Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
South African Journal of Child Health
versão On-line ISSN 1999-7671
versão impressa ISSN 1994-3032
S. Afr. j. child health vol.8 no.4 Pretoria Nov. 2014
http://dx.doi.org/10.7196/SAJCH.702
RESEARCH
Current practice of air medical services in inter-facility transfers of paediatric patients in the Western Cape Province, South Africa
I L HowardI; T B WelzelII
IBTech (EMC), MPhil (EM); Division of Emergency Medicine, University of Cape Town, South Africa
IIMB ChB, Dip PEC (SA), H Dip Int Med (SA), EMDM, MMed Sc (Clin Epi); Division of Emergency Medicine, University of Cape Town, South Africa
ABSTRACT
OBJECTIVE: To describe the utilisation and safety of air medical services (AMS), when being used for inter-facility transfers of paediatric patients in the Western Cape Province, South Africa.
METHODS: A retrospective descriptive analysis was conducted for the time period January 2010 to December 2011. Data were recorded from the Cape Town base of the AMS provider for the Western Cape Provincial Department of Health Emergency Medical Services. Patient demographics, flight and transfer details, interventions performed and adverse events encountered were documented for all patients <13 years of age transferred by either helicopter or fixed-wing aircraft.
RESULTS: A total of 485 patients was analysed. More patients were transported by helicopter (n=263, 54%), with neonates making up the largest category for both modes of transfer. Respiratory (29%), neurological (18%), cardiac (14%) and gastrointestinal disorders (14%) made up the majority of non-traumatic reasons for transfer. Overall, transfers by helicopter were quicker (median mission time 03:00; interquartile range 02:32 - 03:25) compared with fixed-wing transfer (05:24; 04:22 - 06:20). The overall incidence of adverse technical events was relatively high (20%). Physiological adverse events ranged between 2% and 16% overall depending on the variable measured. The incidence of cardiac/respiratory arrest and endotracheal tube obstruction/dislocation was low (<2%). Emergency intubation and desaturation >10% from baseline were the most common critical adverse events encountered (6%).
CONCLUSION: Current utilisation of the AMS for paediatric inter-facility transfer is relatively high, at ~25%. Across both the helicopter and fixed-wing platforms, patients with a diverse range of pathologies of equally varying severities were transferred. The adverse events observed were found to be lower than those of trials examining non-specialised paediatric transfer, and were comparable to those seen with transfer by specialised paediatric retrieval teams. The AMS remain a safe and viable alternative to non-specialised paediatric transfer, and may serve as a potential alternative to specialised paediatric transfer in the Western Cape.
Paediatric inter-facility transfers have evolved significantly over the last decade, largely as a consequence of two major factors. Starting in the 1990s, a growing body of evidence has shown improved patient outcomes associated with the centralisation of paediatric intensive care resources, leading to the widespread adoption of this model of care.[1 , 2] Secondary to this has been a rise in the reported incidence of preventable adverse events associated with paediatric critical care transfer.[3-6] These outcomes consequently laid the foundation for the introduction of specialised paediatric retrieval teams, now in widespread use worldwide and considered by many to be the gold standard of paediatric transfer.
However, this approach is not without its detractors and remains contentious. Proponents assert that these teams offer the benefits of focused training and experience in terms of exposure to the specialised environment, equipment and patients.[5 , 6] Their use is supported by the reported reduction in inter-facility adverse events and reduction in mortality rates in the immediate post-admission period when compared with non-specialised transfer.[7-10] Opponents argue that this approach is resource intensive and requires substantial financial backing to be effectively introduced and maintained, limiting a more widespread adoption.[7, 8] Furthermore, following their introduction, these teams have failed to demonstrate a significant overall reduction in length of hospital stay, hospital resource use or survival to discharge.[7, 8]
Recent evidence has suggested that air medical services (AMS) are a viable alternative to paediatric road transfer, both within a specialised and non-specialised systems.[4, 5, 9] Worldwide, the AMS are becoming an increasingly prevalent and important aspect of the emergency medical services (EMS). Chief among the benefits of these services are the range of access and speed of transportation.[10] Within South Africa (SA), the Western Cape has a long tradition of AMS, beginning in 1966 with the introduction of the first air ambulance in the country, based in Cape Town. This service has now developed to operate a 12-hour/daytime helicopter for short to medium distance transfers (<200 km) and a 24-hour fixed-wing (FW) aircraft for long distance transfers (>200 km). The aircraft are primarily staffed by prehospital advanced life support (ALS) practitioners, supported by a variety of voluntary and seconded crew consisting of additional ALS and intermediate life support (ILS) practitioners, nursing sisters and doctors of varying specialties.
There is limited evidence to show that the AMS are already engaged in the transfer of critical paediatric patients within the Western Cape.[4,11] As such, these services remain a readily available alternative to the traditional road-based paediatric inter-facility transfer used in the province. The purpose of this study was to definitively evaluate the current use and safety of these services, specifically in the role of paediatric transfer within the province.
Methods
Study setting
The study was set in the Western Cape, SA. Data were collected from the records of the AMS provider for the provincial Department of Health, located at Cape Town International Airport.
Study design
All data were collected retrospectively for the period 1 January 2010 to 31 December 2011 from the service provider's patient report forms, captain's logs and flight folios. For each flight, patient demographic data, flight and transfer details, interventions performed and adverse events were recorded.
Demographic data
All patients <13 years of age, undergoing inter-facility transfer by the AMS provider and within the defined study period were included in the analysis. Patients were divided into four age-based categories: Neonate - newborn patients up to and including 28 days; infant - older than 28 days up to and including 364 days (<1 year); toddler - between the ages of 1 year up to and including 3 years 364 days (<4 years); child - between the ages of 4 years up to and including 12 years 364 days. Diagnostic categories were recorded from the patient report forms from the AMS provider, each of which was completed by the transferring clinicians. Patients were categorised as medical, surgical (non-traumatic) or trauma, and patient severity was assessed via the previously validated Rapid Emergency Medical Score (REMS).[12]
Flight and transfer data
Mode of transport was categorised as either helicopter or FW. The time intervals of each mission were divided and classified as follows: Access time - the time between dispatch and arrival at the patient's side; hospital time - the time taken to stabilise and transport the patient to the aircraft; transfer time - the time between lift-off and arrival at the receiving facility; handover time - the time taken for patient handover and transport back to the aircraft. Transferring medical personnel were classified according to their primary qualification, including registered nurse, ILS practitioner, ALS practitioner and doctor. ILS practitioners made up the middle tier of the three-tiered system currently employed by EMS within SA. Training is conducted over 3 months via a short course system in conjunction with a mandatory in-service training period. For ALS practitioners, there are two primary methods in which clinicians receive training and are registered at this level; either by the short course approach, varying between 9 months to a year, or by a formal university-based approach conducted over 3 years.
Interventions performed on each patient both en route and during stabilisation at the referring facility were documented and classified according to one of two previously validated scoring systems, namely the Neonatal Therapeutic Intervention Scoring System (NTISS) and the Therapeutic Intervention Scoring System-28 (TISS-28). [13, 14] Receiving and referring hospitals were classified based on the services offered, surrounding drainage area and bed capacity as follows: day clinic, district-level hospital, regional-level hospital and central/tertiary-level hospital.
Adverse events
All documentation was scrutinised for the presence of adverse events encountered both en route and during stabilisation at the referring facility. The events were classified into the following categories:
- Adverse technical event: Malfunction of monitoring and other medical equipment; absence of equipment generally available as per aircraft equipment checklist; no monitoring equipment in placeab initio; aircraft fault resulting in delay or cancellation of a flight; adverse weather resulting in delay or cancellation of a flight.
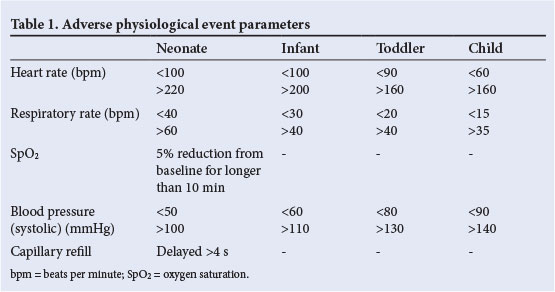
- Adverse physiological event: Respiratory rate (RR), heart rate (HR), blood pressure (BP), oxygen saturation (SpO2) and capillary refill time (CRT) for each patient were evaluated against predefined, age category specific criteria to determine whether abnormal or unexpected for the patient's age category or baseline (Table 1).
- Adverse critical event: This category indicated a critical decline in a patient's condition or otherwise requiring life-saving intervention. This included cardiac, cardiorespiratory or respiratory arrest during stabilisation or transfer, emergency intubation, endotracheal tube obstruction or dislocation, desaturation of 10% from baseline for longer than 10 min (in the absence of a technical malfunction or misplaced probe) and decrease in Glasgow Coma Scale of 3 or more points from baseline (where applicable).
Statistical considerations
Data were entered into a Microsoft Excel (2010) database (Microsoft Corporation, USA) and analysed using the same. A p-value of p<0.05 represented statistical significance and 95% confidence intervals (CIs) were used in hypothesis testing.
Results
Demographic data
The results of the demographic data collected are shown in Table 2. Paediatric inter-facility transfers represented approximately 25% of all flights over the study period. More patients were transported by helicopter overall (263 patients/263 flights, rate ratio = 1), however the greater cabin capacity of the FW allowed more patients to be carried for fewer flights (222 patients/206 flights; rate ratio = 1.2). General medical cases made up the majority of patients in the helicopter group (72%) whereas non-traumatic surgical cases made up the majority in the FW group (54%). Neonates comprised the single biggest group for each mode of transport as well as for each of the above-mentioned diagnostic categories. Respiratory (42%), neurological (16%) and gastrointestinal disorders (10%) accounted for the majority of non-traumatic pathologies affecting patients. Based on the REMS calculated for each patient, those transported by helicopter were found to be more critically ill or injured compared with the fixed-wing group (REMS>10; helicopter n=109 (41%); FW n=41 (18%); p<0.001). Using REMS as a measure of severity, there was a significant number of low acuity patients transferred (REMS<6; n=109 (22%)), more so for the FW group compared with the helicopter group.
Flight and mission data
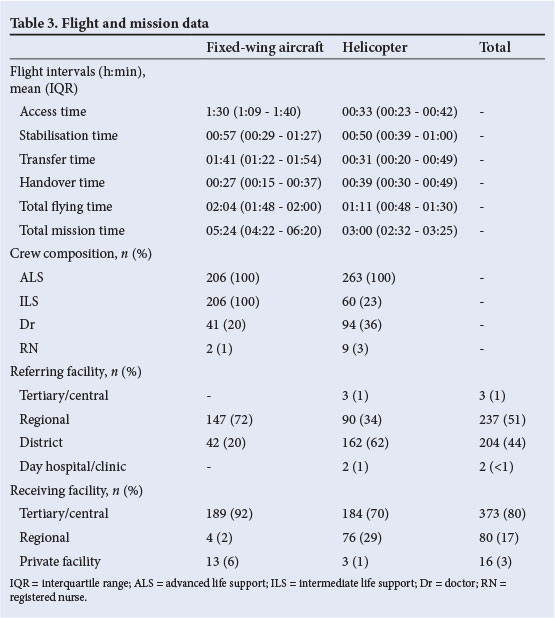
Flight and mission data collected are shown in Table 3. ALS practitioners were the most common medical crew and were present on all flights. The greater capacity of the FW allowed for an ILS practitioner to be present on all FW flights, with an additional medical crew member present on 21% of flights. Regional facilities mostly accounted for referral by FW (72%), whereas district facilities accounted for the majority of helicopter referrals (62%). When evaluating the more critical patient groups (REMS>10), more were referred from regional facilities (n=80 (54%)), compared with district facilities (n=58 (39%); odds ratio 1.83, 95% CI 1.15 - 2.91; p<0.0104). Similarly, patients requiring a higher level of intervention (NTISS/TISS-28 >10) were more often referred from regional-level facilities (n=139 (61%)), compared with district-level facilities (n=90 (39%); odds ratio 2.25, CI 1.56 - 3.22; p<0.001). Tertiary-level facilities made up the majority of receiving facilities in both samples (helicopter, 70%; FW, 92%); however, regional facilities were more commonly referred to for the helicopter group when compared with the FW.
Interventions
The results of the intervention data collected are shown in Table 4. Patients transported by helicopter required more interventions, as per intervention score, compared with FW (p=0.07). Similarly, medication administration was higher in the helicopter group. When comparing specific interventions, higher rates were observed for the helicopter group compared with FW. Of significance were the number of ventilated patients (helicopter n=132 (50%); FW n=54 (24%); p<0.001) and the number of patients requiring intubation by retrieval team (helicopter n=23 (9%); FW n=5 (2%);p=0.02). Using the intervention scores as a secondary measure of patient severity, a high incidence of low-acuity patients was again observed overall (NTISS/TISS-28 ≤10; n=111 (56%)).
Adverse events
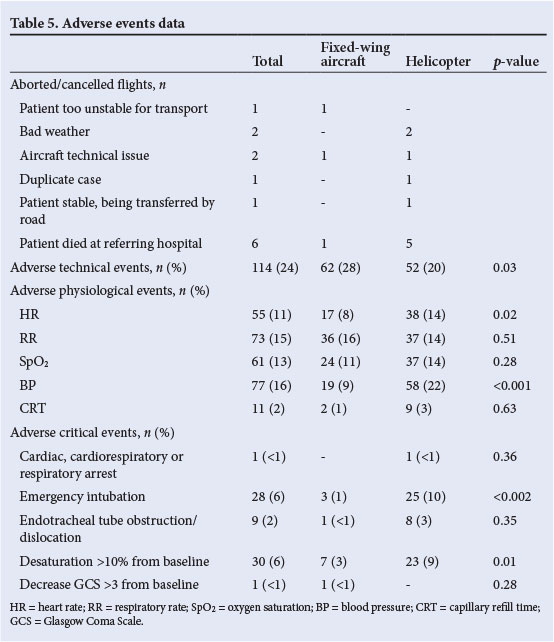
The results of the adverse events data collected are shown in Table 5. The incidence of aborted or cancelled flights was higher in the helicopter group (3%) compared with the FW group (1%); half of these were due to the patient dying prior to arrival of the aircraft. Overall, there were no in-flight deaths recorded. The number of adverse technical events was relatively high in this study, occurring in just under a quarter of all patients transferred. Adverse physiological events were observed in more helicopter patients (n=124 (47%)) compared with patients transported by FW (n=98 (44%); relative risk 1.07, CI 0.88 - 1.29). Similarly, more patients experienced a critical adverse event in the helicopter group (n=41 (16%)) compared with the FW group (n=11 (5%); relative risk 3.15, CI 1.66 - 5.97). For the more critical patients (REMS>10; n=147 (30%)), the prevalence of both adverse physiological events (n=101; 0.9 events/patient) and adverse critical events (n=39; 0.4 events/patient) was higher in the helicopter group.
Discussion
Current practice
Utilisation of the AMS for paediatric transfer has increased significantly compared with previous studies set in the Western Cape.[4, 11] While this shows an increasing trend in use, the high incidence of low-acuity patients observed in this study was unreported in these earlier reviews. Despite this, there is evidence to suggest that overutilisation of the AMS for paediatric transfer is relatively common internationally.[15] Accounting for this can be difficult, especially considering the AMS dispatch criteria currently employed in the Western Cape. Many of these are subjective in nature and generally include a final clause highlighting 'logistical need'. Given the limitation in rural resources, the aircraft are often dispatched when the availability of local ground-based resources are limited or unavailable, regardless of patient severity (A Oliphant, personal communication). This unique stance towards the AMS within the Western Cape can be traced back to an internal report commissioned by the provincial EMS.[16] It found that within the Western Cape, the equivalent service coverage offered by the AMS was approximate to fifty conventional road ambulances yet it operates at only 6% of the cost of these additional vehicles. Far from the conventional perception of the AMS as a luxury, when taking advantage of the unique services, they offer cost savings, increased access and coverage for rural areas, as well as increased safety and quality of care.[16]
From a referral point of view, regional and district-level facilities accounted for the majority of cases. Contrary to the general perception, there was a higher proportion of severely ill or injured patients transferred from regional centres, requiring more intervention when compared with similar patients from district facilities. Comparable results have not been reported in previous studies. Hatherill et al.[4] found an even spread of referrals between academic, metropolitan and rural hospitals in their study. However the majority of these patient transfers were road-based. In this study, the majority of transfers in the helicopter group were from district-level hospitals and could be similarly classified as rural. For the FW group, regional-level facilities made up the majority, and while not academic in nature, they cannot be classified as either rural or metropolitan.
Examination of the specific interventions and medications administered showed a focus on airway management and ventilation. This is consistent with the observation that respiratory disorders accounted for approximately one-third of all medical- and surgical-related transfers (p<0.001). This is similarly consistent with previously reported results from other reviews, including early studies examining paediatric transfer in the Western Cape. [4, 5, 9, 11]
Adverse events
The incidence of adverse technical events reported in this study appears to be high. Furthermore, the majority of these can be considered preventable, as they were largely as a result of missing or malfunctioning equipment. Despite this, the incidence in this review is lower than that reported in a previous one of non-specialised paediatric transfers in SA.[4] Adverse technical events reported in specialised paediatric transfer have varied from 0% to 16%, significantly lower than that reported in this review.[5, 6, 9] Despite this, none of the adverse technical incidents observed translated into a documented deterioration in patient status; a result consistent with that seen in the above-mentioned trials involving specialised transfer teams.
Physiological-related adverse events were strictly defined in this study. Few studies have reported details in this category of events. For non-specialised transfer, the previously reported incidence has varied from 13% to 23%.[3, 4] The incidence observed in this trial was found to be lower, varying from 2% (p=0.63) to 16% (p=0.51) depending on the variable measured. These results were more comparable to the incidence of such events observed with specialised transfer.[5, 6] Adverse critical events encompass the potential incidents considered the most severe or life-threatening. Early observations for this type of adverse event were reported to be as high as 52% for non-specialised transfer.[3] However, recent studies have reported more modest rates for similar critical events between 9% and 20%.[4, 5] The incidence observed in this trial was significantly lower than these previously reported results. The incidence of critical events in specialised transfer varied from 0 - 3%.[5, 6, 9] With the exception of emergency intubation, the incidence reported in this trial is consistent with these previously observed results during specialised transfer.[5, 6, 9]
Discussion of the adverse events encountered can be problematic, especially the adverse physiological and critical events. There are a number of potential confounding variables that make it difficult to separate whether or not the presence of an adverse event is solely owing to the effects of the flight or as a result of mismanagement by the referring facility or transferring crew, especially in the critical patient.
Conclusion
The AMS was found to be involved in a fair number of critical paediatric transfers in this review (25% of all missions), serving a diverse range of pathologies. However, a high incidence of low patient acuity was apparent across both platforms, more so for patients transferred by FW. Despite this, there is some evidence that this method of utilisation may be beneficial in the setting of the Western Cape.
The adverse events encountered in this study were found to be lower than those reported in studies examining non-specialised paediatric transfer. With the exception of adverse technical incidents, the incidence of adverse events observed was comparable to those seen with transfer by specialised paediatric retrieval teams. Of great concern is that the adverse technical events were for the greater part preventable. Based on the results observed, there is evidence to suggest the utilisation of the AMS to be a safe and viable alternative to traditional road-based, non-specialised paediatric transfer within the Western Cape. It would be beneficial to extend and include more recorded parameters into the databases for this and other AMS in the country to increase the power of the results when analysing the effectiveness of the services.
References
1. Pearson G, Shann F, Barry P, et al. Should paediatric intensive care be centralised? Trent versus Victoria. Lancet 1997;349(9060):1213-1217. [http://dx.doi.org/10.1016/S0140-6736(96)12396-5] [ Links ]
2. Shann F, Pearson G. Paediatric intensive care - specialisation reduces mortality. Anaesthesia 1999;54(8):809-810. [ Links ]
3. Barry PW, Ralston C. Adverse events occurring during interhospital transfer of the critically ill. Arch Dis Child 1994;71(1):8-11. [http://dx.doi.org/10.1136/adc.71.1.8] [ Links ]
4. Orr RA, Felmet KA, Han Y, et al. Pediatric specialized transport teams are associated with improved outcomes. Pediatrics 2009;124(1):40-48. [http://dx.doi.org/10.1542/peds.2008-0515] [ Links ]
5. Britto J, Nadel S, Maconochie I, Levin M, Habibi P. Morbidity and severity of illness during interhospital transfer: Impact of a specialised paediatric retrieval team. BMJ 1995;311(7009):836-839. [ Links ]
6. Sajjanhar T, Tibby SM, Hatherill M, Marsh MJ, Murdoch IA. A paediatric retrieval service: Its effect on clinical efficacy, activity and resource use in a tertiary paediatric intensive care unit. Clin Intensive Care 1997;8(4):178-181. [ Links ]
7. Lim MT, Ratnavel N. A prospective review of adverse events during interhospital transfers of neonates by a dedicated neonatal transfer service. Pediatr Crit Care Med 2008;9(3):289-293. [http://dx.doi.org/10.1097/PCC.0b013e318172dbfd] [ Links ]
8. Holt J, Fagerli I. Air transport of the sick newborn infant: Audit from a sparsely populated county in Norway. Acta Pediatr 1999;88(1):66-71. [ Links ]
9. Brown BS, Pogue KA, Williams E, et al. Helicopter EMS transport outcomes literature: Annotated review of articles published 2007-2011. Emerg Med Int 2012;2012:876703. [http://dx.doi.org/10.1155/2012/876703] [ Links ]
10. Pieper CH, Smith J, Kirsten GF, Malan P. The transport of neonates to an intensive care unit. S Afr Med J 1994;84(11 Suppl):801-803. [ Links ]
11. Olsson T, Lind L. Comparison of the Rapid Emergency Medicine Score and APACHE II in nonsurgical emergency department patients. Acad Emerg Med 2003;10(10):1040-1048. [ Links ]
12. Gray JE, Richardson DK, McCormick MC, Workman-Daniels K, Goldmann DA. Neonatal Therapeutic Intervention Scoring System: A therapy-based severity-of-illness index. Pediatrics 1992;90(4):561-567. [ Links ]
13. Miranda DR, de Rijk A, Schaufeli W. Simplified Therapeutic Intervention Scoring System: The TISS-28 items - Results from a multicenter study. Crit Care Med 1996;24(1):64-73. [ Links ]
14. Diller E, Vernon D, Dean JM, Suruda A. The epidemiology of pediatric air medical transports in Utah. Prehosp Emerg Care 1999;3(3):217-224. [ Links ]
15. Daviaud E. Are air emergency services a luxury for cash strapped public sector? Air Mercy Service, 2005. (Internal report. [ Links ])
 Correspondence:
Correspondence:
I L Howard
ianhoward@outlook.com














