Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
SA Orthopaedic Journal
versão On-line ISSN 2309-8309
versão impressa ISSN 1681-150X
SA orthop. j. vol.14 no.3 Centurion Ago./Set. 2015
http://dx.doi.org/10.17159/2309-8309/2015/V14N3A7
ARTHROPLASTY-KNEE
The X-Ray Knee instability and Degenerative Score (X-KIDS) to determine the preference for a partial or a total knee arthroplasty (PKA/TKA)
CR OosthuizenI; S BurgerII; DP VermaakIII; P GoldschmidtIV; R SpangenbergV
IMBChB(Stell), MMed(Ortho); Orthopaedic surgeon, Wilgeheuwel Hospital, Roodepoort, Johannesburg
IIMBChB(Pret), Neurosurgery(SA); Specialist neurosurgeon, Wilgeheuwel Hospital, Johannesburg
IIIMBChB (Pret), MSc(Sport Med)(Pret), MMed(Orth)(UOFS), Arthroplasty Fellowship UK; Little Company of Mary Hospital, Pretoria
IVMBBCh FFRad(D)(SA); Radiologists: Van Rensburg and Partners SA (Inc)
VBCom (Unisa)(Risk Management); Independent
ABSTRACT
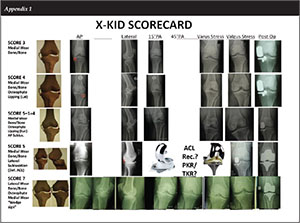
The X-ray Knee Instability and Degenerative Score (X-KIDS) was developed as a tool based on the degenerative and instability patterns seen on routine X-ray views of the weight-bearing compartments and tested on 336 knees, average age 64 years and followed up for 24 months.
It is a study to evaluate the X-KIDS scoring method, which quantifies whether a PKA or TKA is the procedure of choice, comparing it to the surgical procedure done and to a stress X-ray evaluation as a stand-alone when contemplating knee arthroplasty.
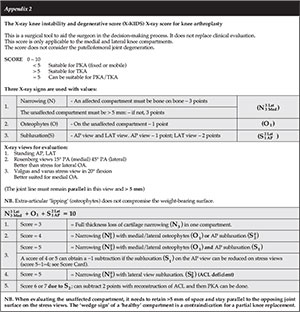
Points are allocated to the following features: narrowing (N), osteophytes (O), and subluxations (S).
The assessed score is out of 10. A patient with a score of at least 3 but less than 5 is suitable for a PKA, a score of 5 could be suitable for a PKA or a TKA and a score exceeding 5 requires a TKA.
There was a 95.82% (321) evaluator consensus with the X-KIDS on the X-ray sequence for a PKA or TKA.
92.3% (310) received the procedure assessed by X-KIDS and 2.98% (10) could have received the procedure evaluated.
90.78% of the stress views indicated the preferred procedure and is not as reliable as X-KIDS to determine the procedure.
Key words: knee, arthroplasty, degenerative, instability, X-ray score
Article summary
Article focus
1. Evaluation of the reproducibility of the X-KIDS as a 'diagnostic tool' with the specified X-ray sequence.
2. X-KIDS correlation with the selected surgical procedure and the clinical influence.
3. X-KIDS comparison with the stress views as a stand-alone test.
4. The incidence of significant OA of the patellofemoral joint on the lateral view.
Key messages
1. The X-KIDS is a reliable tool when contemplating a knee arthroplasty procedure.
2. The X-KIDS classifies the degree of degeneration and instability.
3. The study confirms that the stress test as a 'stand-alone tool' is not reliable.
4. Patellofemoral joint (PFJ) degeneration, in this series, is not a dominant decider for PKA/TKA.
Background
The score should be considered with the patients' clinical requirements and preferences.
The score is reliable, inexpensive and reproducible with two 'new' observations which illuminate the wear pattern of the 'unstable' degenerative knee. These propose that the 45° Rosenberg view is more reliable when illustrating lateral pathology (rather than the stress view) and the 'wedge sign' for evaluating the integrity of the healthy compartment. The co-contributors were a combination of medical specialists, namely a radiologist (20 years' experience), neurosurgeon (9 years), two orthopaedic surgeons (24 and 3 years respectively) and a non-medical volunteer, all of whom, apart from the corresponding author, were blinded to the implemented procedure.
The author acknowledges that the co-contributors' reviews were retrospective; however, their evaluations were not focused on any surgical intervention. The X-KIDS may give false results due to the quality of the X-ray views and their possible misinterpretation together with 'fresh' ligament injuries as the X-ray features develop over time with the subluxation effect only visible after the subsequent failure of the secondary stabilisers. The performance of the X-KIDS may be biased by the author's understanding of the radiographic significance, which may have increased the concordance and it therefore requires further validation in other academic centres.
Introduction
Due to the difficulty experienced when assessing and categorising the degree of instability and degeneration of the knee, a new tool has been developed to improve the decision-making process and address the trepidation when contemplating a specific arthroplasty. The quest for a solution to determine whether an arthroplasty is indicated, and the distinction between a TKA and PKA, has become more relevant in light of Riddle's 20141 study that indicates the high, 'inappropriate' (34%) use of the TKA in the USA, without a conclusive algorithm of treatment. Willis-Owen in 20092 asserted that 47% of knee arthroplasties are suitable for PKA rather than TKA but the various joint registries point to a high failure rate of the PKA despite better functional scores3,4 and blame the infrequent user and inconsistent selection. The interpretation of data assessed is also a problem as illustrated by Goodfellow in his critique about the NZJR (2010).5
The history, clinical examination and routine X-rays with stress X-ray views to assess stability and degeneration, remain the cornerstone for evaluating a knee for PKA or a TKA.6,7 The goal is to determine whether the predominant single compartment degeneration presents with intact ligaments, whether anteromedial degenerative pathology in the varus deformed knee8 is present, and whether lateral valgus deformity is suitable for PKA, or to illustrate bicondylar degeneration suitable for a TKA. The X-rays assess wear and knee ligament integrity, e.g. the anterior cruciate ligament (ACL) wear pattern as evaluated by Keys9 and Deschamps,10 and stability on the stress views.7
The PKA treatment option has regained popularity due to the improved surgical technique, mini-incision approach, preservation of the ligaments, bone stock and appropriate instrumentation.11-13 Excellent outcomes have been achieved by centres that have refined the selection and surgical technique.14-18 The fully congruent mobile PKA demonstrated better functional results2,19 and 20-year surgical results comparable to that of the TKA20-24 with age, obesity level, state of the patellofemoral joint (PFJ) and chondrocal-cinosis not being regarded as contraindications.25,26 The results of PKA revision surgery to a TKA are controversial although they are compared with a primary TKA and not to a revision TKA.27,28 Overall risk of complications with PKA is 4.3% and with TKA 11.4% (Oxford Group).19
A new tool has been developed to improve the decision-making process and address the trepidation when contemplating a specific arthroplasty
The PFJ degeneration is rarely seen to alter the outcome of the TKA or the PKA.2324 In the NJR (England and Wales) of 2013,26 singular PFJ replacements amounted to 1% of all replacements and more often occurred in female patients (70% at an average age of 59 years), compared with the TKA at 69 years. The preference for resurfacing the PFJ in TKA was 7% of cementless procedures and 38% in cemented versions.
By improving the selection algorithm with the correct indication and surgical technique, an excellent long-term functional outcome for an arthroplasty can be achieved, suitable for the patient's requirements.
Method
The study reviewed 335 patients over a 3-year period in a knee clinic with the X-KIDS sequence, and compared the results with the stress views as a stand-alone and the procedure implemented. Comparative studies of the outcome of whether the X-KIDS were used or not, are not available. The author correlated the X-ray appearance with the intra-operative findings and the surgical decision.
The cornerstone of the X-KIDS is bone-on-bone wear and was developed by allocating points to features normally found and easily recognised on routine knee X-rays. The features are narrowing (N), osteophyte formation (O) and subluxation (S). The features are common to knee degeneration and the weighting allocated according to the severity of degeneration when each compartment is individually assessed for bone-on-bone wear or narrowing. The weighting is also applied to the instability features as seen on the AP and lateral views.8,9
X-ray observer factors, namely osteophytes (bony projections at the margins of the joint)29 and subluxations (shifting out from the normal position), are included in the score as they have a bearing on the wear and instability assessment. This can unnecessarily affect the decision for a specific procedure if not assessed.
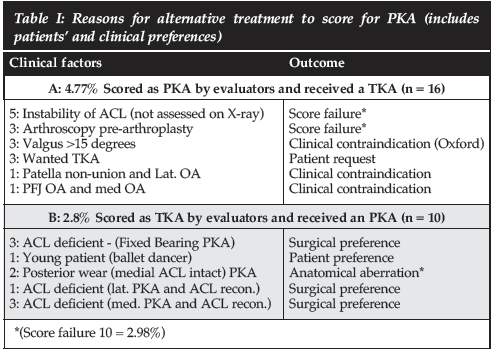
Surgical decisions were taken which did not conform to the score preference and this will be explained, e.g. a TKA was done when the score indicated suitability for a PKA due to excessive valgus (clinical contraindication for PKA > 15°) (Table I).
Although the PFJ was not the focus of this study and rarely influences the decision in arthroplasty as confirmed by Pandit and Beard,23-25 the joint was evaluated on the lateral view by three observers as a separate study of 330 of the X-ray sequences to assess 'significant' PFJ degeneration. Skyline views would be preferable in a follow-up study but could not be done due to the extra costs involved.
The long-term results of the surgical cases cannot yet be assessed but the average time since operation is 26.7 months.
Radiographic imaging
1) Standing antero-posterior (AP) and lateral (LAT) of the knee (Figure 1)

2) PA 15° Rosenberg - medial wear (Figure 2a)
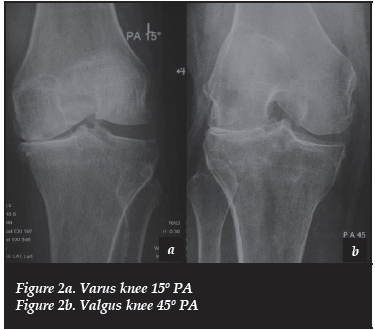
3) PA 45° Rosenberg - lateral wear (Figures 2b and 7b)
4) Varus stress view in 20° flexion (Figures 3 and 4)
1. Narrowing (N) (point count = medial 3; lateral 3) = 6 (Figures 1, 2a, 2b, 3, 7)
Bone-on-bone contact between the femoral condyle and the tibial surface suitable for arthroplasty attracts 3 points (joint line narrowing). The contralateral joint must be >5 mm (= 2.5 mm on femur and tibia) and parallel and if less attracts 3 points and precludes the PKA option.6,30-33
2. Osteophytes (O) (point count = medial 1 or lateral 1) = 1 in total (Figures 1, 2a, 2b, 3, 4)
This may be evident on femoral and tibial margins with one point given medially or laterally, irrespective of the degree. These 'spurs' may reflect degeneration and extra-articular traction due to 'laxity' of the ligaments caused by pseudo-instability.34
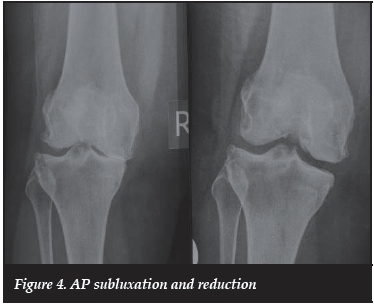
3. Subluxation (S) (point count = AP 1 and lateral 2) = 3 (Figures 4 and 5)
AP view: Subluxation with increasing varus and increasing valgus is seen due to excessive wear in the medial or lateral compartments and the loss of ligament integrity. This attracts a single point but if reduced on the stress view and the healthy joint is maintained >5 mm and parallel, it is subtracted from the accumulated total (Figure 4).
Assessed points: N3O1S1 = 5 - 1 = 4 points
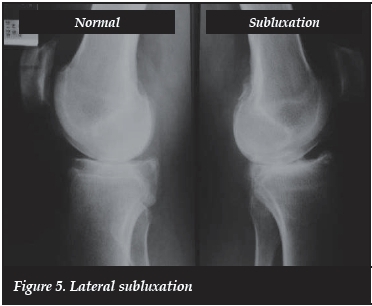
Lateral view: Anterior subluxation of the tibia and posterior wear of the medial tibial plateau as seen with ACL deficiency (Figure 5)
When there is a healthy weight-bearing compartment with anterior subluxation of the tibia which can be rectified and stabilised with an ACL reconstruction, the 2 points assessed can be subtracted and can become suitable for a PKA if an ACL reconstruction is done.
The 45° Rosenberg view evaluates the lateral compartment with, specifically, the predilection for central and posterior wear and the 15° Rosenberg displays the anteromedial pathology (Figures 2, 7a and 7b).34,35
On the stress views the normal compartment must maintain a parallel space of more than 5 mm which relates to 2.5 mm of cartilage on the femur and tibia respectively (Figures 1, 2, 3 and 6).29,33,36-38 If the healthy compartment does not maintain the parallel opposing surfaces (indicating normal cartilage, correctable intra-articular varus, an intact collateral MCL/LCL32 and ACL) and becomes angled, the knee should be regarded as a risk for PKA ('wedge sign') (Figure 6).
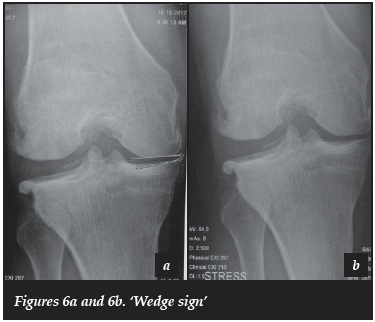
It is important to prevent rotation and magnification of the knee during the stress views.
Anteromedial wear (varus Figures 2a, 2b and 3)
Confirm bone-on-bone wear and the integrity of the lateral joint space with the stress views. The 15° PA is reliable but does not confirm the integrity of the lateral joint space.37
Lateral wear (valgus Figures 2a, 2b, 3, 7a and 7b)
Confirm the lateral compartment wear pattern with the 45° PA. The 20° stress views are best used to confirm the medial joint space retention.
Stress views in 20° flexion do not demonstrate the pathological lateral compartment as reliably, due to the wear pattern laterally being central and often posterior (on the 20° flexion views, the intact antero-lateral tibial cartilage is stressed and this compartment can appear to be intact Figure 7).
Scoring formula
A maximum of 10 points can be accrued with the X-KIDS (N33 + O1 + S12).
1. X-KIDS of 3 and 4 points = PKA (mobile preferred or fixed).
2. X-KIDS of 5 is considered for a PKA (mobile or fixed) (NB clinical findings and surgical corrections).
3. X-KIDS > 5 points a TKA is indicated.
The cornerstone of the X-KIDS is bone-on-bone wear and was developed by allocating points to features normally found and easily recognised on routine knee X-rays
Results
The average age of the 335 patients was 64 years (± SD of 10 years) and the majority were female (54.8%). The average age of the female patients (n = 184) was 65 ± 9 years and for the male patients (n = 151) 63 ± 9.3 years. The actual PKA accounted for 77.9% (n = 261) (98.9% mobile and 1.1% fixed bearing) of the procedures performed and the actual TKA for 22.1% (n = 74).
The cohort composition is due to the surgeon being a referral centre for predominantly PKA procedures (see Table II).
1. In 95.82% of the cases the X-KIDS achieved consensus with all five of the evaluators as they agreed on the procedure to be performed based on the X-KID Score calculated. The agreement of multiple evaluators is recapitulated with Light's Kappa of 0.872 (bootstrapped CI95% [0.819; 0.912]). This indicates almost absolute agreement between evaluators. In 2.98% of the cases the X-KIDS was incorrect in predicting the actual procedure required (undetected ACL deficiency and arthroscope decision).
2. The score failed in ten patients (2.98%) (eight undiag-nosed ACL and two incorrectly diagnosed ACL). Twenty-six (26/336 = 7.38%) patients did not receive the procedure according to the score. This was influenced by the patients' preferences and pre-operative clinical factors, e.g. pre-operative arthroscopic pathological decisions (three), pre-operative PKA contraindications (five), instability of ACL which received a reconstruction ACL and mobile PKA (three) or a fixed-bearing PKA (three) (Table I). In 16 (4.77%) cases the evaluators scored a PKA but a TKA was performed. In ten (2.98%) cases the evaluators scored a TKA but a PKA was performed. The agreement between the X-KIDS and the actual procedure is recapitulated with Cohen's Kappa of 0.753 (bootstrapped 095% [0.674; 0.834]). Since an indeterminate score does not agree with any actual procedure, the measure is conservatively estimated. This indicates substantial, but not absolute agreement (see Table I).
3. A discrepancy between the X-KIDS and the stress test assessment as a stand-alone test was observed in 31 (9.23%) of the 335 cases. In 5.97% of the 335 cases the discrepancy was due to the non-detection of ACL deficiency (n = 20) and 3.27% was due to clinical exclusions not detected (n = 11). As the ACL efficiency group is routinely treated with a TKA this comprises a failure rate of 27.03% (20 out of 74 patients receiving TKA). The Cohen's Kappa between the stress test assessment and the actual procedure is 0.699 (bootstrapped CI95% [0.592; 0.790]). Although still substantial, the level ofagreement is less than the level of agreement between the X-KIDS and the actual procedure.
4. 'Significant' PFJ changes of 330 patients were considered and 46.67% of the cases presented with significant changes. In the PKA group 41.40% (n = 106) of the 256 patients presented with PFJ degenerate changes. This is significantly lower than the TKA group where 64.86% (n = 48) of the 74 patients presented with significant changes (p = 0.0003, one-tailed Fisher's Exact Test). Significant PFJ OA changes did not influence the PKA decision.
5. Four failures were treated after 24 months: 1 medial PKA treated after traumatic ACL rupture with a thicker bearing; and 3 medial PKA procedures treated with lateral PKAs.
Discussion
There have been attempts to classify knee osteoarthritis, e.g. the initial Kellgren-Lawrence 1957 classification,39 Ahlback (1968),38 the Atlas of Line Drawings by Nagaosa Classification 2000,40 the more modern imaging scoring (Whole Organ Magnetic Resonance Imaging Score 'WORMS'),41 and the Boston Leeds Osteoarthritis Knee Score (BLOKS)(2010)31 have been devised. There are the proponents of MRI-only visualisation, e.g. Guermazi (2011)32 and the comparative studies done by Jeffrey Duryea (2001)30 on radiographic joint space width to the cartilage morphometry.
The conclusion drawn is that the two are comparable but the 'gold standard' is still X-ray imaging.
The X-KIDS is different from all the previous evaluation systems, as it incorporates the stability of the knee ligaments and the severity of the weight-bearing degeneration. This can assist the surgeon to improve his decision for a specific arthroplasty which will lead to optimal treatment. The X-KIDS can be used as a classification of degenerative knee pathology and a reference to improve research on arthroplasty selection.
The stress test as a stand-alone tool is unreliable in detecting the required procedure as it cannot evaluate ACL deficiency adequately.
The PFJ rarely determined the procedure implemented. Only one clinically painful PFJ had a TKA (1/335) when scored for a PKA.
The X-KIDS must be understood and applied with due consideration to the clinical indications and contraindications for the PKA and TKA and when used appropriately, the X-KIDS is more than 95% reliable and confirms the appropriate surgical intervention in at least 92% of knees evaluated.
This research received no grant from any funding agency in the public, commercial or not-for-profit sectors. Affiliations: Dr CR Oosthuizen is a consultant to Biomet (SA) and Mathys (Swiss).
Acknowledgements
As evaluators: Dr RP Goldschmidt, Dr D Vermaak, Dr S Burger, Dr CR Oosthuizen, Mr R Spangenberg As Statistical Consulting Services: Maryn Viljoen
References
1. Riddle D, et al. Using a validated algorithm to judge the apprpriateness of total knee arthroplasty in the United States: A multi-center longitudinal cohort study. Arthritis and Rheumatology. Published online June 30 2014. [ Links ]
2. Willis-Owen, Brust et al. Unicondylar knee arthroplasty in the UK National Health Service. The Knee 2009 Dec;16(6):473-78 Epub 2009 May 22. [ Links ]
3. National Joint Registry for England and Wales 2011. 8th annual report ISSN 1745-1450 online. [ Links ]
4. Pearse AJ, Hooper GJ, Rothwell A, Frampton C. Survival and functional outcome after revision of a unicompart-mental to a total knee replacement. The NZN Joint Registry JBJS 2010 April;92(4):508-12. [ Links ]
5. Goodfellow JW, O'Connor JJ, Murray DW. A critique of revision rate as an outcome measure: Re-interpretation of knee joint registry data. JBJS 2010 December 92;(12):1628-31. [ Links ]
6. Goodfellow J, O'Connor J, Dodd C, Murray D. Unicompartmental arthroplasty with the Oxford knee 2006. New York: Oxford University Press 2006. [ Links ]
7. Gibson PH, Goodfellow JW. Stress radiography in degenerative arthritis of the knee. JBJS BR 1986;68(4):608-609. [ Links ]
8. White SH, Ludkowski P, Goodfellow JW. Anteromedial osteoarthritis of the knee. JBJS BR 1991 Jul;73(4):582-86. [ Links ]
9. Keys GW, Carr AJ, Miller RK, Goodfellow JW. The radiographic classification of medial gonarthrosis. Correlation with operation methods in 200 knees. Acta Orthop Scand 1992 Oct;63(5):497-501. [ Links ]
10. Deschamps G, Lapyre B. Rupture of the anterior cruciate ligament: a frequently unrecognised cause of failure of unicompartmental knee prosthesis. French J Orthop Surg 1987;73(7):544-51. [ Links ]
11. Brown NM, Sheth NP, et al. Clinical paper review: Total knee arthroplasty has higher post-operative morbidity than unicompartmental knee arthroplasty: A multicentre analysis. Journal of Arthroplasty, 2012 Sep;27(Suppl):86-90. Doi: 10.1016/j.arth.2012.03.022 Epub online May 4, 2012. [ Links ]
12. Lombardi AV, Berend KR, et al. Is recovery faster for mobile-bearing unicompartmental than total knee arthro-plasty? CORR 2009 Jun;467:1450-57. Doi:10.1007/s 11999009-0. [ Links ]
13. Robertson O, et al. Use of unicompartmental instead of tricompartmental prosthesis for unicompartmental arthrosis in the knee is a cost effective alternative. Acta Orthop Scand. 1999;70(2):170-75. [ Links ]
14. Svârd UC, Price AJ. Oxford medial unicompartmental knee arthroplasty; a survival analysis of an independent series. JBJS-B.2001 Mar;83(2):191-94. [ Links ]
15. Vorlat P, Putzeys G, Cottenie D et al. The Oxford unicom-partmental knee prosthesis; an independent 10-year survival analysis. Knee Surg Sports Traumatol Arthrosc. 2006 Jan;14(10; 40-5 Epub)2005 May 14. [ Links ]
16. Tabor OB, Tabor OB, Bernard M, M Wan JY. Unicompartmental knee arthroplasty: long-term success in middle-age and obese patients. PMID: 16115429 http://europepmc.org/abstract/MED/16115429 Orthop. Adv. 2005;14:59-63. [ Links ]
17. Price AJ, Waite JC, Svard U. Long-term clinical results of the medial Oxford unicompartmental knee arthroplasty. CORR 2005 Jun;435:171-80. [ Links ]
18. Pandit H, Jenkins C, Gill HS, Barker K, Dodd CAF, Murray DW. Minimally invasive Oxford phase 3 unicom-partmental knee replacement - results of 1000 cases. JBJS Br 2011 Feb;93(8):198-204. [ Links ]
19. Liddle, et al. Optimal usage of unicompartmental knee replacement: An analysis of 41 986 cases presented at AAOS 2014. [ Links ]
20. Newman JH, Pydisetty RV, Ackroyd C. Unicompartmental or total knee replacement? The fifteen year results. JBJS Br 1998;80-B:862-65. [ Links ]
21. Cobb, Kozunn, Scott. Unicondylar or total knee replacement; the patients' preference. JBJS 2009:91-B:52-57. [ Links ]
22. Young, Wang, Leo, Lo. Minimally invasive unicondylar versus total condylar knee arthroplasty - Early results of a matched pair comparison. Singapore Med J 2003. [ Links ]
23. Pandit et al, Jenkins C, Gill HS. Unnecessary contraindications for mobile bearing unicompartmental knee replacement. JBJS-B May 1993;5:622-28. [ Links ]
24. Beard DJ, Pandit H, Ostelere S, Jenkins C, Dodd CA, Murray DW. Pre-operative clinical and radiological assessment of the patello femoral joint in unicompart-mental knee replacement and its influence on outcome. JBJS-B 2007 Dec;89(12):1602-607. [ Links ]
25. Ham MD, Chang CB, et al. Correlation of the condition of the patellar articular cartilage and patellofemoral symptoms and functions in osteoarthritic patients undergoing total knee arthroplasty. JBJS 2005;87-B:37. [ Links ]
26. National Joint Registry for England, Wales and Northern Ireland (10th Annual Report). 2013. [ Links ]
27. Australian Orthopaedic Association National Joint Replacement Registry Annual Report ISSN 1445-3657 2011. [ Links ]
28. Pearse AJ, Hooper GJ, et al. Survival and functional outcome after revision of a unicompartmental to a total knee replacement: The NZNJ Registry JBJS April 2010;92-B:508-12. [ Links ]
29. Nagaosa Y, Lanyon P, Doherty M. Characterisation of size and direction of osteophyte in knee osteoarthritis. Ann Rheum Dis. 2002 April;61(4):319-24. [ Links ]
30. Duryea J, Hunter DJ, et al. Comparison of radiographic joint space width to MRI cartilage morphometry: analysis of longitudinal data from the Osteoarthritis Initiative (OAI). Arthritis Care Res (Hoboken) 2010 July;62(70):932-937. DOI: 10.1002.acr 20148. [ Links ]
31. Hunter DJ, Lo GH, et al. The reliability of a new scoring system for the knee osteoarthritis MRI and the validity of bone marrow lesion assessment: BLOKS (Boston Leeds Osteoarthritis Knee Score). Ann Rheum Dis. 2008 February. [ Links ]
32. Guermazi A, Roemer FW, et al. Why radiography should no longer be considered a surrogate outcome measure. Arthritis Research and Therapy 2011;13:247, http://arthritis-research.com/content/13/6/247. [ Links ]
33. Vignon E, Piperno M, Conrozier T, et al. Measurement of radiographic joint space width in the tibiofemoral compartment. Arthritis Rheum. 2003 Feb;48(2):378-84. [ Links ]
34. Buckland-Wright JC. Substantial superiority of semiflexed (MTP) in knee osteoarthritis. J Rheumatol 1999 Dec;26(12):2664-74. [ Links ]
35. Mazzuca SA, Brandt KD, Buckwalter KA, Lane KA, Katz BP. Field test of the reproducibility of the semi-flexed metatarsophalangeal view in repeated radiographic examinations of subjects with osteoarthritis of the knee. Arthritis Rheum. 2002 Jan;46(1):109-13. [ Links ]
36. Hunter DJ, Zhang YQ, Felson DT, et al. Change in joint space width. Arthritis Rheum. 2006 August. [ Links ]
37. Gossec L, Jordan JM, Mazzuca SA, et al. Comparative evaluation of three semi-quantitative radiographic grading techniques. Osteoarthritis Cartilage 2008 Jul;16(7):742-48 Epub 2008 April 15. [ Links ]
38. Ahlback S. Osteoarthritis of the knee: a radiographic investigation. Acta Radiol (Stockh). 1968:Suppl 277;7-72. [ Links ]
39. Kellgren-Lawrence Classification: Knee Osteoarthritis Classification and Treatment Options. Stemcelldoc's Weblog November 13, 2011. [ Links ]
40. Nagaosa Y, Mateus M, et al. Development of a logically devised line drawing atlas for grading of knee osteoarthritis. Ann Rheum Dis. 2000 Aug;59(8):587-95. [ Links ]
41. Felson DT, Lynch J, Guermazi A, et al. Comparison of BLOKS and WORMS scoring systems part II. Longitudinal assessment of knee MRIs for osteoarthritis and suggested approach based on their performance: data from Osteoarthritis Cartilage. 2010 Nov;18(11):1402-7 Epub 2010 Sep 17. [ Links ]
 Correspondence:
Correspondence:
Dr CR Oosthuizen
PO Box 3158
Honeydew 2040
Tel: 011 794 3371; Fax: 011 794 3368
Email: cro@mweb.co.za
Statistical Consulting Services: Maryn Viljoen
Appendix
Please take note of Appendix 1 and 2 after the original article for further clarification.