Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
South African Journal of Child Health
On-line version ISSN 1999-7671
Print version ISSN 1994-3032
S. Afr. j. child health vol.9 n.2 Pretoria Jan./Apr. 2015
http://dx.doi.org/10.7196/SAJCH.828
CASE REPORT
Early renal surveillance: A necessity in a child with tuberous sclerosis complex
S K JohnI; R NallaII; V KumarIII; P L N G RaoIV; S PrabhuV; S P ThotanIII; B KhargaV
IMBBS, MS, FMAS; Department of Paediatric Surgery, Kasturba Medical College, Manipal University, Manipal, India
IIMBBS; Department of Surgery, Kasturba Medical College, Manipal University, Manipal, India
IIIMBBS, MS, MCh; Department of Paediatric Surgery, Kasturba Medical College, Manipal University, Manipal, India
IVMBBS, MS, MCh;Vice-Chancellor, Manipal International University, Nilai, Malaysia
VMBBS, DNB; Department of Paediatric Surgery, Kasturba Medical College, Manipal University, Manipal, India
ABSTRACT
Tuberous sclerosis complex (TSC) is an extremely variable genetic disorder that can affect virtually any organ in the body. Disease manifestations continue to develop over the lifetime of an affected individual. Many manifestations can be life threatening; appropriate surveillance and management are necessary to limit morbidity and mortality in this disease. We report a case of an 8-year-old girl with TSC and bilateral renal cell carcinoma, which is usually thought to be a complication diagnosed in adulthood. Our report emphasises the need for frequent surveillance and renal imaging in paediatric patients with TSC.
Tuberous sclerosis complex (TSC) is a genetic disorder that can affect virtually any organ in the body. Many manifestations can be life threatening. We report a case of an 8-year-old girl with TSC and bilateral renal cell carcinoma, which is usually thought to be a complication diagnosed in adulthood.
Case report
An 8-year-old girl presented with diffuse abdominal pain of 4 days' duration, associated with fever. The patient had been previously diagnosed as a case of tuberous sclerosis complex (TSC). Past history revealed infantile spasms managed with sodium valproate, and computed tomography (CT) of the brain showed subependymal nodules protruding into the lateral ventricles. The patient had undergone enucleation of the right eye for an astrocytic hamartoma. Initial evaluation had not revealed any renal lesions. However, no imaging studies had been done in the last 5 years.
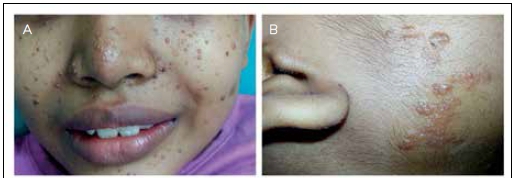
General examination revealed telangiectatic papules over the cheeks (Fig. 1 A) and chin (angiofibromas), flesh-coloured soft plaques with prominent follicular openings over the right cheek (Fig. 1 B) and lumbosacral area (shagreen patches), and ash-leaf-shaped macules over the limbs (Fig. 1 C) and abdomen. Dental pits were also noted. Abdominal examination revealed a large mass of 15 χ 10 cm involving the right hypochondrium and lumbar region.
Ultrasound (US) scan showed bilateral renal masses. CT scan of the abdomen revealed mass lesions in both kidneys (Fig. 1 D). The lesions showed no fat attenuation, with areas of necrosis and calcifications suggestive of bilateral renal cell carcinoma. The parents refused further evaluation and treatment.
Discussion
Tuberous sclerosis complex (TSC) is an extremely variable genetic disorder that can affect virtually any organ in the body. The most common findings are benign tumours in the skin, brain, kidneys, lungs and heart, which can lead to organ dysfunction. TSC is highly variable in clinical presentation and findings. Diagnosis is made based on the updated diagnostic criteria established at the Tuberous Sclerosis Complex Consensus Conference in 2012. Disease manifestations continue to develop over the lifetime of an affected individual. Accurate diagnosis is fundamental to implementation of appropriate medical surveillance and treatment, apart from being crucial for optimal quality of life of the affected. Many manifestations can be life threatening, and appropriate surveillance and management are necessary to limit morbidity and mortality.
Renal manifestations occur frequently in TSC, with varying severity. Estimated rates of involvement range from 48 to 80%.[1] The most common renal lesions are angiomyolipomata and renal cysts, the prevalence of both increasing with age. Angiomyolipoma is a benign renal neoplasm comprising vascular, smooth muscle and fat elements. The estimated incidence of renal cell carcinoma in TSC ranges from 2.2 to 4.2%[1,2] and occurs primarily in women.[3] The median age of diagnosis of renal cell carcinoma in TSC is reported as 28 years, 25 years earlier than the average age at diagnosis in the general population.[2,3] Although renal cell carcinoma has been reported in children with TSC as young as 6 months of age,[4] debate continues over whether TSC mutations increase susceptibility to renal cell carcinoma and whether TSC-related angiomyolipoma can progress to renal cell carcinoma.[1]
At the time of diagnosis, abdominal imaging should be obtained, regardless of age. Magnetic resonance imaging (MRI) is the preferred modality for evaluation of angiomyolipomata, because many can be fat-poor and hence missed in abdominal CT or US.[5] In CT, the only finding that can distinguish angiomyolipoma from renal cell carcinoma is intralesional fat. Fat-poor angiomyolipomata are not uncommon in patients with TSC. Biopsy is often discouraged, as it may cause highly vascular angiomyolipomata to haemorrhage or scatter malignant cells from a renal cell carcinoma.[1] But if there is doubt and the lesions are growing faster than 0.5 cm per year, a needle biopsy or an open biopsy may be considered.[5] Nephrectomy is to be undertaken with caution, since these patients are predisposed to developing additional masses in the remaining kidney and the operation has a high incidence of complications.[1] Prognosis varies, as these tumours frequently metastasise.[3]
This case report illustrates the need for early and frequent renal surveillance and renal imaging in paediatric patients with TSC.
Usually thought to be a complication diagnosed in adulthood, it is important to remember that although scarce, renal cell carcinoma may appear in a paediatric setting. The recommended surveillance protocol was poorly followed in our patient. The current recommendations (Table 1) suggest MRI of the abdomen at the time of diagnosis of TSC and every 1 - 3 years throughout the lifetime of the patient[5] to diagnose polycystic disease, renal cell carcinoma or other tumours, and to monitor changes in angiomyolipoma. Annual clinical assessments of renal function and hypertension are also recommended. Although our case report illustrates renal complications, we would like to emphasise the importance of total surveillance in these patients. Appropriate surveillance and early management are crucial to limit morbidity and mortality in this disease, and improve quality of life of those affected.
References
1. Rakowski SK, Winterkorn EB, Paul E, Steele DJ, Halpern EF, Thiele EA. Renal manifestations of tuberous sclerosis complex: Incidence, prognosis, and predictive factors. Kidney Int 2006;70(10):1777-1782. [http://dx.doi.org/10.1038/sj.ki.5001853] [ Links ]
2. Gil AT, Brett A, Cordinhã C, Gomes C. Bilateral renal cell carcinoma in a paediatric patient with tuberous sclerosis complex. BMJ Case Rep 2013. [http://dx.doi.org/10.1136/bcr-2013-010015] [ Links ]
3. Bjornsson J, Short MP, Kwiatkowski DJ, Henske EP. Tuberous sclerosis-associated renal cell carcinoma. Clinical, pathological, and genetic features. Am J Pathol 1996;149(4):1201-1208. [ Links ]
4. Breysem L, Nijs E, Proesmans W, Smet MH. Tuberous sclerosis with cystic renal disease and multifocal renal cell carcinoma in a baby girl. Pediatr Radiol 2002;32(9):677-680. [http://dx.doi.org/10.1007/s00247-002-0765-9] [ Links ]
5. Krueger DA, Northrup H, International Tuberous Sclerosis Complex Consensus Group. Tuberous sclerosis complex surveillance and management: Recommendations of the 2012 International Tuberous Sclerosis Complex Consensus Conference. Pediatr Neurol 2013;49(4):255-265. [http://dx.doi.org/10.1016/j.pediatrneurol.2013.08.002] [ Links ]
 Correspondence:
Correspondence:
S K John
drsijokjohn@yahoo.com