Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SA Orthopaedic Journal
On-line version ISSN 2309-8309
Print version ISSN 1681-150X
SA orthop. j. vol.12 n.2 Centurion Jan. 2013
PAEDIATRICS
An assessment of the three-point index in predicting the redisplacement of distal radial fractures in children
DA ChiversI; TL HiltonII; SI Dix-PeekIII
IMBChB(Wits) Red Cross Children's Hospital and Maitland Cottage Paediatric Orthopaedic Hospital, Department of Orthopaedics, University of Cape Town
IIMBChB(UCT) DA(SA), DipPEC(SA) Red Cross Children's Hospital and Maitland Cottage Paediatric Orthopaedic Hospital, Department of Orthopaedics, University of Cape Town
IIIMBChB, FCS(SA)Orth, Head of Paediatric Orthopaedics Red Cross Children's Hospital and Maitland Cottage Paediatric Orthopaedic Hospital, Department of Orthopaedics, University of Cape Town
ABSTRACT
BACKGROUND: Distal metaphyseal radial fractures are common in the paediatric population and their management is predominantly conservative. The incidence of redisplacement of these fractures is high and various methods have been described with the view to predict fracture redisplacement. One of these indices is the three-point index (TPI).
METHODS: A retrospective review of 43 patients with distal radius fractures revealed that 19 patients suffered significant redis-placement at 2 weeks after closed manipulation in a plaster cast.
RESULTS: The TPI index in the study was found to have a sensitivity of 84%, a specificity of 37%, a negative predictive value of 75% and a positive predictive value of 51%.:
CONCLUSIONS: It was concluded that the TPI was a sensitive but not specific measure of fracture redisplacement and not practically applicable to influence management of these fractures and therefore not a useful tool in our clinical setting.
Key words: paediatric, fracture, forearm, distal radius, redisplacement, three-point index
Introduction
Distal metaphyseal radial fractures are very common in the paediatric population1,2 and many of these fractures are managed conservatively by reducing the fracture and applying a plaster cast for immobilisation.3 Due to various extrinsic and intrinsic factors this conservative management runs the risk of the fracture re-displacing within the plaster cast.4,5 There have been a number of radiological indices that have been developed to differentiate between the well and poorly applied plaster casts and to assess the quality of moulding, in order to predict fracture redisplacement in plaster casts.6 However the accuracy and clinical value of these indices are questionable. Some of these indices include the cast, padding, Canterbury and three-point index (TPI) (Figure 1).
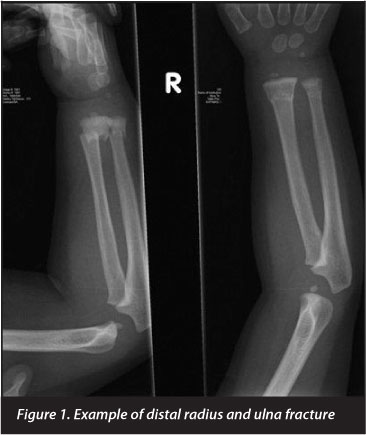
Due to various extrinsic and intrinsic factors this conservative management runs the risk of the fracture re-displacing within the plaster cast
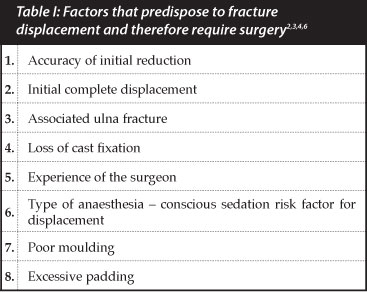
Although the remodelling potential of these fractures is well recognised, up to 30% of these fractures exhibit significant redisplacement requiring further treatment.6 In order to avoid the morbidity of re-manipulation, attempts have been made to identify various factors that serve to predict which fractures will redisplace and therefore should be surgically stabilised. The purpose of this study was to assess the accuracy of the TPI in predicting redis-placement of distal radial fractures in children (Table I).
Rationale behind the TPI
The TPI was originally designed according to the basic principles of cast treatment: three-point fixation and reduction accuracy in terms of the contact area of the fragments in the fracture site3(Figure 2).
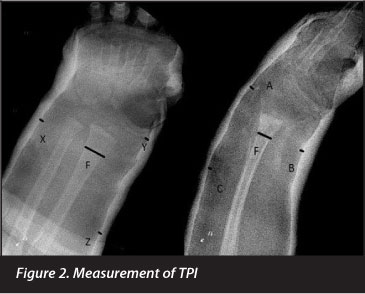
The critical gaps were selected on the basis of the most important points in the cast that maintain the reduction against the common displacement forces. On an AP radiograph, 'Y' should be the narrowest radial-side gap between the cast and the skin around the radiocarpal joint or at the level of the scaphoid bone; 'X' should be the narrowest ulna-side gap between the cast and the skin within 1 cm of the fracture line; and 'Z' should be the narrowest radial-side gap about 3-5 cm proximal to the fracture site.3
On a lateral view, 'A' should be the narrowest dorsal-side gap between the cast and the skin around the radio-carpal joint or the proximal carpal row; 'B' should be the narrowest volar-side gap between the cast and the skin within 1 cm of the fracture line; and 'C' should be the narrowest dorsal-side gap about 3-5 cm proximal to the fracture site.3
Dividing the sums by the contact length of the fracture fragments in each plane provides proportionality for the index, which prevents measurement errors due to magnification of the plain radiographs3(Table II).
Methods
A retrospective review of 65 patients of both sexes under the age of 13 years for a period of one year from January 2011 to January 2012 was conducted. Only dorsally angu-lated or translated fractures were included in the study. Patients that had compound injuries or physeal injuries were not included. Twenty-two patients were excluded because of loss to follow-up or absence of a complete series of X-rays, leaving 43 patients for this analysis.
All patients that were involved in the study had their fractures reduced in theatre by an orthopaedic registrar under general anaesthesia. An above-elbow plaster cast was applied in stages with appropriate moulding of the plaster. The forearm was placed in neutral alignment. An image intensifier was used to confirm the reduction. Patients that went to theatre were observed post-opera-tively for any neurovascular complications before discharge. All post-reduction X-rays and plasters were reviewed by an orthopaedic consultant.
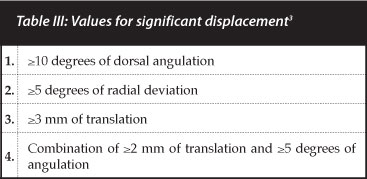
Follow-up X-rays were done at 2 weeks and 6 weeks. If significant displacement was noted at the 2-week interval, patients were re-admitted for remanipulation in theatre. Significant displacement was defined as: >10 degrees of dorsal angulation; >5 degrees of radial deviation; >3 mm of translation; or a combination of >2 mm of translation and >5 degrees of angulation. These were the criteria described by Alemdaroglu in his original article3(Table III).
The TPI was measured on the initial post-reduction X-ray taken in theatre by the image intensifier. All TPI results, 2- and 6-week measurements were tabulated and analysed using the Shapiro-Wilk statistical test to determine normality of the data. Statistical analyses were performed using Stata version 12.1(Statacorp LP, 4905 Lakeway Drive, College Station, TX 77845, USA) using p<0.05 to determine statistical significance.
Results
The initial sample group included 65 patients, all with dorsally angulated or translated distal radius fractures. Twenty-two patients were excluded due to a loss of follow-up or were excluded due to an incomplete series of X-rays. The final number of patients in the study was 43.
The fracture was assessed as either being dorsally angulated or translated. Most of the patients had fractures that were translated dorsally at 62% (27 of 43 patients). The rest at 38% (16 of 43 patients) were dorsally angulated. The average dorsal angulation was measured at 24 degrees (range 10-10 degrees). Seventy-two per cent of the patients had ipsilateral radius and ulna fractures. The least common fracture configuration was an isolated translated radius fracture.
Of the total number of patients (43), 19 (44%) had significant redisplacement at 2 weeks. Not all the significantly redisplaced fractures were remanipulated. Of the 19 patients only five were taken back to theatre for remanip-ulation of their fractures. Of these five, one patient's fracture was deemed too unstable to be placed in plaster alone and was fixed surgically (Table IV).
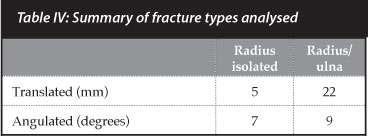
Anatomical reduction was achieved in 93% of the patients. The mean TPI in the series was 1.08 (range 0.45 to 2.2). Thirty-one of the 43 patients had a TPI greater than 0.8 (72%). Of the 31 patients that had a poor TPI, 16 (52%) significantly redisplaced at the 2-week follow-up. Of the 12 patients that had a good TPI, three (25%) redisplaced.
Of the five patients that were remanipulated in theatre due to significant displacement, the average post-manipulation TPI was 0.79 (range 0.73-0.9). None of the remanip-ulated fractures displaced at their 2- or 6-week follow-up.
When looking at the sensitivity and specificity the Receiver Operator Characteristic curve (ROC) was plotted showing their relationship; the area under the curve was calculated at 70.72 (Figure 3).
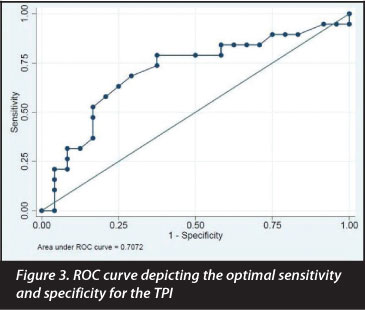
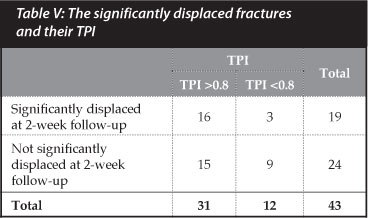
The sensitivity of the TPI is 84% (60.4-96.6) and the specificity is 37% (18.8-59.4). The TPI had a positive predictive value of 51% (33.1-69.8) and negative predictive value of 75% (42.8-94.5) (Table V).
Discussion
Distal radial fractures in children are common and the majority are treated conservatively by closed manipulation and plaster casting with the type of plaster cast (i.e., above vs below elbow casts) not influencing the risk of dis-placement.1-3-7-8 The reasons for this are to avoid the morbidity of surgery and the remodelling potential of a child's metaphysis is great.3 However the maintenance of anatomical alignment, which is essential for a good func-tional1 and cosmetic outcome, is difficult in some fractures. The result may be that the fracture redisplaces, malunites and has a poor functional outcome.2,9 Previously a poor functional outcome was thought not to happen;1 however, recent studies have concluded that even temporary restriction in movement and an abnormal appearance is unsatisfactory for both children and their parents.9 It is these unstable fractures that require identification and more aggressive treatment with surgery and K-wire fixation.7,9,10
That being said surgery carries with it its own set of problems which include pin tract sepsis, hypertrophic scarring and neuropraxia.9 The dilemma for the surgeon lies in deciding which fractures to manage conservatively and which to fix surgically. The literature is full of ways in which to try and predict which fractures will need surgery and which will not - factors such as fracture pattern, displacement, associated fractures and, of course, plaster indices.2-4,7,10,11
The TPI has been purported to have considerably greater sensitivity, specificity, and positive and negative predictive values compared with other radiographic methods of determining poor casting and/or moulding technique.3 The reason suggested for it being a good measure is that it is based on the three-point fixation principle, reduction accuracy at the fracture site as well as taking into consideration the proximal and distal ends of cast fixation.3
Our interest in the TPI was to confirm its accuracy and to decide how it could influence our management of distal radius fractures. In order to ensure that our study would be comparable to the one in which the TPI was first described, we made sure that the distal radial fractures included in our study were managed in a similar way. There were some slight differences however and we feel that these could only add strength to the study. One of these differences was the fact that the patients underwent a general anaesthetic for the manipulation of their fractures while the previous study used conscious sedation. Type of sedation has been said to be a factor resulting in redisplacement of distal radius fractures after conservative treatment.4,12
Only angulated and displaced fractures were included to ensure that no intrinsic stability of the fracture itself could influence the chance of redisplacement.4 All of the patients were under the age of 13 years and were treated within 24 hours of presenting to our hospital. Lastly we ensured that a high percentage of fractures were anatomically reduced after manipulation, which is an important prerequisite for prevention of redisplacement using conservative treatment.1
Once we were satisfied we were analysing a comparable group of patients we looked at the practicality of measuring the TPI. In our setting both printed films and digital images were available for analysis. Any measurements taken on a digital format were to the nearest millimetre and so there was no difference between measurements taken this way and those taken with a standard goniometer. What we did feel to be an issue was deciding where the plaster ended and the skin began. In some circumstances the difference was clear but in others, due to overlapping plaster, it proved difficult. This must be highlighted as a limitation to our study and the measurement of the TPI, despite a contrasting difference to the original authors' description of excellent inter-and intra-observer reliability in reproducing accurate measurements using the TPI.3
Having performed a retrospective study, there was no education about the TPI or increased attention to ensuring meticulous plaster technique prior to registrars in the unit treating these fractures. This is important as casting indices as a whole have been designed in order to assess the quality of plaster application which in itself is a predictor of fracture redisplacement.6 We feel that this is a strength of the study as it would allow for the TPI to be truly tested. We wished to accurately assess without any form of bias the ability of the TPI to assess proficiency of plaster moulding and hence predict fractures that will redisplace based on poor moulding technique.6 From our results we have concluded that this is not the case. There must therefore have been another reason for those plasters with an acceptable TPI to have displaced, and vice versa.
A possible failing of our study could be the relatively small number of patients that were included. Although the initial number of distal radial fractures in the time period we specified was high we wanted to ensure that the study group included only those for which the TPI was designed.
We also found it impractical to measure the index when it mattered most, i.e. in theatre. If the index were to be too large one still has the opportunity to redo the plaster in theatre, improve the index and ensure a plaster that will hold the fracture in position for the duration of treatment. Practically though many of these cases are performed after-hours where transfer to a digital format or printing of the X-rays for measurement is impractical, not to mention time-consuming when the patient is still under anaesthesia. On the image from the intensifier it was felt that the image was not clear enough to accurately take measurements. This is a limitation in this study and in the use of the TPI in our setting as the index depends entirely on the accurate measurement of the points between skin and plaster.
We found it impractical to measure the index when it mattered most, i.e. in theatre
Our study showed that the TPI is sensitive and specific for identifying those fractures that may displace based on casting technique and moulding; however, the current numbers are not as high as previously reported.3 In our clinical setting the TPI was measured on images taken in theatre by an image intensifier. Although the values for the index were not practically available on the image intensifier, the images were transferred to a digital format where measurements were taken. This meant that they were measured only after the patient had returned from theatre. The next question should be what should be done if the TPI was greater than the recommended value? Although none of our patients were re-manipulated based on an inadequate TPI, the question still remains what to do if the TPI value is greater than 0.8. For indices such as the TPI to be adopted into clinical practice they must have a decision-making power and be practically applicable. Our conclusion is that although the TPI is based on solid principles of three-point fixation and anatomical reduction, we did not find it sensitive or specific enough to base clinical decisions on. In fact the numbers we generated were similar to the numbers reported in the literature for other casting indices (Table VI).
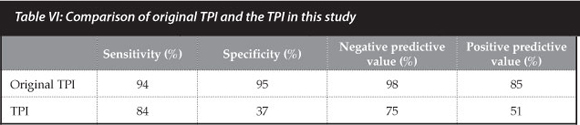
What is important in this type of fracture is determining which fractures are more likely to slip prior to treatment and to treat those more aggressively. There are many fracture characteristics which have been well shown to predict future redisplacement with conservative treat-ment.1-411 It is our feeling that conservative management should continue to be the mainstay of treatment for these fractures, and casting indices be used only as a guide to earmark those fractures that need closer follow-up. However should the fracture exhibit characteristics that predispose to redisplacement then it should be seriously considered for surgical management.
Conclusion
It is well known that distal radial fractures in children have an increased chance of redisplacement with conservative management and that the correct application and good quality of plaster moulding can assist in preventing fracture redisplacement. There have been many indices developed to assess these factors and predict redisplacement based on these factors.2,6 The TPI was purported to be very accurate in predicting redisplacement.3 In evaluating the TPI as a predictor of fracture redisplacement in dorsally displaced distal radius fractures we found that the TPI was a fair predictor of fracture redisplacement but not to the same degree as initially described. We also concluded that although based on good principles of cast moulding, which should be adhered to when reducing a distal radius fracture and applying a plaster cast, its measurement is not practical at the time of manipulation which is when it would be most useful in determining treatment. It should therefore only be used as a guide to a more careful patient surveillance.
No benefits in any form have been or are to be received from a commercial party related directly or indirectly to the subject of the article. The content of this article is the sole work of the authors.
References
1. Haddad F, Williams R. Forearm fractures in children: Avoiding redisplace-ment. Injury 1995;26:691-92. [ Links ]
2. Mazzini J, Martin J. Paediatric forearm and distal radius fractures: risk factors and redisplacement - role of casting indices. International Orthopaedics 2010;34:407-12. [ Links ]
3. Alemdaroglu K, Iltar S, Cimen O, Uysal M, Alagoz E, Aththan D. Risk factors in redisplacement of distal radial fractures in children. J Bone Joint Surg Am 2008;90:1224-30. [ Links ]
4. Monga P, Raghupathy A, Courtman N. Factors affecting remanipulation in paediatric forearm fractures. J of Pediatr Orthop 2010;19-B:81-187. [ Links ]
5. Basson H, Vermaak SS, Visser HF, Rheeder P. Canterbury index: An accurate predictor of fracture redisplacement? SA Orthop J 2011;10:39-47. [ Links ]
6. Bhatia M, Housden P. Redisplacement of paediatric forearm fractures: Role of plaster moulding and padding. Injury Int J Care Injured 2006;37:259-68. [ Links ]
7. Miller B, Taylor B, Widmann R, et al. Cast immobilization versus percutaneous pin fixation of displaced distal radius fractures in children: a prospective, randomized study. J Pediatric Orthop, 2005;25:490-94. [ Links ]
8. Webb G, Galpin R, Armstrong D. Comparison of short and long arm plaster casts for displaced fractures of the distal of the forearm in children. J Bone Joint Surg Am, 2006;88;9-17. [ Links ]
9. McLauchlan G, Cowan B, Annan I, Robb J. Management of completely displaced metaphyseal fractures of the distal radius in children. J Bone Joint Surg Br 2002;84-B:413-17. [ Links ]
10. Proctor M, Moore D, Paterson J. Redisplacement after manipulation of distal radial fractures in children. J Bone Joint Surg Br 1993:75-B:453-54. [ Links ]
11. Hang J, Hutchinson A, Hau R. Risk factors associated with loss of position after closed reduction of distal radial fractures in children. J Paediatr Orthop 2011;31:501-506. [ Links ]
12. Zamzam M, Khoshhal K. Displaced fracture of the distal radius in children. J Bone Joint Surg Br 2005;87-B:841-43. [ Links ]
 Reprint requests:
Reprint requests:
Dr Thomas Hilton
11 Clive Road Vredehoek Cape Town 8001
Email: tlhilton@hotmail.com
Cell: 082 796 7608 Home: 021 461 5831














