Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
South African Journal of Child Health
versão On-line ISSN 1999-7671
versão impressa ISSN 1994-3032
S. Afr. j. child health vol.7 no.1 Pretoria Jan. 2013
CASE REPORT
Human born with a tail: A case report
A H SarmastI; H I ShowkatII; S F MirIII; S R AhmadIV; A R BhatV; A R KirmaniVI
IPostgraduate scholar in Surgery; Sheri-Kashmir Institute of Medical Sciences (SKIMS), Srinagar, India
IIPostgraduate scholar in Internal Medicine; Sheri-Kashmir Institute of Medical Sciences (SKIMS), Srinagar, India
IIIPostgraduate scholar in Surgery; Sheri-Kashmir Institute of Medical Sciences (SKIMS), Srinagar, India
IVPostgraduate scholar in Surgery; Sheri-Kashmir Institute of Medical Sciences (SKIMS), Srinagar, India
VAdditional professor, Neurosurgery; Sheri-Kashmir Institute of Medical Sciences (SKIMS), Srinagar, India
VIProfessor, Neurosurgery; Sheri-Kashmir Institute of Medical Sciences (SKIMS), Srinagar, India
ABSTRACT
CONTEXT: The dorsal cutaneous appendage, or so-called human tail, is often considered to be a cutaneous marker of underlying occult spinal dysraphism. Human tails have always elicited curiosity. A unique case of human dysraphism is described.
CASE REPORT: An interesting case of a child with a tail-like caudal appendage that had been present since birth is reported. Surgical excision of a pseudo-tail was done together with repair of a meningocele.
CONCLUSION: Before any form of treatment for a caudal appendage is undertaken, the patient must be evaluated carefully in case it coexists with a lesion of the intraspinal component.
A human tail is a rare congenital anomaly protruding from the lumbosacrococcygeal region. Some authors have considered this rare and curious condition to be evidence of man's descent from or relation to other animals, while others have made it the subject of superstition. Advanced imaging technology in recent decades has allowed more thorough investigation of these patients and better defined the association of such lesions with spinal dysraphism and tethered spinal cord.[1] Management must include a complete neurological history and examination as well as magnetic resonance imaging or a computed tomography scan. After diagnosis, microsurgery should be performed if there is any intraspinal component, to avoid damage and neurological deficit.[2]
Case report
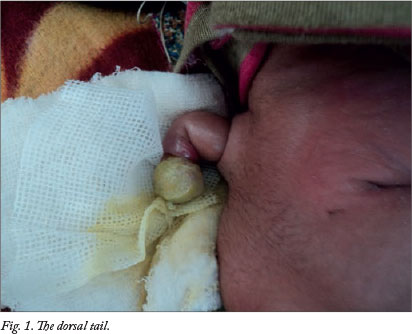
A healthy 4-month-old male infant was brought for investigation of a tail-like structure that had been present in the lumbosacral area since birth (Fig. 1). According to the parents, the tail had measured about 3 cm at birth and had been increasing in size. On physical examination, the appendage was tail-like, soft, well circumscribed, 5 cm long and 0.5 cm thick and was attached to the back of the tip of the coccyx, appearing like a human tail. It was soft, non-tender and covered with normal skin. There was no voluntary movement in the tail. The findings on general and systemic examination were otherwise normal. The child had no other congenital defect, and there was no family history of any developmental or congenital anomaly. The possibility of a true neonatal tail as opposed to a pseudotail (see below) was considered. Imaging of the spine showed a spina bifida in the lumbosacral area (Fig. 2). The patient was moved to the neonatal intensive care unit and the neurosurgeon removed the tail and repaired the meningocele. Histopathological examination revealed that the tail-like structure contained skin, muscle and adipose tissue only. The infant recovered uneventfully and no neurological deficit was evident on follow-up until 12 months of age.

Discussion
Caudal appendages are unusual malformations and are divided into true tails and pseudo-tails (lipoma, teratoma, myelomeningocele and parasitic fetus).
During the 5th and 6th week of gestation, the human embryo has a tail with 10 - 12 caudal vertebrae. This regresses by reduction in the number of vertebrae and fusion, leaving the vestigial coccyx. The tail usually disappears by week 8 of gestation, although the exact time of disappearance varies. A persistent 'true' tail probably arises as a vertebrate remnant of the embryonic tail[3-5] and is therefore a vestigial structure.[4,6] There are very few documented cases of tails containing cartilage or up to five vertebrae. Infrequently, a child is born with a 'soft tail', which contains no vertebrae but only blood vessels, muscles and nerves. Some of these tails may in fact be sacrococcygeal teratomas.[7] The true tail should be thought of as a benign condition, a prolongation beyond the coccygeal or mid-gluteal region, and should not be associated with any underlying malformation.[5,8,9] Modern procedures allow doctors to eliminate the tail within a short period after birth. Simple surgical excision of the true tail has been advocated.[9] However, recent reports emphasise associated midline anomalies that may change the surgical approach in these patients.[3,10,11]
In contrast, like other lumbosacral skin lesions, the caudal appendages mostly occurring with spina biida occulta or spinal dysraphism are pseudo-tails. The appendage is only a cutaneous marker of the underlying spinal dysraphism, since the skin and nerve systems are related by their similar ectodermal origin, and surgical excision is not done for cosmetic reasons alone. Further pre-operative examination and complex surgical intervention are usually necessary.
It is important to distinguish between a true tail and a pseudo-tail in the lumbosacral region, since the treatment and prognosis are different. Several theories have been developed to explain the development of split-cord malformations. One recent generally accepted theory suggests that split-cord malformations originate from a basic error occurring around the time when the primitive neuro-enteric canal closes. The basic error is the formation of an accessory neuro-enteric canal between the yolk sac and amnion, which is subsequently invested with mesenchyme to form an endomesenchymal tract that splits the notochord and neural plate.[12,13] Pluripotential cells of the endomesenchymal tract could develop into a variety of tissues consisting principally of mesodermal elements.[12,13]
In conclusion, the caudal appendage is not difficult to treat. However, before the method of treatment is chosen, it is necessary to evaluate the patient carefully in case the appendage coexists with lesions of the intraspinal component. After the operation, long-term follow-up of the patient for tethered cord is necessary.[14]
References
1. Donovan DJ, Pedersen RC. Human tail with noncontiguous intraspinal lipoma and spinal cord tethering: Case report and embryologic discussion. Pediatr Neurosurg 2005;41(1):35-40. [http://dx.doi.org/10.1159/000084863] [ Links ]
2. Singh DK, Kumar B, Sinha VD, Bagaria HR. The human tail: Rare lesion with occult spinal dysraphism -a case report. J Pediatr Surg 2008;43(9):e41-43.[http:// dx.doi.org/10.1016/j.jpedsurg.2008.04.030] [ Links ]
3. Belzberg AJ, Myles ST, Trevenen CL. The human tail and spinal dysraphism. J Pediatr Surg 1991;26(10):1243-1245. [ Links ]
4. Dao AH, Netsky MG. Human tails and pseudotails. Hum Pathol 1984;15(5):449-453. [http://dx.doi.org/10.1016/S0046-8177(84)80079-9] [ Links ]
5. Ledley FD. Evolution and the human tail. A case report. N Engl J Med 1982;306(20):1212-1215. [http://dx.doi.org/10.1056/NEJM198205203062006] [ Links ]
6. Alashari M, Torakawa J. True tail in a new-born. Pediatr Dermatol 1995;12(3):263-266. [ Links ]
7. Kabra NS, Srinivasan G, Udani RH. True tail in a neonate. Indian Pediatr 1999;36(7):712-713. [ Links ]
8. Lu FL, Wang PJ, Teng RJ, Yau KIT. The human tail. Pediatr Neurol 1998;19(3):230-233. [http://dx.doi.org/10.1016/S0887-8994(98)00046-0] [ Links ]
9. Spiegelmann R. Schinder E, Mintz M, Blaksein A. The human tail: A benign stigma - a case report. J Neurosurg 1985;63(3):461-462. [http://dx.doi. org/10.3171/jns.1985.63.3.0461] [ Links ]
10. Matsumoto S, Yamamoto Y, Okura K. Human tail associated with lipomeningocele: A case report. Neurol Med Chir (Tokyo) 1994;34(1):44-47. [http://dx.doi.org/10.2176/nmc.34.44] [ Links ]
11. Ohhara Y. Human tail and other abnormalities of the lumbosacrococcygeal region relating to tethered cord syndrome. Ann Plast Surg 1980;4(6):507-510. [http://dx.doi.org/10.1097/00000637-198006000-00010] [ Links ]
12. Erşahin E, Demirtaş S, Mutluer A, Tosun R, Saydam S. Split cord malformations: Report of three unusual cases. Pediatr Neurosurg 1996;24(3):155-159. [ Links ]
13. Tubbs RS, Salter EG, Oakes WJ. Split spinal cord malformation. Clin Anat 2007;20(1):15-18. [http://dx.doi.org/10.1002/ca.20248] [ Links ]
14. Cai C, Shi O, Shen C. Surgical treatment of a patient with human tail and multiple abnormalities of the spinal cord and column. Advances in Orthopedics 2011; article ID 153797. [http://dx.doi.org/10.4061/2011/153797] [ Links ]
 Correspondence: HI Showkat (docirfanshahi512@gmail.com)
Correspondence: HI Showkat (docirfanshahi512@gmail.com)














