Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
South African Journal of Child Health
On-line version ISSN 1999-7671
Print version ISSN 1994-3032
S. Afr. j. child health vol.8 n.3 Pretoria Sep. 2014
RESEARCH
SKINNY - Skin thickness and needles in the young
K MarranI; D SegalII
IMB BCh, MRCP, Cert Paed Endo; Department of Paediatrics, Charlotte Maxeke Johannesburg Academic Hospital, South Africa
IIMB BCh, FAAP, FACE; Donald Gordon Medical Centre, University of the Witwatersrand, Johannesburg, South Africa
ABSTRACT
BACKGROUND: Intensive diabetes management requires the use of multiple daily injections. Inappropriate insulin injection technique, inadvertent intramuscular (IM) injections, needle phobia and insulin omission negatively affect glucose control.
OBJECTIVES: To document skin and skin plus subcutaneous skin thickness using high resolution ultrasound (US) in a group of children and adolescents with type 1 diabetes. In addition, injection technique, needle re-use and injection site analysis was performed.
METHODS: Commonly recommended injection sites were examined using high-resolution US. Patient characteristics such as age, body mass index, frequency of injections and favoured sites were analysed.
RESULTS: A total of 40 paediatric and adolescent children aged 4 years 3 months to 18 years were examined. The maximum skin thickness at any site was 2.93 mm. A high rate of IM injection was predicted with the standard 8 mm needle and was reduced but not eliminated with the use of the shortest available 4 mm needle. As the subcutaneous skin thickness increased across injection sites in the following order: arm, thigh, abdomen and buttocks, the risk of IM injection declined.
CONCLUSION: Choice of needle length, injection site and injection technique are important considerations in diabetes management in the paediatric population and are likely to affect quality of glycaemic control. Shorter needles are more acceptable and reduce the risk of IM injections.
The primary goal of diabetes mellitus management is the attainment of near normoglycaemia. The importance of glycaemic control in reducing or delaying microvascular, renal, neuropathic and other complications of diabetes is well established. The Diabetes Control and Complications Study demonstrated that good metabolic control, resulting from intensive insulin therapy, reduces the risk of progression or development of retinopathy, nephropathy and neuropathy in type I diabetes.[1] Intensive insulin therapy requires multiple daily injections. One of the major obstacles to achieving tight control is the omission of insulin. Fear of injections and pain reduce the frequency of injections, and intramuscular (IM) injections increase the risk of low blood sugar reactions that can lead to inappropriate insulin dose reductions or avoidance behaviours, which lead to higher overall blood glucose targets. In addition, inappropriate insulin injection technique has been shown to negatively affect glucose control.[2-4]
In recent decades, the technique of insulin injection has begun to be approached in a scientific fashion. Research on the subject has shown that correct performance of injections is as important to good glucose control as the type and dose of insulin delivered.[5,6] Ideally, injected insulin should be deposited into the subcutaneous (SC) fatty tissue, which has a slow and predictable absorption rate. The primary determinants of injection depth are the needle length, the use of a 'pinched' skin fold and the anatomical injection site. Injecting too shallow into the dermis causes pain, and too deep into the muscle results in bruising; both result in insulin delivery into compartments that have highly variable blood flows, which significantly affects insulin pharmacokinetics and pharmacodynamics.[7,8]
A number of other studies have confirmed the frequency of inadvertent IM injections and have highlighted their deleterious effects on overall glucose control.[2-4,9] Muscle blood flow is greater than that through SC tissue and changes up to seven-fold with exercise. IM injections therefore lead to more rapid insulin absorption and greater risk of hypoglycaemia, which is compounded by exercise.
Concern over the frequency of IM injections resulted in the recommendation to pinch up a skin fold into which the needle should be inserted. Nevertheless, even a pinch-up may not protect children from IM injections when using 12.7 mm and 8 mm needles.[10] These reports suggest that needles even shorter than 8 mm may be needed in children, and needle lengths of 6 mm, 5 mm and 4 mm are now available.
A study comparing a 5 mm needle without a pinch-up to an 8 mm needle with a pinch-up in children found no significant changes in glycated haemoglobin (HbA1c) levels (p=0.59). The pain of injection (standard deviation (SD)) was rated by the children to be significantly lower with the 5 mm needle (1.2 (1.1) v. 4.2 (2.6) on a ten-point scale; p=0.001) and there were fewer hypoglycaemic events during the period in which the 5 mm needle was used (p=0.05). There were no differences in leakage or bleeding at the injection site. The children clearly preferred the 5 mm over the 8 mm on subsequent questioning. The investigators concluded that 'the improvement in hypoglycaemic events could have been a result of fewer IM injections, and the pain and preference advantages of the 5 mm needle may have positive effects on wellbeing and compliance in paediatric populations.'[11]
Newer 4 mm needles are now available. A recent publication on skin and SC thickness in children and adolescents confirmed the reduction in risk of IM injection with 4 mm needles, and that the younger the child and lower the BMI, the greater the risk of IM injection with longer needles.[12]
Objective
Our objective was to document the skin-to-muscle distance in various routinely recommended injection sites across a range of ages in our South African (SA) population. This would enable us to compile evidence-based guidelines for injection techniques and to educate patients and caregivers on age- and site-appropriate injection techniques that would hopefully translate into improved clinical outcomes, patient satisfaction and safety.
Methods
Subjects
The study enrolled 40 children and adolescents with type 1 diabetes, aged 4 years 3 months to 18 years, as they presented consecutively to the outpatient diabetes clinic at Charlotte Maxeke Johannesburg Academic Hospital (CMJAH). There were 17 males and 23 females. All subjects fulfilled the inclusion criteria: having type 1 diabetes and being on insulin for >1 year. None were excluded due to pathology that could have affected the distribution of SC fat, such as lipodystrophy syndromes. Patients were divided into three groups based on age: 2 - 6, 7 - 13 and 14 - 18 years. These categories were chosen to allow comparison with other paediatric studies on this topic and also to factor in pre- and postpubertal physiological and hormonal differences.[12]
The study was approved by the Human Research Ethics Committee of the University of the Witwatersrand and was conducted between October and December 2012.
Measurements
The following demographic data were obtained on each subject: date of birth, sex, height, weight, date of diagnosis of diabetes, number of injections per day, use or not of a lifted skin fold (pinch-up) for injecting, needle length, perpendicular or angled approach to injection, most common site of injection and whether or not they practised site rotation. The body mass index (BMI) was calculated from height and weight values.
The thickness of the skin and SC tissue was then measured using ultrasound (US) at all injection sites by a single observer. All sites were included whether or not the child injected there. The measurement location was standardised using skin surface or palpable landmarks in order to reduce intersubject measurement variability. The following four sites were measured: arm (5 cm directly inferior to the acromium process in children <13 years, 10 cm in older children); thigh (5 cm directly inferior to the greater trochanter in children <13 years, 10 cm in older children); abdomen (5 cm directly lateral to the umbilicus in children <13 years, 10 cm in older children); buttock (the upper outer quadrant, 5 cm below the iliac crest in children <13 years, and 10 cm in older children). No US measurements were made over areas of visible or palpable lipohypertrophy.
Because previous studies have not shown a correlation between HbA1c and skin, or skin and SC thickness,[12] we decided not to measure the level of blood glucose control in our study cohort. Previous studies have also shown a high degree of correlation between the measured skin thickness between the left and right sides of the body, and for this reason we chose to measure a single side only.
Materials
Ultrasound
The MyLabTouch portable US unit with a 33 mm, 13.6 MHz linear transducer/probe ideal for imaging superficial structures (ESAOTE Biomedica Deutschland GmbH, Germany) was used. After ultrasonic gel was applied, the probe was placed perpendicularly to the predetermined area of the body site without a spacer. During the scanning process, the probe was moved within the marked area to obtain clear and focused images. After identification of the landmarks, the images were frozen and measured in triplicate. All images were taken by a single operator.
Statistics
Our sample size allowed for description of site dimensions with 95% confidence margins of ±0.09 mm for skin and ±0.72 mm for SC measurements. Mean, median, SD, minimum, maximum and 95% confidence intervals (CIs) were measured for the entire population, for each paediatric subgroup, and for other grouping parameters such as gender and BMI. Comparisons of subgroups were performed using χ2, analysis of variance, and log linear models, and the threshold for statistical significance was set at α=0.05.
Results
Subject demographics
A total of 17 male and 23 female children ranging from 4 years 3 months to 18 years was enrolled. Patient characteristics are summarised in Table 1. The majority (n=35 (88%)) were using 8 mm needles - standard government issue at CMJAH - and 12% were using 5 mm needles that had been specially bought in as they were not on tender.
Only two subjects (5%) were not using a pinched-up skinfold for injections as was taught in the clinic. Of the subjects, 80% were using a perpendicular and 20% an angled injection approach. Six subjects (15%) were on 2 injections per day, 27 (67.5%) on 3 injections per day and the remaining 7 (17.5%) were on 4 injections per day. The mean number of daily injections in our study cohort was 3 (range 2 - 4). Policy in the state hospital pharmacy dictated that 10 needles were dispensed per patient per month; the average number of injections per needle was 10 (range 3 - 30). Of the 40 patients, 34 (85%) practised site rotation, and the most common injection sites in order of frequency were the abdomen (55%), thigh (25%), buttock (12.5%) and arm (7.5%).
Skin and SC thickness
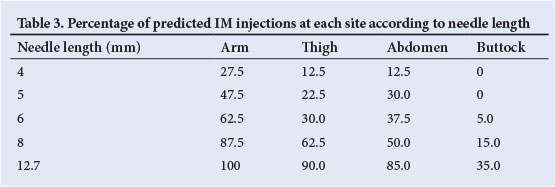
Mean values for the thickness of the skin, and skin plus SC tissue at each injection site are presented in Table 2. Similar to other studies, our study also found that the mean skin thickness increased across sites, from the lowest value in the arm (1.34 mm, range 0.89 - 2.08 mm) to the greatest thickness in the buttocks (1.79 mm, range 1.11 - 2.93 mm), and the thigh thinner than the abdomen.[12] The maximum skin thickness measured at any site was 2.93 mm. The mean values for the thickness of the skin plus SC tissue, i.e. surface-to-muscle distance, are presented graphed against BMI in Figs. 1 - 4 with a 4 mm threshold highlighted, corresponding to the shortest needle currently available. The same general trend as for skin thickness was found in the skin plus SC thickness. The estimated risk of IM injections at the different sites, assuming a non-pinched-up skin fold and a perpendicular injection angle, using different needle lengths currently available is represented in Table 3. The risk of IM injection predictably increases as the needle length increases. The risk also increased across sites with the greatest risk in the arm, followed by the thigh and abdomen. Injecting into the buttocks carries the lowest risk for IM injection.
Discussion
The results of our study are in alignment with others published on similar age groups.[12] and provide additional data on skin and SC thickness in an SA population of children and adolescents with type 1 diabetes. As in other studies, the skin thickness increased with increasing age and increased progressively across common injection sites from the arm, to the thigh, abdomen and buttock. The skin thickness did not exceed 3 mm at any site, across all ages and BMIs studied. Of all currently available needle lengths, the shortest (4 mm) would comfortably enter the SC space while avoiding an intradermal injection.
The greatest risk of pain, bruising and hypoglycaemia in children and adolescents comes from IM injections. This study found an unacceptably high predicted risk of IM injections in all ages at commonly used and recommended injection sites with the arm, thigh and abdomen presenting the greatest risk when injecting with needle lengths >4 mm using a perpendicular injection technique, without a pinch-up.
The risk of IM injections in the arm is extremely high because it has the smallest distance from skin to muscle and the option of a pinched skin fold is technically difficult for a child administering his/her own injections; this even applies to the use of 4 mm needles. The site with the lowest possibility of IM injection, the buttock, also happened to be the least favoured injection site of choice for self-injection. The abdomen and thigh were the preferred injection sites; even at these sites, using a 4 mm needle, the risk of IM injection was 12.5%, i.e. 1 in 8 injections.
In paediatric studies, the use of shorter, finer needles achieved the same level of glycaemic control but with less pain, no difference in reported insulin leakage and greater patient satisfaction[13, 14] Our data and those of others support the use of 4 mm needles as the safest available option to minimise this risk of IM injection. Other clinically proven options for reducing IM injections apart from using shorter needles are to use an angled injection approach or a skin fold pinch-up. Hoffman et al.[15] showed that an angled injection would more consistently deliver the insulin into the SC space with longer needle lengths. There are, however, technical difficulties in younger children with conceptualising and actualising a 45° injection angle. Use of a 4 mm needle with an angled approach may be limited by the foreshortening that could occur due to the needle hub abutting the skin, resulting in shallower intradermal injections. Therefore, injections using 4 mm needles should be given perpendicular to the skin. A skin fold pinch-up does not always alleviate the risk of an IM injection, especially in younger thinner children and when using longer needles.[10] It is important to be consistent in injection recommendations so as to reduce confusion.[16]
Conclusion
Choice of needle length and injection technique are important considerations in the paediatric population. Other considerations include age, injection site and self- v. carer-administered injections. This study highlights the need for a uniform set of guidelines regarding insulin injection techniques. As far as possible, shorter needles should be used in younger children, and children and adolescents with lower BMIs. A pinched-up skin fold and possible angled injection approach should be used if the risk of IM injection is rated to be high based upon the available needle length and planned injection site. Shorter needles should be made more available and accessible to children with diabetes.
References
1. The Diabetes Control and Complications Trial (DCCT) Research Group. The effect of intensive treatment of diabetes on the development and progression of long-term complications in insulin-dependent diabetes mellitus. N Engl J Med 1993;329(14):977-86. [http://dx.doi.org/10.1056/NEJM199309303291401] [ Links ]
2. Vaag A, Pedersen KD, Lauritzen M, Hilderbrandt P, Beck-Nielsen H. Intramuscular versus subcutaneous injection of unmodified insulin: Consequences for blood glucose control in patients with type 1 diabetes mellitus. Diabet Med 1990;7(4):335-342. [http://dx.doi.org/10.1111/j.1464-5491.1990.tb01401.x] [ Links ]
3. Matsumura M, Monden Y, Nakatani T, et al. Improvement of glycaemic control by reeducation in insulin injection technique. Diabetes 2007;56:Abstract 0157-OR. [ Links ]
4. Thow JC, Home PD. Insulin injection technique: depth of injection is important. Br Med J 1990;301:3-4. [http://dx.doi.org/10.1136/bmj.301.6742.3] [ Links ]
5. Thow JC, Johnson AB, Fulcher G, Home PD. Different absorption of isophane (NPH) insulin from subcutaneous and intramuscular sites suggests a need to reassess recommended insulin injection technique. Diabet Med 1990;7(7):600-602. [http://dx.doi.org/10.1111/j.1464-5491.1990.tb01456.x] [ Links ]
6. Frid A, Gunnarsson R, Guntner P, Linde B. Effects of accidental intramuscular injection on insulin absorption in IDDM. Diabetes Care 1988;11(1):41-45. [http://dx.doi.org/10.2337/diacare.11.1.41] [ Links ]
7. Owens DR, Coates PA, Luzio SD, Tinbergen JP, Kurzhals R. Pharmacokinetics of 125I-labeled insulin glargine (HOE 901) in healthy men: Comparison with NPH insulin and the influence of different subcutaneous injection sites. Diabetes Care 2000;23(6):813-819. [http://dx.doi.org/10.2337/diacare.23.6.813] [ Links ]
8. Hildebrandt P, Sestoft L, Nielsen SL. The absorption of subcutaneously injected short-acting soluble insulin: Influence of injection technique and concentration. Diabetes Care 1983;6(5):459-462. [http://dx.doi.org/10.2337/diacare.6.5.459] [ Links ]
9. Lasagni C, Seidenari S. Echographic assessment of age-dependant variations of skin thickness. Skin Res Technol 1995;1(2):81-85. [http://dx.doi.org/10.1111/j.1600-0846.1995.tb00022.x] [ Links ]
10. Polak M, Beregszaszi M, Belarbi N, et al. Subcutaneous or intra-muscular injections of insulin in children: Are we injecting where we think we are? Diabetes Care 1996;19(12):1434-1436. [http://dx.doi.org/10.2337/diacare.19.12.1434] [ Links ]
11. Tubiana-Rufi N, Belarbi N, Du Pasquier-Fediaevsky L, et al. Short needles (8 mm) reduce the risk of intramuscular injections in children with type 1 diabetes. Diabetes Care 1999;22(10):1621-1625. [http://dx.doi.org/10.2337/diacare.22.10.1621] [ Links ]
12. Lo Presti D, Ingegnosic C, Strauss K. Skin and subcutaneous thickness at injecting sites in children with diabetes: Ultrasound findings and recommendations for giving injection. Pediatr Diabetes 2012;13(7):525-533. [http://dx.doi.org/10.1111/j.1399-5448.2012.00865.x] [ Links ]
13. Birkebaek NH, Solvig J, Hansen B, Jorgensen C, Smedegaard J, Christiansen JS. A 4 mm needle reduces the risk of intramuscular injections without increasing backflow to skin surface in lean diabetic children and adults. Diabetes Care 2008;31(9):e65. [http://dx.doi.org/10.2337/dc08-0977] [ Links ]
14. Strauss K, Hannet I, McGonigle J, et al. Ultra-short (5 mm) insulin needles: trial results and clinical recommendations. Pract Diab Int 1999;16(7):22-25. [http://dx.doi.org/10.1002/pdi.1960160711] [ Links ]
15. Hofman PL, Lawton SA, Peart JM, et al. An angled insertion technique using 6 mm needles markedly reduces the risk of intramuscular injections in children and adolescents. Diabet Med 2007;24(12):1400-1405. [http://dx.doi.org/10.1002/pdi.276] [ Links ]
16. Strauss K, De Gols H, Letondeur C, Matyjaszczyk M, Frid A. The Second Injection Technique Event (SITE), May 2000, Barcelona Spain. Pract Diab Int 2002;19(1):17-21. [http://dx.doi.org/10.1002/pdi.276] [ Links ]
 Correspondence:
Correspondence:
D Segal
(david@endo.co.za)














