Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SA Orthopaedic Journal
On-line version ISSN 2309-8309
Print version ISSN 1681-150X
SA orthop. j. vol.12 n.3 Centurion Sep. 2013
UPPER LIMB
Subungual glomus tumours: Report on 11 cases
T SefeaneI; A AdenII; F PetersIII
IBSc(NUL), MBBCh(Wits), FC(Ortho)SA, MMed(Ortho)(Wits) Consultant Orthopaedic Surgeon, Helen Joseph Hospital, Johannesburg
IIMD(SOM), FCS(Ortho)(SA) Senior Consultant Surgeon and Head: Orthopaedic Department, Helen Joseph Hospital, Johannesburg
IIIMBChB(Pret), FC(Ortho)(SA) Consultant Orthopaedic Surgeon, Chris Hani Baragwanath Hospital, Johannesburg
ABSTRACT
Subungual glomus tumours are debilitating tumours that arise from the glomus body in the distal aspect of the digit. They normally present with a triad of severe pain in the digit, cold sensitivity, and point tenderness. There is normally a bluish discolouration under the nail, pin-point tenderness and severe pain with exposure to cold. There is typically a long delay from onset of symptoms and diagnosis.
We present a series of 11 patients who were typically all misdiagnosed multiple times, surgically treated at the Helen Joseph Hospital, Johannesburg, between 2008 and 2012. We conclude that the diagnosis of glomus tumours should be clinical with meticulous history-taking and a high index of suspicion and careful examination. Special investigations are usually not necessary.
Keywords: glomus tumour, pin-point tenderness, cold sensitivity, subungual
Introduction
Glomus tumours were apparently first described by W Wood as early as 1812 in his article: 'On painful subcutaneous nodules' that he presented to the Edinburgh Medical and Surgical journal.1 He described these nodules as highly pain and temperature sensitive, and completely curable by surgical excision. Over the years they have since been found to be rare hamartomatous lesions representing approximately 1% of all hand tumours.2 The subungual glomus tumours originate from the glomus body normally located in the digit on the distal aspect of the pulp of the finger. The glomus body is a neuromyoarterial apparatus which is a carefully controlled arteriovenous shunt between terminal vessels supplying a regulatory function in digital blood flow. Extra digital sites of this tumour include the hand, the wrist, forearm, elbow, arm, shoulder, buttock, thigh, knee, ankle, foot, back, nose, cheek, ear lobe and trachea.3 Even the nerves can be involved: radial nerve4 and digital nerve.5
We present a series of 11 patients treated at the Helen Joseph Hospital, Johannesburg Upper Limb Unit, from 2008 to 2012.
Methods
A total of 11 patients (nine women and two men) with a mean age of 35.5 years ranging from 29 to 69 years, were diagnosed with a subungual glomus tumour at our institution (Helen Joseph Hospital) between 2008 and 2012. The diagnosis was made in all the patients clinically by the history and clinical examination. The time from initial symptomatology to diagnosis was documented in all patients. The only radiological evaluation in all patients was a hand X-ray.
All patients were treated surgically and discharged the day after surgery. The excised tumours were sent for histological analysis. Patients were then followed up after 7 days, then at 6 weeks and finally at 6 months. At final review, pain or recurrence of symptoms were recorded.
Surgical technique (Figures 1-3)
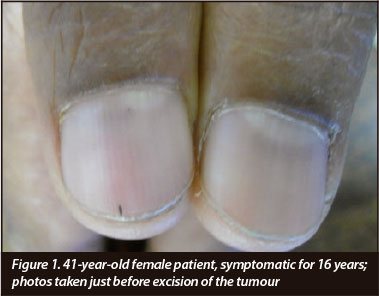
Surgery is performed under either general or peripheral nerve block at the discretion of the attending anaesthetist. A Love's test is repeated before anaesthesia to localise and mark the point of maximum tenderness. A tourniquet was used in all cases to obtain a bloodless field.
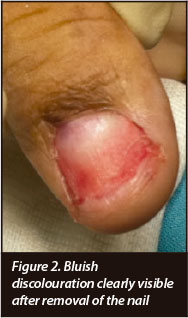
The nail is carefully lifted from the nail bed with a McDonalds and gently peeled off with an artery forceps.
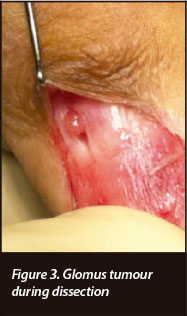
Once the nail bed has been removed, the blue discolouration is identified to accurately localise the lesion (Figure 2). A small longitudinal 0.5 cm incision is made over the bluish discolouration. It is important that the incision is not too deep to involve the underlying tumour. Normally with gentle dissection the tumour will pop out of the incision and this is carefully lifted from the periosteum and delivered whole (Figure 3).
Once the lesion has been excised, gentle pressure is applied to attain haemostasis. The nail bed incision is then closed with intermittent buried monocryl 6(0) sutures. The old nail is used as a nail bed dressing and sutured down with either nylon or monocryl. The finger is dressed with Jelonet and an Adaptac finger dressing.
Results (Table I)
All the procedures were performed by the authors, individually or in combination, using the same surgical technique as outlined. There were nine females and two men in our series with an average age of 35.5 years (29 to 69). In all patients there was a period of delay in diagnosis from the onset of symptoms with multiple consultations and a variety of treatments. This period ranged from 6 months to 16 years.
All the patients in our series had cold intolerance and had a positive Love's test. Blue discolouration was absent in two patients and only one X-ray showed distal phalangeal erosion.
In total, 11 operations were performed on 11 fingers. The operations were uneventful and a small well circumscribed tumour was excised in all the patients (Figure 4). Histology confirmed the diagnosis. The immediate post-operative period was uneventful and on final review all the patients were completely symptom free and extremely satisfied though the new nail that grew was thicker and a bit different from the other nails. To date no tumours have recurred.

Discussion
Subungual glomus tumours have a typical clinical presentation with severe pain in the digit, point tenderness and cold intolerance. Typical findings on examination are a blue discolouration on the nail bed, exquisite localised pain elicited by pressure with a pin head (Love's test), sudden pain on the affected digit with exposure to ice cold water or ethyl alcohol (Joseph Posner test)6 and a reduction in pain and tenderness on exsanguination and ischaemia of the affected part (Hildreth's test). The cold sensitivity test has a sensitivity of 100% and specificity of 100% while the Love's pin test has a sensitivity of 100% and accuracy of 78% from a study in 2002.7 Hildreth's test by comparison showed a sensitivity of 92%, a specificity of 91%, a positive predictive value of 92% and a negative predictive value of 91% in another report, also in 2002.8
Subungual glomus tumours have a typical clinical presentation with severe pain in the digit, point tenderness and cold intolerance
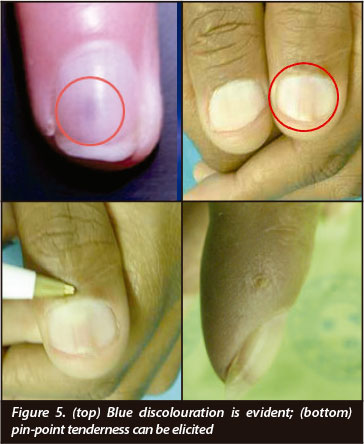
The recurring feature which is almost characteristic of subungual glomus tumour is delay in diagnosis ranging from 4 months to 15 years from the onset of symptoms.1 This aspect has been confirmed in our series where the delay in diagnosis was up to 16 years. This delay in diagnosis is mainly due to lack of attention to detail in history-taking and examination. On examination the patient will typically be apprehensive to touch on the affected digit. A dark bluish discolouration at the base of the nail and a positive Love's test will localise the lesion (Figure 5). All our patients in the series presented with chronic pain in the digit which had been examined by a variety of caregivers over a long period of time. All these patients had established cold intolerance and had a positive Love's pin-point test. Bluish discolouration was present in all except two.
Although the diagnosis is mainly clinical, radiologic evaluation by way of X-rays, ultrasound and magnetic resonance imaging (MRI) has been reported. Carroll and Berman9 reported that plain X-rays normally show erosive changes in about 22% of cases. In our series only one patient out of 11 (9%) presented with an erosive lesion on the distal phalanx (Figure 6).

MRI for diagnosis of this tumour has been studied in many centres and one study reported a sensitivity of 90%, a specificity of 50%, a positive predictive value of 97% and a negative predictive value of 20%.6 The use of colour duplex Doppler sonography has also been studied as an alternative and one study reported a favourable outcome of a 100% detection rate as reported in one series.10 Surgical excision of the tumour is the treatment of choice and provides almost total relief of symptoms.11,12 Excision entails localising the lesion by the bluish tinge on the base of the nail and by the Love's test prior to anaesthesia.
The recurring feature which is almost characteristic of subungual glomus tumour is delay in diagnosis ranging from 4 months to 15 years from the onset of symptoms
The implications and lessons that can be learned from our series is that good, old-fashioned careful listening, meticulous history-taking coupled with a high index of suspicion and proper examination should be enough to make a diagnosis. Although there is good literature support for radiologic investigations by way of ultrasound and MRI, we firmly believe that the diagnosis of subungual glomus tumours is a clinical diagnosis not requiring any special investigations. These (special investigations) have a high cost implication and in developing world centres like ours, where MRIs are not readily available, these debilitating tumours can be accurately diagnosed clinically, and treated surgically with satisfactory results.
Conclusion
In conclusion, we feel that a carefully taken history and clinical examination is adequate to make the diagnosis of a subungual glomus tumour. As stated by Mennen: 'The point is that one does not always need the latest technology to produce good quality hand surgery.'13
No benefits of any form have been received from a commercial party related directly or indirectly to the subject of this article. The content of this article is the sole work of the authors.
References
1. Pater TJ, Richard M. Glomus tumor of the hallux: case presentation and review of the literature Foot & Ankle International 2004 June, Vol. 25, No. 6. [ Links ]
2. Hazani R Houle JM, Kasdan ML, Wilhelmi BJ. Glomus tumors of the hand. Eplasty. 2008;8:e48. Published online 2008 October 8. [ Links ]
3. Schiefer TK, Parker WL, Anakwenze OA, Amadio PC, Carrie Y. Inwards, extradigital glomus tumors: A 20-year experience. Mayo Clinic Proceedings 2006 Oct;81(10):1337-44. [ Links ]
4. Smith KA, Mackinnon SE, Macauley RJB, Mailis A. Glomus tumor originating in the radial nerve: A case report. Journal of Hand Surgery 1992;17A(4):665-67. [ Links ]
5. Mitchell A, Spinner RJ, Ribeiro A, Mafra M, Maria M. Mouzinho, Bernd W. Scheithauer et al. Glomus tumour of digital nerve: case report. Journal of Hand Surgery 2012 Jun;37(6):1180-83. [ Links ]
6. Al-Qattan MM, Al-Namla A, Al-Thunayan A, Al-Subhi F, El-Shayeb AF. Magnetic resonance imaging in the diagnosis of glomus tumours of the hand. J Hand Surg 2005;30B:535-40. [ Links ]
7. Bhaskaranand K, Navagdi BC. Glomus tumour of the hand. J Hand Surg [Br] 2002;27:229. [ Links ]
8. Giele H. Hildredth's test is a reliable clinical sign for the diagnosis of Glomus tumours. Journal of Hand Surgery: Journal of the British Society for Surgery of the Hand 2002 Apr;27(2):157-58. [ Links ]
9. Carroll RE, Berman AT. Glomus tumours of the hand. Journal of Bone and Joint Surgery 1972;54A:691-703. [ Links ]
10. Chen SH, Chen YL, Cheng MH, Yeow KM, Chen HC, Wei FC. The use of ultrasonography in preoperative localization of digital glomus tumours. Plast Reconstr Surg 2003;112:115-19. [ Links ]
11. Tomak Y, Akcay I, Dabak N, Eroglu L. Subungual glomus tumours of the hand: Diagnosis and treatment of 14 cases. Scand J Plast Reconstr Surg Hand Surg 2003;37:121-24. [ Links ]
12. McDermott E, Weiss A-P. Review: Glomus tumours. J Hand Surg 2006;31A:1397-1400. [ Links ]
13. Mennen U. 11th International Federation of Societies for Surgery of the Hand Congress, Seoul, South Korea - Presidential Acceptance Speech. SAOJ 2011;10:10-11. [ Links ]
 Reprint requests:
Reprint requests:
Dr T Sefeane
Email: tatolos@supanet.com














