Servicios Personalizados
Articulo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en Google
Similares en Google
Compartir
SA Orthopaedic Journal
versión On-line ISSN 2309-8309
versión impresa ISSN 1681-150X
SA orthop. j. vol.12 no.3 Centurion sep. 2013
UPPER LIMB
Evaluation of intramedullary nailing in low-velocity gunshot wounds of the radius and ulna
BR GelbartI; AA AdenII
IFCOrth(SA), MMed(Ortho Surg)(Wits) Charlotte Maxeke Johannesburg Academic Hospital/Linksfield Orthopaedic, Sport and Rehabilitation Centre, Johannesburg, South Africa
IIMD(Som), FCS (SA)Orth Helen Joseph Hospital Upper Limb Unit, Johannesburg, South Africa
ABSTRACT
BACKGROUND: The objective is to assess whether intramedullary (IM) nailing of the forearm (radius and/ or ulna) after low-energy gunshot wounds, is a safe and effective form of management for these complex fractures.
METHODS: A prospective consecutive case series was followed from presentation to fracture union. Cases were enrolled from three tertiary level academic hospitals and one private hospital. Twenty-one patients (between April 2006 and February 2008) who sustained low-energy gunshot wounds to the radius and/ or ulna were enrolled. All fractures were stabilised using a single IM rod. Variation in soft tissue management was dependent on surgeon preference and findings. All patients were assessed subjectively; using a DASH score, objectively; by a clinical exam (focusing on range of movement and wound healing) and radiologically; assessing for fracture union.
RESULTS: Fourteen patients, all with comminuted fractures, were evaluated at 1 year post-injury. The median DASH score was 7.5 (range 3.3-84), but this was influenced by soft tissue factors. All the wounds healed without complication, and range of movement was adequately restored. Three patients had residual nerve injuries, which affected outcome. The fracture union rate was high (13/14) and complication rate was limited to one non-union and one mal-union.
CONCLUSION: The use of IM nailing for low-velocity gunshot fractures of the radius/ulna is safe and effective, with predictable results.
Keywords: intramedullary nailing, low-velocity/energy, gunshot wounds, fractured radius, fractured ulna
Introduction
There is a limited amount of literature on the management of gunshot wounds of the radius and/ or ulna.1-5 Low-energy gunshot wounds to the extremities are rare. The final injury pattern is related to numerous factors and is not limited to the muzzle velocity of the bullet.6 The term low-energy is therefore preferred but the terms low-velocity and low-energy can be used interchangeably. The fracture pattern can range from simple to highly comminuted, and the soft tissue injury from a small puncture wound to extensive muscle and neurovascular damage.
In 1986, Street7 proposed intramedullary (IM) nailing as an option for the management of these injuries. However, there has been no clinical assessment of the outcome. It makes theoretical sense that by avoiding the zone of injury in these complex injuries, we could possibly minimise the complication rate.
The purpose of this study is to investigate if IM nailing of low-velocity gunshot fractures of the radius and/or ulna results in reliable fracture healing and is not harmful to the patient. The secondary evaluation includes the level of functional return achieved in these patients.
Patients and methods
This study is a prospective case series. The inclusion criteria were extra-articular comminuted fractures of the radius and/or ulna caused by a low-velocity gunshot (Figure 1). If the patient was unaware of the exact weapon used, then the state of the soft tissues was examined.
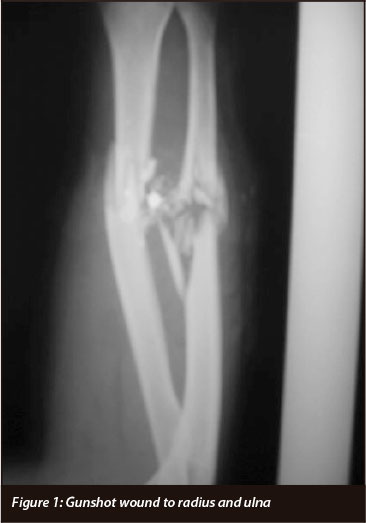
Provided the wound was less than 5 cm in diameter and there was no extended zone of injury, the patient was included. All patients were over the age of 18 years and were able to consent to inclusion.
Patients were excluded if they had sustained a high energy injury or if more than 2 weeks had elapsed between fracture and surgery.
Informed consent was obtained from the patients prior to inclusion.
The timing of surgery depended on the admitting doctor, the availability of theatre time and the general health status of the patient. The surgery was performed by registrars and consultants in the department.
Due to the nature of the injury and the population demographics, follow-up at the clinic was always anticipated as a problem. With this in mind, it was decided to contact all patients who had been enrolled in the study and assess them at a minimum of 12 months post-injury. This assessment consisted of a Disability of the Arm, Shoulder and Hand (DASH) score, examination of wound healing, fracture healing and range of movement of the injured arm and radiographs. The radiographs were assessed for fracture healing, alignment, shortening, loosening and sepsis.
Surgical technique
All of the rods were inserted using the described technique.
All procedures were performed under sterile conditions. Patients received either a general anaesthetic or a regional block.
All patients were given a dose of prophylactic antibiotics prior to inflation of the tourniquet.
C-arm X-ray was positioned to allow ease of intra-operative screening.
The arm was pre-scrubbed with an antiseptic soap solution of choice to remove excessive debris from the arm and hand.
A tourniquet was positioned on the arm but not inflated until just prior to the incision.
The arm was then prepared with an antiseptic surgical preparation in alcohol/Betadine up to the tourniquet and draped with sterile drapes.
Debridement and irrigation of the bullet wounds were performed as decided by the surgeon intra-operatively.
An incision was made over the desired entry point. For the ulna this was over the olecranon, and for the radius this was on the dorsal surface of the distal radial metaphysis, radial to Lister's tubercle. The entry point was then opened using an awl. Sequential reamers were then inserted and the diameter and length of the rod were confirmed.
The appropriate size rod was inserted, ensuring the fracture was reduced. Care was taken to ensure that the proximal and distal radio-ulnar joints were reduced. It is advisable to ensure correct rotation of the distal radius when inserting the rod (supinated for proximal third fractures, neutral for middle third fractures and pronated for distal third fractures) (Figure 2).
The inclusion criteria were extra-articular comminuted fractures of the radius and/or ulna caused by a low-velocity gunshot
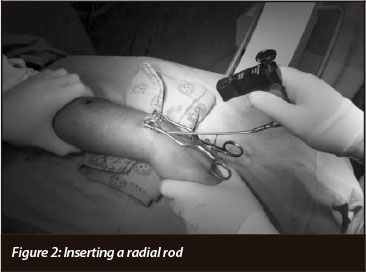
The nail was inserted ensuring that the flange engaged the metaphyseal bone in the opposite segment (distal segment for ulna and proximal for radius).
The rod was then locked with a single screw through a jig on the insertion side of the nail.
The surgical wound was closed in layers according to surgeon's preference. Most patients were splinted but this varied from short arm volar splints to an above-elbow backslab.
Results
Twenty-one consecutive patients who received IM rod fixation for a fractured radius and/or ulna were included in the study. The patients were collected between April 2006 and February 2008.
The demographics can be seen in Table I.
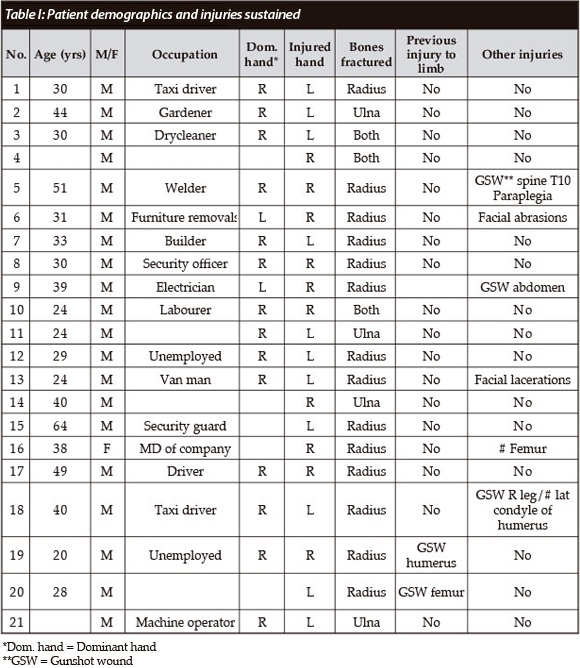
The mean age of the patients was 35.1 years old (range 24-64 years). Twenty out of 21 patients were male.
The occupations of the injured traversed a broad spectrum, from the unemployed to a managing director. Those who were employed ranged from security officers to electricians. None of the patients had previous injuries to the involved forearm.
Eight of the injured were able to positively identify the weapon as a low-velocity firearm. Two were excluded as they identified the weapons as high velocity firearms. The remaining 13 patients were included on the basis of a suspected low-energy gunshot, due to the appearance of the soft tissue injury and fracture configuration.
At the time of injury, seven patients exhibited neurological fallout of one forearm nerve; four of these resolved. No significant vascular injuries were noted in the cohort.
Surgical details
The time period from injury to surgery ranged from 10 hours to 4 days.
The mean duration of surgery for all the cases was 61.5 minutes (range 30-115 minutes).
The management of the gunshot wounds was surgeon dependent and was primarily based on the perceived contamination of the wounds and/or whether there was structural damage, necessitating exploration. Closure of the gunshot wounds was also left to the surgeon's discretion.
All patients received pre-operative antibiotics and at least 24 hours' post-operative intravenous (IV) antibiotics. First generation cephalosporin was the antibiotic of choice. In 3/21 patients antibiotics were continued for more than 24 hours, and two patients received triple antibiotics (cephalosporin, gentamycin and metronidazole) for more than 24 hours.
Follow-up data was collected on 15/21 (71%) of the patients prospectively enrolled in this study. The remaining patients were uncontactable or defaulted on further management in our clinics.
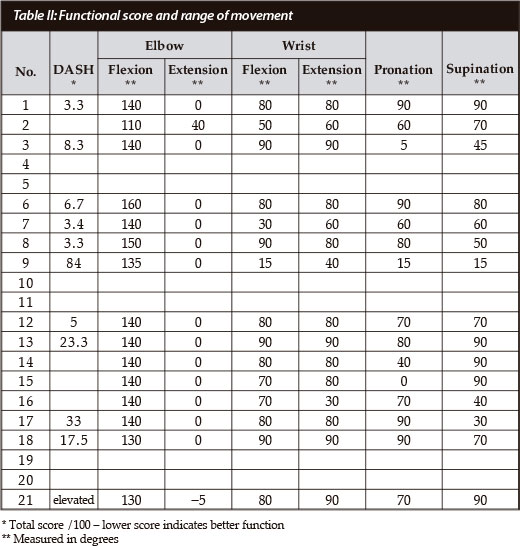
DASH questionnaires were completed by 10/15 (66%) patients; we found language to be the barrier to completion. The median score was 7.5/100 (range 3.384). The outlier score (84) was in one patient who had a painful non-union (Table II).
All of the surgical incisions and gunshot wounds healed without any other complications (Figures 3a and 3b).
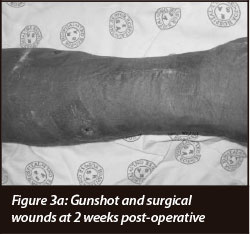
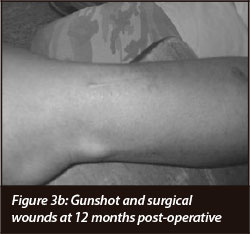
This includes one patient who recovered well from a forearm fasciotomy.
Range of movement (Table II) (Figures 4a and 4b)

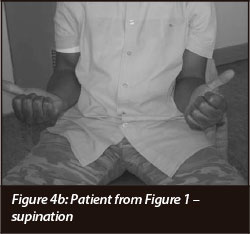
Range of movement was measured at the elbow, wrist and forearm.
Elbow flexion returned to full in all but one patient, who had an isolated proximal ulna injury. Two patients had less than full extension. Both had isolated proximal ulna gunshot wounds.
Wrist extension was only markedly decreased in two patients. One patient could only extend the wrist 30 degrees, but his DASH score was 3.4/100. The other patient, who had a painful non-union had limited wrist extension of 15 degrees; he also had limited flexion.
This same patient had severe limitation of both supination and pronation with just 15 degrees of each. The patient with radial metaphyseal mal-union had supination of 90 degrees but could only pronate to neutral.
Radiography (Table III) (Figure 5)
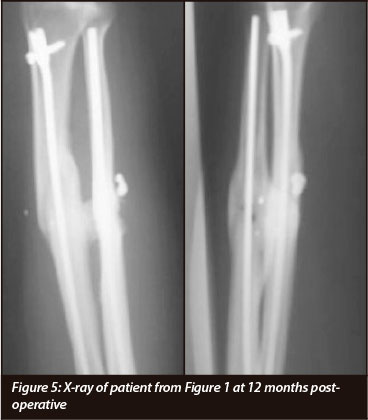
At a minimum follow-up of 12 months, 14/21 patients were available for radiographic follow-up. One other patient had his last follow up X-ray at 3 months post injury.
Due to the comminuted nature of the fractures all the fractures healed by callus formation. As a result complete bridging of all four cortices, two on AP and two on the lateral X-ray, was only seen in three patients (four bones). The healed fractures ranged from bridging two cortices to all four. There was no significant difference in functional ability between the patients who had bridging of two, three or four cortices.
One patient developed a painful non-union at 6 months post-operatively. He had evidence of lucency around the rod, suggesting loosening. The locking screw remained firmly in situ and did not appear loose.
The alignment, length and congruity of proximal and distal radio-ulnar joints were well maintained.
Complications (Table IV)
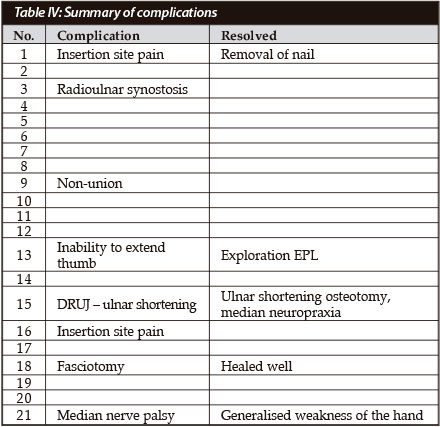
Specific complications that were sought related to the radius and ulna rods individually.
Complications at the insertion site were limited to dorsal wrist pain due to rods that were too proud. This resolved on removal of the rods.
One patient required a fasciotomy for suspected compartment syndrome of the forearm. A delayed primary closure was done and his wounds healed well. He had some slight residual weakness of the forearm, but the fracture united with no sepsis.
The only patient with both radius and ulna fractures, who completed follow-up, developed a synostosis at the fracture site. He did have decreased rotation of the forearm, but his DASH score was 8.3.
There was only one mal-union in a patient with a distal radio-ulna joint (DRUJ) disruption. The DRUJ was incompletely reduced at the time of the initial surgery and this shortened further after the nail was inserted. An ulna shortening osteotomy was performed and he regained good wrist movement, but had a pronation deficit.
The painful non-union may have been due to low-grade infection but this was never proved.
Discussion
This report is the first report detailing the outcomes of IM nailing specifically for gunshot wounds.
There is a paucity of literature describing the results of management of gunshot wounds to the radius and ulna. Extensive review of the literature reveals a small number of case series that review the outcomes of the management of these fractures.1-2,4 The consensus among these papers is that undisplaced fractures can be safely treated by plaster immobilisation, while displaced fractures should be reduced and stabilised by open reduction internal fixation (ORIF).
With time the quality and availability of new IM rods has improved and IM nailing of the radius and ulna has become a much more accepted procedure.
New literature describing the management of forearm fractures now includes IM nailing as one of the options of stabilising a displaced, comminuted fracture.8 However, even this suggestion has no published reference.
The potential benefits of IM nail insertion for gunshots are:
• less disruption of the fracture site and surrounding compromised soft tissue
• easier alignment of the bone ends to an anatomical rod.
The demographic spread of our cohort represents the population group at risk for this type of injury. This population group is the young to middle-aged working male. For many families this person is the bread winner and so a reliable stable fixation of fractures is required to allow the patient to return to work as soon as possible.
The documentation of the soft tissue injury is vital to determine the final outcome. Severe soft tissue injury with vascular and bowel injury, resulting in bacteraemia, may have serious consequences. However, it is the 'lesser' neurological and musculotendinous injuries that may be the most debilitating. Despite adequate bone treatment and fixation, a persistent neurological injury may seriously affect the functional quality as evidenced by our patients with persistent median nerve injury.
The technique of insertion of forearm rods has been refined with new anatomically designed implants, and the uniformly good results are not related to the level of training of the surgeon.
Approximately half of the procedures were performed without an assistant, although an assistant is recommended to aid with the difficult reductions and to position the forearm in the correct amount of rotation to allow the surgeon to insert the rod.
The potential benefit of this procedure is the possibility to fix the bone without opening the fracture site. The closed reduction of the fracture is usually the rate limiting step of the procedure as the rod used in this series does not require a freehand locking screw.
The DASH score was chosen as a subjective measure of outcome for the study. It is a validated, general upper limb functional scoring system. The score does not reflect on the fracture healing but the overall injury caused by the bullet. As evidenced by patients with ongoing neurological injury, the fracture may have healed but the soft tissue injury was the limitation to function and thus resulted in a high score.
None of the other studies published on the management of forearm gunshot wounds have used a subjective scoring system, so it is not possible to compare these results with other studies.
The documentation of the soft tissue injury is vital to determine the final outcome
Inadequate reduction and healing of these complex fractures can lead to limitation of movement. One patient was diagnosed with an incongruent DRUJ at the time of his injury. Although reduction was attempted, at the time of surgery it was incomplete. This patient's radius collapsed further and although the fracture united, he required a distal ulna shortening osteotomy. Patients with distal radius fractures extending into the metaphysis with DRUJ incongruity may not be ideal candidates for an IM rod. The wide distal radial metaphysis does not offer cortical support for the rod, predisposing it to angular deformity. If there is loss of the soft tissue restraints, this slight lack of support and the potential for shortening, if not well impacted, may result in progression of the incongruity.
An attempt was made to assess the radiographic outcome based on fracture union. The healing is by callus formation, which does not necessarily result in restoration of the complete cortex. However, all patients had a solid bridge of bone between the proximal and distal fragments. The more comminuted the fracture, the less uniform this bone bridge is.
Although only one patient with both bones fractured was followed up to union, it would seem that these patients may be predisposed to developing radio-ulnar synostosis. A soft tissue connection between the fracture of the radius and ulna, due to the bullet tract, may allow for bone ingrowth. This observation may not be relevant only in patients who receive an IM rod.
The true immediate benefit to this procedure is the restoration of the coronal and sagittal alignment. The cortical fit of the rod ensures almost guaranteed longitudinal alignment. Distal radial fractures, where there is flaring of the metaphyseal bone, is the one instance where perfect alignment is not guaranteed, but acceptable alignment can be achieved.
Review of the literature reveals two case series,1,2 one case report4 and overviews of the general management of these injuries.3,5
Elstrom et al1 published the first paper looking specifically at the outcomes of fractures due to gunshot wounds of the forearm. Their patient numbers and follow-up was similar to ours.
Initial management of the fractures was to stabilise the fracture by avoiding the zone of injury, either with a cast or external fixation. If necessary, a delayed open reduction internal fixation was performed. They felt that their results were 'unsatisfactory'.
They then treated six patients with ORIF and they felt the results were 'far superior'. They reported no instances of delayed union or mal-union. Only one patient had 'significantly reduced' rotation of the forearm.
Satisfactory use of the forearm was regained in 8 weeks in the ORIF group, and 4 months in the plaster cast group.
This study clearly shows that internal fixation of displaced comminuted fractures due to gunshot wounds is safe and superior to cast management.
Lenihan et al2 reviewed 37 extra-articular gunshot wounds of the forearm, 14 were displaced. Their recommendation was that displaced fractures of the radius and ulna were best treated by ORIF.
Wu4 published a case report of a combined fracture of the radius and ulna treated by debridement and external fixation.
The remaining articles Hahn et al3 and Wilson5 discuss the general management of the soft tissues and bone. They refer to the previously mentioned articles where ORIF is recommended for displaced comminuted fractures, but also mention that IM nailing can be considered. This recommendation is not referenced in either article and it may be their expert opinion.
In our series the DASH score shows a high satisfaction in patients without associated neurological compromise. Objectively, our wound healing and range of movement are at least comparable if not better than the previous studies. Radiographically, all but one patient united within six months post-operatively. These results are similar when compared to those reported for ORIF. The potential benefits of the IM nailing are the preservation of autologous bone in the area, negating the need to harvest new autologous bone from a distant site (e.g. the iliac crest) which has the potential for increased morbidity.
Although Elstrom et al1 performed delayed ORIF, it would seem that it is now possible to perform an early fixation.
There are some limitations. The rods used performed best in midshaft diaphyseal injuries. These rods are not recommended for fractures extending into the distal radial metaphysis or the olecranon.
This study is limited in that it is a case series and does not compare IM nailing directly to ORIF. This limits the conclusions that can be drawn. However, the patient population is too small to obtain adequate numbers, which would provide statistical significance.
Only 15/21 patients were available for follow-up at least three months post-operatively, with 14/21 being finally assessed at union. These numbers are similar to the follow-up obtained in other similar studies and may reflect the patient population. This is despite education of the patients, treating doctors and direct contact with the patients.
In conclusion, the implant design is user-friendly and assists in the reduction of the fracture.
The rod functioned well in maintaining the reduction and there were no cases of implant breakage. The IM nail did not result in delayed healing.
Immediate IM nailing of the radius and ulna does not increase sepsis rates in these patients and does not compromise functional outcome.
Intramedullary nailing for low-velocity gunshot wounds of the radius and ulna is a safe technique. It is recommended, particularly in patients who have displaced and comminuted fractures.
The authors wish to disclose that they have no financial interest in any of the products used in this study. No financial assistance was received in the preparation of this manuscript. Ethical approval was obtained from the Human Research Ethics Committee (Medical) of the University of the Witwatersrand, Johannesburg, protocol number M060450.
Acknowledgements
The authors wish to acknowledge the assistance of the consultants and registrars in the Department of Orthopaedics at the University of the Witwatersrand Medical School, Dr Andrew Barrow and Mr Larry Thomas.
Thanks to Sr Geraldine Nordin for her help with the article and presentation.
References
1. Elstrom JA, Pankovich AM, Egwele R. Extra-articular low-velocity gunshot fractures of the radius and ulna. J Bone Joint Surg Am. 1978 Apr; 60 (3):335-41. [ Links ]
2. Lenihan MR, Brien WW, Gellman H, Itamura J, Kuschner SH. Fractures of the forearm resulting from low-velocity gunshot wounds. J Orthop Trauma. 1992; 6 (1):32-35. [ Links ]
3. Hahn M, Strauss E, Yang EC. Gunshot wounds to the forearm. Orthop Clin North Am. 1995 Jan; 26 (1):85-93. [ Links ]
4. Wu CD. Low-velocity gunshot fractures of the radius and ulna: case report and review of the literature. J Trauma. 1995 Nov; 39 (5):1003-1005. [ Links ]
5. Wilson RH. Gunshots to the hand and upper extremity. Clin Orthop Relat Res. 2003 Mar (408):133-44. [ Links ]
6. Bartlett CS. Clinical update: gunshot wound ballistics. Clin Orthop Relat Res. 2003 Mar(408):28-57. [ Links ]
7. Street DM. Intramedullary forearm nailing. Clin Orthop Relat Res. 1986 Nov(212):219-30. [ Links ]
8. Wilson RHM. Gunshots to the Hand and Upper Extremity. Clin Orthop Relat Res. 2003 March 2003(408):133-44. [ Links ]
 Reprint requests:
Reprint requests:
Dr BR Gelbart
Linksfield Park Medical Centre, Suite 303
24 12th Avenue Linksfield West ,2192
Tel: +27 11 485 1706, Fax: +27 11 640 1838
Email: bradgelbart@icon.co.za
This is a summary of a MMed research report submitted to the University of the Witwatersrand Medical School for the degree of MMed by the first author.














