Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SA Orthopaedic Journal
On-line version ISSN 2309-8309
Print version ISSN 1681-150X
SA orthop. j. vol.17 n.1 Centurion Feb./Mar. 2018
http://dx.doi.org/10.17159/2309-8309/2018/v17n1a1
ARTHROPLASTY
Comparing outcomes between enhanced recovery after surgery and traditional protocols in total hip arthroplasty: a retrospective cohort study
Immelman RJI; de Vos JNII; Venter JHIII
IMBChB(Pret), Registrar in Orthopaedic Surgery, University of Pretoria
IIMBChB(Pret) MMed Orth(Pret), Orthopaedic Surgeon, Wilgers Hospital, Pretoria
IIIMBChB(Pret) MMed Int(Pret), Specialist Physician, Wilgers Hospital, Pretoria
ABSTRACT
BACKGROUND: Traditionally, hip replacement surgery was associated with prolonged recovery and rehabilitation in a hospital setting. Prolonged stay is causing growing concern internationally, where there is an increased drive to cost-effective practice and a realisation that prolonged hospitalisation is not required and may be detrimental. Enhanced Recovery After Surgery (ERAS) protocols address this problem by advocating evidence-based multidisciplinary peri-operative management pathways associated with rapid recovery, without compromising safety. Despite proven efficacy, these protocols are not being implemented in most South African orthopaedic practices.
METHODS: Data from two cohorts (80 patients) undergoing elective primary total hip arthroplasty were included. One group was rehabilitated according to a prolonged stay protocol and the other according to ERAS. Cohorts were matched according to demographics and comorbidities. The functional outcome was compared using the Oxford Hip Score. The 30-day readmission rate was compared to assess the safety of early discharge, and the length of stay of patients was compared.
RESULTS: The readmission rate and Oxford Hip Scores showed no clinically significant difference between the cohorts. The length of stay was markedly decreased in the ERAS group.
CONCLUSION: ERAS protocols can decrease the length of stay in elective total hip replacement without compromising patient safety or functional outcome.
Level of evidence: Level 4.
Key words: ERAS, enhanced recovery, rapid recovery, total hip replacement, arthroplasty
Introduction
Osteoarthritis is a chronic progressive and debilitating disease caused by articular cartilage wear and destruction. Total hip arthroplasty has proved to be a reliable, effective, reproducible and sustainable method of treatment for this disease process. Health-related quality of life assessments have shown that return to function after arthroplasty, and especially after primary total hip arthroplasty, is excellent and that the money spent on these procedures is justified. With the incidence of arthritis on the rise, it is expected that the incidence of total hip replacements will also rise by 174% by 2030, putting these surgeries and the approach towards them in the spotlight.1-3
Length of stay after total hip arthroplasty varies drastically across the literature, ranging between one and 21 days. The trend is that of a decreasing length of stay. Traditionally, in South Africa, the teaching and protocols followed were that of a longer length of stay ranging between four and seven days, with delayed and prolonged hospital mobilisation and rehabilitation. While this is still an accepted method of treatment with excellent outcomes, very little attention is given to new or alternative protocols.2
Enhanced Recovery After Surgery (ERAS) is a concept popularised in the early 2000s by Henrik Kehlet from Denmark. ERAS is an evidence-based peri-operative care pathway that emphasises and advocates pre-, intra- and post-operative interventions that are associated with enhanced recovery and decreased length of stay without compromising patient care. These protocols were originally developed specifically for gastroenterology but have been modified and tailored by the original task team, as well as multiple other authors, to be applied to other surgical procedures. In and around 2010, ERAS found its way into arthroplasty surgery with many European and American centres applying these protocols with success. Results by multiple authors have shown a significant decrease in length of stay without compromising outcome and patient safety. Outcomes with post-operative hip scores were equal and, in certain cases, showed improvement, with readmission rates decreasing in the rapid recovery pathways.4-6
When assessing a new rehabilitation protocol, there has to be certainty that the change does not negatively affect the quality of care and outcome. This implies that the minimal acceptable results are at least equivalent to the results of the previous method. When assessing outcome in joint replacement, one has to compare functional outcome and assess complication rate. In arthroplasty, functional outcome is measured by various scoring systems, with the Harris and Oxford Hip Scores being the most commonly used, validated scoring systems.7 Readmission rate is the accepted way of determining relevant complications requiring intervention. As a result of the early discharge of these patients, this is the most reliable way of determining complications that require intervention, and these can be considered more significant complications. A concern of the ERAS protocol is that patients are rehabilitated and discharged too early, and therefore many complications that could have been prevented, or diagnosed earlier, are now only presenting later with a worse prognosis and unnecessary readmission.116189
The aim of this study is to show that an ERAS protocol can be implemented so as to decrease length of stay without compromising on patient outcome or safety.
Materials and methods
This study was conducted retrospectively in the form of a cohort study, at the practice of the senior author. The institution is a private healthcare hospital setting, situated in Pretoria. This hospital draws many patients from rural Mpumalanga, as well as surrounding Pretoria. Files were reviewed assessing various patient demographics, comorbidity profile and surgical factors in view of comparing cohorts. The main outcomes, readmission rate and post-operative Oxford Hip Scores, were also collected and compared. The Oxford Hip Scores (OHS) were calculated at least six months post-operatively in all patients.
All patients undergoing primary elective total hip replacement were included in this study. The senior author changed practice during this time to an ERAS pathway. Consequently, all patients after the change were assigned to the ERAS group without selection. All patients before the change were assigned to the traditional group, also without selection. The only exclusion criteria were an incomplete file and less than six months' postoperative follow-up. A total number of 80 patients were included for analysis and divided into two cohorts, consisting of 40 patients each.
Data collection for the ERAS group was conducted in a retrospective manner starting on 1 May 2015. This coincided with the senior author changing to an ERAS protocol. At this stage, all patients without any selection, were treated with the ERAS protocol. On consultation with statisticians, the size of the cohorts was determined to be 40 patients in each cohort to achieve statistical significance. The first 40 patients being treated with an ERAS protocol and having at least six months' follow-up were included. Subsequently, the last 40 patients before the change in protocol were included in the traditional group. The data collection period was from 13 October 2014 to 12 March 2016. All patients were followed up for 30 days post-operatively for readmissions, and OHS was done at least six months post-operatively.
All patients had identical surgical treatment. This consisted of a primary total hip replacement done in the lateral decubitus position. The same surgical approach, Hardinge direct lateral, was used. All patients were treated with prostheses, with the same design and from the same manufacturer. This included an uncemented press fit stem and cup.
The difference in approach to these cohorts was the clinical pathway used in each group. As mentioned, ERAS contained pre-, intra- and post-operative components (Table I).
Pre-operative changes included allowing clear fluids up to two hours pre-op, omission of sedative premedication, prophylactic antiemetic (odansetron) and multimodal non-opioid analgesia. Analgesia premedication included two days of oral pregabalin and intravenous ketorolac and paracetamol two hours pre-operatively. The patients also received a crystalloid fluid bolus.
Intra-operatively, changes were mainly pharmaceutical and type of anaesthetic. All patients received spinal anaesthetic. Only if this failed, general anaesthetic was utilised. Opioids were avoided both intravenously and within the spinal block. Patients received conscious sedation and benzodiazepines were replaced by a low dose propofol infusion. Bladder catheterisation was avoided if possible. This unfortunately was necessary at times, but the catheter was removed in theatre post-op or on arrival in the ward. During wound closure, local infiltrative anaesthesia was utilised.
Post-operatively, the patients were not sent to high care, which was previously the case for 1-2 days. Patients were allowed a normal diet directly post-operatively. Previously only clear fluids were administered on day 0, fluids on day 1 and then a normal diet on day 2. The patients received no parenteral opioids, and surgical drains were removed within 12 hours of surgery. Patients were mobilised within 2-4 hours post-op, this included getting out of bed, and mobilising in the ward and out of the room - all under physiotherapy supervision. Day 1 mobilisation included mobilising out of the ward and stair climbing, again with physiotherapy supervision. Ice packs were used over the dressing to minimise swelling. Mobilisation in the traditional cohort was delayed and less aggressive (Table I).
Discharge criteria were similar with the two groups. The only difference was that there was less reliance placed on blood results in the ERAS group. Daily bloods were done to monitor renal functions, haemoglobin and inflammatory markers in the traditional group. Patients were only discharged once the CRP was on a downward trend. This was usually only noted on day 4 to 5. Except for the medical reason stated above, surgical and physiotherapy or mobilisation criteria were identical in both groups. The patient was required to be able to mobilise and cope with their outside environment; pain should be controlled; there should be no medical reasons against discharge; and the wounds and swelling were to be judged as adequate by the surgeon.
Prior to commencing data collection, ethical approval was obtained from the University of Pretoria's Research Ethics Department.
Results
The results were analysed by the Department of Statistics at the Medical Research Council.
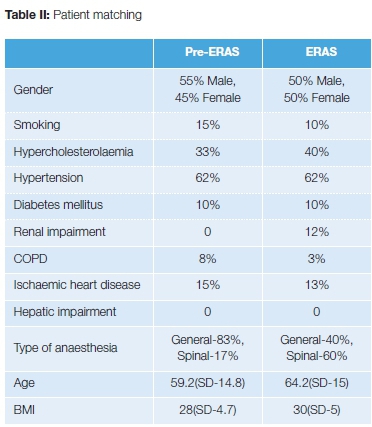
The two cohorts were well matched according to demographics and comorbidity profiles (Table II). Only three variables, namely, the type of anaesthetic, body mass index (BMI) and age stood out and reflected a difference. With regard to the type of anaesthetic in the traditional group, general anaesthetic was favoured, and in ERAS, spinal anaesthetic was preferred. This is in keeping with the ERAS protocol that favours regional anaesthetic. The mean age of the ERAS group was also five years older at 64.2 years (SD 14.8), compared to 59.2 (SD 15). Lastly, the ERAS group had a mean BMI of 30 (SD 5) kg/m2 which was 2 kg/m2 higher than the traditional group at 28 (SD 4.7) kg/m2.
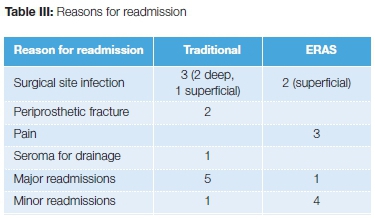
With regard to readmission rate, the ERAS group had a lower readmission rate than the traditional group; however, this was not statistically significant (P-value 0.75). The reasons for readmission were subsequently evaluated (Table III) and divided into major and minor according to the American College of Surgeons' National Surgical Quality Improvement Program (NSQIP). The NSQIP is a database validated in orthopaedic surgery and has been in existence for more than 30 years.10 Major complications encountered are generally complications requiring return to the operating room (periprosthetic infections and fractures) or more serious or life-threatening medical complications such as myocardial infarct, organ failure, stroke and pulmonary embolism. Major complications are associated with prolonged hospital stay and major increases in cost. Major complications encountered in our study included deep surgical site infection, peri-prosthetic fracture requiring surgery, and seroma requiring drainage in theatre. Minor complications include complications that generally do not markedly add to morbidity or return to the operating theatre; these include urinary tract infection, superficial surgical site infection, DVT, blood loss requiring transfusion, and pneumonia.10,11,17 Once the severity of the complications was determined, the ERAS group's major readmission equated to one readmission and the traditional group five. There were three readmissions for pain during early implementation of ERAS. There were no mortalities in either cohort.
The Modified Oxford Hip Scores (out of 60) showed no statistically significant difference. All patients in both groups had an excellent outcome7 with scores ranging between 58 and 60. The mean score in the traditional group was 60 (range 59-60) and the ERAS group 59.7 (range 58-60). Of note is that the traditional group's scores were taken on average 9-12 months after surgery and the ERAS group 6 months. This is due to the timeline of data collection where the traditional cohort had longer follow-up.
Length of stay (LOS) was compared and showed a statistically significant decrease in the ERAS group (P-value 0.0011). The mean LOS was 6.95 (3-59) days in the traditional group, compared to 1.85 (1-7) days in the ERAS group. Two patients in the traditional group had exceptionally long stays, 59 and 24 days, for prosthetic joint infection and pneumonia respectively. If these patients were removed from the cohort, the LOS mean in this group decreased to 5.13 days.
Discussion
Clinical pathways or rehabilitation protocols lack a definition in orthopaedic literature but can be described as a set of orders or interventions determined to standardise the treatment of patients and which aim to optimise a positive outcome. Comparing these protocols with one another is exceedingly difficult, as they consist of multiple interventions which function as cogs in a machine. Isolating and determining the weight each component contributes to outcome, is currently not possible, and further research into the topic is required.12
ERAS is one such pathway. The difference in philosophy between ERAS and other pathways is not major, but definitely significant. First, in ERAS the emphasis placed on the multi-disciplinary approach is fundamentally different from other protocols. In ERAS, each member is tasked with periodically reviewing the best available and up-to-date literature and formulating a plan to implement this. Each member of the team also contributes to the education of patients and the team. Secondly, outcomes criteria are mandated by ERAS. These outcomes should be prospectively defined and collected; they should be comprehensive and used to regularly evaluate and improve care. Lastly, ERAS requires a regular audit of outcomes. This audit process should involve all practitioners and should be critical concerning shortcomings. During audit, the team should re-evaluate interventions and review literature to ascertain if the current approach is still up to date with trends. This process in effect ensures that the ERAS pathway is not a static pathway, but rather constantly evolving towards the newest and highest level of evidence.12,13
The effects of this audit process are evident when considering results in our ERAS cohort. In the ERAS cohort, during the early phase of implementation, three patients (7.5%) of the cohort were readmitted due to pain. One of these patients was admitted in another hospital in the periphery and transferred, the other two at the treating institution. All three patients were not assessed or discussed with an orthopaedic surgeon prior to admission. Sibia et al. showed that pain or swelling was the most common reason for re-presentation to hospital within 30 days in their 655 patients.16 In their study, they divided hospital returns into readmissions and emergency department visits. Emergency department visits were 75% more common than readmissions. As a result of uncertainty regarding the treatment course of patients after total joint arthro-plasty (TJA), and possibly due to the litigious nature of the current healthcare system, these patients are often readmitted by general practitioners or casualty officers. This trend was noted, and pre-operative education and discharge medications were adjusted in an attempt to avoid this situation and improve on post-discharge pain management. This has resulted in no further readmissions for pain in 91 consecutive total hip arthroplasties (THAs) up to the time of the writing of this article. Changes in education included emphasis on post-operative pain and asking patients to call the surgeon's room if pain is not bearable after discharge. The discharge analgesia also included stronger opioid-containing medication to be taken on a pro re nata (PRN) basis.
The study presented similar results when compared to many other studies and showed that ERAS or rapid recovery protocols can be safely implemented and do not compromise outcome. Although this was the aim of the study, several other findings were made. First is the concept of patients at risk, or specific characteristics associated with prolonged stay. It was clear in our study that patients with a length of stay exceeding two days presented common characteristics. These included advanced age (>75 years), high BMI (>30 kg/m2) and comorbidity profile, which was especially relevant if LOS was three or more days (Table IV). This correlated well with a review by Kehlet et al., that certain characteristics are associated with prolonged stay in ERAS.
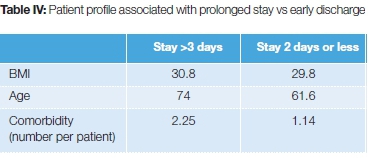
Of note is that Kehlet's review shows that these patients, with more comorbidities, a higher age and BMI are predominantly the patients who benefit most from ERAS. Their LOS, morbidity and mortality rates as a group, show the greatest improvement when ERAS is applied compared to prolonged stay. It is thus imperative to understand that ERAS does not equate to early discharge, but rather earlier and safer discharge for a specific patient profile without compromising clinical outcome.6,9,12,13,15
Discharge criteria are becoming more important to ensure safety, minimise readmission and maximise outcome. Discharge criteria are of pivotal importance in recognising complications and preventing unsafe discharge. Hospital-acquired conditions (HAC) is a term described by Medicaid in the USA as a condition or complication acquired in hospital, specifically due to admission or interventions that are potentially avoidable. The most common HACs in arthroplasty are, in order of frequency, urinary tract infection, surgical site infection, venous thromboembolism and pneumonia. The presence of a HAC is the strongest predictor of early readmission following arthro-plasty. Recognition of these HACs is the responsibility of the surgeon via set criteria and, if recognised prior to discharge, can decrease readmission rate four-fold.16 Avoiding readmission is key as up to 39% of patients readmitted after THA require surgical intervention.14 The discharge approach followed in this study is congruent with ERAS philosophy and includes a team approach. This concept is not new but emphasises input from all team members in assessing readiness for discharge. Both medical and surgical parameters are assessed by the main role players, namely the surgeon, physician, physiotherapist and nursing staff, with the anaesthetist being the only part of the team not involved in discharge. Our approach simplified, included that there should be no surgical or medical reason not to discharge the patients, and the patients should be able to mobilise unaided out of bed and on stairs, and be able to dress and take care of basic personal hygiene.
Traditionally, length of stay after TJA ranges between four and seven days. This LOS was often required to achieve adequate mobility and due to concerns about high rates of complications in the post-operative period. Parvizi stated that the vast majority of complications in TJA are recorded within the first four days, prompting many surgeons to monitor patients for longer in hospital.18 What should be taken cognisance of is that Parvizi's cohort included both knee and hip primary and revision surgery as well as bilateral surgeries. The vast majority of complications were noted in the revision arthroplasties and knee arthroplasties and not in primary hip arthroplasties. Recent literature, including new literature by Parvizi, indicates that these complications are not easily preventable, and that shorter hospital LOS may be protective against readmission and some of these complications, or at the least give equivalent results to longer stay.19,20 The effect of early mobilisation, regional anaesthetic and multimodal, non-opioid analgesia has in turn played a major role in decreasing LOS without increasing morbidity.21
Limitations in this study include the retrospective nature and limited number of patients. Prospective matching of cohorts was thus not done, although the groups happened to be well matched in most aspects due to the specific patient profile undergoing arthroplasty. Treatment of the two cohorts did not run concurrently; this could have had an effect due to possible changes in unknown factors such as hospital and supporting staff caring and managing patients.
Conclusion
Implementation of evidence-based ERAS pathways that are diligently monitored will lead to safe discharge without compromising clinical outcome. In South African healthcare systems, which are hampered by many constraints, implementation of these protocols can go a long way towards improved service delivery by improving turnaround time and saving costs.
Ethics statement
Prior to commencing data collection, ethical approval was obtained from the University of Pretoria's Research Ethics Department.
References
1. Berry DJ, Lieberman J. Surgery of the hip. Elsevier Health Sciences; 2012. [ Links ]
2. Michaud CM, McKenna MT, Begg S, Tomijima N, Majmudar M, Bulzacchelli MT, et al. The burden of disease and injury in the United States 1996. Population health metrics 2006;4(1):1. [ Links ]
3. Ethgen O, Bruyere O, Richy F, Dardennes C, Reginster JY. Health-related quality of life in total hip and total knee arthroplasty. A qualitative and systematic review of the literature. J Bone Joint Surg Am 2004 May;86-A(5):963-74. [ Links ]
4. Kehlet H, Dahl JB. Anaesthesia, surgery, and challenges in postoperative recovery. The Lancet 2003;362(9399):1921-28. [ Links ]
5. Kurtz S, Ong K, Lau E, Mowat F, Halpern M. Projections of primary and revision hip and knee arthroplasty in the United States from 2005 to 2030. J Bone Joint Surg Am 2007 Apr;89(4):780-85. [ Links ]
6. Callaghan JJ, Pugely A, Liu S, Noiseux N, Willenborg M, Peck D. Measuring rapid recovery program outcomes: are all patients candidates for rapid recovery. J Arthroplasty 2015;30(4):531-32. [ Links ]
7. Halawi MJ. Outcome measures in total joint arthroplasty: current status, challenges, and future directions. Orthopedics 2015;38(8):e685-e689. [ Links ]
8. Dawson-Bowling SJ, Jha S, Chettiar KK, East DJ, Gould GC, Apthorp HD. A multidisciplinary enhanced recovery programme allows discharge within two days of total hip replacement; three-to five-year results of 100 patients. Hip International 2014;24(2). [ Links ]
9. Jorgensen CC, Kehlet H, Lundbeck Foundation Centre for Fast-track Hip and Knee Replacement Collaborative Group. Role of patient characteristics for fast-track hip and knee arthroplasty. Br J Anaesth 2013 Jun;110(6):972-80. [ Links ]
10. Pugely AJ, Callaghan JJ, Martin CT, Cram P, Gao Y. Incidence of and risk factors for 30-day readmission following elective primary total joint arthroplasty: analysis from the ACS-NSQIP. J Arthroplasty 2013;28(9):1499-504. [ Links ]
11. Ingraham AM, Richards KE, Hall BL, Ko CY. Quality improvement in surgery: the American College of Surgeons National Surgical Quality Improvement Program approach. Adv Surg 2010;44: 251-67. [ Links ]
12. Soffin E, YaDeau J. Enhanced recovery after surgery for primary hip and knee arthroplasty: a review of the evidence. Br J Anaesth 2016;117(suppl 3):iii62-iii72. [ Links ]
13. Scott NB, McDonald D, Campbell J, Smith RD, Carey AK, Johnston IG, et al. The use of enhanced recovery after surgery (ERAS) principles in Scottish orthopaedic units-an implementation and follow-up at 1 year, 2010-2011 : a report from the Musculoskeletal Audit, Scotland. Arch Orthop Trauma Surg 2013;133(1):117-24. [ Links ]
14. Sibia US, Mandelblatt AE, Callanan MA, MacDonald JH, King PJ. Incidence, risk factors, and costs for hospital returns after total joint arthroplasties. J Arthroplasty 2017;32(2):381 -85. [ Links ]
15. Stambough JB, Nunley RM, Curry MC, Steger-May K, Clohisy JC. Rapid recovery protocols for primary total hip arthroplasty can safely reduce length of stay without increasing readmissions. J Arthroplasty 2015;30(4):521 -26. [ Links ],
16. Raines BT, Ponce BA, Reed RD, Richman JS, Hawn MT. Hospital acquired conditions are the strongest predictor for early readmission: an analysis of 26,710 arthroplasties. J Arthroplasty 2015;30(8):1299-307. [ Links ]
17. Molina CS, Thakore RV, Blumer A, Obremskey WT, Sethi MK. Use of the national surgical quality improvement program in orthopaedic surgery. Clinical Orthopaedics and Related Research® 2015;473(5):1574-81. [ Links ]
18. Pulido L, Parvizi J, Macgibeny M, Sharkey PF, Purtill JJ, Rothman RH, et al. In hospital complications after total joint arthroplasty. J Arthroplasty 2008;23(6):139-45. [ Links ]
19. Sutton JC,3rd, Antoniou J, Epure LM, Huk OL, Zukor DJ, Bergeron SG. Hospital discharge within 2 days following total hip or knee arthroplasty does not increase major-complication and readmission rates. J Bone Joint Surg Am 2016 Sep 7;98(17):1419-28. [ Links ]
20. Rozell JC, Courtney PM, Dattilo JR, Wu CH, Lee GC. Late complications following elective primary total hip and knee arthro-plasty: who, when, and how? J Arthroplasty 2017;32(3):719-23. [ Links ]
21. Zmistowski B, Restrepo C, Hess J, Adibi D, Cangoz S, Parvizi J. Unplanned readmission after total joint arthroplasty: rates, reasons, and risk factors. J Bone Joint Surg Am 2013 Oct 16;95(20):1869-76. [ Links ]
 Correspondence:
Correspondence:
Dr RJ Immelman
408 Berea Street, Muckleneuk, 0002
cell: 0833763848
email: rjimmelman@gmail.com
Received: May 2017
Accepted: September 2017
Published: March 2018
Project completed at Life Wilgers Hospital, Pretoria
Editor: Prof Anton Schepers, University of the Witwatersrand
Funding: The cost of completing this research was covered in whole by the authors, and no external funding was received.
Conflict of interest: None of the authors have any conflict of interest with regard to the content of this article.














