Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
SA Orthopaedic Journal
versão On-line ISSN 2309-8309
versão impressa ISSN 1681-150X
SA orthop. j. vol.11 no.4 Centurion Jan. 2012
CLINICAL ARTICLE
Pelvic fractures in children: experience at a Johannesburg academic hospital
JRT PietrzakI; AJF RobertsonII
IMBBCh(Wits) Senior Registrar, Department of Orthopaedic Surgery, University of the Witwatersrand
IIMBBCh(Wits), MMed(Orth)(Wits) Head: Paediatric Orthopaedics, Charlotte Maxeke Johannesburg Academic Hospital
ABSTRACT
BACKGROUND: Pelvic fractures in the paediatric population are rare. The skeletally immature pelvis is flexible and therefore a pelvic fracture suggests significant force with a high association of concomitant injuries. Despite these being potentially devastating injuries there are no clear outlines with respect to the investigation, classification and management of these fractures.
MATERIALS AND METHODS: We retrospectively reviewed 20 children with pelvic fractures. We utilised the Injury Severity Score (ISS) and Revised Trauma Score (RTS) to assess the physiological instability of the patient. The Torode and Zieg classification was used to describe pelvic fractures. At follow-up the functional independence for self-care, mobility and cognition was assessed.
RESULTS: Pelvic fractures represented only 0.03% of paediatric orthopaedic admissions. Concomitant injuries were present in 55% of patients. Four of the 20 pelvic fractures were unstable (type 4), of which three required ICU admission and external pelvic fixation for haemodynamic instability. At a mean follow-up of 4 months all patients were functionally independent.
CONCLUSIONS: Although rare, pelvic fractures in children have a high rate (55%) of concomitant injuries. The ISS and RTS scoring systems are useful to predict the severity of the injury. Conservative management and external pelvic fixation (in haemodynamically unstable type 4 fractures) resulted in favourable outcomes.
Key words: paediatric, pelvic, fractures, Torode and Zieg classification
Introduction
Pelvic fractures in children are rare.1-13 They are typically associated with high energy trauma1-19 and are often an indicator of other potentially life-threatening injuries.1-4,6,9 For this reason they are an important aspect in the management of paediatric trauma.
The skeletally immature pelvis is more flexible and plastic due to the large percentage of cartilage and the porous nature of its cortical bone. There is increased elasticity of the symphysis pubis and the sacro-iliac (SI) joints.2-4,8 These unique anatomical features allow the paediatric pelvis to absorb substantial energy before a fracture occurs. Thus a fracture in the child's pelvis suggests substantial force and demands a comprehensive, multisystem approach.3
Trauma scoring systems are used to more fully ascertain the severity of injury. The Injury Severity Score (ISS) is an anatomical scoring system that provides an overall score for patients with multiple injuries. It has been proven to be a useful predictor of multiple organ failure14 and morbidity and mortality in children.1,3,10 The definition of a patient with multiple injuries is one with an ISS greater than or equal to 16. Patients with these scores should be transferred to a designated trauma centre.14
The Revised Trauma Score (RTS) is one of the most commonly used physiologic scores.14 It takes into consideration three physiologic parameters: blood pressure (BP); Glasgow Coma Scale (GCS) and respiratory rate. A score of less than 11 is considered an indication for referral to a dedicated trauma facility.14
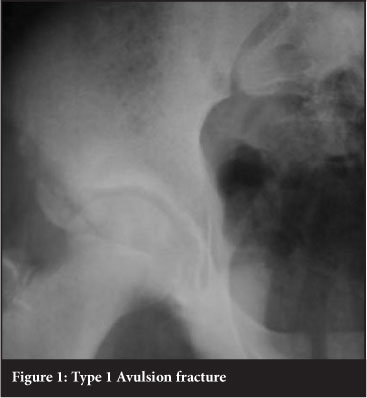
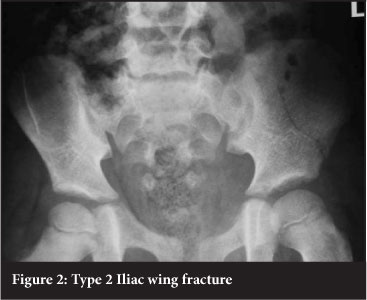
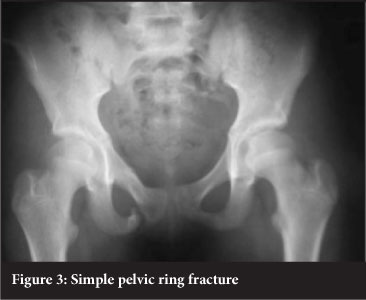
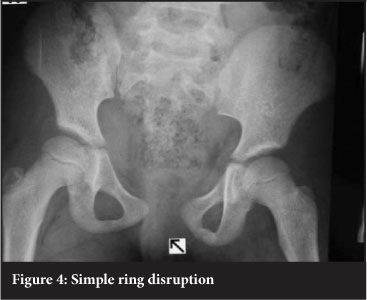
Fracture patterns in the pelvis vary with maturity. No ideal classification system exists for children's pelvic injuries.2,4 The Torode and Zieg classification was proposed in 198515 and is currently the most widely used system in the literature.4,6,7,8 Torode and Zieg type 1 pelvic fractures are avulsion injuries (Figure 1). Type 2 are fractures of the iliac wing (Figure 2). Type 3 fractures are simple ring fractures with no break in the continuity of the pelvis (Figure 3). Type 4 fractures are disruptions of the pelvic ring and are regarded as unstable pelvic injuries (Figure 4). Types 1, 2 and 3 are stable pelvic injuries.
Although there is no consensus over definite mortality rates of pelvic injuries, they have been documented as being 1%-14% (and as high as 25% in one study).1-4,6,8,11,12,14 More children survive pelvic injuries compared to adults, regardless of severity. This, too, poses a tremendous challenge for trauma units.1,5,6,7,9
The aim of this study was to report on our experience with pelvic fractures at Charlotte Maxeke Johannesburg Academic Hospital over a three-and-a-half year period. This unit functions as both an acute trauma care centre and referral institution. The incidence, management and outcomes of these injuries were evaluated.
Patients and methods
Our series included all children up to the age of 16 years admitted with a pelvic fracture to our institution from January 2008 to July 2011.
A retrospective review of the medical records and radiographs of these patients was conducted. Data recorded included age, sex, mechanism of injury, GCS, ISS, RTS radiological investigations, length of hospital stay, length of ICU stay, associated injuries, management (both orthopaedic and non-orthopaedic), length of follow-up and functional outcome. The fracture type was recorded according to the Torode and Zieg classification.
The radiographic evaluation consisted of the advanced trauma life support radiographic trauma series which includes a plain antero-posterior pelvic radiograph. Pelvic inlet and outlet views were not routinely done.
Orthopaedic injuries were defined as all bony fractures excluding skull and facial fractures. Non-orthopaedic injuries were sub-divided by body region: soft tissue, abdominal, genito-urinary, chest and head.
The mechanism of injury was classified as pedestrian vehicle collision, motor vehicle collision (involved as occupant), fall from height and sport injury.
Functional assessment was measured by assessing the child's functional independence in three areas: self-care, mobility and cognition. The parents of the patients who were unable to return for clinical evaluation and questioning were contacted telephonically.
Results
From January 2008 to July 2011 there were 633 trauma-related admissions to our paediatric orthopaedic unit. Twenty patients were admitted with a pelvic fracture. This represents 0.03% of all paediatric orthopaedic trauma admissions.
There were 15 boys and five girls. The average age was 8.6 years (range 3-15 years). The mean GCS at presentation was 13 (range 3-15). The mean ISS was 15 (range 4-35). The mean RTS was 9 (range 8-12). The mean hospital stay was 18 days (range 2-85 days).
Six of the 20 children were admitted to the ICU. The average stay in the ICU was eight days (range 2-28 days). Six children received an emergency blood transfusion on admission.
The most common mechanism of injury was pedestrian vehicle collision, which accounted for 14 cases. This was followed by motor vehicle collisions in which four patients were occupants. Fall from height and sports injuries had one case each.
All 20 patients had pelvic fractures evident on initial plain radiographs. Further radiographic investigations of the pelvis were undertaken in five patients. These were all done in the same five patients in whom abdominal CT scans were also performed. No additional fractures or posterior ring disruption were noted that were not already evident on the initial X-rays.
Eighty per cent of the pelvic fractures were classified as stable fractures. The majority, 13, were Torode and Zieg type 3. Two patients had type 2 injuries while only one patient suffered a Torode and Zieg type 1, with an avulsion of the anterior inferior iliac spine. The remaining four patients were type 4 injuries, with unstable pelvic ring disruptions.
Fifty-five per cent of the patients sustained one or more associated injuries. There were 10 orthopaedic and 14 non-orthopaedic injuries.
Head injuries accounted for 36% of the non-orthopaedic injuries. These included three parenchymal brain injuries, one subdural and one extradural haematoma. Injuries to the chest included two pulmonary contusions and one pneumothorax. The four patients with genito-urinary injuries included two extra-peritoneal bladder ruptures, one vaginal vault laceration and one perinephric haematoma. The abdominal injuries included two liver lacerations and one splenic laceration.
The associated orthopaedic injuries included three femur fractures (one open midshaft, one closed midshaft, one Delbet 3 neck of femur fracture); one C2 spinous process fracture; two tibia fractures; one ankle fracture; one zone 4 extensor tendon injury and one foot degloving injury.
A total of 19 surgical procedures were performed. Seventeen were orthopaedic interventions while two were non-orthopaedic procedures. The latter included an exploratory laparotomy for a liver laceration and a repair of a vaginal vault laceration.
The pelvic fractures in 17 patients were managed non-operatively. These included one unstable type 4 pelvic fracture and the 16 stable pelvic injuries.
External pelvic fixators were placed in the remaining three unstable pelvic fractures.
These patients were severely injured and were haemodynamically unstable. Wrapping the pelvis with a sheet to reduce pelvic volume was the initial intervention to provide temporary control while awaiting theatre.
Table I demonstrates the physiological instability of the three patients (patients 1, 2 and 3) with type 4 pelvic fractures who underwent emergency pelvic external fixation. Note the relative haemodynamic stability of the fourth patient (patient 4) with a type 4 pelvic fracture. This patient was treated conservatively. The rest of the patients (5-20), which include those with types 1, 2 or 3 pelvic fractures, are included as an average. They did not receive any operative intervention for their pelvic injury.
The average hospital stay of patients with a pelvic fracture in our series was 18 days (range 2-85 days). All patients were discharged home, with none being sent to a rehabilitation facility. On discharge all 20 patients were mobilising independently. Those older than 6 years were mobilised with crutches or a walking frame. Patients were only discharged once fully mobile.
The mean follow-up period was 14 months (range 5-28 months). The functional status evaluation was conducted on all 20 patients. Eleven were seen and examined by the author and nine patients' parents were interviewed telephonically.
At latest follow-up all patients were functionally independent. All patients had normal self-care and cognition. No patient required the assistance of a walking aid, and no difficulties were experienced in climbing stairs or running. There were no significant leg length discrepancies, seen on clinical evaluation or as noticed by the parents.
Four patients were still complaining of pain. Three of these had grade 1 pain and one patient had grade 2 pain. Three of the patients complaining of this residual pain had type 4 pelvic fractures. Two of the patients had sacro-iliac joint disruption, including the patient who reported the grade 2 pain. There were no mortalities in our series.
Discussion
Paediatric pelvic fractures differ from their adult counter-parts.2,3,4,7,8,12,13,20 Despite the relative paucity in the literature the disparities are obvious with regard to mechanism of injury, fracture patterns, associated injuries, functional outcomes and mortality rates. These differences may be attributed to the unique characteristics of the child's pelvis and the high energy transfer demanded to cause a fracture.
The incidence of pelvic fractures in the literature ranges from 1%-7%. However, the true incidence is most likely greater as in a study conducted on 66 post-mortem examinations of children killed as a result of blunt trauma it was demonstrated that 93% had significant pelvic ring frac-tures.3,21
Pelvic fractures in children, with the exception of avulsion injuries, occur as a result of high-energy trauma.1-8 Adults are usually injured as drivers or passengers in cars, whereas children are far more commonly hurt as pedes-trians.1-4,8,10,12,13,16,21 In our series 65% were struck by motor vehicles. Of the six patients who sustained concomitant long bone injuries, these fractures were all on the same side as the pelvic fracture indicating side impact forces as in pedestrian vehicle collisions.
Seasonal variation in the incidence of pelvic fractures has been reported.1 It has been suggested that during summer children are outdoors for longer, thus increasing the risk of a fall or pedestrian vehicle collision. In winter there remains the risk of injury through pedestrian collisions as visibility may be poorer.1 In our study, 13 patients (65%) were injured during summer months.
Great amounts of energy are required to cause a fracture in the child's pelvis. The plastic and flexible paediatric pelvis is able to undergo significant displacement before a break occurs. Thus, children have fractures occurring mostly in one area of the pelvic ring.1,4,10 This is in contrast to the double break concept as seen in adults. This is confirmed in our series as 13 patients (65%) had single fractures of the pelvis.
An increased transfer of energy also means an increased number of associated injuries and is well documented.1,3,5,7,14 We confirmed this as 55% of our patients had associated injuries.
Head injury is the most commonly sustained concomitant injury.3,5,8,18,22 Although Rang et al reported 61% concomitant head injuries in their series,3,23 our series revealed 25%. This is consistent with other authors.1,3,5 The average GCS of 13 in our series reflects the severity and regular occurrence of head injuries.
Associated abdominal or visceral injuries are reported as 20%1,3,8,10 and chest trauma as 12-20%.1,2,3,5 This was comparable in our study in which there were three patients (15%) with concomitant abdominal and three (15%) with chest injuries.
The literature describes an increase (as high as 60%)8 in abdominal injuries in multiple fractures of the pelvis. In our series, however, of the seven patients with multiple pelvic fractures only one had an associated abdominal injury. This highlights the fact that any pelvic fracture may have associated injuries.
Most literature reports have shown the same or higher incidence of genito-urinary injuries than in adults.3,5,18 Our incidence of four patients (20%) is relatively higher than the findings in adults - this, despite the fewer mechanisms of injury with anterior-to-posterior forces.
Haemorrhage is a common cause of morbidity and mortality in adults following pelvic fractures.24,25 Thirty per cent of our patients required an emergency blood transfusion. This is less than the transfusion requirements in adults, which concurs with the literature.4,8,12,14 The relative haemodynamic stability of children may be attributed to children having smaller diameter vessels that vasoconstrict more rapidly;4,10,12 fewer sacro-iliac joint disruptions; and the disproportionately high rate of single bone pelvic injuries.4,10,11
Children with an open triradiate cartilage have different fracture patterns. The pelvis with an open triradiate cartilage is immature and more likely to sustain simple ring frac-tures.4,8 This cartilage closes at about 12 years in girls and 14 years in boys. Older children will thus more commonly have acetabular fractures, multiple pelvic fractures and fractures causing a disruption of the pelvic ring.1,3,4,8 However, this was not borne out in our study. The average age of unstable pelvic fractures was 9 years. None of the patients in this group had a closed triradiate cartilage.
A direct correlation with pelvic fracture complexity and overall injury severity has been reported.3,4,7,9 This was confirmed in our review where type 4 pelvic fractures had an average ISS of 28 and RTS of 9 in comparison to the average ISS of 13 and RTS of 10 found in the remaining patients.
A modification of the pre-existing Torode and Zieg classification was proposed in 2012. Due to advancements in diagnostic techniques since this classification system was introduced in 1985, an alteration to the previously grouped 'stable' ring or type 3 fractures was made. In this new system, type 3-A fractures involve anterior fractures of the pubic rami or pubic symphysis. Type 3-B fractures are stable anterior and posterior ring fractures. These represent a more significant trauma and therefore may demand greater efforts during resuscitation and management.26
Operative interventions of paediatric pelvic fractures remain controversial23 and many authors recommend that pelvic fractures in children be treated non-operatively with successful outcomes.1,4,5,6,17,19,22 The high success rates in non-operative interventions in children are based on high union rates, extensive remodelling capacity and the favourable results gained from minimising the risk of further iatrogenic triradiate cartilage injury.3,4,9 Pelvic ring disruptions in children do well as long as leg-length inequality is <2 cm once healing is completed.4,5,19 Blasier et al in a non-randomised series of 43 patients reported no difference between operatively and non-operatively managed patients.20
If the displacement of the SI joint is >3 cm and traction is incapable of achieving adequate reduction, Canale13 recommended surgical intervention. Other texts recommend open reduction and internal fixation if there is >2 cm fracture displacement, intra-articular fractures or tri-radiate cartilage displacement >2 mm.4
Only one patient in our series may have met criteria for internal fixation, with initial SI displacement of 3 cm. However, this patient had significant haemodynamic compromise on admission which necessitated emergency external fixation and skeletal traction on the side of the SI joint disruption. He then developed acute renal failure with protracted physiological instability in ICU which precluded further operative intervention.
Conclusion
Our study confirms the low incidence of pelvic fractures in the paediatric population and the high rate of concomitant injuries. Pelvic fractures are an indicator of multi-system trauma and require a thorough systemic evaluation. We found the RTS and ISS scoring systems to be useful measurements that predict the severity of the injury.
We found the appropriate application of a pelvic external fixation device to be a valuable adjunct in the stabilisation and resuscitation of physiologically unstable patients. However, due to the infrequent need for operative intervention, we recommend that an adult pelvic trauma specialist be consulted for any severely displaced pelvic fracture that may require internal fixation.
Our review established favourable outcomes with no significant functional deficits in a series of children with pelvic fractures that were in essence managed conservatively.
No benefits in any form have been received or will be received from any commercial party related directly or indirectly to the subject of this article.
References
1. Banerjee S, Barry MJ, Paterson MH. Paediatric pelvic fractures: 10 years' experience in a trauma centre. Injury 2009;40:410-13. [ Links ]
2. Smith WR, Oakley M, Morgan SJ. Pediatric pelvic fractures. J Pediatr Orthop 2004;24:130-35. [ Links ]
3. Leonard M, Ibrahim M, McKenna P, Boran S, McCormack D. Paediatric pelvic ring fractures and associated injuries. Injury 2010;10:1-4. [ Links ]
4. Holden CP, Holman J, Herman MJ. Pediatric Pelvic Fractures. J Am Acad Orthop Surg 2007;15:172-77. [ Links ]
5. Subasi M, Arslan H, Necmioglu S, Onen A, Ozen S, Kaya M. Long-term outcomes of conservatively treated pelvic fractures. Injury 2004;35:771-81. [ Links ]
6. Signorino PR, Denomore J, Werner M, Winthrop A, Stylianos S, Guice KS, Oldham KT. Paediatric pelvic injury : functional outcome at 6-month follow-up. J Pediatr Surg2005;40:107-13. [ Links ]
7. Upperman JS, Gardner M, Gaines B, Schall L, Ford HR. Early functional outcome in children with pelvic fractures. . J Pediatr Surg 2000;35:1002-1005. [ Links ]
8. Silber JS, Flynn J M, Koffler KM, Dormans JP, Drummond DS. Analysis of the cause, classification, and associated injuries of 166 consecutine pediatric fractures. J Pediatr Orthop. 2001;21:446-50. [ Links ]
9. Musemeche CA, Fischer RP, Cotler HB, Andrassy RJ. Selective management of pediatric pelvic fractures : A conservative approach. J Pediatr Surg 1987;22:538-40. [ Links ]
10. Ismail N, Bellamane JF, Mollit DC, DiScala C, Koeppel B, Tepas JJ III. Death from pelvic fracture: Children are different. J Pediatr Surg 1996;31:82-85. [ Links ]
11. Keshishyan RA, Rozinov VM, Malakhov OA. Pelvic polyfractures in children. Radiographic diagnosis and treatment. Clin Orthop 1995;32:28-33. [ Links ]
12. Grisoni N, Connor S, Marsh E, Thompson GH, Cooperman DR, Blakemore LC. Paediatric pelvic fractures in a level-1 trauma centre. J Orthop Trauma 2002;16:410-13. [ Links ]
13. Canale ST, Beaty JH. Pelvic and hip fractures. In: Rockwood CA, Wilkens KE, Beaty JH, Editors. Fractures in Children. Vol 3. Philadelphia-Lippincott-Raven 1996, pp 991-1102. [ Links ]
14. Chawda MN, Hildebrand F, Pape HC, Giannoudis PV Predicting outcome after multiple trauma: which scoring system? Injury 2004;35:347-58. [ Links ]
15. Torode I, Zieg D. Pelvic fractures in children. J Pediatr Orthop 1985;5(1):76-84. [ Links ]
16. Gummit CL, Driscoll PA, Whitaker J et al. Trauma systems - state of the art. Resuscitation 2001;48:17-23. [ Links ]
17. Atlihan D, Ales Y, Subasi M. Surgical treatment in unstable pelvic ring fractures. Orthop Surg 1996;6:150-54. [ Links ]
18. Rieger H, Brug E. Fractures of the pelvis in children. Clin Orthop1997;336:226-39. [ Links ]
19. Lane-O'Kelly A, Fogarty F, Dowling F. The pelvic fracture management in childhood: a report supporting non operative management. Injury 1995;26:327-29. [ Links ]
20. Blasier RD, MacAtee J, White R. Disruption of the pelvic ring in paediatric patients. Clin Orthop 2000;376:87-95. [ Links ]
21. Letts M, Davidson O, Lapner P. Multiple trauma in children: predicting outcome and long term results. Can J Surg2002;45:126-31. [ Links ]
22. Reichard SA, Helikson MA, Shorter, White RI Jr, Shemeta DW, Haller JA Jr. Pelvic fractures in children -review of 120 patients with a new look at general management. J Pediatr Surg 1980;15:727-36. [ Links ]
23. Rang M. Children's Fractures, 2nd ed, Philadelphia, PA, JB Lippincourt, 1983. [ Links ]
24. Hak DJ, Smith WR, Suzuki T. Management of haemorrhage in life-threatening pelvic fractures. J Am Acad Orthop Surg 2009;17:447-57. [ Links ]
25. Guthrie HC, Owens RW, Bircher MD. Fractures of the pelvis. J Bone Joint Surg (Br) 2010;92-B:1481-88. [ Links ]
26. Shore BJ, Palmer CS, Bevin C, Johnson MB, Torode IP. Pediatric pelvic fracture: A modification of a pre-existing classification. J Pediatr Orthop 2012;32:162-68. [ Links ]
 Reprint requests:
Reprint requests:
Dr JRT Pietrzak
Email: jrtpietrzak@yahoo.com
Cell: 083 456 8090














