Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
SA Orthopaedic Journal
versão On-line ISSN 2309-8309
versão impressa ISSN 1681-150X
SA orthop. j. vol.12 no.2 Centurion Jan. 2013
UPPER LIMP
SLAP lesions: Clinical experience of 63 cases
A Jiménez-MartínI; FJ Santos-YuberoII; M Zurera-CarmonaIII ; FJ Najarro-CidIV ; FJ Chaqués-AsensiV ; S Pérez-HidalgoVI
IMD, MMed(Orth) Upper Limb Unit (Shoulder and Elbow), Hospital FREMAP Sevilla
IIMD, MMed(Orth) Upper Limb Unit (Shoulder and Elbow), Hospital FREMAP Sevilla
IIIMD, MMed(Orth) Upper Limb Unit (Shoulder and Elbow), Hospital FREMAP Sevilla
IVMD, MMed(Orth) Head of the Upper Limb Unit, Hospital FREMAP Sevilla
VMD, MMed(Orth) Upper Limb Unit (Shoulder and Elbow), Hospital FREMAP Sevilla
VIMD, MMed(Orth) Head of the Orthopaedic and Traumatology Service; Medical Director, Hospital FREMAP Sevilla
ABSTRACT
BACKGROUND: Superior Labrum Anterior and Posterior injuries or SLAP injuries have a frequency of 3.9% to 12%, and up to 35% in contact sportsmen. Our purpose is to check this pathology in our centre and to value clinical and working final results after its treatment.
MATERIAL AND METHODS: An observational, descriptive and retrospective study of 63 patients. Medium age, sex, laterality, profession, type of SLAP, associated injuries, surgical techniques, complications, and Rowe, Constant and UCLA tests among other data, are analysed.
RESULTS: 89% men, 11% women. Median age 45.3 ± 9.8 years. Right shoulders: 68%; left 32%. Intra-operative data: predominant SLAP type was type II (59.5%). We achieved subacromial decompression in 43.5% of cases. Rowe's test: 84.5 ± 18.3 points; Constant's test 72 ± 20.4 points; UCLA test: 29.5 ± 9.1 points.
CONCLUSION: SLAP injuries constitute an important reason for shoulder pain in the labour world, although it is probably unsuspected. Treatment by means of shoulder arthroscopy with bioabsorbable bioknotless anchors is successful in many cases in allowing patients to show clinical improvement and return to work. Other concomitant injuries to SLAP must be investigated to optimise the results of surgical treatment.
Key words: SLAP, bioknotless anchors, shoulder, arthroscopy
Introduction
The labrum increases the depth of the glenoid cavity by up to 75% for the head of the humerus in the vertical direction and by up to 57% in the transversal direction.1 Although injuries to the superior labrum are infrequent, with incidences of 3.9%,2 6%3 or 12%4 reported by different authors, they are more common in people who take part in contact sports, reaching a frequency of 35%.5 In 1985 Andrews6 described injuries of the superior region of the labrum, and five years later, in 1990, Snyder7 published the first classification of these lesions, which are also known as 'SLAP' injuries (Superior Labrum Anterior and Posterior). Our hypothesis is that treatment of SLAP injuries by arthroscopy brings about a clinical improvement and allows patients to return to work. The use of knotless absorbable anchors should improve treatment since it reduces surgical time and offers an easier surgical technique.
SLAP injuries are associated with other causes of shoulder pain that often co-exist with labral lesion. Our aim was to report our own experience with this type of lesion, and to assess the clinical results obtained, using the validated Constant, UCLA and Rowe tests, as well as to review the final outcome concerning the patients' return to work.
The use of knotless absorbable anchors should improve treatment since it reduces surgical time and offers an easier surgical technique
Patients and methods
All the patients signed an informed consent form prior to being included in the study. Our study was authorised by the local ethical committee and was conducted in accordance with the ethical standards of the 1964 Declaration of Helsinki as revised in 2000.
We analysed 63 patients. We revised 63 cases from a series of 70 patients, as seven patients were lost to follow-up. The follow-up time of this series of 63 patients was approximately 2.1 (SD: 0.2) years. Their mean age was 45.3 (SD: 9.8) years, and 89% were male. In 68% of cases the right shoulder was involved, compared to 32% in which the left shoulder was affected.
The most frequent occupation was that of construction labourer, which accounted for 16% of our series, followed by transport workers (10%) and assembly workers, warehousemen and plasterers (each of which provided 10% of the total). Other professions such as crane operators, foremen, teachers, painters and policemen were found in isolated cases. Most patients reported traction of the affected limb as being the cause, with hyperabduction (arm straight above head) in 43% of cases. Direct trauma on shoulder with backward displacement of the arm was the second most frequently reported cause.
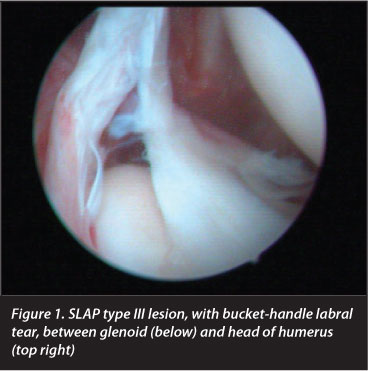
Regarding the pre-operative study, the finding of SLAP injury was confirmed in 48 cases (76.19%), compared to 23.81% in which this finding was not obtained, even though it was later confirmed in the operating room. The type of SLAP injury was classified by MRI at the pre-oper-ative stage in 40 cases (63.49%). Of these 40 cases, 65.7% were SLAP type II, followed by 24.8% SLAP type III, 7.5% type I and 2% types IV and V. Cysts were described in nine cases (14.28%), but these compressed the suprascapular nerve in only six cases (9.5%) (Figure 1). There were eight more cases where SLAP injuries were classified into two types. For this reason we considered these cases as suspicious SLAP injuries but we did not conclude which types they were.
Regarding rotator cuff injuries, in the pre-operative imaging study (ultrasound and MRI) a cuff with no pathological findings was observed in 55% of cases; tendinitis in 30%; partial rupture in 18%; and complete rupture in 12%. A Bankart lesion was found in 19% of all cases, while a Hill-Sachs injury was present in 23%. There were two cases with a history of fracture of the greater tubercle of the humerus and SLAP, and two more cases with previous injury to the acromioclavicular joint, namely associated acromioclavicu-lar arthrosis and a case of previous fracture of the glenoid without displacement, but with SLAP found.
Clinically, during pre-operative examination, we found that 82% had positive signs in the rotator cuff and sub-acromial space, particularly as far as the signs of Yochum, Neer and Hawkins were concerned. Bicipital stress tests using Ludington and Yegarson's tests were positive in 29% of cases, whereas manoeuvres to assess antero-inferi-or instability, such as apprehension manoeuvre, were positive in 43% of cases. Finally, the O'Brien test to assess the superior labral lesions was positive in 61% of patients in our series.
Other specific tests utilised to identify SLAP lesions clinically, such as the Crank test, pretension test or active compression test were not done. In this article we have considered only the O'Brien test.
We also analysed the following background data: age, sex, right or left side, and profession. In the images (X-ray, MRI) we identified the types of SLAP lesion, and the presence of associated lesions such as labral cysts, rotator cuff lesions, Bankart lesions or Hill-Sachs lesions. We have to point out that today MR Arthrography is much better in diagnostic accuracy for labrum tears or SLAP lesions. However, in this research we studied all patients with MRI. We made the diagnosis using clinical examination and MRI. Only when diagnosis was unclear and we suspected this after clinical examination, did we use an arthrogram. We consider contrast injection to be risky, and if we can avoid it we do not submit patients to this complementary test.
We selected all patients who had shoulder pain that prevented them from doing their previous highly demanding jobs. We explored them by analysing the O'Brien sign and hyperabduction injury mechanism and we performed an MRI study. If we suspected SLAP lesion, we operated on the patient by means of arthroscopy.
With regard to the operation, we recorded the operation time, mean length of hospital stay, length of physiotherapy, surgical findings, techniques and procedures, and the number of anchors used. We also noted complications and final results, time before discharge and any disabilities. We carried out an evaluation using the Rowe, Constant and UCLA scales at the end of clinical follow-up, which was continued for at least one year.
The data was analysed using the statistical package SPSS version 15.0. The analysis was basically descriptive, with quantitative variables expressed in means and typical deviations. However, to see the relationship between the numerical variables on the tests before surgery and at the last check-up, after at least one year of follow-up, we used the non-parametric marginal homogeneity test. Only the final results in each of the tests with means and standard deviations were used, since the differences from the pre-operative values, although significant, were not at a level of p<0.05.
Results
Surgery was carried out on 63 of the 63 patients (100%). The other seven patients from the initial sample of 70 patients were lost to follow-up. For this reason, although we started our study with 70 patients, we considered only 63 patients with completed follow-up. The operating time was 85 minutes (SD: 30), and the mean hospital stay was one day (63.2% stayed one day; 34.2% stayed two days and 2.6% for three days), and the length of physiotherapy was four months (SD: 1) - four months being the period applied in 64.1% of the patients who had undergone surgery.
Our rehabilitation plan entailed the following: After surgery we allowed only pendular passive movements from the first to the third week. Patients kept a sling on for the rest of the day. From the third to the sixth week we proceeded with passive assisted exercises. Patients kept the sling on only at night. From the sixth to the ninth week we began with active exercises. From the ninth week a strengthening period commenced.
Among the surgical findings the presence of a SLAP lesion was confirmed in all cases, that is, in 40% more than in pre-operative MRI. Type II was predominant (59.5%), followed by type I (23.4%), type III (16.1%) and type IV (1%); no cases of type V were encountered (Figure 2).

Of the 63 patients who underwent surgery, the rotator cuff was unaffected in 43.2% of cases, whereas tendinitis was found in 37.4%, partial rupture in 6.9% and complete rupture in 14%. A Bankart lesion was detected in 15% of those operated on, while a Hill-Sachs lesion was found in 29.3%. We found a discrepancy between operative and MRI findings.
Procedures that were most widely used were debride-ment of the lesions in all cases; thermocoagulation with arthroscopic vaporiser in 89.7%; subacromial decompression in 43.5%; repair of the rotator cuff in 26.4%; tenotomy of the long part of the biceps in 4%; and labral reinsertion in up to 82% of cases.
The number of bioabsorbable knotless anchors used was one in 60.2% of patients; two in 37.2%; and three in 2.6% of patients subjected to arthroscopy. We used bioabsorbable BioKnotless BR, DePuy Mitek's anchors (Figures 3,4 and 5).
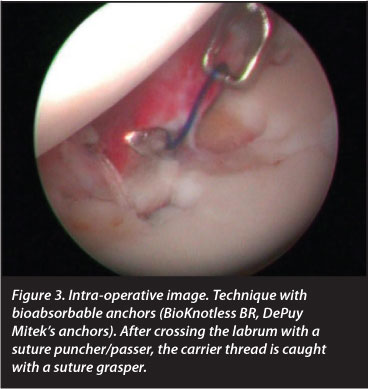
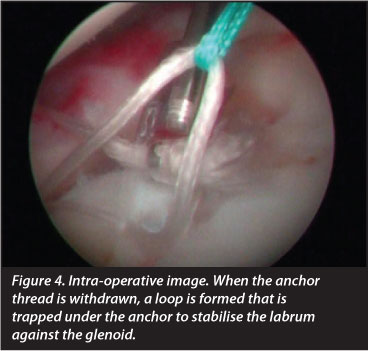
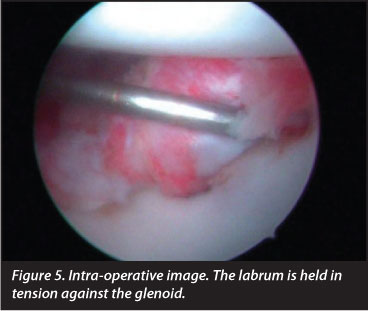
As far as complications are concerned, we found no infections but we observed that implants moved in 15.2% of cases (we performed post-operative MRI to determine this), while tendinopathies occurred in the long part of the biceps in 5.9% of patients; anchors protruded in the glenoid causing residual shoulder discomfort in 8%; failure of the SLAP repair in 7.5%; complex regional pain in 3%; paraesthesia in the area of the median nerve and ulnar nerve in 4%; subluxation in 4%; and a second rupture of the rotator cuff in 5%. Seven cases required a second operation (15.87%) because of persistent shoulder pain. Shoulder pain after surgery could appear after SLAP lesions repair. In this regard shoulder pain at pitching could be due to reinsertion. Shoulder pain post-SLAP repair may be due to over-tensioning the repair. Thus tension in repair may be a source of pain when pitching after SLAP repair.
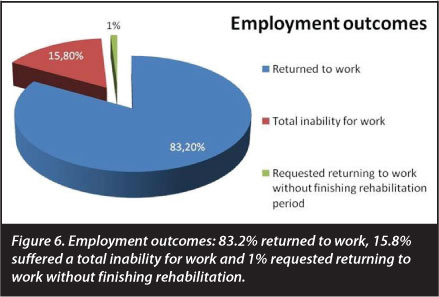
A total of 83.2% of patients returned to work, 15.8% suffered a total inability for work and 1% requested returning to work without finishing rehabilitation (Figure 6). Patients who suffered total inability for work were patients with great stiffness and pain. They had worked previously in high physically demanding jobs.
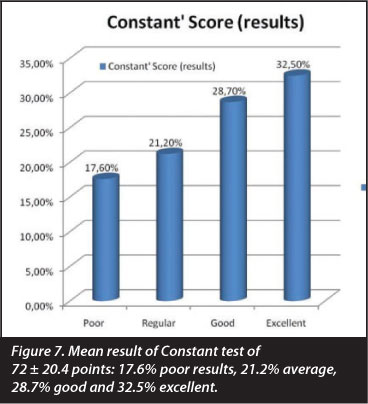
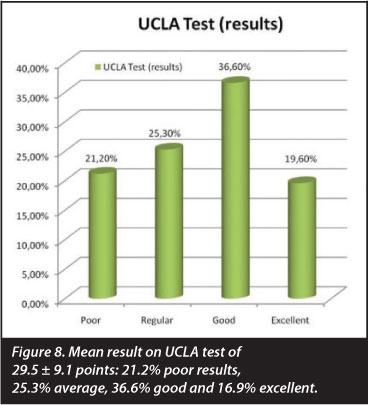
We analysed the results of Rowe's test, Constant's test and the UCLA test. A pre-operative Rowe's test yielded a mean result of 78.1 ± 9 points; the Constant test 61.3 ± 8.3 points;and the UCLA test, 22.8 ± 4.2 points. For the post-operative results Rowe's test yielded a mean result of 84.5 ± 18.3 points; the Constant test 72 ± 20.4 points and the UCLA test 29.5 ± 9.1 points: these were the final results at the end of clinical follow-up for a minimum of 12 months after surgery (Figures 7 and 8). These results illustrate an overall improvement from the pre-opera-tive state, although this improvement is not statistically significant.
Discussion
According to Higgins8 advances in shoulder arthroscopy have made it possible to classify and treat SLAP lesions. Thus in type I (11%)9 the degeneration of the labral region predominates; type II (41-78%) is characterised by a tear of the labrum and the biceps in the superior region of the gle-noid cavity; type III (33-37%) presents a bucket-handle tear only in the superior portion of the labrum in contrast to type IV (5%), in which the tear extends into the biceps. Jin2 found that type II accounted for 41-55% of cases. An intra-observ-er diagnostic variability is found among surgeons of k=0.54 (p<0.001) as reported by Gobezie.10 In our experience MRI enabled us to diagnose a SLAP lesion in 76.19% of patients, and this diagnosis was then confirmed in 100% of the patients in the present series. All this leads us to think that these lesions are probably more frequent than is usually acknowledged, and that they may well often pass unnoticed. The presence of such an injury should be suspected as an aetiological factor in many types of shoulder pain.
Nonetheless, in Maffet's4 view, up to 38% of cases cannot be classified into the four groups described above, and there may be up to ten different types of SLAP lesion. In our experience type II was the most frequent kind (59.5%), followed by type I (23.4%).
Falls with the arm in hyperabduction account for 23-27% of the mechanisms by which the injury is caused,4 while traction of the limb is the cause in 16-25%, and 19% of subluxations may have an underlying SLAP lesion. In fact, inferior subluxation would tend to lead to a type II lesion. The sport most frequently mentioned is rugby (67.8 men injured per 1 000 hours of rugby played5). In our series, over 43% of patients presented episodes of fall in hyperabduction as the mechanism of injury.
SLAP lesions have been associated with injury to the rotator cuff in up to 2.5%11 of cases, a figure which Parentis1 believes to be 10-48% and Jones12 considers to be as high as 77%. They are associated with a Bankart lesion in 17- 22%13 (in our series this was found in 19% of cases in the preoperative study and in up to 15% intra-operatively); with posterior labral lesions in 11%; with labral cysts in 89%14 (in our experience these were present in 14.28%); and with a Buford complex in 83.3% (p<0.003)15 or glenohumeral instability in general (we found a 29.3% frequency of Hill-Sachs lesions). In this context Mihata16 showed that the creation of a SLAP type II lesion in cadavers leads to an anterior glenohumeral translation of 0.6 mm. Only 28% cases are isolated SLAP lesions. Additional factors like rotator cuff tears complicated the final outcome by causing patients to take more time to return to work and a longer rehabilitation period.
Several shoulder lesions have been associated with different SLAP types. Type I lesions appear frequently with injuries to the supraspinatus, with a statistically significant relationship, p=0.012; type II lesions in persons under 40 years of age are associated with Bankart lesions; while those in patients over 40 years are associated with omarthrosis and tears in the supraspinatus. Finally, type III-IV injuries are associated with Bankart17 lesions.
During examination the signs of Kibler, Kim and O'Brien18 yielded a specific diagnosis in 91.5%, 96.9% and 98.5% of cases respectively.1 In our series the O'Brien test was positive pre-operatively in 61% of patients. The diagnosis was then completed by using arthrographic resonance (ArthroMRI)19 with a sensitivity of 89%, specificity of 91% and precision of 90% in the diagnosis of SLAP lesions.20 All our patients had MRI before surgery. An increase in the signal and width between the glenoid edge and superior labrum greater than 2.5 mm had a specificity of 85% for the diagnosis of SLAP lesions.21
For type I lesions Higgins recommends arthroscopic debridement; for type II repair with absorbable anchors is indicated, since debridement alone, in Verma's series, yielded good results in only 37% of cases.22 For type III, arthro-scopic excision of the bucket-handle would be the most appropriate treatment, although if the tear is greater than 50% of the diameter of the labrum, it could be repaired. Finally, for type IV, if injury extends across less than half the length of the bicipital tendon, it should usually be debrided, but if it exceeds 50%, tenodesis is required. The intra-observer variability is k=0.45.10 Arthroscopic treatment brought about an improvement on the DASH test in 73% of cases of SLAP with associated injuries, as reported by Lim.23
Yung24 shows that arthroscopic repair of type II lesions brought about a statistically significant improvement on the UCLA test (p<0.05) in 9.4 months. It is noteworthy that these improvements have been reported in athletes. We think that we can compare this level of physical requirement with jobs like farm work, building construction workers and firemen in our series. We feel that the level of intensity of physical work is equivalent to that of a sportsman.
Neuman25 recently studied 30 shot-putters with SLAP-type labral lesions treated surgically, and found that 84.1% of them returned to the level of sporting activity that they had had prior to surgery in 11.7 months. In fact, they attained 87.9 ± 14.94 points on the ASES scale, with p=0.006. Their degree of satisfaction was around 93.3%. Kanatli26 reports improvements on the UCLA scale: his subjects had a mean of 31.2 points in comparison with 11.8 points before surgery (p<0.01). In our study the mean result was 29.5 ± 9.1 points, which is somewhat lower than the studies cited above.
However, authors such as Katz27 acknowledge that the result of surgical treatment is not always that satisfactory, reporting 32% of poor results after surgery, with up to 9-55% of patients who fail to return to their previous level of sports activity and up to 75% with pain and limitation in the range of movements they can make.
From a technical point of view Oh28 states that arthroscop-ic entry through the rotator cuff is safe and effective, yielding statistically significant clinical improvements (p<0.001).
In our series the O'Brien test was positive pre-operatively in 61% of patients. The diagnosis was then completed by using arthrographic resonance
However, Cohen29 does not recommend access through the rotator cuff, since the results on the ASES scale average 95.6 points, compared with 86.9 points when the rotator interval is used. Kaisidis30 recommends approaching this injury via two portals, and states that his patients showed an improvement on the Constant test in 86.4% of cases. In SLAP lesions associated with a tear of the rotator cuff, if the patient is aged over 50 years, Franceschi31 says that the results are better with repair of the cuff and bicipital tenotomy rather than repair of the cuff and the SLAP lesion (Test UCLA 32.1 points versus 27.9 points, p<0.05). Forsythe32 acknowledges that in patients over 55 years of age, treatment of the SLAP lesion and concomitant rotator cuff tear brings about an improvement ranging from 22.6 to 96.4 points on the ASES scale. However, in the group in which only the cuff was repaired, the range was from 34.3 to 92.3 points. Although there were no significant differences, the results seem to have been somewhat better when the labral lesion was also repaired.
Along similar lines, treatment of the SLAP lesion could affect the patient's recovery from paralabral cysts14 (present in 14.28% of cases in our series), with improvements in cases with compression of the suprascapular nerve (Rowe test from 61.5 to 98 points). In Morgan's33 view, the insertion of anchors posterior to the biceps in repair of SLAP lesions means that the forces of load are more bearable by the upper sutures than when they are in front of or behind the tendon (162.06 N versus 156.28 N). In our cases we used absorbable anchors, which do not require knots; from one to three anchors were used in each case.
Knotless bioabsorbable anchors were used in instability of the shoulder by authors such as Cooke34 with favourable results on the Constant test, and results similar to those obtained in the contralateral arm in 85% ± 7.7% of cases. In fact, 15 out of 20 patients had results on the Constant test greater than 75 points, with only 10% with recurrence of luxation. These anchors, which were used in our series, conserve the strength of the repair in 90% of cases 2 months after surgery, and in 60% after 6 months. Complete absorption occurs after around 4 years.
Oh35 also recommends the use of absorbable anchors in his series of 97 patients operated on for labral lesions, including SLAP injuries. He brought about an improvement on the Rowe test from 68.7 to 92.7 points, and on the Constant test from 79.1 to 96.8 points; and 83.3% of patients were able to take up sport again. Knotless anchors are also recommended by Yian.36 However, Sileo37 recognises that anchors with knots will bear more tension than those without (74 N versus 132 N; P=.043) although the differences are not statistically significant.
It must be explained that although this is a surgical series, we usually treat more patients with SLAP lesions without surgery with good results. All patients we operated on in this study were those who did not improve sufficiently to go back to their previous jobs after non-operative/rehabilitation treatment.
In conclusion, SLAP lesions are a major cause of shoulder pain in the workplace but they are often not properly diagnosed. Early diagnosis by examination, confirmed by MRI, and followed by treatment using the latest shoulder arthroscopy techniques, has enabled many patients who have had continual shoulder pain to return to work. It is important to look for any concomitant injuries that accompany SLAP lesions in order to optimise the results of surgery. The use of knotless absorbable anchors has greatly improved treatment, since it reduces the surgical time and yields good clinical results.
The authors have not received any financial aid in order to carry out this study. Nor have we signed any agreement by which we are likely to receive any profit or fee from any commercial entity. No commercial entity has paid any foundation, educational institution or other non-profit-making organisation to which we are affiliated, nor is any such payment going to be made.
References
1. Parentis MA, Mohr KJ, ElAttrache NS. Disorders of the superior labrum: review and treatment guidelines. Clin Orthop Relat Res. 2002 Jul; (400): 77-87. [ Links ]
2. Jin W, Ryu KN, Kwon SH, Rhee YG, Yang DM. MR arthrography in the differential diagnosis of type II superior labral anteroposterior lesion and sub-labral recess. AJR Am J Roentgenol. 2006 Oct; 187(4): 887-93. [ Links ]
3. Snyder SJ, Banas MP, Karzel RP. An analysis of 140 injuries to the superior glenoid labrum. J Shoulder Elbow Surg. 1995 Jul-Aug; 4(4): 243-8. [ Links ]
4. Maffet MW, Gartsman GM, Moseley B. Superior labrum-biceps tendon complex lesions of the shoulder. Am J Sports Med. 1995 Jan-Feb; 23(1): 93-8. [ Links ]
5. Funk L, Snow M. SLAP tears of the glenoid labrum in contact athletes. Clin J Sport Med. 2007 Jan; 17(1): 1-4. [ Links ]
6. Andrews JR Carson WG Jr., McLeod WD. Glenoid labrum tears related to the long head of the biceps. Am J Sports Med. 1985 Sep-Oct; 13(5): 337-41. [ Links ]
7. Snyder SJ, Karzel RP, Del Pizzo W, Ferkel RD, Friedman MJ. SLAP lesions of the shoulder. Arthroscopy. 1990; 6(4): 274-9 . [ Links ]
8. Higgins LD, Warner JJ. Superior labral lesions: anatomy, pathology, and treatment. Clin Orthop Relat Res. 2001 Sep; (390): 73-82. [ Links ]
9. Nam EK, Snyder SJ. The diagnosis and treatment of superior labrum, anterior and posterior (SLAP) lesions. Am J Sports Med. 2003 Sep-Oct; 31(5): 798-810. [ Links ]
10. Gobezie R, Zurakowski D, Lavery K, Millett PJ, Cole BJ, Warner JJ. Analysis of interobserver and intraobserver variability in the diagnosis and treatment of SLAP tears using the Snyder classification. Am J Sports Med. 2008 Jul; 36(7): 1373-9. [ Links ]
11. Gartsman GM, Taverna E. The incidence of glenohumeral joint abnormalities associated with full-thickness, reparable rotator cuff tears. Arthroscopy. 1997 Aug; 13(4): 450-5 . [ Links ]
12. Jones GL, Galluch DB. Clinical assessment of superior glenoid labral lesions: a systematic review. Clin Orthop Relat Res. 2007 Feb; 455: 45-51 . [ Links ]
13. D'Alessandro DF, Fleischli JE, Connor PM. Superior Labral Lesions: Diagnosis and Management. J Athl Train. 2000 Jul; 35(3): 286-292. [ Links ]
14. Schroder CP, Skare O, Stiris M, Gjengedal E, Uppheim G, Brox JI. Treatment of labral tears with associated spinoglenoid cysts without cyst decompression. J Bone Joint Surg Am. 2008 Mar; 90(3): 523-30 . [ Links ]
15. Bents RT, Skeete KD. The correlation of the Buford complex and SLAP lesions. J Shoulder Elbow Surg. 2005 Nov-Dec; 14(6): 565-9. [ Links ]
16. Mihata T, McGarry MH, Tibone JE, Fitzpatrick MJ, Kinoshita M, Lee TQ. Biomechanical assessment of Type II superior labral anterior-posterior (SLAP) lesions associated with anterior shoulder capsular laxity as seen in throwers: a cadaveric study. Am J Sports Med. 2008 Aug; 36(8): 1604-10. [ Links ]
17. Kim TK, Queale WS, Cosgarea AJ, McFarland EG. Clinical features of the different types of SLAP lesions: an analysis of one hundred and thirty-nine cases. J Bone Joint Surg Am. 2003 Jan; 85-A(1): 66-71. [ Links ]
18. Green RA, Taylor NF, Mirkovic M, Perrott M. An evaluation of the anatomic basis of the O'Brien active compression test for superior labral anterior and posterior (SLAP) lesions. J Shoulder Elbow Surg. 2008 Jan-Feb; 17(1): 16^71. [ Links ]
19. Woertler K, Waldt S. MR imaging in sports-related glenohumeral instability. Eur Radiol. 2006 Dec; 16(12): 2622-36. [ Links ]
20. Bencardino JT, Beltran J, Rosenberg ZS, Rokito A, Schmahmann S, Mota J et al. Mellado JM Zuckerman J Cuomo F Rose D. Superior labrum anterior-posterior lesions: diagnosis with MR arthrography of the shoulder. Radiology. 2000 Jan; 214 (1): 267-71. [ Links ]
21. Tuite MJ, Rutkowski A, Enright T, Kaplan L, Fine JP, Orwin J. Width of high signal and extension posterior to biceps tendon as signs of superior labrum anterior to posterior tears on MRI and MR arthrography. AJR Am J Roentgenol. 2005 Dec; 185(6): 1422-8. [ Links ]
22. Verma NN, Garretson R, Romeo AA. Outcome of Arthroscopic Repair of Type II SLAP Lesions in Worker's Compensation Patients. HSS J. 2007 Feb; 3(1): 58-62. [ Links ]
23. Lim MH, Chan BK, Low CO. Arthroscopic management of superior labral anterior and posterior (SLAP) and associated lesions: clinical features and functional outcome. Ann Acad Med Singapore. 2008 Jan; 37(1): 44-8. [ Links ]
24. Yung PS, Fong DT, Kong MF, Lo CK, Fung KY, Ho EP et al. Arthroscopic repair of isolated type II superior labrum anterior-posterior lesion. Knee Surg Sports Traumatol Arthrosc. 2008 Dec; 16(12): 1151-7. [ Links ]
25. Neuman BJ, Boisvert CB, Reiter B, Lawson K, Ciccotti MG, Cohen SB. Results of Arthroscopic Repair of Type II Superior Labral Anterior Posterior Lesions in Overhead Athletes: Assessment of Return to Preinjury Playing Level and Satisfaction. Am J Sports Med. 2011 Jul 7. [ Links ]
26. Kanatli U, Ozturk BY, Bolukbasi S. Arthroscopic repair of type II superior labrum anterior posterior (SLAP) lesions in patients over the age of 45 years: a prospective study. Arch Orthop Trauma Surg. 2011 Jun 26 . [ Links ]
27. Katz LM, Hsu S, Miller SL, Richmond JC, Ketia E, Kohli N, et al. Poor outcomes after SLAP repair: descriptive analysis and prognosis. Arthroscopy. 2009 Aug; 25(8): 849-55. [ Links ]
28. Oh JH, Kim SH, Lee HK, Jo KH, Bae KJ. Trans-rotator cuff portal is safe for arthroscopic superior labral anterior and posterior lesion repair: clinical and radiological analysis of 58 SLAP lesions. Am J Sports Med. 2008 Oct; 36(10): 1913-21. [ Links ]
29. Cohen DB, Coleman S, Drakos MC, Allen AA, O'Brien SJ, Altchek DW, et al. Outcomes of isolated type II SLAP lesions treated with arthroscopic fixation using a bioabsorbable tack. Arthroscopy. 2006 Feb; 22(2): 136-42. [ Links ]
30. Kaisidis A, Pantos P, Heger H, Bochlos D. Arthroscopic fixation of isolated type II SLAP lesions using a two-portal technique. Acta Orthop Belg. 2011 Apr; 77(2): 160-6. [ Links ]
31. Franceschi F, Longo UG, Ruzzini L, Rizzello G, Maffulli N, Denaro V. No advantages in repairing a type II superior labrum anterior and posterior (SLAP) lesion when associated with rotator cuff repair in patients over age 50:
a randomized controlled trial. Am J Sports Med. 2008 Feb; 36(2): 247-53.
32. Forsythe B, Martin SD. Concomitant arthroscopic SLAP and rotator cuff repair: surgical technique. J Bone Joint Surg Am. 2011 Mar; 93 Suppl. 1:1-9. [ Links ]
33. Morgan RJ, Kuremsky MA, Peindl RD, Fleischli JE. A biomechanical comparison of two suture anchor configurations for the repair of type II SLAP lesions subjected to a peel-back mechanism of failure. Arthroscopy. 2008 Apr; 24(4): 383-8. [ Links ]
34. Cooke S, Ennis O, Majeed H, Rahmatalla A, Kathuria V, Wade R. Clinical results and motion analysis following arthroscopic anterior stabilization of the shoulder using bioknotless anchors. Int J Shoulder Surg 2010; 4: 36-40. [ Links ]
35. Oh JH, Lee HK, Kim JY, Kim SH, Gong HS. Clinical and radiologic outcomes of arthroscopic glenoid labrum repair with the BioKnotless suture anchor. Am J Sports Med. 2009 Dec; 37(12): 2340-8. [ Links ]
36. Yian E, Wang C, Millett PJ, Warner JJ. Arthroscopic repair of SLAP lesions with a bioknotless suture anchor. Arthroscopy. 2004 May; 20(5): 547-51. [ Links ]
37. Sileo MJ, Lee SJ, Kremenic IJ, Orishimo K, Ben-Avi S, McHugh M, et al. Biomechanical comparison of a knotless suture anchor with standard suture anchor in the repair of type II SLAP tears. Arthroscopy. 2009 Apr; 25(4): 34854. [ Links ]
 Reprint requests:
Reprint requests:
Reprint requests:
Dr Antonio Jiménez-Martín
Hospital FREMAP Sevilla Avda. de Jerez s/n CP 41012
Sevilla Spain
Email: antonio_jimenez10@hotmail.com
Ethics Committee approval: This study received a favourable evaluation from the Ethics Committee of the Hospital FREMAP Sevilla.














