Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SA Orthopaedic Journal
On-line version ISSN 2309-8309
Print version ISSN 1681-150X
SA orthop. j. vol.12 n.1 Centurion Jan. 2013
SPINE
Limited pedicle screw constructs in adolescent idiopathic scoliosis surgery and clinical correlation
JH DavisI; RN DunnII
IMBChB(UFS), FCOrth(SA), MMed(Orth)SU. AO Spine Fellow, Groote Schuur Hospital, Division of Orthopaedic Surgery, University of Cape Town
IIMBChB(UCT), FCOrth(SA), MMed(Orth)UCT. Consultant Spine and Orthopaedic Surgeon, Full Professor University of Cape Town, Head: Division of Orthopaedic Surgery, Head: Orthopaedic Spinal Services Groote Schuur Hospital
ABSTRACT
STUDY DESIGN: Retrospective study of 31 patients treated for adolescent idiopathic scoliosis utilising posterior double rod constructs with a limited number of strategically placed screws.
OBJECTIVE: Review of the radiological and clinical outcomes of strategic screw placement in posterior double rod constructs with respect to implant density.
SUMMARY OF BACKGROUND DATA: The trend in scoliosis surgery dictates the use of pedicle screw constructs with anchors at every level. Favourable correction and clinical outcomes have been reported using this technique. The cost burden of such an implant construct is high; with the additional risk of pedicle breach and neurological compromise multiplied by the number of screws. The sustainability of this practice is questionable.
METHODS: Thirty-one patients, treated surgically for adolescent idiopathic scoliosis, with a minimum two-year follow-up, were included. Posterior double-rod constructs were used in all cases. Cobb angles were measured pre-operatively, post-operatively and at two-year follow-up. Patient satisfaction and clinical outcome were evaluated through the SRS22 questionnaire.
RESULTS: Lenke classification yielded 16 type I, seven type II, four type III, two type IV and two type VI curves. The average Cobb angle pre-surgery was 68.5° (±17.6°), with a flexibility of 38%. This was corrected to an average of 24°±11.9°. The correction was maintained at two-year follow-up. In terms of thoracic sagittal profile, 25 patients measured 'normal' (10°-40°) post-operatively, compared to 17 pre-operatively.
This correction was achieved with a 52.2% metal density over an average of nine instrumented segments. Average SRS22 patient satisfaction score was at 89%.
CONCLUSION: Strategic screw placement, in adolescent idiopathic scoliosis surgery, yields adequate correction and curve maintenance. High levels of patient satisfaction were achieved at a dramatically reduced cost, with a diminished risk for pedicle violation.
Key words: adolescent idiopathic scoliosis, posterior fusion, pedicle screws, metal density
Key points
- Extensive implant constructs used in adolescent idiopathic scoliosis surgery are expensive and carry the risk of pedicle violation multiplied by the number of pedicle screws used.
- Adequate correction of the spinal deformity can be achieved using selectively placed pedicle screws in lower numbers, with clinical outcomes and patient satisfaction comparable to more extensive constructs.
- The correction of the deformity is maintained at two years.
- This equates to a marked reduction in cost, as well as a decrease in risk for neurological compromise.
Introduction
The advantages gained using three-column pedicular fixation in scoliosis surgery have been clearly demonstrated in several reports, both in terms of ability to correct deformity as well as the maintenance thereof.1-5 It allows for powerful segmental derotation and correction of severe deformity often negating the need for anterior release and the associated complications.3 The escalating costs associated with the current trend of pedicle screws at every level in the implant construct, contribute towards making this surgery unaffordable in less affluent environments. In South Africa such is the case and reliance on strategically placed fixation points is required. We report our results.
Materials and methods
We performed a retrospective case note review of patients treated surgically, using posterior double rod constructs with strategic pedicle screw placement, for adolescent idiopathic scoliosis, with at least a two-year follow-up. Thirty-one cases were studied, including four males and 27 females. The average age when the deformity was noted was 11.9 (5-14±2.2) years, with presentation to the treating surgeon at 13 (10-15±1.34) years. The average age at time of surgery was 14.3 (12-22±2.2) years. Five patients had a history of spinal deformity in the family.
Radiographic analysis was performed at three time points, viz. pre-operatively, post-operatively and at two-year follow-up. Pre-operative radiographic review included: a standard whole spine - erect (postero-anterior view), lateral view as well as supine side bending views. Two-year follow-up radiographic analysis included a standard postero-anterior view and a lateral view only. Standard Cobb angle measurements quantified both major and compensatory curves, with further measurements performed to delineate sagittal profile, sagittal balance, coronal balance and T1 vertebral angle. Apical vertebral rotation was measured using the Nash-Moe method.
All cases were classified according to the Lenke system of classification6 with supine side bending views used to calculate curve flexibility (degrees of correction divided by initial Cobb angle, expressed as a percentage) and aid with determination of construct end levels.
Metal density was determined to be 100% for the involved level when both pedicles of the specific vertebra were instrumented, 50% with only a single pedicle instrumented for the involved level, and 0% if no pedicle screws were placed at the specific level. A density was calculated by the number of screws divided by the number of pedicles available within the fused segment.
Surgical technique
All surgery was performed by a single surgeon utilising the same technique and type of instrumentation (Synthes Universal Spinal System - Titanium) with fixed pedicle screws.
Surgery was performed with the patient prone on a Relton-Hall frame, with solid fusion of a corrected and balanced spine as the ultimate goal. Instrumentation of the pedicles was attained by means of a 'free-hand' technique. Pedicle screws were placed at the predetermined ends of the structural deformity. Typically four screws would be placed at the caudal foundation, as well as the cephalad end of the construct. Further pedicle screws were then placed at strategically selected levels, typically including more screws in the concavity of the deformity. No standardised formula was used to determine anchor points, but satisfactory screw-bone interface and purchase as well as curve mobility influenced subjective optimal placement. To aid with curve mobility, facetectomies and Ponte osteotomies were added in individual cases. Manually pre-contoured hard titanium rods were then inserted with correction of the deformity established through a combination of rod derotation, translational reduction and, if required, in situ correction with coronal benders. Posterior element decortication was then performed with allograft (demineralised bone matrix) bone grafting performed prior to closure. No thoracoplasties were performed in this series.
Statistical analysis
Statistical analysis was performed using the Student T-test for continuous data, and Fisher Exact for categorical data. The statistical analysis was achieved with aid of Statistica 8 Software.
Results
The curves included 16 Lenke type I curves, seven type II, four type III, two type IV and two type VI curves.
The average major curve deformity as defined by Cobb angle measurements was measured to be 68.5° (40°-111°) ± 17.6°. This deformity corrected to 43.4° (11°-85°) ± 19.5° on average as measured on the supine side bending views, representing an average flexibility of 38% (0-81) ± 19%.
Post-operatively the average Cobb angle measurement was 24° (9°-70°) ± 11.9° for the major curves involved. This represents an improvement average of 65.1% (36.9- 88.9) ± 10.7% (p=0.000).
This correction was maintained at two years with an average Cobb angle measurement of the major curve found to be 27° (8.0°-70.0°) ± 11.8° (well within 5° of intra-observer variability) (p=0.002).
As expected, the degree of curve correction closely followed curve flexibility as shown in the corresponding gradient of the trend lines in Figure 1, reflecting change in Cobb angle to curve flexibility.

The average thoracic sagittal profile was measured at 34.5° (4°-81°) ± 21.4° (superior end-plate T5 to inferior end-plate T12). This measured kyphosis decreased somewhat to 27.5° (0.0°-64.0°) ± 14.4° which was found to be in line with other authors but not to the same extent.7 Again this correction was maintained at two years at 29.2° (1.0°-66.0°) ± 16.3°.
More interestingly, pre-operatively, 14 out of a possible 31 patients fell into the normal (N) bracket of thoracic sagittal profile of 10°-40° as per the Lenke classification. This number increased to 25 following surgery (p=0.008).
Average rotation as per the Nash-Moe: 2.3 (1.0-4.0) ± 0.6 pre-operatively, improved to 1.7 (1.0-3.0) ± 0.5. This correction was maintained at two years and shown to be statistically significant through the Student T-test (P= 0.00000040).
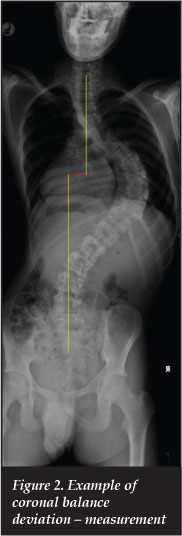
Coronal balance as measured in Figure 2, showed a pre-surgery deviation of 15.8 mm (0.0-40.0) ± 11.7 mm; this was decreased through surgery to 11.2 mm (0.0-40.0) ± 10.8 mm with a further slight improvement noted at two-year follow-up of 9.6 mm (0.0-40.0) ± 9.9 mm (results corrected for direction of deviation) (p=0.05).
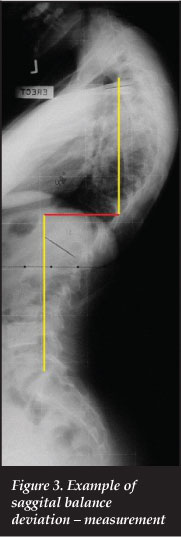
Similarly the sagittal profile, as depicted in Figure 3, showed an improvement from 20.9 mm (0.0-50.0) ± 15.8 mm pre-operatively to 13.6 mm (0.0-60.0) ± 14.3 mm. This was again maintained at two-year follow-up: 13 mm (0.0-60.0) ± 14 mm (results corrected for direction of deviation).
T1 angle as shown in Figure 4 measured 7.6° (0.0°-25.0°) ± 6.4° on average (corrected for direction of deviation) and was altered to 8.4° (0.0°-25.0°) ± 6.6°.

The average number of segments involved in a typical posterior instrumentation construct included nine levels (6-13) ± 2, with the average number of anchor points per construct being 9.2 (6-13) ± 1.7. This represents a metal density of 52.2 % (30.0-68.8) ± 8.8 % (Figure 5). In support of published material our data did not show a dramatic increase in curve correction with an increased number of anchor points and metal density.7

Clinical outcomes and patient perception of the utilised treatment was reflected in an average SRS22 score of 87.9 (68.0-107.0) ± 12.9 out of a possible 110 points (total SRS22 score). This represents a 79.9% favourable clinical outcome.
Strategic screw placement offered adequate coronal plane correction of the measured major curve deformities; with 65.1% improvement in Cobb angle compared to 69%-79.6% reported in various publications.2,9-11,13 The slightly lower coronal plane correction could also account for the lower degree of hypokyphosis of the thoracic spine resulting from surgery with an average decrease in thoracic kyphosis of 7° in comparison with published results ranging from 10° to 12° 3-5,14
It is however noteworthy that in this data series the 65.1% improvement in Cobb angle was achieved using a 52.2% metal density; in comparison to more than 75% (>75%; 84.5%-100%) in the corresponding reports.2,7-11,13 Our cohort had the greatest initial average deformity and the lowest flexibility, when compared to published reports summarised in Table I.
This data series further showed an average 'satisfaction' determinant (subdivision of the SRS22 score) of 8.9 (6.0-10.0) ± 1.3 out of a possible 10. This represents an 89% positive patient perception of the results.
Discussion
The efficacy and maintenance of deformity correction in scoliosis, with the aid of pedicle screw constructs, have been well demonstrated in the published body of literature.1-4,7-11 The contemporary trend in scoliosis surgery compels surgeons to make use of extensive instrumentation constructs with pedicle screws placed at every single involved level and often in every available pedicle.
This practice is not financially sustainable in less affluent regions of the globe due to soaring implant expenses. In addition there is the risk of pedicle violation multiplied by the number of pedicle screws.12
Compared to related literature (originating from authors making use of similar classification and surgical techniques), we found that in our cohort, patients typically presented at a slightly more advanced age, with less curve flexibility evident on supine side bending radiographs.
Conclusion
In our opinion, excellent curve correction and maintenance thereof is possible in adolescent idiopathic scoliosis, with less instrumentation and a corresponding reduction in cost and associated risk.
The content of this article is the sole work of the authors. No benefits in any form have been or will be received from a commercial party related directly or indirectly to the subject of this article.
References
1. Kim YJ, Lenke LG, Cho SK, et al. Comparative analysis of pedicle screw versus hook instrumentation in posterior spinal fusion for adolescent idiopathic scoliosis. Spine 2004;29:2040-48. [ Links ]
2. Kim LJ, Lenke LG, Kim JH, et al. Comparative analysis of pedicle screw versus hybrid instrumentation in posterior spinal fusion of adolescent idiopathic scoliosis. Spine 2006;31:291-98. [ Links ]
3. Dobbs MB, Lenke LG, Kim YJ, et al. Selective posterior thoracic fusions for adolescent idiopathic scoliosis: comparison of hooks versus pedicle screws. Spine 2006;31:291-98. [ Links ]
4. Lehman RA Jr, Lenke LG, Keeler KA, et al. Operative treatment of adolescent idiopathic scoliosis with posterior pedicle screw-only constructs: Minimum three year follow up of one hundred fourteen cases. Spine 2008;33:1598-604. [ Links ]
12. Şarlak HY, Tosun B, Atmaca H, et al. Evaluation of thoracic pedicle screw placement in adolescent idiopathic scoliosis. European Spine Journal, 2009;18(12):1892-97. [ Links ]
13. Lee SM, Suk SI, Chung ER. Direct vertebral rotation: A new technique of three-dimensional deformity correction with segmental pedicle screw fixation in adolescent idiopathic scoliosis. Spine 2004;29:343-49. [ Links ]
14. Lumann SJ, Lenke LG, Kim YJ, et al. Thoracic adolescent idiopathic scoliosis curves between 70 degrees and 100 degrees: Is anterior release necessary? Spine 2005;30:2061-67. [ Links ]
15. Lehman RA, Jr, Lenke LG, Keeler KA. Operative treatment of adolescent idiopathic scoliosis. Spine 2008;33(14):1598-04. [ Links ]
16. Spinal Deformity Study Group. Radiographic Measurement Manual . s.l. : Medtronic Sofamor Danek USA, 2005. [ Links ]
17. Weiss H, Bess S, Wong MS, Patel V, Goodall D, Burger E. Adolescent idiopathic scoliosis - to operate or not? A debate article. Patient Safety in Surgery 2008;2:25. [ Links ]
 Reprint requests:
Reprint requests:
Prof RN Dunn
Division of Orthopaedic Surgery
H49 OMB Groote Schuur Hospital
Anzio Road Observatory 792
South Africa
Tel: +27 21 404 5387 Fax: +27 21 7628796
info@spinesurgery.co.za














