Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
South African Journal of Child Health
versão On-line ISSN 1999-7671
versão impressa ISSN 1994-3032
S. Afr. j. child health vol.11 no.1 Pretoria Jan./Mar. 2017
http://dx.doi.org/10.7196/sajch.2017.v11i1.1148
RESEARCH
doi:10.7196/sajch.2017.v11i1.1148
Individual v. community-level measures of women's decision-making involvement and child survival in Nigeria
J O AkinyemiI, II; S A AdediniI, III; C O OdimegwuI
IPhD; Demography and Population Studies Programme, University of the Witwatersrand, Johannesburg, South Africa
IIPhD; Department of Epidemiology and Medical Statistics, Faculty of Public Health, University of Ibadan, Ibadan, Nigeria
IIIPhD; Department of Demography and Social Statistics, Obafemi Awolowo University, Ile Ife, Nigeria
ABSTRACT
BACKGROUND. Although decision-making authority is associated with maternal healthcare utilisation, the evidence on the relative importance of individual-level v. community-level decision-making participation for child survival in sub-Saharan Africa is limited.
OBJECTIVES. To assess the net effects of individual- and community-level measures of decision-making involvement (DMI) on under-5 mortality in Nigeria.
METHODS. Data on a nationally representative sample of 31 482 children in the 2013 Nigeria Demographic and Health Survey were analysed. Mothers who reported involvement in decision-making on own healthcare, major household purchases and visits to friends and relatives were categorised as having high DMI. Community-level measures of DMI were derived by aggregating the individual measures at the cluster level. Kaplan-Meier estimates of childhood mortality rates were computed. Multilevel discrete-time hazard models were employed to investigate the net effect of individual- and community-level DMI on childhood mortality.
RESULTS. Childhood mortality, at 59 months, was higher among children of women with low DMI (120 per 1 000) compared with those with high DMI (84 per 1 000). The full multilevel model showed that there was no difference in the risk of childhood death between children whose mothers had high v. low DMI (hazard ratio (HR) 1.01, CI 0.90 - 1.12). However, mortality risk was found to be lower among children in communities with medium DMI (HR 0.84, CI 0.74 - 0.96). Maternal age at child's birth, education, household wealth index and preceding birth interval were significantly associated with under-five mortality.
CONCLUSION. Besides socioeconomic and biodemographic characteristics, community- and not individual-level DMI was associated with under-5 mortality. Women's empowerment programmes targeting maternal and child health outcomes should also focus on communities.
Due to the difficulty in empirical measurement of women's empower ment, most earlier studies have used proxy measures such as level of education and proportion (of women) who owned land.[1] Undoubtedly, such indicators reflect socioeconomic status more than empowerment, although the two are positively related. For operational/practical purposes, in this study, empowerment refers to the ability to make choices or take decisions.[2] Subsequent to developing a framework for relationships between sex, gender, population/health/nutrition outcomes, the Demographic and Health Survey (DHS) programme introduced four sets of gender-related questions into the women's core questionnaire in 1999.[3] These questions captured information on women's participation in household decision-making, gender-related hurdles in accessing healthcare and women's acceptance of norms that justify men's control over women. Consequently, relationships between these decisionmaking (empowerment) indicators and reproductive health concepts (such as fertility intention, use of contraceptives and maternal health services utilisation) have been explored in some developing countries.[4,5]
Studies have shown that women's empowerment is positively associated with contraceptive use despite control for education level and other sociodemographic characteristics.[4] Other studies have investigated the link between women's empowerment and use of antenatal care (ANC), skilled/facility delivery and postnatal care services. However, the eveidence was mixed and depended on the type of maternal healthcare service under investigation. The common pattern was that women's empowerment increased the uptake of ANC and postnatal services.[6-8] However, the influence of women's empowerment on skilled delivery care was weak in Ethiopia/ Eriteria[9] and Nairobi, Kenya[10] but significant in Nigeria.[11,12] Aside from maternal healthcare utilisation, Adhikari et al.,[13] and Desai and Johnson[14] reported that women's empowerment was also a significant independent predictor of child mortality. In both studies, infants born to women with decision-making authority were less likely to die.
Apart from the fact that fewer studies have been devoted to child health outcomes, the results also depend on the measures of empowerment. Furthermore, a large proportion of previous studies investigated empowerment at the level of individual women rather than at community level. Women's empowerment at the community level refers to the prevailing community norm with respect to the ability of women to make decisions on matters concerning them, their children and/or their households. Context or the place where a woman lives plays a significant role in her ability to take decisions. If the general belief or attitude in a community is that a woman is free to take certain decisions, women in such communities would enjoy more decision-making autonomy than those in other communities with opposing views.
Meanwhile, there is increasing evidence of the role of context or community as far as maternal and child health outcomes are concerned.[6,15,16] These studies showed that contextual variables such as residence (rural v. urban), community level of education, poverty, prenatal care and ethnic diversity were associated with utilisation of prenatal care, skilled attendance at delivery, postnatal care and childhood mortality. Beyond these factors there is a need to establish the relative importance of individual- v. community-level effects of women's decision-making involvement (DMI) on child health outcomes.
Nigeria has the highest childhoo d mortality rate in sub-Saharan Africa. Alhough progress has been made in recent years, the slow pace has been attributed to poor progress in child survival interventions.[17] Interventions aimed at promoting child survival are targeted at mothers who are the primary caregivers of their children. The uptake or adoption of modern child healthcare practices and any survival intervention will depend on women's decision-making autonomy. Therefore, this study was aimed at investigating the relationship between maternal DMI and childhood mortality in Nigeria. The study distinguished between individual- and community-level measures of decision-making and also determined their net effects while controlling for other background characteristics.
Methods
The data analysed for this study were extracted from the children's recode data file of the 2013 Nigeria Demographic and Health Survey (NDHS). The NDHS 2013 is the fifth round of a national survey conducted to monitor population and reproductive health among Nigerians. For administrative purposes, Nigeria is divided into 36 states and a Federal Capital Territory (FCT). Details of the sample design and survey findings are available in the published report.[18] Specifically, in the NDHS 2013, a stratified three-stage cluster design was used for the selection of respondents. The primary sampling units, referred to as clusters (communities) in this study were enumeration areas selected from a sampling frame prepared based on the 2006 Nigeria population and housing census. With a fixed sample intake of 45 households per 904 clusters (rural = 532, urban = 372), a total of 40 680 households were selected and 38 948 women aged 15 - 49 years were interviewed successfully. Data for 31 482 children nested in 896 clusters, and born within 5 years before the survey, were analysed. These data were based on the reproductive history of the women. As such, they contained variables on women's characteristics as well as detailed information on the birth, sex and survival status of each under-five child.
Variables and measurement
Children constituted the unit of analysis in this study. Therefore, the dependent variable was a child's death, which was treated as an event history outcome. Survival time was age at death, while children who were alive by the survey date were censored at their current age. There were two primary independent variables:
1. Individual-level maternal DMI: This was an indicator variable coded as 1 (high involvement) or 0 (low involvement). It was coded 1 if a woman participated in all of the following decisions: own healthcare, major household purchases and visits to family or relatives. Decision on own healthcare refers to the choice of where to go and what to do for any health problem. Major household purchases implied the purchase of items other than those for daily needs in the households. Decisions on visits to family/friends reflect a woman's freedom of movement and association.
2. Community-level DMI: This captures the community norms about women's DMI. The variable was created from individual-level DMI by aggregating at the cluster (community) level. We first obtained the proportion of women in each community who participate in decision-making using the egen command in Stata (StataCorp, USA). The proportion was then divided into tertiles categorised as low, medium and high. To reduce the problem of multicollinearity between the individual and community measures of DMI, community measures were computed for all women in the cluster irrespective of whether they had children or not.
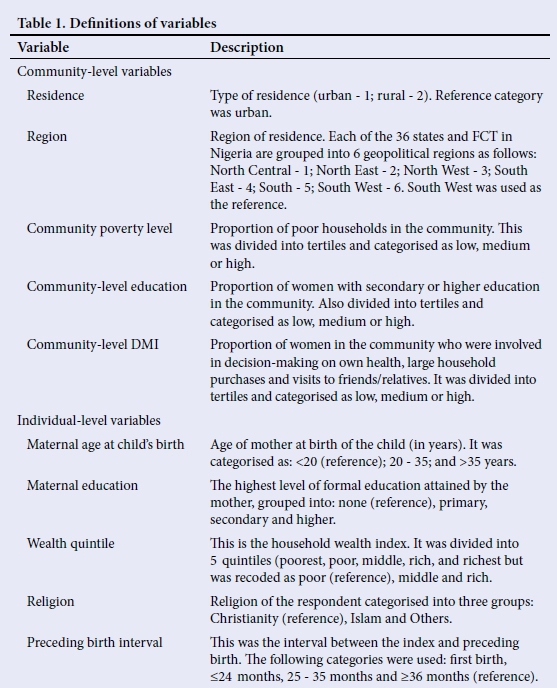
Other individual- and community-level variables that are known from the literature to correlate with women's DMI and child mortality were controlled in the analyses (Table 1). Household wealth index was calculated from the assets possessed by each household using principal component analysis.[19] Apart from region and place of residence, other community-level variables were community level of education and poverty. Derivation of community-level education and poverty followed the same procedure used for the community-level DMI.
Statistical analysis
Frequency distribution was generated to summarise the variables, while the KaplanMeier (KM) method was employed to estimate childhood mortality rates. For multivariate analysis, multilevel discrete-time hazard models were fitted. A distinction was made between individual- and community-level effects of DMI on childhood mortality. Apart from the investigation of community-level effects, this modelling approach also ensured that standard errors were appropriately estimated to account for the hierarchical structure ofthe data. In order to implement the discrete-time hazard model, each record was transformed into person-time records with each new record (in the transformed dataset) corresponding to a unit of time. For this study, a two-level structure was considered: children (level 1) nested in communities (level 2). The model equation is as follows:
Logit(htij) = αt + β1kX1kij + β2kX2kj + Uj + eij
where:
htij = hazards (risk) of death by child i in cluster j
αt = baseline hazard of death at time t
ß1k = coefficients for the individual-level variables
Xkij = individual-level covariates (education, age group, wealth index, etc.) for child i in community j
ß2k = coefficients for the community-level variables
X2kj = community-level covariates (i.e. community-level DMI, residence, region, etc.)
uj = community-level random effect
eij = error terms for the individual-level model.
In essence, two-level random intercept discrete-time hazards models were fitted, with the assumption that individual-level covariates have similar effects across all communities. Error terms were assumed to be normally distributed with zero mean and constant variance at both individual (σe2) and community (σu2) levels. Fixed effects of individual-level variables were presented as hazard ratio (HR) with 95% confidence interval (CI). Random effects that represent the community effects were summarised using the variance (and standard errors) from which the intracluster correlation (ICC) was estimated. The ICC captures the extent to which children's deaths are correlated in the community or the extent to which children in the same community are exposed to the same characteristics associated with the risk of death.
Modelling procedure
Models were fitted in four stages in order to explore the influence of individual-and community-level DMI on childhood mortality. First, the effect of each covariate was assessed using univariate models with one independent variable at a time. The covariates in model I were individual- and community-level DMI. Model II combined model I with other individual-level covariates while model III consisted of model I and community-level variables. In model IV, all variables were included in order to adjust for confounding variables and determine the net effect of the key explanatory variables. All analyses were done using Stata SE version 12.0.
Ethical considerations
This study involved a secondary analysis of anonymised data from the NDHS 2013. The survey was approved by the National Health Research Ethics Committee in Nigeria (ref. no. NHREC/01/01/2007). Informed consent was obtained from respondents during the data collection process. Formal approval to use the data was obtained from the NDHS programme.
Results
Table 2 shows the frequency distribution of individual-level characteristics of all the children, including those who have died.
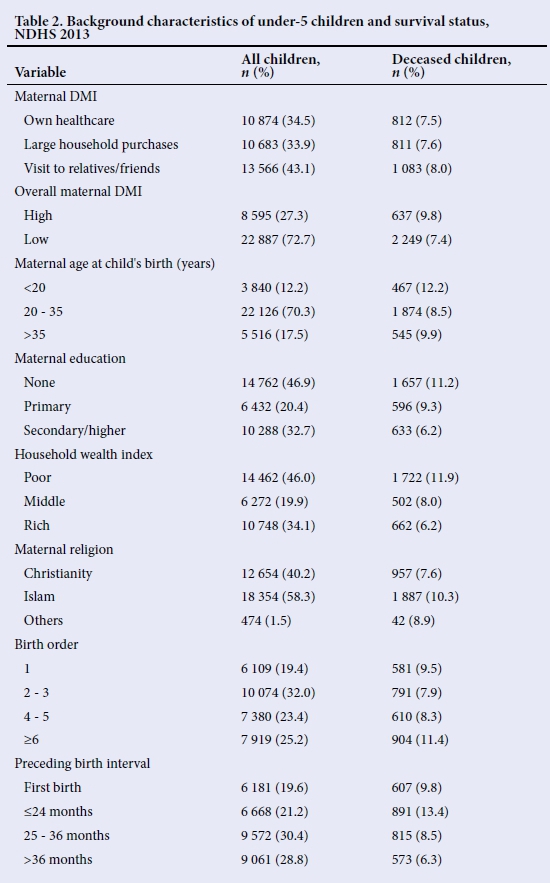
The proportions of children whose mothers were involved in decision-making on their healthcare, large household purchases and visits to friends/relatives were 34.5%, 33.9% and 43.1%, respectively. Overall, 27.3% of 31 482 children had mothers who were involved in decision-making. Close to half (46.9%) belonged to mothers with no formal education, while 32.7% of mothers attained secondary or higher education. In terms of household wealth index and religion, 46.0% of children lived in poor households while 58.3% had Muslim mothers. First births constituted 19.4% among the under-fives. Distribution of the preceding birth interval revealed that 21.2% were born <24 months after a previous birth.
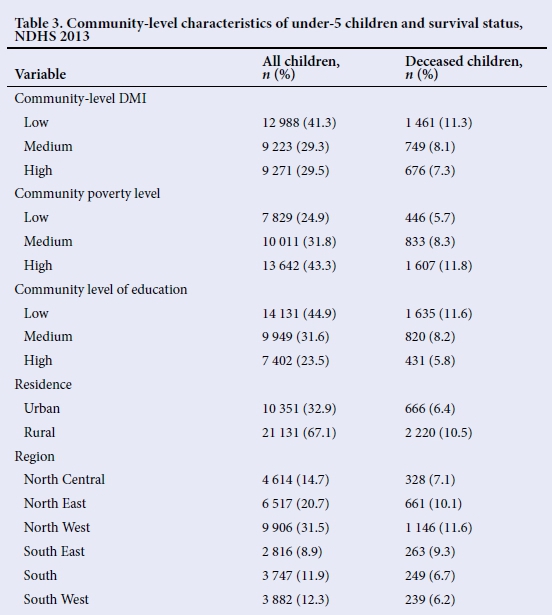
Table 3 shows that 41.3% and 29.5% of children lived in communities with low and high maternal DMI, respectively. Similarly, the largest proportion of children (43.3%) lived in communities with a high poverty level while 44.9% resided in communities with low level of education. About two- thirds (67.1%) were rural dwellers. Regional distribution showed that about one-third (31.5%) were from the North-West region of Nigeria.
Maternal involvement in decision-making and childhood mortality
Fig. 1 illustrates the KM curve for the probability of death according to individual-level maternal DMI. At different ages, mortality was higher among children of women with low DMI. The under-five mortality rate was estimated as 120 per 1 000 live births (low DMI) and 84 per 1 000 live births (high DMI).
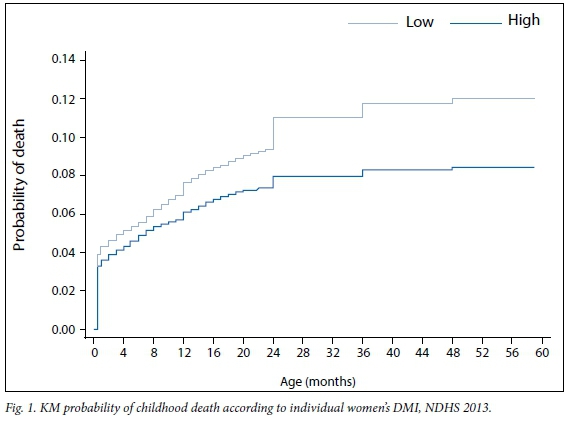
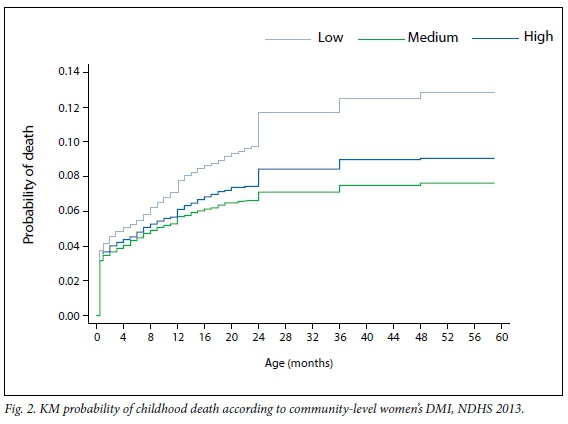
Fig. 2 presents the KM curve according to community-level involvement in decision-making. By the 59th month, the mortality rates were 138 per 1 000 live births (low involvement), 97 per 1 000 live births (medium involvement) and 82 per 1 000 live births (high involvement).
The results of multilevel discrete-time hazard models fitted to further explain the relationship between childhood mortality and maternal involvement in decision-making are shown in Table 4. Panel 1 of Table 4 shows the HR or the univariate models. Children of women with high involvement in decision-making were less likely to die before age 5 (HR 0.81, Cl 0.74 -0.89). Middle and rich household wealth quintiles also showed enhanced child survival. Children with a preceding birth interval <24 months were two times more likely to die than those with an interval of at least 36 months.
At the community level, high DMI (HR 0.62, Cl 0.54 - 0.70) and high education (HR 0.49, Cl 0.43 - 0.56) were protective against child death. Significant regional differences in childhood mortality risk were observed in North East (HR 1.65, Cl 1.37 -1.99), North West (HR 1.94, Cl 1.63 - 2.31) and South East Nigeria (HR 1.56, Cl 1.26 - 1.93) compared with the South Western region.
Model I (Table 4, panel 2) shows that individual DMI was no longer statistically significant, but the community-level measure was. Children in low (HR 0.69, Cl 0.61 - 0.79) and high (HR 0.64, Cl 0.56 - 0.74) decision-making communities were less likely to die before age five.
In model II (Table 4, panel 3), other individual-level variables were controlled to assess the effect on DMI. Low (HR 0.84, CI 0.74 - 0.96) and medium (HR 0.83, CI 0.72 -0.97) community-level DMI were associated with lower risk of childhood mortality. The individual-level variables maintained their direction of effect as in the univariate models.
Model III (Table 4, panel 4) shows the extent to which other community-level measures explained the effect of individual/ community-level decision-making on under-5 mortality. The HRs for DMI remained the same as in model II. With the exception of the South East region (HR 1.47, CI 1.18 - 1.83), the statistical significance of the differentials between South West and other regions (North East and North West) has disappeared.
Panel 5 of Table 4 shows the results of model IV, in which all individual- and comunity-level variables were controlled. There was no difference in the risk of under-5 death between children whose mothers had low v. high DMI. However, community-level decision-making was significant, with lower risks of death among children in communities with medium maternal DMI (HR 0.84, CI 0.74 - 0.96). Other variables associated with lower risk of under-5 death included: maternal age 20 - 35 years (HR 0.82, CI 0.72 - 0.93); secondary/higher education (HR 0.80, CI 0.68 - 0.93); rich household wealth quintile (HR 0.78, CI 0.66 -0.92); and urban residence (HR 0.79, CI0.69 -0.91). Factors found to increase the hazard of under-5 death were being a first birth (HR 11.09, CI 6.92 - 17.75), and birth interval <24 months (HR 2.07, CI 1.85 - 2.31).
Discussion
The status of a woman is directly related to her ability to seek medical and nutritional care for herself and her children. In a patriarchal society such as Nigeria, the ability of women (as direct targets for child survival programmes) to translate knowledge of interventions to child care will depend on their decision-making authority. This study was therefore conducted to explore the effects of individual- and community-level DMI of mothers on child mortality rates in Nigeria.
The risk of childhood mortality was higher among children of women with low DMI. This agrees with results from Nepal,[13] which showed that children of women involved in decision-making on their healthcare were less likely to die before 5 years. The findings also indicate that community-level DMI was associated with a lower risk of child death. This is similar to reports by Desai and Johnson,[14] which revealed that the effects of women's DMI on child health outcomes were stronger at the community than individual level in selected Asian and sub-Saharan African countries (excluding Nigeria). These findings suggest that an individually empowered woman may have limited DMI if she lives in a community where women have limited decision-making power. The implication is that community norms and attitudes about decision-making may be more important for child survival efforts than individual decision-making authority.[2] The lack of relationship between individual women's DMI and childhood mortality is similar to reports from four Asian countries (India, Malaysia, the Philippines and Thailand) in which the association between individual women's autonomy and child survival was found to be weak.[14] It is likely that women are not able to translate their individual decision-making authority into child survival advantages. Alternatively, it could be that appropriate measures of empowerment that adequately capture the type of individual DMI that influences child survival are not being used. Development of empowerment measures that are culturally sensitive in different settings has been advocated, but this would also suffer from global standardisation, which is necessary for intercountry and regional comparisons.[4]
The results further reaffirmed the strong influence of education, type of residence (rural or urban), maternal age and wealth quintile on child survival. The childhood mortality differentials according to these variables have been previously described.[16,17]
The random component in the multilevel model showed significant intracommunity correlation in the risk of child death. This correlation justified the analytical method used in the present study because children in the same community are exposed to similar circumstances, cultural norms and practices, and thus they would not have been completely independent of one another as far as the under-five death rate was concerned. Childcare practices and health-seeking behaviours are greatly influenced by community norms and these also affect child health outcomes.[20]
Study limitations
One limitation in the analyses is the inability to explore contextual variables that capture community norms and practices related to child survival. Such variables were not collected in the NDHS. The modelling procedure, however, adequately controlled for these unobserved variables. Also, there was no measure of decisionmaking about child healthcare. Questions related to decisions about child healthcare would have afforded an assessment of the influence of decision-making (in this regard) on child healthcare. Regardless, the analyses were based on nationally representative data. Therefore, the findings are applicable to current policies and programmes on women's empowerment and child healthcare.
Conclusion
Under-5 mortality is negatively associated with maternal DMI in Nigeria. The effect of community-level women's DMI on the risk of childhood death is greater than that of the individual level, even though the former is partly explained by individual- and community-level education and wealth status. Empowerment programmes should not only target individual women but should also address community norms and beliefs about the ability of women as primary caregivers to take initiative and make timely decisions, especially on matters related to personal health, as well as that of their children. Given the importance of child survival in sustainable development, questions about decision-making on children's health should be included in the next round of demographic and health surveys. This will make it possible to directly assess the extent to which women have autonomy in child care.
Acknowledgements. We acknowledge the ICF Macro International and other implementing partners for granting access to the NDHS data. We also appreciate the University of the Witwatersrand, Johannesburg, South Africa, for providing a research-friendly environment to conduct this study. This research was supported by the Consortium for Advanced Research Training in Africa (CARTA). CARTA is jointly led by the African Population and Health Research Center and the University of the Witwatersrand and funded by the Wellcome Trust (UK) (Grant no. 087547/Z/08/Z), the Carnegie Corporation of New York (Grant no. B8606.R02), and Sida (Grant no. 4100029). The statements made and views expressed are solely the responsibility of the authors.
REFERENCES
1. Bloom SS, Wypij D, das Gupta M. Dimensions of women's autonomy and the influence on maternal health care utilization in a North Indian city. Demography 2001;38(1):67-78. https://dx.doi.org/10.2307/3088289 [ Links ]
2. Kabeer N. Gender equality and women's empowerment: A critical analysis of the third millennium development goal. Gend Dev 2005;13(1):13-24. https://dx.doi.org/10.1080/13552070512331332273 [ Links ]
3. Sunita K. A focus on gender: Collected papers on gender using DHS data. Maryland, USA: ORC Macro, 2005:1-13. [ Links ]
4. Ahmed S, Creanga AA, Gillespie DG, Tsui AO. Economic status, education and empowerment: Implications for maternal health service utilization in developing countries. PLoS ONE 2010;5(6):1-6. https://dx.doi.org/10.1371/journal.pone.0011190 [ Links ]
5. Shimamoto K, Gipson JD. The relationship of women's status and empowerment with skilled birth attendant use in Senegal and Tanzania. BMC Pregnancy Childbirth 2015;15(1):1-11. https://dx.doi.org/10.1186/s12884-015-0591-3 [ Links ]
6. Babalola S, Fatusi A. Determinants of use of maternal health services in Nigeria - looking beyond individual and household factors. BMC Pregnancy Childbirth 2009;9(1):1-13. https://dx.doi.org/10.1186/1471-2393-9-43 [ Links ]
7. Hou X, Ma N. The effect of women's decision-making power on maternal health services uptake: Evidence from Pakistan. Health Policy Plan 2013;28(2):176-184. https://dx.doi.org/10.1093/heapol/czs042 [ Links ]
8. Sado L, Spaho A, Hotchkiss DR. The influence of women's empowerment on maternal health care utilization: Evidence from Albania. Soc Sci Med 2014;114(1):169-177. https://dx.doi.org/10.1016/j.socscimed.2014.05.047 [ Links ]
9. Woldemicael G. Do women with higher autonomy seek more maternal and child health-care? Evidence from Ethiopia and Eritrea. Stockholm: Stockholm University, 2007:1-28. [ Links ]
10. Fotso JC, Ezeh AC, Essendi H. Maternal health in resource-poor urban settings: How does women's autonomy influence the utilization of obstetric care services? Reprod Health 2009;6(1):1-8. https://dx.doi.org/10.1186/1742-4755-6-9 [ Links ]
11. Corroon M, Speizer IS, Fotso JC, et al. The role of gender empowerment on reproductive health outcomes in urban Nigeria. Matern Child Health J 2014;18(1):307-315. https://dx.doi.org/10.1007/s10995-013-1266-1 [ Links ]
12. Ononokpono DN, Odimegwu CO. Determinants of maternal health care utilization in Nigeria: A multilevel approach. Pan Afr Med J 2014;17(2):5-11. https://dx.doi.org/10.11604/pamjs.supp.2014.17.1.3596 [ Links ]
13. Adhikari R, Sawangdee Y. Influence of women's autonomy on infant mortality in Nepal. Reprod Health 2011;8(1):1-7. https://dx.doi.org/10.1186/1742-4755-8-7 [ Links ]
14. Desai S, Johnson K. Women's decision-making and child health: Familial and social hierarchies. Maryland, USA: ORC Macro, 2005:55-67. [ Links ]
15. Ononokpono DN, Odimegwu CO, Imasiku EN, Adedini SA. Does it really matter where women live? A multilevel analysis of the determinants of postnatal care in Nigeria. Matern Child Health J 2014;18(4):950-959. https://dx.doi.org/10.1007/s10995-013-1323-9 [ Links ]
16. Adedini SA, Odimegwu C, Imasiku EN, Ononokpono DN, Ibisomi L. Regional variations in infant and child mortality in Nigeria: A multilevel analysis. J Biosoc Sci 2014;47(2):165-187. https://dx.doi.org/10.1017/s0021932013000734 [ Links ]
17. Akinyemi JO, Bamgboye EA, Ayeni O. New trends in under-five mortality determinants and their effects on child survival in Nigeria: A review of childhood mortality data from 1990-2008. Afr Popul Stud 2013;27(1):25-42. https://dx.doi.org/10.11564/27-1-5 [ Links ]
18. National Population Commission (NPC). Nigeria Demographic and Health Survey 2013. Abuja, Nigeria, and Rockville, Maryland, USA: NPC and ICF International, 2014;377-396. [ Links ]
19. Rutstein SO, Staveteig S. Making the demographic and health surveys wealth index comparable. Maryland, USA: ICF International, 2014:1-59. [ Links ]
20. Fayehun O, Omololu O. Ethnicity and child survival in Nigeria. Afr Popul Stud 2011;25(1):92-112. https://dx.doi.org/10.11564/25-1-258 [ Links ]
 Correspondence:
Correspondence:
J O Akinyemi
joshua.akinyemi@wits.ac.za














