Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
South African Journal of Child Health
versão On-line ISSN 1999-7671
versão impressa ISSN 1994-3032
S. Afr. j. child health vol.12 no.3 Pretoria Jul./Set. 2018
http://dx.doi.org/10.7196/sajch.2018.v12i3.1455
ARTICLE
Double trouble: Addressing stunting and obesity via school nutrition
L GrahamI; T HochfeldI; L StuartII
IPhD; Centre for Social Development in Africa, Faculty of Humanities, University of Johannesburg, South Africa
IIMPhil; Centre for Social Development in Africa, Faculty of Humanities, University of Johannesburg, South Africa
ABSTRACT
BACKGROUND. South Africa (SA), as a middle-income country, faces the nutrition transition and associated double burden of undernutrition and obesity. School feeding programmes are one way of ensuring that malnutrition in children is addressed, but questions remain about whether they can address both undernutrition and obesity.
OBJECTIVES. To compare the obesity and stunting outcomes for children receiving different combinations of school feeding programmes in a rural district of SA.
METHODS. The evaluation involved a comparative design that compared the stunting and obesity levels of three groups of children. Group 1 received one lunch meal a day for a prolonged period, group 2 both lunch and breakfast, and group 3 had started receiving a daily lunch shortly before the commencement of the research.
RESULTS. Group 1 had stunting levels in line with the national average. Group 2 had lower stunting levels than those receiving only the lunch meal. Children from group 3 had lower stunting levels than groups 1 and 2. Rates of obesity and overweight were markedly different between the groups. Group 3 had very high rates of overweight and obesity - above the national average of 28%. In contrast, group 1 had far lower rates of overweight and obesity, and group 2 exhibited the lowest levels. There was a significant decrease in the percentage of learners classified as overweight in group 3 over the 6-month period, from 26.1% to 19.2%.
CONCLUSION. One lunch meal a day is associated with positive outcomes in relation to rates of stunting and obesity, and the lowest rates of obesity were measured when a breakfast meal was added. The addition of a breakfast meal to a lunch feeding programme shows promise, but this requires further investigation to understand whether causal linkages exist.
School nutrition programmes exist worldwide, and are considered an effective means of impacting positively on poor children's nutritional health, as well as improving school attendance and educational outcomes.[1,2] Many school nutrition programmes, particularly in low-income countries, are intended to address the outcomes of undernutrition, such as wasting and stunting.[3] Middle-income countries often face the 'nutrition transition, where rapid urbanisation and the Westernisation of diets exist alongside traditional diets and poverty.[4] This phenomenon results in what is known as the double burden of nutrition, where serious food insecurity, and consequent undernutrition, exists alongside increasing obesity and associated non-communicable diseases, often within the same subpopulation.[4-6] Despite this trend, there is limited research that assesses the effect of school nutrition programmes on addressing the consequences of both undernutrition and obesity within the same population. In this article, we address this gap and provide evidence of how a lunch programme and a combination lunch-and-breakfast programme address stunting and obesity levels within one rural community in South Africa (SA).
Akin to other middle-income countries, SA is faced with a nutrition transition,[4] with concomitant effects on both stunting and obesity levels. The double burden of undernutrition and obesity has implications for the national disease picture in SA and many other middle- to low-income countries.[7] Stunting, while still a problem, has improved, as 15% of children currently suffer the effects, down from 25% in 1994.[2] Childhood obesity, commonly believed to be a developed-world problem, has increased in developing countries[6] owing to low-quality diets high in fat, starch, sugar and salt, and low in nutritional benefits. In SA, as of the most recent figures (2014), 28% of children are considered to be overweight.[8] As shown in other parts of the world, this combination creates, on top of conditions of undernutrition such as kwashiorkor and rickets, a second layer of diseases that until quite recently were mainly confined to the developed world, with diabetes, hypertension and cardiovascular problems being the most common.[5] SA is already experiencing the costs of this double burden.[9]
School nutrition studies generally focus on evaluating the impact of school feeding on either undernutrition or obesity, depending on the context, but not the impact on these coexisting health problems. For instance, research has demonstrated good results in decreasing underweight and stunting through nutritional interventions in schools, in low-income contexts such as Bangladesh, Zambia and Ethiopia.[3] In addition, obesity has been positively affected by school nutrition programmes in higher-income contexts such as the USA and the UK, as well as in middle-income countries such as Mexico,[4] by facilitating the consumption of micronutrients and nutrient-dense foods. One important finding is that consistent breakfast consumption contributes to the reduction of body weight, especially for children and adolescents, and further contributes significantly to improved micronutrient status.[10] While these studies provide important insights into the effects of school nutrition programmes in particular contexts, no single study has considered how a school nutrition programme can protect against both obesity and the effects of undernutrition, such as stunting.
SA runs a large National School Nutrition Programme (NSNP) that provides a daily meal to 9 million children during school terms.[11] In addition, a privately funded nutrition programme provides a second daily meal, in the form of breakfast, to approximately 40 000 children in selected schools already receiving the NSNP. This arrangement allowed us to conduct a comparative assessment of the effects of the NSNP on its own, and in combination with the breakfast programme, on childhood stunting and obesity. In this article, we consider whether different combinations of school nutrition programmes can have effects on levels of stunting and overweight in a sample of rural SA primary-school children.
Methods
The school nutrition programmes
In SA, state schools are classified according to the socioeconomic status of the area they serve, from the poorest schools (category 1) to the wealthiest (category 5). Schools in categories 1 - 3 are classified as poor schools (albeit at different levels of poverty). All learners at these schools receive a daily lunch that follows a prescribed menu consisting of a starch, a protein (often soya based) and vegetables or a fruit, through the NSNP. This menu has been assessed as a balanced diet.[12] The privately funded breakfast programme targets the poorest schools (mainly category 1 schools), and delivers a daily breakfast consisting of a fortified cooked cereal.
Study design
The study, conducted in Lady Frere - a rural district of the Eastern Cape Province, SA - took the form of a comparative design. Three groups of children (aged 6 - 12 years) were compared, at a single point in time in the course of a school year (April 2015). The first group of children (group 1) attended primary schools that received the NSNP lunch only, from schools across the three categories. Group 2 consisted of children from primary schools that were receiving the breakfast programme in addition to the NSNP. These schools were predominantly category 1 schools. A true control group was not possible, since all children in schools within the first three categories receive the NSNP. However, some schools in the province had been recently reassessed to take into account their level of disadvantage, and subsequently reclassified from category 4 to category 3, qualifying them to receive the NSNP. Of these reassessed schools, two schools in a neighbouring district were fairly similar to the group 1 and 2 schools selected for the study, in terms of demographics and location, but were slightly better off socioeconomically (category 3 only). These two schools formed a third comparison group (group 3). They had only started receiving the NSNP 2 months prior to the data collection point. This allowed us to assess the relative benefits of having received the NSNP since starting school, receiving the NSNP and a breakfast since starting school, and receiving the NSNP only for a short period of time. In addition, for group 3 we were able to assess whether any intrapersonal changes occurred over a 6-month period, after children had begun receiving the lunch meal. Therefore, for group 3 schools only, we introduced a longitudinal element to the study.
Participants/sampling
The 158 schools in the Lady Frere district were grouped into those receiving the NSNP only (128 primary schools), and those receiving the additional breakfast (31 primary schools). A proportional (25%) sample of schools was randomly drawn from these groups. A total of 31 schools were randomly selected for group 1, and 8 for group 2. Two schools were purposively selected for group 3, as described above. Within each school, stratified sampling by grade and sex was used to determine which students would participate in the study.
Measures
The children's weight, stature and sitting height were measured. All anthropometric measurements were taken according to the International Standards for Anthropometric Assessments.[13] The learners wore light clothing without shoes, and were weighed using portable electronic scales. A stadiometer and anthropometric tape measure were used to measure weight and height, respectively.
The inter-rater reliability of the anthropometric measurements was enhanced by ensuring that two people were present to take and check measurements, each measuring every child with the other present. Standardised, calibrated equipment was used throughout the data collection. All the fieldworkers were accredited Level 1 International Society for the Advancement of Kinanthropometry (ISAK) anthropometrists.
Analysis
The data were analysed using the World Health Organization (WHO) Child Growth Standards.[14] Height-for-age and BMI [body mass index]-for-age z-scores were calculated using the WHO Stata macros developed to assess data against the Child Growth Standards. This process accounts for age and sex differentials in weight and height. It does so by calculating z-scores for each measure to assess a child's weight, height or BMI, adjusted for their age and sex, relative to a universal external reference point.[15] For undernutrition, we focused on height-for-age. Height-for-age z-scores that fall between two and three standard deviations below the universal median are classified as stunted, and those that fall more than three standard deviations below the median are classified as severely stunted. For obesity, we assessed the BMI-for-age. If a child's BMI-for-age z-score falls between one and two standard deviations above the universal median, they are classified as overweight, and as obese if their BMI-for-age z-score falls more than two standard deviations above the universal median.
Analysis of difference was conducted between groups. First, x2 tests were used to assess differences in the proportions of children from each group who fell into the overweight/obese and the stunted categories. Second, one-way analysis of variance (ANOVA) or Brown-Forsyth tests were used to assess differences in the mean z-scores for height-for-age and BMI-for-age. Finally, for group 3, we assessed whether there was any change in obesity/overweight levels over time, by conducting a paired f-test. Differences were determined to be significant at the p=0.005 level.
Ethics
Ethical approval for the study was granted by the University of Fort Hare's Research Ethics Committee (ref. no. GEN011), and permission granted by the national and provincial departments of education. Parents of selected children were provided with an informed consent form in their first language. Children were provided with an opportunity to assent. Only children who had assented to the study and whose parents had given consent were recruited. Measurements were taken by fieldworkers of the same sex as the participants. All data were anonymised to protect the confidentiality of participants.
Results
Overview of sample
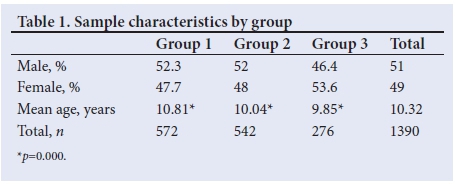
The sample composition is shown in Table 1. An analysis of age demonstrates that there are small but significant differences in the mean age for each group (p=0.000), with group 1 learners having a higher mean age than both groups 2 (p=0.000) and 3 (p=0.000). The age differences are accounted for by the standardised z-score analysis. No significant differences were noted in the proportion of boys and girls in each group (p=0.227).
Stunting
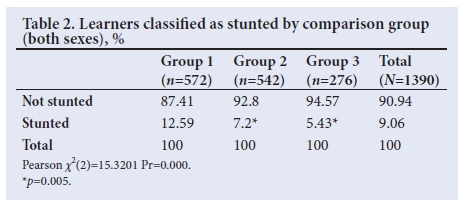
We observed statistically significant differences in the prevalence of stunting across the three groups (Table 2). Those receiving both breakfast and lunch had stunting rates that were 5.3% lower than those receiving lunch only. Pairwise analysis shows this finding to be significant (p=0.003). Children from group 3 schools had stunting levels 7% lower than group 2 learners (p=0.001).
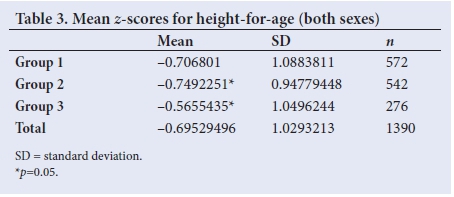
An assessment of the mean z-scores for height-for-age confirms the differences discussed above (Table 3). However, a Brown-Forsythe test demonstrated that these differences are not significant (p=0.02).
Obesity
Rates of children who were overweight and obese were different among the groups. Group 3 schools had very high rates of overweight and obesity. By contrast, children who had been receiving one meal a day over a prolonged period had overweight/obesity levels that were 12.3% lower. Children receiving two meals a day were even less likely to be overweight or obese, with rates 3.5% and 15.8% lower than groups 2 and 3, respectively.
An analysis of the mean z-scores for BMI-for-age confirms the above results (Table 5). The Brown-Forsythe test reveals that these differences are significant between group 1 and group 2 (p=0.000), and between group 2 and group 3 (p=0.000).
For group 3 only, we assessed whether the introduction of the lunch meal made any difference, over time, to overweight and obesity levels. The percentage of learners classified as obese declined from 26% at time point 1 to 19% at time point 2 (6 months later).
A paired f-test demonstrates a significant decrease in the mean BMI-for-age z-scores over the 6-month period (Table 6).
Discussion
The results presented above demonstrate that both programmes contributed positively to children's anthropometric outcomes. The children receiving only the NSNP had stunting levels of 12.59%, a rate similar to the national rate of 15.4% (for children aged 2 - 14 years),[9] which is to be expected given that over 63% of children in SA live in the poorest 40% of households,[17] and therefore receive the NSNP Children at the relatively poorer schools that were receiving two meals (group 1) had lower stunting levels than group 2 learners. The findings pertaining to the lower levels of stunting among learners receiving two meals are surprising. The research literature demonstrates that stunting is very resistant to change, particularly as children age.[18] Ideally, undernutrition effects need to be dealt with in early childhood, to avoid stunting. However, more recent literature has raised debate about the resistance of stunting to change. Prentice ef al.[19] suggest that children can catch up from stunting later on in life, although it seems that cognitive delays are particularly resistant to change.[20] The data presented here may mean that the combined effects of a breakfast and a lunch meal can shift stunting levels, corroborating a previous study conducted in an urban area on the combined effects of breakfast and lunch, where stunting was reduced by almost 5 percentage points over a 10-month period.[21]
The findings on overweight and obesity levels also point to promising effects of such programmes in contexts of the nutrition transition and the double burden of disease. The reduction over time in the percentage of learners who were overweight in the slightly higher socioeconomic status group 3 schools is promising. Studies on transitions out of overweight and obesity for children and adolescents in the context of school nutrition are largely focused on high-income contexts[10,22] and there is a paucity of previous evidence demonstrating the transition occurring at the same rate in middle- or low-income contexts. A systematic review of 22 studies in low- and middle-income countries reported that school-based obesity reduction programmes had favourable effects in 82% of programmes, but only one of these interventions was a breakfast programme[23] Some middle-income countries with increasingly obesogenic environments, such as Brazil and Chile, have redesigned their school nutrition programmes specifically to combat obesity.[241 We are therefore cautious in attributing our results to the school nutrition programme alone, which was not specifically designed to reduce obesity. Nonetheless, as the NSNP could have contributed to this shift, the study suggests that the NSNP might have protective effects for overweight and obesity, and implies that a carefully managed, diverse, nutritious daily meal may be a key protective factor for managing childhood obesity.
Furthermore, the lower rates of overweight and obesity among children receiving two meals a day point to the value of the addition of a breakfast to further reduce the risk of obesity for children. This latter finding is supported by data from a previous study evaluating this in-school breakfast programme that showed that levels of obesity were reduced over a 10-month period after the introduction of a school breakfast.[21]
School meals are one of a number of emerging platforms for addressing adolescent nutrition for enhanced benefits beyond early childhood.[25] While literature has previously noted that 'weight gains [from school feeding programmes1 can be either positive (in underweight populations) or negative (when risks of obesity are high)',[26] the present study raises the possibility that school nutrition can have positive impacts on stunting and overweight simultaneously.
Limitations
These findings illustrate trends in school nutrition impacts in a sample of rural SA school children, but there are various limitations that preclude relationships of causality. Firstly, the comparability of the third group of schools to the first two is limited. Because the NSNP feeds children at all schools in the first three socioeconomic categories, there was no naturally existing control school. Further, excluding qualifying children from the NSNP would have been ethically indefensible. The closest possible comparison schools were those that had been re-categorised. However, these schools were in a different geographic area, and were probably serving children of a slightly higher socioeconomic status. In addition, the comparability of the first two groups also has limitations, in that group 1 schools were drawn from across the first three socioeconomic groups, whereas those schools receiving the additional breakfast were from the poorest schools (predominantly category 1).
Secondly, the length of time that elapsed between the two data collection points for group 3 introduced a limitation. The process of gaining permission for the study at the national and provincial levels meant that the first measurement point was delayed. Schools were also averse to data collection taking place in the last term, which meant that the second measurement point was earlier than planned. This resulted in a relatively short period between measurement points. Ideally, a longer period should have elapsed, as anthropometric changes typically occur over a longer time period.
Thirdly, school effects were not taken into account in the analysis, our assumption being that these would be corrected for by the random selection. We also observed the schools and interviewed principals and teachers to determine whether there were any major differences at the school level that may have affected results. None were noted.
This article therefore offers a set of tentative conclusions that can assist in designing further research and in contributing to public and policy debate on school nutrition and children's health.
Conclusion
Investments in nutrition during school years are important, as 'nutrition is foundational to both individual and national development' in economic, health and human development terms.[20-22] Positive outcomes in relation to rates of stunting in the schools receiving breakfast are very encouraging, and point to the need for further research into what interventions can shift stunting in middle-childhood and during puberty.
In addition, the data presented here tentatively demonstrate the effects of the NSNP, and the additional benefits of the breakfast programme, in protecting children in these schools from childhood obesity. Poor nutrition in childhood has implications for the burden of disease, and a rise in rates of childhood obesity is directly linked to a rise in non-communicable diseases of adulthood.[24]
These outcomes suggest that well-managed and balanced school nutrition programmes, and the inclusion of breakfast, could play an important role in other countries battling the double burden of nutrition, with both childhood stunting and obesity public health concerns, although further research is required to corroborate these findings.
Acknowledgements. Prof. Eleanor Ross for review and editing of the article. Mr Zoheb Khan for statistical review of the article. Dr Maya van Gent and her team of kinanthropometrists for data collection and capture. Dr Anniza de Villiers for advisory support. The Department of Basic Education and Eastern Cape Department of Education for granting permission and negotiating access to the sampled schools. The Tiger Brands Foundation for supporting the study.
Author contributions. LG and TH conceptualised the study and the article focus. LG and TH were involved in the data collection. LG was responsible for the analysis. TH and LS verified the analysis. LS developed the literature review. All authors discussed the results and contributed to the final manuscript.
Funding. The Tiger Brands Foundation funded the study.
Conflicts of interest. None.
References
1. Briggs B. School feeding programmes: Summary of the literature and best practices. Village Hope Technical Report 6. Idaho, USA: Village Hope, 2008:3-4. [ Links ]
2. Iverson PO, du Plessis L, Marais D, Morseth M , H0isaether EA. Nutritional health of young children in South Africa over the first 16 years of democracy. S Afr J Child Health 2011;5(3):72-77. [ Links ]
3. International Food Policy Research Institute. Global Nutrition Report 2014: Actions and Accountability to Accelerate the World's Progress on Nutrition. Washington: IFPRI, 2014. [ Links ]
4. Popkin BM, Adair LS, Ng SW. Now and then: The global nutrition transition -the pandemic of obesity in developing countries. Nutr Review 2012;70(1):3-21. https://doi.org/10.1111/j.1753-4887.2011.00456.x [ Links ]
5. Haddad L, Cameron L, Barnett I. The double burden of malnutrition in SE Asia and the Pacific: Priorities, policies and politics. Health Pol Plann 2014;30(9):1193-1206. https://doi.org/10.1093/heapol/czu110 [ Links ]
6. Ng M, Fleming T, Robinson M. Global, regional, and national prevalence of overweight and obesity in children and adults during 1980 - 2013: A systematic analysis for the Global Burden of Disease Study. Lancet 2014;384(9945):766-781. https://doi.10.1016/S0140-6736(14)60460-8 [ Links ]
7. Popkin BM, Richards MK, Montiero CA. Stunting is associated with overweight in children of four nations that are undergoing the nutrition transition. J Nutr 1996;126(12):3009-3016. https://doi.org/10.1093/jn/126.12.3009 [ Links ]
8. Shisana O, Labadarios D, Rehle T, et al. South African National Health and Nutrition Examination Survey (SANHANES-1). Cape Town: HSRC Press, 2014. [ Links ]
9. Mayosi BM, Flisher AJ, Lalloo UG, Sitas F, Tollman SM, Bradshaw D. The burden of non-communicable diseases in South Africa. Lancet 2009;374(9693):934-947. https://doi.org/10.1016/S0140-6736(09)61087-4 [ Links ]
10. Affenito SG, Thompson D, Dorazio A, Albertson AM, Loew A, Holschuh NM. Ready-to-eat cereal consumption and the school breakfast program: Relationship to nutrient intake and weight. SCL Health 2013;83(1):28-35. https://doi.10.1111/j.1746-1561.2012.00744.x. [ Links ]
11. Department of Basic Education. Annual Report 2013/2014. Pretoria: Department of Basic Education, 2014. [ Links ]
12. Nhlapo N, Lues R, Kativu E, Groenewald W. Assessing the quality of food served under a South African school feeding scheme: A nutritional analysis. S Afr J Sci 2015;111(1/2): 1-9. https://doi.org/10.17159/sajs.2015/20140044 [ Links ]
13. Stewart A, Marfell-Jones M, Olds T, de Ridder H. International standards for anthropometric assessment. Palmerston North, New Zealand: International Society for the Advancement of Kinanthropometry, 2011. [ Links ]
14. World Health Organization. WHO Child Growth Standards. Geneva: WHO, 2006. www.who.int/growthref/en/ (accessed 28 August 2011). [ Links ]
15. Anderson, M. Body mass index in children and adolescents: Considerations for population-based applications. Int J Obesity 2006;30:590-594. https://doi.org/10.1038/sj.ijo.0803300 [ Links ]
16. Mascie-Taylor CG, Goto R. Human variation and body mass index: A review of the universality of BMI cut-offs, gender and urban-rural differences, and secular changes. J Physio Anthro 2007;26(2):109-112. https://doi.org/10.2114/jpa2.26.109 [ Links ]
17. Hall K, Sambu W. Demography of South Africa's children. In: Delany A, Jehoma S, Lake L, eds. South Africa Child Gauge. Cape Town: University of Cape Town, 2016. [ Links ]
18. Leroy J, Ruel M, Habicht J. Letters to the editor: Critical windows for nutritional interventions against stunting. Am J Clin Nutr 2013;98:854-855. [ Links ]
19. Prentice A, Ward K, Goldberg G, et al. Critical windows for nutritional interventions against stunting. Am J Clin Nutr. 2013;97(5):911-918. https://doi.org/10.3945/ajcn.112.052332 [ Links ]
20. Casale D, Desmond C. Recovery from stunting and cognitive outcomes in young children: Evidence from the South African Birth to Twenty Cohort Study. J Dev Orig Health Dis 2016;7(2):163-171. https://doi.org/10.1017/S2040174415007175 [ Links ]
21. Hochfeld T, Graham L, Patel L, Moodley J, Ross E. Does breakfast make a difference? An evaluation of a public-private investment in human capital development. Int J Edu Dev 2016;51:1-9. https://doi.org/10.1016/j.ijedudev.2016.07.005 [ Links ]
22. Jaime P, Lock K. Do school based food and nutrition policies improve diet and reduce obesity? Prevent Med 2009;48(1):45-53. https://doi.org/10.1016/j.ypmed.2008.10.018.23 [ Links ]
23. Verstraeten R, Roberfroid D, Lachat C, et al. Effectiveness of preventive school-based obesity interventions in low- and middle-income countries: A systematic review. Am J Clin Nutr 2012;96(2):415-438. https://doi.org/10.3945/ajcn.112.035378 [ Links ]
24. Doak C. Large-scale interventions and programmes addressing nutrition related chronic diseases and obesity: Examples from 14 countries. Pub Health Nutr 2002;5(1A):275-277. https://doi.org/10.1079/phn2001304 [ Links ]
25. Bhutta ZA, Das JK, Rizvi A, et al. Evidence-based interventions for improvement of maternal and child nutrition: What can be done and at what cost? Lancet 2013;382(9890):452-477. https://doi.org/10.1016/S0140-6736(13)60996-4 [ Links ]
26. Ruel MT, Alderman M, the Maternal and Child Nutrition Study Group. Nutrition-sensitive interventions and programmes: How can they help to accelerate progress in improving maternal and child nutrition? Lancet 2013;382:536-551. https://doi.org/10.1016/S0140-6736(13)60843-0 [ Links ]
 Correspondence:
Correspondence:
L Graham
lgraham@uj.ac.za
Accepted 23 April 2018














