Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
SA Orthopaedic Journal
versão On-line ISSN 2309-8309
versão impressa ISSN 1681-150X
SA orthop. j. vol.11 no.2 Centurion Abr. 2012
CLINICAL ARTICLE
No loosening of an uncemented acetabular component at a minimum of 15 years
Nicolas Martin MBChB, FCS(Orth); Marc Nortje MBChB, FC Orth, MMed; Brendan Dower MBChB, FCS(Orth); Ian Learmonth MBChB, FRCS(Orth); Garth Grobler MBChB, FCS(Orth), MMed
ABSTRACT
One hundred consecutive total hip replacements using a cementless Duraloc 300 cup were reviewed at a minimum of 15 years. All acetabular metal components were found to be stable with no evidence of loosening.
Key words: Hip, arthroplasty, acetabular, loose, fixation
Introduction
In our previous 10-year review of these patients we found a zero rate of loosening and a mean polyethylene wear rate of 0.12mm per year.1
The purpose of this paper is to retrospectively review the ongoing radiological results of this cohort of consecutive total hip replacements.
Patients and methods
Between August 1991 and July 1993, we performed 100 consecutive total hip replacements in 93 patients (48 men and 45 women). Two experienced hip surgeons performed 93 operations and seven were undertaken by registrars under supervision. The surgery was performed via a modified anterior approach as previously described.1 The Duraloc 300, tri-spiked, Porocoat acetabular implants were used with a polyethylene liner containing a 10° long wall, that was gamma irradiated in air.
Of the original 100 hips, 35 patients died (37 hips) at an average of seven years post surgery. None of these patients had undergone a re-operation and all had a satisfactory fixation of the acetabular cup as seen on radiographs taken on average 1.7 years before death. Six patients (seven hips) were lost to follow-up leaving 56 hips available for analysis after a minimum duration of follow-up of 15 years.
The patients' radiographs (post-operative, 10 year, 15 year) were analysed with respect to loosening,2,3 liner wear,4,5 granuloma evolution6 as well as bone graft incorporation post liner revision. Migration or position of the liner was assessed according to the method of Massin et al.3
Results
At 15-year follow-up none of the acetabular implants showed any evidence of loosening. We defined loosening as cup migration or lucent lines of more than 1 mm diameter present in all three zones (as per Hodgkinson et al.2).
The average wear at 15-year follow-up was 0.08 mm/y. This was less than the 0.12 mm/y at 10-year follow-up. Fourteen hips had granulomas at 15-year follow-up. Eleven of these granulomas were situated in zone 2, which may be related to the fact that a hole eliminator had not been used in these cups.
Eleven patients required revision surgery. Two had well-fixed cups removed at the time of stem revision at another institution, one had the long wall repositioned for early dislocation, five had liner revision and underwent impaction bone grafting to granulomas, three had liner exchange for excessive wear without granuloma present.
Four of these revisions took place in the last 5 years. Three were liner revisions only (two for excessive wear, one during granuloma bone-grafting), while one had the liner changed during revision of a loose stem post periprosthetic fracture.
In the five hips that were revised for granuloma around the cup, all showed good graft incorporation and remodelling. There were no complications related to the revision surgery.
Statistics
Kaplan-Meier survivorship analysis was performed with radiological loosening and liner revision as an end point. The survival at 15 years for loosening was 100%. The survival for liner revision was 84.93% (95% confidence interval of 76.02-93.83%)
Discussion
The zero radiological loosening rate of the Duraloc 300 cups at 15 years would indicate that spiked Porocoated cups provides sufficient bone in-growth for long-term stability even in cases with granuloma formation.
The wear rate of 0.08 mm/year is less than the one found at 10-year follow-up. We assume that this decrease is due to a combination of decreased activity levels in the ageing study cohort as well as less statistical impact of the initial running-in wear over the extended time period.7
The predominance of zone 2 granuloma indicates that wear particles gained entry to the bony acetabulum via the apex hole for the cup introducer. Use of a hole eliminator would be prudent (Figures 1-4).
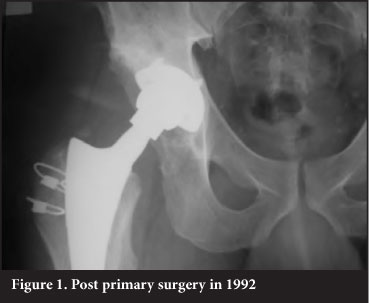
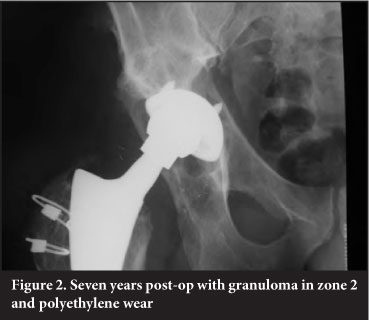
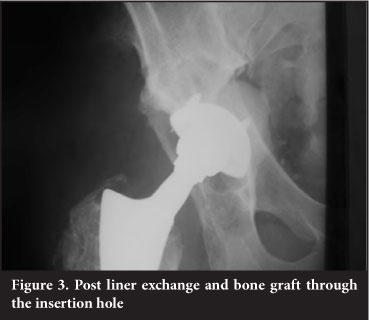
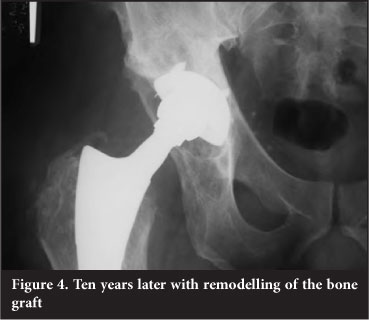
The cases that required liner revision and bone grafting were easy to perform and in all cases graft material showed evidence of incorporation.
At 15 years all surviving patients had well-fixed, functioning acetabular components.
Improvements in bearing surfaces may improve wear rates and granuloma formation in the future but fixation rates cannot be improved. If we solve the problem of wear, could joint replacement surgery offer a permanent solution?
References
1. Grobler GP, Learmonth ID, Bernstein BP, Dower BJ. Ten-year results of a press fit, porous-coated acetabular component. J Bone and Joint Surg (Br) 2005;87-B:786-89. [ Links ]
2. Hodgkinson JP, Shelley P, Wroblewski BM. The correlation between the roentgenographic appearance and operative findings at the bone-cement junction of the socket in Charnley low friction arthroplasties. Clin. Orthop. 1988; 228:105-109. [ Links ]
3. Massin P, Schmidt L, Engh CA. Evaluation of cementless acetabular component migration. An experimental study. Journal of Arthroplasty. 1989;4:245-51. [ Links ]
4. Hui A, McCalden R, Martell J, MacDonald S, Bourne R, Rorabeck L. Validation of two and three dimensional radiographic techniques for measuring polyethylene wear after total hip arthroplasty. Journal of Bone and Joint Surgery [Am]. 2003;85-A:3;505-11. [ Links ]
5. Martell J, Berdia S. Determination of polyethylene wear in total hip replacements with use of digital radiographs. Journal of Bone and Joint Surgery [Am]. 1997;79:1635-41. [ Links ]
6. De Lee JG, Charnley J. Radiological demarcation of cemented sockets in total hip replacements. Clinical Orthopaedics. 1976;121:20-32. [ Links ]
7. Garvin KL, Hartman CW, Mangla J, Murdoch N, Martell JM. Wear analysis in THA utilizing oxidized Zirconium and crosslinked polyethylene. Clin Orthop Relat Res 2009:467;141-14. [ Links ]
 Reprint requests:
Reprint requests:
Dr M Nortje
Department of Orthopaedic Surgery
University of Cape Town H 49 OMB
Groote Schuur Hospital Observatory,
7700 Cape Town South Africa
Tel: +27 21 4045108
Email: mbnortje@yahoo.com














