Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SA Orthopaedic Journal
On-line version ISSN 2309-8309
Print version ISSN 1681-150X
SA orthop. j. vol.13 n.2 Centurion Apr./Aug. 2014
SPINE
Atlanto-axial fusion: Magerl transarticular versus Harms instrumentation techniques
RN DunnI; H StanderII
IMBChB, MMed, FCS(SA) Orth; Pieter Moll and Nuffield Chair of Orthopaedic Surgery
IIMBChB(Stell), FCOrth(SA); Registrar (at time of study) Department of Orthopaedic Surgery, University of Cape Town
ABSTRACT
Transarticular screw fixation offers acceptably high fusion rates but is not possible in 18% of patients due to a high riding vertebral artery. It also requires pre-operative anatomical reduction which is not always possible.
The Harms technique utilises a posterior C1 lateral mass and C2 pedicle screw. This allows easier access due to the angle of drilling and has become an increasingly popular surgical technique.
AIM: The aim of this study is to review and compare the above techniques with regard to surgery, complications and outcome.
METHODS: A retrospective case note and radiographic review of 42 patients undergoing posterior C1-2 fusion in a single institution during the period 2003 to 2011, identified on a prospectively maintained database, was performed.
The indication for surgery was atlanto-axial instability with post-traumatic and rheumatoid arthritis the commonest aetiologies. There was no difference in age and gender between the two groups.
RESULTS: The Harms method had a slightly higher mean blood loss compared to the transarticular method. The surgical time was no different.
The transarticular technique was abandoned in three cases due to inability to place the screw safely. The Harms technique was successfully completed in all cases.
There were four unilateral vertebral artery injuries in the transarticular group and one in the Harms group.
There were three intra-operative unintentional durotomies in the transarticular group with one in the Harms.
All but one transarticular case fused, with five transarticular cases taking more than 9 months.
CONCLUSION: Although the Harms technique had an increased blood loss, the incidence of vertebral artery and dura injury was lower. Fusion was similar in both groups with the only non-union occurring in the transarticular group.
The Harms technique offers the advantage of intra-operative reduction and a smaller exposure due to the direction of access but at a higher instrumentation cost.
Key words: atlanto-axial fusion, Harms, transarticular
Introduction
Atlanto-axial instability may occur following indirect trauma resulting in transverse ligament disruption or dens fracture. It may also occur insidiously in inflammatory conditions such as rheumatoid arthritis with progressive attenuation of the transverse ligament. Less frequently it may be associated with dysplasias such as achondroplasia, Down's syndrome with a small dens or mucopolysaccha-ridosis such as Morquio syndrome.
Traditional wiring techniques such as the Gallie and Brookes are technically simple but provide poor biome-chanical control necessitating concomitant rigid external orthosis application and unacceptable non-union rates.1
Magerl's transarticular screw fixation offers high fusion rates but is not possible in 18% of patients due to a high riding vertebral artery.2 It also requires pre-instrumen-tation anatomical reduction which is not always possible. Access can also be a problem due to thoracic kyphosis hindering drill direction.
The Harms technique utilises a posterior C1 lateral mass and C2 pedicle screw.3 This allows easier access due to the more perpendicular direction of drilling and has become an increasingly popular surgical technique.
The aim of this study is to compare the above techniques with regard to surgery, complications and outcome.
Material and methods
Following institutional research ethics committee approval, a retrospective case note and radiographic review was performed on all patients undergoing posterior C1-C2 fusion by the senior author.
Forty-two consecutive patients were identified from a prospectively maintained database. Twenty-seven underwent transarticular fusion and 15 the Harms technique. This largely represented a change in the surgeon's choice of procedure, initially performing the transarticular technique as the default operation with transition to the Harms procedure.
The two groups were similar in terms of age and gender. The median age was 43 years (21-69 ± 15.7) in the transarticular group and 35 (12-74 ± 20.7) in the Harms group. The difference was not statistically significant (p=0.14). There were 18 males and nine females in the transarticular compared to nine males and seven females in the Harms group (p=0.53)
In both techniques the patient was positioned prone on a Relton Hall frame with the skull held with a Mayfield clamp. The neck was positioned to optimise access by slight flexion at the occiput but extended in the sub-axial spine. An attempt was made to reduce the C1-2 articulation during this positioning process. Both procedures were performed with lateral fluoroscopy only.
A midline incision was made over C1-2 but extended distally in the transarticular group to allow the required drill angulation. Sub-periosteal exposure of the C1 arch and C2 posterior elements was done. A right-angled hook was used to run on the inner cortex of the C2 lamina in a lateral direction to palpate the medial isthmus, and thus the medial border of the screw placement.
In the transarticular group, a starting point was based about 2-3 mm lateral to this medial isthmic palpation, inferiorly on the C2 lamina, directed in a cephalad direction and neutral in terms of medial-lateral angulation. This was done under lateral image guidance. The C1-2 joint was crossed and anterior C1 lateral mass perforated. Titanium 3.5 mm cortical screws were placed (Figure 1).
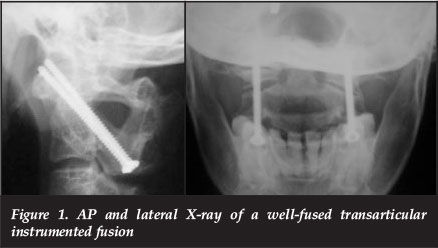
In the Harms group, the posterior aspect of the C1 lateral mass was visualised after sub-periosteal exposure of the posterior arch and a plane developed inferiorly onto the lateral mass. A Watson-Cheyne was placed into the C1-2 joint, after penetrating the capsule, to allow inferior retraction of the C2 root and improve access to the entry point. A burr was used to create a cortical breach in the lateral mass as it joins the arch superiorly. This allowed stable initial placement of the 2.7 mm drill bit. The path was drilled parallel to the arch with 10-15° convergence. This was observed on lateral image while drilling. A screw was placed with the tulip at the level of the arch, i.e. part of the proximal screw shaft remained visible. C2 pedicle screws were then placed under lateral image after medial isthmic/ pedicle palpation (Figure 2).
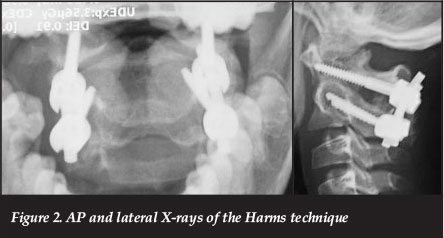
Cortico-cancellous bone graft was harvested from the iliac crest in all cases and placed from the C1 arch to C2 lamina.
Patients were managed in a Philadelphia collar when up, for 6 weeks.
Patient demographics, surgical indications, intra-operative variables, complications and radiographic outcome were assessed. X-rays pre-op, post-op, and follow-up at 6 weeks, 3 months, 6 months, 12 months and 24 months were evaluated for successful instrumentation and subsequent fusion.
Results
Trauma predominated over aetiology by accounting for half the cases. The remainder was due to rheumatoid arthritis, os odontoidium, a pathological fracture from tuberculosis and neurofibromatosis-related destruction. This is tabulated in Table I.
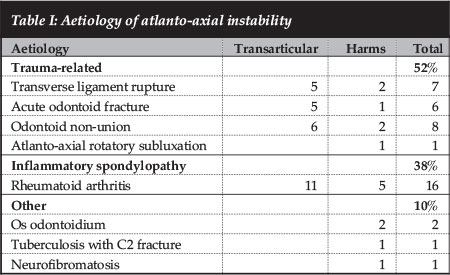
There was a small statistically significant difference in blood loss between the two groups with a median of 150 ml in the transarticular group and 250 ml in the Harms group. When considering the number of cases that bled more than 500 ml, it was clearly more frequent in the Harms group (p=0.016). The cases that bled excessively were two rheumatoid cases (one converted from an aborted transarticular screw), two Dens non-unions and the tuberculosis pathological fracture. There was no difference in surgical time between the two techniques (Table II).
The transarticular technique was abandoned in three cases due to inability to place the screw safely. The Harms technique was successfully completed in all cases.
There were five unilateral vertebral artery injuries, four in the transarticular group and one in the Harms group. These were easily controlled with screw placement in the former group but the other side not drilled. The Harms injury occurred while tapping for the C1 screw and lacerating the artery as it passes on the C1 arch. The patients suffered no clinically evident effect from the single vertebral artery injuries (Table III).
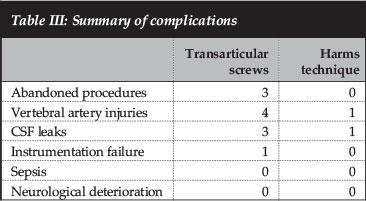
There were four intra-operative unintentional durotomies with CSF leaks. Three were in the transar-ticular group. These were successfully dealt with at the time of surgery with surgical, muscle and/ or Duroseal.
There was one case of instrumentation failure with bilateral screw fracture in the transarticular group. Despite this the patient went onto successful fusion.
There were no cases of neurological deterioration or sepsis.
Median time to union was similar in both groups at around 5 months (Table IV). All Harms patients were fused by 9 months, with 18% of the transarticular group taking longer than this and one requiring revision for an established non-union.
Discussion
Atlanto-axial instability is a concern due to the risk of myelopathy and sudden death from proximal spinal cord compression.4 The decision to arthrodese the joint is based on the appreciation of this risk and the expectation that stabilisation will not occur spontaneously with conservative means.
In the case of trauma, transverse ligamentous rupture recognised by an atlanto-dens interval of more than 5 mm on the lateral X-ray, is a clear indication as it is not expected to heal.5 Dens fractures however may heal with restriction of motion but older patients, with marked displacement or angulation are recognised as a high non-union risk. Theoretically, anterior Dens osteosynthesis allows stabilisation without rotational motion sacrifice but this is often not the case due to spontaneous loss of motion.5,6 This may be due to associated C1-2 joint injury or the period of postoperative immobilisation and local inflammatory response to injury and surgery. In addition, reverse oblique fractures are not amenable to screw fixation. In non-compliant patients, rigid posterior fusion is the better option in our opinion.
Historically, uninstrumented and posterior wiring techniques (Gallie and Brookes) have been employed.7 Although simple they provide poor biomechanical control of translation and necessitate rigid external orthoses and have a high non-union risk.
Magerl described the transarticular technique.2 It offers a stable construct which can be augmented with a posterior tension band between the C1 arch and C2 spine with so-called three-point fixation. This technique is demanding as it requires passage of the drill bit and screw medial and superior to the vertebral artery as it exits C2. Up to 18% of patients have a high riding artery precluding this technique. We have also anecdotally noted that advanced rheumatoid patients tend to have enlarged vertebral artery foramina leaving less bone available for safe screw passage. The risk of vertebral artery injury is 5% per case.8 Although a single vertebral artery injury is usually not clinically significant, it creates surgeon distress and necessitates an alternative technique if it occurs with the first screw as the second artery cannot be risked.
The technique also demands anatomical reduction of C1 and C2 to allow a safe trajectory of the drill and subsequent screw. This is not always possible and can be difficult to maintain once reduced.9
The Harms technique is initially more challenging to the surgeon as it requires visualisation of the C1 lateral masses which are a least a centimetre deep to the arch.3 The access can be difficult and excessive epidural bleeding can be encountered, which obliterates the surgeon's view and prevents safe drill placement. This is due to the extensive venous plexus or epidural mesh of veins over the C2 root and posterior thecal sac. It is difficult to control with bipolar as once cauterised, the venous walls become hard and crack easily with further dissection increasing the bleeding. Through trial and error, we have found the most efficient access is by sub-periosteal dissection on the inferior half of the C1 arch. The sharp side of the Watson -Cheyne is used to lift to the periosteum inferiorly, creating a path on the posterior aspect of the C1 lateral mass.
The Harms technique is initially more challenging to the surgeon as it requires visualisation of the CI lateral masses
The Watson-Cheyne is then punctured into the C1-2 joint capsule bearing in mind the oblique nature form supero-medial to infero-lateral. This is then levered inferiorly by the assistant to retract the C2 root and create space over the C1 lateral mass. Usually the surgeon retracts the space medially or laterally with a small sucker tip and creates a cortical notch under vision with a burr at the apex of the lateral mass where it joins the arch. There may be venous bleeding from laterally around the vertebral artery which can be controlled with a small patty. The drill is then placed in the starter hole and directed parallel to the C1 arch, assisted with lateral imaging. Bicortical drilling is done to facilitate bicortical screw engagement. Any residual bleeding can be controlled with small quantities of Surgicel®.
This is an extremely powerful screw and allows intra-operative reduction of C1 to C2. The C2 screws should be locked first, rods bent in lordosis and even a tool applied to the C2 screw head during reduction to ensure maximum C1 retro-translation without forward tilt of the rods at the C2 screw-rod interface.
The downside of the Harms is the increased expense of four polyaxial screws versus two cortical screws but the advantages outweigh this. The incision is smaller due to the required trajectories being less steep than the transarticular screws.
The risk of increased blood loss is present, but with experience can be avoided with the aforementioned techniques. In our experience, the blood loss is minimal in most cases but if encountered, can be extensive due to the venous plexus over the screw insertion area. This was confirmed by Hu in his review of manual screw position. Their average blood loss was 450 ml but encountered a maximum of 1 200 ml. They had no vascular or neurological complications and post-op CT confirmed adequate placement of the freehand-inserted screws.10
Conclusion
Although the Harms technique had an increased blood loss, the incidence of vertebral artery and dural injury was lower. Fusion was similar in both groups with the only non-union occurring in the transarticular group.
The Harms technique offers the advantage of intraoperative reduction and a smaller exposure due to the direction of access but at a higher instrumentation cost.
References
1. Bransford RJ, Lee MJ, Reis A. Posterior fixation of the upper cervical spine: contemporary techniques. The Journal of the American Academy of Orthopaedic Surgeons [Internet]. 2011 Feb;19(2):63-71. Available from: http://www.ncbi.nlm.nih.gov/pubmed/21292929 [ Links ]
2. Magerl F, Seeman P. Stable posterior fusion of the atlas and axis by transarticular screw fixation. In: Kehr P, Weidner A, editors. Cervical Spine. 1st ed. Wien, New York, Springer Verslag.; 1987. p. 322-27. [ Links ]
3. Harms J, Melcher R. Posterior C1-C2 fusion with polyaxial screw and rod fixation. Spine (Phila Pa 1976). 2001;26(22):2467-71. [ Links ]
4. Dreyer SJ, Boden SD. Natural History. Clinical orth. 1999;(366):98-106. [ Links ]
5.. Hsu WK, Anderson PA. Odontoid Fractures: Update on. J Am Acad Orthop Surg. 2010;18(7):383-94. [ Links ]
6. Bormann RPB Von, Uct M. Dens screw fixation: Is it all it's cut out to be? SA Orthopaedic Journal 2007 Winter: 18-24. [ Links ]
7. Santavirta S, Konttinen Y, Laasonen E, Honkanen V, Antti-Poika I, Kauppi M. Ten year results of operations spine for rheumatoid cervical disorders. J Bone Joint Surg Br 1991;73-B:116-20. [ Links ]
8. Low H, Redfern R. C1-C2 transarticular screw fixation for atlantoaxial instability: a 6-year experience, and C1-C2 transarticular screw fixation-technical aspects. Neurosurgery. 2002;50(5):1165-66. [ Links ]
9. Dunn R, Ombachi R. Transarticular screw fixation of the atlanto-axial spine: a safe and effective option. SAOJ.2006;(August):1-6. [ Links ]
10. Hu Y, Kepler CK, Albert TJ, Yuan Z-S, Ma W-H, Gu Y-J, et al. Accuracy and complications associated with the freehand C-1 lateral mass screw fixation technique: a radiographic and clinical assessment. J Neurosurg Spine 2013 Apr;18(4):372-7. Available from: http://www.ncbi.nlm.nih.gov/pubmed/23373564 [ Links ]
 Correspondence:
Correspondence:
Prof Robert Dunn
Tel: 021 404 5108
Email: robert.dunn@uct.ac.za
The content of this article is the sole work of the authors, and no benefit of any form has been received or will be received from any commercial party.
This article is also available online on the SAOA website (www.saoa.org.za) and the SciELO website (www.scielo.org.za). Follow the directions on the Contents page of this journal to access it.














