Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SA Orthopaedic Journal
On-line version ISSN 2309-8309
Print version ISSN 1681-150X
SA orthop. j. vol.12 n.1 Centurion Jan. 2013
PEDIATRIC
Leiomyoma of the calf muscle in a child with calcification and ossification - a case report
MN RasoolI; S SinghII; PK RamdialIII
IFCS(SA)Orth. Consultant Orthopaedic Surgeon, Department of Orthopaedics, University of KwaZulu-Natal, Nelson R Mandela School of Medicine
IIMBChB(Natal). Registrar Anatomical Pathology, Department of Anatomical Pathology, University of KwaZulu-Natal
IIIMD, FC Path(Anat)SA. Professor, Department of Anatomical Pathology, University of KwaZulu-Natal
ABSTRACT
Leiomyomas (smooth muscle tumours) arising in skeletal muscle are extremely rare in children, especially in the extremities.
A 3-year-old girl presented with a slow-growing mass in the left calf which had been present since the age of 6 months. Plain radiographs revealed a well-circumscribed mass, fusiform in shape, not attached to bone. There was widespread calcification of the tumour. MRI confirmed extensive calcification and ossification in the soleus and medial head of the gastrocnemius displacing the neurovascular bundle anteriorly. A diagnosis of a sarcoma was suggested.
The mass was well defined at surgical exploration, encapsulated and easily dissected from the soleus, gastrocnemius muscles and blood vessels.
The tumour was gritty on cutting with a saw and histology confirmed a leiomyoma of the soleus muscle. Immunohistochemical markers for smooth muscle actin and desmin were positive. The recovery was uneventful at five-month follow-up.
Key words: leiomyoma, calf muscle, calcification, ossification, immunohistochemistry
Introduction
Leiomyomas are extremely rare in the deep soft somatic tissues of the body. Those described have been seen mainly in the cutaneous and subcutaneous tissues and in the genito-urinary tract and abdominal cavity mainly in adult females. Leiomyoma of deep soft tissue, arising in skeletal muscle of the extremity, is rarely seen by an orthopaedic surgeon.1,2
The lesion may be calcified or even rarely show ossification with calcification. These radiological features can be misdiagnosed for more familiar conditions like calcified tuberculous nodes, calcified haematoma, myositis ossificans, tumoral calcinosis or benign and malignant tumours of soft tissue seen in the musculoskeletal system.3,4
Normal smooth muscle is widely distributed in the body being present in the walls of the genito-urinary, gastrointestinal, respiratory tracts, skin and blood vessels. Leiomyoma arising in skeletal muscle is thought to be of vascular origin.2 Yannopoulos and Stout expressed a probable venous origin.5 Goodman suggested that these tumours arose from undifferentiated mesenchymal cells or smooth cell rests.6 Kransdorf in a ten-year review of benign soft tissue tumours in about 40 000 cases found no deep leiomyomas in children <14 years old.7
Farman in a review of 7 748 leiomyomas found that 95% occurred in the female genital tract and the remainder were distributed over various sites.8 Billings in a large study found only three children with deep soft tissue leiomyomas, two involved the forearm and one in the thigh.9 Eleven cases involving the extremities in children have been described in the literature and seven cases involving skeletal muscle have been reported.510-13 Calcified lesions have been described on six occasions.3-613,14 Calf muscle involvement has been reported in two children previously.4,13 Ossification with calcification was seen in one case only.12
The aim of this report is to increase the awareness of the clinicopathological features of leiomyoma of deep soft tissue in children, and to include the tumour in the differential diagnosis of diffuse calcification in soft tissue in children.
Case report
A 3-year-old girl presented with a swelling over the posteromedial aspect of the left calf. The swelling was noticed at 6 months and gradually increased in size. Pain and a limp were the initial presenting features. There was no history of trauma. On clinical examination there was a fusiform swelling over the posteromedial aspect of the left leg in the calf muscle ± 10 cm x 6 cm (Figure 1).
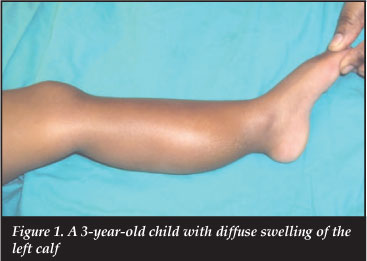
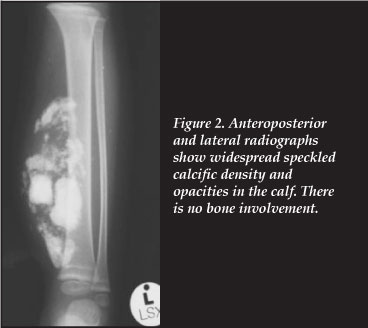
The surface temperature was normal, the mass was smooth, firm with well-defined edges, not attached to bone or skin, with no fluctuance. Pain was elicited on pressure, and the child walked with a limp. The tendo-Achilles was contracted and dorsiflexion to neutral was elicited. There was no neurovascular deficit. No local or generalised lymph nodes were palpated. The child was apyrexial. The plain radiographs of the left leg showed an oval, well-circumscribed lesion in the calf with calcific densities and areas of opacification (Figure 2). A rim of calcification around the lesion suggested a pseudo capsule. Magnetic resonance imaging (MRI) with intravenous contrast showed an oval mass in the middle and distal calf, with no bony involvement, in the posterior compartment (Figures 3 a and b). The mass had a heterogeneous signal intensity and demonstrated intense enhancement. Areas of ossification were demonstrated. The lesion demonstrated expansion of the calf muscles with anterior displacement of the neuro-vascular bundle. The suggested diagnosis was a soft tissue tumour such as a rhabdomyosarcoma. The chest X-ray was normal. The laboratory tests (full blood count, urea and electrolytes, liver-function tests and inflammatory markers) were essentially normal. The erythrocyte sedimentation rate was 24 mm/hr. The Mantoux skin test was normal. The bone scan showed no other areas of uptake apart from the left calf region.
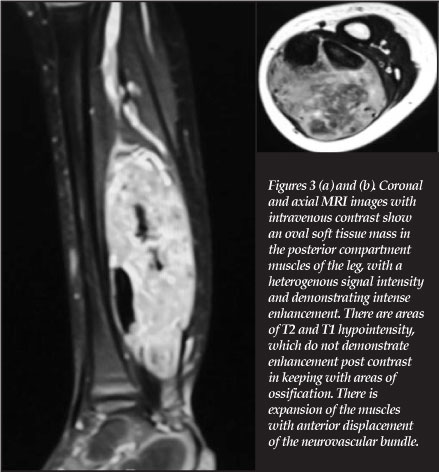
Surgical exploration was performed under tourniquet control. The mass was well delineated arising proximally deep to the medial gastrocnemius, from the soleus muscle belly and extending distally to the tendinous junction between soleus and gastrocnemius. The muscles were stretched over the mass and the neurovascular bundle was stretched and adherent anterior to the mass, but dissected off easily. The mass was oval, well-defined, and rubbery in consistency with a pseudocapsule (Figure 4).
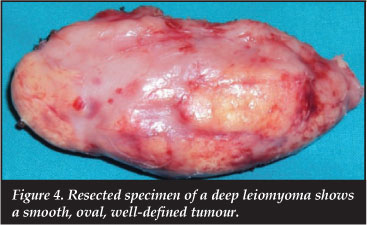
There was no increase in vascularity in the region and bleeding was minimal. The mass measured 9 cm x 5 cm.
Macroscopically the specimen was firm, solid and had to be sectioned with a band saw and showed calcific flecks and multifocal areas of ossification. It was grey-white in colour, with a firm solid consistency. A gritty sensation was noted on sectioning.
Microscopic staining with haematoxylin and eosin (H&E) demonstrated a spindle cell tumour with large areas of hyalinisation, calcification and ossification. Necrosis was not seen. The tumour pattern was one of interlacing fascicles. The individual tumour cells contained clear and eosinophilic cytoplasm, elongated, blunt-ended nuclei with minimal size variation, and variable cytoplasmic vacuolation was evident. The mitotic count was <1 per 50 high power fields (HPF). Special stains confirmed a smooth muscle immunophenotype confirmed by alpha smooth muscle actin and desmin immunopositivity. The immunohistochemical markers for skeletal muscle, neural, epithelial, melanocytic, chondroid and endothelial lineage were negative. Necrosis, cellular pleomorphism, haemorrhage and vascular or perineural invasion was not seen. Entrapped aponeurotic and atrophic skeletal muscle tissue was seen. There was no atypia or features of malignancy. Epstein Barr virus encoded RNA testing was negative. The histopathological features suggested a myoid tumour compatible with a deep leiomyoma. The excision margins were free of tumour. The post-operative course was uneventful. The radiographs at follow-up were normal (Figure 5).
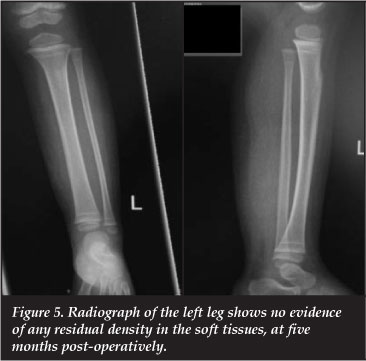
Discussion
Leiomyoma of deep soft tissue is exceptionally rare compared to its malignant counterpart. Leiomyoma is a benign, usually solitary tumour of smooth muscle origin commonly involving the organs of the body composed of smooth muscle such as the uterus, urogenital tract and gastrointestinal tract.1,2 When found in soft tissue, it usually involves the dermis and subcutaneous layer. It very rarely affects the deep soft tissue.1,2,13 The deep leiomyomas have been found most frequently within skeletal muscle originating from vessels with unstriated muscle. They are more common in adults and rarely described in children.13 The tumour usually shows calcification in 58% of cases.13 The largest tumour described in children measured 7.5 cm.6
The radiological appearance can resemble various familiar conditions seen in orthopaedics and the diagnosis can be challenging.
Leiomyoma involving skeletal muscles of the extremities in children has been reported in nine children only, viz: thigh muscles = 3, arm = 1, calf = 2, deltoid = 1, pectoralis major = 1 and subscapularis = 1. Calcification occurred in six cases.3-6,13,14 Calcification with ossification was only seen once.1,2 A history of minor trauma was recorded in three patients.
Histologically, these lesions are composed of well-differentiated, smooth muscle cells with abundant eosinophilic cytoplasm similar to vascular smooth muscle.1,2 The existence of leiomyomas of deep soft tissue has been ques-tioned.2,10 The tumours should be diagnosed using the most stringent criteria.9 They are highly differentiated smooth muscle tumours. Somatic leiomyomas should show no necrosis, at most mild atypia, virtually no mitotic activity with <1 mitosis per 50 HPF. Spindle cells are arranged in a parallel fashion with eosinophilic cytoplasm. The cells appear to originate from the outer layers of vascular channels. Tumour cells are usually positive for vimentin, desmin and smooth muscle actin.
Calcification is usually macroscopic and visible as opacities on radiographs. Microscopic calcification is also reported.5 The precise nature and pathogenesis of calcification in deep leiomyomas is uncertain. Classically, they have been considered to be dystrophic changes following tumour haemorrhage, necrosis or lique- faction.3,11 More recently, alkaline phosphatase, similar to uterine myoma, has been detected in the tumour, suggesting that the enzyme may play a role in the pathogenesis of calcification.13 Calcification may be scattered foci.11 In one report, the calcifications consisted of laminated, concentric spherules.3 In another, the calcifications appeared 'mulberry' in type, in the sub- scapularis muscle and the calf.3,4
Calcific deposits in soft tissue can cause diagnostic challenges in orthopaedics. Among the conditions which produce localised soft tissue calcification are calcified haematoma, myositis ossificans, tumoral calcinosis, tuberculous lymphadenitis, pilomatrixomas, calcifying fibrous pseudotumour, synovial sarcoma, mesenchymal chondrosarcoma and extraskeletal osteosarcoma. These have similar radiological findings to leiomyomas in deep soft tissue.3,4,14
The calcified haematoma is composed of granulation and fibrous tissue, siderophages, inflammatory cells and coarse calcification. The granulation tissue reflects the reactive nature of the process. Myositis ossificans also occurs in muscle. Microscopically, it is well circumscribed and has a zonal pattern that is reflective of the degree of cellular maturation. The outermost zone is composed of mature, including lamellar, bone; and the innermost zone is composed of richly vascular fibroblastic tissue. The intermediate zone contains ill-defined trabeculae of admixed fibroblasts, calcification, osteoblasts, osteoid and ectatic vascular channels. The ossific appearance of the radio opaque mass and its conformity to muscle planes make the distinction from the popcorn-like calcification of leiomyomas. The morphology of tumoral calcinosis depends on the stage of the disease. In the early proliferative phase, foamy histiocytes, fibroblast-like cells and siderophages are seen. In the active stage, macrophages, giant cells, osteoclast-like giant cells characterised by fibrosis and calcification are seen. A smooth, muscle-rich component is not a feature of any stage. Fluid levels may be seen in the tumour. Calcified lymph nodes of tuberculosis demonstrate variable fibrocalcific alterations with stippled and coarse calcification. A variable palisade of histiocytes, granulomas and hyalinisation are seen.
Pilomatrixomas are tumours of hair follicle origin that are composed of sheets of basaloid, epithelial cells and anucleate ghost cells. A spindle-cell component is not a feature of this tumour in the cellular or late calcified and ossified stage. These tumours are benign calcifying epithe-liomas which occur in the skin and the subcutaneous tissue. Radiographically, they are well-delineated soft tissue tumours which contain fine sand-like calcification.15
Parasitic cysts due to hydatidosis and cysticercosis may calcify. While granulomas, histiocytes and eosinophils may be variably present around the calcified cyst wall, there is no evidence of an associated smooth muscle proliferation.
Scleroderma, calcification due to calcium gluconate extravasation, haemangiopericytoma, fibrosarcoma and ossifying lipofibroma can also produce localised soft tissue calcification.
Calcifying fibrous pseudotumours are hypocellular, hyalinised, fibrosclerotic tumours with psammomatous calcification. There is a variable inflammatory background with germinal centre formation. It contrasts with the cellular nature of leiomyoma.
Monophasic synovial sarcoma shares the spindle-cell morphology of leiomyoma. There may be fine coarse calcification and ossification. However, the cells lack the eosinophilic cytoplasm that is characteristic of smooth muscle cells. In addition, synovial sarcoma expresses variable epithelial membrane antigen and cytokeratin immunopositivity.
Extraskeletal osteosarcoma contains pleomorphic osteoblasts in osteoid. There is hypercellularity, increased mitotic activity and necrosis. Leiomyoma lacks pleomorphism, necrosis, high mitotic activity and malignant osteoblasts.
Mesenchymal chondrosarcoma is a biphasic tumour with sheets of undifferentiated spindle, round and oval cells, a haemangiopericytic pattern and lobules of hyaline cartilage. Focal calcification and ossification of the cartilaginous component may be present. Leiomyoma lacks these characteristics.
Epstein Barr virus (EBV)-associated smooth muscle tumours are a recently emerging entity that occur in the setting of immunocompromised patients at a greater frequency than the general population.2 Smooth muscle tumours have now been reported in patients with various types of organ transplants in patients with Aids and in those with congenital immunodeficiency.2 The common denominator in all cases appears to be EBV virus infection in the setting of immunocompromise. EBV can be detected by in situ hybridisation in virtually all tumours studied.2 In these patients the tumours are mainly visceral. In a five-year clinico-pathological review, Ramdial et al described six leiomyomas in patients with Aids associated with the EBV to increase the awareness of this association. Two of these children had masses in the dermis of the lower limbs. They also had associated tuberculosis of the chest. The intramural EBV status of all tumours was determined by EBV-encoded RNA in situ hybridisation.16,17
Conclusion
The outcome of treatment of leiomyoma of deep soft tissue is usually good. In previously reported cases of leiomyoma, total excision of the tumour provided complete cure without recurrence. Leiomyomas very rarely undergo malignant transformation.3,9,10 The location of the tumour reported in this study is uncommon. The progressive calcification with ossification is unique and important in differential diagnosis. A well-defined circumscription with a pseudocapsule is a characteristic feature.
No benefits of any form have been received from a commercial party related directly or indirectly to the subject of this article. All subjects included in this study provided their written informed consent.
References
1. Weiss SW, Goldblum JR. Benign tumors of smooth muscle in Weiss SW and Goldblum JR, eds Enzinger and Weiss's soft tissue tumors. 5th ed. St Louis Mosby-Harcourt 2001, pp. 517-43. [ Links ]
2. Weiss SW. Smooth muscle tumors of soft tissue. Adv in Anat Pathol 2002;9:351-59. [ Links ]
3. Ledesma-Medina J, Oh KS, Girdany BR. Calcification in childhood leiomyoma. Radiology 1980;135:339-41. [ Links ]
4. Ross LS, Eckstein MR, Hirschhorn R, et al. Calcified leiomyoma -an unusual cause of large soft tissue calcification of the calf in childhood. NY State J Med 1983;83:747-49. [ Links ]
5. Yannopoulos K, Stout AP. Smooth muscle tumors in children. Cancer 1962;15:958-71. [ Links ]
6. Goodman AH, Briggs RC. Deep leiomyoma of an extremity. J Bone Joint Surg 1965;47A:529-32. [ Links ]
7. Kransdorf MJ. Benign soft-tissue tumors in a large referral population. AJR 1995;164:395-402. [ Links ]
8. Farman AG. Benign smooth muscle tumors. S Afr Med J 1975;49:1333-40. [ Links ]
9. Billings SD, Folpe AL, Weiss SW. Do leiomyomas of deep soft tissue exist? An analysis of highly differentiated smooth muscle tumors of deep soft tissue supporting two distinct subtypes. Am J Surg Pathol 2002;25:1134-42. [ Links ]
10. Botting AJ, Soule EH, Brown AL. Smooth muscle tumors in children. Cancer 1965;18:711-20. [ Links ]
11. Bulmer JH. Smooth muscle tumors of the limbs. J Bone Joint Surg 1967;49B:52-58. [ Links ]
12. Kilpatrick SE, Mentzel T, Fletcher CDM. Leiomyoma of deep soft tissue: clinic pathologic analysis of a series. Am J Surg Pathol 1994;18:576-82. [ Links ]
13. Lopez-Barea F, Rodriguez-Peralto JL, Burgos E, et al. Virchows Archiv 1994;425:217-20. [ Links ]
14. Manojlovic S, Aljinovic-Ratkovic N, Kruslin B. Calcified leiomyoma of the lateral pterygoid muscle in an 8 year old boy. Oral Radiol Endod 2000;89:199-203. [ Links ]
15. Haller JO, Kassner EG, Ostrowitz A, et al. Pilomatrixoma (calcifying epithelioma of Malherbe): radiographic features. Radiology 1977;123:151-53. [ Links ]
16. Ramdial PK, Sing Y, Deonarain J, et al. Extrauterine myoid tumors in patients with acquired immunodeficiency syndrome: a clinico-pathological appraisal. Histopathology 2011;59:1122-34. [ Links ]
17. Ramdial PK, Sing Y, Deonarain J, et al. Dermal Epstein Barr Virus - associated leiomyosarcoma: Tocsin of acquired immuno-deficiency syndrome in two children. Am J Dermato pathology 2011;33:392-96. [ Links ]
KEY WORDS REQUIRED IN ARTICLES
The South African Orthopaedics Journal (SAOJ) has been accepted by the Academy of Science of South Africa as a publication on their online facility, the Scientific Electronic Library Online (SciELO). This open access facility is linked to Google and is an enormous step forward for our Journal.
SciELO has requested that all authors of articles include five key words at the beginning of each article in order to make it easier to conduct a search when published online. We ask all authors to kindly comply with this request.
 Reprint requests:
Reprint requests:
Mr MN Rasool
Dept of Orthopaedics
University of KwaZulu-Natal
Nelson R Mandela School of Medicine
Private Bag 7 Congella 4013














