Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SA Orthopaedic Journal
On-line version ISSN 2309-8309
Print version ISSN 1681-150X
SA orthop. j. vol.14 n.1 Centurion Feb./Mar. 2015
SPINE
Pantoea agglomerans as a rare cause of cervical spondylodiscitis
C de V MaraisI; S MearsIV; SI Dix-PeekII; K PillayIII; RN DunnV
IMBChB(Stell), Dip PEC Registrar; Groote Schuur Hospital and Red Cross War Memorial Children's Hospital in Department of Orthopaedic Surgery, University of Cape Town, South Africa
IIMBBCh, FCS(SA)Orth, MMed Consultant; Head of Paediatric Orthopaedics Red Cross War Memorial Children's Hospital, Division Orthopaedic Surgery University of Cape Town
IIIMBChB, PCPath(SA), FRCPath(UK), MMed Ant Path(UCT) Consultant; Histopathologist/Senior Lecturer National Health Laboratory Service and University of Cape Town and Red Cross War Memorial Children's Hospital, South Africa
IVMBChB(Stell), FCS(SA)Orth Consultant; Groote Schuur Hospital and Red Cross War Memorial Children's Hospital in Department of Orthopaedic Surgery, University of Cape Town, South Africa
VMBChB, MMed(Orth), FCS(SA)Orth Professor and Head of Department; Groote Schuur Hospital and Red Cross War Memorial Children's Hospital in Department of Orthopaedic Surgery, University of Cape Town, South Africa
ABSTRACT
OBJECTIVE: To present a case report of a rare cause for cervical spondylodiscitis caused by Pantoea agglomerans.
CASE PRESENTATION AND INTERVENTION: A 10-year-old girl presented with a destructive lesion of the C4 vertebral body with raised infective markers and a radiological picture suggestive of tuberculosis spondylodiscitis. Further investigations revealed multiple sites of involvement. No evidence of tuberculosis was found. Histology after biopsy showed focal granuloma formation in response to necrotic bone fragments and on tissue cultures in which Pantoea bacteria was isolated. The patient was successfully treated with a six-week course of co-amoxiclav. On follow-up the cervical lesion as well as the other sites of involvement showed signs of resolution
CONCLUSION: Pantoea agglomerans is a rare pathogen in the aetiology of spondylodiscitis. The organism is usually associated with penetrating trauma by plant material or contaminated intravenous products. Neither of these factors was present in this case
Key words: Pantoea agglomerans, cervical spondylodiscitis, paediatrics
Case report
A 10-year-old girl presented with a nine-month history of progressive neck pain and reduced cervical spine range of motion. No obvious precipitating events or trauma were reported. The child was in good general health. She did not have a tuberculosis contact or any constitutional symptoms of tuberculosis.
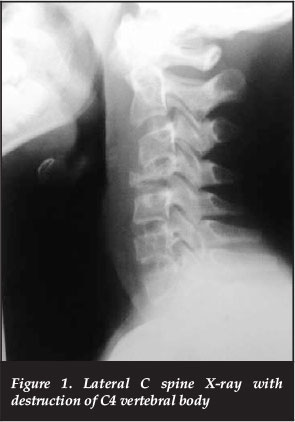
X-ray examinations identified collapse of the C4 vertebral body with preservation of adjacent discs and posterior elements
On examination, there was posterior midline tenderness over the C4 vertebra and reduced range of motion, especially rotation. The neurological examination was normal.
X-ray examinations identified collapse of the C4 vertebral body with preservation of adjacent discs and posterior elements (Figure 1). Her chest X-ray was normal. Laboratory investigations showed a raised CRP of 16.6 mg/L and an ESR of 47 mm/hour. Her WCC was 9.95 χ 109.
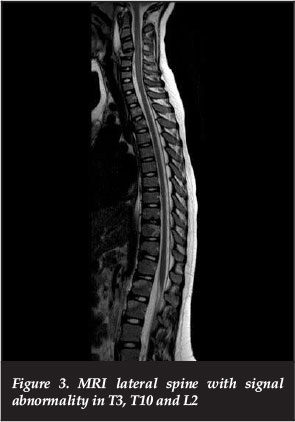
A working diagnosis of atypical tuberculosis was made -atypical due to the single body involvement. The Mantoux test was negative. The MRI confirmed collapse of the C4 vertebra with anterior extrusion of the vertebral body content into the prevertebral space. There was a prever-tebral collection extending from C1-C5 (Figure 2). Similar signal abnormalities were present in vertebral body of T3, T10 and L2 (Figure 3).

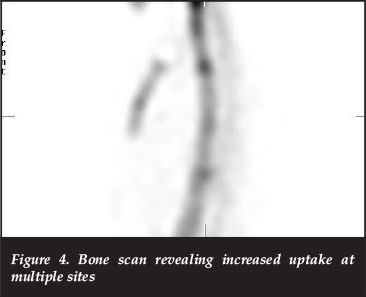
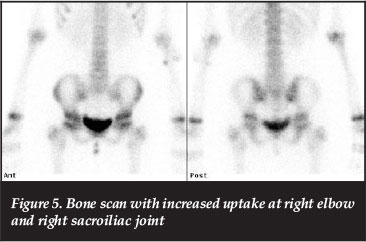
A technetium-99m bone scan demonstrated increased uptake in the C4, T3 and T12 vertebrae (Figure 4), as well as increased uptake in the right elbow and the right sacroiliac joint (Figure 5). X-rays of the elbow and sacroiliac joint revealed no abnormalities.
An open biopsy of the C4 vertebral body was performed via the Smith-Robinson approach and multiple specimens were sent for laboratory evaluation.
Histology of the bony fragments confirmed granulation tissue with a mixed acute and chronic inflammatory infiltrate and a focal foreign body granulomatous reaction to necrotic bony fragments. There was no evidence of caseation (Figure 6).
Multiple Ziehl-Nielsen stains on the tissue samples were negative for acid-fast bacilli. Polymerase chain reaction (PCR) and cultures for tuberculosis were also negative.1 Aerobic cultures isolated a Pantoea species.
Although this can be a contaminant, the biopsy was a sterile procedure and histology confirmed chronic, non-caseating inflammation. All the TB tests were negative and the diagnosis of Pantoea multifocal osteomyelitis was made. The patient was managed with a six-week course of amoxicillin clavulanate 375 mg 8 hourly.
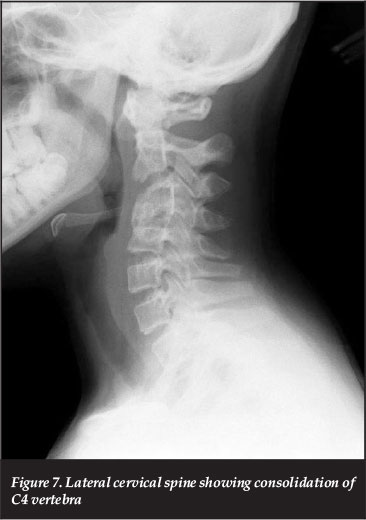
At the six-week follow-up the patient was pain-free and X-rays confirmed healing of the C4 vertebra with some kyphosis (Figure 7). A follow-up bone scan showed normal uptake at the previous abnormal sites of the elbow, sacroiliac joint, T3 and T12 vertebrae. Increased uptake at level C3/C4 was reported as a result of healing rather than continuing infection. A follow-up MRI confirmed that the prevertebral collection had resolved and no further changes were noted at levels T3, T10 and L2. The patient will be followed up until skeletal maturity due to the risk of progression of kyphosis.
Discussion
Pantoea agglomerans, previously known as Enterobacter agglomerans, is a Gram-negative bacterium from the Enterobacteriaceae family. It is mainly a plant epiphyte commonly found on plant material and in soil, but it has been reported as an opportunistic pathogen in humans.2,3 Destructive bone lesions after direct penetrating injuries have been described. It is an uncommon cause, with only 31 cases found in the literature (Pantoea was however not isolated in all 31 cases).4,5 Durr et al. published a case report of a destructive lesion in the first metatarsal bone. It was thought to be a tumour, but on biopsy a 2 cm thorn was found within the lesion. The cortex of the metatarsal was destroyed and replaced with granulation tissue. Histology revealed chronic granulation and Pantoea agglomerans was isolated in cultures.4
Further reports of ten cases of osteomyelitis were found: one case after an open fracture, eight cases associated with penetrating injuries without fractures and one case after a closed fracture with overlying abrasions.3,6
A single case of discitis caused by Pantoea has been reported. The case involved a 22-year-old farmer on long-term tetracycline therapy for acne. The author postulated that the patient's normal flora may have been altered and was colonised by Pantoea.7
This case report is unique as no direct inoculation occurred and haematogenous spread from an unnoticed skin penetration is the presumed cause. The child was not on long-term antibiotics or immunocompromised to predispose her to opportunistic infections.
Although Pantoea agglomerans is a rare cause of infection of the spine, it may be worth including in a differential diagnosis. Currently Pantoea agglomerans strains are considered as promising biocontrol agents for a number of bacterial and fungal plant diseases by the agricultural industry. Several strains of Pantoea agglomerans are already registered and sold as commercial biocontrol agents in New Zealand, the United States and Canada.8 In future contact with and interaction between humans and Pantoea agglomerans are bound to increase.
This case report is unique as no direct inoculation occurred and haematogenous spread from an unnoticed skin penetration is the presumed cause
This case highlights the need for biopsy and culture-guided antibiotic treatment rather than empiric antibiotic treatment. Due to the favourable antibiotic resistance profile, the Pantoea infection would have resolved with nearly any antibiotic regimen, including tuberculosis treatment. This would have exposed the patient to an unnecessary prolonged antibiotic course with multiple side effects.9,10
The content of this article is the sole work of the authors. No benefits in any form have been or are to be received from a commercial party related directly or indirectly to the subject of this article. Ethics approval was obtained from the University of Cape Town Ethics Committee as well as informed consent from the parents of the patient.
References
1. Laubscher M, Held M, Zar HJ, Dunn R. GeneXpert polymerase chain reaction for spinal tuberculosis - An accurate and rapid diagnostic test. Valencia: s.n., 2014. IMAST Meeting. [ Links ]
2. Andrews JH, Harris RF. The ecology and biogeography of microorganisms on plant surfaces. Annual Review Phytopathology 2000; 38: 145 - 180. [ Links ]
3. Cruz AT, Cazacu AC, Allen CH. Pantoea agglomerans, a plant pathogen causing human disease. Journal of Clinical Microbiology 2007; June: 1989 - 1992. [ Links ]
4. Durr HR, Muller PE, Refior HJ. Thorn-induced pseudotumor of the metatarsal. The Journal of Bone & Joint Surgery 2001; April: 580 - 585. [ Links ]
5. Kratz A. Pantoea agglomerans as a cause of septic arthritis after palm tree thorn in jury. Arch Dis Child 2003; 88: 542-544. [ Links ]
6. Labianca L, Montanaro A, Turturbo F. Osteomyelitis caused by Pantoea agglomerans in a closed fracture in a child. Orthopedics 2013; 36: 252 - 256. [ Links ]
7. Porter P, Wray C. Enterobacter agglomerans spondy-lodiscitis. Spine 2000; 25: 1287 - 1289. [ Links ]
8. Rezzonico F, Smits T, Montesinos E, Frey J, Duffy B. Genotypic comparison of Pantoea agglomerans plant and clinical strains. BMC Microbiology 2009; 9: 204. [ Links ]
9. Yee D, Valiquette C, Pelletier M, Parisien I, Rocher I, Menzies D. Incidence of serious side effects from first line antituberculosis drugs among patients treated for active tuberculosis. American Journal of Respiratory and Critical Medicine 2003; 167: 1472 - 1477. [ Links ]
10. Schaberg T, Rebhan K, Lode H. Risk factors for Side-effects of isoniazid, rifampin and pyrazinamide in patients hospitalized for pulmonary tuberculosis. European Respiratory Journal 1996; 9: 2026 - 2030. [ Links ]
 Correspondence:
Correspondence:
Dr C de V Marais
Email: Christoff_marais@yahoo.com














