Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
SA Orthopaedic Journal
versão On-line ISSN 2309-8309
versão impressa ISSN 1681-150X
SA orthop. j. vol.11 no.4 Centurion Jan. 2012
CASE REPORT
An unusual case of a transabdominal, transdiscal stab wound to the spine
M HeldI; M LaubscherII; P NavsariaIII; RN DunnIV
IDrMed Registrar: Department of Orthopaedics
IIMBChB Registrar: Department of Orthopaedics N Kruger MBChB, FCOrtho(SA) Consultant, Spine Unit, Department of Orthopaedics
IIIMBChB, FCS(SA), MMed Deputy Head: Trauma Centre, Groote Schuur Hospital Associate Professor: Department of Surgery
IVMBChB(UCT), MMed(UCT)Ortho, FCS(SA)Orth Consultant Spine and Orthopaedic Surgeon Professor and Head: Department of Orthopaedics Head: Orthopaedic Spinal Services, Groote Schuur Hospital Spine Deformity Service, Red Cross Children's Hospital University of Cape Town
ABSTRACT
BACKGROUND: Anterior stab wounds to the spine are extremely rare. Depending on the weapon, trajectory and anatomical level, patients are likely to present with associated damage to large vessels, the lungs, heart, and the gastrointestinal, as well as genitourinary system.
METHODS: In this case report, we describe the management of a 21-year-old male patient who presented with an injury to the cauda equina after an abdominal stab with a glass bottle. The patient escaped a thorough secondary survey and neurological examination due to massive intra-abdominal injuries, which required initial damage control surgery. Weak left-sided dorsiflexion of the ankle with paraesthesia in the left L4 and L5 nerve root distribution was initially overlooked.
RESULTS: During a follow-up appointment, one month after discharge, chronic pain and cauda equina symptoms were noted. Further imaging revealed a large glass fragment, which had been driven, transabdominally, through the L4/L5 disc into the spinal canal. The fragment was removed through a posterior approach, which alleviated the chronic pain, although the neurological deficit remained unchanged.
CONCLUSION: Neurological damage through anterior stab wounds to the spine has not yet been described. The best approach to these patients is a staged management initially directed at treating life-threatening injuries in the form of damage control surgery. Once stable, a thorough neurological reassessment must follow to rule out spinal cord injuries
Key words: anterior stab to the spine, cauda equina injury, foreign body spine
Introduction
Penetrating spinal cord injuries are most often caused by gunshots or stab wounds. In stabs, in almost all cases the direction of injury is from posterior. Anterior thoracic or abdominal stab wounds leading to spinal cord injury have not been reported to our knowledge. We present a rare case where an abdominal stab with a glass bottle resulted in a transabdominal, transdiscal cauda equina injury.
Patient case presentation
A 21-year-old male patient received a single stab in the abdomen with a broken glass beer bottle and arrived at our trauma unit with eviscerated bowel, unrecordable blood pressure, a Glasgow Coma Scale of 5/15 (eyes 1, verbal 1-intubated, motor 3), Injury Severity Score of 34, lactate of 7.5 mg/dl, and pH of 7.06. After intubation and fluid resuscitation he was taken for an emergency exploratory laparotomy by a dedicated trauma team (surgeon: PN).
During laparotomy, a haemoperitoneum (1.5 litres) and gross intra-abdominal contamination of stool were found. Lacerations to the left common iliac vein and artery were treated with a ligation of the vein and repair of the artery as part of the initial damage control surgery. The ileum and sigmoid had multilevel lacerations and were tied off. The abdomen was left open with four abdominal swabs in situ. During the procedure, the patient required a massive blood transfusion with an estimated blood loss of 17.5 litres. After the laparotomy he was admitted to a surgical intensive care unit on high doses of inotropes.
The patient improved haemodynamically and underwent a relook laparotomy 30 h after the initial surgery. The hollow viscus injuries were repaired, abdominal swabs were removed, and the abdomen was closed. The patient was transferred to a low care ward three days later and discharged home seven days later. His complaints of continuing pain and a mild limp were documented but were ascribed to the abdominal surgery, and an injury to the spine was overlooked. No imaging of the abdomen or spine had been performed up to this stage.
One month later the patient was referred to the orthopaedic team (NK) with severe sciatica in his left leg, which had been present since his discharge. A straight leg raise test was positive at 30° on the left and a cross straight leg raise test was present on the right. Weak dorsiflexion of the left ankle of 4/5 (Medical Research Council Scale for muscle strength) and pain with paraesthesia of his anterior and lateral lower leg was noted. These findings were confirmed by a dedicated spinal surgeon and documented according to the American Spinal Injury Association (ASIA) scoring. Subsequent X-ray, magnetic resonance imaging (MRI) and computer tomography (CT) investigations revealed a foreign body in the spinal canal at the level of L4/L5 (Figures 1 and 2).
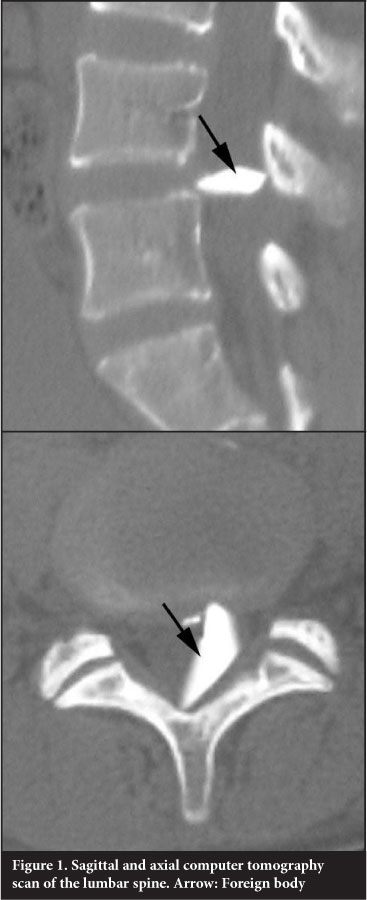
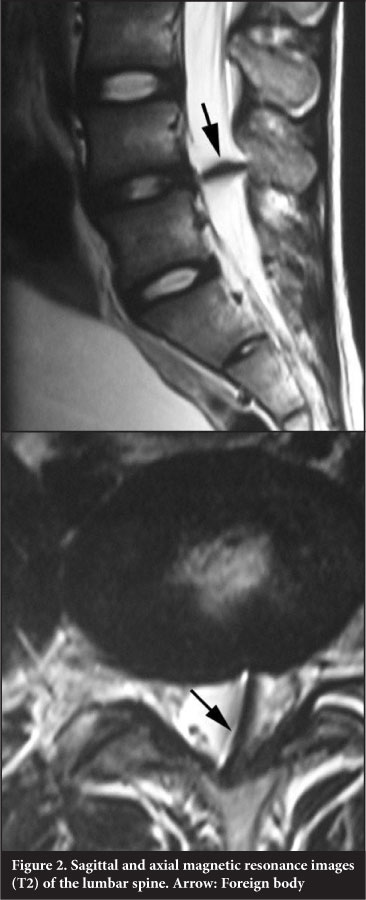
The foreign body was removed six weeks after the injury through a posterior approach. The posterior elements were all intact. A L4 and L5 laminectomy was performed and a glass fragment (1 x 1.5 cm) was removed after posterior durotomy. The L4/L5 disc annulus showed evidence of recent injury with fibrous scarring. The overlying dura was adherent to the annular scar tissue and had been lacerated.
The cauda equina was inflamed and the nerve roots were draped over the glass foreign body. Some intrathecal nerve rootlets had been divided by the glass. The wound was washed and the dural sac was closed with running sutures. No signs of sepsis were noted and no bacterial growth was found on intra-operative wound swabs.
After an uneventful post-operative course, the patient was discharged with resolution of his sciatic pain. The motor deficit remained unchanged. He was followed up one month post-operatively without any signs of complications regarding the surgery, such as wound sepsis or progression of his neurological deficit. His lumbar X-rays did not show any features of discitis and the blood tests showed a normal white cell count and ESR. Consent was obtained from the patient to report and publish this case.
Discussion
The three mechanisms causing spinal cord or nerve injury through a stab are most likely (1) direct cord damage caused by the weapon or bone fragments resulting in a durotomy and transection; (2) damage to the vascular supply of the spinal cord with resulting oedema; and (3) spinal cord contusion when the spinal cord is wedged between the weapon and the spinal canal.1 Intra-operatively, we found an anterior dural tear, which had sealed off at the time of surgery, six weeks after the injury. The cauda equina was inflamed and an injury to the nerve rootlets within the cauda equina was noted. In spite of bowel contamination there was no evidence of intra-operative sepsis and the swabs were negative on culture.
Most stab wounds are found in the thoracic region (63%), followed by cervical and lumbar stab wounds. Knives are used as weapons in 84%, followed by screwdrivers, axes, bicycle spokes and scissors. Most penetrating wounds to the spine are caused by posterior stabs in an upward direction sliding along posterior structures before entering the spinal cord causing partial transection of the cord.1 Rubin reported a case where a stab wound took a lateral, almost horizontal, route between C1 and C2, which allowed the blade's entrance into the spinal canal and caused complete transection.2 Similar to this uncommon direction of assault, the stab wound of our patient had avoided the natural protection from the posterior structures. It was directed from anterior and travelled through the left iliac fossa, breached the left common iliac artery and vein, and a glass fragment was driven through the L4/L5 intervertebral disc into the spinal canal.
Associated injuries increase the severity of the trauma for patients with stab wounds to the spine. Cervical spine injuries tend to have a high incidence of vascular complications, while thoracic stab wounds often have additional pulmonary and cardiac injuries. Lumbar knife injuries may be associated with damage to abdominal viscera, major vascular structures and the genitourinary system.3
Diagnosis
A thorough clinical examination is the single most important factor in diagnosing spinal cord injuries. In the severely unstable patient an initial neurological examination is often difficult to perform and a careful reassessment, once stabilised, is essential to minimise the risk of missing an injury.3 Our patient escaped a thorough secondary survey due to cardiovascular collapse on presentation and massive intra-abdominal injuries which required emergency surgery. Neurological deficits were missed, even after transfer to the low care ward and prior to discharge. Slow mobilisation and complaints of back pain were ascribed to the severe abdominal injury and multiple laparotomies. Up to this point, X-rays or CT scans of the abdomen or the spine were not available to rule out an injury to the spine.
Imaging of stab wounds to the spinal cord remains controversial, yet has its place in patients undergoing spinal surgery.4 In all penetrating spinal injuries a routine radiological examination of the involved area should be obtained. Specific attention should be directed towards detecting fractures and retained fragments. Foreign bodies can be seen as radio-opaque (i.e. metal, gravel, glass) or radiolucent (i.e. plastic, wood).5
Our protocol is to perform a CT scan on all patients with penetrating spinal column trauma in which routine radiographic evaluations were not adequate to define fracture patterns, localise retained fragments, or to understand the direction of the tract. MRI studies are rarely necessary and are reserved for patients with deteriorating or unexplained neurological symptoms.4
Surgical management
Early spinal surgery is focused on cord decompression and avoiding secondary injury by stabilising the spine. This should be performed once blood loss and contamination are under control.3 The indications for surgical treatment with spinal stab wounds are rare. They include: (1) infection; (2) retained fragments; (3) cerebrospinal fluid (CSF) fistula; (4) pseudomeningocoele; (5) instability; (6) chronic pain; and (7) toxicity of foreign bodies.6-8 In our patient, we felt that persistent chronic pain and neurological symptoms in association with the retained fragment supported the indication of spinal surgery and the removal of the foreign body.
Conclusion
Spinal cord injuries through abdominal stab wounds are rare. The intervertebral disc space in this case was an unusual portal of entry to the spinal canal. Due to the anatomy in this region our patient presented with associated injuries to the gastrointestinal tract and large vessels in the pelvis. While focusing on these life-threatening injuries the full extent of the damage in the form of a cauda equina injury by a glass fragment was missed. This demonstrates the importance of a thorough clinical examination and secondary survey in all trauma patients.
The content of this article is the sole work of the authors. No benefits of any form have been or are to be received from a commercial party related directly or indirectly to the subject of the article.
References
1. Peacock WJ, Shrosbree RD, Key AG. A review of 450 stab wounds of the spinal cord. S Afr Med J. 1977;51(26):961-64. [ Links ]
2. Rubin G, Tallman D, Sagan L, et al. An unusual stab wound of the cervical spinal cord: a case report. Spine. 2001;26(4):444-47. [ Links ]
3. Kossmann T, Trease L, Freedman I, et al. Damage control surgery for spine trauma. Injury. 2004;35(7):661-70. [ Links ]
4. Jacobsohn M, Semple P, Dunn R, et al. Stab injuries to the spinal cord: A retrospective study on clinical findings and magnetic resonance imaging changes. Neurosurgery. 2007;61(6):1262. [ Links ]
5. Horton LK, Jacobson JA, Powell A, et al. Sonography and radiography of soft-tissue foreign bodies. Am J Roentgenol. 2001;176(5):1155-59. [ Links ]
6. Heary RF, Vaccaro AR, Mesa JJ, et al. Thoracolumbar infections in penetrating injuries to the spine. Orthop Clin North Am. 1996;27(1):69-81. [ Links ]
7. Potter BK, Groth AT, Kuklo TR. Penetrating thoracolumbar spine injuries. Curr Opin Orthop. 2005;16:163-68. [ Links ]
8. Steinmetz MP, Kirshnaney AA, McCormick W, et al. Penetrating spinal injuries. Neurosurg Q. 2004;14:217-23. [ Links ]
 Reprint requests:
Reprint requests:
Dr M Held
Orthopaedic Department
H49 Old Main Building,
Groote Schuur Hospital
Observatory 7925
South Africa
Tel: 0027214066157
Fax: 0027 21472709














