Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
SA Orthopaedic Journal
versão On-line ISSN 2309-8309
versão impressa ISSN 1681-150X
SA orthop. j. vol.12 no.2 Centurion Jan. 2013
KNEE
Total knee replacement infected with Mycobacterium tuberculosis: A case study and review of the literature
JD BurgerI; H de JonghII
IMBChB(Stell), FCS(Ortho) Registrar Department of Orthopaedic Surgery, Stellenbosch University
IIMBChB(Stell), MMed(Ortho), DA Head: Arthroplasty Unit Department of Orthopaedic Surgery, Stellenbosch University
ABSTRACT
Prosthetic joint infection is an infrequent complication occurring in approximately 1% of primary joint arthroplasty.1,2 It often is a devastating complication necessitating prolonged treatment and multiple surgeries.3 The majority are due to staphylococcal infections followed by Gram-negative bacilli and Streptococcus species, but atypical and zoonotic infections do occur.4,5
Mycobacterium tuberculosis infections of prosthetic joints have been described in sporadic reports. Osteoarticular tuberculosis (TB) historically accounts for between 1% and 4% of all TB infections, making it one of the more common extra-pulmonary sites.6 During the past decade reported TB infections in South Africa have doubled and the estimated incidence over the last 15 years has risen three-fold. This staggering rise is exclusively due to the Human Immunodeficiency Virus (HIV) pandemic with more than half being HIV positive.7 However, only 20% of osteoarticular TB is associated with pulmonary disease.6,8
Despite significant efforts TB remains one of the most challenging global health problems affecting not only developing countries. Its relevance has been promoted by recent reports from, among others, the United Kingdom and the Netherlands, indicating that there has been a reversal of its decline in these developed countries which directly relates to immigration.9,10,11 The emergence of multidrug-resistant (MDR) and extensively drug-resistant (XDR) tuberculosis has further complicated its treatment, with the largest number of reported XDR tuberculosis cases coming from South Africa.12
Key words: total knee replacement, Mycobacterium tuberculosis, peri-prosthetic joint infection, review
Case report
A 70-year-old man presented to us complaining of chronic knee pain. His pain had worsened over several years resulting in limitation of his walking distance and activities of daily living. Radiographs revealed degenerative changes in all three compartments of his right knee and a 14° intra-articular valgus deformity (Figures 1-3). A diagnosis of osteoarthritis was made but in retrospect the presence of peri-articular osteopaenia was noted as seen with an inflammatory or infective arthritis. There was however no history of any inflammatory rheumatologic disease and he had no history of any previous TB disease, exposure to a TB contact or constitutional symptoms suggesting an occult infection. No signs of immune compromise were apparent and subsequent HIV testing was non-reactive.

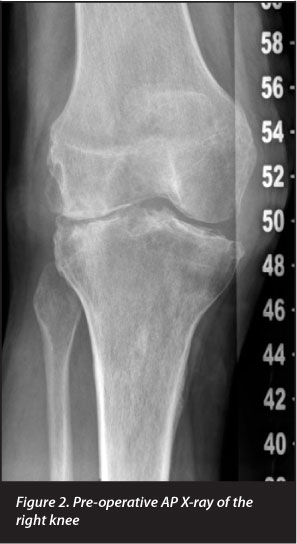

The decision was made to perform a cemented total knee replacement (TKR).
Pre-operative workup included a normal chest radiograph, white cell count of 4.3 χ 109/L and an erythrocyte sedimentation rate (ESR) of 51 mm/hour. Urine microscopy and culture was clear and pre-operative screening swabs did not culture Staphylococcus. Rheumatologic screen was normal and no aetiology could be found for the elevated ESR.
Despite significant efforts TB remains one of the most challenging global health problems affecting not only developing countries
A cemented TKR was ¡ performed in July 2009 I with intra-operative | findings in keeping | with the diagnosis of ¡ primary osteoarthritis. | The synovium did not have the macroscopic appearance of hyper-trophic or caseating necrosis as seen in tuberculous arthritis. | Post-operative recovery ¡- was uncomplicated and at the 6-week follow-up his wound had healed and he had active motion of his right knee in an arc from 5° to 90°. Eight weeks post-operatively he presented with painful erythema infero-lateral to his tibial tubercle, an ESR of 25 and a CRP of 19. He was admitted and treated with intravenous cloxaállin. His condition deteriorated and he developed an abscess infero-lateral to the tibial tubercle, subsequently forming a draining sinus. Formal debridement of the joint was performed three months post-operatively in theatre with synovial tissue negative for Gram stain and aerobic and anaerobic bacterial cultures. Neither of the components was found to be loose and was therefore retained. Thereafter he was treated with a six-week course of intravenous cloxacillin and rifampicin.
Following initial improvement, the pain and swelling returned after three months with an ESR of 42 and CRP of 60.-
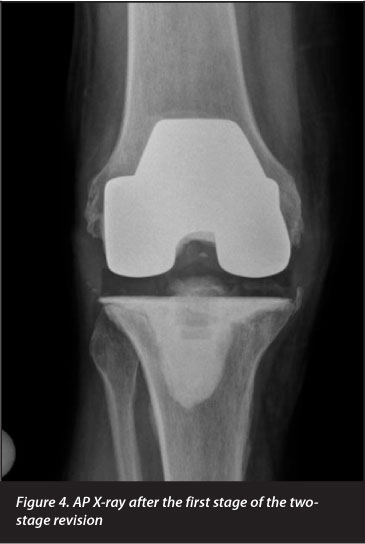
The first stage of a two-stage revision was performed with removal of both components and replacement of the femoral component after it was autoclaved (Figures 4 and 5). Synovial tissue sent for microscopy and culture again failed to isolate an organism. Three months of antibiotic treatment with oral cloxacillin, rifampicin and ciprofloxacin were given. The infection resolved clinically and the second stage revision with replacement of both components was performed 10 months after the first stage.

In May 2011 a painful erythematous swelling and sinus returned and a third debridement with component removal and replacement of the autoclaved femoral part was performed. Synovial tissue again did not culture any aerobic or anaerobic bacteria. Microscopy did not show any acid-fast bacilli but specific TB culture was requested and Mycobacterium tuberculosis was cultured after 15 days.
Medical treatment consisted of a four-drug TB regimen (rifampicin, isoniazid, ethambutol and pyrazinamide) for 18 months. A rapid clinical response resulted in full resolution of the infectious symptoms after 3 months. Retrospective review of a chest CT done for a suspected post-operative pulmonary embolus after the first stage revision revealed mediastinal lymphadenopathy in keeping with tuberculosis. Despite this his chest radiographs remained normal.
Post-operative recovery was uncomplicated and at the 6-week follow-up his wound had healed and he had active motion of his right knee. Eight weeks post-operatively he presented with painful erythema infero-lateral to his tibial tubercle
Discussion
Prosthetic joint infection with Mycobacterium tuberculosis is | rare. One retrospective review of 2 116 prosthetic joint infections over a 22-year period found only seven such cases.13 In 1977, McCullough reported the first case of tuberculous infection of a total hip arthroplasty (THA) seven years after implantation.14 TB of a prosthetic joint can follow one of three patterns: active undiagnosed TB arthritis present at the time of surgery; haematogenous spread from a focus elsewhere; or most commonly, reactivation of latent TB arthritis following arthroplasty.515 | Previously trauma and surgery were mentioned as possible risk factors for reactivation but recent studies point to HIV as the leading risk factor for reactivation of TB in pre-viously infected joints.1617 It has been documented to occur up to 61 years after the initial infection.13,18 The risk for reactivation has been reported to be between 0% and 31%, with TKA (27%) more at risk than THA (6%).13
Despite the fact that there were no intra-operative findings suggesting TB arthritis one needs to consider this as a possible diagnosis at presentation. If this was indeed the case it acts as a reminder of TB as 'the great imposter'. The focus of this review is TB of prosthetic joints in patients with no known previous TB infections. On review of the English literature only 29 cases were found. It usually involved total hip or knee replacements but two cases of TB of shoulder prostheses have been reported.13-1519-38
Similar to other TB infections it presented insidiously and diagnosis was almost always delayed - in this series averaging five months from presentation to culture diagnosis. The duration from joint replacement to infection does not seem to follow a distinct pattern and ranged from two months to 38 years. Non-specific symptoms like pain and swelling predominated with sinus formation present in more than half.
Despite the fact that there were no intra-operative findings suggesting TB arthritis one needs to consider this as a possible diagnosis at presentation
Systemic symptoms were uncommon with fever reported in only five cases, all being immune-compromised and of which two were secondarily infected.15,22,24,26,38 One of these warranting special mention was an HIV-positive patient who died of disseminated multi-drug resistant TB ten months after receiving a total knee replacement. Dissemination may have resulted from a total knee replacement done in a joint with unsuspected osteoarticular tuberculosis.15
Inflammatory markers including ESR and CRP were usually elevated to some degree but are non-specific. The ESR has been found to often return to pre-operative levels only after 90 days and can be elevated for more than a year following arthroplasty surgery, making it difficult to interpret.39,40
Radiographic changes in native joints follow Phemister's triad of joint tuberculosis (joint space narrowing, subchondral osteopaenia and lateral osseous erosions) which resemble signs of osteoarthritis, and retrospectively were probably diagnosed as such in two cases.15,33 Pre-operative chest radiographs were reported as abnormal in only three which showed apical scarring suggestive of previous pulmonary TB.19,22,24 Chest radiographs therefore do not seem to be very sensitive and although careful examination of the pre-oper-ative joint radiographs may be indicative in the cases of active but subclinical TB arthritis, it can be exceedingly difficult to differentiate from osteoarthritis in this setting.
Diagnosis proved difficult in nearly all the cases. Most importantly this can be attributed to the fact that the initial microbiological investigations did not include specific requests for TB culture. Another factor is co-infection which complicated 37% of cases and can mask the diagnosis of TB. Staphylococcal species were the most common co-infecting organism but multiple organisms were cultured in several cases that had a draining sinus.14,22,24,26,3233,34,38
Positive culture is essential to confirm the diagnosis and exclude other pathogens in atypical infections including fungi, zoonotic microorganisms and other mycobacterium species.5 The diagnosis was made by isolating Mycobacterium tuberculosis by culture of tissue or synovium in 55%; culture of aspirated fluid in 18%; positive Ziehl-Nielsen (ZN) stain in 23%; and by Polymerase Chain Reaction (PCR) on synovial tissue culture in one case. In six cases that eventually cultured TB the initial ZN stain was negative. Positive culture was obtained after average culture duration of 4.5 weeks highlighting the importance of continued culture and follow-up of results. Specific requests to the laboratory for TB culture are imperative and cultures need to continue for at least six weeks.41 Histology can be helpful and showed chronic granulomatous inflammation in 73%, including three cases that stained ZN negative but went on to culture TB. Osteoarticular TB is a pauci-bacillary disease and owing to its high sensitivity PCR shows much potential for diagnostic purposes.35,42,43
Medical management with multidrug anti-TB therapy according to proven sensitivities remains the mainstay of treatment. Duration of therapy is controversial with nine months the minimum. The average duration in this series was 15 months but a definite trend towards shorter treatment periods can be observed with only two cases in the last decade receiving treatment for longer than 12 months.
Surgical treatment depends on the quality of component fixation. If it remains stable components may be retained and medical treatment with or without debridement may suffice. This strategy was successful in seven cases (two THA and five TKA).14,26,30,33,35-37 In five of these there was little diagnostic delay with anti-TB treatment started within a month of presentation. Diagnosis in the other two was delayed by four months or more, the one being complicated by sinus formation and secondary infection.26,30 Repeated debridement and coverage with gastrocnemius flap achieved complete wound healing in this case.26 In the presence of component loosening or secondary bacterial infection, removal and staged revision is advised and achieved satisfactory outcomes in three cases. Insertion of an antibiotic-impregnated spacer may help to preserve the soft tissue envelope.
Staged arthrodesis was done in three cases and is aimed to eliminate the disease but is not without its problems, with knee arthrodesis being particularly poorly tolerated. In six hips excision arthroplasty was performed.13,22,23,29,31 A Girdlestone excision arthroplasty continues to be a viable option and although the infection was successfully treated in all of these it does not guarantee a satisfactory functional outcome.
Conclusion
Prosthetic joint infection with TB in the absence of a prior TB history is rare and as such the diagnosis is usually delayed. A high index of suspicion is invaluable for its diagnosis. The clinical signs that may suggest prosthetic joint infection due to tuberculosis are on-going symptoms despite negative cultures, resistance to treatment and progression to sinus formation. Obtaining synovial specimens and specifically requesting TB culture and histology are the most helpful investigations. Early diagnosis and treatment may prevent prosthetic loosening and avoid revision surgery with great benefit to the patient and preservation of resources.
The increasing life expectancy seen in patients living with HIV makes them possible candidates for joint replacement surgery. This together with the high prevalence of TB both potentially increases the risk for this condition. As presented at the recent congress of the South African Society for Arthroplasty, joint replacement surgery is also increasingly becoming a treatment modality available to many in developing countries in which TB and HIV often has a high prevelance.44,45 The combination of these factors has the potential to lead to an increased incidence of prosthetic joint infection with TB.
References
1. Phillips JE, Crane TP, Noy M, Elliott TS, Grimer RJ. The incidence of deep prosthetic infections in a specialist orthopaedic hospital: a 15-year prospective survey. J Bone Joint Surg Br. 2006 Jul;88(7)943-8. [ Links ]
2. Pulido L, Ghanem E, Joshi A, Purtill JJ, Parvizi J. Periprosthetic joint infection: the incidence, timing, and predisposing factors. Clin Orthop Relat Res. 2008 Jul;466(7):1710-15. [ Links ]
3. Bozic KJ, Ries MD. The impact of infection after total hip arthroplasty on hospital and surgeon resource utilization. J Bone Joint Surg Am. 2005 Aug;87(8):1746-51. [ Links ]
4. Peel TN, Buising KL, Choong PF. Prosthetic joint infection: challenges of diagnosis and treatment. ANZ J Surg. 2011 Jan;81(1-2):32-9. [ Links ]
5. Marculescu CE, Berbari EF, Cockerill FR 3rd, Osmon DR. Fungi, mycobacteria, zoonotic and other organisms in prosthetic joint infection. Clin Orthop Relat Res. 2006 Oct;451:64-72. [ Links ]
6. Tuli SM. General principles of osteoarticular tuberculosis. Clin Orthop Relat Res. 2002 May;(398):11-19. [ Links ]
7. World Health Organisation. Global TB Control Report 2011 www.who.int/tb/data. [ Links ]
8. Davies PD, Humphries MJ, Byfield SP, et al. Bone and joint tuberculosis: a survey of notifications in England and Wales. J Bone Joint Surg Br 1984;66-B:326-50. [ Links ]
9. Jutte PC, van Loenhout-Rooyackers JH, Borgdorff MW, van Horn JR. Increase of bone and joint tuberculosis in The Netherlands. J Bone Joint Surg Br. 2004 Aug;86(6)901-14. [ Links ]
10. Talbot JC, Bismil Q, Saralaya D, Newton DA, Frizzel RM, Shaw DL. Musculoskeletal tuberculosis in Bradford - a 6-year review. Ann R Coll Surg Engl. 2007 May;89(4):405^09. [ Links ]
11. Bennett J, Pitman R, Jarman B, Innes J, Best N, Alves B, Cook A, Hart D, Coker R. A study of the variation in tuberculosis incidence and possible influential variables in Manchester, Liverpool, Birmingham and Cardiff in 1991-1995. Int J Tuberc Lung Dis. 2001 Feb; 5 (2):158-63. [ Links ]
12. Nathanson E, Nunn P, Uplekar M, Floyd K, Jaramillo E, Lõnnroth K, Weil D,Raviglione M. MDR tuberculosis-critical steps for prevention and control. N Engl J Med. 2010 Sep 9; 363 (11):1050-58. [ Links ]
13. Berbari EF, Hanssen AD, Duffy MC, Steckelberg JM, Osmon DR. Prosthetic joint infection due to Mycobacterium tuberculosis: a case series and review of the literature. Am J Orthop (Belle Mead NJ). 1998 Mar;27(3)219-27. [ Links ]
14. McCullough CJ. Tuberculosis as a late complication of total hip replacement. Acta Orthop Scand 1977;48:508-10. [ Links ] 15. Marschall J, Evison JM, Droz S, Studer UC, Zimmerli S. Disseminated tuberculosis following total knee arthroplasty in an HIV patient. Infection. 2008 Jun;36 (3) 274-78. [ Links ]
16. Horsburgh CR Jr. Priorities for the treatment of latent tuberculosis infection in the United States. N Engl J Med. 2004 May 13; 350 (20) 2060-67. [ Links ]
17. Johnson R, Barnes KL, Owen R. Reactivation of tuberculosis after total hip replacement. J Bone Joint Surg Br. 1979 May; 61-B (2):148-50. [ Links ]
18. de Haan J, Vreeling AW, van Hellemondt GG. Reactivation of ancient joint tuberculosis of the knee following total knee arthroplasty after 61 years: a case report. Knee. 2008 Aug;15(4)33&38. [ Links ]
19. Bryan WJ, Doherty JH Jr, Sculco TP. Tuberculosis in a rheumatoid patient. A case report. Clin Orthop Relat Res 1982;171206-208. [ Links ]
20. Zeiger LS, Watters W, Sherk H. Scintigraphic detection of prosthetic joint and soft tissue sepsis secondary to tuberculosis. Clin Nucl Med 1984;9:638-39. [ Links ]
21. Wolfgang GL. Tuberculosis joint infection following total knee arthroplasty. Clin Orthop Relat Res 1985;201:162-66. [ Links ]
22. Levin ML. Miliary tuberculosis masquerading as late infection in total hip replacement. Md Med J 1985;34:153-55. [ Links ]
23. Baldini N, Toni A, Greggi T, Giunti A. Deep sepsis from Mycobacterium tuberculosis after total hip replacement. Case report. Arch Orthop Trauma Surg 1988;107:186-88. [ Links ]
24. Tokumoto JI, Follansbee SE, Jacobs RA. Prosthetic joint infections due to Mycobacterium tuberculosis: report of three cases. Clin Infect Dis 1995;21:134-36. [ Links ]
25. Lusk RH, Wienke EC, Milligan TW, Albus TE. Tuberculous and foreign-body granulomatous reactions involving a total knee prosthesis. Arthritis Rheum 1995;38:1325-27. [ Links ]
26. Spinner RJ, Sexton DJ, Goldner RD, Levin LS. Periprosthetic infection due to Mycobacterium tuberculosis in patients with no prior history of tuberculosis. J Arthroplasty 1996;11:217-22. [ Links ]
27. Kreder HJ, Davey JR. Total hip arthroplasty complicated by tuberculous infection. J Arthroplasty 1996;11:111-14. [ Links ]
28. Al-Shaikh R, Goodman SB. Delayed-onset Mycobacterium tuberculosis infection with staphylococcal superinfection after total knee replacement. Am J Orthop 2005;32:302-305. [ Links ]
29. Fernandez-Valencia JA, Garcia S, Riba J. Presumptive infection of a total hip prosthesis by Mycobacterium tuberculosis: a case report. Acta Orthop Belg 2003;69:193-96. [ Links ]
30. Marmor M, Parnes N, Dekel S. Tuberculosis infection complicating total knee arthroplas-ty: report of 3 cases and review of the literature. J Arthroplasty 2004;19:397-400. [ Links ]
31. Kaya M, Nagoya S, Yamashita T, Niiro N, Fujita M.Peri-prosthetic tuberculous infection of the hip in a patient with no previous history of tuberculosis. J Bone Joint Surg 2006;88-B :394-95. [ Links ]
32. Khater FJ, Samnani IQ, Mehta JB, Moorman JP,Myers JW. Prosthetic joint infection by Mycobacterium tuberculosis: an unusual case report with literature review. South Med J 2007;100:66-69. [ Links ]
33. Shanbhag V, Kotwal R, Gaitonde A, Singhal K. Total hip replacement infected with Mycobacterium tuberculosis. A case report with review of literature. Acta Orthop Belg 2007;73:268-274. [ Links ]
34. Hattrup SJ, Bhagia UT. Shoulder arthroplasty complicated by mycobacterium tuberculosis infection: a case report. J Shoulder Elbow Surg. 2008 Nov-Dec;17(6):e5-7. [ Links ]
35. Neogi DS, Kumar A, Yadav CS, Singh S. Delayed periprosthetic tuberculosis after total knee replacement: is conservative treatment possible? Acta Orthop Belg. 2009 Feb;75(1):136-40. [ Links ]
36. Uppal S, Garg R. Tubercular infection presenting as sinus over ankle joint after knee replacement surgery. J Glob Infect Dis. 2010 Jan;2(1):71-72. [ Links ]
37. Lee CL, Wei YS, Ho YJ, Lee CH. Postoperative Mycobacterium tuberculosis infection after total knee arthroplasty. Knee. 2009 Jan;16(1):87-89. [ Links ]
38. Lederman E, Kweon C, Chhabra A. Late Mycobacterium tuberculosis infection in the shoulder of an immunocompromised host after hemiarthroplasty: a case report. J Bone Joint Surg Am. 2011 Jun 15;93(12):e67(1-4). [ Links ]
39. Park KK, Kim TK, Chang CB, Yoon SW, Park KU. Normative Temporal Values of CRP and ESR in Unilateral and Staged Bilateral TKA. Clin Orthop Relat Res. 2008 Jan;466(1):179-88. [ Links ]
40. Aalto K, Osterman K, Peltola H, Rãsânen J. Changes in erythrocyte sedimentation rate and C-reactive protein after total hip arthroplasty. Clin rthop Relat Res. 1984 Apr;(184) :118-20. [ Links ]
41. Ellis ME, el-Ramahi KM, al-Dalaan AN. Tuberculosis of peripheral joints: a dilemma in diagnosis. Tuber Lung Dis 1993;74:399-404. [ Links ]
42. Sun YS, Lou SQ, Wen JM, Lv WX, Jiao CG, Yang SM, Xu HB. Clinical value of polymerase chain reaction in the diagnosis of joint tuberculosis by detecting the DNA of Mycobacterium tuberculosis. Orthop Surg. 2011 Feb;3(1):64-71. [ Links ]
43. Nakano N, Wada R, Yajima N, Yamamoto N, Wakai Y, Otsuka H. Mycobacterial infection of the musculoskeletal tissues: the use of pathological specimens for identification of causative species by PCR-direct sequencing of 16S rDNA. Jpn J Infect Dis. 2010 May;63(3):188-91. [ Links ]
44. Lubega N, Mkandawire NC, Sibande GC, Norrish AR, Harrison WJ. Joint replacement in Malawi: establishment of a National Joint Registry. J Bone Joint Surg Br. 2009 Mar;91(3):341-43. [ Links ]
45. Lisenda, L. Development of Lower Limb Arthroplasty service in a developing country: Botswana experience. Paper presented at the South African Society for Arthroplasty Congress. South Africa 2013 April 17-20. [ Links ]
 Reprint requests:
Reprint requests:
Dr JD Burger
PO Box 19063 Tygerberg 7505
Tel: 021 938 5458
Email: dawidburger@mweb.co.za














