Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SA Orthopaedic Journal
On-line version ISSN 2309-8309
Print version ISSN 1681-150X
SA orthop. j. vol.14 n.1 Centurion Feb./Mar. 2015
SHOULDER
Biceps pulley lesions associated with subscapularis tears and subacromial impingement: The triad of the rotator interval lesion
M HeldI; S RocheII; M LaubscherII; P MagoschIII; S LichtenbergIII; P HabermeyerIV; B VrettosV
IFC(Orth)(SA), MMed(SA); Orthopaedic Department, Groote Schuur Hospital, University of Cape Town
IIFC(Orth)(SA); Orthopaedic Department, Groote Schuur Hospital, University of Cape Town
IIIDr med; Department of Shoulder and Elbow Surgery, Atos Klinik, Heidelberg, Germany
IVPhD; Department of Shoulder and Elbow Surgery, Atos Klinik, Heidelberg, Germany
VMBChB, LRCP, LRCS, LRCP S, FRCS(Eng), FCS(SA)Orth, MMed(Orth)UCT; Orthopaedic Research Unit, University of Cape Town
ABSTRACT
AIM: The aim of this study was to describe the association of biceps pulley lesions with subscapularis tendon tears and subacromial impingement, and present the outcome of surgical management
METHODS: Twenty-six consecutive patients with a mean age of 55 years (range 16-77) were included in this study. All of the patients were arthroscopically diagnosed with pulley lesions and associated subscapularis tears. The data was collected prospectively. Subacromial impingement was evident in 22 patients (92%). A final postoperative evaluation was carried out after a mean of 43 months
RESULTS: Ninety-two per cent of patients with pulley lesions and subscapularis tears showed subacromial impingement. Twelve cases (46%) had a selective tenodesis to treat partial tears or subluxations of the long head of the biceps (LHB). Subscapularis tears were repaired in 22 patients (85%) and debrided in four cases (15%). Associated SSP tears were sutured in nine and debrided in four of 13 patients. The Constant score improved from a mean of 64.8 points pre-operatively to 84.7 points post-operatively (P=0.003
CONCLUSION: There is a high association of pulley lesions with subscapularis tears and subacromial impingement. Rotator cuff repair and subacromial decompression led to favourable results in the treatment of these patients. LHB tenodesis is recommended if partial tears or subluxations of the biceps tendon are encountered
Key words: pulley lesion, subscapularis lesion, long head of biceps, rotator interval, subacromial impingement
Introduction
The prevalence of pulley lesions is thought to be between 7% and 18% for all patients undergoing diagnostic arthroscopy of the shoulder.1,2 This increases to 79% for those with rotator cuff tears and 73% specifically for patients with subscapularis tendon tears.3 Walch et al.
showed massive rotator cuff tears in 70% of dislocations of the long head of biceps (LHB).4
The tendon of the LHB originates from the superior glenoid rim and follows a course through the joint, which is almost perpendicular to the conduit within the bicipital groove. The exit from the joint is reinforced by the pulley system, acting as a tendoligamentous sling (Figure 1).
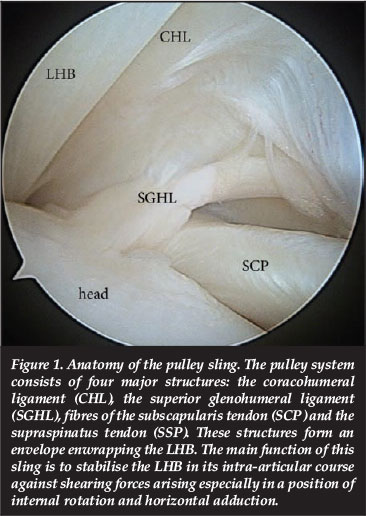
This sling is a component of the rotator interval, a triangular part of the capsule located between the supraspinatus (SSP) and the subscapularis (SCP) tendon.5,6 The main function of the sling is to stabilise the LHB in its intra-articular course against shearing forces arising especially in a position of internal rotation and horizontal adduction.7,8 As part of the rotator interval this pulley system consists of four major structures:9 the coraco-humeral ligament (CHL), the superior glenohumeral ligament (SGHL), and fibres of the subscapularis tendon (SCP) and the supraspinatus tendon (SSP). The CHL originates from the coracoid process and inserts on the greater and lesser tuberosity of the humeral head. Together with fibres of the SSP it forms the roof of the pulley system.10 The SGHL originates from the anterosuperior rim of the labrum and leads to the proximal part of the lesser tuberosity. Its medial aspect forms a pouch parallel to the course of the LHB. Further lateral it transforms into the u-shaped floor of the pulley system, reinforced by fibres of the subscapularis.9 Internal rotation and adduction in the horizontal plane lead to subluxation of the LHB in the presence of a pulley lesion. As the LHB glides over the humeral head it causes partial articular-side tears of the rotator cuff. Depending on the movement of the shoulder this leads to lesions of the SCP tendon during a medial subluxation and of the SSP tendon during a lateral subluxation. As the condition advances the LHB wipes over the cartilage of the humeral head causing chondral lesions, known as the windshield-wiper mechanism.11
Habermeyer et at.11divided intra-articular pulley lesions into four groups (Figure 2):
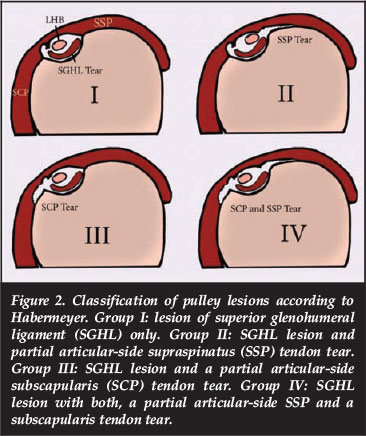
- Group I: SGHL lesion only
- Group II: SGHL lesion and partial articular-side SSP tendon tear
- Group III: SGHL lesion and a partial articular-side SCP tendon tear
- Group IV: SGHL lesion with both, a partial articular-side SSP and a SCP tendon tear
Lesions of the pulley system can be caused either by trauma or through degenerative changes. A fall on the outstretched arm in full internal or full external rotation, as well as a fall backwards on the hand or elbow is the most common traumatic mechanism. Intrinsic changes of the pulley system are thought to be caused by anterior superior impingement (ASI), which describes an internal impingement of the biceps and SCP tendon against the anterior superior glenoid.12 Furthermore, repetitive active contraction of the biceps in internal rotation is believed to cause strain on the pulley sling.9 A sudden stop of the forearm during deceleration of elbow extension amplifies this tension, such as in a throwing or batting athlete.11 This eventually leads to lesions of the pulley sling.
The purpose of this study was to establish the association of pulley lesions with biceps subluxations, SCP tears and subacromial impingement and to assess the treatment of this triad of pathology around the rotator interval.
Methods
This study included 26 (21 male) consecutive patients who were diagnosed with an associated pulley lesion and SCP tear during a standardised intra-operative diagnostic arthroscopy. Their mean age was 55 years (range 16-77). Pre- and post-operative evaluation for impingement, biceps tendon pathology and rotator cuff tears were collected prospectively. A final post-operative evaluation was carried out on average 43 months after the intervention (range: 31-87). Seventeen patients (65%) were evaluated based on a clinical assessment and Constant score performed by one shoulder surgeon. The remaining nine (35%) patients completed and sent back a questionnaire (patient-based Constant score) for evaluation purposes. Data obtained from a Constant score with a surveyor present and the data obtained from a patient-based Constant score correlate significantly, therefore comparison of the two is acceptable.13 Anteroposterior X-rays, Y-views and SSP outlet views of the affected shoulder were obtained in all patients.
Arthroscopic technique
For the standardised arthroscopic examination, all patients were placed in the beach-chair position. The scope was introduced through a standard posterior portal. The glenohumeral inspection started from origin of the LHB. Its intra-articular and intertubercular course was assessed with a probe. After the examination of the LHB, the articular side of the SSP tendon and the articular side of the SCP tendon were inspected. The anterosuperior glenoid rim and labral structures were examined. The subacromial space was evaluated through the posterior portal. All arthroscopic findings were documented using a standardised shoulder documentation sheet.
Lesions of the LHB were treated with soft tissue tenodesis. Partial tears of the rotator cuff were debrided with a shaver system, and lesions of more than 50% involving the osseous attachment of the tendon were repaired with a suture anchor. The decision to perform subacromial decompression as described by Ellmann14 was based on typical signs of subacromial impingement such as fraying or the occurrence of a bone spur on the under-surface of the acromion. Furthermore, clinical and radiological findings of an active acromio-clavicular (AC) joint osteoarthritis led to the decision to perform an arthroscopic AC-joint resection.
Statistical methods
The univariate analysis of the data was performed using SPSS, version 13.0 for Windows (Inc. Chicago, Illinois). With the following nominal data, relative frequencies were calculated: pain at rest, pain during motion, pain at night, pain due to strain, as well as all the test results of the clinical examination such as impingement tests and rotator cuff tests.
Furthermore, a standard deviation and mean value were described for the following metrical data: strength measurements, Constant score results in points and percentage, age, and for the time passed until postoperative assessment in months. The comparison of the metrical data of the patient groups was determined using the Wilcoxon-Signed-Ranks Test. The Mann-Whitney-U Test was carried out to calculate differences within a patient group (pre- versus post-operative). In addition, binominal tests were used to analyse the discrepancy of the nominal data.
Results
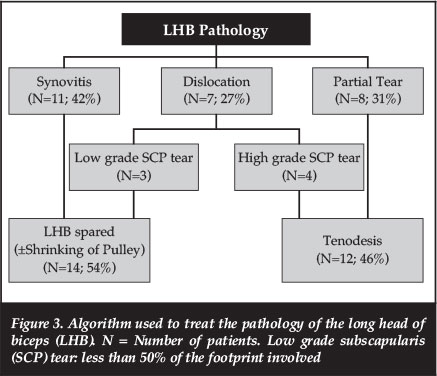
All 26 patients had a pulley lesion confirmed during diagnostic arthroscopy. Two patients sustained their injury due to a fall. The other 24 patients' pathology was attributed to degenerative changes. The SGHL was ruptured in 14 patients (54%) and elongated in 12 patients (46%). Thirteen patients (50%) had an isolated SCP tendon tear (Habermeyer Grade 3). The remaining 13 patients (50%) had a combination of SCP and SSP tendon tears (Grade 4). The LHB was dislocated in seven patients (27%), partial LHB tears were present in eight patients (31%) and synovitis of the LHB was found in 11 patients (42%). The SCP tendon was sutured in 22 patients (85%) and debrided in four cases (15%). The SSP tendon was sutured in nine of the 13 patients in group 4, and debrided in the other four patients. A LHB tenodesis was done in 12 cases (46%). Eight of these 12 patients had a partial tear of the LHB. The remaining four had a dislocation of the LHB. The LHB was left alone in 14 patients (54%), 11 of these patients showed a synovitis, and three patients had a dislocated LHB. These three patients had suturing of the SGHL. Seven of the remaining 11 patients had their pulley lesion treated with shrinking of the SGHL (Figure 3). Twenty-two patients (92%) showed signs of subacromial fraying and an acromioplasty was performed in these cases.
The decision to perform subacromial decompression as described by Ellmann14 was based on typical signs of subacromial impingement
The post-operative evaluation showed a significant improvement in impingement tests, rotator cuff tests and LHB tests as well as in Constant scores. Pre-operative Neer Test and Hawkins Test were used to assess impingement and were positive in 20 patients (77%) and 15 patients (58%) respectively. In all these patients the evidence of subacromial impingement was confirmed during diagnostic arthroscopy. All these tests became negative at post-operative follow-up (P<0.001). The Palm-up Test and O'Brien Test were used to assess the LHB. The pre-operative Palm-up Test was positive in 16 patients (61.5%), and 14 patients (54%) had a positive O'Brien Test. These were all negative post-operatively (P<0.001).
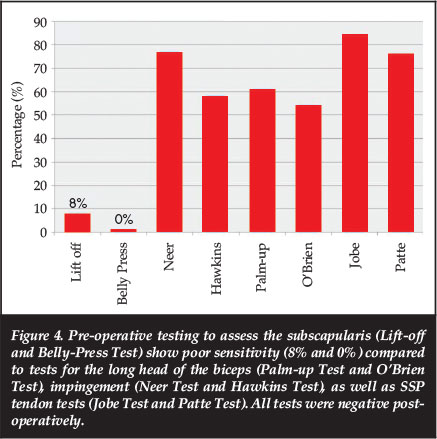
The SSP tendon was assessed with tests described by Jobe and Patte, which were positive in 22 patients (84%) and 20 patients (76%) respectively (Figure 4). The postoperative tests were negative in all of the patients (P<0.001). The SCP tests (Lift-off and Belly-Press) showed poor sensitivity with correct positive testing in only 8% (Lift-off) and 0% (Belly-Press). None of the patients tested positive after the operation. The Constant score was documented in points and improved significantly from a mean of 66.3 (range: 40-83) to 84.7 (range: 65-100) points post-operatively (P=0.003).
Discussion
The pulley system of the LHB tendon acts as a sling securing the tendon within the bicipital groove. If this mechanism is lost, the LHB dislocates out of the sling and wipes over the head of the humerus causing rotator cuff tears and later on osteochondral lesions.11 A progression of these events is likely, unless the initial pathology is addressed. The focus should therefore lie in preventing the LHB from dislocating out of the sulcus. Three patients from a group of 14 (54%) in whom the SGHL was ruptured presented with a dislocated LHB and only had minor SCP tendon tears involving less than 50% of the footprint. In these cases we decided to suture the SGHL. Seven of 11 patients with LHB synovitis had an elongated pulley sling and were treated with electro-thermal shrinking. All of these patients presented with low grade rotator cuff tears. On the other hand, a tenodesis or tenotomy was performed in all of our patients with partial tears of the LHB (eight patients, 31%) and in dislocations of the LHB with associated high grade SCP tendon tears involving more than 50% of the footprint (four patients, 16%). We used the Palm-up Test and O'Brien Test to assess the LHB. A pre-operative Palm-up Test was positive in 16 patients (61.5%) and 14 patients had a positive O'Brien-Test. Post-operatively, all of the tested patients showed a significant improvement as none of them tested positive (P<0.001).
The SCP tendon tears were classified according to Fox15 and SSP tendon tears according to Ellmann.16 We regarded tears with an involvement of the footprint of more than 50% to be an indication for an arthroscopic rotator cuff repair. The SCP tendon was sutured in 22 patients (85%) and debrided in four cases (15%). The SSP tendon was sutured in nine of the 13 patients in group 4, and debrided in four of 13 patients in this group. The SSP tendon was assessed with tests described by Jobe and Patte, which were positive in 22 patients (84%) and 20 patients (76%) respectively. The post-operative tests showed a significant improvement and were negative in all of the patients (P<0.001). The SCP tests such as the Lift-off and Belly-Press tests showed a poor sensitivity in our pre-operative testing with correct positive testing in only 8% (Lift-off) and 0% (Belly-Press). Various studies have shown a high variability of sensitivities for SCP tendon tests and some of the authors describe their own clinical test, which increases sensitivities up to 88%.17-20 This might be due to the fact that SCP tendon tears rarely occur as an isolated pathology and are often associated with tears of other rotator cuff tendons, subacromial impingement and LHB pathologies.1, 3, 18 This might have confounded clinical testing in our study and we might have to rely more on pre-operative imaging with ultrasound or MRI studies to give a more accurate assessment of the SCP tendon in future.21
Our study had some weaknesses. We did not include a control group of patients in whom the LHB was left alone, as we felt this would have been suboptimal in cases of dislocations or partial tears of the LHB.
Furthermore, our study showed a heterogeneous spectrum of pathology with a high prevalence of subacromial impingement (92%). It can be argued that the improvement in our post-operative assessment could simply result from subacromial decompression rather than addressing pulley lesions, LHB dislocations and low-grade rotator cuff tears. Yet, the subacromial impingement may be seen as a consequence of the pulley lesion and subsequent dislocation of the biceps tendon rather than a separate pathological entity. In pulley lesions, the compressive joint retraction mechanism of the LHB and the rotator cuff is lost and as a result, the humeral head migrates into an anterosuperior position, causing impingement of structures such as the rotator cuff and the pulley system itself.11, 22 The involvement of the subacromial space due to superior migration is a natural progression of this process leading to subacromial impingement. The question why tenodesis of the LHB should lead to a decrease rather than an increase in the glenohumeral joint compression force has been raised. We believe the main purpose of the tenodesis, especially in partial tears and dislocations, is to prevent further damage to the repair of the rotator cuff, which regains its function of glenohumeral centring. Furthermore, scarring and tightening of the rotator interval after suturing or shrinking of the SGHL may play a role in counteracting an upward migration of the humeral head, although the impact of this has not been established.
Conclusion
In 92% patients with SCP tears and associated pulley lesions, subacromial impingement was evident. Subacromial decompression and SCP tendon repair seems favourable in these patients. Tenodesis of the LHB should be considered in cases of partial tears or dislocations of the LHB to avoid jeopardising the repair of the SCP tendon. We further noticed that clinical testing for SCP tears has a poor sensitivity when associated with pulley lesions.
The authors did not and will not receive any commercial benefits for this study.
References
1. Baumann B, Genning K, B/dhm D, Rolf O, Gohlke F. Arthroscopic prevalence of pulley lesions in 1007 consecutive patients. Journal of shoulder and elbow surgery / American Shoulder and Elbow Surgeons [et al] 2008;17:14-20. [ Links ]
2. Bennett WF. Subscapularis, medial, and lateral head coraco-humeral ligament insertion anatomy. Arthroscopic appearance and incidence of 'hidden' rotator interval lesions. Arthroscopy 2001;17:173-80. [ Links ]
3. Braun S, Horan MP, Elser F, Millett PJ. Lesions of the biceps pulley. The American Journal of Sports Medicine 2011;39:790-95. [ Links ]
4. Walch G, Nove-Josserand L, Boileau P, Levigne C. Subluxations and dislocations of the tendon of the long head of the biceps. J Shoulder Elbow Surg 1998;7:100-8. [ Links ]
5. Neer CS, 2nd. Impingement lesions. Clin Orthop Relat Res 1983:70-7. [ Links ]
6. Harryman DT, 2nd, Sidles JA, Harris SL, Matsen FA, 3rd. The role of the rotator interval capsule in passive motion and stability of the shoulder. J Bone Joint Surg Am 1992;74:53-66. [ Links ]
7. Habermeyer P. [Tendon ruptures of the shoulder]. Orthopade 1989;18:257-66; discussion 66-7. [ Links ]
8. Kask K, Pvuldoja E, Lont Tn, et al. Anatomy of the superior glenohumeral ligament. Journal of Shoulder and Elbow Surgery I American Shoulder and Elbow Surgeons [et al] 2010;19:908-16. [ Links ]
9. Werner A, Mueller T, Boehm D, Gohlke F. The stabilizing sling for the long head of the biceps tendon in the rotator cuff interval. A histoanatomic study. Am J Sports Med 2000;28:28-31. [ Links ]
10. Gaskill TR, Braun S, Millett PJ. Multimedia article. The rotator interval: pathology and management. Arthroscopy 2011;27:556-67. Epub 2011 Feb 4. [ Links ]
11. Habermeyer P, Magosch P, Pritsch M, Scheibel MT, Lichtenberg S. Anterosuperior impingement of the shoulder as a result of pulley lesions: A prospective arthroscopic study. J Shoulder Elbow Surg 2004;13:5-12. [ Links ]
12. Gerber C, Sebesta A. Impingement of the deep surface of the subscapularis tendon and the reflection pulley on the antero-superior glenoid rim: A preliminary report. J Shoulder and Elbow Surg. 2000; 9:483-90. [ Links ]
13. Boehm D, Wollmerstedt N, Doesch M, Handwerker M, Mehling E, Gohlke F. [Development of a questionnaire based on the Constant-Murley-Score for self-evaluation of shoulder function by patients]. Unfallchirurg 2004;107:397-402. [ Links ]
14. Ellman H, Kay SP: Arthroscopic subacromial decompression for chronic impingement. Two- to five-year results. 1991; 73:395-98. [ Links ]
15. Fox J, romeo AA. Subscapularis tendon tear: Fox and Romeo classification. In: annual meeting of AAOS; 2003. [ Links ]
16. Ellman H. Diagnosis and treatment of incomplete rotator cuff tears. Clin Orthop Relat Res 1990:10. [ Links ]
17. Tokish JM, Decker MJ, Ellis HB, Torry MR, Hawkins RJ. The belly-press test for the physical examination of the subscapu-laris muscle: electromyographic validation and comparison to the lift-off test. J Shoulder Elbow Surg 2003;12:427-30. [ Links ]
18. Gerber C, Krushell RJ. Isolated rupture of the tendon of the subscapularis muscle. Clinical features in 16 cases. J Bone Joint Surg Br 1991;73:389-94. [ Links ]
19. Scheibel M, Magosch P, Pritsch M, Lichtenberg S, Habermeyer P. The belly-off sign: a new clinical diagnostic sign for subscapularis lesions. Arthroscopy 2005;21:1229-35. [ Links ]
20. Barth JR, Burkhart SS, De Beer JF. The bear-hug test: a new and sensitive test for diagnosing a subscapularis tear. Arthroscopy 2006;22:1076-84. [ Links ]
21. Nakata W, Katou S, Fujita A, Nakata M, Lefor AT, Sugimoto H. Biceps pulley: normal anatomy and associated lesions at MR arthrography. Radiographics 2011;31:791-810. [ Links ]
22. Pagnani MJ, Deng XH, Warren RF, Torzilli PA, O'Brien SJ. Role of the long head of the biceps brachii in glenohumeral stability: a biomechanical study in cadavera. J Shoulder Elbow Surg 1996;5:255-62. [ Links ]
 Correspondence:
Correspondence:
Michael Held, MD
Orthopaedic Department, Groote Schuur Hospital
University of Cape Town Address: H49 Old Main Building, Groote Schuur Hospital, Observatory 7925, RSA
Tel: 0027 214066157; Fax: 0027 21472709
Email: Michael.held@uct.ac.za
Statistician:
H Carrara
University of Cape Town
Email: henry.carrara@uct.ac.za














