Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SA Orthopaedic Journal
On-line version ISSN 2309-8309
Print version ISSN 1681-150X
SA orthop. j. vol.18 n.2 Centurion May./Jun. 2019
http://dx.doi.org/10.17159/2309-8309/2019/v18n2a2
SPINE
A survey of the use of traction for the reduction of cervical dislocations
Workman ΜII; Kruger NII
IBSc Physio, MBBCh; Registrar, Department of Orthopaedic Surgery, University of Cape Town, South Africa
IIBSc, MBChB, FRCS, FCOrthSA; Consultant, Department of Orthopaedics, Groote Schuur Hospital, University of Cape Town, South Africa
ABSTRACT
BACKGROUND: Literature supports early decompression of low energy cervical spine dislocations. Closed reduction can safely and rapidly achieve this; however, its use and acceptance among specialists is poorly described. This study aimed to assess the training, experience and decision-making of trainees and surgeons who manage cervical spine dislocations with the goal of reinforcing educational programmes as necessary. The objective was to assess the need to implement further training for trainees and specialists involved in the management of cervical spine dislocations
METHODS: Orthopaedic and neurosurgery registrars and specialists in South Africa were emailed a questionnaire consisting of 13 questions related to their training, experience and management of cervical dislocations
RESULTS: Seventy-nine per cent (n=62) of surgeons were taught closed reduction during specialist training. Ninety-two per cent (n=12) of neurosurgeons covered spine trauma compared to 66% (n=42) of orthopaedic surgeons. Of surgeons covering trauma, 21% (n=16) would refer the patient on, accepting a 2-hour delay in treatment. Forty-two per cent (n=5) of neurosurgeons vs <2% (n=1) of orthopaedic surgeons preferred MRI before closed reduction. Fifty-six per cent (n=40) of surgeons thought that the risk of worsening neurology during traction was up to 25%. Sixty-nine per cent (n=54) of surgeons felt emergency room (ER) doctors could safely perform closed cervical reduction with training. Fifty-one per cent of surgeons do not think cervical reduction is routinely possible in under 4 hours
CONCLUSION: The public and specialists have misconceptions around cervical traction which may affect best clinical practice and optimum management. Cervical traction does not require prior MRI and carries a very low risk of worsening a patient's condition. Closed cervical traction reduction is the most rapid, safe mechanism to reduce cervical dislocations and requires specific education of undergraduates, emergency doctors, and specialists to increase awareness of the reduction process
Level of evidence: Level 4
Key words: cervical spine dislocation, closed reduction of cervical spine dislocation, unifacet dislocation, bifacet dislocation
Introduction
Cervical spinal cord injuries (SCI) are a relatively common problem, not only in the Western Cape, but worldwide accounting for 3-6% of all trauma cases.1 They are potentially devastating with high morbidity and poor prognosis if not managed promptly and appropriately.1-5
The major demographic involved in cervical spine dislocations are young male adults.2-5 In South Africa, violence and motor vehicle accidents (MVAs) are the main causes of traumatic spinal cord injury.2,6 Vasiliadis reports that 25% of traumatic SCI are cervical.6 In our institution, bifacet and unifacet dislocations are the most common cause of a cervical SCI,2 and occur most commonly at C5 neurological level.
Cervical dislocations carry a high incidence of devastating neurological injury. Animal models and class III medical evidence support early reduction to improve neurological outcomes. Cervical reduction restores bony canal dimensions and indirectly decompresses the cord. Anecdotally, our experience is that the relatively simple procedure of cervical traction is perceived as a specialist-only procedure that is potentially risky and that specialists have little practice in reductions. In many hospitals, spinal injuries are managed by general orthopaedic or neurosurgeons who are uncomfortable with the procedure, and delays in reduction are common.
In addition to these concerns, a 2015 South African Constitutional Court judgement ruled that all low energy cervical dislocations should be reduced within 4 hours. This has put the spotlight on the emergency management of cervical dislocations, from first emergency response to definitive specialist management.
This study aimed to determine the training, experience and decision-making of orthopaedic and neurosurgical trainees and specialists in the closed reduction of low energy cervical spine injuries. The subject group would also comment on the feasibility of the 4-hour judgement ruling in the South African context. As noted, this information is instrumental in addressing any undergraduate or postgraduate educational needs relevant to cervical reductions as well as highlighting the skill requirements for specialists who provide emergency cover.
Methods
A questionnaire consisting of 13 questions relating to the field of specialisation, training, decision-making and management of cervical dislocations was constructed (see Appendix 1). The hypothetical clinical scenario presented was: a rugby player referred by the emergency room (ER) 2 hours post injury with a C5/6 bifacet cervical dislocation on X-ray and motor complete (ASIA A) neurological injury.
Qualified specialists and registrars in orthopaedics and neurosurgery in South Africa were identified using their respective professional member listings and university registrations. Email databases from the South African Orthopaedic Association, the Society of Neurosurgeons of South Africa and the South African Spine Society were used. The study outline and an online questionnaire link were emailed to all of the above registered specialists and trainees in South Africa. Voluntary participation was requested, and non-responders were sent a single email reminder before closure of the survey. Incomplete survey responses were excluded. No tracking of survey responses was used, and it was completed anonymously.
Data was collected on Excel sheets. A biostatistician was consulted for data analysis.
Results
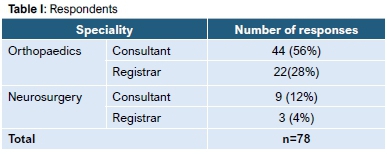
A total of 78 responses were recorded (Table I) from 420 emailed questionnaires (18.6% response rate). These were predominantly from orthopaedic registrars and consultants (84%, n=64). The majority (79%, n=62) of respondents were taught closed reduction during specialist training with the remainder having training during internship or medical officer posts. Ninety-two per cent (n=12) of neurosurgeons cover emergency spine conditions compared to 66% (n=42) of orthopaedic surgeons. Sixty-two per cent (n=47) of respondents had performed or supervised closed cervical spine reduction within the last year.
Of clinicians covering spinal emergencies, 64% (n=52) would confidently perform closed reduction. Twenty-one per cent (n=16) of respondents, however, when presented with a patient with deteriorating neurological deficit, would prefer to refer the patient on and accept a 2-hour delay in reduction. Fifty-six per cent (n=40) thought that the risk of worsening neurology with closed reduction was between 1% and 25% or greater.
Forty-two per cent (n=5) of neurosurgeons and <2% (n=1) of orthopaedic surgeons would require an MRI prior to performing closed cervical spine reduction even though this resulted in a 2-hour delay in treatment. If presented with an MRI showing a herniated cervical disc (disc at risk),7 39% (n=21) of respondents would take the patient urgently to theatre rather than attempt closed reduction. Eighty-one per cent (n=42) of respondents covering spinal emergencies considered that open reduction in theatre in under 4 hours was unachievable, but 48% (n=37) thought closed cervical reduction was feasible in under 4 hours. Sixty-nine per cent (n=54) of respondents felt ER doctors could perform closed cervical reduction if properly trained.
Discussion
The literature shows closed reduction to be safe and effective in 80% of patients. An overall permanent neurological complication rate of 1% is reported.8 Numerous studies favour early reduction to maximise the chance of neurological recovery. On admission to hospital the standard of care for cervical dislocations is urgent closed reduction with skeletal traction. Surgical stabilisation can then occur at the next theatre opportunity without it having to be an emergency procedure. Emergency reduction restores bony canal alignment and offers indirect decompression to the compressed spinal cord.9 This has been shown to have improved outcomes and is supported by animal models and case series of dislocation injuries with class III medical evidence.10-14
This standard of care of urgent closed reduction relates to district hospitals as well as tertiary centres. Not all hospitals have the skills or resources to perform spinal surgery. Where a cervical dislocation presents at a district hospital, the cervical reduction can be performed with minimal equipment and resources. Once reduced, the patient can be transferred to the regional spinal centre where surgical stabilisation and definitive treatment15-21 can take place non-emergently.
The recent South African Constitutional Court Ruling (Oppelt vs Department of Health Provincial Administration: Western Cape) on 14 October 2015, found that the Department of Health was negligent in not performing cervical reduction within 4 hours of the injury.22 This conclusion was based on a single publication from the Conradie Hospital experience of rugby injuries involving 57 players with cervical dislocations. The primary author, Dr Newton, claimed that patients with bilateral cervical facet dislocation sustained in low velocity impact have a 64% chance of a complete recovery if the dislocation was decompressed within 4 hours of the injury. In their conclusions, the authors recommended that cervical dislocations should probably be reduced within 4 hours of injury.23 These findings are controversial especially relating to the 4-hour deadline; however, there are no studies giving contrary evidence and most of the available literature supports early as possible reduction. The 4-hour theory was accepted by the court.
This ruling is particularly important since the Constitutional Court is the highest court in the land and the judgement would be extremely difficult, if not impossible, to overturn. This has far-reaching ramifications involving emergency transport from the accident scene, triage and primary ER management. Subsequent treatment by clinicians including ER doctors and specialists is directly affected by the 4-hour ruling. These issues apply equally to state and private hospitals.
The lay public and courts assume that all specialists covering spinal injuries are competent and skilled in cervical closed reduction. This is incorrect. Of concern is that 21% of specialists in this study had no formal training in cervical reductions at postgraduate level. Undergraduate education was poor with only 2% having had training. Only 62% had performed or supervised a reduction in the past year, which reinforces our view that the procedure is very infrequently performed outside tertiary referral hospitals.
In practice, especially in the private sector, many specialists are orthopaedic or neurosurgical generalists and do not have a specific interest in spinal surgery. They cover emergencies and minor acute spinal conditions such as back pain and sciatica, but certainly would not be comfortable performing cervical reduction. This is borne out by the 21%, who in the clinical case scenario, preferred to refer the patient elsewhere. Non-spinal surgeons do not carry medico-legal specific spinal cover due to the high costs of insurance and there may be concerns that their indemnity would not extend to the management of a cervical dislocation. In communication with insurers (Dr GR Howarth, Medical Protection Society; and JP Ellis, EthiQal Medical Risk Protection, pers. comm.), there was written confirmation that cervical closed reductions are considered non-surgical emergency procedures and would be indemnified even where spinal work is broadly excluded from the orthopaedic surgeon's policy schedule. This indemnification extends to any clinician performing an emergency non-surgical cervical reduction if they have the appropriate training and skill.
In the Western Cape, the average time from injury to ER is 3 hours.24 Under the court ruling that low energy cervical dislocations need to be reduced within 4 hours, the 21% of specialists choosing to refer a patient on (accepting a 2-hour delay in treatment) are putting themselves at risk for medico-legal challenges. We feel it is unacceptable for a specialist entrusted with covering spinal emergencies to be unable to perform closed cervical reduction.
A further concern was the relatively high percentage of surgeons who would request an MRI prior to closed reduction (predominantly neurosurgeons 42% vs orthopaedic 1%). The literature clearly does not support the routine use of pre-reduction MRI. In a qualitative medical evidence-based review published in Neurosurgery 2013,9 the authors concluded that the use of pre-reduction MRI did not improve the safety or efficacy of closed traction-reduction of patients with acute dislocations. There were concerns that an MRI would unnecessarily delay treatment and was not without further risk to the patient.
A significant finding from this study was how the MRI changed surgeon behaviour. When given the scenario of a disc-at-risk on MRI, the percentage of closed reducers declined from 67% to 42%. Of those declining closed reduction, 28% would perform emergent open reduction and 30% would prefer to refer the case on and accept a 2-hour delay in treatment. This is particularly worrying since numerous large clinical series have failed to establish a relationship between pre-reduction disk herniation and subsequent neurological deterioration during closed traction-reduction.25
What is evident, however, is that obtaining an MRI causes delay in treatment, in some instances hours to days.26,27 MRI is not without risk to the patient, who needs to be transferred off the spinal stretcher into and out of the scanner. Treatment is delayed with little useful information being obtained by the MRI. To comply with best clinical practice, an MRI should not be routinely performed pre-reduction.
Twenty-eight per cent of surgeons would perform emergency surgery with a pre-reduction MRI demonstrating a disc at risk. The procedure of choice would be anterior cervical decompression, removal of the disc, and open reduction of the dislocation. Most acute dislocations are able to be safely reduced in this manner. Our concern is that the surgical time taken to perform open reduction would be in excess of 4 hours. If one considers time taken to arrange the MRI, source staff, prepare sets, anaesthetise the patient, drape and proceed ( assuming there is an available theatre waiting), most surgeons would be hard pressed to achieve reduction within 4 hours of injury. From this survey, 54% of surgeons did not think open reduction was feasible within the timeframe.
There was a perception that the risks of worsening neurological status during closed reduction were high. Fifty-one per cent thought the risks could be as high as 25%. Less than half of the respondents (44%) recognised that closed awake cervical reduction carries a very low risk of worsening neurological status (<1%).
Many junior doctors feel cervical reduction is only the domain of specialists. However, in this survey, 69% of respondents felt that an adequately trained ER doctor could perform closed cervical spine reductions.
Most specialists do not stay on site when covering emergencies and often need to travel a distance to the hospital. This is problematic when a cervical dislocation requires urgent management in a very small timeframe. One solution would be to train ER doctors to perform or at least initiate cervical reduction. At the University of Cape Town, our position is that cervical reduction is a cord-saving procedure. It is no less an essential skill than cardiopulmonary resuscitation, intercostal drain insertion and intubation. These skills are taught to every medical doctor as part of the MBChB curriculum. The UCT orthopaedic department includes cervical traction reduction as standard teaching to all medical students.
The Constitutional Court judgement is controversial among specialists. Many consider it to be based on weak evidence and impractical to implement. Most ERs, especially in state hospitals, are inundated with severe life-threatening injuries, and many patients need to wait several hours for management. With the court judgement, there is now increased pressure to prioritise cervical dislocations ahead of other critically injured patients, presenting an ethical dilemma to clinicians. We are unaware of any other court judgement worldwide where a specific timeline has been applied to the reduction of low energy cervical dislocations.
In this survey, 78% of specialists did not agree with the judgement ruling. Of concern, was that 19% were unaware of the ruling. This is staggering, given the Constitutional Court's enormous award of R19 000 000 damages to the plaintiff for delayed reduction. It would be anticipated that the various hospital groups would align their management of cervical dislocations to the time limitations, set up protocols, educate staff and acquire the relevant low-cost equipment. To our knowledge this has only happened in the state sector in the Western Cape, where policy changes and educational programmes have been put in place.
In its judgement media summary, the minority judgement acknowledged that Dr Newton's 4-hour theory was new, unpublished, and unknown at the time of the plaintiff's injury in 2002.22 That is no longer the case and the enormous implications of this ruling should be clearly understood by every hospital manager, emergency response services and medical staff dealing with these injuries.
This study primarily aimed to identify what percentage of orthopaedic and neurosurgery specialists and registrars would be able to reduce a cervical spine dislocation within 4 hours of referral, with the aim of implementing further training for both specialists and ER doctors. As depicted in Figure 1, only 49% of respondents envisage achieving this end point, highlighting the necessity for education, training and establishment of protocols.
This survey targeted all specialists managing cervical spine trauma. As noted above, the response was poor from both neurosurgical specialists and registrars (16% of the sample size despite channelling their surveys through the Spinal Society, Neurosurgical Society and medical schools), which may have biased the results in terms of a smaller sample size from this group. This is particularly disappointing considering that in South Africa, a greater proportion of neurosurgeons practise spinal surgery than orthopaedic surgeons, and cervical dislocation management is very relevant to them. A strong response was, however, recorded from orthopaedic specialists and registrars, with comparable answers indicating a similar approach to the management of this condition.
There may have been bias with a higher response rate from the authors' institution (University of Cape Town) respondents, who would naturally align themselves with the authors' teaching and viewpoints. This may explain the relatively high reported rate of cervical reductions (60% reductions in previous year) which does not match our anecdotal observations of the cervical reduction rates outside of the teaching hospitals. This bias effect may have increased the pro-reduction percentage and the proportion who would not perform MRI scan.
Unfortunately, being an anonymous survey, we were not permitted to track where respondents practised or trained, nor could we establish the percentage response from different universities. Thus, it is important to note that there may well be a much higher percentage of clinicians who are not comfortable with cervical spine reduction, who think an MRI pre-reduction is indicated and who are not aware of the court's 4-hour ruling.
In this survey, 69% supported closed reduction by trained ER personnel. This is an important component of acute care since ER doctors are on-site and in the event of a patient presenting with a cervical dislocation, they can immediately commence calliper application and initiation of the reduction process. Since time is of critical importance, delays for off-site specialists are avoided.
It follows from the above that education of medical personnel in the emergent closed reduction of cervical spine dislocations is vital. This is already part of the undergraduate curriculum at the University of Cape Town as we consider this to be a generalist essential skill. ER doctors should have competency in cervical spine assessment and reductions. Specialists covering spinal emergencies need to be comfortable performing reductions. Hospital managers have a burden of responsibility to provide protocols for cervical reductions, have reduction equipment sets readily available, and ensure all staff are knowledgeable about the time constraints.
Conclusion
This survey demonstrates misconceptions around cervical traction which may compromise optimum management. Only 67% of specialists would perform urgent reduction in the most urgent of case scenarios. MRI in acute facet dislocation is still being employed against recommendations. Surgeons are less inclined to perform closed reduction after MRI and in this survey, a significant proportion would not primarily manage the patient, thus incurring a further 2-hour delay. Most surgeons are comfortable with ER doctors managing cervical reductions and do not agree with the Constitutional Court ruling. In the Western Cape, with an average travel time of 3 hours to ER, there are unreasonable time constraints placed by the court ruling and unfair priority given to cervical dislocations over other critically injured patients. For the present however, a legal requirement remains around the management of low energy cervical dislocations and clinicians need to adhere to best clinical practice.
Ethics statement
This research was approved by the University of Cape Town Department of Surgery Research committee (2016/024) and the University of Cape Town Faculty of Health Sciences Ethics Committee (HREC/REF:310/2016).
The authors declare that this submission is in accordance with the principles laid down by the Responsible Research Publication Position Statements as developed at the 2nd World Conference on Research Integrity in Singapore, 2010.
Declaration
The authors declare authorship of this article and that they have followed sound scientific research practice. This research is original and does not transgress plagiarism policies.
Acknowledgements
Mr Michael McCaul, biostatistician, Department of Biostatistics, Stellenbosch University, South Africa.
Author contributions
MW contributed to proposal write-up, data collection and analysis, and final write-up of manuscript. NK contributed to original study concept and conceptualisation, design, data collection and analysis, and write-up of final manuscript.
References
1. Ghafoor AU, Martin TW, Gopalakrishnan S, Viswamitra. Caring for the patients with cervical spine injuries: what have we learned? Journal of Clinical Anaesthesia Jan 2006;17(8):640-49. [ Links ]
2. Fielingsdorf K, Dunn RN. Cervical spine injury outcome - a review of 101 cases treated in a tertiary referral unit. SAMJ Mar 2007;97(3):203-207. [ Links ]
3. Frankel HI, Coll JR, Charlifue SW etal. Long-term survival in spinal cord injury: A fifty-year investigation. Spinal Cord 1998;36:247-56. [ Links ]
4. Gerhart KA. Spinal cord injury outcomes in a population-based sample. J Trauma 1991;31:1529-35. [ Links ]
5. Vaccaro AR, Daugherty RJ, Sheehan TP, et al. Neurologic outcome of early versus late surgery for cervical spinal cord injury. Spine 1997;22:2609-13. [ Links ]
6. Vasiliadis AV. Epidemiology map of traumatic spinal cord injuries: A global overview. International Journal of Caring Sciences. Sept 2012;5(3):335-47. [ Links ]
7. Fleming MA, Westgarth-Taylor T, Candy S, Dunn R. How does pre-reduction MRI affect surgeons' behaviour when reducing distraction-flexion (dislocation) injuries of the cervical spine? SAOJ 2015;14:42-46. [ Links ]
8. Initial closed reduction of cervical spine fracture-dislocation injuries. In: Guidelines for the management of acute cervical spine and spinal cord injuries. Neurosurgery 2002 Mar;50:S44-50. [ Links ]
9. Gelb DE, Hadley, MN, Dhall SS, Hurlbert RJ, Rozzelle CJ, Ryken TC, Theodore N, Walters BC. Initial closed reduction of cervical spine fracture-dislocation injuries. Neurosurgery 2013;72:73-83. [ Links ]
10. Ackland H. The Alfred Spinal Clearance Management Protocol. The Alfred National Trauma Research Institute, Melbourne. Updated June 2006. [ Links ]
11. Hadley MN, Walters BC, et al. Guidelines for the Management of Acute Cervical Spine and Spinal Cord Injuries. Section on Disorders of the Spine and Peripheral Nerves of the American Association of Neurological Surgeons and the Congress of Neurological Surgeons 2013. [ Links ]
12. Rathore FA. Spinal cord injuries in the developing world. International Encyclopedia of Rehabilitation. 2013 - Centre for International Rehabilitation Research Information and Exchange (CIRRIE). [ Links ]
13. Como JJ, Diaz JJ, Dunham M, Chiu WC, Duane TM, et al. Practice Management Guidelines for Identification of Cervical Spine Injuries Following Trauma: Update from the Eastern Association for the Surgery of Trauma Practice Management Guidelines Committee. J Trauma 2009;67:651-59. [ Links ]
14. Pimentel L, Diegelmann L. Evaluation and management of acute cervical spine trauma. Emerg Med Clin N Am 2010;28:719-38. [ Links ]
15. Hagen EM, Rekand T, Gilhus NE, Grunning M. Traumatic spinal cord injuries- incidence, mechanisms and course. Tidsskr Nor Legeforen 2012;132(3):831-37. [ Links ]
16. Cervical Traction. Department of Orthopaedic Surgery - University of Stellenbosch, South Africa. Website: www0.sun.ac.za/ortho/webct-ortho/general/trac/trac-3.html Accessed on 1 July 2013. [ Links ]
17. Miller MD, Thompson SR, Hart J. Review of Orthopaedics, 6th Edition. Elsevier Philadelphia 2012. [ Links ]
18. Flyn JM. Orthopaedic Knowledge Update 10. American Academy of Orthopaedic Surgeons 2011 Rosemont IL. [ Links ]
19. Kleyn PJ. Dislocation of the cervical spine: closed reduction under anaesthesia. Paraplegia 1984;22:271-81. [ Links ]
20. Cotler HB, Miller LS, DeLucia FA, Cotler JM, Davne SH. Closed reduction of cervical spine dislocations. Clin Orthop Relat Res 1987 Jan;214:185-99. [ Links ]
21. Papadopoulos SM, Selden NR, Quint DJ, Patel N, Gillespie B, Grube S. Immediate spinal cord decompression for cervical spinal cord injury: feasibility and outcome. Journal of Trauma and Acute Care Surgery 2002 Feb;52(2):323-32. [ Links ]
22. Constitutional Court of South Africa Case CCT 185/14 In the matter between: Charles Oppeld Applicant and Head: Health, Department of Health Provincial Administration Western Cape. [ Links ]
23. Newton D, England M, Doll H, Gardner BP. The case for early treatment of dislocations of the cervical spine with cord involvement sustained playing rugby. J Bone Joint Surg Br. 2011 Dec;93(12):1646-52. [ Links ]
24. Potgieter MSW, Davis J. A review of the success of reduction of cervical facet dislocation in Tygerberg hospital. Presented COMOC 2016, Cape Town, South Africa. Currently submitted for publication. [ Links ]
25. Vaccaro AR, Falatyn SP, Flanders AE, Balderston RA, Northrup BE, Cotler JM. Magnetic resonance evaluation of the intervertebral disc, spinal ligaments, and spinal cord before and after closed traction reduction of cervical spine dislocations. Spine 1999;24(12):1210-17. [ Links ]
26. Tomycz ND, Chew BG, Chang YF, Darby JM, Gunn SR, Nicholas DH, Ochoa JB, Peitzman AB, Schwartz E, Pape HC, Spiro RM, Okonkwo DO. MRI is unnecessary to clear the cervical spine in obtunded/comatose trauma patients: the four-year experience of a Level I trauma center. J Trauma. 2008;64:1258-63. [ Links ]
27. Battistuzzo CR, Armstrong A, Clark J, Worley L, Sharwood L, Lin P et al. Early decompression following cervical cord injury: Examining the process of care from accident scene to surgery. Journal of Neurotrauma 2016 Jun 15;33(12):1161-69. [ Links ]
 Correspondence:
Correspondence:
Dr MI Workman
Department of Orthopaedics, Old Main Building, Groote Schuur Hospital
Anzio Road, Observatory 7925, Cape Town, South Africa
email: matthew.workman1@gmail.com
tel: +27 83 297 5059
Received: June 2018
Accepted: November 2018
Published: May 2019
Funding: This research received no funding.
Conflict of interest: Both authors have no conflicts of interest to declare.
Appendix 1
Survey questionnaire
Skeletal traction for cervical dislocations: perceptions and use among specialists in South Africa
Dear Colleague,
As you may be aware, the recent Constitutional Court of South Africa has placed a 4-hour timeframe on the reduction of low energy cervical reductions with huge medico-legal ramifications. This study is an effort to measure the training, perceptions and experience of the specialists and registrars who are tasked with these reductions.
Thank you for taking your valuable time to complete this survey of 13 questions which should take 5 minutes to complete.
1. What is your registered speciality?
Orthopaedic surgeon
Neurosurgeon
Orthopaedic registrar
Neurosurgery registrar
2. Describe your formal training in the use of cervical traction:
None
Undergraduate training
Internship or medical officer level
During specialist orthopaedic or neurosurgical training
Refresher course or lectures post specialisation
3. Describe your practice:
Registrar
State employed specialist
State/private practice
Private practice
4. Categorise your practice:
Do not do emergency cover
Cover emergency general orthopaedics/neurosurgery and spinal conditions
Cover emergency general orthopaedics/neurosurgery but not spinal conditions
5. After hours: If presented with an acute cervical dislocation from the emergency room, choose the most applicable option:
I treat spine emergencies and would manage a cervical dislocation with closed traction myself
I treat spine emergencies but would rather refer the patient to a colleague for closed reduction
I don't treat any spine emergencies and would refer the patient to a colleague for treatment
6. Give an indication of your medico-legal insurance status:
I have spine cover and would perform cervical reduction in an emergency
I have no spine cover and would perform cervical reduction in an emergency
I have spine cover and would not perform cervical reduction in an emergency
I have no spine cover and would not perform cervical reduction in an emergency
7. How many closed cervical reductions did you perform or supervise in the last year?
0
<5
>5
I do not treat emergency spine conditions and would refer to a colleague
8. A rugby player is referred by your emergency room 2 hours after injury with a C5/6 bifacet cervical dislocation diagnosed on X-rays, motor complete (Frankel A). Your immediate management is:
Closed cervical skeletal traction reduction
MRI before closed reduction
Urgent theatre without MRI
Urgent theatre after MRI
Refer to a specialist who covers spine conditions accepting that is will involve a further 2-hour delay
9. The same rugby player who presented within 2 hours of a C5/6 bifacet cervical dislocation diagnosed on X-rays, motor complete (Frankel A), has an MRI pre-reduction which shows an uncontained herniated cervical disc (disk at risk). Your management is:
Closed reduction
Urgent theatre
Refer to a specialist who covers spine conditions accepting that is will involve a further 2-hour delay
10. What is the shortest time you envisage you would be able to surgically open reduce a dislocated cervical spine after receiving the telephone call from the emergency room? Consider pre-operative imaging, arranging theatre and an anaesthetist, requesting sets, travel time, set-up in theatre and scrubbing etc?
< 4 hours
>4 hours
Non-spinal surgeon
11. In a cervical dislocation with normal or partial neurology, what do you feel is the risk of causing the neurological level to deteriorate during closed cervical traction reduction?
>50%
25-50%
1-25%
<1%
12. Do you feel an adequately trained emergency room doctor is competent to perform a closed cervical skeletal traction reduction if indicated?
Yes - with proper training
No - it is only a specialist procedure
13. In your practice, would you be able to reduce a cervical spine dislocation within 4 hours of referral?
No - I do not treat emergency spine conditions
No - This time frame is too short
Yes - by performing closed cervical skeletal traction
Yes - by performing surgical open reduction














