Servicios Personalizados
Articulo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en Google
Similares en Google
Compartir
SA Orthopaedic Journal
versión On-line ISSN 2309-8309
versión impresa ISSN 1681-150X
SA orthop. j. vol.11 no.2 Centurion abr. 2012
CASE REPORT AND REVIEW OF THE LITERATURE
Irreducible or missed lateral patellar dislocation
PLouwMMed (Orth)UFSI; NJ Jansen van RensburgMBChB USII
IConsultant, Department of Orthopaedic Surgery, University of the Free State
IIRegistrar, Department of Orthopaedic Surgery, University of the Free State
ABSTRACT
The most common direction of patellar dislocation is lateral. The dislocation is usually recognised early and easily reduced. This case report highlights a young girl in which the dislocation was not recognised and subsequently became irreducible requiring an open reduction.
CASE PRESENTATION: A 17-year-old girl sustained a lateral patellar dislocation during a twisting motion of the right knee while doing karate. On clinical examination the patient had a lateral patellar dislocation but the initial radiographs appeared fairly normal. Pre-operative CT examination confirmed the diagnosis. Closed reduction failed necessitating an open reduction. The lateral retinacular defect after reduction of the patella was filled using the anterior half of the iliotibial band. Eighteen months following surgery the patella was stable and the patient regained a good range of motion.
CONCLUSION: Lateral patellar dislocation may be subtle and misdiagnosed. Not obtaining the necessary radiographs may contribute to not diagnosing the condition. Doubtful cases should have a CT scan to confirm the diagnosis. Mobilising part of the ITB is a viable option to obtain healthy living tissue to cover a lateral retinacular defect.
Key words: Irreducible, patella, dislocation, knee, ITB graft
Case report
In 2009, a 17-year-old girl presented at our hospital complaining of a painful right knee. She reported injuring her knee during karate training one month prior. She was performing a kick with the left leg and sustained twisting injury to the supporting right leg. She presented to her local emergency department where she was diagnosed with a soft tissue injury to the knee. Initially she received a bandage to the knee, which she wore for two weeks. This was subsequently changed to a plaster of Paris cast for a further three weeks. She reported to our department two weeks following removal of plaster of Paris.
Physical examination revealed a lower limb with normal alignment. The right knee appeared swollen. The knee was not very tender to touch. The knee was not warm. Active and passive flexion was limited to 15° and was painful. The medial collateral ligament and lateral collateral ligament was intact. The patella was subluxed laterally (Figures 1 and 2).
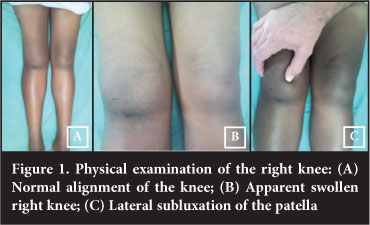
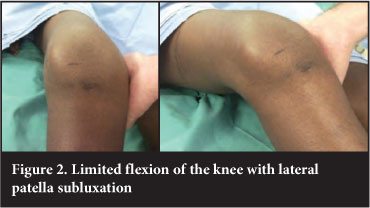
Radiographic examination included plain AP and lateral radiographs (Figure 3). On the AP view, the patella appeared slightly laterally displaced from the normal position and on the lateral the patella was not obviously displaced. Further evaluation included a computed tomography scan which confirmed lateral dislocation of the patella with an abnormally concave medial facet of the patella, at 90° to the lateral facet (Figure 4). In addition the femoral sulcus is flat, measuring 166°, in keeping with Dejour grade A trochlear dysplasia. The tibial tubercle-trochlear groove (TT-TG) distance could not be measured.
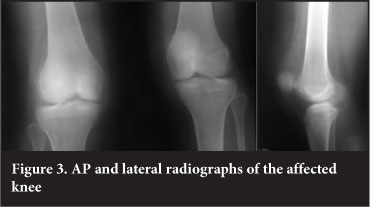
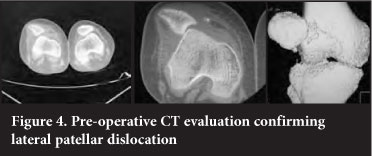
An attempt at closed reduction in Casualty and later under general anaesthesia was unsuccessful and we proceeded to open reduction of the patella through an anterior approach.
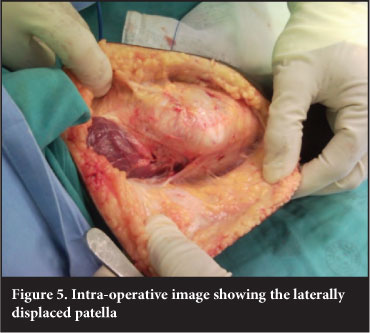
The patient was scheduled for closed reduction under anaesthesia; this was unsuccessful and we proceeded to open reduction of the patella (Figure 5). To achieve reduction of the patella a lateral retinacular release was performed. The patella returned to its normal position and full passive flexion was obtained without resistance. It was evident that there was an impaction injury on the lateral aspect of the lateral femoral condyle with eroded cartilage, but the patella appeared crossly uninjured. Secondary to the prolonged lateral dislocated position, the lateral retinaculum was contracted and after reduction there was a retinacular defect of no less than 1.5 cm by 5 cm. On the medial side the retinaculum was stretched and redundant following reduction.
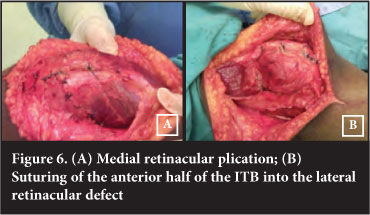
In order to achieve and maintain stability the medial retinaculum was plicated (Figure 6). We were still confronted with the soft tissue defect on the lateral side. To obtain closure of this gap the anterior half of the iliotibial band was mobilised and sutured into position. The decision to fill the gap was made to prevent the development of a persistent synovial fistula and drainage as has been experienced in a previous patient. To assess the likelihood of a fistula developing we injected normal saline intra-articular. There was no leakage of fluid through either medial or lateral suture lines. Intra-operative passive range of motion showed the patella to be tracking normally.
Post-operatively, the knee was managed with a knee ranger. The knee was kept in full extension for the first two weeks post-operatively and afterwards the amount of flexion was gradually increased over the next two weeks. The patients post-operative course was complicated by a superficial skin infection which was managed with wound care and subsequently resolved. Post-operative rehabilitation was unsatisfactory and prolonged both as a result of a lack of resources and patient compliance.
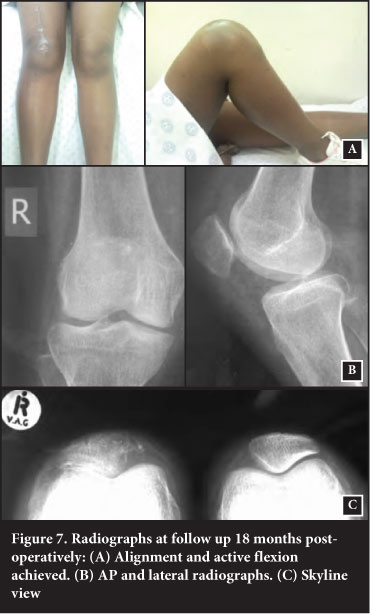
The patient saw us again for follow-up 18 months following the initial surgery. She did not return to sport participation but the knee was largely asymptomatic. She regained approximately 110° of knee flexion. The patella was stable as assessed with the apprehension test. Radiographs showed the patella in a satisfactory position but with residual lateral inclination on the skyline view and a concave medial patella facet with some new bone formation at the attachment to the retinaculum. The angle between medial and lateral facets measures 86° on the dislocated side compared to 114° on the normal side (Figure 7).
Discussion
Several directions of patella dislocation have been described, with the lateral patellar dislocation being the most common. It is usually easily diagnosed and reduced. Probably many patellar injuries which by history sound like lateral patellar dislocations either reduce spontaneously following knee extension, or are reduced at the scene by the individual or bystanders with minimal effort. A missed/irreducible lateral patellar dislocation however is rare. A search of the literature showed only a few articles related to irreducible lateral patellar dislocation.1-3 Other irreducible dislocations of the patella mentioned in the literature include superior dislocation,4,5 intra-articular dislocation of the patella,6,7 patellar dislocation with rotation around the vertical axis8,9 and lateral patellar dislocation with impaction fracture of the patella.
In this case the lateral patella dislocation was not noticed initially. This was followed by a prolonged period of immobilisation. Failure to reduce spontaneously in this patient, despite fully extending the knee, may have been due to the abnormal form and orientation of the medial facet of the patella.
It is possible but unlikely that the patellar changes noted were caused by an impaction fracture because it appeared grossly intact while there were definite articular changes noted to the corresponding area of the lateral femoral condyle. The delay in reduction resulted in contracture of the lateral and stretching of the medial retinacular tissue. Following release of the lateral retinaculum and reduction of the patella a substantial lateral gap was evident. Use of the ITB did not interfere with its function as a lateral stabiliser of the knee.
Conclusion
Lateral patellar dislocation may be subtle and misdiagnosed. Not obtaining the necessary radiographs may contribute to not diagnosing the condition. Doubtful cases should have a CT scan to confirm the diagnosis. We think that mobilising part of the ITB is a viable option to obtain healthy living tissue to cover a lateral retinacular defect.
Consent
Informed consent was obtained from the patient and her guardian to use the case and pictures for publication.
Competing interests
The authors have no conflicting interests.
References
1. PM Phaltnakar, SH Bridle. Locked lateral patellar dislocation with impaction fracture of the patella. Ann R Coll Surg Engl 2002;84:125-26. [ Links ]
2. RJ Feibel, N Dehghan, AA Cwinn. Irreducible lateral patella dislocation: the importance of impaction fracture recognition. J EmergMed 2007 Jul;33(1):11-15. [ Links ]
3. Hackl W, Benedetto KP, Fink C, Sailer R, Rieger M. Locked lateral patellar dislocation: a rare case of irreducible patellar dislocation requiring open reduction. Knee Surg Sports Traumatol Arthrosc. 1999;7(6):352-55. [ Links ]
4. DH Bartlett, LA Gilula, WA Murphy. Superior dislocation of the patella fixed by interlocked osteophytes. JBJS Sept 1976;58-A, no 6. [ Links ]
5. RS Bassi, BA Kumar. Superior dislocation of the patella; case report and review of literature. Emerg Med J 2003;20:97-98 [ Links ]
6. EK Frangakis. Intra-articular dislocation of the patella. JBJS March 1974; 56-A, no 2. [ Links ]
7. RA Dimentberg. Intra-articular dislocation of the patella: case report and literature review. Clin J Sport Med 1997 7:126-28 [ Links ]
8. F Michels, N Pouliart, D Oosterlinck. J Med Case Reports 2008; 2:371 [ Links ]
9. VT Inman, BW Smart. Irreducible lateral dislocation of the patella with rotation. JBJS July 1941:Vol XXIII, No 3. [ Links ]
 Reprint requests:
Reprint requests:
Dr NJ Jansen van Rensburg
Department of Orthopaedic surgery
University of the Free State
National hospital
Private BagX20598
Bloemfontein 9301














