Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SA Orthopaedic Journal
On-line version ISSN 2309-8309
Print version ISSN 1681-150X
SA orthop. j. vol.11 n.2 Centurion Apr. 2012
CASE REPORT AND REVIEW OF THE LITERATURE
Ultrasound diagnosis of femoral nerve neurostenalgia: a cause of hip pain in a young adult
Z OschmanI; A KoekemoerII
IMBChB, MSc Sports Medicine, University of Pretoria
IIMBChB, University of Pretoria
ABSTRACT
Femoral neurostenalgia is a compressive neuropathy which is an uncommon cause of hip pain in active young adults. Compression of the nerve can cause debilitating pain and an inability to walk. Correct clinical diagnosis and correct treatment can result in complete relief of symptoms. We present a case of a young female with a spontaneous acute onset of severe hip pain for ten months. After seeing several specialists and having undergone numerous special investigations, femoral nerve compression by the iliopsoas was demonstrated on ultrasound, but only confirmed during surgery for a suspected femoral hernia. After decompression of the nerve the patient was completely pain free.
Keywords: Femoral nerve, neurostenalgia, compressive neuropathy, entrapment, ultrasound
Introduction
Hip pain in young adults is often characterised by nonspecific symptoms; it is often difficult to identify the source and mechanism of pain and to determine the correct treatment.1 Femoral nerve neurostenalgia is an uncommon cause of hip pain in young adults; compression of the nerve can cause debilitating pain and an inability to walk.2 Several peripheral nerves are susceptible to entrapment, which is most commonly due to their anatomic position in relation to muscles, ligaments, bones or retinaculae.3 These entrapments are usually self-limiting, but persistent symptoms can cause severe morbidity and necessitate surgical intervention.4
In the hip the most frequently described peripheral nerve entrapments include the sciatic nerve by the piriformis and the lateral cutaneous nerve by the inguinal ligament near its attachment to the anterior superior spina iliaca known as meralgia paraesthetica.3 Entrapment of the femoral nerve is uncommon and usually low down on the differential diagnoses list, particularly in active young adults, where it is more frequently caused by athletic injuries, trauma, hip pathology and referred pain.
A missed diagnosis may lead to prolonged discomfort, debilitating pain and a delay to an athlete's return to sport. An accurate history and clinical examination is important in diagnosing femoral nerve entrapment and ruling out other causes.2 According to the literature search, ultrasound diagnosis of femoral nerve neurostenalgia by the iliopsoas has not been described before.
Case report
An active 24-year-old female nursing student who jogs every day presented in April 2010 with an acute spontaneous pain in her left groin and leg after a two-hour flight. The leg felt heavy/'dead' and appeared swollen. The pain was so severe that she had great difficulty in walking. A venous duplex Doppler of the leg revealed no thrombus; the veins were reported as patent with normal compressibility and flow. Blood investigations including thrombotic work-up were normal. X-rays of the lumbar spine and femur, MRI of the femur and a bone scan did not show any abnormalities.
The debilitating symptoms persisted; in June 2010 a neurosurgeon referred her for a MRI of the pelvis and spine, which was reported as normal.
In October 2010 she consulted a neurologist, and although the EMG results were normal he indicated that her clinical presentation was suggestive of a femoral neuropathy and referred her for an ultrasound examination. In December 2010 the ultrasound examination revealed femoral nerve neurostenalgia by the iliopsoas muscle. The nerve was thickened with a round appearance and located deep between the iliopsoas and the femoral vessels (Figure 1). Normally the femoral nerve is located superficial to the iliopsoas muscle with a flatter appearance (Figure 2). No atrophy of the quadriceps muscles was seen at this stage; the appearance and thickness was similar to the opposite side.
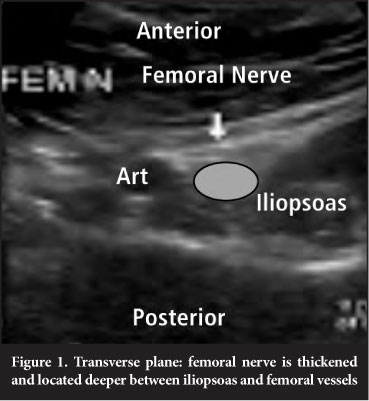
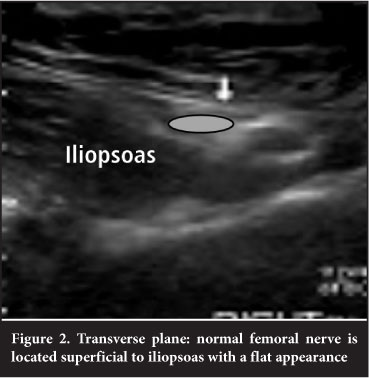
In January 2011 the neurologist referred her to an orthopaedic surgeon who referred her to a general surgeon who suspected a femoral hernia and had her booked for a hernia repair. No hernia was found, but it was discovered that the femoral nerve was entwined and impinged by iliopsoas. A 15 cm release was done and the nerve repositioned superficial to the iliopsoas. With her discharge she did not have the tremendous pain she had experienced for almost ten months. Her recovery was rapid and with the removal of the stitches she was completely pain free with only a slight loss of sensation in the right leg.
Discussion
The femoral nerve is the largest branch of the lumbar plexus.4 It is formed by the posterior divisions of the ventral rami of L2, L3, L4 and occasionally L1and/or L5. It emerges from the lateral margin of the psoas and descends in a groove between the psoas and iliacus deep to the iliac fascia and passes underneath the inguinal ligament lateral to the femoral artery to enter the thigh.3 The femoral nerve, iliacus, psoas and femoral vessels occupy a tight compartment bounded by the iliac fascia.5
After extending from the pelvis the femoral nerve divides into motor branches supplying muscles of the thigh and sensory branches supplying the skin of the medial and anterior thigh and medial calf down the to the ankle.4
The 'critical zone' of femoral entrapment has been described as the fibro-muscular ring that is bound anteriorly by the inguinal ligament, posteriorly by the iliopsoas, and medially by the iliopectineal band; the space between the psoas and iliacus has also been regarded as a zone of 'entrapment risk'.3
The most frequent cause of femoral nerve injury is iatrogenic and has been reported after hip arthroplasties, obstetric and gynaecological procedures, renal transplants, femoral artery surgery, and inguinal and femoral hernia repairs.5 Entrapment has also been described in cyclists and dancers, and after a drunken stupor dubbed as 'hanging leg syndrome'.6 Natelson also described a number of cases with compression of the femoral nerve by the iliopectineal ligament that was solved by surgical release.6 Vazquez et al were the first to describe femoral nerve entrapment due to its relationship with the muscular fibres of the iliopsoas. In a study of 121 cadavers they found in 89.5% that the femoral nerve was split by a muscular slip or sheet and in 10.5%, it was covered by a muscular slip.3
Nerve entrapment results in pain, often severe and debilitating, with weakness and numbness in the sensory distribution of the nerve. The pain varies from case to case, from dull and aching to intermittently severe and burning, and can cause an inability to walk or stand without help.3,4
A complete history and physical examination may indicate whether pain is intra-articular, extra-articular or referred. Special investigations include X-rays, computed tomography, bone scans, EMG, MRI and ultrasound. X-rays and MRI are the preferred initial imaging modalities. Analysis of blood, urine and synovial fluid can help diagnose inflammation, infection and systemic rheumatologic diseases.1
Conclusion
Femoral nerve neurostenalgia is an uncommon cause of hip pain in an active young adult. As seen in this case study a missed diagnosis resulted in more than 10 months of discomfort, significant physical disability and emotional stress. Diagnoses of femoral nerve neurostenalgia can be made clinically by the history of dysaesthesia of the anterior thigh, weakness of hip flexion and a Tinel sign on clinical exami-nation.2
The patient saw five specialists (orthopaedic surgeons, a neurosurgeon, a neurologist and a general surgeon) and had several special investigations including MRIs, a bone scan and EMG without resulting in a diagnosis. It was only after surgery for a suspected femoral hernia that the diagnosis of femoral nerve neurostenalgia as demonstrated on ultrasound was confirmed. After decompression of the nerve she was completely pain free and able to finish her nursing degree a year later. This case serves as a reminder of the importance of a complete history and clinical examination.
References
1. Traum OM, Crues JV. The young adult with hip pain: diagnosis and medical treatment circa 2004. Clin Orthop 2004;418:9-17. [ Links ]
2. Phang ISK, Biant LC, Jones TS. Neurostenalgia of the femoral nerve: a treatable cause of intractable hip pain in a young adult. J Athroplasty 2010;25(3):498. [ Links ]
3. Vázques MT, Murillo J, Maranillo E, et al. Femoral nerve entrapment: a new insight. Clin Anat 2007;20:175-79. [ Links ]
4. Seid AS, Amos E. Entrapment neuropathy in laparoscopic herrniography. Surg Endos 1994;8:1050-53. [ Links ]
5. Garcia-Urena MA, Vega V, Rubio G et al. The femoral nerve in the repair of inguinal hernia: well worth remembering. Hernia 2005;9:384-87. [ Links ]
6. Natelson SE.Surgical correction of proximal femoral nerve entrapment. Surg Neurol 1997;48:326-29. [ Links ]
 Reprint requests:
Reprint requests:
Dr Zanet Oschman
Jakaranda Hospital
Room 102 Muckleneuk, Pretoria
Tel: (012) 343 5003
Fax: (012) 343 0277
Email: zanet@mweb.co.za














