Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SA Orthopaedic Journal
On-line version ISSN 2309-8309
Print version ISSN 1681-150X
SA orthop. j. vol.15 n.2 Centurion May./Jun. 2016
http://dx.doi.org/10.17159/2309-8309/2016/v15n2a10
PAEDIATRICS
Traumatic simultaneous bilateral femoral neck fracture in a child: A case report
Patrick Wendpouiré Hamed DakouréI; Malick DialloII; Antonio Martinez PuenteIII; Souleymane OuédraogoIV; Massadiami SoulamaV
IMD FWCS Associate Professor in Orthopaedics and Trauma at the University Hospital of Bobo-Dioulasso (Burkina Faso)
IIMD Lecturer in Orthopaedics and Trauma Surgery at the University Hospital of Bobo-Dioulasso (Burkina Faso)
IIIMD Orthopaedic Surgeon
IVMD Junior Resident
VMD Orthopaedic Surgeon
ABSTRACT
BACKGROUND: Traumatic bilateral fracture of femoral necks in healthy children is a rare occurrence. A delay in surgery can impair anatomic closed reduction of a femoral neck fracture
CASE PRESENTATION: The authors report a rare case of a traumatic bilateral fracture of the femoral neck in a 9-year-old schoolgirl. This case was an unusual association of a transcervical fracture and an intertrochanteric fracture. This is the first known case of these two fracture types described in the same patient. Primary skin traction and a late closed surgical management gave a good result, although if possible early surgery is advised
CONCLUSION: The main mechanism of injury in this case is a two-step trauma. In this case, a delay to surgery by closed reduction and internal fixation by percutaneous screw fixation led to an acceptable outcome
Key words: traumatic, child, femoral neck fracture, bilateral bone screws
Introduction
A traumatic fracture of the femoral neck in children is a rare occurrence, comprising less than 1% of all paediatric fractures.1 Bilateral fractures are even rarer, with only ten cases reported in the literature.2-10 Usually, a high energy trauma is involved, such as a fall from a height and motor vehicle accident.1,4,6,8,11
We report the case of a 9-year-old schoolgirl who presented with traumatic bilateral fractures of the femoral neck after a fall from a height. Primary skin traction and secondary closed reduction with percutaneous cannulated screws fixation (PCSF) was performed. The girl recovered completely in seven months. Anatomical characteristics, mechanism of injury and late surgical management are discussed.
Case presentation
A 9-year-old schoolgirl with no history of hip disease presented to our Emergency Unit with closed trauma of both her hips. When playing with schoolmates, she slipped and fell off a 17 foot-high bridge. First, her right limb struck an edge of the bridge and then she fell down on her left hip.
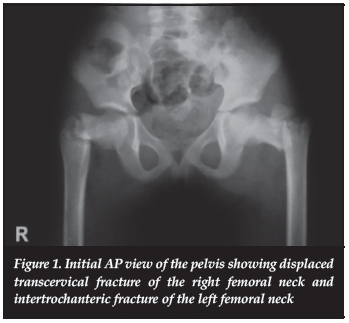
On admission, the patient laid in supination with the two lower limbs externally rotated. She complained of severe pain in the groin area and could not move her hips. Distally, the neurovascular status was normal. The AP pelvic radiograph showed a displaced transcervical fracture of the right femoral neck and an intertrochanteric fracture of the left femoral neck, classified as Delbet type III and IV respectively (Figure 1).
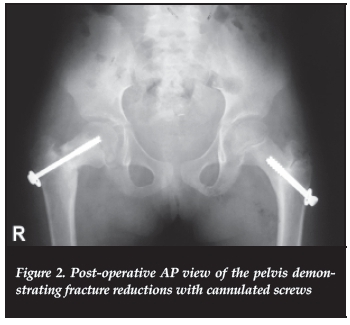
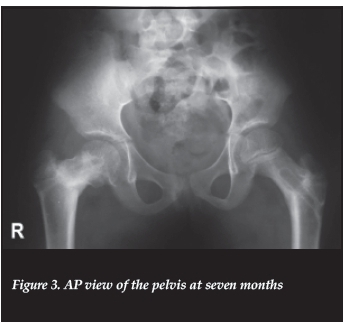
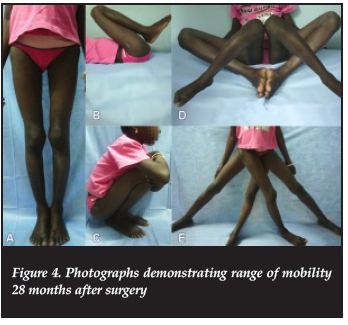
Skin traction was first applied. On the seventeenth day, under general anaesthesia, closed reduction was performed by traction and internal rotation. Fluoroscopic-guided percutaneous partially threaded cannulated screws with washers were used as internal fixation. A double plaster spica was applied immediately after surgery. The reduction was perfect on the left side with a measured cervicodiaphyseal angle (CDA) of 130 degrees. On the right side, the reduction was acceptable with a CDA of 128 degrees (Figure 2). The delay was due to our hospital's lack of materials, and the screws were the best we had available at the time of surgery. The post-operative period was uneventful. No post-operative rehabilitation was performed. The surgical wounds were healed in ten days, the spica was removed after a month and partial weight-bearing with crutches was allowed after seven weeks. Ten weeks after surgery, the hips were pain-free and she was able to walk without crutches. Follow-up pelvic radiographs showed signs of union at seven weeks, consolidation at seven months and signs of bone remodelling at 14 months. Screws were removed at seven months. There was no radiographic sign of femoral head necrosis or osteoarthritis but a shortened femoral neck and overgrowth of the greater trochanter was present on the left side (Figure 3). At 28 months, there was no lower limb shortening and the range of motion of both hip joints was: 120° for flexion, 15° for extension, 60° for abduction, 45° for adduction, 45° for external rotation and 30° for internal rotation (Figure 4). Finally the patient returned in school.
Discussion
A traumatic bilateral fracture of the femoral neck in children is an unusual injury. All previous cases described in the literature were due to high energy trauma as a result of a motor vehicle accident or fall from a height (Table I).2-10 In polytrauma cases, it is important to check the hips to avoid a delayed diagnosis.6 The average age at time of trauma was seven years (range 4-11) and the male to female ratio was 1:1.2.
Anatomical characteristics
Cervicotrochanteric and transcervical fractures are more frequently reported in the cases published in the literature2-7,9-11(Table I). Saied et al.2reported one case of associated transepiphyseal fracture (Delbet type I). No such case of associated intertrochanteric fracture was previously reported with another contralateral proximal femur fracture.
Mechanism of injury
A traumatic fracture occurs as a result of a particular position of the limb, and a precise point of impact to produce the injury. In reported cases of traumatic bilateral fracture of femoral neck, three main kinds of mechanisms were hypothesised: a direct 'one-injury fracture',2 an indirect 'two-injury fracture',4,6,9 and an indirect axial load fracture:10
• In the one-injury fractures, the mechanism is a lateral compression (LC) on a fixed pelvis. This mechanism seems similar to the LC type of the Young-Burgess System Classification.12
• In the two-injury fractures or 'abduction-adduction fractures', the first indirect impact occurs on the medial side of the thigh with the leg forced in abduction and external rotation, and the second direct impact occurs on the hip lateral side with the leg in adduction and internal rotation.
• In the axial load fractures, the force is transmitted from feet to flexed hips, through extended knees.
We are of the opinion that the mechanism in our case was that of a two-injury fracture type.
Injury management
The management of displaced femoral neck fractures is surgical by reduction and internal fixation.1,7 The closed reduction with PCSF followed by a spica plaster for seven weeks (4-16) gave best results in bilateral femoral neck fractures.3,4,6,7 According to Dhar,3 early surgery was necessary for a good outcome. Good results, however, were also observed with delayed surgery from two to 77 days with or without skin traction mainly by open reduction5,6,9,10(Table I). Our 17-day delay explains the non-anatomic reduction at the right hip. We think that primary skin traction is important for pain management.
Many authors used a hip spica cast as complementary immobilisation.2-5,7,10 It secures the internal fixation for eight weeks on average (range 4-16) without any secondary hip stiffness. The weight bearing time is linked to radiographic signs of bone union. Full weight bearing is allowed at around 12 weeks.4-6 The mean time of bone consolidation was 24 weeks in the literature described (range 12-52) (Table I).
Reported complications of surgical management are avascular necrosis of the femoral head, osteoarthritis, premature closure of the proximal femoral epiphysis, varus or valgus deformity,7,10 shortening of the femoral neck and overgrowth of the greater trochanter.10 A non-perfect reduction of a transcervical fracture (Delbet type III) may lead to shortening of the femoral neck and overgrowth of the greater trochanter. The current case shows AVN and coxa vara on the right side with no complications on the left side. According to Togrul et al.,8AVN is more frequent in bilateral hip fractures. The literature review found only one other case of AVN and varus deformity on a Delbet type III fracture7(Table I). We think that a longer follow-up time and the use of MRI would be useful to evaluate the true rate of AVN. A non-perfect anatomic reduction of a Delbet type III fracture led to an earlier physeal closure with overgrowth of the greater trochanter and varus/ valgus deformity7,10
Conclusion
The authors reported a first case of bilateral hip fracture in a child with a Delbet III and a Delbet type IV fracture. The mechanism of injury of the current case confirms the two-injury theory. A significant delay to surgery did not result in an adverse clinical result. However, a better outcome is observed with an earlier and perfectly closed reduction and a PCSF.
Acknowledgements
The authors thank Dr Herve Ouattara for his help in the preparation of this paper.
Compliance with Ethics Guidelines Informed consent: The patient and her parents were informed that data concerning the case would be submitted for publication. They agreed to this. They granted permission to use photographs. Patient confidentiality will be protected according to the US Health Insurance Portability and Accountability Act (HIPAA).
Competing interests: PWH Dakouré, M Diallo, AM Puente, S Ouédraogo and M Soulama declare that they have no competing interests.
References
1. Ratliff AHC. Fractures of the neck of the femur in children. J Bone Joint Surg Br. 1962;44-B(3):528-42. [ Links ]
2. Saied A and Jalili A. Bilateral simultaneous femoral neck fractures in a child. Eur J Orthop Surg Traumatol. 2009;19(5):349-51. [ Links ]
3. Dhar D. Bilateral traumatic fracture of neck of femur in a child: a case report. Malays Orthop J. 2013;7(3):34-36. [ Links ]
4. Sané JC, Kassé AN, Kéita K, Diallo MB, Diallo M, Camara EHS, Thiam B, Bousso A and Sy MH. Bilateral femoral neck fractures of the chilhood, diagnostic & management of a case. Orthop Emmerg Afr. 2013;2(4):34-35. [ Links ]
5. Gopinathan NR, Chouhan D, Akkina N and Behera P. Case report: Bilateral femoral neck fractures in a child and a rare complication of slipped capital epiphysis after internal fixation. Clin Orthop Relat Res. 2012;470(10):2941-45. [ Links ]
6. Upadhyay A, Maini L, Batra S, Mishra P and Jain P. Simultaneous bilateral fractures of femoral neck in children-mechanism of injury. Injury. 2004;35(10):1073-75. [ Links ]
7. Gilban HM, Mirdad TM and Jenyo M. Simultaneous post traumatic bilateral cervico-trochanteric femoral neck fractures in a child: a case report. West Afr J Med. 2005;24(4):348-49. [ Links ]
8. Togrul E, Bayram H, Gulsen M, Kalaci A and Özbarlas S. Fractures of the femoral neck in children: long-term follow-up in 62 hip fractures. Injury. 2005;36(1):123-30. [ Links ]
9. Kumar P, Singh GK and Singh MP. Traumatic simultaneous bilateral fractures of femoral neck in children-mechanism of injury. J Orthop. 2006;3(3). [ Links ]
10. Mazurek T, Lorczynski A and Ceynowa M. Bilateral femoral neck fracture in a child: a 17-year follow-up. J Pediatr Orthop B. 2011;20(5):295-98. [ Links ]
11. Mirdad T. Fractures of the neck of femur in children: an experience at the Aseer Central Hospital, Abha, Saudi Arabia. Injury. 2002;33(9):823-27. [ Links ]
12. Young JW, Burgess AR, Brumback RJ and Poka A. Pelvic fractures: value of plain radiography in early assessment and management. Radiology. 1986;160(2):445-51. [ Links ]
 Correspondence:
Correspondence:
Dr Malick Diallo
malikijallo@yahoo.com
malick-diallo@univ-bobo.bf
Phone: (+226) 65193236
Study Performed at Trauma & Orthopedics Department, CHU Sourô Sanou de Bobo Dioulasso, Avenue du Gouverneur William Ponty, 01 BP 676 Bobo-Dioulasso, Burkina Faso (West Africa) Phone: (+226) 20970044 or 20970045 or 20970047.














