Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
SA Orthopaedic Journal
versão On-line ISSN 2309-8309
versão impressa ISSN 1681-150X
SA orthop. j. vol.16 no.3 Centurion Ago./Set. 2017
http://dx.doi.org/10.17159/2309-8309/2017/v16n3a1
HIP
The radiological outcome of uncemented femoral stems in rheumatoid patients undergoing total hip arthroplasty: results at minimum eight years
MS AbughalyaI; P RyanII; IE GogaIII
IHDip(Ortho), FCS Ortho(SA), Consultant Orthopaedic Surgeon, Department of Orthopaedic Surgery, University of KwaZulu-Natal, Durban, South Africa
IIMBChB(UCT), HDip(Orth), MMed(Ortho), FCOrth(SA), Specialist Orthopaedic Surgeon at Arthroplasty and Sports Medicine units, Department of Orthopaedics, Inkosi Albert Luthuli Central Hospital, Durban, KwaZulu-Natal, South Africa
IIIMD, FRCS(Edin), FCS Orth(SA), Professor and Head of Department Orthopaedic Surgery, Inkosi Albert Luthuli Central Hospital, Durban, KwaZulu-Natal, South Africa
ABSTRACT
BACKGROUND: Rheumatoid arthritis is a multi-systemic disease which affects all synovial joints. Compromised bone quality may have a negative impact on prosthesis incorporation after total hip replacement, resulting in an increased risk of aseptic loosening and early implant failure.
MATERIALS AND METHODS: Between 2002 and 2007, 49 patients (age 29-80 years) underwent total hip replacement. Radiographs were evaluated for signs of loosening or failure.
RESULT: Of the 49 hips, there was one case of stem subsidence, and one case of aseptic loosening. There were no revisions in the current series. Complications included eight (16.3%) intra-operative calcar fractures, which healed uneventfully.
CONCLUSION: We report satisfactory radiological results, and revision rate in a group of rheumatoid patients at mid-term review following total hip replacement with uncemented femoral stems.
Key words: rheumatoid arthritis, uncemented stem, femoral stem, hip, total hip arthroplasty, radiological assessment
Introduction
Rheumatoid arthritis (RA) is a chronic systemic inflammatory disorder characterised by multiple joint involvement. The hip joint is commonly affected (15-30% of patients).1
The disease process, medication and steroid use affect bone properties which lead to changes in bone bio-mechanics.2,3 Destruction of articular cartilage, bony deformity and protrusion are commonly seen in rheumatoid hip disease. Alterations to joint morphology, as well as bone quality contribute to an increased risk of intra- and post-operative complications.4
There is a two-fold increase in the frequency of osteoporosis compared to the general population.5 This results in a decreased potential for bony in/on-growth to uncemented prosthesis, and a decrease in fixation strength, with early aseptic loosening. For this reason, cemented total hip replacement (THR) has been considered by many to be the gold standard for patients with RA.1 With modern cementing techniques, stem survival rates are increased as the relative risk for stem loosening decreases.6
The use of uncemented prostheses for hip arthroplasty continues to rise as shown in numerous national joint registries.7,8 Although there have been some disappointing results for certain uncemented femoral stem designs used in this patient group - with high rates of subsidence and loosening - others have been more encouraging.
With this in mind, we set out to perform a mid-term review of the radiological outcomes of a group of rheumatoid patients who had total hip replacements at our institution.
Methods and materials
This study was conducted at the local arthroplasty unit in Durban, KwaZulu-Natal. From 2002 to 2007, 61 cementless primary total hip replacements were performed in 46 rheumatoid patients. At the time of review, three patients had demised, and nine were lost to follow-up.
In the remaining 34 patients, 49 uncemented THRs were performed.
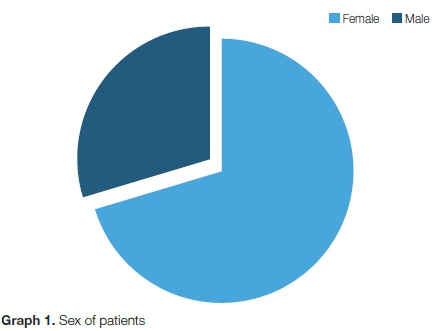
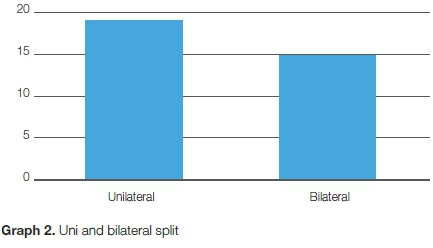
At the time of hip arthroplasty, the patients were aged between 29 and 80 years (mean of 58.4 years) (SD=12.12) (Table I). There were ten males, and 24 females (Graph 1), with 70.8% of the patients being female. Fifteen patients had bilateral THRs and 19 patients had unilateral THRs (Graph 2).

All patients were operated on through a modified Harding approach. All patients had index surgery without previous hip surgery. The femoral component was a collarless fully hydroxy-apatite coated stem (Corail, De Puy international Ltd) in 34 hips and a tapered grit blasted stem (CLS Zimmer, Warsaw) in four.
Follow-up ranged from 8 to 13 years (mean of 8.8 years) (SD=1.70).
The hips were evaluated radiographically pre-operatively and post-operatively by standardised anteroposterior view and lateral view of the hips. All measurements were taken by using Siemens syngo.plaza software, and magnification errors were accounted for.
The radiological assessment was made according to the following criteria:
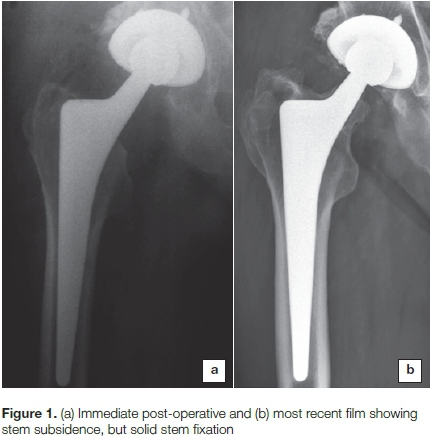
• Stem subsidence defined as a >5 mm change in distance between the top of the stem and greater trochanter9 as in Figure 1
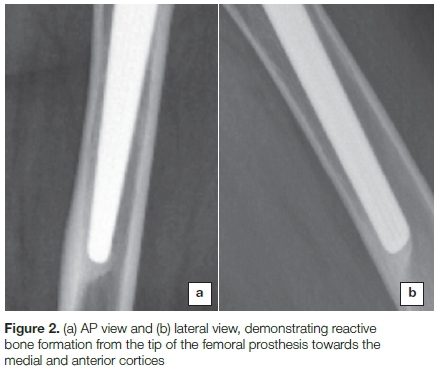
• Stem position in relation to the long axis of the femoral shaft in anteroposterior view as shown in Figures 2a and b, valgus or varus more than 3 degrees10
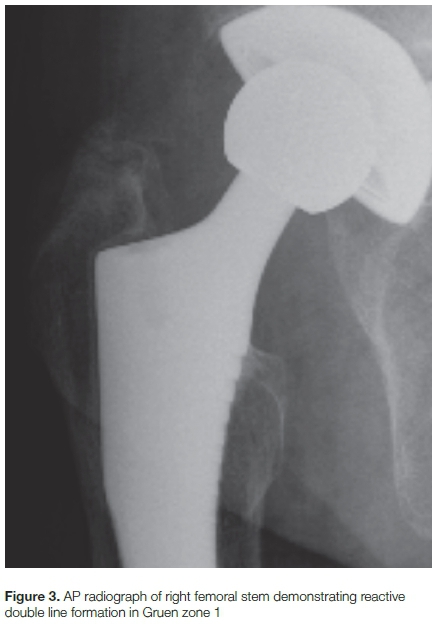
• Loosening of the stem based on Gruen zones11 as result of subsidence >5 mm, progressive change in the stem position >3 degrees, or continuous radiolucency more than 2 mm12 (Figure 3)
• Stability of the femoral stem was graded as stable ingrown fixation or unstable according to Engh's criteria13
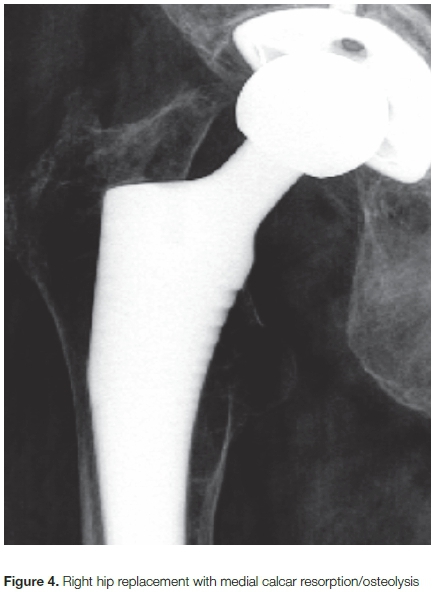
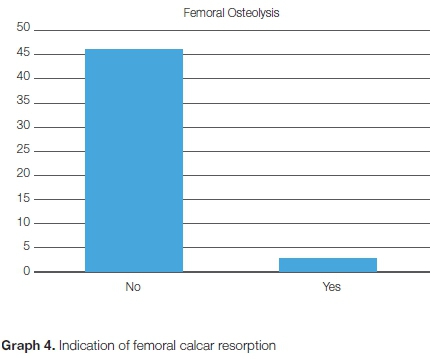
• Femoral remodelling as evidenced by calcar resorption, cortical hypertrophy (Figure 4)
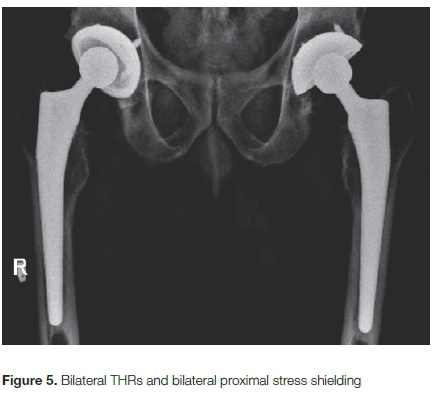
• Stress shielding as evidenced by a decrease of bone quality of the trochanters due to unloading of the proximal femur (Figure 5).
Data was analysed with Stata v.12. Descriptive statistics were calculated for the data, including mean and standard deviation for continuous data, and frequency and proportions for categorical data. Chi-squared tests were used to identify significant associations between categorical variables. A significance level of p<0.05 was deemed significant.
Results
The records and radiographs of 49 patients were retrospectively analysed.
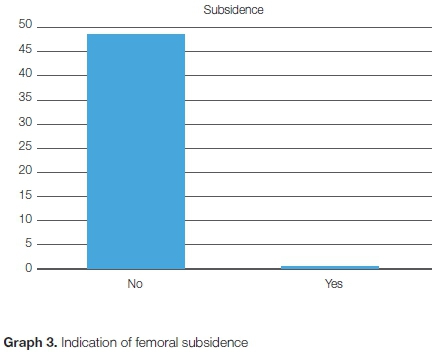
The stem position was central in 42 hips, varus in six hips, and valgus in one. There was one (1.9%) case of femoral subsidence (Graph 3). This was noted in the six-week follow-up X-ray, and is considered to be due to undersizing of the femoral component (Figure 1). There were eight cases (16.3%) of intra-operative calcar cracks, six of which were fixed with Charnley wire, and two which were not. All fractures healed uneventfully, with no subsidence.
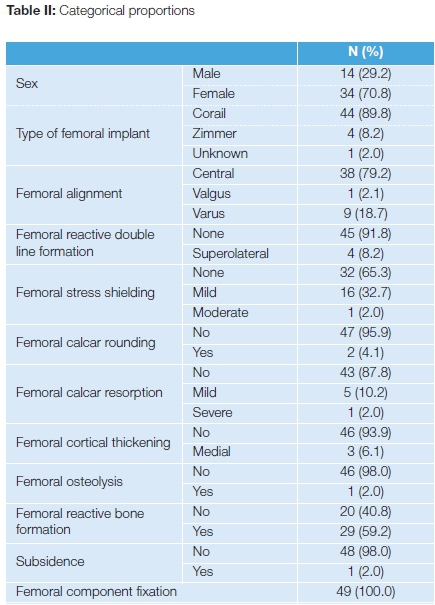
Reactive double line formation from bone remodelling was noted in zone 1 in five hips (Figure 3), and at the distal tip of the component in 28 hips (57.14%). Femoral calcar resorption was noted in two cases (Graph 4), mild stress shielding was seen in 17 cases (33%), and more significant stress shielding in two hips (3.9%) (Table II).
Although, one hip was deemed to be radiologically loose, there were no revisions in this group.
Chi-squared tests (Fischer's exact) indicated a significant association between femoral calcar resorption and femoral osteolysis (p=0.001), femoral stress shielding (p=0.012) and femoral alignment (p=0.001). However, no significant association was observed between femoral osteolysis and femoral calcar rounding (p=0.12), and femoral alignment (p=0.072). The sex of the patient was not significantly associated with any of the variables.
Discussion
Total hip replacement has been shown to be a hugely beneficial and cost-effective procedure in rheumatoid patients, improving hip function, relieving pain, and improving quality of life.14,15 However, there remain concerns regarding periarticular bone stock in the rheumatoid patient. Akesson et al.16 reported that compared to patients with primary osteoarthritis, rheumatoid patients going for hip arthroplasty showed an increase in bone turnover and a greater amount of unmineralised bone. This is postulated to be the cause of early implant loosening in rheumatoid patients.
Reported series of the use of cemented THRs in rheumatoid patients show varying degrees of success. Poss et al.17 reported results at seven years' follow-up: 96% of the patients in this study were happy with their outcome, and were clinically improved. Despite 31 % femoral stem subsidence, there was only a 1.6% revision rate.17 Ranawat et al.18 reported 8% femoral loosening at an average 4.3 years' follow-up with cemented stems. Severt et al.19 reviewed 75 rheumatoid patients at an average of 7.4 years, and reported three loose stems, and one revision for aseptic loosening. Creighton et al.20 found that cemented prosthesis survival in RA patients is comparable, if not better, compared to other diagnoses.
With the introduction of modern cementing techniques, femoral stem survival rates have improved. Rasquinha21 reported on 15 THRs at 15-year follow-up, with no aseptic loosening or stem revisions.
When considering cemented THR one should remain cognisant of the risk of haemodynamic instability inherent during the cementing process.22,23 Deep infection rates may also be increased due to the increase in operating time, and the local deep tissue injury from cement curing.17,19,24-27 The calculated cost of utilising cemented prostheses should include the increase in theatre time, which may be as much as 20 minutes longer on average than uncemented THR.28
Cementless fixation of femoral stems has become more popular, and good long-term results can be expected if there is solid biological integration. However, subsidence rates as high as 80% have been reported.29 Implant loosening does not necessarily correlate with implant survival. Unger et al.25 reported an overall 16.7% revision rate in RA patients at 12.1 year follow-up, with a further 15.7% prostheses being radiologically loose.
According to a study from the national Finnish register, uncemented prostheses performed better in both juvenile and old rheumatoid patients when compared to matched groups of patients with cemented stems.30,31
In the Swedish Hip Arthroplasty Registry between 1992 and 2007, it was shown that the risk of revision for uncemented femoral stems for any reason was lower than that for cemented stems. Revision for aseptic loosening was also lower in the uncemented group, after adjusting for age, sex, and underlying diagnosis.
However, reasons for revision differed between the two groups, with a higher proportion of the revisions in the uncemented hips being for fractures (17%) compared to that of cemented stems (6% of the revisions in this group).27
Although we had one case of subsidence, and one case of femoral component loosening, there were no revisions in this series.
Several studies report the most common complication in uncemented total hip arthroscopy (THA) is intra-operative fracture, which may or may not need fixation. Such fractures do not necessarily affect implant stability or long-term survival.32-35 In this series, there was a 16.3% fracture rate; however, none of these stems subsided, or were radiologically loose.
Conclusion
In this current retrospective case series, we have demonstrated satisfactory radiological results at a minimum of eight years post-surgery. Although, previous studies consider cemented femoral prostheses as the gold standard for rheumatoid patients, this study confirms that cementless femoral stem fixation is a safe alternative.
Compliance with ethics guidelines
Ethics clearance was approved by BREC (Biomedical Research Ethics Cpmmittee) which is registered with the South African National Health Research Ethics Council (REC-290408-009) and has US Office for Human Research Protections (OHRP) Federal-wide Assurance (FWA678).
References
1. Thomason HC, Lachiewicz PF. The influence of technique on fixation of primary total hip arthroplasty in patients with rheumatoid arthritis. J Arthroplasty. 2001;16(5):628-34. [ Links ]
2. Trancik T, Mills W, Vinson N. The effect of indomethacin, Aspirin, and Ibuprofen on the bone growth into a porous-coated implant. Clin Orthop. 1989;249:113-21. [ Links ]
3. Wheeler DL, vander Griend RA, Wronski TJ, et al. The short- and long-term effects of methotrexate on the rat skeleton. Bone. 1995;16: 215-16. [ Links ]
4. Zwartele RE, Witjes S, Doets HC, Stijnen T, Poll RG. Cementless total hip arthroplasty in rheumatoid arthritis: a systematic review of the literature. Arch orthop Trauma Surg. 2012;132:535-46. [ Links ]
5. Haugeberg G, Uhlig T, Falch JA, Halse JI, Kvien TK. Bone mineral density and frequency of osteoporosis in female patients with rheumatoid arthritis. Arthritis Rheum. 2000;43:522-30. [ Links ]
6. Onsten I, Besjakov J, Carlsson AS. Improved radiographic survival of the Charnley prosthesis in rheumatoid arthritis and osteoarthritis: results of new versus old operative techniques in 402 hips. J Arthroplasty. 1994;9:3-8. [ Links ]
7. No authors listed. The Canadian Joint Replacement Registry. http://secure.cihi.ca (date last accessed 24 Sep. 2015). [ Links ]
8. No authors listed. The Swedish Joint Registry. http://www.shpr.se/Libraries/Documents/AnnualReport_2013-04-1_1.sflb.ashx. [ Links ]
9. Garcia-Cimbrelo E, Cruz-Pardos A, Madero R, Ortega-Andreu M. Total hip arthroplasty with use of the cementless Zweymuller Alloclassic system. A ten to thirteen-year follow-up study. J Bone Joint Surg Am. 2003;85:296-303. [ Links ]
10. Barrack RL, Mulroy RD, Harris WH. Improved cementing techniques and femoral component loosening in young patients with hip arthro-plasty. A 12-year radiographic review. J Bone Joint Surg Br 1992;74:385-89. [ Links ]
11. Gruen TA, McNeice GM, Amstutz HC. 'Modes of failure' of cemented stem-type femoral components: a radiographic analysis of loosening. Clin Orthop Relat Res. 1979;141:17-27. [ Links ]
12. Sanz-Reig J, Lizaur-Utrilla A, Llamas-Merino I, Lopez-Prats F. Cement-less total hip arthroplasty using titanium, plasma-sprayed implants: a study with 10 to 15 years of follow-up. J Orthop Surg 2011;19:169-73. [ Links ]
13. Engh CA, Bobyn JD, Glassman AH. Porous-coated hip replacement. The factors governing bone ingrowth, stress shielding, and clinical results. J Bone Joint Surg Br. 1987;69:45-55. [ Links ]
14. Liang M, Cullen K, Larson M, Thompson M, Schwartz J, Fossel A. Cost effectiveness of total joint arthroplasty in osteoarthritis. Arthritis Rheum 1986;29:937-43. [ Links ]
15. Jonsson B, Larsson S. Functional improvements and costs of hip and knee arthroplasty in destructive rheumatoid arthritis. Scand J Rheumatol 1991;20:351-57. [ Links ]
16. Akesson K, Onsten I, Obrant KJ. Periarticular bone in rheumatoid arthritis versus arthrosis: histomorphometry in 103 hip biopsies. Acta Orthop Scand. 1994;65:135-38. [ Links ]
17. Poss R, Maloney JP, Ewald FC, et al. Six to 11 year results of total hip arthroplasty in rheumatoid arthritis. Clin Orthop. 1984;182:109-16. [ Links ]
18. Ranawat CS, Dorr LD, Inglis AE. Total hip arthroplasty in protrusio acetabuli of rheumatoid arthritis. J Bone Joint Surg Am 1980;62:1059-65. [ Links ]
19. Severt R, Wood R, Cracchiolo III A, Amstutz HC: Long-term follow-up of cemented total hip arthroplasty in rheumatoid arthritis. Clin Orthop 1991;265:137- 45. [ Links ]
20. Creighton MG, Callaghan JJ, Olejniczak JP, Johnston RC. Total hip arthroplasty with cement in patients who have rheumatoid arthritis: a minimum ten-year follow-up study. J Bone Joint Surg Am 1998;80:1439-46. [ Links ]
21. Rasquinha VJ, Dua V, Rodriguez JA, Ranawat CS. Fifteen-year survivorship of a collarless, cemented, normalized femoral stem in primary hybrid total hip arthroplasty with a modified third-generation cement technique. J Arthroplasty. 2003;18:86-94. [ Links ]
22. Ereth MH, Weber JG, Abel MD, et al. Cemented versus noncemented total hip arthroplasty embolism, hemodynamics, and intrapulmonary shunting. Mayo Clin Proc 1992;67:1066-74. [ Links ]
23. Nolan JP. Arterial oxygenation and mean arterial blood pressure in patients undergoing total hip replacement: cemented versus uncemented components. Anaesthesia 1994;49:293-99. [ Links ]
24. Maric Z, Haynes RJ. Total hip arthroplasty in juvenile rheumatoid arthritis. Clin Orthop 1993;182:109-19. [ Links ]
25. Unger AS, Inglis AE, Ranawat CS, Johanson NA. Total hip arthroplasty in rheumatoid arthritis: a long-term follow-up study. J Arthroplasty 1987;2:191-97. [ Links ]
26. Witt JD, Swann M, Ansell BM. Total hip replacement for juvenile chronic arthritis. J Bone Joint Surg Br 1991;73:770-73. [ Links ]
27. Hailer NP, Garellick G, Kärrholm J. Uncemented and cemented primary total hip arthroplasty in the Swedish Hip Arthroplasty Register. Acta Orthop 2010;81:34-41. [ Links ]
28. Barrack RL, Castro F, Guinn S. Cost of implanting a cemented versus cementless femoral stem. J Arthroplasty 1996;11:373-76. [ Links ]
29. Smilowicz M, Kowalczewski JB. Long-term results after total hip replacement; cemented and cementless in young rheumatic patients. Chir Narzadow Ruchu Ortop Pol 2005;70:319-23. [ Links ]
30. Eskelinen A, Paavolainen P, Helenius I, Pulkkinen P, Remes V. Total hip arthroplasty for rheumatoid arthritis in younger patients. Acta Orthop 2006;77:853-65. [ Links ]
31. Mäkelä KT, Eskelinen A, Pulkkinen P, Virolainen P, Paavolainen P, Remes V. Cemented versus cementless total hip replacement in patients fifty-five years of age or older with rheumatoid arthritis. J Bone Joint Surg Am 2011;93:178-86. [ Links ]
32. Turula K, Savioja S, Innes A, et al. Early results of cementless total hip replacement in inflammatory joint disease. Scand J Rheumat 1987;67:61-63. [ Links ]
33. Zwartele R, Peters A, Brouwers J, Olsthoorn P, Brand R, Doets C. Long-term results of cementless primary total hip arthroplasty with a threaded cup and a tapered, rectangular titanium stem in rheumatoid arthritis and osteoarthritis. Int Orthop 2008;32:581-87. [ Links ]
34. Araujo J, Gonzalez J, Tonino A, International ABG study group. Rheumatoid arthritis and hydroxyapatite-coated hip prostheses. J Arthroplast 1998;13:660-67. [ Links ]
35. Arnold P, Schule B, Schroeder-Boersch H, Jani L. Review of the results of the ARO multicenter study. Orthopade 1998;27:324-32. [ Links ]
 Correspondence:
Correspondence:
Dr MS Abughalya
Email: dr.abughalya@gmail.com
Tel: +27 812 711935
Received: March 2016
Accepted: October 2016
Published: August 2017
Funding: No funding was received for the writing of this article.
Conflict of interest: The authors declare they have no conflicts of interest relating to this article.