Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
SA Orthopaedic Journal
versão On-line ISSN 2309-8309
versão impressa ISSN 1681-150X
SA orthop. j. vol.18 no.3 Centurion Ago./Set. 2019
http://dx.doi.org/10.17159/2309-8309/2019/v18n3a3
TRAUMA
A survey of the management of posterior malleolar ankle fractures in South Africa
Workman MlI; Wever GSII; McCollum GAIII
IBSc Physio, MBBCh; Registrar; Department of Orthopaedics, Groote Schuur Hospital, University of Cape Town, Cape Town, South Africa
IIMBBCh; Registrar; Department of Orthopaedics, Groote Schuur Hospital, University of Cape Town, Cape Town, South Africa
IIIMBChB, MMed(UCT), FC Orth SA; Consultant; Department of Orthopaedics, Groote Schuur Hospital, University of Cape Town, Cape Town, South Africa
ABSTRACT
BACKGROUND: Posterior malleolus fractures are associated with poorer functional outcomes compared to simpler malleolar fractures. Traditional teaching states that if a posterior malleolus fracture involves less than 25% of the distal tibia, it can be managed without fixation. Current literature has shown that fixation should not be based on the size of the posterior fragment but rather on the fracture pattern, instability and awareness that reduction and fixation is biomechanically advantageous. We hypothesised that current management of ankle fractures with posterior malleolus involvement in South Africa is not evidence-based and is suboptimal.
We sought to assess the training, experience and decision-making of surgeons and trainees who are involved in the management of ankle fractures. Another aim was to develop evidence-based algorithms for the management of posterior malleolus and complex ankle fractures.
METHODS: An email survey consisting of questions related to the management of ankle fractures was sent to specialists, registrars and medical officers who voluntarily completed an online survey.
RESULTS: A total of 103 out of 456 emails sent drew responses to the survey. Responses included 28% from consultants, 54% from registrars and 18% from medical officers. Forty-six per cent of responders believed that posterior malleolus fractures can be managed non-operatively if less than 20% of the tibial plafond is involved. Only 49% would CT scan a posterior malleolus prior to operating. Thirty-eight per cent of the responders were not familiar or comfortable with the posterior-lateral approach used for fixation of the posterior malleolus directly.
CONCLUSION: Understanding of ankle fractures has progressed. A significant proportion of responders to the survey are not following best practice and current literature. Posterior malleolus fractures are not benign and have poorer outcomes compared to bi-malleolar or lateral malleolus ankle fractures. All patients with posterior malleolus fractures should receive pre-operative CT scan. All posterior malleolar fractures that can be held with a plate or screws should be fixed.
Level of evidence: Level 5
Key words: trimalleolar ankle fracture, open reduction of posterior malleolus, syndesmosis injury, Haraguchi classification, CT scan of ankle fractures.
Introduction
The incidence of ankle fractures is approximately 187 per 100 000 people per year. Two-thirds of these are isolated malleolar fractures, with bimalleolar fractures occurring in one-fourth and trimalleolar fractures making up the remainder. Risk factors for ankle fractures include increased body mass index and the elderly. Open fractures are rare.1
Management of ankle fractures ranges from non-operative treatment to surgery and prolonged non-weight-bearing. The consequences of inadequate treatment can lead to a poor outcome and further reconstructive surgery. Missed or insufficient syndesmotic injury management is associated with ankle joint failure. The presence of a posterior malleolus fracture is associated with poorer functional outcomes compared to more simple fractures.2
Fractures involving the posterior malleolus frequently include damage to the articular cartilage which is likely to contribute significantly to rapid onset of severe arthritis.3 These injuries occur secondary to a pronation-external rotation type force and result in a Weber B or C type pattern of injury to the distal fibula with or without a medial injury.4 Depending on the degree of force imparted to the ankle at the time of injury, progressive failure of the syndesmotic ligaments occurs, from the anterior inferior tibia fibular ligament (AITFL) anteriorly, through the interosseous ligament (IOL) and the posterior inferior tibial fibular ligament (PITFL) posteriorly. When a posterior fragment is visualised on radiographic imaging, this indicates that the PITFL has avulsed the Volkmann's fragment, completely destabilising the syndesmosis.5-7
Traditional teaching states that, if a posterior malleolus fracture involves less than 25% of the distal tibia, it can be managed without fixation. Reducing and fixing the medial and lateral malleolar fractures and inserting a syndesmotic screw became the accepted treatment.5,89 Rigid fixation of the syndesmosis with a syndesmotic screw has, however, been associated with inhibition of the normal motion at the tibia-fibula syndesmosis, sometimes resulting in pain and/or failure of the screw.10 The likelihood of malreduction at this joint is also significant. Current understanding and emerging evidence is that fixation should not be based on the size of the posterior fragment but rather on the awareness that reduction and fixation is biomechanically advantageous and may have fewer adverse sequelae. Fixation stabilises the PITFL of the syndesmosis, potentially negating the need for a syndesmotic fixation.11 Beumer et al. suggest that syndesmotic screw fixation does not adequately stabilise the syndesmosis with early weight-bearing.12
The technical requirement of approaching the posterior malleolus may discourage surgeons unfamiliar with the postero-lateral approach. As opposed to the traditional direct lateral approach to the subcutaneous fibula, the postero-lateral approach requires dissection through the flexor mass and protection of neurovascular structures. The patient also needs to be positioned either in the lateral position or prone. Once mastered, however, this is a relatively simple approach that provides excellent exposure for reduction and fixation of posterior and lateral malleolus fractures.13
Considering the above, it is hypothesised that current management of ankle fractures is suboptimal. The indications for non-operative management may be based on outdated evidence and posterior malleolus fractures may not be reduced and fixed. This study aimed to assess the training, experience and decision-making of the surgeons who are involved in the management of ankle fractures with the aim of implementing a technical update or training as necessary.
Methods
This was a descriptive cross-sectional survey analysis. Qualified specialists, registrars and medical officers in orthopaedics in South Africa were identified using their respective professional member listings and university registrations. Email databases from the South African Orthopaedic Society were used to email a questionnaire using the Google Forms platform. This consisted of questions related to the management of ankle fractures (see Appendix). These questions were based on questions from the Consensus of the 7th Round Table held in Cardiff in September 2017. These are the thoughts and opinions, with consensus where possible, of 30 orthopaedic foot and ankle consultant surgeons gathered from across Europe and the United Kingdom.14 The specialists, registrars and medical officers voluntarily completed an online survey regarding ankle fractures with respect to experience, training and decision-making.
This was a single email survey. Non-responders were sent a reminder after one week.
Our data management plan entailed analysis of Google Forms responses in Excel. We used simple descriptive statistics to analyse the data. We reported categorical data in tables with frequencies and percentages. We tested normality of the data qualitatively.
A sample size of 100 was required to estimate a hypothesised sample point of 50% for the primary outcome ('Are ankle syndesmosis injuries treated non-operatively when they should be operatively fixated?') with a 10% error either side of the mean.
This is a qualitative questionnaire. Validity was determined by face, content and construct validity. Reliability was enhanced by targeting responses from a large population group. Responses were analysed according to current accepted standards of care.
Results
One hundred and three out of 456 emails sent drew responses to the survey (22.6% response rate). Of these, 28% (n=29) were from consultants; 54% (n=52) from registrars; and 18% (n=19) from medical officers. Most those who responded (49%, n=50) had between five and ten years of experience in orthopaedics; 38% (n=40) had less than five years of orthopaedic experience; and 13% (n=13) of responders had more than ten years of experience.
Thirty-two per cent (n=33) of responders would treat an undisplaced Weber A type fracture with weight-bearing as tolerated in a boot. Fifty-six per cent (n=58) would manage this fracture non-weight-bearing in a moulded cast while the remainder (12%, n=12) would perform reduction and internal fixation with a syndesmosis fixation in 2.8% (n=3).
Forty-nine per cent (n=50) would treat a displaced Weber B type fracture with mortice shift and deltoid ligament avulsion with reduction and fixation and no syndesmotic fixation. Twenty-seven per cent (n=28) would use open reduction internal fixation (ORIF) with syndesmosis fixation. Twenty-four per cent (n=25) would manage in a moulded cast.
Eighty-one per cent (n=83) of responders would reduce and fixate the syndesmosis for a Weber C type fracture. Nine per cent (n=9) would not use syndesmosis fixation (but open reduce and fixate), and the remainder would treat in moulded plaster or a boot (10%, n=10).
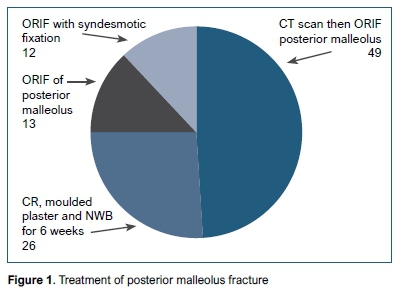
With regard to a trimalleolar fracture shown on X-ray, 49% (n=50) would CT scan and then plan to open reduce and fixate the posterior malleolar fragment. Thirteen per cent (n=13) would proceed to surgery of the posterior malleolus without a CT scan. Twelve per cent (n=12) would ORIF with syndesmotic fixation (no CT scan), and 26% (n=27) would manage it in a moulded plaster, non-weight-bearing for six weeks (Figure 1).
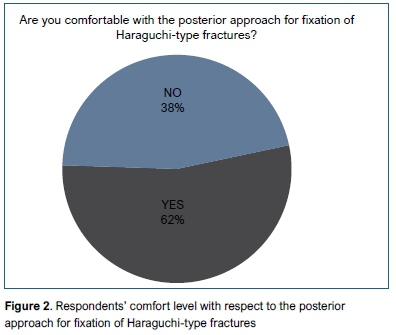
Forty-six per cent (n=47) of respondents would not fix a posterior malleolar fragment that was <20% of the total joint surface area. Fifty-one per cent (n=53) would not CT scan a posterior malleolar fracture identified on X-ray prior to surgery. Sixty-two per cent (n=64) of respondents feel comfortable performing the posterior approach to fix a posterior malleolar fracture (Figure 2).
Sixty-five per cent (n=67) fix syndesmotic injuries with a screw, 25% (n=26) use a combination of screw-and-tightrope type device and 10% use only a tightrope type device. Eighty-five per cent (n=88) do not routinely offer removal of syndesmosis fixation.
Discussion
By the nature of this study being a survey, a low response rate is to be expected. Questions were validated, but some of the questions can be perceived to be leading due to the accompanying X-ray images. This study clearly highlighted the differing opinions on the management of ankle fractures by orthopaedic surgeons in South Africa.
Although this study aimed primarily to assess current practice with regard to the management of posterior malleolar fractures, it also questioned the management of Weber A, B and C type fractures. Of note here is that the understanding of a stable fracture (one with no syndesmotic disruption) versus those requiring that the syndesmosis be addressed to avoid ankle joint failure, appears to be deficient. This may be related to responses from junior surgeons but is of concern as ankle fractures are frequently left to the junior team members to perform. Correct understanding is therefore critical. Unfortunately, not tracking responses for confidentiality reasons meant that this could not be investigated further.
Stable fractures such as Weber A type may be managed with early weight-bearing. Clinical examination and further investigations should aim to elicit any evidence of syndesmosis injury, which should prompt fixation.
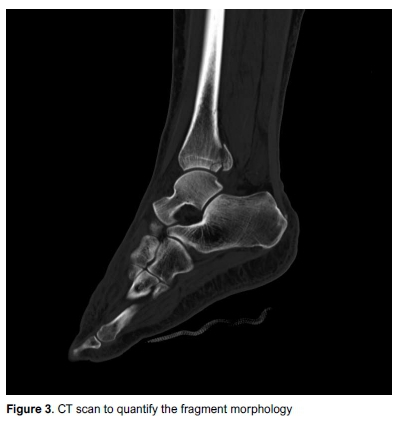
Current literature refutes the long-held belief that posterior malleolus fractures constituting less than 25% of the total joint surface area do not need to be fixed.15 Rather, sufficient imaging in the form of a CT scan should be obtained routinely. This allows the heterogeneous nature of these fracture patterns to be optimally appreciated. The functional outcome does not correlate with the size of the fragment. Without a CT scan, the size of the fragment is often underestimated as the fracture line may run in oblique planes to the standard AP and lateral radiographs. Meijer et al. showed that it is impossible to quantify the size of a posterior malleolar fracture on X-ray. This makes application of the 'rule of 25s' impossible. A CT scan is therefore always required to quantify the fragment morphology.16 Additionally, a flipped fragment of articular surface is often encountered once the posterior malleolus fragment is mobilised and needs to be reduced to correctly reduce and recreate the joint surface. This is visualised on CT scan as shown in Figure 3.
The Haraguchi classification of posterior malleolar fractures (Figure 4) describes the fracture pattern but does not address the mechanism of injury. Mason et al. have suggested a classification system of posterior malleolar fractures that progresses in severity, indicating the pathomechanics of the fracture and then guides surgical fixation.17 Attempting to address the syndesmosis without reduction and stabilisation of the posterior malleolus often results in malreduction of the syndesmosis.
Gardner et al., in a cadaveric model, demonstrated that fixation of the posterior malleolus restored about 70% of syndesmosis stability compared to 40% after syndesmotic screw fixation.18 Reduction was found to be more accurate when the posterior malleolus was fixed.19 There is also evidence to suggest that midterm functional outcomes were equivalent to what might be expected with a unimalleolar ankle fracture.20
Conclusion
The understanding of ankle fractures has progressed. We have shown that a significant proportion of responders to the survey are not following best practice and current literature. Posterior malleolus fractures, particularly, are not benign and have poorer outcomes compared to bi-malleolar or lateral malleolus ankle fractures. Size is not in itself an indicator for fixation. For surgeons to optimally manage posterior malleolus fractures, a pre-operative CT scan should be performed on all patients. They need to familiarise themselves with the surgical management of posterior malleolus fractures and with this, the postero-lateral approach to the ankle. Current literature supports the fixation of posterior malleolar fractures. There is certainly further to go regarding the understanding and treatment of these injuries.
Ethics statement
This research was approved by the University of Cape Town Department of Surgery Research Committee (2018/023) and the University of Cape Town Faculty of Health Sciences Ethics Committee (HREC/REF: 314/2018).
The authors declare that this submission is in accordance with the principles laid down by the Responsible Research Publication Position Statements as developed at the 2nd World Conference on Research Integrity in Singapore, 2010. Informed consent was obtained.
Declaration
The authors declare authorship of this article and that they have followed sound scientific research practice. This research is original and does not transgress plagiarism policies.
Acknowledgement
Dr Christof Marias, foot and ankle surgeon, Netcare Blouberg Hospital, Cape Town, South Africa.
Author contributions
MW contributed to the original study concept, proposal write-up, data collection and analysis, and final article write-up; GW assisted with the article and proposal write-up and final article additions; GM contributed to the study design, data analysis and final article concepts.
ORCID
Ml Workman © http://orcid.org/0000-0002-7999-9069 GS Wever © http://orcid.org/0000-0001-7072-1565
References
1. Egol K, Koval K, Zuckerman J. Handbook of Fractures 4th Ed. Philadelphia, PA: Wolters Kluwer Health/Lippincot Williams and Wilkins, 2010. [ Links ]
2. Velleman J, Nijs S, Hoekstra H. Operative management of AO type 44 ankle fractures: determinants of outcome. JFAS, Dec 2017. [ Links ]
3. Lauge-Hansen N. Fractures of the ankle I. Combined experimental-surgical and experimental-roentgenologic investigations. Arch Surg 1950;60:957-85. [ Links ]
4. Reudi TP, Murphy WM. AO Principles of Fracture Management. Stuttgart, Germany: Thieme. 2000. [ Links ]
5. Burns WC II, Prakash K, Adelaar R, Beaudoin A, Krause W. Tibiotalar joint dynamics: indications for the syndesmotic screw: a cadaver study. Foot & Ankle 1993;14:153-58. [ Links ]
6. Close JR. Some applications of the functional anatomy of the ankle joint. JBJS 1956;38:761-81. [ Links ]
7. Scheidt KB, Stiehl JB, Skrade DA, Barnhardt T. Posterior malleolar ankle fractures: an in vitro biomechanical analysis of stability in the loaded and unloaded states. J Orthop Trauma 1992;6:96-101. [ Links ]
8. Phillips WA, Schwartz HS, Keller CS, Woodward HR, Rudd WS, Spiegel PG, Laros GS. A prospective, randomized study of the management of severe ankle fractures. JBJS 1985;67:67-78. [ Links ]
9. Mast JW, Teipner WA. A reproducible approach to the internal fixation of adult ankle fractures: rationale, technique, and early results. Orthop Clin North Am. 1980;11:661-79. [ Links ]
10. Needleman RL, Skrade DA, Stiehl JB. Effect of the syndesmotic screw on ankle motion. Foot & Ankle 1989;10:17-24. [ Links ]
11. Van den Bekerom MP, Haverkamp D, Kloen P. Biomechanical and clinical evaluation of posterior malleolar fractures: a systematic review of the literature. J Trauma 2009;66:279-84. [ Links ]
12. Beumer A, Campo MM, Niesing R, Day J, Kleinrensink GJ, Swierstra BA. Screw fixation of the syndesmosis: a cadaver model comparing stainless steel and titanium screws and three and four cortical fixation. Injury 2005;36:60-64. [ Links ]
13. Tornetta P 3rd, Ricci W, Nork S, Collinge C, Steen B. The posterolateral approach to the tibia for displaced posterior malleolar injuries. J Orthop Trauma 2011;25:123-26. [ Links ]
14. Malhotra K, Wright S, Jeyaseelan L, Singh D. Consensus of the 7th Round Table, Aspects of Foot and Ankle Surgery. Cardiff, September 2017. [ Links ]
15. Drifthout van Hooff CC, Verhage SM, Hoogendoorn, JM. Influence of fragment size and postoperative joint congruency on long-term outcome of posterior malleolar fractures. Foot & Ankle Int. Feb 2015;36(6):673-78. [ Links ]
16. Meijer DT, Doornberg JN, Sierevelt IN, et al. Guesstimation of posterior malleolar fractures on lateral plain radiographs. Injury 2015 Oct;46(10):2024-29. [ Links ]
17. Mason LW, Marlow WJ, Widnall J, Molloly AP. Pathoanatomy and associated injuries of posterior malleolus fracture of the ankle. Foot and Ankle Int. 2017 Nov;38(11):1229-35. [ Links ]
18. Gardner MJ, Brodsky A, Briggs SM, Nielson JH, Lorich DG. Fixation of posterior malleolus fractures provides greater syndesmotic stability. Clin Orthop Rel Res. 2006;447:165-71. [ Links ]
19. Miller AN, Corroll EA, Parker RJ, Boraiah S, Helfet DL, Lorich DG. Direct visualisation for syndesmotic stabilization of ankle fractures. Foot & Ankle Int. 2009;30(5):419-26. [ Links ]
20. Robert V, Mason LW, Harrison E, Molloy A, Mangwani J. Mid-term functional outcomes of reduced and malreduced fractures in two university teaching hosptials. Bone & Joint Journal. 2016;98-B(SUPP 19):16. [ Links ]
 Correspondence:
Correspondence:
Dr MI Workman
Department of Orthopaedics, Old Main Building
Groote Schuur Hospital
Anzio Road, Observatory 7925
Cape Town, South Africa
email: matthew.workman1@gmail.com
tel: +27 83 297 5059
Received: October 2018
Accepted: April 2019
Published: August 2019
Editor: Prof NP Saragas, University of the Witwatersrand, Johannesburg, South Africa
Funding: None.
Conflict of interest: None of the authors have any conflict of interest to declare with respect to this research.
A survey of the management of ankle fractures in South Africa
Dear Colleague
Thank you for taking your valuable time to complete these 10 questions on how you manage minimally displaced ankle fractures. This should take 3 minutes.
1. What is your current position?
A: Medical Officer B: Registrar C: Specialist
2. Years of experience in orthopaedics?
A: less than 5 B: 5-10
C: more than 10
3. How would you treat the fracture below?
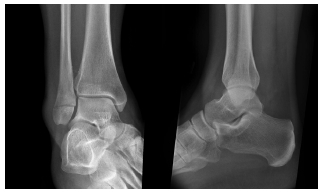
A: Weight-bearing (WB) as tolerated in boot
B: Closed reduction (CR), moulded plaster, non-weight-bearing (NWB) for 6 weeks
C: Open reduction internal fixation (ORIF) with no syndesmotic fixation
D: ORIF with syndesmotic fixation
4. How would you treat the injury below?
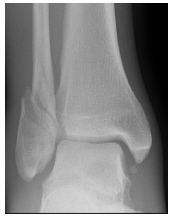
A: WB as tolerated in boot
B: CR, moulded plaster and NWB for 6 weeks
C: ORIF without syndesmotic fixation
D: ORIF with syndesmotic fixation
5. How would you treat the injury below?
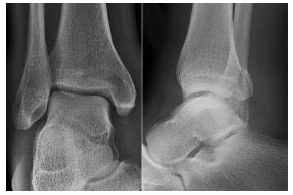
A: WB as tolerated in boot B: CR, moulded plaster and NWB for 6 weeks C: ORIF without syndesmotic fixation D: ORIF with syndesmotic fixation
6. How would you treat the injury below?
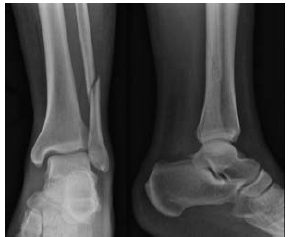
A: CR, moulded plaster and NWB for 6 weeks
B: ORIF with syndesmotic fixation
C: ORIF of posterior malleolus
D: CT scan then ORIF posterior malleolus
7. Would you fix a posterior malleolus fracture of <20% total joint surface area?
A: Yes
B: No
8. Are you comfortable with the posterior approach for fixation of Haraguchi-type fractures?
A: Yes B: No
9. How do you fixate syndesmotic injuries? A: Screw
C: Tightrope D: Combination
10. Do you offer routine screw removal?
A: Yes B: No














