Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
SA Orthopaedic Journal
versão On-line ISSN 2309-8309
versão impressa ISSN 1681-150X
SA orthop. j. vol.12 no.3 Centurion Set. 2013
GENERAL
Leave against medical advice (LAMA) from in-patient orthopaedic treatment
SO PopoolaI; NOC OnyemaechiII; JN KortorIII; KS OluwadiyaIV
IFMCS(Ortho). Department of Surgery, Benue State University Teaching Hospital, Makurdi, Nigeria/Federal Medical Centre Makurdi, Nigeria
IIFWACS(Ortho). Department of Surgery, Benue State University Teaching Hospital, Makurdi, Nigeria/Federal Medical Centre Makurdi, Nigeria
IIIFMCS (Ortho). Department of Surgery, Benue State University Teaching Hospital, Makurdi, Nigeria/Federal Medical Centre Makurdi, Nigeria
IVFMCS(Ortho). Department of Surgery, Ekiti State University Teaching Hospital, Ado-Ekiti, Nigeria
ABSTRACT
Leave Against Medical Advice (LAMA) poses potentially serious consequences on the utilisation of resources and may impact on an institution's finances. This study investigated hospital characteristics, patient factors and physician obligations regarding LAMA in Makurdi, Nigeria.
A 12-month prospective study involving orthopaedic in-patients in a tertiary health institution with many catchment areas was conducted. A proforma was designed for the socio-demographic profiles and the contexts surrounding the act of LAMA.Fifty-eight (13.9%) of the patients managed within the stipulated period took LAMA. Injury sustained in motor vehicle collisions was the major indication for admission while disagreement on treatment modality and poor financial status were the main reasons for LAMA. The major destination after taking LAMA was the Traditional Bone Setter's home.
'Disagreement on treatment/duration' and 'patronage of the Traditional Bone Setters' are issues linked mostly to the poor financial status of patients. Educational awareness, implementation of health insurance for all citizens and establishment of a well-equipped orthopaedic division within the hospital are laudable solutions.
Keywords: Leave Against Medical Advice, orthopaedics
Introduction
Leave Against Medical Advice (LAMA), also called discharge against medical advice (DAMA), is an act whereby a patient takes his/her discharge contrary to the recommendation or will of the attending physician. The issue concerns hospital management, staff and patient as well as the third party where applicable.1-4 The staff, especially doctors and nurses, having certified the ethical considerations and professional obligations, may be faced with issues regarding quality assurance and litigation.5 The patient involved in LAMA may take a dangerous decision without considering immediate and subsequent results. The third party (people other than the parents or relations), usually the employer or legal adviser, is occasionally involved in the decision. However, for those patients who have insurance policies, the decision to take the option of LAMA may be the end of financial support, which explains why the majority of the patients who take LAMA are uninsured or not covered by any medical aid.6 Studies in developing countries have implicated poor financial and low socio-economic status as the main reasons for LAMA.7-9 In developed countries human immunodeficiency virus (HIV) related conditions are contributing factors.10,11
In practice the management of ethical considerations regarding LAMA presents more complex issues than simply identifying and potentially prioritising the relevant ethical principles; physician-patient communication, informed consent and underlying psychiatric issues are all relevant.12 Patients taking LAMA must be educated regarding health issues so that they have the capacity to obtain, process and understand the basic health information and services needed to take appropriate decisions.1 After LAMA the physician's responsibility is to ensure the safety of the act. The alliance does not end with LAMA; it only transfers its management to another setting.13 However, this is not the case in some countries, including Nigeria, where there are no hard-and-fast policies or rules that should guide doctors and nurses when confronted with such a situation.4,14 Paediatric patients are not qualified to take decisions themselves; parents or guardians take such decisions on their behalf.15
Very few studies highlight LAMA among orthopaedic patients. A study conducted in Spain shows an incidence of 0.26% among orthopaedic patients.16 This study investigated and specified strategies and interventions to palliate the effects of taking LAMA.
Method
The study was conducted at the Federal Medical Centre, Makurdi (FMCM), Benue State, North Central Nigeria, after having obtained approval from the Ethics and Research committee. The hospital is a tertiary institution with all specialties and is located in the heart of the city. It operates many annexes within and outside the city. It is a referral institution for all secondary healthcare centres in the 23 Local Government Areas of the state, and a favourable catchment area for the nearby Kogi and Nasarawa States. Orthopaedic patients are recruited from the Accident and Emergency Department (AED) and clinics or are transferred from other wards.
A proforma document was designed to collect data from November 2010 to October 2011. The socio-demographic profile of each patient and the contexts surrounding the act were included.
When a patient desired to leave, the decision was either communicated directly to a member of the Orthopaedic and Trauma Surgery team or through the nurses. After having had the implications of the decision explained to them, the patient and/or third party involved would be questioned and counselled. If the patient still insisted on leaving, a clinical psychologist would be called upon to further counsel the patient. If the patient finally decided to leave, the proforma document for the study would be completed. As the patient was not under any obligation to follow our medical advice, the proforma document would then be certified by a doctor in the unit and witnessed by a nurse on duty. In accordance with hospital policy all treatment or intervention would be terminated and such a patient would have to settle all outstanding bills before leaving the hospital.
Results
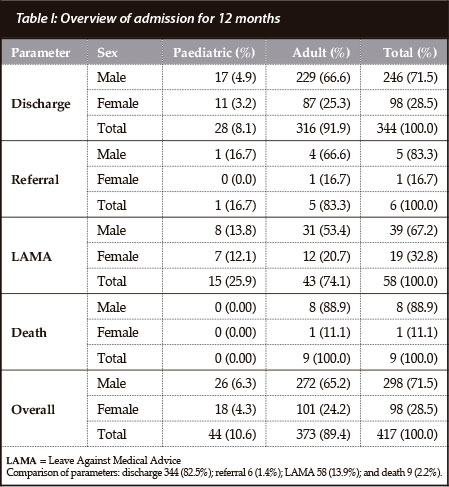
Fifty-eight out of 417 in-patients left against medical advice from 1 November 2010 to 31 October 2011. There were 15 (25.9%) paediatric patients (under 18 years of age), while adults (over 18 years) totalled 43 (74.1%). The mean age was 30 years, the mode 40 years, the median 30.5 years and the age range 2-70 years. The educational level of the participants was as follows: No education 5 (8.6%); primary education 21 (36.2%); secondary education 16 (27.6%); tertiary education 13 (22.4%) and 3 (5.2%) were infants. Indications for admission: road traffic crash (RTC) 43 (74.1%); fall 7 (12.1%); diabetic foot 3 (5.2%); assault 2 (3.4%); neoplasm 2 (3.4%); and infection 1 (1.7%). The overview of admission within the stipulated period (Table I) highlights the comparison of activities in the unit.
The comparison in Table II depicts plausible issues: the higher the number of injuries, the higher the tendency towards an emergency mode of admission. Trauma was the major indication for admission. There was no significance (p = 0.374) between source of income and destination after taking LAMA; similarly, none between mode of admission and destination.
Twenty-five patients (43.1%) took the decision to LAMA in the AED and the majority, 33 patients (56.9%), did so in the wards. The period taken to make the decision was four hours to five weeks with the majority doing so within two days. Of the 58 patients that left against medical advice, 23 (39.7%) had non-operative intervention while four (6.9%) had been operated upon and 31 (53.4%) were still awaiting surgery.
Trauma was the major indication for admission
The intended procedures were never performed due to non-provision of necessary materials needed by patients. The total period spent after admission ranged from one day to six weeks. The destination after taking LAMA was as follows: Traditional bone setter (TBS) 36 (62.1%); home 10 (17.2%); undecided 6 (10.3%); other orthodox centres 5 (8.6%); and church/mosque 1 (1.7%).
Discussion
Leaving against medical advice (LAMA) is an unpleasant phenomenon in clinical practice. In this study the incidence is 13.9% compared to 0.26% among orthopaedic patients in Spain which is a developed country.16 The high incidence in Nigeria, perhaps, due to limited health facilities and low socio-economic status, calls for attention. The low literacy level (8.6%) and low level of tertiary education (22.4%) among the patients are other drawbacks. This study and the ones conducted by Onyeriuka9 and Mabiala-Babela17 showed that the higher the level of education the lower the rate of leaving against medical advice.
Adults (74.1%) seemed to have greater choice of action: perhaps they could decide for themselves what they wanted, unlike children who were subjected to the decisions of their parents. Parents might also be influenced by the fragile and unstable physiological nature of children and had to abide by the advice of the treating physicians until conditions were satisfactory for discharge.
As the majority (70.7%) of patients was admitted on emergency, they probably waited for adequate resuscitation and stabilisation before heading to the TBS, irrespective of the medical team's counselling and encouragement. Although counselling by clinicians and psychologists ordinarily should discourage patients to LAMA, our patients with musculoskeletal lesions were not dissuaded. In Nigeria, the fact that the TBS and other alternate practitioners are allowed to advertise their services while orthodox practitioners are not, is an issue that needs to be addressed.18,19
RTC in 43 cases (74.1%) was the major indication for admission in patients who took LAMA. The majority of these patients (69.0%) were admitted directly from the AED while others were referred from peripheral hospitals. The hospital's permanent site housing Casualty (14 km from the metropolis where most of the collisions occur) is not favourable for urgent intervention. Therefore victims are sometimes conveyed to nearby private hospitals where there are no facilities for initial resuscitation of patients with musculoskeletal injuries. It is a known fact that pre-hospital management is virtually not practised in Nigeria.20 Passers-by and eyewitnesses may decide to convey the victims of RTC to any nearby health centre, and on rare occasions to the TBS/alternate practitioners.20
In Table III, 'disagreement on both treatment and duration of hospital stay' with 17 (29.4%) topped the list of reasons for taking LAMA. Some patients, according to a study by Solagberu,21 believe that TBS treatment is faster. Our own interpretation of this report is founded on the fact that patients view orthodox treatment as time-consuming since they have no foreknowledge of the scientific or natural healing process of bone lesions. Moreover, most of these patients could not procure materials (implants) necessary for the management of their lesions.

Financial statements indicated that 75.8% of these patients earned between ten and forty thousand naira per month, which was actually not enough to carry out a major orthopaedic operation, let alone for settling other hospital and non-hospital charges. Similar reports appeared in previous studies across Nigeria.7-9 Based on these reasons, our patients prefer seeking help from TBS/alternative practitioners who by virtue of their socio-cultural heritage know how to extract money from their patrons in a piecemeal manner. The National Health Insurance Scheme (NHIS) could be of assistance but it does not cover all aspects of management. Besides, it is currently applicable to federal workers who constitute a minor fraction of the total work force in Nigeria. The high rate of return to orthodox medication in Ilorin,21 North Central Nigeria, should encourage a rethink in Makurdi (in the same zone): it is high time Benue people embraced orthodox care.
Five (8.6%) of the patients took LAMA a few days after admission and, having had adequate resuscitation and wound care, claimed they had no relatives to sponsor their treatment. This group of patients also declined referral to other orthodox institutions and our inquisition established that they were interested in TBS. Two (3.4%) of patients who cited 'slow improvement' as the reason for taking LAMA had attained a tertiary level of education; perhaps they opted for LAMA because of lack of knowledge of the period for the natural healing process of musculoskeletal injuries. They might have also failed to understand the limited theatre space for carrying out elective surgery in this setting.
The shortest interval to take the decision to leave after admission was four hours. This category of patients and their relations probably resented orthodox practice at the time of admission. A total of five weeks was recorded as the longest period to take the decision to leave among patients who were financially handicapped and preferred to buy time with non-operative measures. Similarly, the same conduct was noted in patients who had associated severe soft tissue or head injury. However, our findings showed that the rate of leaving was reduced among patients who stayed longer after admission and who understood the peculiar challenges to make things work with limited health facilities in this low-income country.14
A few patients (6.9%) had operative intervention where indicated, while 53.4% were still awaiting surgery before leaving the hospital. The reasons for declining operative treatment were poor financial status, the long waiting time for elective cases, the socio-cultural belief in TBS and fear of general anaesthesia. The long waiting time had no amelioration because of limited theatre space and other essential facilities.
The major destination after LAMA was the Traditional Bone Setter's home. This further demonstrated the menace of TBS and other alternate practitioners as the leading cause of complications being combated by Orthopaedic and Trauma Surgeons in Nigeria.22
There was a significant correlation between age and decision/signing of LAMA forms (p<0.001). Parents and relatives who signed for their older children and family members, showed the dominant role of parents and family members in Nigerian society.14 Comparison of age group and destination after LAMA (Table II) shows that more of the children were taken to other orthopaedic centres, perhaps to seek another surgeon's opinion because of their fragile physiological nature. The reverse is true for adults who preferred the TBS. The correlation between aetiology of injury and hospital admission is significant (p<0.001); the majority of RTC victims presented directly to the hospital for better management. This initial good intention might have been defeated by the low socio-economic status of the patients who thereafter took leave to consult cheaper unscientific TBS/alternative practitioners.
Conclusion/recommendation
The high incidence of LAMA among orthopaedic patients in Nigeria calls for exploration of the contributory hospital, patient and physician factors. The low level of literacy among patients who took LAMA as detected in this study and others9,17 can be reduced by encouraging education up to tertiary level. This should ensure a better appreciation of the advantages of orthodox treatment over unscientific TBS techniques.
RTC was reported to be the major indication for admission among orthopaedic patients; since trauma cannot be eradicated, it should be reduced to the barest minimum by observing all road safety measures. For government, the state of Nigeria's roads calls for urgent attention. Nigerian roads rank second worst in the world - 191st out of 192 countries whose roads are currently rated bad on safety standards.23
As disagreement regarding treatment/duration, financial constraint and socio-cultural belief in TBS are big challenges in the management of these patients, the NHIS has demanded restructuring to accommodate all Nigerian citizens. Hospital management should give better recognition to a well-equipped Orthopaedic and Trauma Surgery as a division with special clinics, wards and theatres. This will enhance the quality of services, thereby discouraging patients from questioning our treatment modalities. Public-Private Partnership in terms of 'provision of facilities', if allowed, will complement healthcare delivery in the hospital, since the latter cannot procure all necessary materials.
The low level of literacy among patients who took LAMA can be reduced by encouraging education up to tertiary level. This should ensure a better appreciation of the advantages of orthodox treatment over unscientific TBS techniques
Acknowledgement
The authors wish to acknowledge the contributions of resident doctors, nursing staff, clinical psychologists and other people who made the study possible.
No benefits of any form have been received from a commercial party related directly or indirectly to the subject of this article. The content of this article is the sole work of the authors.
References
1. Alfandre DJ. 'I'm Going Home' Discharges Against Medical Advice. Mayo Clinic Proc. 2009;84(3):255-60. [ Links ]
2. Eze B, Agu K, Nwosu J. Discharge against medical advice at a tertiary centre in southeastern Nigeria: sociodemographic and clinical dimensions. Patient Intelligence 2010:227-31. [ Links ]
3. Ibrahim SA, Kwoh CK, Krishnan E. Factors Associated with Patients who Leave Acute-Care Hospitals Against Medical Advice. American Journal of Public Health 2007;(97)2204-2208. [ Links ]
4. Moyse HS. Discharges against medical advice: a community hospital's experience. Can J Rural Med 2004;9(3):148-53. [ Links ]
5. Jeffrey TB. Discharge Against Medical Advice: Ethical Consideration and Professional Obligations. Journal of Hospital Medicine 2008;3(5):403-408. [ Links ]
6. Long JP, Marin A. Profile of patients signing against medical advice. J Fam Pract 1982;15:551-56. [ Links ]
7. Okechukwu AA. Discharge against medical advice in children at the University of Abuja Teaching Hospital, Gwagwalada, Nigeria. Journal of Medicine and Medical Science 2011;949-54. [ Links ]
8. Meremikwu MM, Ehiri JE, Nkanga DG, Udoh EE, Ikpatt OF, Alaje EO. Socioeconomic constraints to effective management of Burkitt's Lymphoma in south-eastern Nigeria. Tropical medicine and international health 2005;10:92-98. [ Links ]
9. Onyeriuka AN. Discharge of hospitalized under-fives against medical advice in Benin-City, Nigeria. Niger J Clin Pract 2007;10:200-204. Available from: http://www.ajol.info/index.php/njc/article/view/11328/0 Accessed 12/09/2011. [ Links ]
10. Anis AH, Sun H, Guh DP, Palepu A, Schechter MT, O'Shaughnessy MV. Leaving hospital against medical advice among HIV hospital patients. Can Med Assoc. 2002;167:633-37. [ Links ]
11. Saitz R. Discharges against medical advice: time to address the causes. CMAJ 2002;167:647-48. [ Links ]
12. Berger JT. Discharge Against Medical Advice: Ethical Considerations and Professional Obligations. Journal of Hospital Medicine 2008;3:403-408. [ Links ]
13. Dostal KU, Schmidt MJ. The dilemma of the patient who wishes to leave the hospital against medical advice. Semin Med Pract. 2007;10:9-17. [ Links ]
14. Nwokediuko SC, Arodiwe EB. Discharge Against Medical Advice in Enugu, South Eastern Nigeria. Some Ethical and Legal Aspects. Journal of College of Medicine 2008;13:34-38. [ Links ]
15. Roodpeyma S, Hoseyni SAE. Discharge of children from hospital against medical advice. World J Pediatr. 2010;1-4. [ Links ]
16. Duno R, Pousa E, Sans J, Tolosa C, Ruiz A. Discharge against medical advice at a general hospital in Catalonia. General Hospital Psychiatry 2003:46-50. [ Links ]
17. Mabiala-Babela JR, Nika ER, Ollandzobo LC, Samba LC, Mouko A, Mbika CA, Moyen GM. Discharge of children against medical advice at CHU of Brazzaville (Congo). Bull Soc Pathol Extot 2011;104(5):331-35. [ Links ]
18. Nwofia JC. Is it time for doctors to start advertising in Nigeria? Available from: http://nigerianhealthjournal.com/?author=1 Accessed 24/08/2011. [ Links ]
19. Olasinde AA, Oluwadiya KS, Olawoye AO, Badru OS, Oginni LM, Adegbehingbe OO. Knowledge, Attitude and Practice about the Traditional Bone Setters among Health Workers in Federal Medical Centre, Owo, Nigeria. Sahel Medical Journal 2003;6(3):79-82. [ Links ]
20. Popoola SO. Comparison of Kampala Trauma Score (KTS) with Revised Trauma Score (RTS) in a Nigerian Teaching Hospital. National Post-graduate Medical College of Nigeria 2009. Available from: http://www.npmcn.edu.ng/DISSERTATIONS_OF_NPMCN.DOC Accessed 11/07/2011. [ Links ]
21. Solagberu BA. Long bone fractures treated by traditional bone setters: a study of patient behavior. Trop Doct. 2005;35(2):106-107. [ Links ]
22. Popoola SO, Kortor JN, Onyemaechi NOC, Oluwadiya KS. Knowledge and Attitude of Healthcare Workers towards Traditional Bone Setters in Benue State, Nigeria. Journal of Orthopaedics and Trauma 2012;11(1):1-7. [ Links ]
23. Chidoka S. FRSC: Nigerian Roads Second Worst in the World. Available from: http://www.thisdaylive.com/news Accessed 20/08/2012. [ Links ]
 Reprint requests:
Reprint requests:
SO Popoola
E-mail: ogunsuyipopoola@yahoo.com














