Servicios Personalizados
Articulo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en Google
Similares en Google
Compartir
SA Orthopaedic Journal
versión On-line ISSN 2309-8309
versión impresa ISSN 1681-150X
SA orthop. j. vol.12 no.3 Centurion sep. 2013
UPPER LIMB
Restoration of teardrop angle (TDA) in distal radius fractures treated with volar locking plates
G PienaarI; C AnleyII; A IkramIII
IMBChB(Stell) Orthopaedic Registrar
IIMBChB Orthopaedic Registrar
IIIMBBS, FCS Orth(SA) Senior Consultant, Head of Hand Unit Department of Orthopaedics, Tygerberg Academic Hospital
ABSTRACT
BACKGROUND: Distal radius fractures are among the most common fractures of the upper extremity. Failure to reduce and stabilise the lunate facet fragment intra-operatively has been shown to result in poor functional and radiographic outcomes. Medoff5 introduced the teardrop angle (TDA), which can herald the presence of articular incongruity of the lunate facet. We assess the reduction of the TDA in intra-articular distal radius fractures treated with volar locking plates.
METHODS: This was a retrospective review of the pre- and post-operative TDA in two groups of patients. One group had arthroscopy-assisted reduction prior to volar locking plate fixation, while the other had volar locking plate fixation with fluoroscopy alone to guide reduction. We measured the TDA using the 'central axis' method on the standard lateral wrist X-ray as well as the distal radial tilt angles both pre- and post-operatively.
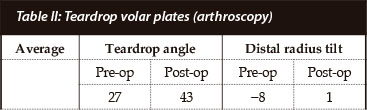
RESULTS: In the arthroscopy group, the average pre- and post-surgery TDA was 27° and 43° respectively, while in the fluoroscopy group, the average TDA pre- and post-operatively was 26° and 42° respectively. There was no significance between the two groups (p=0.98) and none of the fractures had a normal TDA post reduction.
CONCLUSION: Whichever technique was used to reduce fractures, the average TDA was not restored to normal. The unawareness of this radiological landmark, its measurement and the significance thereof might be the reason for this. Volar tilt angles were restored close to normal values, a parameter that is well known and actively looked at during reduction under fluoroscopy.
Keywords: distal radius fractures, volar locking plates, arthroscopy, lunate facet, teardrop angle
Introduction
Distal radius fractures are common fractures of the upper extremity, estimated to account for one-sixth of all fractures seen and treated in emergency rooms.1-3 These fractures are seen in a bimodal age distribution and usually result from a low-energy trauma. Displaced fractures involving the articular surface of the distal radius have the worst prognosis because of the potential for incongruity and arthrosis of the radiocarpal and distal radio-ulnar joints.4 On plain radiographs, Robert Medoff5 introduced the teardrop angle (TDA), which is a radiographic parameter that gives information on the congruity of the lunate facet. This is measured as the angle formed between the central axis of the teardrop and the radial shaft. Although many surgeons are unaware of this parameter, it is important because an abnormal TDA can herald the presence of articular incongruity of the lunate facet.
The purpose of this study was to assess the reduction of the lunate facet in intra-articular distal radius fractures before we became aware of the importance of the TDA.
Materials and methods
Definition of TDA
The teardrop is the U-shaped outline of the volar rim of the lunate facet of the distal radius. It is identified on the lateral wrist X-ray view and is particularly distinct on the 10° lateral view. The teardrop angle is formed between a line through the central axis of the teardrop and a line in the centre of the distal radius.
Subject characteristics
We looked at two separate groups of skeletally mature patients with distal radius fractures. All had surgical treatment in the form of a volar locking plate. Patients had a CT scan of the wrist prior to surgery and only the fractures involving the lunate facet were reviewed. We wanted to determine if there was any difference in reduction of the lunate facet using arthroscopy assistance compared to fluoroscopy alone.
Our first group of patients were taken from a study done in 2010 (Jan-Dec) in our Hand Unit. All of these patients had a standard Henry's approach to the distal radius. Fracture fragments were reduced under fluoroscopy and K-wires used for provisional stabilisation of fracture. The radio-carpal joint was then examined arthroscopically to assess reduction, and changes were made if there were any articular steps or incongruity. This was followed by internal fixation with a volar locking plate. The mean age was 40.7 years (range: 20-79 years) and there were 12 males and 18 females. Fractures were classified according to the AO Müller classification and included 14 type C1s; four type C2s and 12 type C3 fractures.
The TDA is formed between a line through the central axis of the teardrop and a line in the distal radius
In the other group of 30 patients, the same fractures types were treated with a volar locking plate using fluoroscopy alone intra-operatively to guide reduction. These patients were taken from the same time period as the arthroscopy group and there were no specific selection criteria. The mean age was 39.4 (range: 17-66 years) and there were 15 males and females each in this group. It included ten type C1s; eight type C2s and 12 type C3 fractures.
Radiographic parameter measurement
We measured the TDA using the 'central axis' method on standard lateral wrist X-rays. This is the angle formed between a line drawn through the central axis of the teardrop and a line through the central axis of radial shaft (Figure 1).

The distal radial tilt angles were formed between a line perpendicular to the central axis of the radius and a line connecting the dorsal and palmar margins of the articular surface of the distal radius. All measurements were made on computer radiology workstations (iSite, PACS). Data was analysed and the average determined for each parameter and group before and after surgery.
Statistical analysis
Statistical analysis was done with STATICTICA version 11. The paired t-test was used for group comparison with an alpha error of 0.05. Values of P < 0.05 indicated statistical significance.
Results
Results obtained in our study show that the TDA in both groups were almost similar pre- and post-operatively (p=0.98) and that the TDA was not restored to normal value. (Average TDA were 43°, compared to the normal TDA of 70°.) As a secondary result, we saw that the distal radial tilt angles were restored close to normal in both groups (Tables I and II).

Discussion
The purpose of this study was to assess the reduction of the TDA in intra-articular distal radius fractures before we became aware of this radiological parameter and its significance. To understand the complexity of these fractures one should be aware of the main fracture fragments produced in intra-articular distal radius fractures.
The purpose of this study was to assess the reduction of the TDA in intra-articular distal radius fractures before we became aware of this radiological parameter and its significance
Melone3 described these fragments: radial styloid facet, the dorsal lunate facet, and the volar lunate facet. The term 'die-punch' is used for an impacted fracture of the lunate facet. Fractures involving the lunate facet are a challenge to treat effectively.4 The volar rim of the lunate facet is an important bony structure in maintaining stability of the radiolunate articulation, and failure to reduce and stabilise the lunate facet intra-operatively, has been shown to result in poor functional and radiographic outcomes.4,5 With axial loading injuries of the intermediate column of the distal radius, the lunate is driven into the lunate facet, with resulting dissociation of the volar and dorsal articular surfaces. With further impaction into the metaphyseal bone, the volar rim rotates dorsally (hyperextends) into the metaphyseal cavity.6
Once parameters like the volar tilt and radial inclination are restored intra-operatively, depression of the TDA is the only evidence that reduction is incomplete and articular incongruity remains. The key for success is the accurate assessment of standard radiographs. Being able to recognise subtle changes on radiographs can provide significant information that can be used to understand the pattern of the fracture. Unfortunately, much of the information may be missed if the surgeon is not trained to recognise it.6 With the advances of CT scan and MRI, complex fractures can be assessed accurately prior to surgery but the routine use of these special investigations is not possible at certain centres.
As mentioned before, the TDA gives us information on the alignment of the lunate facet. A change in the normal TDA may indicate a displaced intra-articular fracture fragment. Studies show that loss of TDA between the fractured and uninjured wrist significantly related to reduced grip strength and worse DASH score.7
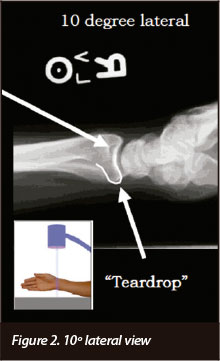
Because the radial inclination of the ulnar, two-thirds of the articular surface is 10° to the long axis of the shaft; it gives an oblique projection of the joint surface on standard lateral view. With the forearm in 10° elevation or the XR tube 10° proximally directed, it allows direct visualisation of the lunate facet, with greater detail, in order to evaluate any sagittal plane offset (Figure 2).
Studies done by Medoff6 showed that the normal TDA is 68° (67-70) and there is no significant difference between genders. On the contrary, another study found a difference in the TDA measurement using standard and 10° lateral, and showed that there is an increased reliability of the measurement on the 10° lateral view.8
Looking at the results obtained in our study, we found that whichever technique was used to determine reduction success (arthroscopy or fluoroscopy), the average TDA was not restored to normal. The reason arthroscopy was not useful in that regard is because determining the amount of angular deformity with a scope is very difficult. It can be used to reduce the articular step-off, but once the step is reduced, an angular deformity of the teardrop can still be present and will not be appreciated by the arthroscopy. The slight improvement in post-reduction TDAs can be attributed to the reduction of the associated metaphyseal fracture that also influences the angle. The failure to reduce the TDA in the fluoroscopy group can be attributed to the fact that this was never assessed intra-operatively. Very few surgeons are aware of the TDA and its significance, and therefore it is not something that is routinely assessed during reduction in theatre. The 10° lateral wrist X-ray gives a very good outline of the lunate facet and makes measurement under fluoroscopy easy to assess proper fracture reduction.
The volar tilt angle was adequately reduced in both groups, possibly because that is one of the landmarks actively being assessed during reduction under fluoroscopy.
The possible limitations in the study were the fact that there were no standardisation criteria for the lateral wrist X-rays and the fact that we used the standard lateral to the 10° lateral view as advocated by Fujitani et al.8
We think that the teardrop angle is a reliable parameter for measurement of the lunate facet displacement in intra-articular distal radius fractures. The TDA measurement may also be helpful in assessment of the quality of reduction intra-operatively and post-reduction.
The content of this article is the sole work of Dr Pienaar and the senior author, Dr Ajmal Ikram. No benefits of any form have been received from a commercial party related directly or indirectly to the article. The research on scope-assisted reduction prior to volar plating has been approved by the ethical committee.
References
1. Golden GN. Treatment and prognosis of Colles' fracture. Lancet 1963; 1:511-14. [ Links ]
2. Jupiter JB. Current concepts review - Fractures of the distal end of radius. J Bone Joint Surg Am. 1991; 73A:461-69. [ Links ]
3. Melone CP Jr. Distal radius fractures: patterns of articular fragmentation. Orthop Clin North Am 1993; 24:239-53. [ Links ]
4. Harness NG, Ring D, Zurakowski D, Harris GJ, Jupiter JB. The influence of three-dimensional computed tomography reconstructions on the characterization and treatment of distal radial fractures. J Bone Joint Surg Am. 2006; 88:1315-23. [ Links ]
5. Fernandez JJ, Gruen GS, Herndon JH. Outcome of distal radius fractures using the short form 36 health survey. Clin Orthop Relat Res 1997; 341:36-41. [ Links ]
6. Medoff, RJ. Essential radiographic evaluation for distal radius fractures. Hand Clin 2005; 21:279-88. [ Links ]
7. Forward D, Davis T. The teardrop angle and AP distance in fractures of the distal radius. J Bone Joint Surg Br 2011; 93-B:Supp I 6. [ Links ]
8. Fujitani R, Omokawa S, Iida A, Santo S, Tanaka Y. Reliability and clinical importance of teardrop angle measurement in intra-articular distal radius fracture. JHS. 2012; 17A:454-59. [ Links ]
 Reprint requests:
Reprint requests:
Dr G Pienaar
Email: Gerhardpienaar@gmail.com














