Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
South African Journal of Child Health
versão On-line ISSN 1999-7671
versão impressa ISSN 1994-3032
S. Afr. j. child health vol.7 no.4 Pretoria Abr. 2013
RESEARCH
Outcomes in malnourished children at a tertiary hospital in Swaziland after implementation of the World Health Organization treatment guidelines
O BenyeraI; F L M HyeraII
IMB ChB, Dip HIV Man, MSc (Clinical Epidemiology); School of Health Systems and Public Health, University of Pretoria, South Africa, and Department of Paediatrics, Mbabane Government Hospital, Mbabane, Swaziland
IIMD, PGDip (ObGyn), DTM&H, DOM&H, MSc (Community Health), MMed (Community Health) School of Health Systems and Public Health, University of Pretoria, South Africa
ABSTRACT
BACKGROUND: Swaziland adopted the World Health Organization (WHO) guidelines for the inpatient treatment of severely malnourished children in 2007, with the aim of reducing high case fatality rates for childhood malnutrition. However, no follow-up studies have been conducted to determine the reduction in these rates after implementation of the guidelines.
OBJECTIVES: To determine the case fatality rate for childhood malnutrition after implementation of the WHO treatment guidelines.
METHODS: A retrospective observational study was undertaken. Demographic, anthropometric and clinical characteristics and outcomes for all children aged under 5 years admitted for inpatient treatment of malnutrition between January 2010 and December 2011 were recorded and analysed.
RESULTS: Of the 227 children who met the study inclusion criteria, 179 (64.6%) were severely malnourished and 98 (35.4%) had moderate malnutrition; 111 children died during admission, giving an overall case fatality rate of 40.1%. Mortality was significantly higher among severely malnourished children than among those with moderate malnutrition (46.9% v. 27.6%) (odds ratio (OR) 3.0, 95% confidence interval (CI) 1.7 - 5.3). Co-morbid pneumonia and gastroenteritis were significant predictors of mortality (OR 2.0, 95% CI 1.2 - 3.4 and OR 1.9, 95% CI 1.1 - 3.2, respectively).
CONCLUSION: Case fatality rates for childhood malnutrition remain high despite adoption of the WHO treatment guidelines. There is a need for periodic clinical audits and mortality review meetings to reduce deaths from childhood malnutrition so as to meet the WHO mortality target of less than 5% and improve child survival.
Worldwide an estimated 8.1 million children die each year before they reach their 5th birthday, and 99% of these deaths are in the developing world.[1-2] Malnutrition is associated with more than 50% of these deaths,[3-4] and is therefore an important risk factor for the burden of disease in developing countries.[5]
Hospital management of severe malnutrition is an important component of a comprehensive approach to the problem of undernutrition.[6] A review of case management worldwide has revealed a median case fatality rate of approximately 25%, with rates in some hospitals as high as 50%.[6-8] Many of these deaths are avoidable, and are due to outdated procedures and protocols and lack of familiarity with modern management practices.[6]
The World Health Organization (WHO) has developed consensus treatment guidelines to help improve the quality of hospital care for malnourished children, and suggests that if these are strictly adhered to mortality should be less than 5%.[9-10] Case fatality rates over 20% are considered unacceptable, 11 - 20% is poor, 5 - 10% is moderate, 1 - 4% is good, and <1% is excellent.[11] Studies after implementation of the guidelines have shown improvements in death rates.[7-9]
The WHO conducted training on the inpatient treatment of severely malnourished children in Swaziland in 2003, in response to a rising incidence of severe malnutrition. Case fatality rates at Mbabane Government Hospital were in excess of 50%,[12] and no specific guidelines on the treatment of severe malnutrition were in use. However, it was not until 2007 that the WHO guidelines were fully adopted under a programme called the Integrated Management of Acute Malnutrition (IMAM). The present study was conducted to determine the case fatality rate after adoption of the WHO-recommended guidelines and to evaluate the level of adherence to the guidelines at Mbabane Government Hospital.
Objectives
The objective of the study was to determine the case fatality rate for childhood malnutrition after implementation of the WHO guidelines for the inpatient treatment of severely malnourished children.
Methods
Setting and participants
A retrospective observational study was conducted in the paediatric unit at Mbabane Government Hospital. It is the national referral hospital for Swaziland and also serves as a primary care facility for Mbabane and the surrounding areas.
Paediatric inpatient admission procedure
All children admitted to the unit are screened for malnutrition regardless of the initial presenting complaint or diagnosis. A structured admission form captures their weight, height and weight for height and the presence of nutritional oedema. The anthropometric measurements are then compared with WHO growth standards and a diagnosis of malnutrition is made according to the WHO definition.[11] All children found to be moderately or severely malnourished are then managed according to the WHO guidelines, regardless of the initial presenting diagnosis.
Inclusion criteria
All children aged under 5 years admitted with malnutrition (according to the WHO definition)[11] and managed using the WHO guidelines between January 2010 and December 2011, regardless of other primary diagnoses, were included.
Exclusion criteria
Children with incomplete anthropometric data were excluded from the study. Children whose parents requested discharge against medical advice were also excluded because of non-compliance with the guidelines.
Data collection
For all children who met the inclusion/exclusion criteria, demographic, anthropometric and clinical findings, co-morbid conditions and the outcome of admission were abstracted from the notes, using a structured form. Data were then entered into a Microsoft Office Access database.
Permission to access patient records was obtained from the Senior Medical Officer, Mbabane Government Hospital. The study protocol was approved by the Main Ethics Committee of the Faculty of Health Sciences, University of Pretoria, and the Scientific and Research Ethics Committee of Swaziland.
Analysis
Stata release 11 (Stata LP, Texas, USA) was used for statistical analysis. Data were described using standard statistics for continuous and categorical variables. Categorical variables were compared using the chi-square test and medians using the Wilcoxon rank sum test. Multivariate logistic regression analysis was used to identify risk factors for death. Significant variables in the univariate analyses (p<0.30) were included in the multivariate model. The final model was obtained through the backward-stepwise procedure. The Pearson chi-square goodness-of-fit test was used to determine the fit of the model. Odds ratios (ORs) and their 95% confidence intervals (CIs) are specified where applicable. A p-value of <0.05 was considered statistically significant.
Results
A total of 1 995 children were admitted to the paediatric ward during the study period. Of these, 337 (16.9%) were children aged under 5 years with malnutrition. Twenty-three children were excluded from the study because their parents requested discharge against medical advice. A further 37 children were excluded because their case notes did not contain sufficient information for them to be classified accurately in the study.
Two hundred and seventy-seven children therefore met the inclusion criteria. Of these, 119 (43.0%) were females. The median age of admission was 12 months (interquartile range (IQR) 7 - 17 months) (Table 1).
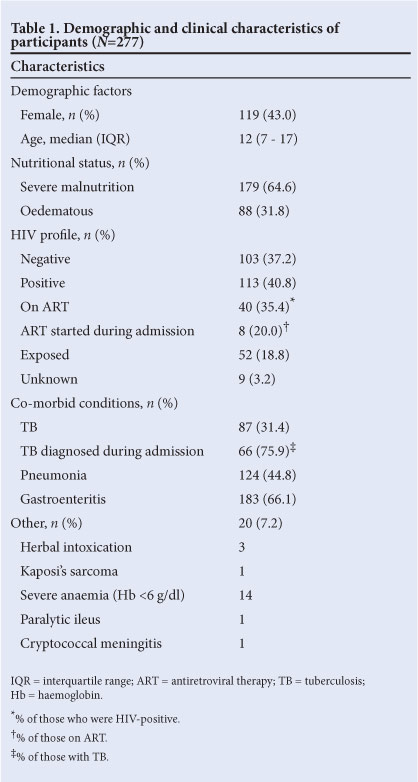
Ninety-eight children (35.4%) had moderate malnutrition and 179 (64.6%) had severe acute malnutrition (SAM). Of the 179 who had SAM, 91 (50.8%) were severely wasted and 88 (49.2%) had oedematous SAM.
One hundred and three children (37.2%) were HIV-negative, 113 (40.8%) were HIV-positive, 52 (18.8%) were HIV-exposed, and 9 (3.2%) were of unknown HIV status. Of the 113 children who were HIV-positive, 40 (35.4%) were on antiretroviral therapy (ART); only 8 of them were initiated on ART during the admission period. Among children with SAM, those who were HIV-positive were significantly more likely to be wasted compared with those who were HIV-negative (OR 2.2, 95% CI 1.1 - 4.5).
Eighty-seven children (31.4%) were treated for tuberculosis (TB), which was diagnosed during the admission period in 66 cases (75.9%). Diagnosis was based on clinical suspicion in children with persistent fever despite at least 7 days of intravenous antibiotics or who failed to gain weight, if a chest radiograph raised suspicion of TB, or at the clinician's discretion. HIV-positive children were more likely to be treated for TB than HIV-negative ones (OR 3.1, 95% CI 1.6 - 5.8).
One hundred and twenty-four children (44.8%) were diagnosed with pneumonia. This was more likely in HIV-positive children compared with HIV-negative ones (OR 2.6, 95% CI 1.4 - 4.6). One hundred and eighty-three children (66.1%) had gastroenteritis (GE). There was no statistically significant difference in the occurrence of GE between HIV-positive and HIV-negative children.
Fourteen children had severe anaemia that necessitated blood transfusion (haemoglobin concentration <6 g/dl). Three children had concomitant herbal intoxication on admission, 1 had cryptococcal meningitis, 1 had Kaposi's sarcoma, and 1 developed paralytic ileus during the course of treatment.
Outcomes
One hundred and eleven (40.1%) of the 277 children died in hospital, 31 deaths (27.9%) occurring within 48 hours of admission. Mortality was significantly higher among patients with SAM than among those with moderate malnutrition (46.9% v. 27.6%, p<0.001). Among patients with SAM, there was no significant difference in mortality between the two types of malnutrition (oedematous SAM 48.9% v. severe wasting 45.1%, p=0.61)
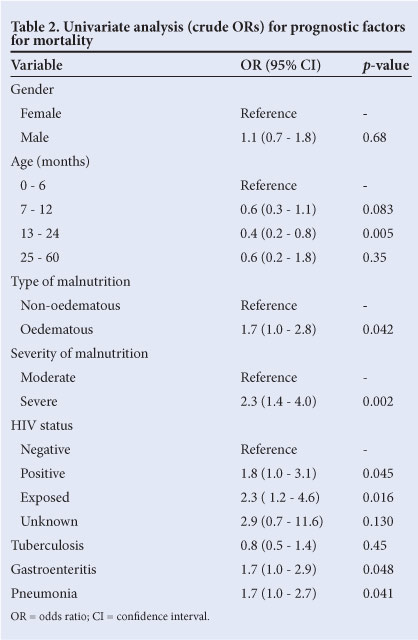
Several factors were identified as indicating a poor prognosis (i.e. death) in the univariate analysis (Table 2). However, after multivariate logistic regression analysis, 4 factors remained significant predictors of mortality (Table 3). There was no significant difference in mortality between children aged 0 - 6 months and those aged 7 - 12 months (OR 0.5, 95% CI 0.3 - 1.0), but children aged 13 - 24 months fared much better than those aged 6 months and under (OR 0.3, 95% CI 0.2 - 0.6).

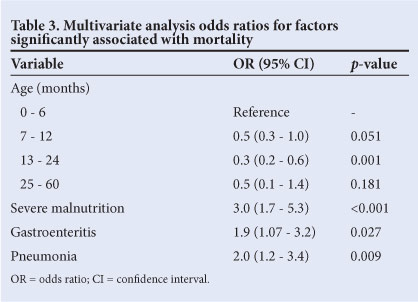
Pneumonia and GE were significant predictors of mortality (OR 2.0, 95% CI 1.2 - 3.4; p=0.009 and OR 1.9, 95% CI 1.1 - 3.2; p=0.027, respectively).
Mortality was highest among children of HIV-unknown status (55.6%), followed by HIV-exposed (50.0%), HIV-positive (43.4%) and HIV-negative children (30.1%). However, HIV was not a significant predictor of mortality in the multivariate model, and neither was TB.
The median length of hospital stay was 10 days (IQR 6 - 15 days). Children who died had a shorter duration of hospital stay than those who were discharged (median 5 v. 12 days; p<0.001).
Discussion
This study confirms that case fatality rates for childhood malnutrition remain very high at Mbabane Government Hospital, despite implementation of the WHO treatment guidelines. The overall case fatality rate for childhood malnutrition was 40.1%, and the WHO considers rates above 20% unacceptable. Even the rate for moderate malnutrition was alarmingly high, at 27.5% almost 6 times the targets for severe malnutrition established by the WHO.
Our findings contrast with other implementation studies that show significant improvements in case fatality rates. In South African hospitals, case fatality rates of 50% and 28% fell by ~25% after implementation of the WHO treatment guidelines.[6] After introduction of the guidelines at the International Centre for Diarrhoeal Disease Research in Bangladesh, case fatality rates decreased to 9% and subsequently to 3.9% from an initial 17%.[9]
The severity of malnutrition and the presence of co-morbid conditions have been shown to confer additional mortality risk among malnourished children.[4] In our study sample, mortality was found to be significantly higher for severe compared with moderate malnutrition (46.9% v. 27.6%, p<0.001). However, among children with SAM there was no significant difference in mortality between oedematous and severely wasted children (48.9% v. 45.1%, p=0.61). Children with co-morbid pneumonia and those with GE were almost twice as likely to die as those without (OR 2.0 and 1.9, respectively).
The prevalence of HIV among the study participants was 40.8%, a figure comparable to those in other African studies, which reported rates between 17% and 54%.[13,14] However, in the final logistic regression model HIV status was not a significant predictor of mortality. This contrasts with earlier studies, which found that HIVpositive children were up to six times more likely to die compared with HIV-negative children.[14] The lack of significant differences in case fatality rates among the various HIV subgroups strongly suggests fundamental deficiencies in the treatment of malnutrition. Co-morbid TB was not associated with increased mortality, as demonstrated in other studies.[13]
Our study did not intend to measure the level of adherence to each of the ten steps of treatment listed in the WHO guidelines. However, during data collection fundamental flaws in patient management were noted that could explain the high case fatality rates. Firstly, hypoglycaemia was not actively diagnosed or managed. In some cases children were not started on therapeutic feeds for up to 24 hours after admission, despite doctors' orders. Secondly, hypothermia was not adequately diagnosed or prevented. The paediatric ward did not have adequate heating, and furthermore the kangaroo technique was not being used in younger children.
Caution was not exercised when rehydrating malnourished children, which is critical to survival and recovery.[9] Antibiotics were not always prescribed as advised by the WHO guidelines. In some instances children were put on oral antibiotics when their clinical condition warranted intravenous therapy. Second-line antibiotics were not routinely prescribed to children with continued signs of infection after 48 hours of first-line therapy. Furthermore, prescription choices were often limited by the frequent drug stock-outs that affected the hospital. The above factors could explain the excessive risk of mortality associated with co-morbid pneumonia and gastroenteritis.
In our opinion, lack of proper and adequate laboratory support negatively affected case management. Routine tests ordered during case management were often not available, or inaccurate results were provided. Poor laboratory support made the management of children with electrolyte disturbances or severe anaemia difficult. Other operational factors such as low staff morale, poor staffing levels and lack of knowledge due to infrequent training on the use of the guidelines also contributed greatly to suboptimal care.
Study limitations
The study was retrospective, so analysis of risk factors associated with mortality was limited by the information that could be obtained from the patient charts. Information on various other prognostic factors was either missing or poorly recorded and therefore of no use.
Conclusion and recommendations
Implementation of the WHO guidelines for the inpatient treatment of severely malnourished children did not improve the case fatality rates for childhood malnutrition at Mbabane Government Hospital. There is a need for periodic clinical audits and mortality review meetings to identify and address factors associated with excessive mortality. Furthermore, the hospital needs to fully address operational factors that negatively affect patient management, such as drug stock-outs, poor staffing levels, low staff morale, poor laboratory functioning and inadequate training on use of the guidelines.
References
1. United Nations Department of Economic and Social Affairs. The Millennium Development Goals Report 2011. New York: United Nations, 2011. [ Links ]
2. World Health Organization. Improving Child Health in the Community. WHO/FCH/CAH/0212. Geneva: WHO, 2002. [ Links ]
3. Caulfield LE, de Onis M, Blossner M, Black RE. Undernutrition as an underlying cause of child deaths associated with diarrhea, pneumonia, malaria and measles. Am J Clin Nutr 2004;80(1):193-198. [ Links ]
4. Black RE, Morris SS, Bryce J. Where and why are 10 million children dying every year? Lancet 2003;361(9376):2226-2234. [http://dx.doi.org/10.1016%2FS0140-6736%2803%2913779-8] [ Links ]
5. Nemer L, Gelband H, Jha P. Commission on Macroeconomics and Health. The Evidence Base for Interventions to Reduce Malnutrition in Children under Five and School-age Children in Low- and Middle-Income Countries. CMH working paper No. WG5:11. Geneva: WHO, 2001. [ Links ]
6. Puoane T, Sanders D, Ashworth A, Chopra M, Strasser S, McCoy D. Improving the hospital management of malnourished children by participatory research. Int J Qual Health Care 2004;16(1):31-40. [http://dx.doi.org/10.1093%2Fintqhc%2Fmzh002]
7. Ashworth A, Chopra M, McCoy D, et al. WHO guidelines for management of severe malnutrition in rural South African hospitals: Effect on case fatality and the influence of operational factors. Lancet 2004;363(9415):1110-1115. [http://dx.doi.org/10.1016%2FS0140-6736%2804%2915894-7] [ Links ]
8. Schofield EC, Ashworth A. Why have mortality rates for severe malnutrition remained so high? Bull World Health Organ 1996;74(2):223-229. [ Links ]
9. Ashworth A, Khanum S, Jackson A, Schofield C. Guidelines for the Inpatient Treatment of Severely Malnourished Children. New Delhi: WHO Regional Office for South-East Asia, 2003. [ Links ]
10. World Health Organization. Management of the Child with a Serious Infection or Malnutrition: Guidelines for Care at the First-Referral Level in Developing Countries. Geneva: WHO, 2000. [ Links ]
11. World Health Organization. Management of Severe Malnutrition: A Manual for Physicians and Other Senior Health Workers. Geneva: WHO, 1999. [ Links ]
12. WHO Swaziland responds to rising incidence of severe malnutrition. Senior health care workers receive WHO training. http://www.who.int/disasters/repo/12698.pdf ( accessed 28 May 2011). [ Links ] De Maayer T, Saloojee H. Clinical outcomes of severe malnutrition in a high tuberculosis and HIV setting. Arch Dis Child 2011;96(6):560-564. [http://dx.doi.org/10.1136%2Fadc.2010.205039] [ Links ]
13. Chinkhumba J, Tomkins A, Banda T, et al. The impact of HIV on mortality during in-patient rehabilitation of severely malnourished children in Malawi. Trans R Soc Trop Med Hyg 2008;102(7):639-644. [http://dx.doi.org/10.1016%2Fj.trstmh.2008.04.028] [ Links ]
 Correspondence: O Benyera (drobenyera@yahoo.com)
Correspondence: O Benyera (drobenyera@yahoo.com)














