Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
SA Orthopaedic Journal
versão On-line ISSN 2309-8309
versão impressa ISSN 1681-150X
SA orthop. j. vol.11 no.2 Centurion Abr. 2012
CASE REPORT AND REVIEW OF THE LITERATURE
MRI findings of cyclops lesions of the knee
C Minné MBChB (Pret)I; FC Rad Diag (SA)I; MMed Rad D (UL)I; MD Velleman MBChB (Pret)II; FC Rad Diag (SA)II; MMed Rad D (Pret)II; FE Suleman MBChB (Natal)III; FC Rad Diag (SA)III; MMed Rad D (UL)III
IUniversity of Pretoria, Department of Radiology
IIRadiologist, Little Company of Mary Hospital
IIIUniversity of Pretoria, Department of Radiology
ABSTRACT
Cyclops lesions develop in the anterior aspect of the intercondylar notch typically after anterior cruciate ligament (ACL) reconstruction or injury. It is a lesion consisting of fibrous tissue with or without cartilage and bony components. A cyclops lesion is one of the causes for reduced extension and, in the cases reported here, also knee pain or discomfort after ACL reconstruction. We present the MRI features, particularly the features on proton density weighted turbo spin echo (PDW TSE) and proton density weighted turbo spin echo fat saturation (PDW TSE FS) sequences of four cases of cyclops lesions, and distinguish between the MRI findings of large and small lesions. We also describe a cyclops lesion after a posterior cruciate ligament reconstruction, not described in literature before.
Key words: Cyclops lesion, arthrofibrosis, ACL repair complication, PCL repair complication, motion loss, knee stiffness, post-operative knee pain
Introduction
Cyclops lesions or focal anterior arthrofibroses are lesions that develop in the anterior aspect of the intercondylar notch, typically after anterior cruciate ligament (ACL) reconstruction or injury. They are lesions consisting of fibrous tissue with or without cartilage and bony components. Cyclops lesions are one of the causes for reduced extension after ACL reconstruction; however, in three out of four cases reported here, knee pain and discomfort was the main complaint. We present cyclops lesions in four patients, including a patient with a previous posterior cruciate ligament (PCL) repair, which has not been described in literature.
Case 1
A 23-year-old male patient had a single bundle bonepatellar tendon-bone ACL reconstruction three weeks after a rugby injury. Four months after ACL reconstruction he presented with complaints of intermittent knee locking and posterior knee pain. An MRI of the right knee was done to investigate the cause.
The MRI (Figure 1 a and b) demonstrated an intact ACL repair, patellar tendon thickening, small supra-patellar effusion, synovitis in the region of Hoffa's fat pad and a cyclops lesion (2.8 ÷ 2.8 ÷ 1.5 cm) anterior to the ACL in the intercondylar notch of the femur. The lesion demonstrated a mild heterogeneous intermediate signal that was higher than muscle on proton density weighted turbo spin echo (PDW TSE) sequences (Figure 1a).
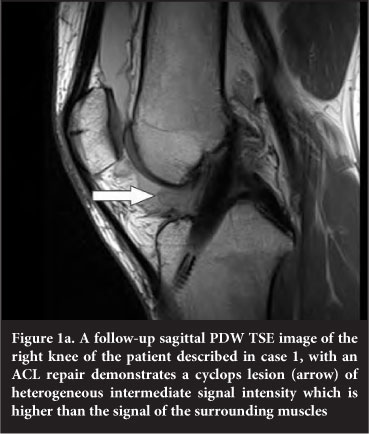

It was heterogeneous and hyperintense with a low signal intensity rim on proton density weighted turbo spin echo fat saturation (PDW TSE FS) sequences (Figure 1b). The lateral collateral ligament was thickened and oedematous due to the previous repair. No impingement was demonstrated to account for any of the clinical features. Arthroscopy revealed a cyclops lesion.
Case 2
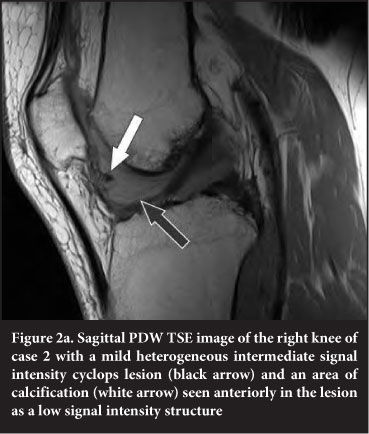
A 36-year-old male presented with knee pain and a history of previous posterior cruciate ligament (PCL) repair. MRI of the right knee, done to find the cause for the knee pain (Figure 2a and b), revealed patellar tendon thickening and traction changes, a small effusion and synovial thickening in the supra-patellar bursa. The patellar cartilage was thinned and degenerative. Mild thinning of the femoral condyle cartilage with early osteophyte formation was observed. The posterior horn of the medial meniscus had signal disturbance and morphology indicating previous surgery or injury. The lateral meniscus had a small vertical tear in the peripheral zone with an associated para-meniscal cyst. Both ACL and PCL had signal changes but were intact. The PCL was thickened. A cyclops lesion (2.8 ÷ 2.7 ÷ 1.6 cm) was noted anterior to the ACL in the intercondylar notch and mild synovitis was present in the region of Hoffa's fat pad. The cyclops lesion was heterogeneous on all sequences with a hypo-intense rim. There was mainly hyperintense signal on PDW TSE FS (Figure 2a) and a mildly heterogeneous intermediate signal higher than muscle on PDW TSE sequences (Figure 2b). A very low signal intensity nodule was seen within the lesion along the antero-superior border. A cyclops lesion was confirmed and excised at arthroscopy.

Case 3
A 27-year-old male presented with anterior knee pain without knee lock or extension block seven months after an ACL repair. MRI of the right knee (Figure 3) showed a thickened patellar tendon, supra-patellar effusion, bone contusion and oedema in the anterior aspect of the tibial plateau as well as anterior and superior to the bony tract of the ACL repair. The repaired ACL was intact. A cyclops lesion (2.2 ÷ 1.4 ÷ 2.4 cm) was seen anterior to the ACL in the intercondylar notch. The lesion demonstrated a mild heterogeneous intermediate signal that was higher than muscle on PDW TSE sequences. It was heterogeneous hyperintense on PDW TSE FS sequences. A subsequent arthroscopy revealed a cyclops lesion correlating with the MRI findings.

Case 4
A 22-year-old male athlete with a previous ACL reconstruction and medial meniscus repair presented after a re-injury. He complained only of lateral knee discomfort. An MRI of the left knee demonstrated thickening of the patel-lar tendon, a small supra-patellar effusion, bone oedema and contusion in the postero-lateral tibia. There was thinning of the cartilage over the medial and lateral femoral condyles and signal disturbance in the posterior horn of the medial meniscus due to previous meniscus repair. A small cyclops lesion (0.9 ÷ 0.9 ÷ 1.1 cm) was seen at the apex of Hoffa's fat pad anterior to the ACL in the inter-condylar notch. It was heterogeneous and isointense to muscle on the PDW TSE sequences (Figure 4), isointense to muscle on the PDW TSE FS sequences and hyperintense on short tau inversion recovery (STIR) sequences.

The lesion contained a bony fragment seen as a high signal intensity structure with a very low signal intensity rim within it. The repaired ACL was intact. The cyclops lesion demonstrated on MRI was confirmed and excised at arthroscopy.
Discussion
Loss of knee extension is a post-operative complication of ACL reconstruction. The most common cause for impaired knee extension is graft impingement, followed by cyclops lesions, also known as localised arthrofibrosis.1,2 Other causes include excessive graft tension, nonanatomical graft position, inadequate rehabilitation, fibrosis of the fat pad, supra-patellar and intercondylar adhesions, entrapment of the patella and capsular con-tracture.1,3
A cyclops lesion is an intra-articular fibrous nodule at the anterior edge of the intercondylar notch anterior to the ACL.1,4 It is most frequently seen after ACL reconstructive surgery but has also been reported after injury. The reported frequency of cyclops lesions after ACL graft reconstruction is 1%-10%.2 Arthroscopically the cyclops lesion is a nodule with a focal area of reddish-blue discoloration due to vascular channels.1
The pathogenesis of a cyclops nodule is not certain but is most likely multi-factorial. Jackson and Schaefer postulated that debris raised by drilling of the tibial tunnel, or broken graft fibres, gives rise to a cyclops lesion. However, Marzo et al suggested micro-trauma from graft impingement.1,5 Histologically the cyclops lesion has a centre of granulation tissue surrounded by dense fibrous tissue.1,6 As the lesion matures it develops fibrocartilaginous tissue and may also contain bone, synovium, fat and fibrous tis-sue.1,2,4 These lesions may originate from one of the following: the ACL graft, a residual ACL stump, a tibial tunnel trap door, intercondylar fibrosis or metaplasia in Hoffa's fat pad.2,4
Cyclops syndrome is diagnosed when a patient has a cyclops nodule demonstrated by MRI and presents with loss of knee extension. Cyclopoid scars on the other hand contain only fibroproliferative tissue and do not prevent full extension.5 Only the first case presented here had intermittent knee locking and would thus be regarded as cyclops syndrome; the other cases only presented with knee pain or discomfort without knee lock or flexion deformity and thus only qualify as cyclopoid scars.
The second case in the described case series developed a cyclops lesion after a PCL repair. This is most unusual as no other case report could be found in the literature of a cyclops lesion following a PCL repair.
MRI sensitivity to diagnose a cyclops lesion in general is reported as 85%, specificity as 84.6% and accuracy of 84.8 %.4 Larger lesions (more than 1cm in at least one dimension) increases specificity to 100% and accuracy to 91% but sensitivity remains 85%. The content of a cyclops nodule will determine its MRI appearance and therefore there is a variety of possible signal intensities. The most commonly reported appearances are: low-to-intermediate signal intensity on T1-weighted sequences, heterogeneous or intermediate signal intensity on T2-weighted sequences and intermediate-to-high signal intensity on PDW sequences.1,2,4,5,7,8 In the case series reported here, the large cyclops lesions (cases 1, 2 and 3) have a similar MRI appearance to each other while the small lesion in case 2 differs from the rest. Large cyclops lesions are reported in the literature to have heterogeneous high signal intensity on PDW TSE FS as in our patients with large lesions. They have slightly heterogeneous intermediate signal intensity on PDW TSE but with higher signal intensity than muscle. The small cyclops lesion in case 4 had a homogeneous signal intensity isodense to muscle on PDW TSE FS and PDW TSE. This lesion also had a central bony component seen as a high signal intensity structure with a very low signal intensity rim. No link could be found in the literature between the aetiology, the size of the cyclops lesion and the presence of a bony component.
The type of reconstruction must also be taken into account when evaluating the MRI of a patient who had an ACL reconstruction as a remnant bundle reconstruction can mimic a cyclops lesion.9 None of the patients presented here, however, had a remnant bundle reconstruction.
Conclusion
Cyclops lesions are the second most common reported cause for loss of knee extension after ACL repairs, although not a frequent finding. In this case series knee pain was a more prominent feature than loss of knee extension. A cyclops lesion can thus be a cause for knee pain and discomfort after cruciate ligament reconstruction and should therefore be excluded in patients presenting with persistent knee pain post-operatively. Furthermore this is the first description of a cyclops lesion after a PCL repair that we are aware of and indicates that cyclops lesions are not exclusively found after ACL reconstructions.
References
1. Dhanda S, Sanghvi S, Pardiwala D. Case Series: Cyclops lesion - Extension loss after ACL reconstruction. (muscu | loskeletal). Indian J of Radiol and Imaging. 2010;20:208. [ Links ]
2. Giaconi JC, Allen CR, Steinbach LS. Anterior cruciate liga | ment graft reconstruction clinical, technical and imaging overview. Top Magn Reson Imaging. 2009;20:129-50. [ Links ]
3. Austin JC, Phornphutkul C, Wojtys EM. Loss of knee exten | sion after anterior cruciate ligament reconstruction: Effects of knee position and graft tensioning. J Bone joint Surg Am. 2007;89:1565-74. [ Links ]
4. Bradley DM, Bergman AG, Dillingham MF. MR imaging of cyclops lesions. Am J of Roentgenol. 2000;174:719-26. [ Links ]
5. Runyan BR, Bancroft LW, Peterson JJ, Kransdorf MJ, Berquist TH, Ortiguera CJ. Cyclops lesions that occur in the absence of prior anterior ligament reconstruction. Radiographics. 2007 August 21 [cited 2011 July 21];27 (e26):1. Available from: http://radiographics.rsna.org/con j tent/2 7/6/e26.full?sid=138a191b-7c30-4dff-90f1- j efff0ab864a9
6. Creighton RA, Bach BR. Arthrofibrosis: evaluation, prevention and treatment. Techniques in knee surgery. 2005;4:163-72. [ Links ]
7. Miller TT. MR imaging of the knee. Sports Med Arthrosc Rev. 2009;17:56-64. [ Links ]
8. Recht MP, Kramer J. MR imaging of the postoperative knee: A pictorial essay. Radiographics. 2002;22:765-74. [ Links ]
9. Cha J, Choi S-H, Kwon JW, Lee S-H, Ahn JH. Analysis of cyclops lesions after different anterior cruciate ligament reconstruction: a comparison of the single-bundle and remnant bundle preservation techniques. Skeletal Radiol. 2012 January 05 [cited 2012 May 01]; DOI 10.1007/s00256-011-1347-4: [6 p.]. Available from: http://www.springerlink.com/content/1v6716m04jw70p1u/
 Reprint requests:
Reprint requests:
Dr Cornelia Minné
Email: riaminne@gmail.com
Cell: 073 228 8031














