Servicios Personalizados
Articulo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en Google
Similares en Google
Compartir
SA Orthopaedic Journal
versión On-line ISSN 2309-8309
versión impresa ISSN 1681-150X
SA orthop. j. vol.12 no.2 Centurion ene. 2013
HIP
Bilateral ankylosis of the hip: A case report
Dr L du PlessisI; Prof TLB le RouxII
IMBChB(UP) Orthopaedics Registrar, Department of Orthopaedics, 1 Military Hospital, University of Pretoria, Faculty of Health Sciences, School of Medicine, South Africa
IIMBChB(Pret), MMed(Orth)(Pret), FCS(Orth) Orthopaedics Registrar Department of Orthopaedics, 1 Military Hospital, University of Pretoria, Faculty of Health Sciences, School of Medicine, South Africa
ABSTRACT
Bilateral ankylosis of the hip is a surgical challenge even to the experienced surgeon. We present a case of bilateral ankylosis of the hips and review of literature in order to see if there are any tips and tricks to be kept in mind before attempting this type of surgery.
Key words: bilateral ankylosis hips, surgery, approach
Introduction
Bilateral hip ankylosis is a rare entity. In the past an arthrodesis was performed for symptomatic patients but numerous studies have however proven that the outcome of total hip arthroplasty in ankylosis is favourable.1-7 Ankylosis of the hip is very difficult to treat surgically and should only be attempted by an experienced surgeon together with comprehensive pre-operative planning.1
It is furthermore important to inform the patient about the possible complications of this procedure. A study performed by the Centre of Hip Surgery in the UK evaluated 187 patients (208 hips). Some of the complications reported were: nerve palsies, infection, dislocations and heterotroph-ic ossification. Implant survival was 96.1% at ten years, and 72% at 26 years.1
Conversion of an ankylosed hip is especially indicated if the patient has pain, functional disability, leg length discrepancy and osteoarthritis of other adjacent joints (especially the lumbar spine and knees) due to the deformity.2-5
Ankylosis of the hip is very difficult to treat surgically and should only be attempted by an experienced surgeon together with comprehensive pre-operative planning
Case report
We report on a case of a patient who presented at the age of 19 years with severe left hip pain for two weeks. It was a spontaneous onset with no history of trauma, TB contact, fever, allergies, alcohol usage or smoking. There was also no history of surgery. A history of weight loss was the only significant symptom.
Clinical examination
Normal vital signs. Severe limited range of motion due to the pain in his left hip. His neurovascular examination was normal. No lymphadenopathy was present.
Blood results
CRP: 20.6; WCC: 5.3; ESR: 24
Radiology report (2002)
No fractures or dislocations, no sclerosis, no lytic areas were reported. The possibility of a left hip effusion was mentioned.
An arthrotomy was performed and specimens were sent to the laboratory. The results were as follows: • MC&S: negative; TB PCR: negative; AFB negative. Histology: Chronic inflammatory changes, possibly TB.
It was decided to start the patient on TB treatment. He completed a 9 months' course of TB treatment and responded well.
The patient followed up to apply for a disability grant in 2005 (three years after being treated initially). His pelvic X-ray was repeated at that time and bilateral sacroileitis: bilateral narrowing of the hip joints with a coarse trabecular pattern of unsure aetiology was reported. Chest, thoracic and lumbar spine X-rays were normal. The clinical notes stated that he had pain in both hips; was walking with difficulty; sitting with his hips in full extension and had no range of motion.
He defaulted on treatment until 2010. He was then seen at the clinic and re-evaluated. Significant X-ray changes were noted: Bilateral ankylosis of the hips, visible axial migration of the hip joint with bilateral loss of joint space and ankylosis of both SI joints (Figures 1-3). Chest X-rays were normal.
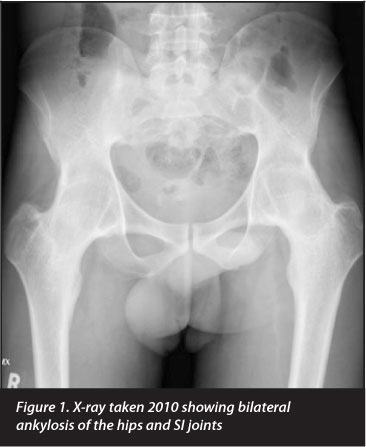
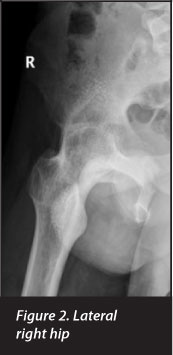

The patient followed up again in 2012 (Figures 4-8). He had no range of motion of his hips; both hips were in extension. He tilted his pelvis in order to be able to sit and had a type of 'swing through-locked' gait. Mobility was only possible due to him using his lumbar spine and knees to achieve this 'swinging through-locked' gait. The decision was made to perform a total hip replacement in order to allow him the ability to stand, walk and sit. This would improve his quality of life.
Discussion and literature review
Spontaneous ankylosis of the hip is rare, and not often documented in the literature. It can occur spontaneously -due to infective or inflammatory conditions, tuberculosis and/or trauma (Table I).

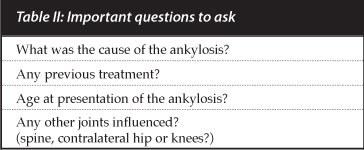
Pre-operative planning is very important and should include a proper history (Table II).
It has been reported that patients who had a previous arthrodesis for ankylosis had a poorer outcome post total hip replacement.3,7 Some studies suggested a higher failure rate in younger patients and patients with trauma to the hip.3
Clinical evaluation should be thorough with special attention paid to leg length discrepancy, deformities, range of motion and abductor function. Evaluation of the abductor function is very important, specifically in those patients whose hips fused before puberty. This is associated with a higher rate of dislocation.1,6 Pre-operative X-ray templating should be used in order to plan surgery. A CT scan can also be used in this regard.4
The positioning of the patient on the operating table and cup positioning can be very difficult and it is important to recognise this when planning the surgery. Different surgical approaches (anterolateral, posterolateral, lateral, ± trochanteric osteotomy) have been used in this type of surgery and are surgeon-dependent.1,2,4,6,9,10
Hardinge et al2 performed a lateral approach to the hip with a trochanteric osteotomy in the supine position. Kim et al10 used a posterolateral approach and Sathappen et al9 a direct lateral approach and trochanteric osteotomy.
Swanson etal8 suggest that whatever surgical procedure is used, the surgeon must aim for adequate surgical exposure in order to remove previous hardware; to identify the anterior and posterior column of the acetabulum adequately; to correct femoral deformities; and to decrease tension on the neurovascular structures and soft tissue intra-operatively.
Morsi et al11 did a prospective study in order to evaluate an adequate pre-operative plan and surgical technique to limit difficulties. They suggested using the trans-trochanteric approach in order to minimise damage to the abductor muscles. The neck-pelvis junction must be visualised for the neck cut. Make it 10 mm from the pelvis. They performed iliop-soas and subcutaneous adductor tenotomies in order to ascertain the position of the acetabular and femoral components. Subperiosteal dissection of the proximal femur in order to make it more mobile for preparation was performed. The adductor tubercle of the medial femoral condyle was used as a landmark of rotation as the lesser trochanter might be absent or malpositioned. Acetabular preparation was mostly done under screening. Use the 'edgeof the neck' cut; drill a hole in the centre of the edges and measure the depth; and ream until at least 5 mm of bone is left in the acetabulum wall. These authors concluded that identification of the edge, centre and depth before reaming is most important.
Numerous studies showed a good outcome after total hip replacement in these patients.1-7 One study by Kim et aF reported good results in patients with bilateral ankylosed hips and who underwent bilateral total hip replacement (average Harris hip score of 82.3). They however noted that it is important to remember that malpositioning of the con-tralateral limb during the procedure can cause a pelvic tilt which has to be taken into consideration with cup place-ment.5 When reaming for cup placement the surgeon must be sure of direction especially if the patient has a fixed flexion contracture. Ream until good bone stock is reached; however, beware if the patient is osteopaenic.
Malhotra et al12 suggested leaving a spike of bone at the supero-lateral acetabular margin when reaming to ensure purchase at cup placement. Increased anteversion of the femoral neck intra-operatively can cause intra- and postoperative complications. These complications include: impingement of the prosthetic neck or greater trochanter; struggling with the reduction; and anterior instability post-operatively.12
Kim et al10 evaluated the outcome of cemented hip arthro-plasty versus uncemented and found no statistical significant difference between the two. A revision rate of 17% in the cemented and 18% in the uncemented was noted. Osteolysis was 52% in the cemented and 58% in the unce-mented group.10 It is however important to note that they deliberately chose the patient population for each group.
The positioning of the patient on the operating table and cup positioning can be very difficult and it is important to recognise this when planning the surgery
Cementless procedures were used in the less severe deformities and cemented in more complicated deformities. They suggested landmarks to palpate in order to identify the acetabulum:
• Anterior: Pubic bone or anterior inferior iliac spine
• Posterior: Sciatic notch
• Inferior: obturator foramen10
Swanson et al8reported a higher risk for failure in patients younger than 50 years and with ankylosis due to prior surgery. They presented six valuable tips for surgery:
1. Look for the abductor muscles and protect them during surgery.
2. The surgeon should know exactly where the rotational centre of the acetabulum is.
3. Make sure adequate medialisation and sizing of the component by concentric reaming of the acetabulum is achieved.
4. Do not place the acetabular cup too cephalic.
5. Address the leg length discrepancy.
6. Avoid impingement and instability by correcting the femoral offset.
Always remember to counsel your patient with regard to possible complications. It has been shown that there are more complications in a patient with hip ankylosis undergoing a total hip replacement than in those with primary hip replacements (Table III).
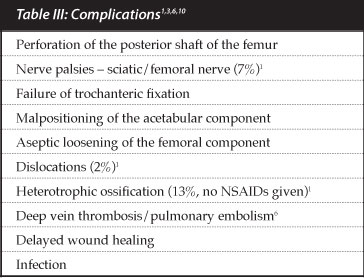
Always remember to counsel your patient with regard to possible complications
We found this surgery to be very difficult and reviewed the literature in order to guide us with 'tips and tricks' for this condition. It is a very complicated procedure and should only be performed by the experienced surgeon.
No benefits in any form have been or will be received by the authors from any commercial party related directly or indirectly to the subject of this article.
References
1. Joshi AB, Markovic L, Hardinge K, Murphy JC. Conversion of a fused hip to total hip arthroplasty. J Bone Joint Surg [Am]. 2002 Aug;84-A(8):133-41.
2. Hardinge K, Williams D, Etienne A, MacKenzie D, Charnley J. Conversion of fused hips to low friction arthroplasty. J Bone Joint Surg [Br]. 1977 Nov;59-B(4):38-92. [ Links ]
3. Kilgus DJ, Amstutz HC, Wolgin MA, Dorey FJ. Joint replacement for anky-losed hips. J Bone Joint Surg [Am] 1990 Jan;72(1):4M4. [ Links ]
4. Howard MB, Bruce WJ, Walsh W, Goldberg JA. Total hip arthroplasty for arthrodesed hips. J Orthop Surg 2002 Jun;10(1):29-33. [ Links ]
5. Kim YL, Shin SI, Nam KW, Yoo JJ, Kim YM, Kim HJ. Total hip arthroplasty for bilaterally ankylosed hips. J Arthroplasty 2007 Oct;22(7):1037-41. [ Links ]
6. Hamadouche M, Kerboull L, Meunier A, Courpied JP, Kerboull M. Total hip arthroplasty for the treatment of ankylosed hips: a five to twenty-one-year follow-up study. J Bone Joint Surg [Am]. 2001 Jul;83-A(7):992-98. [ Links ]
7. Strathy GM, Fitzgerald RH,Jr. Total hip arthroplasty in the ankylosed hip. A ten-year follow-up. J Bone Joint Surg [Am] 1988 Aug;70(7):963-66. [ Links ]
8. Swanson MA, Huo MH. Total hip arthroplasty in the ankylosed hip. J Am Acad Orthop Surg 2011 Dec;19(12):737-45. [ Links ]
9. Sathappan SS, Strauss EJ, Ginat D, Upasani V, Di Cesare PE. Surgical challenges in complex primary total hip arthroplasty. American Journal of Orthopedics (Chatham, Nj) 2007 Oct;36(10):534-41. [ Links ]
10. Kim YH, Oh SH, Kim JS, Lee SH. Total hip arthroplasty for the treatment of osseous ankylosed hips. Clin Orthop 2003 Sep(414):136-48. [ Links ]
11. Morsi E. Total hip arthroplasty for fused hips; planning and techniques. J.Arthroplasty 2007 Sep;22(6):871-75. [ Links ]
12. Malhotra J. Mastering orthopaedic techniques Total Hip Arthroplasty. Jaypee Brothers Medical Publishers; 2012. [ Links ]
 Reprint requests:
Reprint requests:
Dr L du Plessis
Department of Orthopaedics
1 Military Hospital Thaba Tshwane Pretoria South Africa
Tel: +27 12 314 0044 Cell: +27 83 635 0338
Email: leonoreduplessis@gmail.com
KEY WORDS REQUIRED IN ARTICLES
The South African Orthopaedics Journal (SAOJ)has been accepted by the Academy of Science of South Africa as a publication on their online facility, the Scientific Electronic Library Online (SciELO). This open access facility is linked to Google and is an enormous step forward for our Journal.
SciELO has requested that all authors of articles include five key words at the beginning of each article in order to make it easier to conduct a search when published online. We ask all authors to kindly comply with this request.














