Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
South African Journal of Child Health
versão On-line ISSN 1999-7671
versão impressa ISSN 1994-3032
S. Afr. j. child health vol.10 no.4 Pretoria Dez. 2016
http://dx.doi.org/10.7196/sajch.2016.v10i4.1145
REVIEW
The management of persistent pulmonary hypertension of the newborn: A review
L G LloydI; J SmithII
IMB ChB, DCH (SA), FC Paed (SA), MMed (Paed), Cert Neonatology (SA); Division of Neonatology, Department of Paediatrics and Child Health, Stellenbosch University and Tygerberg Children's Hospital, Cape Town, South Africa
IIMB ChB, MMed, FC Paed (SA), PhD (Paed); Division of Neonatology, Department of Paediatrics and Child Health, Stellenbosch University and Tygerberg Children's Hospital, Cape Town, South Africa
ABSTRACT
Persistent pulmonary hypertension of the newborn is a neonatal emergency with a high mortality rate in spite of several advances in the management thereof. The underlying pathophysiology is complex and multifactorial. The gold standard of treatment is inhaled nitric oxide, yet up to a third of patients will not respond to standard treatment. This article reviews treatment modalities available, as well as the evidence to support the use of these treatment options.
The first literary reference to persistent pulmonary hypertension (PH) of the newborn (PPHN) can be found in 1969 by Gersony et al.,[u] who described it as persistence of physiologic characteristics of the fetal circulation in the absence of disease. Defined as a failure of normal circulatory transition at birth, or more specifically as failure of the pulmonary vasculature to relax after birth, with continued shunting of non-oxygenated blood into the systemic circulation via fetal channels (ductus arteriosus and foramen ovale), it remains a challenging neonatal emergency to manage.[3-6] Term and near-term infants are most commonly affected, but PPHN can occur in premature infants.[4]
The incidence of PPHN in developed countries has been estimated as 1.9 per 1 000 live births; however, the incidence is likely to be higher in developing countries.[2,3,5,7] PPHN constitutes ~10% of neonatal intensive care unit (NICU) admissions, with the reported mortality rate ranging from 10 to 20%.[4,5,8-10]
Physiology
The normal physiological state of a fetus is best described as hypoxaemic, with PH and reduced pulmonary blood flow, and with the placenta responsible for gas and nutrient exchange.[3,4,6,10]It is important to understand that the fetus is not hypoxic, as adequate oxygen delivery to the tissues is maintained and facilitated by a high cardiac output and high fetal haemoglobin levels with increased oxygen affinity.[3]
Factors involved in maintaining an increased pulmonary vascular resistance (PVR) in utero include fluid-filled lungs, decreased nitric oxide (NO) and prostacyclin (PGI2), and increased endothelin-1 (ET-1).[4] Products ofthe prostaglandin pathway, such as thromboxane and leukotriene, also play a role. Serotonin increases fetal PVR, which brings into question the safety of using selective serotonin reuptake inhibitors (SSRIs) during pregnancy.[3,4,6,11]
Fetal circulation
The systemic and pulmonary circulations of the fetus function in parallel, where both ventricles essentially eject blood into the aorta and use the foramen ovale and ductus arteriosus to bypass the pulmonary circulation. Only 13 - 25% of blood ejected will reach pulmonary circulation.[3,4,6,11]
Transition to extrauterine life
The normal transition from 'parallel' to 'series' circulation starts with a rapid decrease in PVR with the first breath, and an increase in systemic vascular resistance with the removal of the low-resistance placenta after umbilical cord clamping.[3,10] The first breath fills the lungs with air, causing an eight-fold increase in pulmonary blood flow. The resulting shear stress and oxygenation up-regulates the expression of endothelial NO synthase (eNOS).[3,4,6] Endothelial NO synthesised from l-arginine activates soluble guanylyl cyclase (sGC), converting cyclic guanosine triphosphate (cGTP) to cyclic guanosine monophosphate (cGMP), which facilitates smooth muscle relaxation.[4-6] Oxygenation also inhibits phosphodiesterase-5 (PDE5), increasing the availability of cGMP.[4]
The production of prostaglandin endoperoxides from arachadonic acid in the endothelium, specifically PGI2, stimulates adenylyl cyclase to convert adenosine triphosphate (ATP) to cyclic adenosine monophosphate (cAMP), which also facilitates pulmonary vaso-dilatation.[4,6] Phosphodiesterase-3 (PDE3) increases the availability of cAMP. Prostaglandins decrease PVR less than does NO.[4]
Aetiology and pathophysiology
When there is failure of the normal transition to extra-uterine life, with the persistence of increased PVR, PPHN occurs. Hypoxia, acidosis and hypercarbia cause vasoconstriction, and play an important role in the underlying pathogenesis.[10]
The causes of PPHN can be classified into four groups: underdevelopment, maldevelopment, maladaptation and intrinsic obstruction (Table 1).[3,4,6]
Meconium aspiration syndrome (MAS) is the most common cause of PPHN.[4,6] Meconium-stained liquor occurs in 5 - 24% of normal pregnancies, and of these 5% will develop MAS. Meconium causes airway obstruction, inactivation of surfactant and chemical pneumonitis, owing to the release of proinflammatory cytokines. The resultant decreased ventilation/perfusion ratio, with hypoxaemia and hypercarbia, may lead to PPHN.[3]
Idiopathic or 'black-lung' PPHN occurs in 20 - 25% of cases, with 'black lung' referring to the paucity of pulmonary vascularity.[3,4,6,8] There is an absence of parenchymal lung disease, as the underlying problem is vascular smooth muscle hyperplasia of the normally muscle-free arteries. A questionable association with antenatal use of non-steroidal anti-inflammatory drugs and SSRIs exists.[12]
Congenital diaphragmatic hernia is associated with lung hypoplasia and the decreased cross-sectional area of the pulmonary vascular bed. Lung damage is often exacerbated by volutrauma, hyperoxia and mechanical ventilation.[6]
PH can occur in premature infants, with one-third of patients with bronchopulmonary dysplasia (BPD) having an underlying diagnosis of PH. The combination of BPD and PH is associated with a poor outcome.[3,6,8]
Congenital cardiac disease, such as total anomalous pulmonary venous return and hypoplastic left heart syndrome, may also present with PPHN.[4]
Risk factors
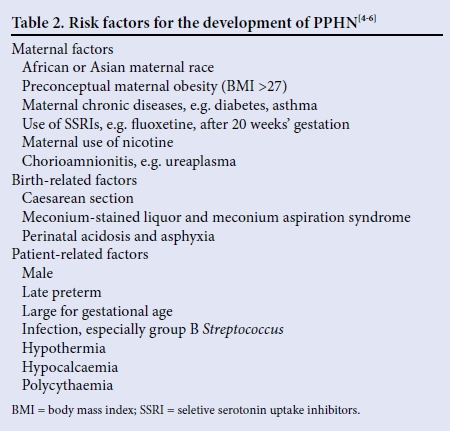
Several risk factors have been identified, including an unfavourable perinatal fetal environment which, in combination with certain epigenetic factors, may play a role in the expression of genes involved in the regulation of perinatal pulmonary circulation (Table 2).[2]

Diagnosis
PPHN presents in the first 24 hours of life. The classic clinical presentation includes respiratory distress, cyanosis, hypoxaemia and acidosis.[5] The echocardiogram is the gold standard for the diagnosis of PPHN (Table 3).[3-5,9]

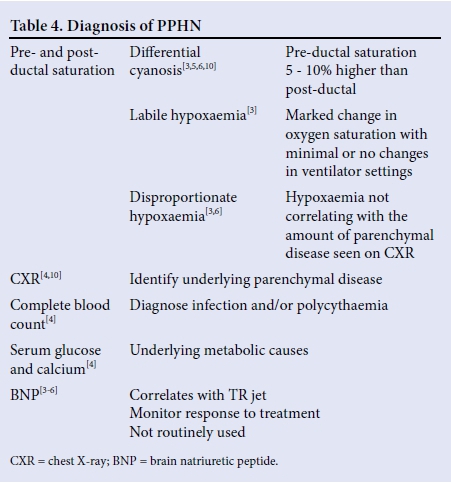
Although the echocardiogram is the gold standard for the diagnosis of PPHN, it is often not available in resource-limited settings, therefore other special investigations are of critical importance (Table 4).[13] The traditional comprehensive structural and functional echocardiogram performed by cardiologists can be supplemented by training neonatologists to perform a targeted neonatal echocardiogram (TnEcho) to expedite diagnosis of PPHN and to monitor the response to therapy.[14]

Severity of PPHN
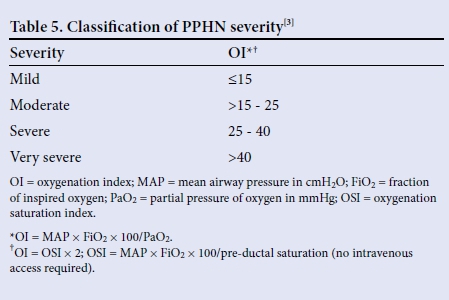
The severity of PPHN can be calculated using the oxygenation index (Table 5).[3]
Management
General management
The first-line management includes ventilation, oxygenation, maintaining systemic blood pressure and maintaining homeostasis.[10] Stabilisation, establishing venous access and treating the underlying cause are critically important.
Supportive care
Hypothermia, acidosis, polycythaemia, hypoglycaemia, hypocal-caemia and hypomagnesaemia should be corrected appro-priately.[3,10] Correction of acidosis with controlled alkalosis using an alkali infusion and hyperventilation is no longer advocated due to the association with sensorineural hearing loss and impaired cerebral perfusion.[3,10]
Minimal handling and judicious sedation is advised to avoid labile hypoxaemia. Antimicrobial therapy should be initiated if underlying infection is suspected.[6]
Mechanical ventilation and oxygenation
Oxygen is a pulmonary vasodilator; however, hyperoxia and ventilation with 100% oxygen has been associated with a reduced response to NO in experimental lamb models.[3,4] The aim of mechanical ventilation should be to maintain a PaCO2 of 40 - 60 mmHg (5.3 - 8.0 kPa) and PaO2 of 60 - 90 mmHg (8 - 12 kPa) by using gentle ventilation to optimise lung volume.[4,5] High-frequency oscillatory ventilation (HFOV) can minimise lung injury, but has not been proven to have a clear benefit over conventional ventilation, except when used in combination with inhaled NO (iNO) in the treatment of MAS.[4,5,15] HFOV is recommended if peak inspiratory pressures (PIP) of >28 cmH2O or tidal volumes > 6 mL/kg are required to maintain PaCO2 <60 mmHg (<8 kPa).[3]
Surfactant
In patients with MAS or pneumonia, surfactant may reduce the need for extracorporeal membrane oxygenation (ECMO), but does not reduce the duration of ventilation, length of the hospital stay or incidence of complications.[4,5] Prior to giving the surfactant, adequate recruitment of lung volume should be prioritised. [4,5]The greatest benefit was seen when administered at an OI of 15 - 25.[3,6] Dosages of 50 - 200 mg/kg may be used up to four times in the first 24 hours.[16] The use of a surfactant in CDH is not recommended, unless there is clear evidence of surfactant deficiency, and then only 50% of the dose should be given because of the underlying pulmonary hypoplasia.[3]
Management of systemic hypotension
Systemic hypotension should be managed with fluids, vasopressors and inotropes. The optimal blood pressure (BP) has not been determined in a randomised controlled trial (RCT), and should therefore be maintained at the normal value for the gestational age.[5,6] Supraphysiologic BP ought to be avoided, as it may add to ventricular strain and increase endothelial dysfunction by increasing shear stress in the constricted pulmonary circuit.[3]
Inotropic support should be considered early, as decreased systemic BP exacerbates right-to-left shunting and worsens hypox-aemia.[3,10] Dopamine is commonly used, but at doses >10 μg/kg/ min it is not selective to systemic vasculature and may increase the PVR.[17] Dobutamine increases cardiac output and has limited effects on systemic pressure.[17] Norepinephrine is effective in improving oxygenation and improving systemic BP, and in newborn lambs was associated with improved postnatal adaptation and significantly decreased oxygen requirement.[17] Vasopressin and hydrocortisone may also be considered.[17]
Pulmonary vasodilators Inhaled NO
iNO is a potent and selective pulmonary vasodilator that leads to improved oxygenation and reduced need for ECMO by stimulating sGC activity to increase cGMP, a second messenger in the vasodilation pathway.[4,8,15] The use of iNO was FDA approved in 1999 for term and near-term infants with PPHN, especially when the OI is greater than 25.[3,6] The Neonatal Inhaled Nitric Oxide Study (NINOS) determined that the most effective starting dose of iNO is 20 ppm, and response should be seen within 30 - 60 minutes with an increase in PaO2 of 53 mmHg (8.6 kPa) or a decrease in OI of 15.[4,5,18,19] The use of iNO has significantly reduced the mortality of PPHN; however, ~40% of patients will not respond to iNO.[2,6,10] Failure to respond to 20 ppm is rarely followed by a response at a higher dosage.[8,18] The American Academy of Pediatrics (AAP) recommends the use of ECMO in non-responders.[20] Methaemoglobinaemia and increased nitrogen dioxide are known side-effects that occur more frequently at dosages greater than 20 ppm.[3,4] In patients with CDH, iNO can be attempted early with optimal ventilation and recruitment, but should be discontinued if no improvements are seen.[21]
iNO requires gradual weaning to avoid rebound PH (Table 6). The rebound phenomenon may appear even in patients who did not show any improvement on iNO initially.

In patients with PPHN refractory to iNO, ensure adequate lung recruitment, repeat echocardiogram and consider alternative treatments.[2]
Sildenafil
Sildenafil is a PDE5 inhibitor, which results in increased availability of cGMP, and subsequent selective reduction in PVR.[3-5,8,22] Increased PDE5 activity was documented in animal models with PPHN.[2] Enteral sildenafil, dose range 1 - 3 mg/kg every 6 hours, reduced mortality in resource-limited settings where iNO is not available and reduced rebound PH after the withdrawal of iNO.[4-6,13,22-24] A Cochrane review recommended this as a significant alternative for PPHN treatment when iNO is not available.[25]
In the treatment of PH secondary to BPD, sildenafil at doses of 0.5 mg/kg every 8 hours to 2 mg/kg every 6 hours is considered safe and effective, and contributes to improved survival at 12 months.[23,26]
Milrinone
Milrinone is a PDE3 inhibitor that leads to increased availability of cAMP, with resultant positive inotropic effects, peripheral vasodilatation, left ventricular afterload reduction and increased myocardial contractility.[3,5,8,23]There are case reports of improved oxygenation in cases of PPHN refractory to iNO,[3,23] but there are also reports of an increased incidence of intracranial hae-morrhages.[27] Safety and efficacy is unknown, and therefore it is recommended for use only within randomised controlled trials (RCTs).[28]
Other drug therapies
Other promising treatment modalities include PGI2, magnesium sulphate, bosentan, adenosine, steroids and apocynin, but there is insufficient evidence to recommend any for routine or combination use (Table 7).
Extracorporeal membrane oxygenation
Although ECMO is viewed as the ultimate rescue therapy in developed countries, it is not freely available in low-resource countries, therefore rendering its usefulness in developing countries questionable.[3,6]
Special categories
Special consideration should be given when treating a patient with PPHN and perinatal asphyxia, as the treatment of PPHN may affect cerebral blood flow.[3,32] Inhaled NO does not significantly alter neurodevelop-mental outcome.[3,32] The effects of moderate therapeutic hypothermia at 33.5oC for 72 hours does not result in a significant increase in PPHN.[3] There are case reports that preceding hypoxia requiring FiO2 >50% and/or iNO may be associated with exacerbation of PPHN with hypothermia and/or rewarming.[3] Fluid boluses are not recommended in these patients, unless there is hypovolaemia, as it may increase cerebral oedema.[3,32]
Outcome
The long-term neurological outcome is largely determined by the underlying condition. Neurodevelopmental impairment has been reported in up to 25% at 2 years of age and hearing impairment in 23%.[3,5]
At school age, there were 24% persistent respiratory problems, 60% abnormal chest X-rays, 6% sensorineural hearing loss, 9% IQ <90, and 7% IQ 70 - 84.[3] These infants require long-term multidisciplinary follow-up.
Conclusion
PPHN is an acute neonatal disorder with complex underlying pathophysiology, which has a high mortality rate despite several advances in the management thereof. Inhaled NO is a safe and effective clinical strategy in the majority of patients, but is not always available in resource-limited settings. Oral sildenafil is a relatively safe alternative option in these settings. Newer drugs need to be studied before any recommendations can be made for routine use.
References
1. Gersony WM, Duc GV, Sinclair JC. "PFC" syndrome (persistence of fetal circulation). Circulation 1969;40(suppl 1):3-87. [ Links ]
2. Distefano G, Sciacca P. Molecular physiopathogenetic mechanisms and development of new potential therapeutic strategies in persistent pulmonary hypertension of the newborn. Ital J Pediatr 2015;41(1):6. http://dx.doi.org/10.1186/s13052-015-0111-0 [ Links ]
3. Sharma V, Berkelhamer S, Lakshminrusimha S. Persistent pulmonary hypertension of the newborn. Matern Health Neonatol Perinatol 2015;1:14. http://dx.doi.org/10.1186/s40748-015-0015-4 [ Links ]
4. Puthiyachirakkal M, Mhanna MJ. Pathophysiology, management, and outcome of persistent pulmonary hypertension of the newborn: A clinical review. Front Pediatr 2013;1:23. http://dx.doi.org/10.3389/fped.2013.00023 [ Links ]
5. Bendapudi P, Rao GG, Greenough A. Diagnosis and management of persistent pulmonary hypertension of the newborn. Paediatr Respir Rev 2015;16(3):157-161. http://dx.doi.org/10.1016/j.prrv.2015.02.001 [ Links ]
6. Nair J, Lakshminrusimha S. Update on PPHN: Mechanisms and treatment. Semin Perinatol 2014;38(2):78-91. http://dx.doi.org/10.1053/j.semperi.2013.11.004 [ Links ]
7. Jain A, McNamara PJ. Persistent pulmonary hypertension of the newborn: Advances in diagnosis and treatment. Semin Fetal Neonatal Med 2015:20(4):262-271. http://dx.doi.org/10.1016/j.siny.2015.03.001 [ Links ]
8. Porta NFM, Steinhorn RH. Pulmonary vasodilator therapy in the NICU: Inhaled nitric oxide, sildenafil, and other pulmonary vasodilating agents. Clin Perinatol 2012;39(1):149-164. http://dx.doi.org/10.1016/j.clp.2011.12.006 [ Links ]
9. Aggarwal S, Natarajan G. Echocardiographic correlates of persistent pulmonary hypertension of the newborn. Early Hum Dev 2015;91(4):285-289. http://dx.doi.org/10.1016/j.earlhumdev.2015.02.008 [ Links ]
10. Bendapudi P, Barr S. Diagnosis and management of pulmonary hypertension of the newborn. Paediatr Child Health 2014;24(1):12-16. http://dx.doi.org/10.1016/j.paed.2013.05.021 [ Links ]
11. Hillman NH, Kallapur SG, Jobe AH. Physiology of transition from intrauterine to extrauterine life. Clin Perinatol 2012;39(4):769-783. http://dx.doi.org/10.1016/j.clp.2012.09.009 [ Links ]
12. Huybrechts KF, Bateman BT, Palmsten K, et al. Antidepressant use late in pregnancy and risk of persistent pulmonary hypertension of the newborn. JAMA 2015;313(21):2142-2151. http://dx.doi.org/10.1097/01.ogx.0000472158.66771.3e [ Links ]
13. Engelbrecht AL. Sildenafil in the management of neonates with PPHN: A rural regional hospital experience. S Afr J Child Health 2008;2(4):166-169. [ Links ]
14. El-Khuffash A, Herbozo C, Jain A, Lapointe A, McNamara PJ. Targeted neonatal echocardiography (TnECHO) service in a Canadian neonatal intensive care unit: A 4-year experience. J Perinatol 2013;33(9):687-690. http://dx.doi.org/10.1038/jp.2013.42 [ Links ]
15. Kinsella JP, Abman SH. Inhaled nitric oxide and high frequency oscillatory ventilation in persistent pulmonary hypertension of the newborn. Eur J Pediatr 1998;157(Suppl 1):S28-30. http://dx.doi.org/10.1378/chest.114.1_supplement.100s [ Links ]
16. Ullah A. Surfactant therapy in meconium aspiration syndrome (MAS). New Indian J OBGYN 2014;1(1):24-29. http://journal.barpetaogs.co.in/pdfs/1124.pdf [ Links ]
17. Tourneux P, Rakza T, Bouissou A, Krim G, Storme L. Pulmonary circulatory effects of norepinephrine in newborn infants with persistent pulmonary hypertension. J Pediatr 2008;153(3):345-349. http://dx.doi.org/10.1016/j.jpeds.2008.03.007 [ Links ]
18. The Neonatal Inhaled Nitric Oxide Study Group. Inhaled nitric oxide in full-term and nearly full-term infants with hypoxic respiratory failure. N Engl J Med 1997;336(9):597-604. http://dx.doi.org/10.1056/nejm199702273360901 [ Links ]
19. Finer NN, Barrington KJ. Nitric oxide for respiratory failure in infants born at or near term. Cochrane Database Syst Rev 2001;Issue 4:Art. no. CD000399. http://dx.doi.org/10.1002/14651858.cd000399 [ Links ]
20. Lakshminrusimha S, Keszler M. Persistent pulmonary hypertension of the newborn. Neoreviews 2015;16(12):e680-692. http://dx.doi.org/10.1542/neo.16-12-e680 [ Links ]
21. Pierro M, Thébaud B. Understanding and treating pulmonary hypertension in congenital diaphragmatic hernia. Semin Fetal Neonatal Med 2014;19(6):357-363. http://dx.doi.org/10.1016/j.siny.2014.09.008 [ Links ]
22. Michelakis ED, Tymchak W, Noga M, et al. Long-term treatment with oral sildenafil is safe and improves functional capacity and hemodynamics in patients with pulmonary arterial hypertension. Circulation 2003;108(17):2066-2069. http://dx.doi.org/10.1161/01.cir.0000099502.17776.c2 [ Links ]
23. Lakshminrusimha S, Mathew B, Leach CL. Pharmacologic strategies in neonatal pulmonary hypertension other than nitric oxide. Semin Perinatol 2016;40(3):160-173. http://dx.doi.org/10.1053/j.semperi.2015.12.004 [ Links ]
24. Baquero H, Soliz A, Neira F, Venegas ME, Sola A. Oral sildenafil in infants with persistent pulmonary hypertension of the newborn: A pilot randomised blinded study. Pediatrics 2006;117(4):1077-1083. http://dx.doi.org/10.1542/peds.2005-0523 [ Links ]
25. Shah PS, Ohlsson A. Sildenafil for pulmonary hypertension in neonates. In: Shah PS, ed. Reviews. Chichester, UK: Wiley-Blackwell, 2011. http://dx.doi.org/10.1002/14651858.cd005494.pub3 [ Links ]
26. Wardle AJ, Wardle R, Luyt K, Tulloh R. The utility of sildenafil in pulmonary hypertension: A focus on bronchopulmonary dysplasia. Arch Dis Child 2013;98(8):613-617. http://dx.doi.org/10.1136/archdischild-2012-303333 [ Links ]
27. James AT, Corcoran JD, McNamara PJ, Franklin O, El-Khuffash AF. The effect of milrinone on right and left ventricular function when used as a rescue therapy for term infants with pulmonary hypertension. Cardiol Young 2016;35(11):913-918. http://dx.doi.org/10.1017/s1047951114002698 [ Links ]
28. Bassler D, Kreutzer K, McNamara P, Kirpalani H. Milrinone for persistent pulmonary hypertension of the newborn. Cochrane Database Syst Rev 2010;(11):CD007802. http://dx.doi.org/10.1002/14651858.CD007802.pub2 [ Links ]
29. Kelly LK, Porta NFM, Goodman DM, Carroll CL, Steinhorn RH. Inhaled prostacyclin for term infants with persistent pulmonary hypertension refractory to inhaled nitric oxide. J Pediatr 2002;141(6):830-832. http://dx.doi.org/10.1067/mpd.2002.129849 [ Links ]
30. Ho JJ, Rasa G. Magnesium sulfate for persistent pulmonary hypertension of the newborn. Cochrane Database Syst Rev 2007;(3):CD005588. http://dx.doi.org/10.1002/14651858.CD005588.pub2 [ Links ]
31. Wedgwood S, Lakshminrusimha S, Farrow KN, et al. Apocynin improves oxygenation and increases eNOS in persistent pulmonary hypertension of the newborn. Am J Lung Cell Mol Physiol 2012;302(6):L616-626. http://dx.doi.org/10.1152/ajplung.00064.2011 [ Links ]
32. Lapointe A, Barrington KJ. Pulmonary hypertension and the asphyxiated newborn. J Pediatr 2011;158(2 Suppl):e19-24. http://dx.doi.org/10.1016/j.jpeds.2010.11.008 [ Links ]
 Correspondence:
Correspondence:
L G Lloyd
lgl@sun.ac.za
Accepted 20 July 2016














