reported in Table 2. Of the 531 children, both genders were of equal numbers, most were age 36 - 59 months, and further age-group stratification is detailed in Table 2. Regarding maternal/caregivers' characteristics, a majority had secondary education. Most respondents were of the Christian faith and of Zulu ethnic origin. Houses were generally made of brick and access to drinkable water and a toilet were mostly indoors.
Patterns of healthcare utilisation and barriers affecting access to child healthcare
The results in Table 3 indicate that CHBAH was reported as place of delivery for almost half of the sampled children. Also, caregivers were asked about their first and second choices of health facility if their children became ill. An overwhelming majority reported a clinic as their first choice while 84.2% indicated hospital as their second point of call. About 5% of caregivers preferred faith-based or traditional healers as their second point of call. The results in Table 3 confirm proximity to health facility as an important factor in the choice of health facility for child healthcare, as about 90% of respondents indicated proximity to health facility as the reason for their choice of facility for child healthcare.

Findings on barriers to child healthcare showed that slightly more than half of the sampled respondents reported barriers to child healthcare services. When barriers to child healthcare were disaggregated by problem/type of barrier, the results indicated health system barriers such as long queues at health facilities as the main problem constituting a barrier to child healthcare utilisation in the study areas. Other health system barriers included poor attitudes of healthcare workers and lack of medicines in the health facility. Distance to health facility was also reported as a problem by about 60% of caregivers.
Results from bivariate analysis
Table 4 presents results from bivariate analysis which examined the relationship between barriers to child healthcare and selected characteristics. The results of cross-tabulations indicated a significant relationship between religion, ethnicity, type of housing material, distance to health facility and access to child healthcare services (p<0.05).
The analysis indicates that barriers to healthcare uptake were reported for almost half of all children. Barriers to child healthcare services were mostly reported for children <1 year old compared with those >1 year old. Educated caregivers were less likely to report barriers to child healthcare. Type of housing material was used as a proxy variable for household socioeconomic status, with the assumption that the very poor are likely to live in shacks and dwellings made of metal sheets. Results indicate that higher numbers of mothers/ caregivers living in shacks experienced barriers to child healthcare services than those living in brick dwellings. Distance to health facility was reported as a significant factor affecting access to child healthcare (p<0.001). The association of barriers to child healthcare with other characteristics is set out in Table 4.
Results from multivariable analysis
Table 5 presents the results from binary logistic regression analysis which examined the relationship between barriers to child healthcare services and selected variables. Results in Model 1 indicate a significant association between access to child healthcare and some characteristics, including religion, ethnicity, type of housing material and distance to health facility. For instance, respondents whose religion was African traditional had twice the probability of reporting barriers to child healthcare than their Christian counterparts (OR 2.05, 95% CI 1.30 - 3.23; p<0.05). Results in Model 1 also indicate a significant association between residence in shacks and barriers to child healthcare (OR 4.13, 95% CI 2.51 - 6.81; p<0.001). Distance to health facility was significantly associated with barriers to child healthcare services.
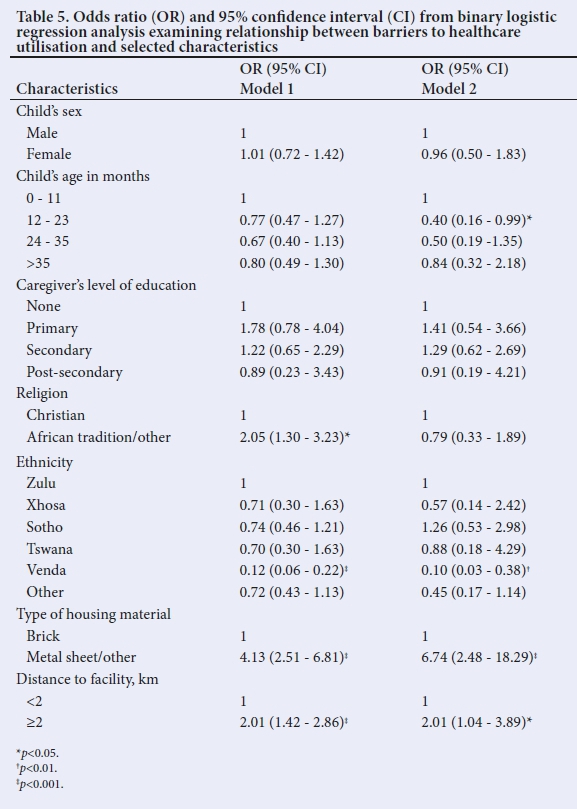
Results from Model 2 (Table 5) indicate lower odds ofreporting barriers to healthcare for children aged 12 - 23 months than those <1 year old (OR 0.40, 95% CI 0.16 - 0.99; p<0.05). Ethnicity remained significantly associated with access to child healthcare (p<0.001). The association of barriers to child healthcare with the proxy variable for socioeconomic status, and distance to health facilities, was echoed in Model 2. For instance, respondents living in shacks (OR 6.74, 95% CI 2.48 - 18.29; p<0.001) and those residents more than 2 km from the nearest health facility (OR 2.01, 95% CI 1.04 - 3.89; p<0.05) had significantly higher odds of reporting barriers to child healthcare services.
Discussion
This study was a sub-national analysis of patterns of healthcare utilisation and barriers to accessing child healthcare services. Growing inequalities exist in access to quality and affordable healthcare services in many SSA countries,[2-16] including SA. Given that adequate access to healthcare holds great potential for good child health outcomes,[1,2] understanding the barriers affecting access to child healthcare, particularly from caregivers' perspectives, is important when designing appropriate public health programmes.
Our findings indicate that although the sampled children in the selected locations were delivered in ~60 different hospitals/ clinics, almost half of these children were delivered in CHBAH alone. The literature suggests that women prefer giving birth at health facilities, and particularly in hospitals, because there are enough resources and trained health practitioners.[17]-Our findings also established that long queues and poor attitudes of healthcare workers were major health system barriers affecting access to child healthcare services in the study settings. It is well established that overstretching of healthcare resources is a major barrier to the delivery of safe and high-quality healthcare.'18-201 This issue therefore requires attention, particularly in the public health sectors.
Although our data showed that most respondents were resident within 2 km of the nearest hospital or clinic, it is unclear why most people would prefer to travel long distances to seek child healthcare. As previously established, plausible reasons for seeking care in distant locations, instead of near-by facilities, may include concerns about poor quality of care, lack of commitment of health workers to the needs of children and caregivers, quackery and problems about availability and affordability of satisfactory healthcare services.[16,21,22]
Most caregivers in the selected study locations preferred clinics as their first choice, with hospitals mainly the second point of call for child care. This finding is consistent with evidence from the nationally representative study (2017 General Household Survey (GHS)) which found that more than 70% of households made use of clinics, hospital or other public facilities as the first point of access if any household member needed medical attention.'231 Hospitals were perhaps the second choice because they offer 24-hour services and are better equipped to attend to emergencies and referrals. The present study also found that some caregivers consulted faith-based and traditional healers for child healthcare. This establishes a healthcare context of medical pluralism in SA, showing that alternative healthcare providers such as traditional birth attendants, traditional/faith healers, and patent medicine sellers have the patronage of women and other caregivers, as in other SSA countries.[21] Prior studies suggest that caregivers tend to patronise alternative healing practitioners when they observe that biomedicine and orthodox medical practices have failed to improve their children's health.[24-27]
Moreover, the present analysis established that more than half of respondents reported barriers to child healthcare in the selected locations. The reasons adduced included long queues at the facilities, poor attitudes of healthcare personnel and lack of medicine in the facilities. Results from our multivariable analysis established poverty and distance to health facility as significant predictors of barriers to child healthcare. Therefore the need to eliminate both demand- and supply-side barriers affecting access to quality and affordable healthcare services is particularly urgent in the selected locations in SA. Considering that a right to health is a constitutional provision in the country, addressing the identified barriers affecting access to child healthcare is an important public health investment and priority. Although evidence shows there are many ongoing activities within the public healthcare system in SA that aim to improve access to affordable care,[16,22,28] much still needs to be done to ensure universal healthcare coverage, particularly for children.
Study limitations
The study has some limitations. Firstly, it was a small-scale study and its findings may not be generalisable or representative of SA. Secondly, a number of relevant variables such as socioeconomic and poverty status that could influence access to healthcare, are not available in the datasets, and hence proxy variables were used to measure poverty status. Also, being a cross-sectional survey, a cause-effect relationship could not be established. Notwithstanding these limitations, the study has filled an important gap in the public health literature, particularly as regards evidence on access to child healthcare at the sub-district level and in low-income urban settings in SA.
Conclusion
Despite the fact that primary healthcare is free for children and pregnant women in SA, a significant proportion of caregivers face enormous barriers to quality child healthcare in the selected study locations. Considering the benefits of unrestricted access to adequate care for positive child health outcomes, this study suggests the need to address various barriers affecting access to quality healthcare in the selected locations and other similar settings in SA; this would serve as a part of important strategies to firmly place the country on the path towards the attainment of SDG targets on child health and survival.
Declaration. None.
Acknowledgements. The authors gratefully acknowledge the roles of the field and data management teams, as well as the study participants who consented and participated in the study. An earlier version of the paper was presented at the 8th African Population Conference held in Entebbe, Uganda, in 2019. The authors thank participants at the session for their comments.
Author contributions. SAM conceptualised the research idea and reviewed the paper for critical inputs. SAA reviewed the literature, analysed the data and drafted the manuscript. MS and DT were involved in the study design, data collection, review of literature, and data analysis. All authors reviewed and approved the final version of the paper.
Funding. The study was funded by the Bill & Melinda Gates Foundation. The funders had no role in the conduct of the study or the write-up of the results.
Conflicts of interest. None.
References
1. Rutherford ME, Mulholland K, Hill PC. How access to health care relates to under-five mortality in sub-Saharan Africa: Systematic review. Trop Med Int Health 2010;15(5):508-519. https://doi.org/10.1111/j.1365-3156.2010.02497.x [ Links ]
2. Adedini SA, Odimegwu C, Bamiwuye O, Fadeyibi O, De Wet N. Barriers to accessing health care in Nigeria: Implications for child survival. Glob Health Action 2014;7. https://doi.org/10.3402/gha.v7.23499 [ Links ]
3. Lungu EA, Biesma R, Chirwa M, Darker C. Healthcare seeking practices and barriers to accessing under-five child health services in urban slums in Malawi: A qualitative study. BMC Health Serv Res 2016;16(410). https://doi.org/10.1186/s12913-016-1678-x [ Links ]
4. Bayham M, Blevins M, Lopez M, et al. Predictors of health-care utilisation among children 6-59 months of age in Zambézia Province, Mozambique. Am J Trop Med Hyg 2017;96(2):493-500. https://doi.org/10.4269/ajtmh.16-0233 [ Links ]
5. Gage AJ. Barriers to the utilisation of maternal health care in rural Mali. Soc Sci Med 2007;65(8):1666-1682. https://doi.org/10.1016/j.socscimed.2007.06.001 [ Links ]
6. Ononokpono DN, Odimegwu CO, Imasiku EN, Adedini SA. Does it really matter where women live? A multilevel analysis of the determinants of postnatal care in Nigeria. Matern Child Health J 2014;18(4):950-959. https://doi.org/10.1007/s10995-013-1323-9 [ Links ]
7. Yaya S, Uthman OA, Okonofua F, Bishwajit G. Decomposing the rural-urban gap in the factors of under-five mortality in sub-Saharan Africa? Evidence from 35 countries. BMC Public Health 2019;19(1):616. https://doi.org/10.1186/s12889-019-6940-9 [ Links ]
8. O'Donnell O. Access to health care in developing countries: Breaking down demand side barriers. Cadernos de Saúde Pública 2007;23:2820-2834. [ Links ]
9. Statistics South Africa. South Africa Demographic and Health Survey 2016: Key Indicator Report. Pretoria: StatsSA, 2017. [ Links ]
10. United Nations Children's Fund, World Health Organization, World Bank, United Nations Population Division. Under-five mortality estimates by the UN Inter-agency Group for Child Mortality Estimation 2018. https://data.worldbank.org/indicator/SH.DTH.MORT (accessed 24 February 2018). [ Links ]
11. National Department of Health, Statistics South Africa, South African Medical Research Council, ICF International. South Africa Demographic and Health Survey 2016. Pretoria: NDoH, 2017. [ Links ]
12. Statistics South Africa. Census 2011 Statistical release - P0301.4/Statistics South Africa. Pretoria: StatsSA, 2011. [ Links ]
13. Mayosi BM, Benatar SR. Heath and health care in South Africa - 20 years after Mandela. N Engl J Med 2014;371(14):1344-1353. https://doi.org/10.1056/NEJMsr1405012 [ Links ]
14. World Health Organization. Good health and well-being 2018. https://www.who.int/sdg/targets/en/ [ Links ]
15. Zwi J. The changing trends in paediatric hospital admissions at Chris Hani Baragwanath Hospital 1992 - 1997. MMed (Paed ) research report. Johannesburg: University of Witwatersrand, 1998. [ Links ]
16. Meyer JC, Schellack N, Stokes J, et al. Ongoing initiatives to improve the quality and efficiency of medicine use within the public healthcare system in South Africa: A preliminary study. Front Pharm 2017;8:751. https://doi.org/10.3389/fphar.2017.00751 [ Links ]
17. Kanmiki EW, Bawah AA, Agorinya I, et al. Socio-economic and demographic determinants of under-five mortality in rural northern Ghana. BMC Int Health Hum Rights 2014;14(1):24. https://doi.org/10.1186/1472-698X-14-24 [ Links ]
18. Dyrbye LN, Shanafelt TD, Sinsky CA, et al. Burnout among health care professionals: A call to explore and address this underrecognized threat to safe, high-quality care. NAM Perspective. 2017. Discussion Paper. [ Links ]
19. Khamisa N, Peltzer K, Ilic D, Oldenburg B. Effect of personal and work stress on burnout, job satisfaction and general health of hospital nurses in South Africa. Health SA Gesondheid 2017;22:252-258. https://doi.org/10.4102/hsag.v22i0.1011 [ Links ]
20. Maslach C, Leiter MP. New insights into burnout and health care: Strategies for improving civility and alleviating burnout. Med Teach 2017;39(2):160-163. https://doi.org/10.1080/0142159X.2016.1248918 [ Links ]
21. Izugbara CO, Wekesah F. What does quality maternity care mean in a context of medical pluralism? Perspectives of women in Nigeria. Health Pol Plan 2017;33(1):1-8. https://doi.org/10.1093/heapol/czx131 [ Links ]
22. Harris B, Goudge J, Ataguba JE, et al. Inequities in access to health care in South Africa. J Pub Health Pol 2011;32(1):S102-S123. https://doi.org/10.1057/jphp.2011.35 [ Links ]
23. Statistics South Africa. General Household Survey 2017. Pretoria: StatsSA, 2018. [ Links ]
24. Goudge J, Gilson L, Russell S, Gumede T, Mills A. The household costs of health care in rural South Africa with free public primary care and hospital exemptions for the poor. Trop Med Int Health 2009;14(4):458-467. https://doi.org/10.1111/j.1365-3156.2009.02256.x [ Links ]
25. Goudge J, Gilson L, Russell S, Gumede T, Mills A. Affordability, availability and acceptability barriers to health care for the chronically ill: Longitudinal case studies from South Africa. BMC Health Serv Res 2009;9(1):75. https://doi.org/10.1186/1472-6963-9-75 [ Links ]
26. Opwora AS, Laving AM, Nyabola LO, Olenja JM. Who is to blame? Perspectives of caregivers on barriers to accessing healthcare for the under-fives in Butere District, Western Kenya. BMC Public Health 2011;11(1):272. https://doi.org/10.1186/1471-2458-11-272 [ Links ]
27. Bedford KJA, Sharkey AB. Local barriers and solutions to improve care-seeking for childhood pneumonia, diarrhoea and malaria in Kenya, Nigeria and Niger: A qualitative study. PloS ONE 2014;9(6):e100038. https://doi.org/10.1371/journal.pone.0100038 [ Links ]
28. Delobelle P. The health system in South Africa. Historical perspectives and current challenges. South Africa in focus: Economic, political and social issues. Hauppauge: Nova Science Publishers, 2013:159-196. [ Links ]
 Correspondence:
Correspondence:
S A Adedini
adedinis@rmpru.co.za
Accepted 3 July 2019.














