Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
South African Journal of Child Health
versão On-line ISSN 1999-7671
versão impressa ISSN 1994-3032
S. Afr. j. child health vol.7 no.2 Pretoria Mai. 2013
RESEARCH
Characteristics of children presenting with newly diagnosed type 1 diabetes
Y ReddyI; Y GanieII; K PillayIII
IMB ChB, DCH, Dip HIV Man, FCP (Paed). Department of Paediatrics and Child Health, Nelson R Mandela School of Medicine, Faculty of Health Sciences, University of KwaZulu-Natal, Durban, South Africa. Division of Paediatric Endocrinology, Inkosi Albert Luthuli Central Hospital, Durban, South Africa
IIMB ChB, DCH, FCP (Paed), Cert Paed Endo. Department of Paediatrics and Child Health, Nelson R Mandela School of Medicine, Faculty of Health Sciences, University of KwaZulu-Natal, Durban, South Africa. Division of Paediatric Endocrinology, Inkosi Albert Luthuli Central Hospital, Durban, South Africa
IIIMB ChB, DCH, FCP (Paed), Cert Paed Endo. Division of Paediatric Endocrinology, Inkosi Albert Luthuli Central Hospital, Durban, South Africa. Centre for Paediatric Endocrinology and Diabetes, Westville Hospital, Durban, South Africa
ABSTRACT
BACKGROUND: The clinical presentation of type 1 diabetes in children can be acute or insidious, and symptoms may be subtle and frequently misinterpreted. Presentation with diabetic keto-acidosis (DKA) may be associated with significant morbidity and mortality in the paediatric population. This study aims to determine the characteristics of children presenting to the paediatric endocrine service at Inkosi Albert Luthuli Central Hospital (IALCH) with DKA at the time of diagnosis, and to determine the frequency of missed diagnoses in the previous month.
METHODS: A retrospective study was done at IALCH, the paediatric tertiary referral centre for KwaZulu-Natal, South Africa. The study sample included all children with an initial diagnosis of type 1 diabetes between January 2008 and June 2010. Children presenting with DKA were compared with those who presented without DKA.
RESULTS: During the period under review, 63 children presented with type 1 diabetes. Of these, 44 (69.8%) had DKA at the time of diagnosis. The median duration of symptoms preceding diagnosis in the DKA group was 2 weeks, versus 4 weeks in the non-DKA group (p=0.002). There was no significant difference between the groups when ethnicity, gender and age at presentation were compared. Of 42 patients who presented to healthcare facilities in the month preceding diagnosis, 27 (64.3%) were misdiagnosed.
CONCLUSION: Patients who presented with DKA had a shorter duration of symptoms than the non-DKA group. Ethnicity had no effect on characteristics at presentation. There was an unacceptable rate of missed diagnoses of type 1 diabetes in both the private and public sectors.
There are currently 250 million people living with diabetes worldwide. Of these, half a million are children under the age of15 years diagnosed with type 1 diabetes. Type 1 diabetes is increasing in incidence worldwide at a rate of 2 - 5% per year, and roughly 200 children are diagnosed with new-onset type 1 diabetes every day.[1] The condition is increasing in all age groups, with a disproportionately steep increase in preschool children.[1] Unfortunately there are no published data on its incidence in South Africa (SA).
The clinical presentation of type 1 diabetes in children can be acute or insidious. It is generally easy to diagnose based on a history of polyuria, polydipsia, polyphagia, weight loss and generalised body weakness, together with simple bedside tests such as urine dipsticks and glucose test strips. However, in very young children symptoms may be subtle and are frequently misinterpreted. In addition, poor history taking by the clinician may delay diagnosis. Without an early diagnosis initial presentation may be with diabetic keto-acidosis (DKA), which can be life threatening.
The frequency of DKA as an initial diagnosis in type 1 diabetes is between 15% and 70% in Europe and North America.[2] DKA is associated with significant morbidity and mortality in the paediatric population. Cerebral oedema and haemodynamic instability are the main causes of morbidity. The mortality rate ranges from 0.15% to 0.3% in developed countries and is as high as 26% in developing ones, notably Ghana, Tanzania and Kenya.[3-5]
The high rate of misdiagnosis of type 1 diabetes in both First-World and developing countries in the month prior to diagnosis has both public health and clinical implications. It is well known that long-term glycaemic control is adversely affected by late presentation in DKA, and the need for high-care beds and associated laboratory and clinical management places an additional strain on healthcare resources.
Studies in First-World countries have shown that DKA as an initial presentation of type 1 diabetes is more frequent in children under 5 and that ethnicity has no effect on presentation.[2] There has been a recent worldwide focus on programmes to reduce the incidence of DKA at diagnosis. However, there is a paucity of research on characteristics of children presenting with type 1 diabetes in SA and other developing countries.
This study aims to determine the characteristics of children with newly diagnosed type 1 diabetes seen at the paediatric endocrine service at Inkosi Albert Luthuli Central Hospital (IALCH), a tertiary referral centre in KwaZulu-Natal, SA, and to establish the frequency of missed diagnoses in the month before diagnosis.
Methods
The study design was a retrospective chart review. The study sample was all children presenting to IALCH with an initial diagnosis of type 1 diabetes from January 2008 to June 2010. It must be emphasised that the protocol is for all newly diagnosed paediatric diabetic patients in the public sector in KwaZulu-Natal to be referred to IALCH, but there is no way to monitor its consistent implementation.
The study sample was divided into patients who presented with DKA and those who did not, and each group was further assessed in terms of age, sex, ethnicity, symptom duration and health-seeking behaviour in the month before diagnosis.
Data were collated on an Excel spreadsheet and analysed using SPSS version 15. Categorical variables were assessed using Pearson's chi-square test and quantitative variables using the Mann-Whitney U-test and Student's t-test. A p-value of <0.05 was considered significant.
Results
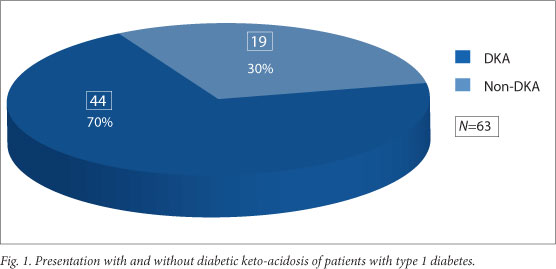
Sixty-three patients were referred to the tertiary paediatric endocrine service with newly diagnosed type 1 diabetes over the 30-month study period. Of these, 44 (69.8%) presented with DKA at initial diagnosis (Fig. 1). There was a female predominance overall (60.3% (38) girls). Female predominance was especially marked in the DKA group, in which there were 28 girls versus 16 boys, but this was not statistically significant (Fig. 2).

The majority of patients in both groups were black Africans (73.6% in the non-DKA group and 68.1% in the DKA group). There was a similar proportion of white and Indian patients in both groups and only 2 coloured patients in the entire sample, both of whom presented in DKA. Ethnicity had no significant effect on presentation with DKA (p=0.813, Pearson's chi-square test).
The youngest child in the study was 13 months old and the oldest was 13 years and 6 months (Fig. 3). There was a trend towards presentation at an earlier age in the DKA group, where the mean age was 7 years and 4 months versus 8 years and 6 months for the non-DKA group (p=0.17, t-test). Patients were divided into four age groups: 0 - 4 years, 5 - 8 years, 9 - 12 years and 13 - 16 years. Overall 31 of the 63 patients (49.2%) were in the 9 - 12-year, 18 (28.6%) in the 5 - 8-year, 12 (19.0%) in the under-4 and 2 (3.2%) in the 13 - 16-year age group. Looking at the age groups when the patients had been divided into the DKA and non-DKA cohorts, it is striking that all of the patients in the 5 -8-year age category presented in DKA. There was no difference with regard to presentation with DKA in the 0 - 4-year age group, which is inconsistent with First-World data.

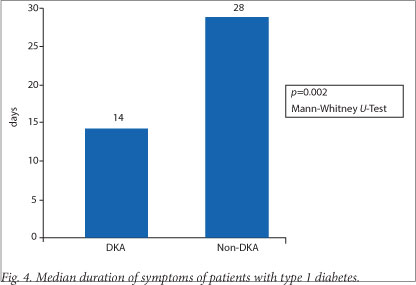
The median duration of symptoms in the month before diagnosis was 14 days in the DKA group versus 28 days in the non-DKA group (p=0.002, Mann-Whitney U-test) (Fig. 4). Of 63 patients, 42 (66.7%) had presented to a healthcare facility in the month before diagnosis. There was no difference in health-seeking behaviour between the groups.
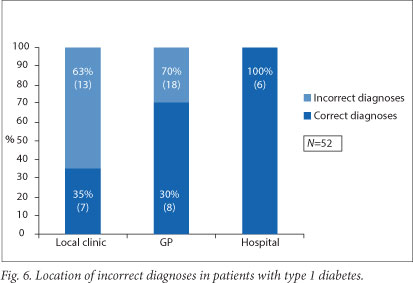
Interestingly, there was no difference in the proportions of missed diagnoses in the two groups, with 64.3% of diagnoses missed overall (27 out of 42 patients) (Fig. 5). Nine patients had multiple visits to healthcare facilities prior to diagnosis. Overall, in both groups there were 52 opportunities for early diagnosis, with 37 of those resulting in misdiagnosis (69.2% of presentations to a GP (18 of 26), 100% of presentations to a hospital (6 of 6), and 65.0% of presentations to the local clinic (13 of 20)) (Fig. 6).

Discussion
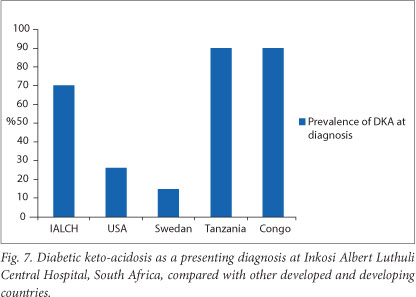
The prevalence of DKA as a presenting diagnosis in children with type 1 diabetes between January 2008 and June 2010 at Inkosi Albert Luthuli Hospital was 69.8%. This is high compared with rates in developed countries such as the USA (26%) and Sweden (15%).[2,6] The difference could be attributed to higher levels of awareness of diabetes on the part of both health professionals and the general public in developed countries. However, when compared with developing countries such as Tanzania and Congo, with prevalence rates of DKA at diagnosis of 90%, SA is not faring too badly[5] (Fig. 7).
Patients who presented with DKA had a shorter duration of symptoms than the non-DKA group (14 v. 28 days) (p=0.002). This implies lack of recognition of classic symptoms by parents, caregivers and schoolteachers. Patients are usually taken to the hospital when critically ill with easily recognisable signs such as a decreased level of consciousness and laboured breathing.
Ethnicity had no effect on the characteristics of our patients at presentation, in keeping with findings from a large population- based study in the USA (2008).[2] In SA ethnicity has historically been a surrogate marker for socio-economic status. There may have been bias because all the data were from a public hospital, excluding the more affluent patients who use private healthcare facilities.
All the children in the 5 - 9-year age group presented with DKA. It is possible that older children are more likely to draw attention to their symptoms, and may be able to understand health education campaigns. Symptoms in younger children are more subtle and tend to be overlooked. Surprisingly, and out of keeping with data from First-World countries, there was no difference in the frequency of initial presentation with DKA in the under-4 age group.
There is an unacceptable rate of missed diagnosis of type 1 diabetes in both the private and public sectors (64.3%). Type 1 diabetes is a simple diagnosis, and the high rate of misdiagnosis implies clinicians' failure to recognise symptoms or carry out routine investigations like urine dipstick testing. 36.3% (16 of 44) of patients did not present to any healthcare facility prior to developing DKA, despite having typical symptoms. This indicates lack of awareness of symptoms on the part of the public.
Recommendations
There is a need to improve knowledge about signs and symptoms of type 1 diabetes and so decrease the morbidity and mortality associated with DKA. This involves early recognition of symptoms by parents, asking the correct questions by medical personnel, and routine use of inexpensive basic bedside tests like urine dipsticks to make the diagnosis. This will have beneficial effects not only for patients but for our already stretched public healthcare system in SA.
References
1. International Diabetes Federation. IDF Diabetes Atlas. 4th ed. Brussels: International Diabetes Federation, 2009. [ Links ]
2. Rewers A, Klingensmith G, Davis C, et al. Presence of diabetic ketoacidosis at diagnosis of diabetes mellitus in youth. Pediatrics 2008;121(5):1258-1266. [http://dx.doi.org/10.1542/peds.2007-1105] [ Links ]
3. Wolfsdorf J, Craig ME, Daneman D, et al. Diabetic ketoacidosis in children and adolescents with diabetes. Pediatr Diabetes 2009;10:118-133. [http://dx.doi.org/10.1111/j.1399-5448.2009.00569.x] [ Links ]
4. Otieno CF, Kayima JK, Omonge EO, Oyoo GO. Diabetic ketoacidosis: Risk factors, mechanisms and management strategies in sub-Saharan Africa. East Afr Med J 2005;82:197-203. [http://dx.doi.org/10.4314/eamj.v82i12.9382] [ Links ]
5. Majaliwa ES, Munubhi E, Ramaiya K, et al. Survey on acute and chronic complications in children and adolescents with type 1 diabetes at Muhimbili National Hospital in Dar es Salaam, Tanzania. Diabetes Care 2007;10(9):2187-2192. [http://dx.doi.org/10.2337/dc07-0594] [ Links ]
6. Hekkala A, Knip M, Verjola R. Ketoacidosis at diagnosis of type 1 diabetes in children in Northern Finland. Diabetes Care 2007;30(4):861-866. [http://dx.doi.org/10.2337/dc06-2281] [ Links ]
 Corresponding author: YReddy (yavred@gmail.com)
Corresponding author: YReddy (yavred@gmail.com)














